Best GLP-1 Providers for Prior Authorization — 2026 Verified Guide
Best GLP-1 Providers That Help With Prior Authorization (2026)
If you’re looking for the best GLP-1 providers that help with prior authorization, here’s the short answer: Ro is the strongest choice for most commercially insured adults. We scored nine telehealth platforms on PA support depth, and Ro had the clearest documented concierge — a dedicated team that checks your coverage, submits PA paperwork on your behalf, communicates with your insurer, and pivots you to FDA-approved cash-pay GLP-1s starting at $149/month if insurance doesn’t come through.
If you want in-network obesity care or need a Medicare-friendly provider, Form Health is the stronger fit — its care team submits prior authorizations and advocates for patients, all billed through insurance.
But here’s the part nobody tells you: “accepts insurance” and “handles prior authorization” are not the same thing. Some providers only check whether your plan covers GLP-1s. Some submit the actual PA paperwork. Some fight denials and file appeals. And some — including well-known names — have contradictory policies depending on which program you join.
If your plan flatly excludes weight-loss GLP-1s — meaning the drug category itself isn’t covered, not just that you haven’t been approved yet — prior authorization won’t help you. Jump to your non-insurance options →
Free GLP-1 Insurance Coverage Check — Ro
Ro’s coverage checker shows your plan’s GLP-1 coverage before you pay anything. If you qualify, their concierge handles the full PA process.
Check your GLP-1 insurance coverage on Ro ↗Free coverage check — no commitment, no prescription required
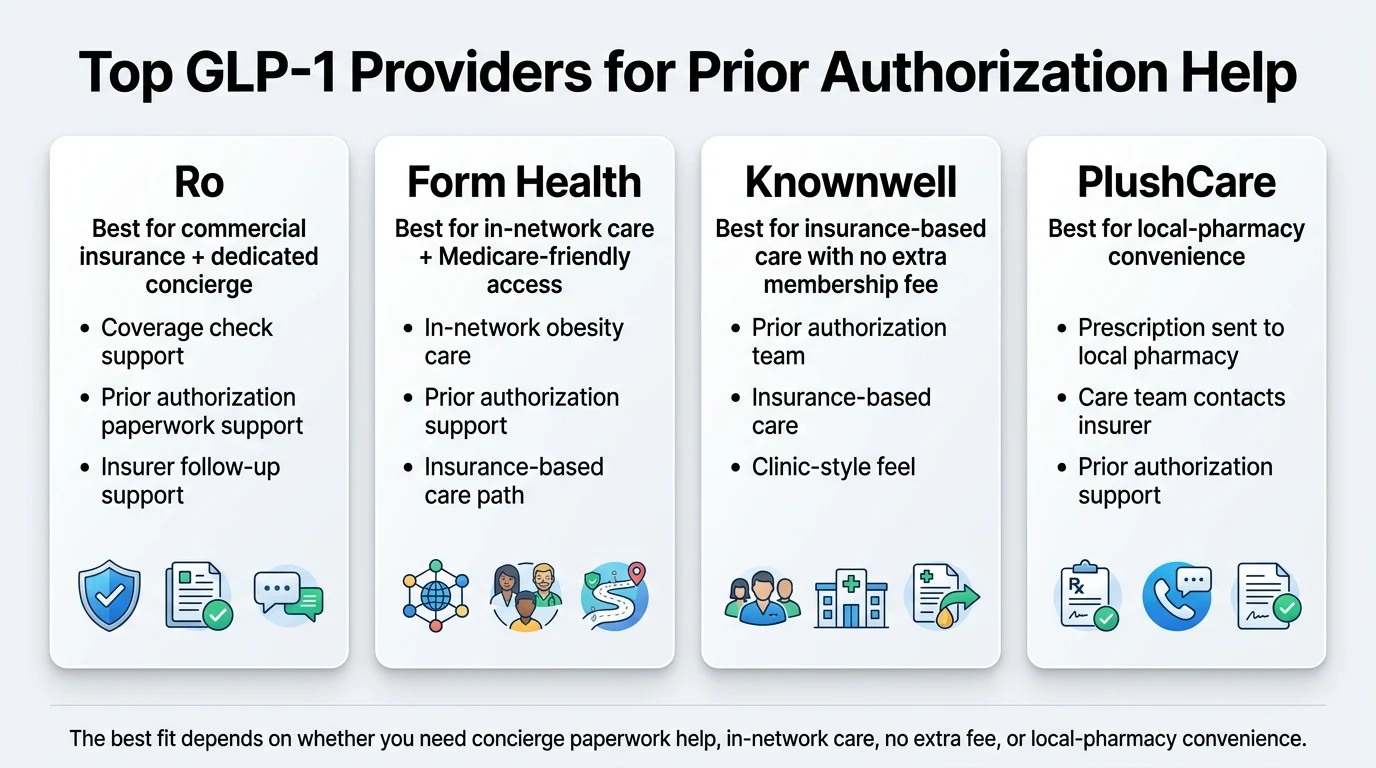
Which GLP-1 Providers Actually Help With Prior Authorization?
Most telehealth platforms blur “accepts insurance,” “checks coverage,” and “handles prior authorization” into one marketing claim. Those are three different things. A coverage check tells you whether your plan lists a GLP-1 on its formulary. PA submission means the provider’s team actually files paperwork with your insurer to get the prescription approved. Appeals handling means they fight back when the insurer says no.
We reviewed the official FAQ, terms, insurance workflow pages, and pricing of nine GLP-1 telehealth providers to determine exactly what level of PA support each one offers.
The RX Index Prior Authorization Support Matrix
Last verified: · Sources: each provider’s official website, FAQ, terms, and insurance pages · Full methodology →
| Provider | PA Score | Submits PA? | Appeals? | Visits Billed to Insurance? | Medicare? | Starting Cost | Best For | Evidence |
|---|---|---|---|---|---|---|---|---|
| Ro | 8.5/10 | ✅ Dedicated concierge | ✅ Yes | ❌ Membership cash-pay | FEHB only | $45 first mo, $149/mo + meds | Commercial PA concierge | Explicit |
| Form Health | 8.5/10 | ✅ Care team submits | ✅ Advocacy stated | ✅ In-network | ✅ Yes | $299/mo self-pay | In-network, Medicare | Explicit |
| Knownwell | 7/10 | ✅ PA team stated | ⚠️ Partial | ✅ Insurance-based | ✅ Yes | No membership fee | Clinic-style, no extra fee | Explicit (PA), partial (appeals) |
| PlushCare | 6.5/10 | ✅ Auto PA workflow | ⚠️ Varies | ✅ In-network | Some plans | ~$19.99/mo + copay | Local pharmacy, PCP-style | Explicit |
| Sesame | 6/10 | ✅ Weight-loss program only | ⚠️ Partial | ❌ Subscription cash-pay | ❌ | $59/mo + meds | Same-day visits, PA help | Explicit (weight-loss only) |
| Noom Med | 6/10 | ✅ Care coordinators | ⚠️ Partial | Limited | Not confirmed | Varies by program | Coaching + PA support | Explicit (PA), partial (ins.) |
| WeightWatchers | 5.5/10 | ⚠️ Care team assists | Limited | Partial | ❌ | $25 first mo, $74/mo | Coaching-heavy users | Partial-plus |
| Found | 5.5/10 | ✅ Supports documentation | Limited | ✅ Partial (branded meds) | ❌ | $49/mo + med cost | Broad med menu, coverage check | Partial / workflow split |
| Walgreens Wt Mgmt | 0/10 | ❌ Explicitly no | ❌ | ❌ | ❌ | $49/visit + meds | NOT for PA help | Explicit negative |
Scoring weights: coverage verification (0–2 pts), explicit PA submission (0–3 pts), appeals/advocacy (0–2 pts), refill/reauthorization support (0–1 pt), in-network/insurer-billed care (0–1 pt), public transparency (0–1 pt). Full methodology →

Two things jumped out during verification. First, the gap between the top tier (Ro and Form Health) and everyone else is significant — both explicitly document the full PA lifecycle from coverage check through appeals. Second, Sesame presented a contradiction: its general FAQ says providers can’t complete insurance paperwork, but its weight-loss program pages explicitly state providers handle PA paperwork for weight-loss medications.
Start a free coverage check on Ro — if you qualify for treatment, their concierge handles the PA process from submission to appeals.
Check your GLP-1 coverage on Ro ↗Which GLP-1 Provider Is Best for Your Exact Insurance Situation?
The comparison table tells you what each provider does. This section tells you which one to choose based on where you’re starting from.
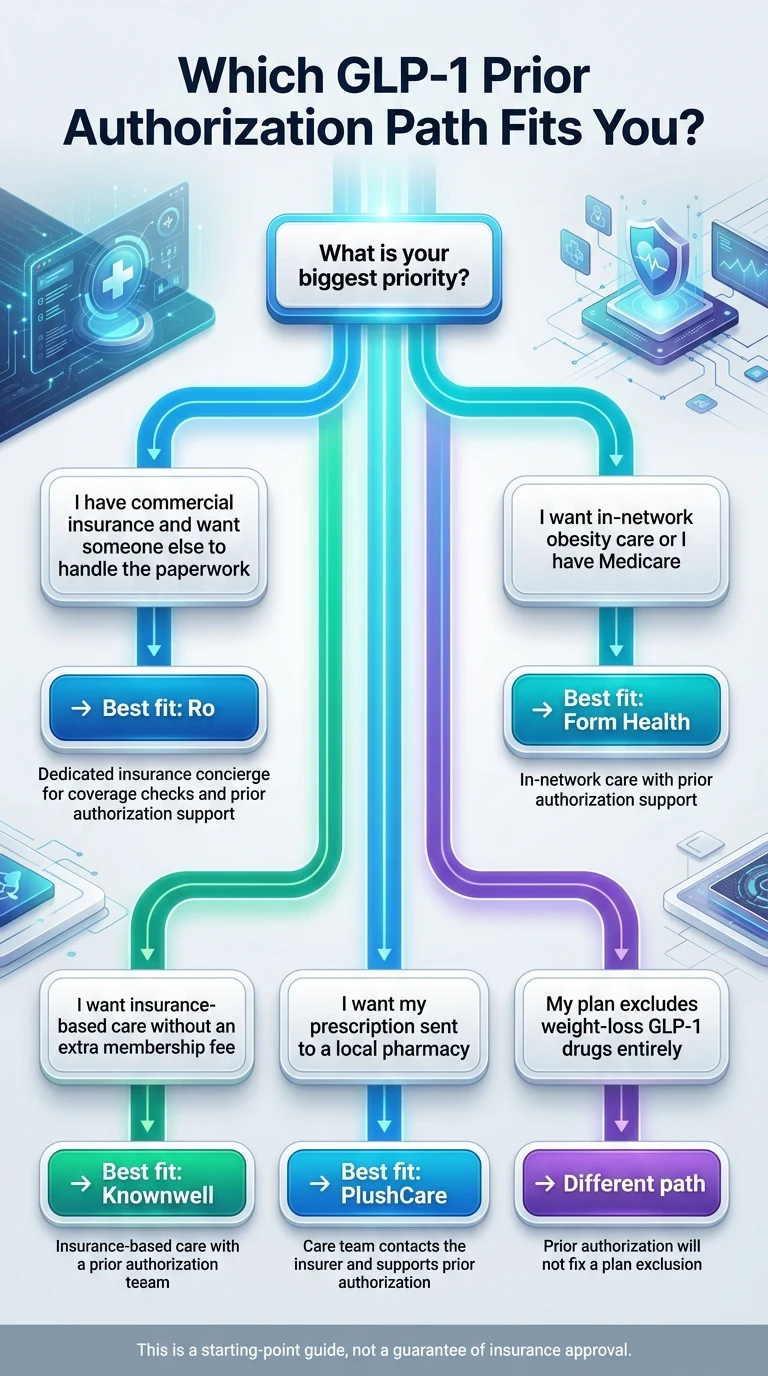
You have commercial insurance and want someone else to handle the PA → Ro
This is the most common scenario. Your employer plan covers GLP-1s (or you think it might), and you want a team that will check your coverage, submit the PA, deal with the insurer, and tell you what’s next. That’s exactly what Ro’s insurance concierge does. Your visits are paid through your membership ($45 first month, $149/month ongoing, or as low as $74/month with annual prepay), but the medication itself can be billed through your insurance — and that’s where the real savings are.
Check your GLP-1 coverage on Ro ↗You want visits billed in-network or you have Medicare → Form Health
If keeping everything inside your insurance network matters — especially if you’re on Medicare — Form Health is the better fit. Its care team is in-network with major national insurance plans including Medicare, and both your visits and your medication can be billed through insurance. Form Health explicitly states its team submits prior authorizations and advocates on your behalf. For Medicare patients, the Medicare GLP-1 Bridge program beginning July 2026 creates a new pathway for eligible beneficiaries at $50/month.
See if Form Health is in-network with your plan ↗You want clinic-style care with no membership fee → Knownwell
Knownwell’s public pages describe a prior-authorization team that works to get GLP-1 medication covered, with no membership fee on top. Insurance — including Medicare and most major commercial plans — is billed directly. If you want something that feels more like a traditional doctor’s office than a telehealth subscription, Knownwell is worth checking.
Check whether Knownwell accepts your insurance plan ↗You want a local-pharmacy, PCP-style experience → PlushCare
PlushCare is in-network with most major insurers and documents an automatic PA process where the care team reaches out to your insurer. Average insurer decisions take 7–14 business days through their workflow. If you want your GLP-1 prescription sent to your local pharmacy, PlushCare is the natural choice. If dedicated PA concierge service is your top priority, Ro’s model is more focused on the insurance navigation problem.
See if PlushCare is in-network for your plan ↗Your plan excludes weight-loss GLP-1s entirely → different path
If your plan categorically excludes obesity medications — not just requires PA, but doesn’t cover the drug class at all — prior authorization won’t help. No appeal will overturn a categorical exclusion. Your options: wait for open enrollment to switch plans, check whether a secondary indication (cardiovascular risk for Wegovy, sleep apnea for Zepbound) provides a coverage pathway, or go cash-pay.
Cash-pay options:
Compounded medications are not FDA-approved as finished products.
Ro — Best Overall for Prior Authorization Help
Ro is the clearest winner for prior authorization support for most commercially insured adults. Here’s what we verified from Ro’s official pages.
What Ro’s Insurance Concierge Actually Does
Ro’s PA workflow follows a specific sequence. First, you complete an online health assessment. If a Ro-affiliated provider determines treatment is appropriate and writes a prescription, the insurance concierge takes over. They review your insurance benefits to determine whether your GLP-1 medication can be covered without PA. If automatic coverage isn’t available, they submit a prior authorization request to your insurer. They handle the back-and-forth — gathering additional documentation, communicating with your insurer, and following up. If denied, they help you appeal or pivot to an FDA-approved cash-pay alternative.
The entire process typically takes 2–3 weeks from signup to medication when using insurance. Cash-pay patients can receive medication in under a week.
What We Verified
Sources: ro.co/weight-loss/insurance, ro.co/weight-loss/pricing, ro.co/weight-loss/coverage-checker-report
- Dedicated insurance concierge that submits all PA paperwork and communicates with your insurer
- Free GLP-1 Insurance Coverage Checker — shows your plan’s GLP-1 coverage before you pay for treatment
- 43% of Coverage Checker users had some form of GLP-1 coverage (Ro’s 2025 Coverage Checker Report)
- Half of covered patients paid $50/month or less in copays (same report)
- Membership pricing: $45 first month, $149/month ongoing; as low as $74/month with annual prepay
- Cash-pay backup: FDA-approved Wegovy pill from $149/month for new patients; Zepbound KwikPen from $299/month first month
- Labs included at Quest Diagnostics locations
- Does NOT support Medicare or Medicaid PA coordination — FEHB is the exception
- Insured brand-name GLP-1s can be picked up at your pharmacy; cash-pay products ship to your door
The Honest Tradeoff
Ro does NOT bill your visits to insurance. The membership is cash-pay only. If your priority is having everything — visits, labs, medication — billed through your insurance network, Form Health is the better fit. But because Ro’s entire model is built around solving the medication-coverage problem, its concierge is the most dedicated PA support system we found. For most commercially insured adults, the medication is where the real money is.
What Real Patients Say About Ro’s PA Support
“From the team at Ro literally handling all the insurance — I’d never heard of a prior authorization much less knew how to get one! — to tracking down medication so I never had to miss a dose... makes my membership a huge value.”
“Ro’s team switched my prescription from Wegovy to Zepbound and completed the new prior authorization through my insurance within about a week when shortages affected my original medication.”
“I went from assuming I’d need to pay $1,000/month to picking up my prescription at CVS for $25 after Ro ran the PA and connected me with a manufacturer savings card.”
Testimonials from Ro’s official site. Members were compensated for sharing their stories.
Who Should Skip Ro
- Medicare or Medicaid patients — try Form Health or Knownwell instead
- People who want visits billed to insurance, not just medication
- People who need medication this week — for immediate cash-pay access, see MEDVi
Form Health — Best for In-Network Care and Medicare
Form Health earns the same 8.5/10 PA Support Score as Ro, but through a fundamentally different model. Where Ro is a cash-pay membership with an insurance concierge for medications, Form Health is an in-network obesity medicine practice where your visits, labs, and medication all flow through insurance.
What We Verified
Source: formhealth.co/faqs, formhealth.co/how-it-works
Form Health’s FAQ and workflow pages explicitly state that the care team reviews insurance coverage, submits prior authorizations, and advocates on the patient’s behalf. It is in-network with major national insurance plans, including Medicare. Self-pay pricing is $299/month for patients without coverage.
Why Form Health Wins for Medicare Patients
Medicare patients searching for PA help have limited options. Ro explicitly states it cannot coordinate PA for government insurance plans. Form Health accepts Medicare, making it the strongest fit for Medicare beneficiaries — particularly as the Medicare GLP-1 Bridge program begins in July 2026.
Medicare GLP-1 Bridge — July 2026
CMS is launching a temporary nationwide demonstration giving eligible Part D beneficiaries access to weight-loss GLP-1s at a $50/month copay. Covered medications: Foundayo (all formulations), Wegovy (injection and tablets), and Zepbound (KwikPen only). PA goes through a CMS central processor — not your Part D plan. Source: CMS.gov
Eligibility tiers:
- BMI ≥35 (alone)
- BMI ≥30 plus HFpEF, uncontrolled hypertension on two antihypertensive meds, or CKD stage 3a+
- BMI ≥27 plus pre-diabetes (ADA-defined), prior MI, prior stroke, or symptomatic PAD
The Honest Tradeoff
Form Health is NOT the fastest answer if all you want today is a free coverage check. Ro’s Insurance Coverage Checker gives you a coverage snapshot before you commit. But if you want long-term obesity care that lives inside the insurance system — specialists, labs, medication, visits, all billed through your plan — Form Health is the more complete solution.
“I lost 45 pounds in six months.” — Form Health patientSee if Form Health is in-network for your plan ↗
Knownwell — Best Clinic-Style Option With No Membership Fee
Knownwell’s public pages describe a prior-authorization team that works to get GLP-1 medication covered through insurance, with no membership fee on top. Insurance — including Medicare and most major commercial plans nationwide — is billed directly.
Knownwell explicitly states it accepts Medicare and most major commercial insurance plans. The PA team is explicitly mentioned. Appeals and denial support are partially documented but not as prominently featured as Ro’s or Form Health’s concierge language.
Patients who want insurance-based care — including Medicare — without a monthly telehealth subscription fee will find Knownwell the natural fit. If the $149/month Ro membership feels like unnecessary overhead when your insurance should be covering things, Knownwell is the natural alternative.
Check whether Knownwell accepts your insurance plan ↗PlushCare — Best for Local-Pharmacy Prescriptions
PlushCare documents an automatic PA workflow and states that its doctor and care team can reach out to the insurer on the patient’s behalf. It’s in-network with most major insurers, and average insurer decisions take 7–14 business days through their system.
PlushCare works more like a traditional doctor visit — your prescription can be sent to your local pharmacy. Public pricing signals show approximately $19.99/month for the membership plus standard copays when in-network, or about $129 per visit without insurance.
If dedicated PA concierge service is your top priority, Ro’s model is more focused on the insurance navigation problem. PlushCare is a general telehealth platform that also handles GLP-1 PA — Ro is specifically built around solving GLP-1 access and cost.
See if PlushCare is in-network for your plan ↗Sesame, WeightWatchers, Noom, and Found — Situational Options
These providers offer varying degrees of PA support, but none match the dedicated concierge infrastructure of Ro or the in-network depth of Form Health. They’re worth considering if coaching, affordability, or a broader wellness platform matters to you.
Sesame (Success by Sesame)
Sesame presented an interesting contradiction during our review. Its general FAQ says providers can’t complete insurance paperwork. But its weight-loss program pages tell a different story — they explicitly state: “Your Sesame provider will work directly with your insurance to handle any prior authorization paperwork.” The Success by Sesame subscription starts at $59/month, medication not included. Same-day video visits with a provider of your choice are a genuine differentiator.
Source: sesamecare.com/service/online-weight-loss-program, sesamecare.com/blog/sesame-vs-ro-weight-loss
WeightWatchers Clinic (Med+)
WeightWatchers’ public pages state the care team works to get GLP-1 medication covered by insurance, and WW’s terms indicate that if a member provides insurance information, the provider can submit claims for covered services. Pricing starts at $25 for month one and $74/month after that on a 12-month commitment, medication not included.
Noom Med
Noom’s branded-meds support page says care coordinators manage insurance steps including PA and refill support. The behavior-change coaching is Noom’s real differentiator. Insurance model and pricing are less transparent in the public sources we reviewed compared to Ro or Form Health.
Found
Found starts at $49/month, checks insurance coverage, and supports prior authorization and documentation for branded medications. Found’s pages state it works with your insurance for telehealth visits. However, Found’s free checker FAQ clarifies that the checker report itself doesn’t submit treatment requests or write prescriptions — there’s a workflow split between the coverage check and the treatment path.
The Provider to Avoid If PA Help Is Your Priority
Walgreens Weight Management — 0/10
Walgreens explicitly states its current weight-management service is for self-pay patients at $49/visit (medication separate) and does not handle insurance or prior authorizations for GLP-1s. Potentially useful for a one-off cash-pay consultation, but not for this search.
If you need someone to handle the PA process, stick with providers that publicly document they submit and manage it. Your time matters too much to sign up somewhere, pay the first month, and discover they expect you to handle the insurer yourself.
What if Your Doctor Won’t Do the Prior Authorization?
This might be the single most frustrating scenario in the GLP-1 access landscape. People in patient communities describe calling their doctor’s office repeatedly, waiting weeks, hearing “we don’t really do that here,” or being told the PA “didn’t go through” with no follow-up.
Here’s why it happens: GLP-1 prior authorizations are genuinely complex. Insurance policies vary by plan, documentation requirements are specific and insurer-dependent, and many primary care offices don’t have dedicated PA staff. You have three paths forward.
Path 1: Ask Your Insurer for the Exact Criteria
Call the number on the back of your insurance card and ask: “What specific documentation do you need for prior authorization of [Wegovy/Zepbound]?” Get the criteria in writing. Then bring that list back to your doctor. Sometimes the issue is that the office submitted incomplete paperwork — once they know exactly what the insurer wants, they can resubmit successfully.
Path 2: Move to a Provider With a Dedicated PA Team
This is the fastest path for most people. Telehealth providers like Ro have teams that specialize in GLP-1 insurance navigation. They know what each major insurer requires, they submit PAs consistently, and they follow up because their business model depends on getting patients treated.
Need a provider who will submit the PA for you? Start with Ro ↗Path 3: If Already Denied, Resubmit or Appeal
If a PA was already submitted and denied, the denial letter tells you why. Fix the specific gap and resubmit — or ask for a peer-to-peer review, which is a phone call between your prescribing provider and the insurer’s medical reviewer. Many denials are overturned through this process when the right documentation is provided.
What Documents Make GLP-1 Approval More Likely?
Walking into your first telehealth visit with the right documentation already assembled can shave weeks off the PA timeline. Most denials happen because the submission didn’t match the insurer’s specific criteria — not because the patient didn’t qualify. That’s a paperwork problem, not a medical one.

| Document | Why Insurers Require It | Where to Find It |
|---|---|---|
| Insurance card (front and back) | Identifies plan, PBM, and group number | Your wallet or insurer’s app |
| Two documented BMI measurements | Most plans require BMI ≥30, or ≥27 with comorbidity | Recent doctor visits — request records if needed |
| Lab results (A1C, lipid panel, metabolic panel) | Proves comorbidities and establishes baseline | Your PCP or lab portal (Quest, Labcorp) |
| Comorbidity documentation | Type 2 diabetes, hypertension, sleep apnea, CVD | Diagnosis notes, medication lists, treatment records |
| Record of prior weight-loss attempts | Many insurers require documented diet/exercise/counseling | Provider notes, program receipts, personal logs |
| Current medication list | Rules out contraindications, shows treatment history | Your pharmacy or provider portal |
| Plan formulary | Confirms whether your specific GLP-1 is listed | Insurer website or member portal |
| Benefits summary | Shows whether weight-loss drugs are a covered category | HR department or insurer member services |
Pro tip that prevents a common denial trap
Document your baseline weight the day you start treatment. Most plans require renewal every 6–12 months with evidence of at least 5% weight loss from baseline. If you don’t have a documented starting weight, the renewal can be denied even if you’ve lost significant weight — because the insurer has nothing to compare against.
What Happens If Your Prior Authorization Is Denied?
Do not give up. Denial is not the end — it’s often the beginning of a process that works better than the initial submission. Studies on insurance appeal outcomes consistently show that a significant portion of initial PA denials are overturned when the specific denial reason is addressed with additional documentation.
Step 1: Read the Denial Letter
Common reasons for GLP-1 PA denials:
- Incomplete documentation — BMI not recent enough, missing comorbidity codes, no evidence of prior weight-loss attempts
- Step therapy not met — the insurer requires you to try a cheaper medication first (like Saxenda before Wegovy)
- Plan exclusion — the drug category itself isn’t covered (this can’t be overturned through appeal)
- Wrong diagnosis codes — obesity codes vs. diabetes codes matter enormously
Step 2: Request a Peer-to-Peer Review
Ask your provider to request a peer-to-peer review — a phone call between your prescribing doctor and the insurer’s medical reviewer. It’s often faster than a written appeal and gives your doctor a chance to advocate directly. Providers like Ro handle this as part of their concierge service.
Step 3: File a Formal Appeal
Don’t just resubmit the same paperwork. Add the specific documentation that addresses the denial reason.
Step 4: Escalate to External Review If Needed
Under the Affordable Care Act, if your internal appeal is denied, you can request an external review by an independent third party. Insurers are required to honor the external reviewer’s decision if it rules in your favor.
When to Change Strategy
If your plan categorically excludes weight-loss medications — not just denied your PA, but doesn’t cover the drug class at all — stop fighting and change paths.
Compounded medications are not FDA-approved as finished products.
When Should You Skip Prior Authorization and Pay Cash Instead?
Prior authorization exists because insurance could save you hundreds of dollars per month. But sometimes the math doesn’t work — and the time cost of fighting the PA battle exceeds what you’d save.
High-deductible plan
If your deductible is $3,000+ and you haven’t met it, you’re paying full price anyway until you do.
Tier 4 or 5 copay
Some plans place GLP-1s on the highest cost-sharing tier, meaning copays of $200–$500/month even after PA approval. At that point, compounded GLP-1s at $179/month through MEDVi may cost less than your “covered” copay.
Repeated denials
If you’ve been denied twice and the appeal process will take months, you’re losing time you could spend on treatment your provider actually recommends.
Step therapy delays
If your plan requires 3–6 months on a different medication first, that’s time spent on a treatment your doctor didn’t choose for you.
A Practical Approach
Consider starting the PA process with a provider like Ro (whose concierge handles the paperwork) while also exploring cash-pay options so you’re not waiting without medication. If the PA comes through and your copay is lower, switch to the insured brand-name medication.
Compounded medications are not FDA-approved as finished products.
Will Insurance Even Cover Wegovy or Zepbound for Weight Loss?
Before investing weeks in the PA process, it’s worth understanding the current landscape so your expectations are calibrated.
Commercial Employer Plans
Coverage is growing but far from universal. According to KFF’s employer health benefits research, only about 19% of large employers cover GLP-1s for weight loss. Even when coverage exists, over 88% of patients still face additional requirements — prior authorization, step therapy, enrollment in a coaching program, or documentation of prior weight-loss attempts.
Plans That Cover Diabetes GLP-1s But Exclude Obesity Medications
Your plan may cover Ozempic (semaglutide) for type 2 diabetes but deny Wegovy (also semaglutide) for weight loss. Insurers treat them as categorically different because the FDA approvals are for different indications. If you have both obesity and type 2 diabetes, your doctor can sometimes pursue coverage through the diabetes diagnosis. The ICD-10 code on the PA submission — E11.x for diabetes vs. E66.x for obesity — can determine whether the same drug gets approved or denied.
What “Step Therapy” Means in Practice
Step therapy requires you to try a cheaper treatment before the insurer will approve the GLP-1. Some plans require a trial of Saxenda before Wegovy, or 3–6 months of documented diet and exercise counseling. Your provider may be able to request a step therapy exception if there’s a clinical reason the cheaper medication isn’t appropriate.
Medicare and the GLP-1 Bridge Program — What Changes in July 2026
Medicare’s relationship with GLP-1s is changing faster than any other insurance category this year.
Medicare Today
Medicare Part D does not cover GLP-1 medications prescribed solely for weight loss. It does cover Wegovy specifically for cardiovascular risk reduction in patients with established heart disease and BMI ≥27, and Ozempic/Mounjaro for type 2 diabetes.
Medicare GLP-1 Bridge (July 1 – December 31, 2026)
CMS launched the Medicare GLP-1 Bridge — a temporary nationwide demonstration giving eligible Part D beneficiaries access to weight-loss GLP-1s at a $50/month copay. PA goes through a CMS central processor — not the beneficiary’s Part D plan. Source: CMS.gov, updated April 6, 2026
| Covered Medications | Formulations |
|---|---|
| Foundayo | All formulations |
| Wegovy | Injection and tablets |
| Zepbound | KwikPen only (single-dose vial not included) |
Eligibility tiers:
- BMI ≥35 (alone)
- BMI ≥30 plus HFpEF, uncontrolled hypertension on two antihypertensive meds, or CKD stage 3a+
- BMI ≥27 plus pre-diabetes (ADA-defined), prior MI, prior stroke, or symptomatic PAD
What Comes Next: BALANCE Model (January 2027)
The BALANCE Model extends GLP-1 coverage into Medicare Part D plans and Medicaid on a voluntary, state-by-state basis. To maintain coverage after the Bridge ends, beneficiaries will need to be enrolled in a Part D plan that participates in BALANCE — which may require switching plans during the October–December 2026 open enrollment.
How Long Does GLP-1 Prior Authorization Actually Take?
The timeline depends on your provider’s PA infrastructure, your insurer’s processing speed, and whether the initial submission is complete.
| Phase | Best Case | Typical | Common Delay |
|---|---|---|---|
| Coverage verification | Same day | 1–3 days | Insurer slow to respond |
| PA submission | Day 1 after verification | Day 3–5 | Documentation gaps |
| Insurer review (standard) | 5 business days | 7–15 business days | Missing criteria, internal queues |
| Insurer review (expedited) | 24–72 hours | 72 hours | Must demonstrate medical urgency |
| Appeal (if denied) | 5 business days | Up to 30 days | Peer-to-peer scheduling delays |
| Total: signup to medication | ~10 days | 2–3 weeks | Can stretch to 6+ weeks with denials |
Sources: Ro states 2–3 weeks typical. PlushCare states 7–14 business days for insurer review. CMS requires Medicare/Medicaid plans to decide expedited requests within 72 hours and standard requests within 7 days under CMS-0057-F provisions effective January 2026.
What you can do to speed things up: Have your documentation ready before your first appointment (use the checklist above), choose a provider with a dedicated PA team, and respond immediately to any requests for additional information.
What “Prior Authorization Help” Actually Means — Four Levels
Not all PA support is created equal. When providers say they “help with insurance,” they could mean any of four very different things.
Level 1: Coverage Check Only
The provider checks whether your plan lists GLP-1s on its formulary. They do NOT submit any paperwork to your insurer. This is a starting point, not a solution.
Level 2: Coverage Check + PA Submission
The provider checks coverage AND submits the prior authorization paperwork. This is the minimum threshold for genuine PA help. PlushCare, Sesame (weight-loss program), Noom, and WeightWatchers operate at approximately this level.
Level 3: Coverage Check + PA + Appeals / Advocacy
The provider checks coverage, submits PA, AND actively advocates when the insurer pushes back — resubmitting with additional documentation, requesting peer-to-peer reviews, helping with formal appeals. Ro and Form Health operate at this level, which is why they score highest.
Level 4: Full In-Network PA Management
Everything in Level 3, plus visits and labs are also billed through insurance. Form Health and Knownwell are the closest to this model.
How We Verified These Providers
Every row in the PA Support Matrix was checked against the provider’s official website — specifically their pricing pages, FAQ pages, insurance/workflow pages, and terms of service — as of April 9, 2026. We did not rely on third-party reviews, press releases, or marketing materials for the core PA-support claims.
Scoring methodology
- Coverage verification (0–2 pts): Whether the provider runs an explicit coverage check before PA submission.
- Explicit PA submission (0–3 pts): Whether official pages clearly state the team submits PA paperwork to insurers.
- Appeals/advocacy (0–2 pts): Whether the provider explicitly documents fighting denials, resubmitting, or peer-to-peer reviews.
- Refill/reauthorization support (0–1 pt): Whether annual renewal PAs are handled by the provider.
- In-network or insurer-billed care (0–1 pt): Whether visits and labs can also be billed through insurance.
- Public transparency of workflow (0–1 pt): Clarity of the published PA workflow on the provider’s site.
Evidence confidence labels
- Explicit — Official pages use clear, specific language about PA submission
- Partial — Some PA support stated, but full workflow less transparent
- Explicit negative — Official pages explicitly state they do NOT do PA
What we could not verify: Actual PA approval rates (no platform publishes this), internal appeal success rates, exact turnaround times beyond provider-stated estimates, and Noom’s Medicare acceptance status.
This page is verified monthly. Provider pricing and PA workflows are rechecked against official pages. The “Last verified” date reflects our most recent full review.
Frequently Asked Questions
Which online GLP-1 provider is best for prior authorization help?+
Do all GLP-1 telehealth companies submit prior authorization paperwork?+
What if my doctor won't fill out my Wegovy or Zepbound prior authorization?+
How long does prior authorization take for Wegovy or Zepbound?+
Which provider is best if I want insurance to cover the medication but not my visits?+
Which provider is best if I want visits billed in-network?+
Does Medicare cover Wegovy for weight loss?+
What if my insurance denies my GLP-1 request?+
What documents should I gather before starting a GLP-1 prior authorization?+
Which GLP-1 providers should I avoid if prior authorization help is my main priority?+
Still not sure which GLP-1 program is right for you?
Answer a few questions about your insurance, budget, and preferred care style, and we’ll match you with the best next step — whether that’s a PA-focused provider like Ro, an in-network option like Form Health, or a cash-pay path that skips insurance entirely.
Take the free 60-second GLP-1 matching quiz →Related GLP-1 Guides
Affiliate & Editorial Disclosure
The RX Index is an independent comparison resource for GLP-1 telehealth providers. We may earn a commission if you purchase through our links, at no extra cost to you. Rankings are based on verified prior-authorization support depth scored against public documentation — not commission rates. Every factual claim on this page links to its source — provider websites, CMS communications, and KFF research verified as of April 9, 2026. We did not rely on third-party reviews, press releases, or marketing materials for the core PA-support claims. If we could not verify a claim publicly, we marked it rather than filling in the blank.