By The RX Index Editorial Team · 5 provider paths reviewed · Cigna coverage policies IP0206, IP0701, CNF-684, CNF-908, CNF-950 verified
Last verified: · Evernorth benefit materials verified from evernorth.com
Editorial Standards · Affiliate Disclosure · Next audit: July 2026
GLP-1 PROVIDERS THAT ACCEPT CIGNA — 2026 VERIFIED GUIDE
GLP-1 Providers That Accept Cigna: 5 Real Paths to Wegovy or Zepbound (2026)
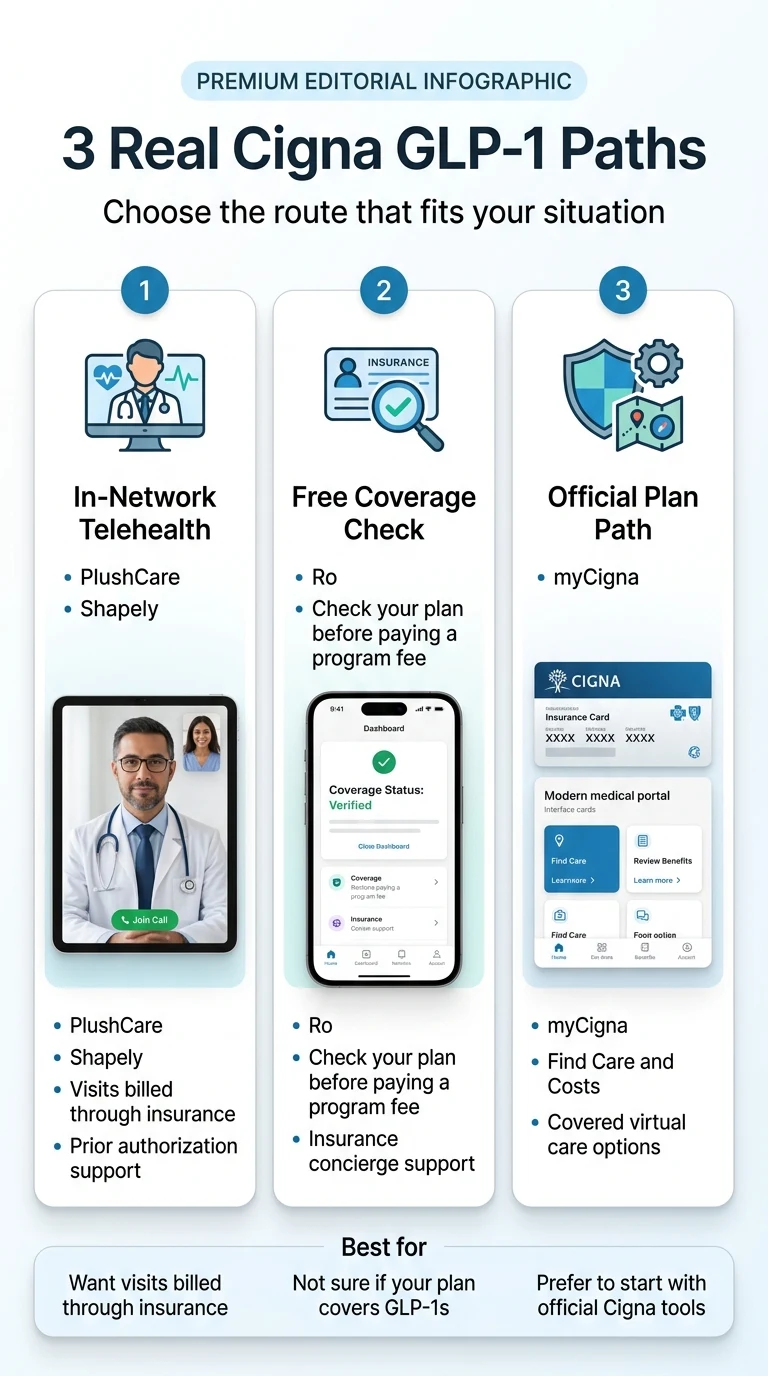
If you're searching for GLP-1 providers that accept Cigna, here's the short version: PlushCare is the strongest nationwide option — it's in-network with Cigna, handles prior authorization, and prescribes brand-name GLP-1 medications including Wegovy, Zepbound, Ozempic, Mounjaro, Rybelsus, and Saxenda in all 50 states. Most patients with in-network insurance pay $30 or less per visit. Shapely is the best exact-match Cigna option if you're in California, Florida, New York, or Texas — visits are billed directly through your Cigna plan.
But here's what most pages won't tell you upfront: Cigna GLP-1 coverage varies dramatically by employer and plan segment. Reuters reported in September 2025 that more than 50% of Evernorth's large-employer clients cover obesity drugs for weight management — but only 15–20% of Cigna Healthcare's smaller-employer clients do. Your employer decides whether your plan includes weight-loss drug coverage, and no provider — not even an in-network one — can fix a plan exclusion.
That's not a dead end. It just means you need to know which path is actually real for your specific situation. We built this page to give you that answer in one place — no opening five tabs, no guessing, no signing up for a program fee only to discover your plan won't cover the medication.
Disclosure: Some links on this page are affiliate links. If you purchase through these links, we may earn a commission at no extra cost to you.
GLP-1 Providers That Accept Cigna: Quick Comparison
We verified each provider's Cigna compatibility, prior authorization support, pricing, and reach from their official pages in April 2026. Provider-stated information — verify directly before enrolling.
| Provider | Bills Cigna for Visits? | Handles Prior Auth? | FDA Meds? | Pricing (Provider-Stated) | States | Best For |
|---|---|---|---|---|---|---|
| PlushCare | ✅ Cigna in-network | ✅ Yes | Wegovy, Zepbound, Ozempic, Mounjaro, Rybelsus, Saxenda | $19.99/mo; most pay ≤$30/visit | All 50 states | Cigna members with drug coverage |
| Shapely | ✅ Cigna in-network | ✅ Yes | Brand-name via insurance | $49/mo + plan copays | CA, FL, NY, TX only | Insurance-billed visits |
| Ro | ❌ Cash-pay membership | ✅ Free checker + concierge | Wegovy, Zepbound + cash-pay | $45 mo 1; $145/mo after | All 50 states | Free coverage check first |
| myCigna | ✅ Official Cigna | Varies by provider | Whatever your provider prescribes | Plan copays | Wherever Cigna operates | Official plan path |
| Evernorth $200 Cap | ✅ Through enrolled employer plans | ✅ Simplified PA | Wegovy & Zepbound only | ≤$200/mo (counts toward deductible) | Employer plan-dependent | Members with EncircleRx benefit |
Sources: PlushCare (plushcare.com/weight-loss), Shapely (getshapely.com/weightloss/insurance/cigna), Ro (ro.co), Evernorth press release May 2025. All claims provider-stated; verified April 2026.
Does Cigna Actually Cover GLP-1s for Weight Loss?
Sometimes — but less often than most articles imply. Cigna has real GLP-1 coverage pathways, but whether yours is real depends on three separate questions that most people (and most websites) blur together.
We pulled Cigna's actual coverage policy documents — the ones providers use to determine approval — and translated them from insurance-speak into plain English.
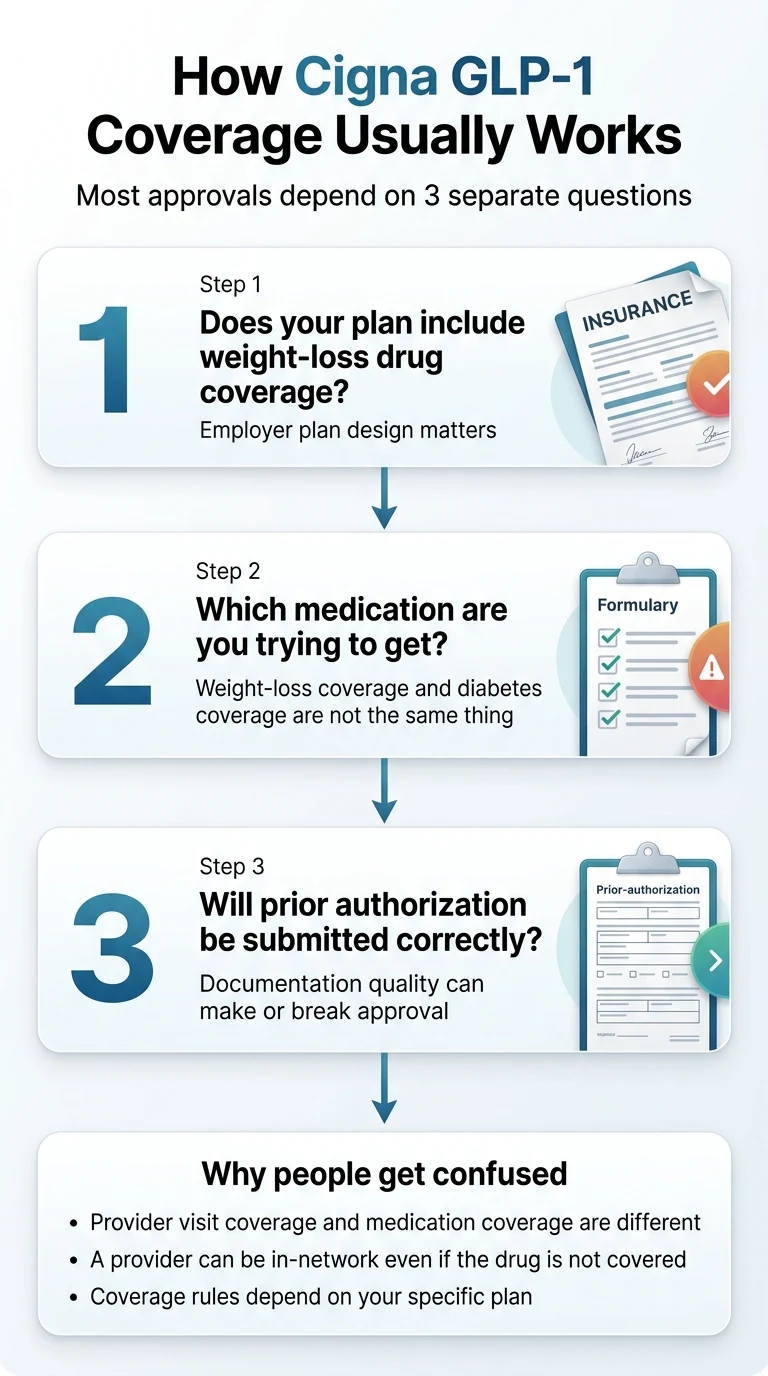
The 3 Questions You Need to Answer
Question 1: Does your Cigna plan include weight-loss drug coverage at all?
Many employer-sponsored Cigna plans specifically exclude anti-obesity medications. This isn't a prior authorization issue — it's a plan design choice your employer made. According to Reuters (September 2025), more than half of Evernorth's large-employer clients cover obesity drugs, but only about 15–20% of Cigna Healthcare's smaller-employer clients do. Your coverage depends on your employer's size, segment, and benefit design.
Question 2: If your plan does cover weight-loss drugs, which ones?
Cigna treats each medication differently based on its FDA-approved indication. The most important distinction: Ozempic and Mounjaro are diabetes drugs. Wegovy, Zepbound, and Saxenda are weight-loss drugs. If you want a GLP-1 for weight loss, you need one of the weight-loss-labeled medications — and your Cigna plan needs to cover them specifically.
| Medication | Covered for T2D? | Covered for Weight Loss? | PA Required? |
|---|---|---|---|
| Wegovy injection | ❌ Use Ozempic | ⚠️ Plan-dependent | Yes, always |
| Wegovy tablet (oral) | ❌ Use Rybelsus | ⚠️ Standard policy: yes; EncircleRx: not currently targeted | Yes, always |
| Zepbound | ❌ Use Mounjaro | ⚠️ Plan-dependent; also OSA pathway | Yes, always |
| Saxenda | ❌ | ⚠️ Plan-dependent | Yes, always |
| Ozempic | ✅ Yes, with PA | ❌ Not FDA-approved for weight loss | Yes |
| Mounjaro | ✅ Yes, with PA | ❌ Not FDA-approved for weight loss | Yes, always |
Sources: Cigna policies IP0206, IP0701, CNF-684, CNF-908, CNF-950 from static.cigna.com. Verified April 2026.
Question 3: Will someone actually submit the prior authorization?
Even when your plan covers Wegovy or Zepbound, Cigna requires prior authorization. Every time. That means your provider needs to submit documentation proving you meet specific criteria before Cigna will approve the prescription. This is where many people get stuck — their PCP either won't do it, doesn't know how, or submits incomplete paperwork. This is exactly why your choice of provider matters as much as your insurance card.
The Evernorth $200/Month Path Most Cigna Members Don't Know About
In May 2025, Cigna's health services division Evernorth launched a program that caps patient out-of-pocket costs for Wegovy and Zepbound at $200/month. Evernorth negotiated directly with Novo Nordisk and Eli Lilly to make this work. The $200 counts toward your annual deductible. PA is simplified and partially automated. Evernorth estimates patients save up to $3,600/year — and the EncircleRx program has enrolled over 11 million people.
The catch: This is a plan-sponsor benefit, not a universal Cigna member benefit. Your employer has to opt into it. To find out: call the number on your Cigna card and ask whether your plan participates in EncircleRx, or ask your HR department directly.
If You Have Cigna and Want ___, Pick This Path
Not every Cigna member needs the same thing. Some want their visits billed through insurance. Some want someone to fight the prior authorization battle. Some just want a fast yes-or-no on coverage before paying a monthly program fee.
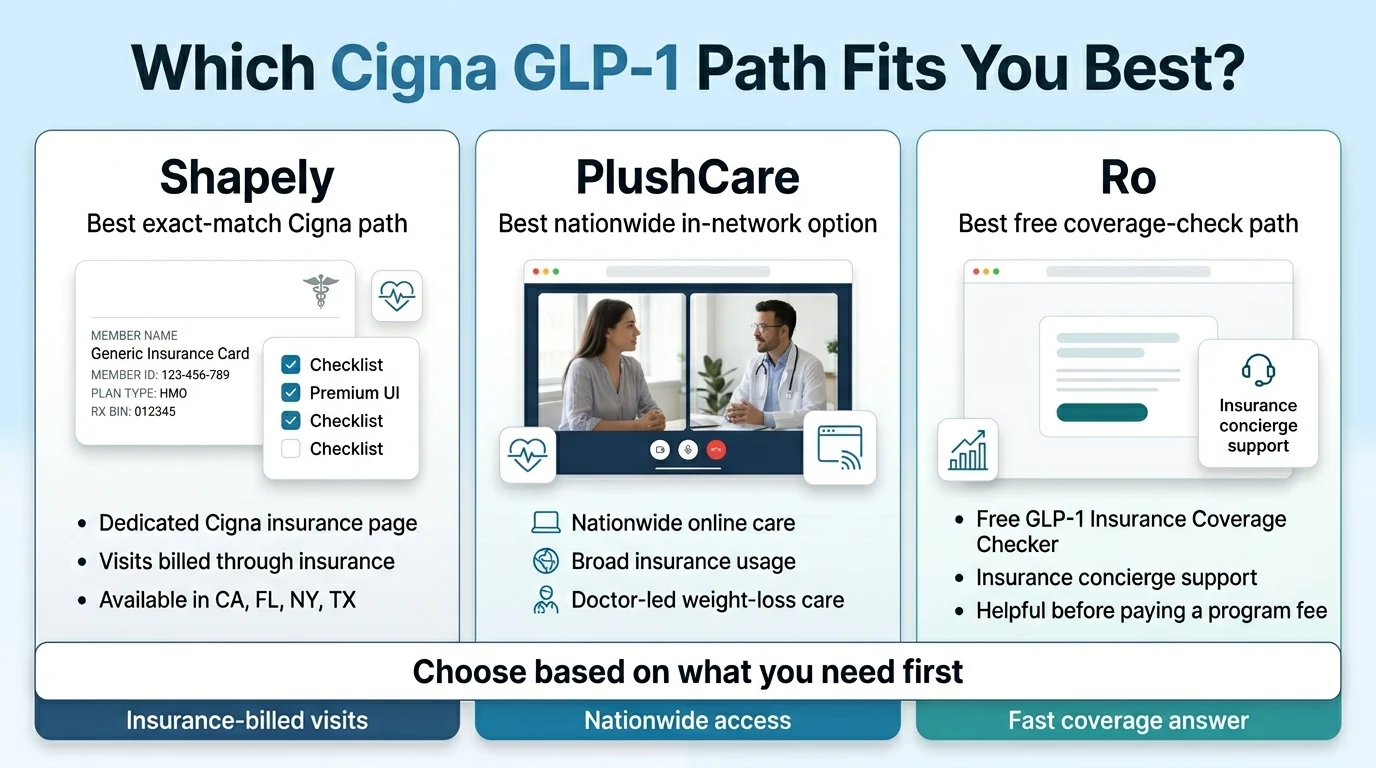
If you want visits billed directly through your Cigna plan → Shapely
CA, FL, NY, TX onlyShapely is the clearest exact-match option for Cigna members who want the full experience — visits, medication, dietitian support — billed through their insurance. It publicly states it's in-network with Cigna on its dedicated insurance page. $49/month membership fee covers app access, chat support, and care coordination. Visit copays and medication copays are billed through your Cigna plan. Their team navigates prior authorization on your behalf and includes access to a registered dietitian.
The honest limitation: Shapely currently serves adults in California, Florida, New York, and Texas only.
Check If Shapely Is Available for Your Cigna Plan →If you want a nationwide Cigna-accepting telehealth provider → PlushCare
PlushCare is the most practical Cigna option for the other 46 states — and for anyone who wants a broader healthcare relationship beyond just weight loss. It's in-network with over 100 insurance plans including Cigna. Most patients with in-network insurance pay $30 or less per visit. Their team submits prior authorization for GLP-1 medications and prescribes brand-name options including Wegovy, Zepbound, Ozempic, Mounjaro, Rybelsus, and Saxenda in all 50 states.
The honest limitation: PlushCare is a general telehealth platform, not a weight-loss-specific company. It's a doctor's appointment — a very good, very convenient one — not a structured program with coaching.
See PlushCare Cigna Pricing — All 50 States →If you want a free coverage check before paying anyone → Ro
Here's the scenario we see constantly: someone with Cigna signs up for a telehealth membership, starts the process, and discovers their plan doesn't cover GLP-1s. They've paid for a month of membership before they even know whether insurance will help.
Ro solves that problem. Their free GLP-1 Insurance Coverage Checker lets you find out whether your specific Cigna plan covers Wegovy or Zepbound — before you pay a program fee. If covered, Ro submits prior auth and your medication fills at your pharmacy copay. If denied, FDA-approved cash-pay options are available immediately — Wegovy pill from $149/month, Zepbound vials from $299/month through LillyDirect.
The honest limitation: Ro's membership is cash-pay ($45 first month, $145/month after). Your Cigna plan won't cover Ro's program fee — only the medication benefit once approved.
Check Your Cigna GLP-1 Coverage Free on Ro →If you trust the official Cigna path → start with myCigna
Before signing up for any third-party platform, check your coverage through Cigna's own tools:
- Log in to myCigna.com or the myCigna app
- Check your formulary — search for Wegovy or Zepbound
- Use “Find Care and Costs” to find in-network weight management providers
- Check virtual care options — Cigna partners with MDLIVE and others
- Ask about EnGuide Pharmacy — Cigna's specialized home delivery for Evernorth-enrolled plans
The advantage: you're using tools your insurer built for this purpose. The disadvantage: Cigna's tools explain coverage but won't advocate for you.
How Cigna Prior Authorization Works in 2026 (Decoded from Actual Policy Documents)
Prior authorization is the single biggest friction point between “my Cigna plan covers GLP-1s” and “I actually have the medication in my hands.” We read through Cigna's coverage policy documents — the ones clinicians use, not the member-facing marketing materials — and translated the approval criteria into a checklist you can actually use.

For Wegovy and Zepbound (Weight Loss in Adults) — Cigna Policy IP0206 and CNF-684
Cigna requires ALL of the following for initial approval:
- ✅BMI ≥30, OR BMI ≥27 with at least one weight-related comorbidity (hypertension, type 2 diabetes, high cholesterol, obstructive sleep apnea, heart disease, NAFLD/NASH, and others qualify)
- ✅You are NOT currently taking another GLP-1 medication or another weight-loss medication
- ✅Your provider has documented a trial of behavior modification including a reduced-calorie diet
- ✅The medication is prescribed by a licensed provider for an FDA-approved indication
EncircleRx Override Plans Have Different Thresholds
If your employer uses one of Cigna's EncircleRx benefit-exclusion-override programs, the eligibility criteria may differ from the standard policy:
- BMI ≥32 pathway (CNF-908): Lower threshold, designed for broader access
- BMI ≥35 pathway (CNF-950): Higher threshold with additional comorbidity requirements
Continuation Criteria
- Wegovy (weight loss): ≥5% baseline body weight loss required for continuation
- Zepbound (OSA): ≥10% baseline body weight loss plus stability in OSA signs and symptoms for continuation
Zepbound's Separate Obstructive Sleep Apnea Path
What Cigna Explicitly Will Not Approve
- ✗You're prescribed Ozempic or Mounjaro for weight loss (these are diabetes drugs, not approved for weight management)
- ✗You're already taking another GLP-1 or weight-loss medication simultaneously
- ✗Your BMI doesn't meet the threshold for your specific policy tier
- ✗Comorbidity documentation is missing or incomplete
- ✗The prescriber hasn't documented prior behavior modification attempts
What to Do If Cigna Denies Your GLP-1
A denial doesn't always mean no. But the right response depends entirely on why you were denied. We mapped the four most common Cigna GLP-1 denial scenarios to specific next moves.
Scenario 1: “Not medically necessary”
Usually means documentation was incomplete — missing BMI measurement, no comorbidity records, or no documented behavior modification history. The most fixable denial.
Next move: Ask your provider to submit an appeal with a formal Letter of Medical Necessity. Request a peer-to-peer review — a direct conversation between your prescribing doctor and Cigna's medical reviewer. These often succeed when written appeals don't.
Scenario 2: “Plan exclusion — weight-loss medications not covered”
This means your employer's Cigna plan specifically excludes anti-obesity drugs. A PA appeal won't fix this — the benefit doesn't exist in your plan.
Options: (A) Talk to HR — some employers are adding GLP-1 coverage. (B) Ask your doctor about the Zepbound OSA pathway if you have sleep apnea symptoms. (C) Skip the insurance fight and go cash-pay.
Scenario 3: “Step therapy required”
Cigna may require you to try a lower-cost intervention first — metformin, oral weight-loss medications, or a documented lifestyle program. Not a permanent denial; a sequence requirement.
Next move: Ask your provider to document any prior medications or programs you've already tried. Prior metformin use, Contrave, or a structured weight program may satisfy the requirement retroactively.
Scenario 4: “Continuation criteria not met”
If you've been on a GLP-1 for a year, Cigna may deny continuation if weight loss is below the policy threshold (≥5% for Wegovy weight loss; ≥10% plus OSA stability for Zepbound OSA).
Next move: Make sure your provider documents all measurable progress — weight change, A1C, blood pressure, waist circumference, CPAP data — before submitting for re-authorization.
Cash-Pay Prices If Insurance Doesn't Work Out
If your plan excludes weight-loss drugs entirely, FDA-approved brand-name GLP-1s are available at known cash-pay prices:
| Medication | Cash-Pay Price | Source |
|---|---|---|
| Wegovy pill | $149–$299/mo depending on dose | Ro / NovoCare (April 2026) |
| Wegovy injection | $349/mo (all doses after intro) | Ro / NovoCare (April 2026) |
| Zepbound vials (2.5 mg) | $299/mo | LillyDirect (Dec 2025 price cut) |
| Zepbound vials (5 mg) | $399/mo | LillyDirect |
| Zepbound vials (7.5–15 mg) | $449/mo | LillyDirect Self Pay Journey Program |
Verified April 2026. Prices can change — confirm before purchasing.
See Cash-Pay GLP-1 Options and Pricing on Ro →Which GLP-1 Medication Gives You the Cleanest Cigna Path?
Not all GLP-1s are treated equally by Cigna. The cleanest coverage path depends on your diagnosis — and a lot of people get this wrong by asking for the medication they saw on TV instead of the one their plan is most likely to approve.
Wegovy (semaglutide injection or tablet)
Cigna path: Weight loss in adults with BMI ≥30 or BMI ≥27 with comorbidities. Also CV risk reduction (BMI ≥27 + established CVD).
Cleanest route if: You meet the BMI threshold, have documented comorbidities, and your employer's plan covers weight-loss medications. Worth knowing: Cigna's standard policy does reference Wegovy tablet, but both EncircleRx override policies explicitly state that Wegovy tablet is not currently targeted in those programs.
Zepbound (tirzepatide) — Two Pathways
Cigna path: Weight loss (same as Wegovy) OR moderate-to-severe obstructive sleep apnea in adults with obesity.
Cleanest route if: You have a sleep apnea diagnosis. The OSA indication gives Zepbound a second approval pathway that Wegovy doesn't have — and in some Cigna plans that exclude weight-loss drugs, the OSA pathway may still be open. If you snore, wake up gasping, or have daytime fatigue, ask your doctor about a sleep study.
Saxenda (liraglutide)
Cigna path: Cigna's standard weight-loss policy also targets Saxenda for weight loss in adults.
It's an older GLP-1 that requires daily injections rather than weekly, with more modest clinical results than Wegovy or Zepbound. But it's a legitimate covered option in plans that include weight-loss drugs.
Ozempic & Mounjaro — Cigna: Type 2 Diabetes Only
Cigna will generally not approve these for weight loss because they're not FDA-approved for that indication. If you see a provider offering “Ozempic for weight loss through insurance,” be cautious — Cigna's policy explicitly doesn't cover off-label use. If you don't have type 2 diabetes, Wegovy contains the same active ingredient as Ozempic with the correct FDA weight-loss label.
7 Things to Verify Before You Sign Up for Any Provider
This checklist exists because “accepts Cigna” means at least three different things depending on who's saying it. We built this from the specific friction points we've seen trip up Cigna members.
Does the provider bill Cigna for visits, or only help with the medication?
Shapely and PlushCare bill Cigna directly for your provider visits — your visit copay goes through your plan like any other doctor's appointment. Ro charges you directly for the membership and visits — they help navigate Cigna for the medication prescription, but the program fee is out-of-pocket. Both models work, but know which you're signing up for.
Is your specific medication actually on your plan's drug formulary?
A provider being in-network with Cigna means your visits may be covered. Whether your medication is covered is a completely separate question answered by your plan's drug formulary. Check on myCigna.com under prescription benefit details, or call the number on your Cigna card.
Will the provider actually submit prior authorization, or just hand you a form?
"We help with insurance" can mean full PA submission and follow-up — or it can mean they give you a prescription and wish you luck. PlushCare, Shapely, and Ro all submit PA documentation directly. Confirm this explicitly before signing up with any other provider.
Which pharmacy or PBM is handling your prescription?
Many Cigna plans use Express Scripts as their pharmacy benefit manager. If your plan is enrolled in Evernorth's programs, you may have access to EnGuide Pharmacy for specialized GLP-1 dispensing with 24/7 clinical support.
Has your employer excluded anti-obesity medications from the plan?
This is the question that renders everything else irrelevant if the answer is yes. In February 2026, a federal appeals court upheld Cigna's right to exclude weight-loss drugs from employer plans. No provider can fix this — only your employer can change it at the next benefit design cycle.
Is the provider available in your state?
Shapely: CA, FL, NY, TX only. PlushCare: all 50 states. Ro: all 50 states. Confirm before you start a registration process.
What's the real monthly cost after introductory pricing?
Some providers offer first-month discounts. PlushCare: $19.99/month membership + visit copay (consistent). Shapely: $49/month + plan copays (consistent). Ro: $45 month 1, then $145/month for membership — medication billed separately.
| Provider | Month 1 | Month 2+ | Medication Included? |
|---|---|---|---|
| PlushCare (with insurance) | $19.99 + visit copay | $19.99 + visit copay | No — at pharmacy copay |
| Shapely (with insurance) | $49 + plan copays | $49 + plan copays | No — at pharmacy copay |
| Ro (cash-pay membership) | $45 + medication | $145 + medication | Separate — Wegovy pill from $149/mo |
Prices from official provider pages, verified April 2026. Your medication copay depends entirely on your Cigna plan's drug benefit.
Not sure which path is right for your situation?
Answer a few questions about your Cigna plan, state, and diagnosis — get a personalized recommendation in 60 seconds.
Find My Cigna GLP-1 Path — Free →The Cigna GLP-1 Coverage Path Finder
Instead of reading through Cigna's 25-page policy documents, use this simplified logic to find your exact next step:
✅ Yes, my plan covers weight-loss medications
Start with PlushCare (all states) or Shapely (CA/FL/NY/TX) for in-network visits + PA help.
⚠️ No / I'm not sure if my plan covers GLP-1s
Use Ro's free GLP-1 Insurance Coverage Checker first. Takes 2 minutes, no cost. Then decide your provider based on the result.
❌ My plan excludes weight-loss drugs
Three options: (1) Ask your doctor about the Zepbound OSA pathway if you have sleep apnea symptoms. (2) Ask HR whether your employer is adding coverage next cycle. (3) Go cash-pay through Ro or LillyDirect/NovoCare for FDA-approved brand-name medications at transparent pricing.
📋 I was already denied
Read the denial letter. If documentation-related, appeal with stronger medical necessity evidence through your provider. If plan exclusion, cash-pay is likely your fastest path.
How We Verified This Page
Cigna coverage policies verified from static.cigna.com:
- • IP0206: Weight Loss – GLP-1 Agonists (the main weight-loss coverage policy)
- • IP0701: Diabetes – GLP-1 Agonists
- • CNF-684: Weight Loss GLP-1 Agonists Prior Authorization
- • CNF-908: Weight Loss GLP-1 Agonists Benefit Exclusion Override (EncircleRx, BMI ≥32)
- • CNF-950: Weight Loss GLP-1 Agonists Benefit Exclusion Override (EncircleRx, BMI ≥35)
What you should confirm yourself:
- • Whether your specific employer plan covers weight-loss GLP-1 medications (call the number on your Cigna card)
- • Whether your employer participates in EncircleRx (ask HR)
- • Whether a specific provider is in-network with your specific Cigna plan (confirm during enrollment)
We will re-verify every element of this page by July 2026. If you notice something that's changed, let us know.
Frequently Asked Questions
Does Cigna cover Wegovy for weight loss?↓
Does Cigna cover Zepbound?↓
Which online GLP-1 provider actually accepts Cigna?↓
Does Ro accept Cigna insurance?↓
Does Cigna cover Ozempic for weight loss?↓
Can Zepbound be covered through Cigna for sleep apnea?↓
What if my employer's Cigna plan excludes weight-loss drugs?↓
What is the Evernorth $200/month GLP-1 cap?↓
What documents help a Cigna prior authorization get approved?↓
Still not sure which GLP-1 program is right for you?
Check your Cigna coverage free — 2 minutes, no commitment, know your answer before you pay anyone.
Or: Check if Shapely accepts your Cigna plan (CA, FL, NY, TX)
Related Guides
The RX Index is an independent comparison resource for GLP-1 telehealth providers. Some links on this page are affiliate links — we may earn a commission if you start a program through our links, at no extra cost to you. This never influences our rankings or recommendations. Provider claims verified from official pages in April 2026. Cigna coverage policy documents (IP0206, IP0701, CNF-684, CNF-908, CNF-950) verified from static.cigna.com. This content is for informational purposes only and does not constitute medical advice. Your coverage depends on your specific employer plan — verify directly with Cigna before enrolling.
Last verified: · Next scheduled review: July 2026