Pricing Guide · Verified April 2026
Cheapest Tirzepatide Online With Insurance
By The Rx Index Editorial Team · Last verified: April 2026 · All hidden fees shown · Affiliate disclosure
Bottom line
The cheapest legitimate way to get tirzepatide online with insurance is brand-name Zepbound or Mounjaro through a commercial plan that covers it, combined with Eli Lilly’s savings program — which can bring eligible fills to as low as $25/month. Your cheapest online provider depends on whether your visits are in-network: PlushCare often totals the least ($19.99/mo + copay). If you need to check coverage before paying, Ro offers a free coverage report — no commitment.
The $25/month claim is real, but it’s only the medication copay. Your total is that drug copay plus whatever the online provider charges for their platform, visits, and support. Those two numbers live in completely different buckets.
Don’t know if you’re covered?
Ro’s free GLP-1 Insurance Coverage Checker contacts your insurer and sends you a personalized report. No payment, no commitment.
Check your coverage free with Ro →Already know you’re covered?
PlushCare charges $19.99/month + your visit copay. Estimated best-case total with Lilly savings: ~$50–$75/month all-in.
Check PlushCare pricing →We may earn a commission when you visit a provider through our links. This does not affect our rankings or the price you pay. Full disclosure. Not medical advice.
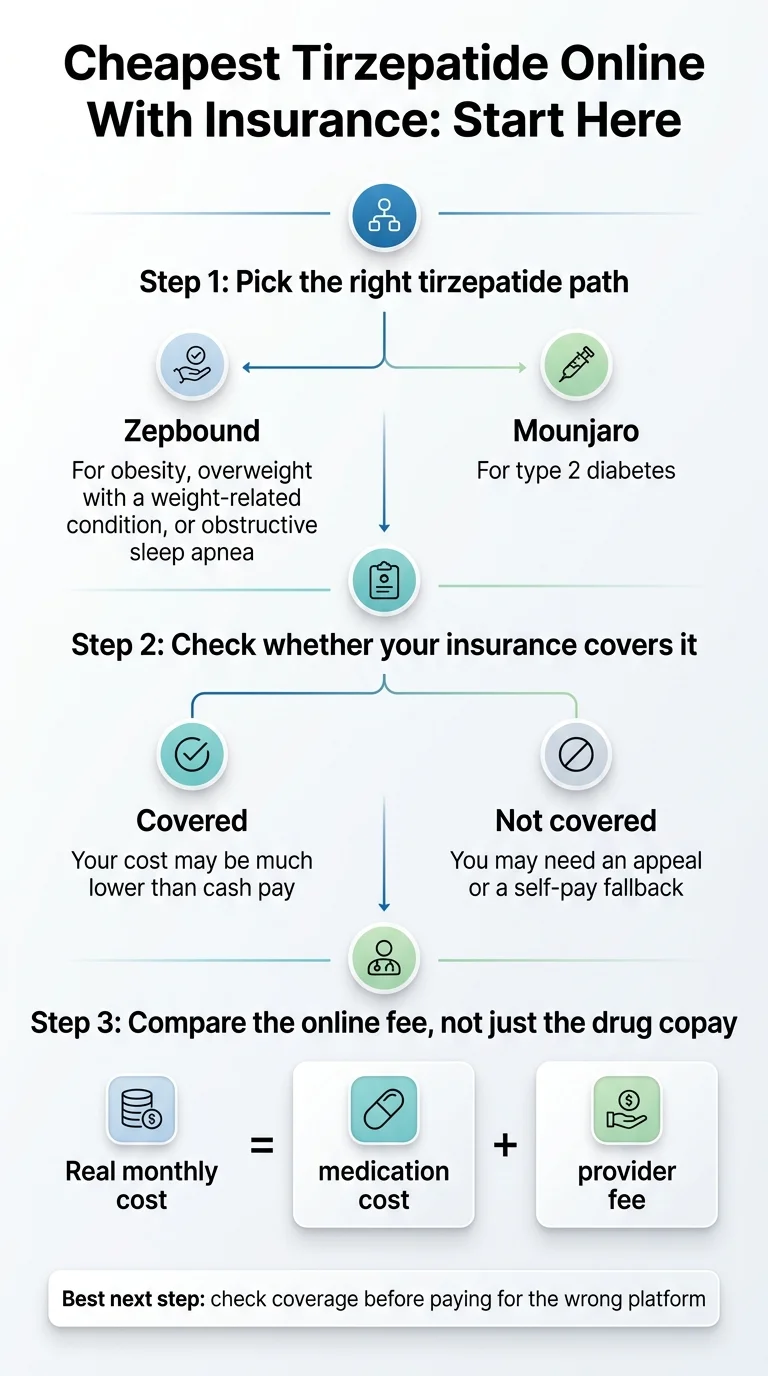
Your Cheapest Path at a Glance
Find your situation. All estimates combine drug copay after savings plus provider fee. Pricing verified April 2026 from official manufacturer and provider pages.
| Your Situation | Cheapest Path | Drug Cost | Provider Fee | Best-Case Monthly | PA Help? |
|---|---|---|---|---|---|
| Commercial plan covers Zepbound + in-network telehealth | PlushCare + Lilly savings | As low as $25 | ~$20 + visit copay | ~$50–$75 | Yes |
| Commercial plan covers Zepbound + want concierge help | Ro + Lilly savings | As low as $25 | $145 ($45 first mo) | ~$170 | Yes — full concierge |
| Commercial plan covers Zepbound + want coaching | WW Clinic + Lilly savings | As low as $25 | $74 ($25 first mo) | ~$99 | Yes |
| Don't know if you're covered | Ro free checker first | Unknown | $0 to check | Free to find out | Free check; PA help if enrolled |
| Commercial plan denied / excludes weight-loss drugs | Appeal → then LillyDirect | $299–$449+ | Varies | $299–$594+ | Depends on provider |
| Have type 2 diabetes | Mounjaro + savings (easier coverage) | As low as $25 | Varies | $25–$170+ | Yes, via most providers |
| Medicare | GLP-1 Bridge (Jul–Dec 2026) or LillyDirect | $50 Bridge / $299+ self-pay | Varies | $50+ Bridge / $299+ self-pay | Limited |
| Medicaid | State-dependent | Varies by state | Varies | Varies | Varies |
Estimates assume eligible savings programs, met deductibles, and one monthly visit where applicable. Actual costs vary by plan, deductible status, and visit cadence.
What Does Tirzepatide Actually Cost With Insurance in 2026?
The real cost ranges from $25 to over $1,086 per month. Most commercially insured patients who get coverage approved land between $25 and $350, depending on their plan’s formulary tier, deductible status, and whether they activate the manufacturer’s savings program.
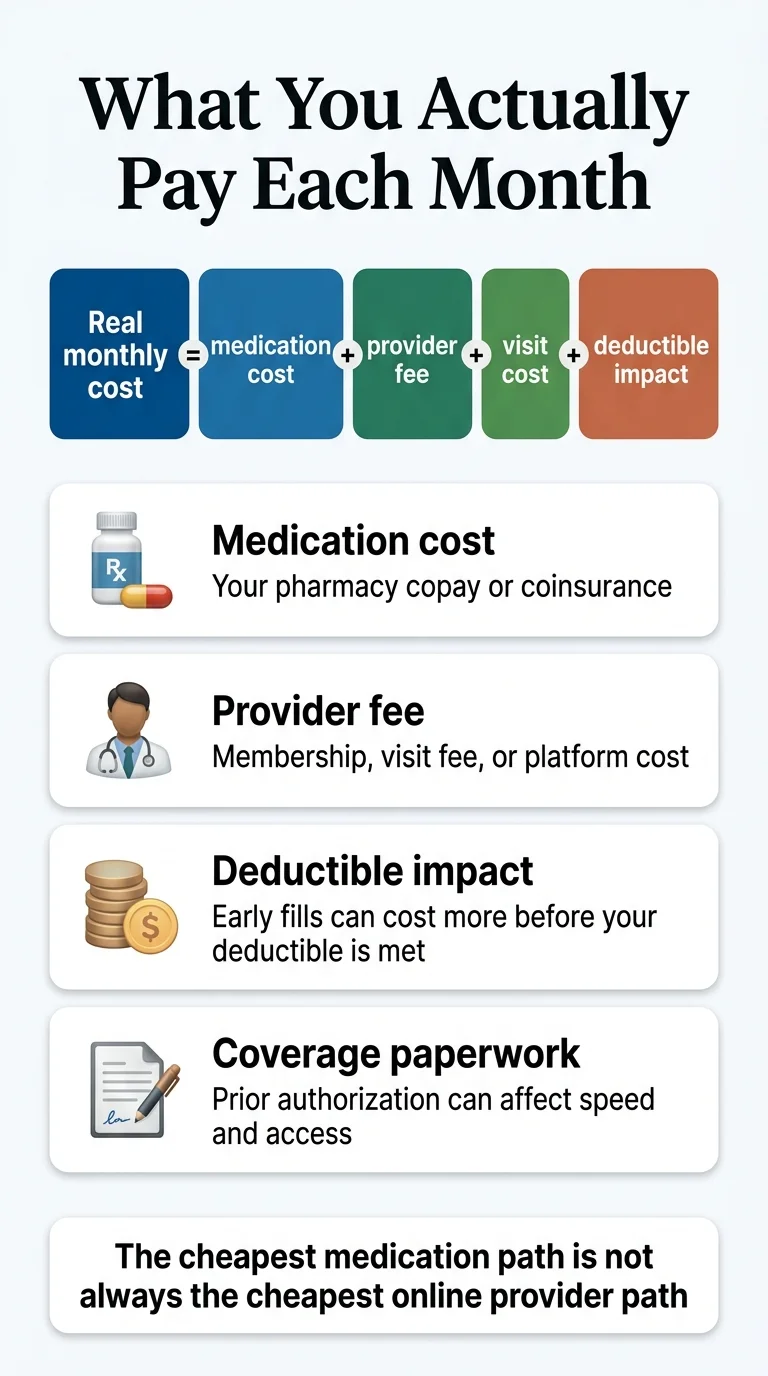
The list price (what almost nobody pays)
$1,086 for Zepbound, $1,080 for Mounjaro — both for a 28-day supply (pricinginfo.lilly.com). This is the number Eli Lilly charges wholesalers. It's the same regardless of dose.
Your copay or coinsurance (what your plan sets)
What mattersIf your commercial plan covers tirzepatide, your share is typically $100–$350/month depending on formulary tier. With Lilly's savings program stacked on top, eligible patients can bring that down to as low as $25.
The online provider fee (the number most pages leave out)
Most missedThis is the membership, visit fee, or subscription you pay the telehealth platform. It ranges from $0 (your own doctor) to $145/month (Ro). Most pricing pages present this separately from the medication cost. We add them together — because your wallet doesn't care which bucket the money comes from.
| Cost Component | What It Covers | Typical Range |
|---|---|---|
| Drug copay/coinsurance | The medication at your pharmacy | $25–$350 with coverage |
| Manufacturer savings program | Reduces copay (Zepbound: up to $100/fill) | Can bring copay to ~$25 if eligible |
| Telehealth membership/visit | Clinician access, prescriptions, support | $0–$145/month |
| Deductible (if not yet met) | Your plan's annual threshold | $500–$3,000+ before coverage kicks in |
| Prior authorization | Required by most plans with GLP-1 coverage | Free, but costs time |
| Labs (if required) | Some providers require bloodwork | $0–$100+ |
Find Your Cheapest Path by Insurance Type
Most people don’t need a universal recommendation. They need the cheapest path for their exact situation. Find yours below.
I have commercial insurance and think it covers Zepbound
Your path: lowest-fee clinician + Lilly savings. If your plan covers Zepbound, the medication can cost as little as $25 per fill. Your only remaining variable is how much you’re paying to access a prescriber. If your primary care doctor prescribes it, your provider fee may be just your visit copay — potentially $0–$50. If you want online convenience, PlushCare’s membership ($19.99/month) plus your visit copay is likely the lowest online total.
Don’t overpay for concierge help you don’t need. If your insurance already covers the drug, a $145/month membership to get coverage assistance is solving a problem you don’t have.
I have commercial insurance but don’t know if tirzepatide is covered
Your path: free coverage check before you pay anything. This is where Ro’s free GLP-1 Insurance Coverage Checker earns its place. Ro’s team contacts your insurer, checks your formulary, and sends you a personalized coverage report — no payment, no commitment. That report tells you whether to pursue the $25 insured route or pivot to a self-pay strategy.
Check your tirzepatide coverage free with Ro →I have type 2 diabetes
Your path: Mounjaro, not Zepbound. Mounjaro is FDA-approved specifically for type 2 diabetes, and commercial insurance coverage for diabetes medications is substantially more common than coverage for weight-loss drugs. Most plans already include diabetes treatments on their formulary. Coverage is usually smoother, denials are less common, and prior authorization documentation is more straightforward because diabetes is an established indication. Both products have savings programs that can bring the copay to as low as $25 for eligible commercially insured patients, but the specific terms differ.
I have obesity or overweight with a health condition
Your path: Zepbound. FDA-approved for chronic weight management in adults with BMI ≥30 or overweight (BMI ≥27) with at least one weight-related comorbidity — like high blood pressure, type 2 diabetes, high cholesterol, or obstructive sleep apnea. Coverage is harder to get than Mounjaro for diabetes — only about 1 in 5 large employers cover GLP-1 for weight loss specifically — but it’s not impossible.
My plan excludes weight-loss drugs entirely
Your path: appeal first, then pivot. A denial is not the end — AMA data shows 83.2% of prior authorization appeals result in partial or full overturn. If the appeal fails, LillyDirect self-pay: $299/month for 2.5 mg, $399 for 5 mg, and $449 for 7.5–15 mg under the current self-pay journey offer (timely refills required to maintain higher-dose pricing).
See full denial playbook ↓I have Medicare
Medicare Part D does not currently cover tirzepatide for weight loss through standard benefits. However, CMS has published the Medicare GLP-1 Bridge program, running July 1 through December 31, 2026. Eligible beneficiaries in qualifying Part D plan types who meet prior-authorization criteria can access covered Bridge products for a $50 copay. For Zepbound, only the KwikPen formulation is included — the single-dose pen and vial are not. The Lilly commercial savings card cannot be used with any government insurance.
If the Bridge doesn’t apply to you, LillyDirect self-pay vials start at $299/month. If you have type 2 diabetes, Medicare may cover Mounjaro — check with your Part D plan directly.
I have Medicaid
Medicaid obesity-drug coverage remains limited and state-dependent. KFF reports that 13 state Medicaid programs covered GLP-1s for obesity as of January 2026. All states cover GLP-1s prescribed for type 2 diabetes. Under CMS’s BALANCE model, Medicaid access to obesity treatments can begin as early as May 2026 in participating states — but it is not automatic or nationwide. Medicaid beneficiaries are not eligible for Lilly’s savings programs.
Can You Really Get Tirzepatide for $25 a Month?
Yes — but only if three things are true at the same time. Most pages toss out the “$25” number without explaining the conditions.
Condition 1
You have commercial insurance
Employer-sponsored, ACA marketplace, or individual commercial plan. Medicare, Medicaid, VA, TRICARE, and all other government insurance are excluded. This is federal law, not Lilly's decision.
Condition 2
Your plan covers Zepbound (or Mounjaro)
"Having insurance" and "having coverage for tirzepatide" are not the same thing. Over 109 million Americans have commercial insurance with zero Zepbound coverage, according to GoodRx research. You must verify your specific formulary.
Condition 3
You activate Lilly's savings program
For Zepbound, the current savings card covers up to $100 off your copay per 28-day fill, with an annual cap of $1,300. If your copay is $125, you pay $25. If your copay is $175, you pay $75. Valid through December 31, 2026, covering up to 13 fills per year.
What about the $499 path?
The current Zepbound savings program also includes a non-covered commercial path: if your commercial plan does not cover Zepbound single-dose pens, eligible patients may pay as low as $499/month. That’s still less than the $1,086 list price, but it’s a very different number than $25.
The fastest way to find out which track you’re on:
Check whether your plan covers tirzepatide in the first place. If Ro’s free checker confirms you’re covered, you could be picking up your first prescription within two weeks. If it shows you’re not covered, you’ll know exactly which backup path to take.
Check your coverage free with Ro →The Formulation Detail That Most Pages Miss
| Formulation | Insurance + Savings | Self-Pay Price | Key Restriction |
|---|---|---|---|
| Single-dose pen | As low as $25/fill | ~$1,086 list | Must have commercial coverage |
| Single-dose vial (LillyDirect) | N/A — self-pay only | $299 (2.5mg), $399 (5mg), $449 (7.5–15mg) | Cannot use with insurance; timely refill required for higher-dose pricing |
| KwikPen (multi-dose) | Separate savings terms; included in Medicare Bridge | $449 (7.5–15mg under journey offer) | 45-day refill window to maintain discounted higher-dose pricing |
Zepbound vs. Mounjaro: Which Should You Try to Get Covered?
This decision matters more than which telehealth platform you pick, because pursuing the wrong one can lead to a denial that wastes weeks and costs money in unnecessary provider fees.
| Zepbound | Mounjaro | |
|---|---|---|
| FDA-approved for | Weight loss/management, OSA | Type 2 diabetes |
| Insurance coverage likelihood | Lower — many plans exclude weight-loss drugs | Higher — diabetes is standard coverage |
| Best path if you have | Obesity, overweight + comorbidity, or OSA | Type 2 diabetes |
| Savings program | As low as $25 with eligible commercial coverage | As low as $25 with eligible commercial coverage |
| List price | $1,086/month | $1,080/month |
The OSA angle worth knowing
If you have moderate-to-severe obstructive sleep apnea and obesity, Zepbound’s FDA-approved OSA indication may give your doctor stronger leverage in the prior authorization process. A sleep study documenting your condition can be powerful documentation that is harder to deny.
Best Online Providers for Tirzepatide With Insurance
Each provider has a different fee structure, a different level of insurance support, and a different all-in monthly total. Ranked by total cost to you — not just the drug price.

PlushCare — Lowest total cost for well-insured readers
$19.99/mo membership · PA support included
Best for: People whose insurance already covers tirzepatide and whose telehealth visits are in-network. PlushCare charges a $19.99/month membership. Insured visit copays are often $30 or less. Their care team handles prior authorization. Estimated best-case total: ~$50–$75/month.
Ro — Best free coverage check and insurance concierge
Free pre-check · Full concierge · $145/mo membership
Best for: People who don’t know their coverage status and want someone to handle the insurance work. Before you spend a dollar, Ro’s team contacts your insurer, checks your formulary, and delivers a personalized coverage report. No payment, no commitment. The paid membership ($45 first month, then $145/month) includes full insurance concierge, prior authorization paperwork, licensed clinician management, and ongoing support. Medication is separate.
“I had been putting this off for months because the insurance part felt overwhelming. Ro’s team checked my coverage, told me I was eligible, and walked me through the savings card. I picked up Zepbound at my pharmacy for $25.”— Ro member (disclosed paid partnership)Run your free coverage report with Ro →
WeightWatchers Clinic — Best if you want coaching bundled
$74/mo ($25 first mo) · Coaching + clinician access · Meds separate
Best for: People who want a full behavior-change program around the medication, not just a prescription. WW Clinic pairs tirzepatide prescribing with the WeightWatchers ecosystem — coaches, nutrition guidance, behavioral tools, and app-based tracking.
Note: WW’s insurance coordinators currently work only with commercial insurance plans. Government-sponsored plans are not supported.
See WW Clinic eligibility and full plan terms →Sesame — Solid lower-fee middle ground
From $59/mo · PA assistance · No free pre-check
Best for: People who want a lower recurring fee than Ro without going fully DIY. Sesame’s tirzepatide-focused programs start from $59/month — less than Ro’s $145, more than PlushCare’s $20. Sesame providers can assist with prior authorization and insurance coordination. Estimated best-case total with savings: ~$84/month ($59 + $25 copay).
“They helped me get the cheapest prescription I have ever gotten!”— Kevin, Houston, TX (Sesame member)See Sesame's current program pricing →
Walgreens Weight Management — Not a fit for insurance users
No PA supportWalgreens’ GLP-1 weight-management program is currently designed for out-of-pocket patients and does not handle insurance billing or prior authorizations for tirzepatide. If insurance support matters to you — and if you’re reading this page, it probably does — Ro, PlushCare, WW, or Sesame will serve you better.
Full Provider Comparison: All-In Estimated Cost With Insurance
| Provider | Monthly Fee | Insurance Help? | Free Pre-Check? | Best-Case Total |
|---|---|---|---|---|
| Your own doctor | Visit copay only | N/A | N/A | $25–$75 |
| PlushCare | $19.99 + copay | Yes (in-network) | No | ~$50–$75 |
| Sesame | From $59 | Yes | No | ~$84 |
| WW Clinic | $74 ($25 first mo) | Yes (commercial) | No | ~$99 |
| Ro | $145 ($45 first mo) | Yes — full concierge | Yes — free | ~$170 |
| Walgreens | From $299 (program) | No | No | $299+ |
What You’ll Actually Pay: The Full Cost Breakdown
Drug copay vs. service fee: two separate bills
Your insurer pays for (or denies) the medication. Your telehealth provider charges separately for their platform and clinician time. These two costs come from different buckets, and they’re almost always quoted separately. When Ro says “$45 first month” — that’s the service. When Lilly says “$25 copay” — that’s the drug. When WW says “$74/month” — that’s the coaching platform. The medication is always on top.
Your deductible can inflate the first few months
“Covered” does not always mean “cheap today.” If your plan has a $2,000 pharmacy deductible and you haven’t met it, your first few fills of Zepbound could cost the full $1,086 per fill until you hit that threshold. The Zepbound savings card helps — it covers up to $100 per fill regardless of deductible status — but it won’t eliminate a large deductible gap entirely.
Ask your insurer: “Is tirzepatide subject to my pharmacy deductible, or does it go straight to my copay tier?” That one question can save you hundreds.
Savings program restrictions most people miss
- ⚠Commercial insurance only — government plans excluded by federal law
- ⚠Up to $100 max savings per 28-day fill — if your copay is $200, you still pay $100
- ⚠$1,300 annual cap — after that, you're back to your full copay for the rest of the year
- ⚠13 fills per year maximum
- ⚠Terms can change — the current card expires December 31, 2026
- ⚠Applies to single-dose pens with coverage — different rules for KwikPen and self-pay vials
How to Check Coverage Before You Pay Anyone
Don’t sign up for a $145/month membership to find out your plan doesn’t cover tirzepatide. Check first. Here’s the most efficient sequence:
Check your formulary
Call the number on the back of your insurance card and ask: "Is Zepbound on my plan's formulary for weight management?" If you have type 2 diabetes, ask about Mounjaro instead. Get the answer in writing — screenshot the online formulary or ask for a reference number.
Ask about prior authorization
GoodRx reports that for covered GLP-1 weight-loss drugs, over 88% still come with additional requirements such as prior authorization. Ask: "What documentation does my doctor need to submit?" Common requirements include BMI ≥30, documentation of lifestyle interventions, and sometimes step therapy.
Use a free coverage verification tool
Ro's GLP-1 Insurance Coverage Checker is the most robust free option we've found. You enter your insurance info, their team contacts your plan, and you get a personalized report. No charge, no obligation.
Gather your documentation before your first visit
Have ready: recent BMI measurement, list of comorbidities, history of diet/exercise/lifestyle interventions, any previous weight-loss medication trials. The stronger your documentation, the faster the prior authorization.
Save your insurer's answer in writing
If they confirm coverage verbally, ask for a reference number and the representative's name. Insurance companies occasionally walk back verbal confirmations. Written proof protects you.
What to Do If Your Insurance Says No
A denial stings. But it’s not the end — and it’s far more common than most people realize. AMA data shows 83.2% of prior authorization appeals result in partial or full overturn. Most people never appeal. That means most people leave coverage on the table.
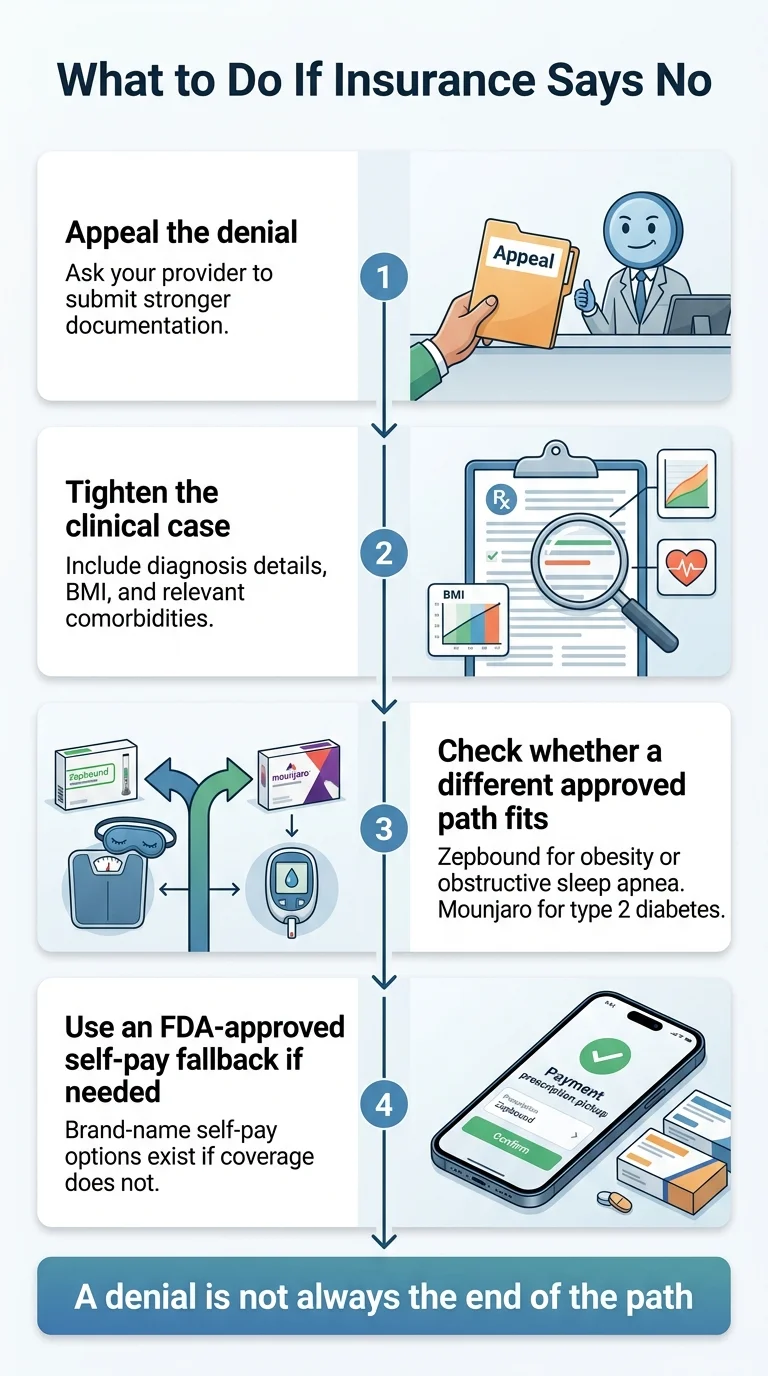
Appeal the denial
Ask your provider to submit: a letter of medical necessity, BMI documentation, evidence of comorbidities (diabetes, hypertension, sleep apnea, high cholesterol), history of lifestyle interventions (diet, exercise, behavioral counseling), and why tirzepatide specifically is appropriate. The Obesity Action Coalition provides free sample appeal letter templates.
Tighten the clinical framing
If your initial submission was vague, add specifics. Include lab results (A1C, lipid panel), sleep study results if applicable, and any documented weight-related health events. The more clinical evidence, the harder it is for the insurer to justify the denial.
Ask about alternate indications
If you have a documented clinical condition like obstructive sleep apnea or type 2 diabetes, your doctor may be able to frame the prior authorization around that indication — where coverage is more likely. Worth asking about.
Know your cheapest FDA-approved backup
If the appeal fails, LillyDirect self-pay pricing: $299/month (2.5 mg), $399/month (5 mg), $449/month (7.5–15 mg under journey offer with timely refills). You need a prescription — Ro or any licensed provider can write one and route it through LillyDirect. Same FDA-approved medication at a fraction of retail pen pricing.
More than 4 out of 5 appeals succeed at least partially. And even if the appeal doesn’t work, you have a clear backup path at $299/month.
Want help with the appeal? Ro's paid membership includes PA and appeal support →Why This Page Recommends FDA-Approved Paths First
If you’ve been researching tirzepatide online, you’ve probably seen compounded options at lower cash-pay prices. We cover those in our compounded GLP-1 vs name brand guide. But for this question — cheapest tirzepatide with insurance — compounded is almost never the right answer.
Insurance doesn't cover compounded medications
If your goal is to use your insurance to reduce costs, compounded tirzepatide doesn't help. It's cash-pay by definition.
FDA-approved is the insurance path
Zepbound and Mounjaro are the only tirzepatide products that can be billed to insurance, qualify for Lilly's savings programs, and go through standard pharmacy benefit channels.
The regulatory landscape has shifted
The FDA resolved the tirzepatide shortage and in March 2026 issued warnings to 30 telehealth companies regarding misleading compounded GLP-1 marketing. If you're pursuing insurance coverage, the FDA-approved route is both most relevant and safest.
Can You Use HSA or FSA to Pay for Tirzepatide?
Yes — prescription tirzepatide and qualifying medical expenses are generally HSA/FSA-eligible
This includes your drug copay and deductible costs. Telehealth program or membership fees may also qualify when the program treats a physician-diagnosed condition such as obesity, diabetes, hypertension, or heart disease — per IRS guidance on weight-loss expenses. However, this is not automatic for every fee.
Check with your plan administrator before assuming a specific membership qualifies. Any tax advantage depends on your own tax situation and bracket.
How We Verified Every Price on This Page
| Claim | Source | Checked |
|---|---|---|
| Zepbound $25 commercial copay with savings card | pricinginfo.lilly.com/zepbound | Apr 2026 |
| Savings card terms ($100/fill, $1,300/year, 12/31/2026) | zepbound.lilly.com/savings | Apr 2026 |
| LillyDirect self-pay vial pricing ($299/$399/$449) | zepbound.lilly.com/savings | Apr 2026 |
| 45-day refill rule for higher-dose journey offer | zepbound.lilly.com/savings terms | Apr 2026 |
| Ro membership $45 first month / $145 ongoing | ro.co/weight-loss/pricing | Apr 2026 |
| PlushCare $19.99 membership | plushcare.com/membership | Apr 2026 |
| WW Med+ $25/$74, meds not included | weightwatchers.com terms | Apr 2026 |
| Sesame from $59/month | sesamecare.com/medication/tirzepatide | Apr 2026 |
| Walgreens: no insurance/PA support for GLP-1s | walgreens.com/zepbound | Apr 2026 |
| 83.2% PA appeal overturn rate | AMA prior authorization data | Apr 2026 |
| 109M+ with no Zepbound commercial coverage | GoodRx insurance tracking | Apr 2026 |
| Medicare GLP-1 Bridge: Jul 1–Dec 31, 2026; $50; KwikPen only | CMS.gov | Apr 2026 |
| 13 state Medicaid FFS programs cover GLP-1s for obesity | KFF | Apr 2026 |
| FDA March 2026 compounded GLP-1 enforcement | FDA.gov | Apr 2026 |
What “all-in cost” means on this page: We add the provider’s service fee to the likely medication cost (including savings programs if applicable). We note when deductibles, labs, or other variable costs may apply. We never quote just the drug copay as if that’s the total.
For errors or outdated pricing: corrections@therxindex.com
Frequently Asked Questions
Can you get tirzepatide online with insurance?+
Can you really get Zepbound for $25 a month?+
Can you really get tirzepatide for $25 a month with insurance?+
What is the cheapest online provider for tirzepatide with insurance?+
Does Ro's $145 monthly fee include the medication?+
Does WeightWatchers include tirzepatide in the monthly price?+
Is Zepbound or Mounjaro easier to get covered by insurance?+
What should I do if my insurance denies tirzepatide?+
Does Medicare cover Zepbound for weight loss in 2026?+
Does Walgreens handle insurance for Zepbound?+
Can I use HSA or FSA to pay for tirzepatide?+
Is compounded tirzepatide covered by insurance?+
Still not sure which GLP-1 program is right for you?
Answer a few quick questions about your insurance, goals, and budget — we’ll show you the most affordable path for your exact situation. No signup required.
Related guides and comparisons
- Cheapest Tirzepatide Online Without Insurance: All Options Compared
- GLP-1 Cost Without Insurance: Every Option Compared (2026)
- How to Get GLP-1 Without Insurance in 2026: Every Path Explained
- How to Get Insurance to Cover GLP-1 (2026)
- Does Insurance Cover Wegovy for Weight Loss? (2026)
- Compounded GLP-1 vs Name Brand: Honest 2026 Verdict
- Cheapest Zepbound Without Insurance: $299/Mo Path (2026)
- Mochi vs Ro for GLP-1: 9 Real Differences in 2026
- MEDVi vs Hims: Full 2026 Comparison
Written by The Rx Index Editorial Team. Last verified: April 2026. Next audit: May 2026.
The Rx Index is an independent research platform. We may earn a commission when you visit a provider through our links — this does not affect our rankings, recommendations, or the price you pay. Full affiliate disclosure · Editorial standards
This content is for informational purposes only and does not constitute medical advice. Tirzepatide (Zepbound, Mounjaro) is a prescription medication and should only be used under the guidance of a licensed healthcare provider. Insurance coverage, savings card terms, and provider pricing are subject to change — always verify current terms directly with your insurer and chosen provider.