By The RX Index Editorial Team · Medically reviewed by Dr. Jennifer Brown, MD · 9 providers and pharmacy programs verified
Last verified: · Kaiser NW criteria PDF (rev. 12/11/25), FEHB/PSHB brochure 2026, and regional PA forms verified
Editorial Standards · Affiliate Disclosure · Next audit: July 2026
GLP-1 PROVIDERS THAT ACCEPT KAISER — 2026 VERIFIED GUIDE
GLP-1 Providers That Accept Kaiser: What Actually Works in 2026
If you're searching for GLP-1 providers that accept Kaiser, here's the honest answer most pages won't give you: almost no telehealth GLP-1 provider directly bills Kaiser Permanente. Kaiser is a closed HMO system — your doctors, pharmacy, and insurer are all the same entity — which means outside providers can't simply “accept Kaiser” the way they accept Aetna or UnitedHealthcare.
But that does not mean you're stuck.
We reviewed Kaiser's official formulary documents across all 8 regions, verified pricing on 9 providers and pharmacy programs, and mapped every real path a Kaiser member has to GLP-1 treatment in 2026. The result is the RX Index Kaiser GLP-1 Compatibility Matrix — built from official Kaiser formulary pages, regional criteria PDFs, federal-plan brochures, and provider pricing pages.
Bottom line for most Kaiser members: If Kaiser has already denied you or you don't want to wait months for their step-therapy process, you have affordable cash-pay options that require zero Kaiser involvement. MEDVi offers compounded semaglutide starting at $179/month with no prior authorization and no membership fees. If you want FDA-approved medication specifically, Ro offers Wegovy starting at $149/month — and their free GLP-1 Insurance Coverage Checker will tell you whether Kaiser might pay first before you spend anything.

Disclosure: Some links on this page are affiliate links. If you purchase through these links, we may earn a commission at no extra cost to you.
The 3 Real Kaiser-Compatible GLP-1 Paths (At a Glance)
Every Kaiser member's situation falls into one of three lanes. This table gives you the 10-second version.
| Path 1: Inside Kaiser | Path 2: Insurance-First Outside Provider | Path 3: Cash-Pay (No Kaiser Needed) | |
|---|---|---|---|
| How it works | Kaiser PCP prescribes through Kaiser pharmacy | Outside provider helps navigate Kaiser coverage or prescribes independently | Provider prescribes and ships directly — Kaiser is not involved |
| Timeline | Months (step therapy + PA) | 1–3 weeks (coverage check + enrollment) | 3–7 days |
| Monthly cost | Plan copay or 50% coinsurance (FEHB/PSHB) | Membership + copay or cash-pay | $149–$349/month all-in |
| Prior auth required? | Yes — strict criteria | Provider may help submit PA | No |
| Best for | FEHB/PSHB, weight-loss drug rider, or Type 2 diabetes | Members who want to test Kaiser coverage before paying cash | Members who want to start now and skip the insurance process |
| Start here | Call Kaiser Member Services | Free coverage check on Ro → | Check MEDVi eligibility → |
Sources: Kaiser formulary documents (NW, FEHB/PSHB), provider pricing pages. Verified April 2026.
Which Kaiser Path Fits Your Situation?
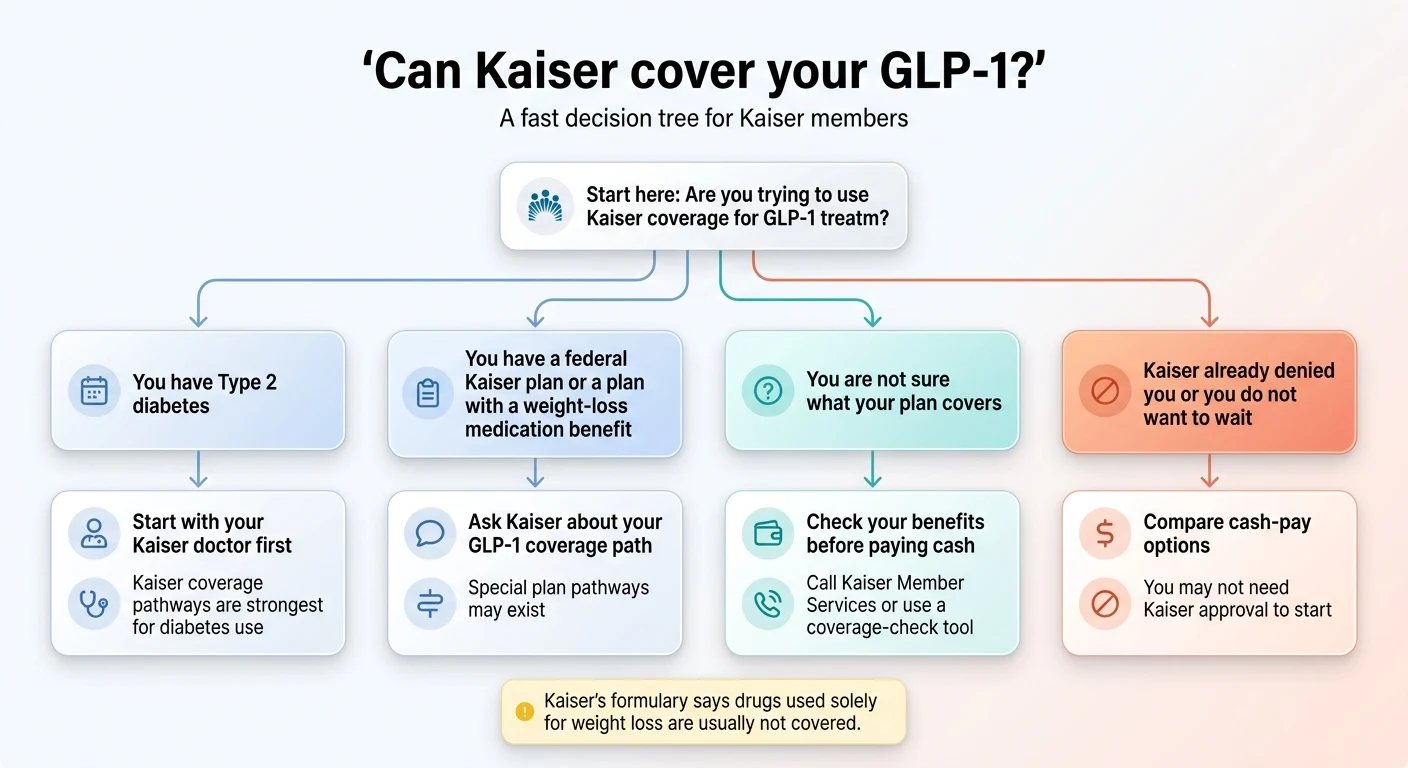
🩺 You have Type 2 diabetes
Good news. Kaiser's formulary covers Ozempic (semaglutide) for diabetes management with prior authorization in most regions. Start with your Kaiser PCP — you have the strongest coverage pathway. If they prescribe Ozempic for diabetes, Kaiser pharmacy can fill it at your formulary copay.
💼 Your employer purchased Kaiser's optional weight-loss drug rider
You may have GLP-1 coverage that most Kaiser members don't. Ask your HR department whether your group plan includes the weight-loss medication benefit. If it does, your Kaiser PCP can initiate the prior authorization process for Wegovy or Zepbound.
🏛️ You have a federal plan (FEHB or PSHB) through Kaiser
Kaiser's 2026 FEHB/PSHB documents confirm GLP-1 coverage lanes exist for federal and postal employees, with 50% coinsurance of the plan allowance after prior authorization and weight management program participation.
📋 You're in California and Kaiser won't prescribe a GLP-1 for weight loss
Starting January 1, 2025, Kaiser's official business communications confirm that anti-obesity medications are no longer covered under base plans when prescribed solely for the purpose of weight loss. Disease-management uses (such as for diabetes) remain covered. If your plan doesn't include the employer-purchased weight-loss drug rider, your fastest path is cash-pay.
⚡ Kaiser already denied you, or you don't want to wait
Skip to cash-pay providers. You can start treatment within days for $149–$179/month.
❓ You're not sure what your plan covers
Start with Ro's free GLP-1 Insurance Coverage Checker. Ro contacts your insurer, checks your specific benefits, and sends you a personalized coverage report — before you spend a dollar.
Best first move if you want to know whether Kaiser will pay
Ro's free GLP-1 Insurance Coverage Checker contacts Kaiser on your behalf and sends you a personalized report. Free personalized report. No prescription required to run the check.
Check Your GLP-1 Coverage on Ro — Free →Can Kaiser Cover Wegovy, Ozempic, or Zepbound?
Yes — but only in specific, narrow lanes that most Kaiser members don't qualify for. Kaiser's general drug formulary states that medications used solely for weight loss are “usually not covered.” That single sentence is why Kaiser is one of the hardest insurers for GLP-1 access.
The RX Index Kaiser GLP-1 Regional Coverage Matrix
Built from Kaiser's own formulary PDFs, regional criteria documents, FEHB/PSHB brochures, and broker communications. Verified April 2026.
| Kaiser Region | Wegovy (Weight Loss) | Ozempic (Diabetes) | Zepbound (Weight Loss) | Key Requirement | Confidence |
|---|---|---|---|---|---|
| California (SoCal + NorCal) | Not covered base plans (Jan 2025) | ✅ Covered T2D with PA | Not on standard formulary | Employer must purchase weight-loss rider | Verified |
| Northwest (OR/WA) | ⚠️ Covered with strict step therapy | ✅ Covered T2D, Tier 3 | ⚠️ Only after 6-mo semaglutide trial + 2 failed meds | Most documented criteria publicly available | Verified |
| Mid-Atlantic (MD/VA/DC) | Varies; PA form exists for Kaiser and/or participating providers | ✅ Covered T2D with PA | Listed on PA form | Participating-provider pathway documented | Verified |
| Colorado / Georgia / Hawaii | Plan-specific | ✅ Covered T2D | Plan-specific | Contact Member Services | Not independently verified |
| FEHB/PSHB (All Regions) | ⚠️ Coverage lanes exist; 50% coinsurance | ✅ Covered T2D | ⚠️ Coverage lanes exist with step therapy | Weight management program + PA + monthly exams | Verified |
Sources: Kaiser NW formulary criteria PDF (revised 12/11/25, effective 02/05/26), Kaiser FEHB/PSHB weight management requirements (2026), Kaiser Mid-Atlantic HMO Exchange PA form, Kaiser CA business communications (2024). Verified April 2026.
What Kaiser Requires Before They'll Approve a GLP-1
Even when Kaiser plans do cover GLP-1 medications, approval is not fast or easy. Based on Kaiser's Northwest criteria document (the most detailed publicly available) and FEHB/PSHB materials, here is the typical step-therapy sequence:
Enroll in Kaiser's weight management program
This includes nutritional counseling, lifestyle coaching, and behavioral health support. Participation is mandatory before GLP-1 medications are even discussed.
Trial of older, less expensive weight-loss medications
Kaiser typically requires documented failure of or intolerance to at least 2 prior weight-loss medications — commonly phentermine, diethylpropion, Qsymia, or Contrave.
Documentation of BMI and comorbidities
Kaiser Northwest requires BMI ≥30 (or ≥27 with hypertension, diabetes, or hyperlipidemia) plus documented failure of the medications above.
For Zepbound specifically — a 6-month semaglutide trial first
Kaiser Northwest requires patients to have tried semaglutide (Wegovy or Ozempic) for at least 6 months before Zepbound will even be considered.
Prior authorization submission
Your Kaiser PCP submits extensive paperwork justifying medical necessity.
If approved — ongoing monitoring
FEHB/PSHB materials document monthly (every 4 weeks) in-office exams after treatment starts, including weight monitoring.
Why Kaiser Is Different From Every Other Insurance Search
This is the section that explains why “GLP-1 providers that accept Kaiser” is fundamentally a different question than “GLP-1 providers that accept Blue Cross.”
Kaiser Permanente is not just an insurance company. It is an integrated health system where your insurer, your doctor, and your pharmacy are all the same organization. In most Kaiser markets, your PCP works for Kaiser, your prescriptions are filled at Kaiser pharmacies, and outside providers cannot bill into the system the way they can with a PPO network.
1. Your doctor has less prescribing flexibility
Because Kaiser doctors follow internal protocols tied to the insurer's formulary, getting an “off-formulary” medication is harder than with an independent doctor billing a separate insurance company.
2. Outside prescriptions don't automatically transfer with coverage
Kaiser does allow prescription transfers — their pharmacy management page confirms members can request transfers online — but transferring a prescription into Kaiser does not guarantee the medication will be covered. It only means the pharmacy can technically fill it. You'd still need to meet formulary and PA requirements.
3. “Accepts insurance” almost never means “accepts Kaiser”
When providers like Ro, Hims, or PlushCare say they “accept insurance,” they typically mean commercial PPO and HMO plans from major carriers. Kaiser's closed model falls outside that standard integration. Searching for a GLP-1 provider that “accepts Kaiser” in the traditional sense leads to directory pages that don't solve your actual problem.
Looking for GLP-1 providers that work with other insurers? See our complete guide: Best GLP-1 Providers That Accept Insurance (2026) →
Can an Outside Doctor or Telehealth Provider Work With Kaiser at All?
Sometimes, yes — but the mechanics are more limited than with other insurers. We found three documented pathways:
1. Participating-provider pathway (Mid-Atlantic)
Kaiser Mid-Atlantic's prior authorization form for weight management agents (Wegovy, Saxenda, Zepbound) is explicitly designed for use by “Kaiser Permanente and/or participating providers.” This proves that in at least one region, an outside provider with a participating relationship can submit prior authorization through Kaiser's system.
2. Prescription transfer
Kaiser's pharmacy management page confirms that existing members can request prescription transfers into Kaiser pharmacies. However, transfer does not guarantee the medication will be covered — coverage still depends on your formulary and PA requirements.
3. Insurance concierge services from outside providers
Providers like Ro offer to contact your insurance company, check your benefits, and handle prior authorization on your behalf. This is not “accepting Kaiser” — it's helping you understand what Kaiser will and won't cover so you can make an informed decision before paying anyone.
7 Questions to Ask Kaiser Before You Enroll Anywhere
Before you spend a dollar on any outside provider, call Kaiser Member Services or check your Evidence of Coverage document and confirm:
Does my specific plan include a weight-loss medication benefit?
Are Wegovy, Ozempic, or Zepbound on my plan's formulary — and at what tier?
What prior authorization requirements apply?
How many prior medications do I need to have tried first?
Can a participating or community provider submit a PA request for me?
Can I transfer an outside prescription into Kaiser pharmacy?
If I pay cash for medication through an outside provider, will any of it count toward my out-of-pocket maximum?
Which Outside Provider Is Best If You Want Kaiser to Pay If Possible?
If you haven't given up on getting Kaiser to cover your GLP-1, Ro is the best first click for the insurance-navigation path. Not because Ro directly bills Kaiser, but because Ro offers a free GLP-1 Insurance Coverage Checker that does the legwork most Kaiser members don't know how to do themselves.
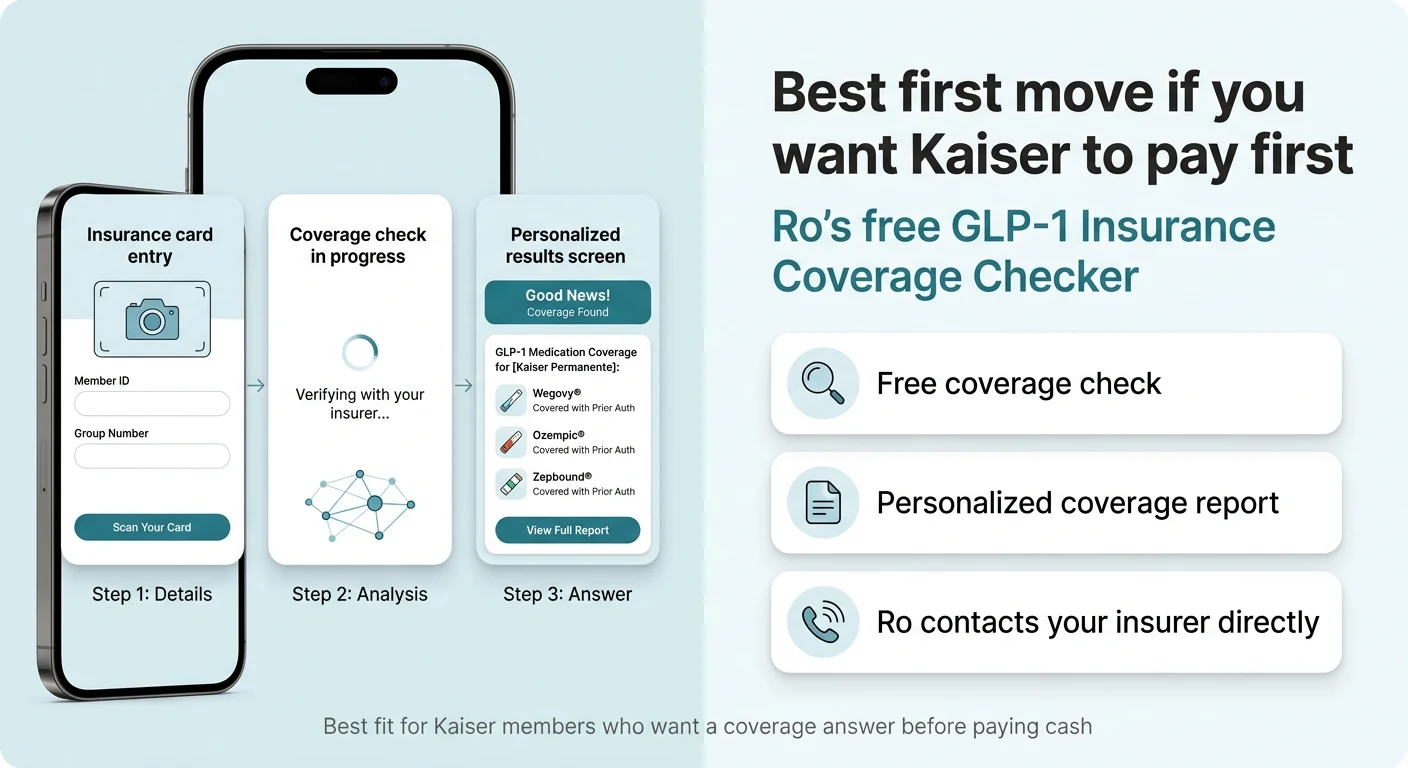
Here's what Ro's insurance-first path looks like:
- 1Fill out a form with your insurance information
- 2Ro contacts your insurer directly and checks your specific benefits
- 3You get a free, personalized coverage report telling you what's covered and what's not
- 4If coverage exists, Ro's insurance concierge handles prior authorization paperwork
- 5If coverage doesn't exist, you can switch to Ro's cash-pay medication options
Ro pricing (verified April 2026):
- • Ro Body membership: $45 first month, then $145/month ongoing
- • Wegovy pill (FDA-approved): $149–$299/month depending on dose
- • Wegovy injection (FDA-approved): $199/month intro (first 2 fills through June 30, 2026), then $349/month
- • Insurance concierge: included in membership
- • HSA/FSA at checkout: No (but you may submit for reimbursement through your plan)
GLP-1 Providers That May Work With Kaiser for In-Network-Style Care
If what you want is a clinical weight-loss program where a doctor manages your care and insurance might help cover it, two providers are worth verifying for Kaiser compatibility before you enroll. We did not find direct public Kaiser-acceptance statements from either provider — you'll need to verify directly before enrolling.
Form Health
Form Health says it is in-network with national plans including Medicare, bills visits, labs, and medications through insurance in many cases, and can submit prior authorization paperwork. Prescribes only FDA-approved weight-loss medications. Self-pay is $299/month if insurance doesn't cover the program.
What to ask Form before enrolling: “Can you bill my Kaiser plan, or would I need to pay the self-pay rate?”
Verify Coverage With Form Health →PlushCare
PlushCare says its weight-loss program is available with or without insurance, that insurance is accepted, and that most in-network patients pay $30 or less for visits. Without insurance, initial visits are $129. PlushCare offers PCP-style care with local pharmacy fill options.
What to ask PlushCare before enrolling: “Is my Kaiser HMO plan in your network for weight-loss visits?”
Check PlushCare Network Fit →Which Providers Are NOT a Real Kaiser Solution?
This section saves you time and money by being direct about what doesn't work.
WeightWatchers Clinic: Explicit Kaiser Exclusion
WeightWatchers' GLP-1 program page states clearly that its insurance coordinators only work with commercial plans — and that members on a Kaiser plan must either pay out of pocket for a GLP-1 or choose a non-GLP-1 included medication option. If you've been considering WeightWatchers for your Kaiser GLP-1 access, this is a dead end.
LifeMD: Does Not Accept Insurance for GLP-1 Programs
LifeMD's support center states it does not accept insurance for its weight-loss programs. This makes it a weaker fit than providers that offer insurance navigation tools.
Sesame: Cash-Pay Program, Partial Insurance Help
Sesame's weight-loss program itself is not billed to health insurance. Sesame providers can help with prior authorization paperwork for prescribed medications, so there's a partial insurance play at the medication layer — but it's not what most people mean when they search for a provider that “accepts Kaiser.”
What If Kaiser Says No and You Need a Cash-Pay Backup?
This is where most Kaiser members end up — and honestly, it's where the path gets simpler and faster. Once you know Kaiser won't cover your GLP-1, the decision changes from “how do I get insurance to pay” to “which cash-pay provider gives me the best combination of price, support, and transparency.”

The RX Index Kaiser Cash-Pay Alternative Comparison
| Provider | Medication | Month 1 | Ongoing | HSA/FSA? | Insurance Help? |
|---|---|---|---|---|---|
| MEDVi | Compounded semaglutide | $179 | $299/mo | ✅ Yes | No |
| Eden | Compounded semaglutide | $149 | $249/mo (month-to-month) | ✅ Yes | No |
| Ro (FDA-approved) | Wegovy pill | $149 + $45 membership | $299/mo + $145 membership | No checkout; may reimburse | ✅ Free checker + concierge |
| NovoCare Pharmacy | FDA-approved Wegovy pill | $149 (need Rx) | $199–$299/mo | Varies by pharmacy | N/A — pharmacy only |
| LillyDirect | FDA-approved Zepbound | $299 (2.5mg, need Rx) | $399 (5mg); $449 (7.5mg+) | Varies | N/A — need Rx |
All pricing verified from official provider and manufacturer websites, April 2026. Prices can change — always confirm at checkout. NovoCare and LillyDirect require an existing prescription. Compounded medications are not FDA-approved as finished products.
MEDVi: Our Top Pick for Kaiser Members Going Cash-Pay
For most Kaiser members who need to bypass insurance entirely, MEDVi offers the strongest combination of entry price, included services, and simplicity.
What $299/month includes (after $179 first month):
- ✓Compounded semaglutide or tirzepatide, shipped in temperature-controlled packaging
- ✓Licensed physician evaluation through a U.S. provider network
- ✓Personalized treatment plan with titration schedule and dosing guidance
- ✓24/7 unlimited provider messaging
- ✓Anti-nausea medication if needed — no extra cost
- ✓Dose adjustments at no extra charge (many competitors charge $50–$100 per dose increase)
- ✓Free standard shipping with cold packs
- ✓$0 membership fee — the price you see is the total price
“Medvi was not my first choice but is my last. The first two programs I tried turned me down and their pricing was just too steep. Medvi accepted me into the program for semaglutide and I got on board approximately 31 pounds ago.” — ConsumerAffairs review
Eden: Lower Ongoing Price, Flat-Rate Dosing
Eden is the strongest alternative for Kaiser members whose primary filter is lowest ongoing monthly cost.
Eden pricing (verified April 2026):
- • Compounded semaglutide injection: $149 first month, $249/month ongoing (month-to-month)
- • Compounded tirzepatide: $249 first month, $329/month ongoing
- • $0 membership fee, free shipping included
- • Same price at every dose — cost doesn't increase when dosage is adjusted upward
- • Also offers brand-name Wegovy, Ozempic, Zepbound, and Mounjaro at brand-name pricing
- ✓Available in all 50 states
- ✓Members self-reported average weight loss of 29.3 lbs in the first 6 months
- ✓24/7 provider messaging, meal plans, workout guides, and community support included
- ✓Uses PCAB-accredited partner pharmacies
- ✓Same-day provider review of your health questionnaire
- ✓HSA/FSA cards accepted at checkout
Eden's $249 ongoing price is $50/month lower than MEDVi's $299. Over a year, that's $600 in savings. Eden also offers the widest medication selection — compounded and brand-name, injectable and oral.
See Eden's Current Pricing — $149 First Month →Compounded vs. FDA-Approved GLP-1s: What Kaiser Members Should Know
FDA-Approved (Wegovy, Zepbound)
- • Manufactured by Novo Nordisk or Eli Lilly
- • Completed rigorous clinical trials
- • FDA-approved for specific indications
- • STEP 1 trial: avg 14.9% body weight loss over 68 weeks
- • Cash-pay: $149–$349/month (manufacturer programs)
Compounded (MEDVi, Eden)
- • Prepared by licensed U.S. compounding pharmacies
- • Under Section 503A of the FD&C Act
- • NOT FDA-approved as finished products
- • FDA has raised concerns about quality in some compounded products
- • Cash-pay: $149–$299/month
Can You Use Your Kaiser HSA or FSA for Cash-Pay GLP-1 Providers?
In many cases, yes. GLP-1 medications prescribed by a licensed physician to treat a specific diagnosed condition are generally eligible HSA and FSA expenses under IRS rules.
| Provider | Accepts HSA/FSA at Checkout? | Source |
|---|---|---|
| MEDVi | ✅ Yes | MEDVi website |
| Eden | ✅ Yes | Eden website |
| Ro | No at checkout — may submit for reimbursement separately | Ro pricing FAQ |
At a 24% federal tax rate, $299/month becomes roughly $227/month in after-tax terms when using HSA/FSA funds. Confirm eligibility with your plan administrator.
How to Appeal a Kaiser GLP-1 Denial (And When It's Not Worth It)
If Kaiser denies your GLP-1 request, you have appeal rights — but whether it's worth exercising them depends on your state and situation.
When to appeal
- • You're in California (strongest external review)
- • You have Type 2 diabetes, cardiovascular disease, or sleep apnea
- • You've documented compliance with Kaiser's weight management program and prior medication trials
When to skip the appeal and go cash-pay
- • Your plan explicitly excludes weight-loss medications (a benefits design decision, not medical necessity)
- • You're outside California
- • You've been in step therapy for months and don't want to wait longer
What Should You Do Before You Spend Money on the Wrong Provider?
Complete these steps before paying any provider — it takes about 30 minutes and can save you months of frustration.
Confirm your exact Kaiser plan and region
Log into your Kaiser member portal or find your Evidence of Coverage (EOC) document. Your region and plan type determine everything.
Ask if you have a weight-loss drug benefit
Call Kaiser Member Services or check your EOC. The weight-loss medication rider is an add-on that your employer chooses to purchase (or not). Many members don't know whether their employer opted in.
Check formulary status
Ask whether Wegovy, Ozempic, or Zepbound are formulary, nonformulary, or exception-only for your specific plan.
Ask about outside/participating provider options
In some regions (confirmed in Mid-Atlantic), participating providers can submit PA requests through Kaiser's system. Ask if this applies to your market.
Gather your documentation
If you plan to pursue Kaiser coverage: documented BMI and weight history, comorbidities list, records of prior weight-loss medication trials, and proof of weight management program participation.
Decide your priority — coverage or speed
If you're willing to invest months pursuing Kaiser coverage and have reasonable odds of approval, the inside-Kaiser path can save you money long-term. If you want to start treatment now, the cash-pay path gets you there within days.
Choose your lane and commit
- Kaiser coverage lane: Start with your Kaiser PCP or Ro's free coverage checker
- FDA-approved cash-pay: Ro's Wegovy program or NovoCare Pharmacy
- Compounded cash-pay: MEDVi ($179 first month) or Eden ($149 first month)
Want a personalized recommendation?
Answer a few questions about your Kaiser plan, state, and diagnosis — get a personalized recommendation in 60 seconds.
Find My Kaiser GLP-1 Path — Free →How We Verified This Comparison
Sources verified directly from official pages:
- • Kaiser NW Wegovy/Ozempic criteria PDF (revised 12/11/25, effective 02/05/26)
- • Kaiser FEHB and PSHB weight management program and GLP-1 requirements brochure (2026)
- • Kaiser Mid-Atlantic HMO Exchange prior authorization form for weight management agents
- • Kaiser general drug formulary (“How the Formulary Works” page)
- • Kaiser business communications — GLP-1/AOM coverage changes flyer (2024)
- • California DMHC FAQ (IMR overturn statistics)
- • MEDVi, Eden, Ro, PlushCare, Form Health official pricing pages
- • WeightWatchers GLP-1 program page (Kaiser exclusion language); LifeMD support center
- • NovoCare/Novo Nordisk Wegovy pricing; LillyDirect Zepbound savings page
What we could NOT verify directly:
- • Whether any specific outside telehealth provider has a direct billing relationship with Kaiser — no provider publicly markets Kaiser acceptance
- • Region-specific GLP-1 criteria for Colorado, Georgia, and Hawaii — no public criteria documents found
We refresh pricing and insurance FAQ monthly; Kaiser formulary and regional criteria quarterly; Kaiser coverage policy changes at each plan-year change (typically January).
Frequently Asked Questions
Does Kaiser cover Wegovy for weight loss?↓
Does Kaiser cover Ozempic for weight loss?↓
Does Kaiser cover Zepbound?↓
Can I use Ro with Kaiser?↓
Can an outside doctor send my GLP-1 prescription to Kaiser pharmacy?↓
Does WeightWatchers work with Kaiser?↓
What should I do if Kaiser denies my GLP-1?↓
Are MEDVi and Eden prescribing compounded GLP-1 medications?↓
Can I use my HSA or FSA to pay for MEDVi or Eden?↓
How much does a GLP-1 cost if Kaiser won't cover it?↓
Still not sure which GLP-1 program is right for you?
Know your options before you pay anyone — coverage check is free.
Related Guides
The RX Index is an independent comparison resource for GLP-1 telehealth providers. Some links on this page are affiliate links — we may earn a commission if you start a program through our links, at no extra cost to you. This never influences our rankings or recommendations. Provider claims verified from official pages in April 2026. Kaiser formulary information verified from Kaiser NW criteria PDF (revised 12/11/25), Kaiser FEHB/PSHB brochure (2026), and Kaiser Mid-Atlantic HMO Exchange PA form. This content is for informational purposes only and does not constitute medical advice. Compounded GLP-1 medications have not been reviewed or approved by the FDA for safety, effectiveness, or quality. Your coverage depends on your specific Kaiser plan and region — verify directly with Kaiser Member Services before enrolling.
Last verified: · Next scheduled review: July 2026