GLP-1 Providers That Accept Aetna: 5 Real Options in 2026
Looking for GLP-1 providers that accept Aetna? Start with PlushCare — it's in-network with Aetna, works in all 50 states, and handles prior authorization for FDA-approved GLP-1s like Wegovy and Zepbound. Most patients with in-network insurance pay $30 or less per visit.
But here's the part most sites skip: whether a provider “accepts Aetna” matters less than whether your specific Aetna plan actually covers weight-loss GLP-1s. Aetna's own employer page states that employers can “choose to customize your benefits to include or exclude GLP-1 drug coverage for weight management.” That means two people with Aetna cards from the same company can have completely different GLP-1 coverage.
Bottom Line
PlushCare is the safest national starting point for Aetna members who want an FDA-approved GLP-1 through insurance. It's in-network with Aetna, prescribes brand-name GLP-1 medications including Wegovy, Zepbound, Ozempic, and Mounjaro, and its weight-loss prior-authorization decisions average 7–14 business days.
If your Aetna plan excludes weight-loss drugs, no provider can override that — skip straight to the denial and fallback section.
This page is for
Aetna members who want FDA-approved GLP-1 access and the least-friction insurance path.
This page is NOT for
Members who already know their plan won't cover GLP-1s. See our cash-pay GLP-1 guide instead.
Jump to: Full comparison · How Aetna coverage works · Provider details · Drug-by-drug coverage · What you'll pay · Check your plan · If Aetna says no · FAQ
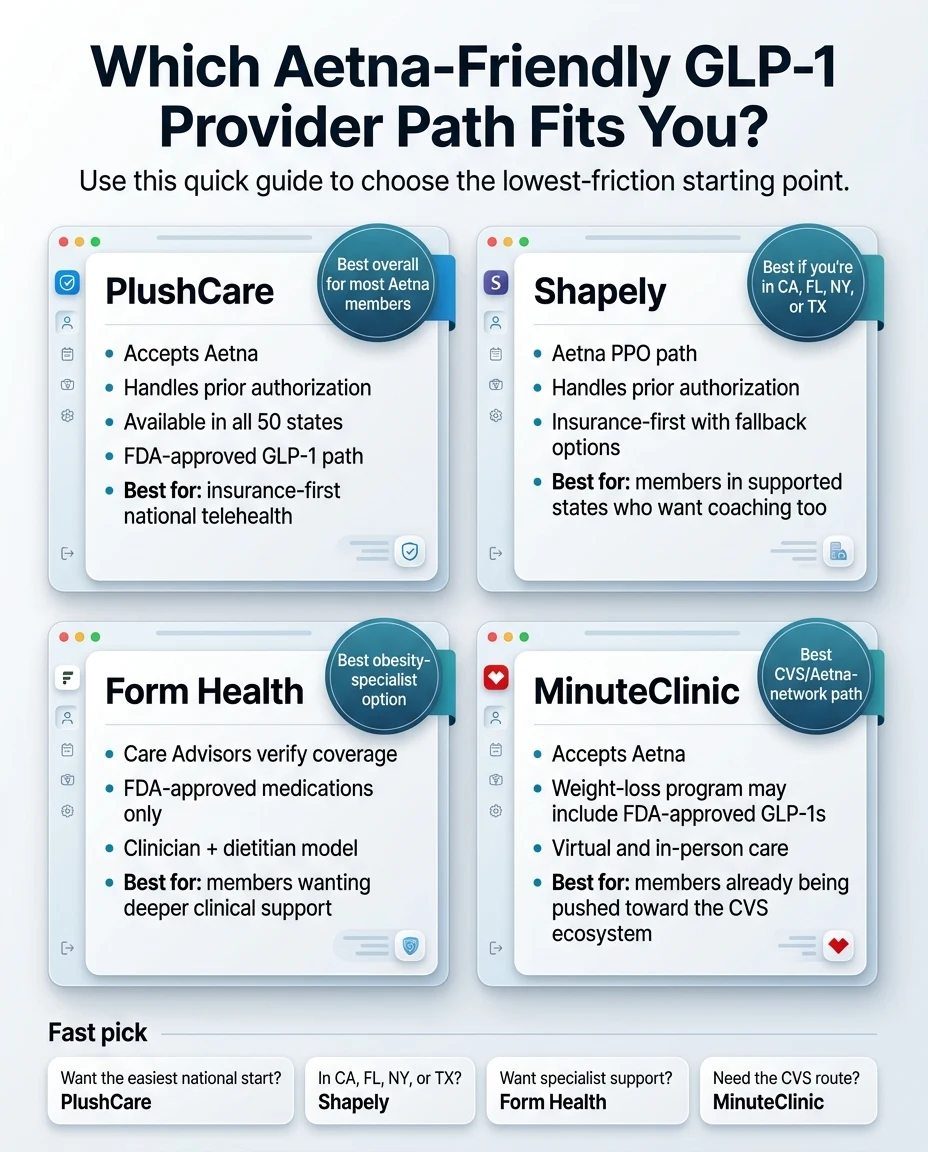
The RX Index Aetna GLP-1 Provider Fit Matrix
We assembled this comparison from each provider's current insurance pages, pricing pages, and published workflows — cross-referenced against Aetna's own formulary documents and clinical policy bulletins. Anything we couldn't independently confirm on a consumer-facing source is marked NEEDS VERIFICATION.
Sources cited per row. Verify all provider claims directly before committing. Last verified April 2026.
| Provider | Accepts Aetna? | PA Help? | Program Fee | Visit Cost | States | Best For |
|---|---|---|---|---|---|---|
| PlushCare★ Best Overall | ✅ Yes, in-network | ✅ Handles PA | $19.99/mo | $30 or less (most in-network) | All 50 states | Most Aetna members wanting insurance-first |
| Shapely | ✅ Aetna PPO in-network | ✅ Handles PA | $49/mo membership | Copay varies by plan | CA, FL, NY, TX | Aetna PPO members in 4 states wanting coaching too |
| Form HealthNEEDS VERIFICATION | ⚠️ Likely — verify first | ✅ Care Advisors check | In-network copay or $299/mo self-pay | Copay varies | 50 states NEEDS VERIFICATION | Obesity-specialist + dietitian care |
| MinuteClinic | ✅ Aetna in-network | ⚠️ Moderate | Insurance copay varies | Copay varies | Broad retail; GLP-1 not all states | CVS/Aetna ecosystem members |
| Ro | ❌ Cash-pay membership | ✅ Strong insurance concierge | $145/mo (first mo $45) | N/A — cash membership | National | PA help without needing in-network visit billing |
→ Already know your Aetna plan covers GLP-1s?
Check Eligibility on PlushCare — They Handle the Aetna Paperwork→ Not sure if your plan covers it?
Keep reading — we break down the exact steps to find out in 10 minutes, starting with the 4-Gate Friction Map below.
How Aetna GLP-1 Coverage Actually Works: The 4-Gate Friction Map
Most pages will tell you “Aetna covers Wegovy” or “Aetna requires prior authorization.” Both statements are technically true and practically useless — because Aetna approvals fail at one of four specific gates. Knowing which gate you're stuck at determines whether you need a better provider, a different drug, an appeal, or an entirely different strategy.
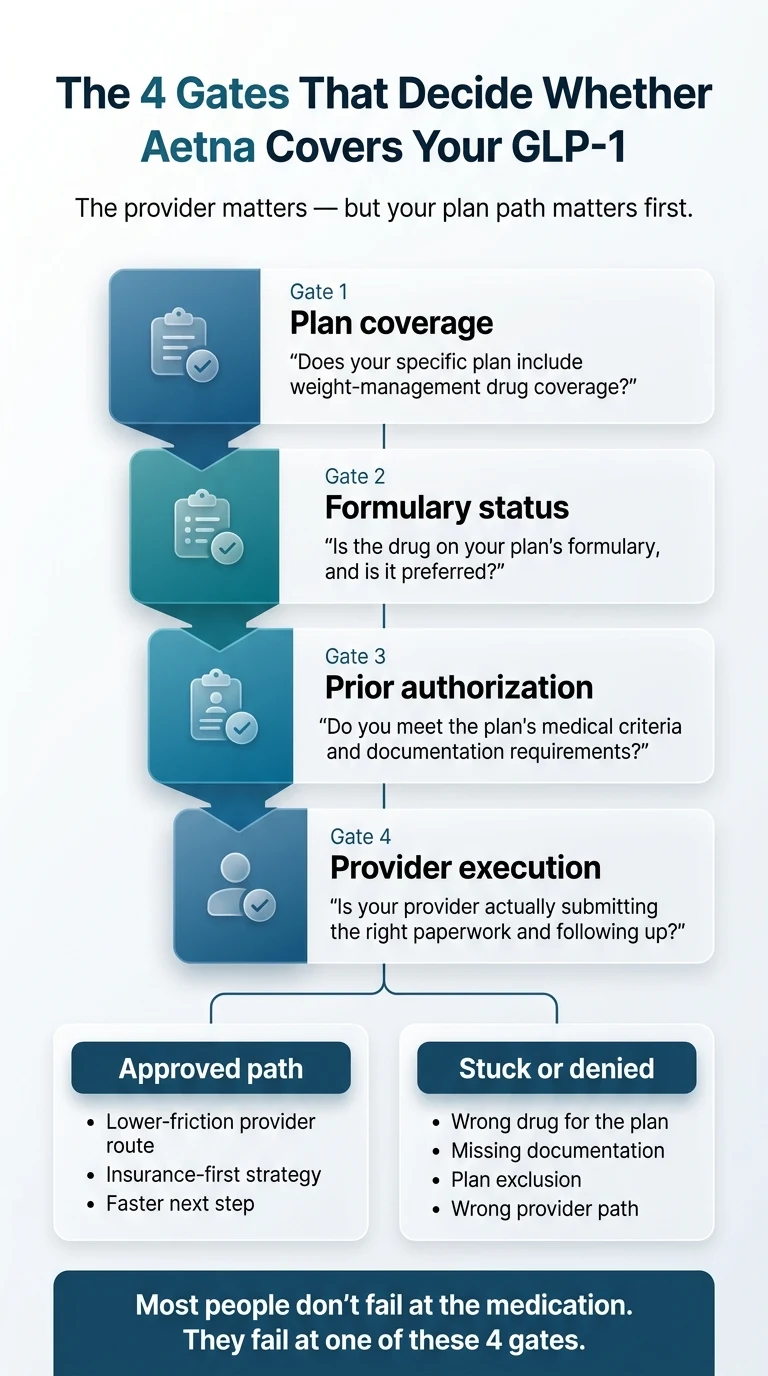
Gate 1: Does Your Plan Even Include Weight-Loss GLP-1 Coverage?
This is the gate that wastes the most time. Aetna is not one plan — it's hundreds of plan configurations. Aetna's employer page says explicitly that employers can choose to include or exclude GLP-1 weight-management coverage.
Plans that may cover weight-loss GLP-1s
- ✓Employer-sponsored commercial plans (fully insured) — many cover Wegovy with PA, but some employers opt out
- ✓ACA marketplace plans — may cover when medically necessary
Plans with known coverage restrictions
- ✗AFA level-funded plans — Word & Brown 2026 carrier guide confirms weight-loss medication coverage is excluded
- ✗Self-funded employer plans — depends entirely on what your employer chose
- ✗Aetna Medicare Advantage — Medicare does not currently cover GLP-1s for weight loss (Medicare GLP-1 Bridge launches July 1, 2026)
- ✗Aetna Medicaid — policies vary by state; some programs cover Wegovy only for cardiovascular risk reduction
How to tell which plan you have: Call the Member Services number on the back of your Aetna card. Ask specifically: “Does my plan cover prescription medications for chronic weight management?” Don't ask “does Aetna cover Wegovy” — the answer will be “some plans do,” which doesn't help you.
Sources: Aetna employer GLP-1 coverage page; Word & Brown 2026 carrier guide (AFA exclusion); Aetna Better Health Medicaid policy (IL/FL/PA, effective 4/2/2026); CMS Medicare GLP-1 Bridge FAQ (updated April 6, 2026).
Gate 2: Is Your Target Drug on the Formulary — and Is It Preferred?
Even if your plan includes weight-loss coverage, each drug has different formulary status. Here's what we found on Aetna's 2026 Standard Plan drug guide and clinical policy bulletins:
| Medication | FDA Approved For | Aetna Status (Weight Loss) | PA Required? |
|---|---|---|---|
| Wegovy (semaglutide) | Weight loss + CVD risk | ✅ On formulary — anti-obesity list | Yes |
| Zepbound (tirzepatide) | Weight loss + OSA | ⚠️ Preferred-options friction — Wegovy listed as preferred | Yes |
| Ozempic (semaglutide) | Type 2 diabetes | ❌ Not on anti-obesity formulary — covered for diabetes only | Yes (diabetes) |
| Mounjaro (tirzepatide) | Type 2 diabetes | ❌ Not on anti-obesity formulary — covered for diabetes only | Yes (diabetes) |
| Saxenda (liraglutide) | Weight loss | ⚠️ Appears on preferred-options table | Yes |
Source: Aetna 2026 Standard Plan drug guide PDF; Aetna antidiabetics formulary. Last verified April 2026.
The practical takeaway: Wegovy is the cleanest weight-loss coverage path on most Aetna plans. If your doctor is trying to get Zepbound covered for weight loss, they may hit preferred-drug friction. Ask your provider about starting with Wegovy unless there's a specific clinical reason for Zepbound.
Gate 3: Do You Meet the Prior-Authorization Criteria?
Prior authorization is Aetna's way of confirming the drug is medically necessary before they'll pay. Here's where it gets tricky: different Aetna policy bulletins specify different thresholds depending on the drug and policy version.
What we found across current Aetna PA bulletins
- BMI threshold: One current non-Medicare bulletin (6450-C) uses BMI ≥35. Other Aetna bulletins reference BMI ≥30, or BMI ≥27 with at least one weight-related comorbidity (hypertension, T2D, dyslipidemia, or OSA).
- Weight-management documentation: Six months of documented participation in a weight management program (diet, exercise, behavioral modification) is commonly required before PA approval.
- Renewal criterion (from 1/1/2026): For renewals, the prescriber must show the patient has maintained at least 5% weight loss from baseline.
Pro tip for your doctor's office: Aetna's Pharmacy Management Precertification Unit: 1-800-414-2386. Your provider can also access precertification forms through Aetna's provider portal.
Sources: Aetna Pharmacy Clinical Policy Bulletin 6450-C (Weight Loss BMI 35); Bulletin 4774-C (Wegovy); Aetna 2026 Standard Plan documentation.
Gate 4: Is Your Provider Actually Executing the Paperwork?
A PCP who doesn't regularly prescribe GLP-1s may not know which Aetna bulletin applies, how to document the weight-management requirement, or when to push back on a denial. A provider that specializes in GLP-1 prescribing handles this routinely.
This is the core reason this page exists. Not all providers who “accept Aetna” are equally skilled at navigating the approval process. The five providers in our matrix were selected because they each publish a documented workflow for handling insurance-based GLP-1 prescribing.
Handles PA · All 50 states · Most in-network patients pay $30 or less per visit
Which GLP-1 Providers That Accept Aetna Are Worth Trying First?
We evaluated over a dozen telehealth and in-person providers against one question: does this provider actually take Aetna AND actively help with the GLP-1 insurance process? Plenty of providers prescribe GLP-1s. Far fewer fight for coverage on your behalf. These five earned their spots.
PlushCare
PlushCare is the safest national starting point because it does three things most competitors don't do simultaneously: explicitly accepts Aetna insurance, prescribes multiple brand-name FDA-approved GLP-1 medications, and handles prior authorization as part of the standard workflow.
What you're getting: A scheduled video visit with a board-certified physician (average 15 years of clinical experience, per PlushCare). Same-day appointments are often available. Your doctor reviews your health history, discusses medication options, orders labs through Quest Diagnostics if needed, and sends the prescription to your preferred pharmacy including retail pharmacies like CVS and Walgreens. PlushCare's team handles the prior-authorization submission.
Medications available: Wegovy, Zepbound, Ozempic, Mounjaro, Saxenda, and Rybelsus, plus non-GLP-1 weight-loss options like Contrave and Xenical.
What it costs with Aetna
Honest limitation
PlushCare is a general telehealth platform, not an obesity-specialist program. There's no structured coaching, no dietitian support, no accountability curriculum. It's a doctor's visit — a very good, very efficient one — but if you want someone guiding your nutrition alongside the medication, Form Health or Shapely offer more. For this specific query (finding Aetna-accepting providers), PlushCare's insurance-first efficiency wins.
Who should choose PlushCare
- ✓Aetna members whose plans cover weight-loss GLP-1s
- ✓People who want brand-name FDA-approved medication through insurance
- ✓Anyone who values speed — same-day appointments, all 50 states
Who should skip PlushCare
- ✗Members who already know their plan excludes weight-loss drugs
- ✗Anyone who wants structured coaching or dietitian support
“It cost me no more than what I would have paid to visit an office.” — Featured patient review on PlushCare's website
In-network with Aetna · All 50 states · Handles prior authorization
Shapely
Shapely earns a full section because it's one of the few providers with a dedicated Aetna landing page, explicit in-network status for Aetna PPO members, and a clearly published fallback path if insurance doesn't cover your medication.
What you're getting: Virtual medical visits, nutrition coaching, dietitian-led lifestyle support, and a team that handles prior authorization for FDA-approved GLP-1s. If your Aetna plan covers Wegovy or Zepbound, Shapely bills insurance. If it doesn't, they offer self-pay alternatives starting at $99/month for compounded semaglutide and $166/month for compounded tirzepatide.
What it costs with Aetna
The catch: Shapely currently serves only California, Florida, New York, and Texas. If you're outside those four states, this isn't your option — go with PlushCare instead.
Who should choose Shapely
- ✓Aetna PPO members in CA, FL, NY, or TX
- ✓People who want both insurance-first AND a self-pay fallback in one provider
- ✓Members who value nutrition coaching alongside medication
Who should skip Shapely
- ✗Anyone outside the 4 covered states
- ✗Aetna HMO members (Shapely specifies PPO)
CA, FL, NY, TX only · Aetna PPO in-network
Form Health
Form Health is the pick for Aetna members who want more clinical depth — an obesity medicine specialist (not a general PCP) plus a registered dietitian, working together on a structured program with FDA-approved GLP-1s only.
The Aetna question: Form Health's employer-facing materials show Aetna in their in-network section, and their FAQ states they accept “most major private insurance.” Their Care Advisors verify your specific coverage before your first visit. However, we could not find explicit consumer-facing confirmation that says “we accept Aetna” in the same clear language PlushCare and Shapely use. We've marked this NEEDS VERIFICATION and recommend confirming directly with Form's Care Advisors before booking.
What it costs
Form Health does NOT try to be the fastest, cheapest path. If speed and low cost are your priority, PlushCare is better. But because Form is built specifically around obesity medicine — with clinicians trained in this specialty and dietitians working alongside them — it's the stronger fit for members who want deeper clinical oversight and structured support alongside their medication.
Verify Aetna acceptance directly before booking
MinuteClinic
If you've been getting letters about CVS Weight Management or Aetna's Health Optimizer program, MinuteClinic is worth knowing about. CVS confirms that MinuteClinic accepts Aetna insurance and offers a weight-loss program that may include GLP-1 medications when clinically appropriate.
Why this matters for Aetna members: Aetna is part of the CVS Health family. CVS Caremark manages Aetna's pharmacy benefits. Some Aetna members report being directed toward CVS Weight Management or Health Optimizer programs as part of their coverage path — MinuteClinic is one of the in-network clinical options within that ecosystem.
The honest limitations: MinuteClinic's GLP-1 prescribing isn't available in every state. The experience is closer to a retail clinic visit than a telehealth program. MinuteClinic doesn't offer the same level of dedicated PA-chasing that PlushCare or Shapely provide.
GLP-1 availability varies by state and location
Ro
We're including Ro because if you search for GLP-1 providers that accept Aetna, Ro will appear in your research — and the distinction matters.
Ro does NOT accept Aetna for its membership. The Ro Body Program is cash-pay: $145/month (first month $45), which includes coaching, labs, and an insurance concierge. Medication is separate and billed through your pharmacy.
What Ro DOES do well: Its insurance concierge verifies your Aetna benefits, submits prior-authorization requests for FDA-approved GLP-1s, helps navigate denials, and works to find pharmacy stock. Ro says its insurance path can take about 1–3 weeks. If your Aetna plan covers Wegovy, Ro's concierge can help you access it — the membership is just the service wrapper.
The practical question: Is paying $145/month for Ro's concierge + coaching worth it compared to $19.99/month for PlushCare, which is actually in-network with Aetna? For most Aetna members who haven't tried using their insurance yet: start with PlushCare or Shapely first. But if you've already been denied and want aggressive concierge-level advocacy, Ro's prior-auth support is among the strongest in telehealth.
Cash-pay membership · Strong PA concierge for denied members
Does Aetna Cover Wegovy, Zepbound, Ozempic, or Mounjaro?
The short answer is yes for some, no for others, and “it depends on your exact plan” for the rest. Here's the drug-by-drug breakdown so you can match your situation.
Wegovy With Aetna: The Cleanest Weight-Loss Path
Wegovy (semaglutide) is the most likely GLP-1 to be covered by your Aetna plan for weight loss. It appears on Aetna's 2026 Standard Plan formulary under anti-obesity agents.
Wegovy is also the only GLP-1 with FDA approval for both chronic weight management AND cardiovascular risk reduction (reducing the risk of heart attack, stroke, and cardiovascular death in adults with established heart disease and obesity or overweight). That dual indication strengthens your coverage case if you have cardiovascular risk factors — and it's why some Aetna Medicaid programs cover Wegovy specifically for cardiovascular risk reduction even when weight-loss-only use is excluded.
Oral Wegovy: Novo Nordisk launched Wegovy pills in early 2026. Whether your Aetna plan covers the oral form is still evolving — formulary additions often lag behind FDA approvals. Ask your provider or call Aetna Member Services to check current status.
Wegovy savings card: If your Aetna plan covers Wegovy, the Novo Nordisk savings offer may bring your copay down to as little as $25/month (maximum savings of $100 per fill, terms updated January 2026). Not available for government insurance (Medicare, Medicaid, TriCare).
Zepbound With Aetna: Why “Preferred Option” Friction Matters
Zepbound (tirzepatide) is FDA-approved for weight loss and obstructive sleep apnea. On Aetna's 2026 Standard Plan drug guide, Zepbound appears in the preferred-options table — but with Wegovy, Qsymia, and Saxenda listed as preferred alternatives. That means if you want Zepbound specifically, your provider may need to demonstrate why those alternatives aren't appropriate for you.
Zepbound may still be covered for obstructive sleep apnea on some Aetna plans. If you specifically want tirzepatide for weight loss, ask your provider about the preferred-alternatives process, or explore whether a sleep-apnea or other indication might apply.
Ozempic and Mounjaro: A Different Path
Ozempic (semaglutide) and Mounjaro (tirzepatide) are FDA-approved for Type 2 diabetes, not weight loss. Aetna covers both for diabetes management with prior authorization. They do not appear on Aetna's anti-obesity formulary.
If you have a Type 2 diabetes diagnosis, these may be the appropriate medications — and they produce weight loss as a clinical effect. Your provider can prescribe them for their approved indication.
Prescribes Wegovy, Zepbound, Ozempic, Mounjaro, Saxenda, Rybelsus
What You'll Actually Pay With Aetna
“Accepts insurance” doesn't mean free. The real cost is a stack of separate fees, and nobody on page one breaks this down honestly. Here's what we found:
| Your Situation | Provider Fee | Medication Cost | Realistic Monthly Range |
|---|---|---|---|
| Aetna covers Wegovy + savings card | $19.99/mo (PlushCare) + ~$30 visit (periodic) | ~$25/mo (savings card) | $50–$80/mo |
| Aetna covers Wegovy, no savings card | $19.99/mo (PlushCare) + ~$30 visit (periodic) | Specialty tier copay varies by plan | $70–$200+/mo |
| Plan excludes — cash-pay compounded | Included in MEDVi fee | $149–$299/mo (varies by provider and dose) | $149–$299/mo |
| Plan excludes — cash-pay oral Wegovy (FDA-approved) | Hims membership separate | Starting at $149/mo medication | $188–$300+/mo |
| Full retail no assistance | $129 self-pay visit (one-time) | $1,349/mo (Wegovy list price) | $1,350+/mo |
HSA and FSA note: Many GLP-1 medications may qualify as HSA/FSA-eligible medical expenses, which can effectively reduce your cost by 20–35% depending on your tax bracket. Eligibility rules vary — check with your plan administrator and review IRS qualified medical expense guidelines before assuming coverage.
You'll know what you'd pay before you commit
How to Check Your Exact Aetna Coverage in 10 Minutes
Before you book with any provider, 10 minutes of homework will save you weeks of frustration.
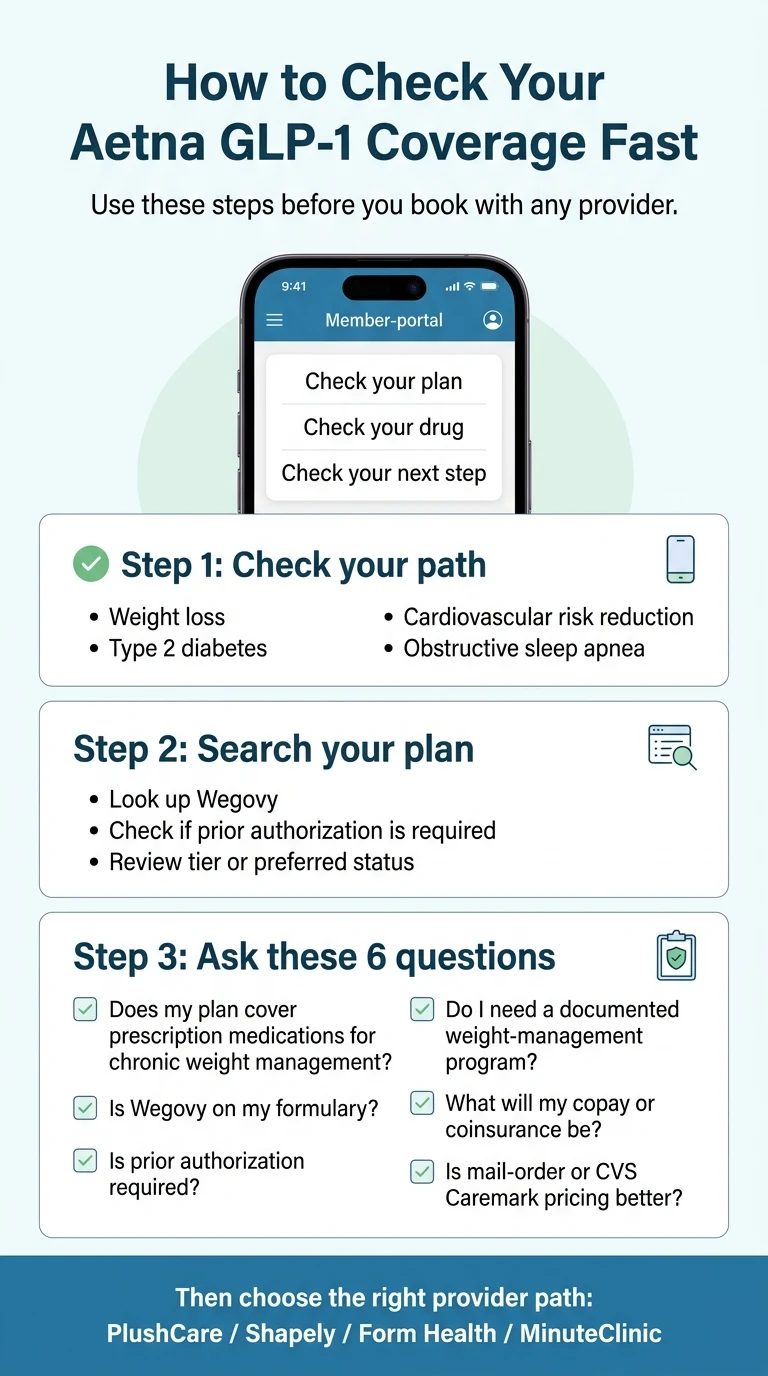
Step 1: Log Into Aetna's Member Portal
Go to aetna.com and log into your member account. Navigate to the “Find a Medication” drug search tool. Search for “Wegovy” and check whether it appears as covered on your specific plan, which tier it's on, and whether PA is required.
Step 2: Identify Your Path
Your coverage depends on WHY you need the medication:
- Weight loss: Wegovy is the primary option — check anti-obesity coverage
- Type 2 diabetes: Ozempic or Mounjaro — check diabetes medication coverage
- Cardiovascular risk reduction: Wegovy — may strengthen your PA case
- Obstructive sleep apnea: Zepbound — coverage varies by plan
Step 3: Call Member Services With These 6 Questions
Call the number on the back of your Aetna card. Use this exact script:
6-Question Aetna Call Script
- 1Does my specific plan cover prescription medications for chronic weight management?
- 2Is Wegovy on my plan's formulary? What tier is it on?
- 3What are the prior-authorization requirements for Wegovy on my plan — specifically, what BMI threshold and documentation do I need?
- 4Do I need to complete a weight-management program before approval? If so, what counts as documented participation?
- 5What is my copay or coinsurance for specialty-tier medications? Does my deductible apply first?
- 6Can I use a mail-order pharmacy through CVS Caremark for better pricing?
Write down the answers. Bring them to your provider appointment.
Step 4: Book the Right Provider
Now that you know your coverage status:
- Covered with PA required: PlushCare (national) or Shapely (CA/FL/NY/TX)
- Covered but want specialist care: Form Health (confirm Aetna status first)
- CVS program involvement: MinuteClinic
- Not covered or excluded: Skip to the denial/fallback section
Step 5: Gather Documents Before Your Appointment
Your provider will need:
- Your most recent BMI (measured at a doctor's visit)
- Documentation of weight-related comorbidities (hypertension, T2D, high cholesterol, sleep apnea)
- Records of your weight-management efforts (food logs, gym records, dietitian visits, program enrollment)
- A list of any medications you've tried for weight loss previously
Skip the phone call? PlushCare checks your Aetna coverage when you sign up — their team handles the verification so you don't have to sit on hold.
They handle the paperwork · Takes 60 seconds to sign up
What If Aetna Denies or Excludes Your GLP-1?
This is where most “Aetna GLP-1 coverage” articles end. The critical first step: denial is not the same as exclusion. The fix is completely different depending on which one you're facing.
If Your Plan Excludes Weight-Loss Drugs Entirely
No provider — not PlushCare, not Shapely, not Ro — can override a plan-level exclusion. If your Aetna plan was configured to exclude weight-loss medications, no amount of paperwork changes that.
Your options:
- Talk to your HR benefits manager. They can request a plan design change for the next enrollment period. If enough employees ask, employers sometimes add coverage.
- Switch to a cash-pay path. This is where the insurance conversation ends and the affordability conversation begins.
If You Were Denied for Weak Documentation
This is the most common fixable denial. The PA was submitted but lacked adequate BMI documentation, weight-management program records, or comorbidity evidence.
Fix: Ask your provider to resubmit with complete documentation. Have your doctor include a detailed letter of medical necessity addressing the specific criteria in the Aetna PA bulletin that applies to your plan.
If You Were Denied Because the Drug Isn't Preferred
If you requested Zepbound and got denied because Wegovy is the preferred option, the simplest fix is often switching to Wegovy (unless there's a clinical reason not to). Your provider can also submit a formulary exception request explaining why the non-preferred drug is medically necessary.
If You Were Denied and Want to Appeal
Data from Honest Care's GLP-1 Patient Access Report (Q3/Q4 2025), analyzing 1,000+ U.S. GLP-1 denial cases, found that 65%+ of appealed denials were overturned when properly documented. You have the right to appeal, and for claims of $500 or more, Aetna's own policy allows you to request an independent external review.
Appeal Steps
- 1Get the denial reason in writing from Aetna
- 2Ask your provider for a peer-to-peer review with Aetna's medical director
- 3Submit a formal appeal with strengthened documentation — Novo Nordisk provides a sample appeal letter template your provider can customize
- 4If the appeal is denied, request an external independent review
- 5Contact your HR benefits manager if you're on an employer plan — they may have leverage on plan design
If All Else Fails: Your Cash-Pay Fallback Options
If your Aetna plan won't cover GLP-1s and appeals haven't worked, you're not out of options — you're on a different path.
Most Affordable Compounded Option
MEDVi offers compounded semaglutide starting at $149–$179 for the first month and $299/month ongoing (pricing varies by current promotion — verify on MEDVi's site). Price includes physician consultations, support, and free shipping. No insurance needed, no prior authorization, no waiting.
Important: Compounded semaglutide is prepared by state-licensed compounding pharmacies. It is NOT FDA-approved as a finished product and has not been independently evaluated by the FDA for safety, efficacy, or quality as a completed medication.
Ships to your door · No prior authorization · Aetna denial not a barrier
Brand-Name FDA-Approved on Cash-Pay
Oral Wegovy is available starting at $149/month for medication through providers like Hims, though a separate membership fee applies. Check Hims' current pricing page for total cost including membership.
Medication + membership — check for total cost
What About Aetna's Health Optimizer and CVS Weight Management?
If you're an Aetna member, you may have received a letter or email about “Health Optimizer” or “CVS Weight Management.” These are programs within the Aetna/CVS ecosystem designed to support weight management alongside GLP-1 therapy.
What Aetna's own page describes: CVS Weight Management includes one-on-one dietitian counseling, a digital coaching app, connected devices (like a smart scale), and support for members both with and without existing GLP-1 prescriptions. Aetna frames it as an optional add-on that employers can choose to include.
What this means for you: If your employer has added CVS Weight Management to your plan, participation may help satisfy the weight-management documentation requirement that strengthens your PA case. Whether it's required or supplementary for your specific plan is something only Aetna Member Services can confirm.
If you're confused: Ask Aetna directly: “Is participation in CVS Weight Management or Health Optimizer required for my GLP-1 prior authorization, or is it supplementary?” Get the answer in writing.
If You're Still Stuck: The Quick Decision Filter
| Your Situation | Best First Move |
|---|---|
| Aetna plan covers GLP-1s, want national telehealth | PlushCare |
| Aetna PPO in CA, FL, NY, or TX | Shapely |
| Want obesity-specialist + dietitian (confirm Aetna first) | Form Health |
| Keep getting directed to CVS programs | MinuteClinic |
| Want aggressive PA help, don't mind cash-pay membership | Ro |
| Aetna excludes weight-loss meds, want compounded | MEDVi |
| Aetna excludes, want brand-name cash-pay | Oral Wegovy via Hims |
| On Aetna Medicare, waiting for July 2026 Bridge | Talk to your doctor now — prep with our Medicare GLP-1 guide |
| Not sure about anything yet | Take the 60-second quiz |
How We Verified These Providers
Every claim in this article has a specific source. Here's our process:
Aetna coverage data: Sourced from Aetna's employer-facing GLP-1 coverage page, Aetna's 2026 Standard Plan drug guide PDF (updated the first week of each month per Aetna's documentation), Aetna Pharmacy Clinical Policy Bulletins (6450-C for weight loss, 4774-C for Wegovy), Aetna Better Health Medicaid policy documents (IL/FL/PA, effective 4/2/2026), the Word & Brown 2026 carrier guide for AFA plan exclusions, and CMS Medicare GLP-1 Bridge FAQ (updated April 6, 2026).
Provider data: Each provider's insurance acceptance, pricing, state availability, and PA workflow was verified on their official website as of April 2026. Where we could not independently confirm a claim on a consumer-facing source (like Form Health's Aetna acceptance), we marked it NEEDS VERIFICATION.
What NEEDS VERIFICATION means: We found evidence suggesting the claim is likely true (e.g., from an employer-facing page or general insurance statement) but couldn't confirm it on a consumer-facing source. Verify directly with the provider before committing.
How often we update: Provider pricing and Aetna formulary status: monthly. PA criteria, provider state availability, and CVS program language: quarterly. The “Last verified” date at the top reflects our most recent audit.
Frequently Asked Questions
Does Aetna cover Wegovy for weight loss?▾
Does Aetna cover Zepbound for weight loss?▾
Does Aetna require prior authorization for GLP-1s?▾
Can a telehealth provider get around an Aetna plan exclusion?▾
Which online provider is the safest first try if I have Aetna?▾
Does PlushCare accept Aetna?▾
Does Shapely accept Aetna?▾
Does Form Health accept Aetna?▾
Does MinuteClinic accept Aetna?▾
Does Ro accept Aetna?▾
What is Aetna's Health Optimizer?▾
How long does Aetna GLP-1 prior authorization take?▾
Will Aetna Medicare cover GLP-1s for weight loss?▾
What if my Aetna plan doesn't cover GLP-1s and I can't afford retail pricing?▾
Still not sure which GLP-1 program is right for you?
Answer 6 questions. We'll route you to the right path based on your Aetna plan, budget, and preferences.
Take the Free 60-Second GLP-1 Matching Quiz →Written by The RX Index Editorial Team · Last verified · The RX Index is an independent comparison resource for GLP-1 telehealth providers.