How to Switch From Compounded Semaglutide to Ozempic (Without Losing Progress or Going Broke)
By The RX Index Editorial Team · Last verified: April 1, 2026
Yes — you can switch from compounded semaglutide to Ozempic. But don't try to convert your syringe units to pen doses on your own. There is no validated universal conversion chart, and compounded concentrations vary too much for a safe 1:1 swap.
Here's what actually matters: Your clinician will review your current regimen and choose the right Ozempic starting point — typically the labeled initiation of 0.25 mg weekly for 4 weeks, then 0.5 mg, individualized from there based on your history and tolerance. And Ozempic does not have to cost $1,000+. Its list price is $1,027.51, but through the NovoCare self-pay program, new patients start at $199/month for the first two fills (through June 30, 2026) — or as low as $25/month with commercial insurance and the Novo Nordisk savings card.
If you're using semaglutide primarily for weight loss and don't have type 2 diabetes, Wegovy might be the better FDA-labeled fit — we cover that distinction below.
This page covers the safe switching process, what dose to expect, real 2026 costs across every pathway, what to bring to your appointment, what to watch for in the first month, and what to do if you can't afford brand-name pricing. Every price and fact verified against primary sources in April 2026.
At a Glance: The Key Facts
| Question | Answer |
|---|---|
| Can you switch? | Yes, with a new prescription and clinician guidance |
| Is there a 1:1 conversion chart? | No validated universal chart exists |
| Ozempic labeled start dose? | 0.25 mg weekly × 4 weeks, then 0.5 mg |
| Best if… | You have type 2 diabetes, want the branded pen, or need insurance-backed access |
| Ask about Wegovy if… | Your primary goal is weight loss only |
| Current self-pay pricing | $199/mo intro for first 2 fills (0.25/0.5 mg through 6/30/26), then $349/mo (0.25–1 mg) or $499/mo (2 mg) |

Your Ozempic Cost Pathways at a Glance
The question keeping people up at night. Here's what you'd actually pay — not the sticker price.
| Pathway | Monthly Cost |
|---|---|
| Commercial insurance + Novo Nordisk savings card | As low as $25/mo |
| NovoCare self-pay (intro pricing) | $199/mo for first 2 fills |
| NovoCare self-pay (ongoing) | $349/mo (0.25–1 mg) / $499/mo (2 mg) |
| Ro (clinician + insurance support) | $45 first month, then $145/mo membership; medication cost separate |
| Novo Nordisk Patient Assistance | $0 (with eligibility) |
Prices verified against NovoCare.com, Ozempic.com, and Ro.co as of April 2026.
Why You're Probably Reading This Right Now
We know why you're here. Your compounding pharmacy stopped filling your prescription, or they're about to. Maybe your telehealth provider sent a transition email. Maybe you saw a headline about the FDA enforcement and thought now what?
You found something that was working. The weight was coming off. Your blood sugar was stabilizing. And now it feels like someone pulled the rug. You're not overreacting.
Here's what happened: On February 21, 2025, the FDA determined the semaglutide injection shortage was resolved. FDA's enforcement-discretion periods ran until April 22, 2025 for 503A compounders and May 22, 2025 for 503B outsourcing facilities. Compounded semaglutide is now only legally available in very narrow circumstances.
The good news: the transition to brand-name Ozempic is medically straightforward, and it does not have to cost a fortune.
This guide addresses three fears:
1. “Will I lose my progress?” — Continuity of treatment matters, and a seamless switch with proper guidance helps maintain your trajectory.
2. “Can I afford this?” — Multiple pathways exist well under $500/month, and the Patient Assistance Program provides Ozempic at no cost for qualifying patients.
3. “Will I get sick again?” — Some GI adjustment is possible during re-titration, but it's typically transient and manageable.
Can You Switch From Compounded Semaglutide to Ozempic?
Yes. People switch from compounded semaglutide products to Ozempic routinely. But the switch should be treated as a new, documented medication plan — not a self-directed swap.
This matters in 2026. The FDA has sharpened its language around compounded GLP-1 products. Compounded semaglutide may use different salt forms (semaglutide sodium or semaglutide acetate), different concentrations, and different inactive ingredients than what's in the Ozempic pen. The FDA has stated that these salt forms are different active ingredients than those in approved products. That's not to alarm you — it's to explain why the transition requires a clinician's involvement. Moving to Ozempic is generally considered a step toward more consistent dosing and manufacturing quality.
Who This Page Is For — And Who Should Read Something Else
This page is specifically for people transitioning to the brand-name Ozempic pen. That usually means:
- You have type 2 diabetes (or your prescriber uses Ozempic off-label)
- You want the standardized, FDA-approved semaglutide injection
- You want insurance-backed access or the NovoCare self-pay route
- You want a clinician to map your transition properly
If that's not quite you:
- Goal is weight loss only, no diabetes → Switching to Wegovy guide
- Looking for the cheapest GLP-1 pathway in 2026 → GLP-1 cost without insurance guide
- Comparing multiple GLP-1 providers broadly → Best telehealth for GLP-1
How to Switch From Compounded Semaglutide to Ozempic Safely: 7 Steps
The process typically takes 2–4 weeks from decision to stable dosing.
Find Your Compounded Vial Label
Before you talk to anyone, dig up your vial or pharmacy records. You need:
- Concentration (mg/mL) — printed on the vial label
- Units or volume you inject per dose
- Frequency — weekly, twice weekly, daily
- Delivery method — subcutaneous injection, sublingual drops, oral tablets
- Any additives — B12, glycine, L-carnitine, etc.
Can't find the label? Call your compounding pharmacy and request a detailed breakdown. This documentation is the foundation of your safe switch.
Calculate Your Actual Weekly mg
This is the number your clinician needs. Forget “units” for a moment.
The formula
Concentration (mg/mL) × Volume injected per week (mL) = Your weekly mg
Example: 5 mg/mL × 0.2 mL/week = 1.0 mg semaglutide/week
If your vial mentions semaglutide sodium or semaglutide acetate, note that specifically. The FDA considers these different active ingredients than the semaglutide base form used in Ozempic.
Record Your Last Dose Date and Tolerance History
Write down: when you took your last compounded injection, side effects you've experienced (nausea, GI issues, fatigue), how your body responded at different doses, and whether you ever had to skip or reduce a dose and why. This helps your clinician gauge how to approach your Ozempic start.
Clarify Your Treatment Goal
This determines which brand-name semaglutide to discuss:
- Type 2 diabetes management → Ozempic is the right FDA-labeled conversation
- Weight loss only (no diabetes) → Wegovy may be the better fit
- Both → Your clinician will decide which brand makes sense for your insurance and clinical picture
If you tell your provider you want “Ozempic for weight loss,” know that this is off-label prescribing. Your insurance may not cover it for that indication. Wegovy has the FDA label for weight management and may actually be easier to get approved.
Check Your Insurance Coverage
Do this before your appointment so you're not blindsided at the pharmacy.
- Call the member services number on your insurance card
- Ask: “Is Ozempic on my formulary? What tier is it? Do I need prior authorization?”
- If Ozempic isn't covered, ask about Wegovy
- If neither is covered, ask what GLP-1 medications are on formulary
Have a Clinician Map Your Ozempic Start Dose
Bring your documentation from Steps 1–4 to a licensed prescriber. Here's what they're weighing:
| Factor | Why It Matters |
|---|---|
| Your documented mg/week | Establishes a baseline, but doesn't map 1:1 to Ozempic doses |
| Duration of any treatment gap | Gaps over 2 weeks often mean a more conservative restart |
| GI tolerance history | Prior nausea or vomiting → slower titration |
| Diabetes vs. weight loss goal | Determines Ozempic vs. Wegovy and impacts dosing targets |
| Salt form on your vial label | Semaglutide sodium/acetate ≠ semaglutide base form |
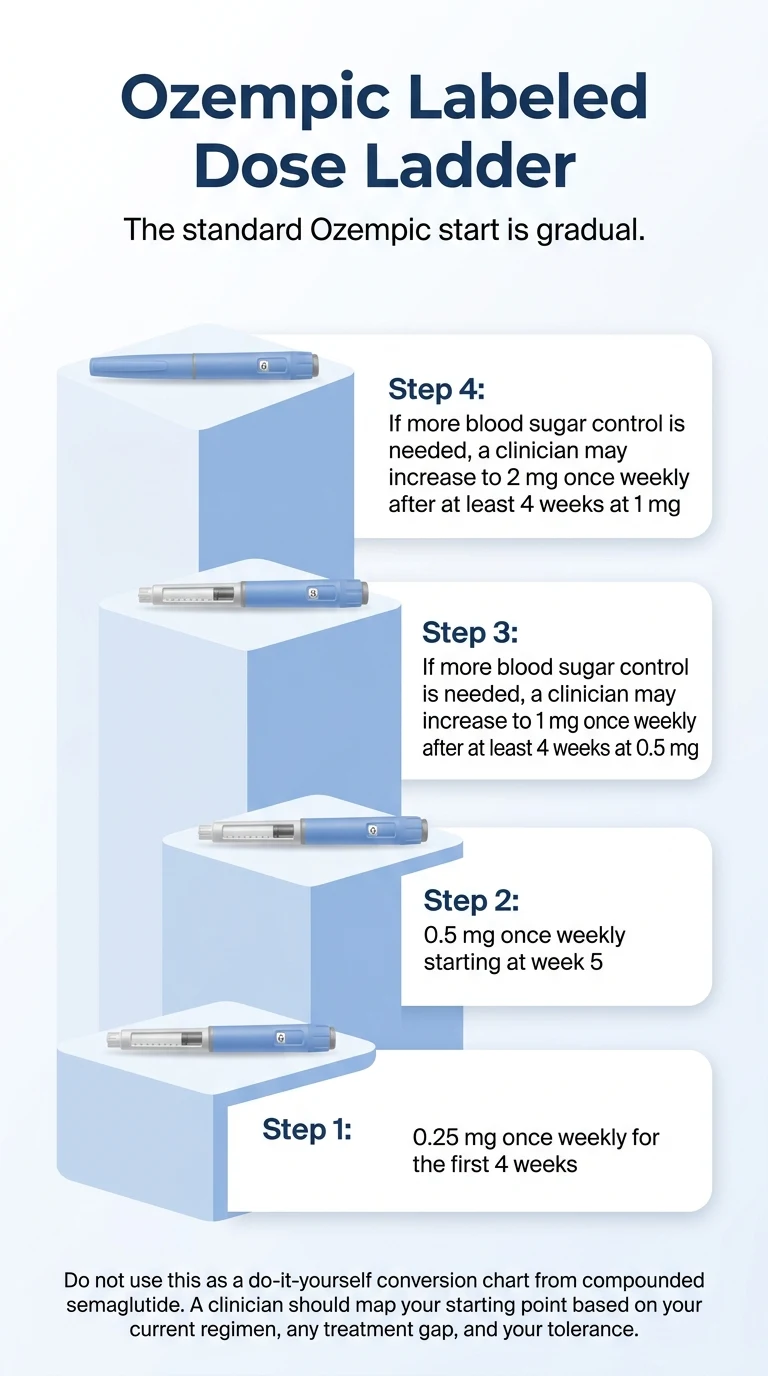
Ozempic's labeled dose ladder:
| When | Dose |
|---|---|
| Weeks 1–4 | 0.25 mg once weekly |
| Week 5+ | 0.5 mg once weekly |
| After ≥4 weeks at 0.5 mg, if needed | 1 mg once weekly |
| After ≥4 weeks at 1 mg, if needed | 2 mg once weekly |
Source: Ozempic FDA prescribing information. Do not use this as a DIY conversion — a clinician should map your start based on your current regimen and tolerance.
Fill Through a Legitimate Pharmacy Pathway
Get your prescription filled through:
- Your local retail pharmacy (covered by insurance)
- NovoCare Pharmacy (Novo Nordisk's direct channel — delivers to your door)
- A telehealth platform like Ro (handles prescription, insurance navigation, and pharmacy coordination)
Avoid online sources that don't require a valid prescription or that market their products using language the FDA has flagged. Use the FDA's BeSafeRx tool to verify any online pharmacy.

Do Not Convert Syringe Units to Ozempic Doses on Your Own
This deserves its own section because it's the single biggest mistake people make — and it's the one most likely to cause real problems.
Compounded concentrations are not standardized. One pharmacy's 2.5 mg/mL formulation is not guaranteed to deliver the same effective dose as another's. Manufacturing processes, inactive ingredients, salt forms, and stability can all affect bioavailability.
“Units” on a syringe are not milligrams. A standard insulin syringe measures volume (1 unit = 0.01 mL), but the semaglutide content depends entirely on your specific vial's concentration.
The Ozempic pen eliminates this guesswork. Each pen delivers a fixed, validated dose — 0.25 mg, 0.5 mg, 1 mg, or 2 mg. No math required. No concentration variability.
What to do instead: Calculate your weekly mg using the formula in Step 2, bring that number to your clinician, and let them decide where you start on the Ozempic dose ladder. That 15-minute conversation replaces hours of anxious Googling — and it's exactly the kind of conversation telehealth providers like Ro handle every day.
How Much Does Ozempic Cost After Switching From Compounded Semaglutide?
Ozempic's list price is $1,027.51 per pen. That's the manufacturer list price. Here's what real people actually pay in 2026:
If You Have Commercial (Employer) Insurance
Best case: as low as $25/month. The Novo Nordisk savings card covers up to $100/month in copay costs for commercially insured patients whose plans cover Ozempic. Valid for up to 48 months. No income verification required.
What to do: Activate the card at NovoCare.com or Ozempic.com, then present it at your pharmacy with your insurance card. This card cannot be used with Medicare, Medicaid, or other government insurance. If your copay is even close to manageable with the savings card, this is almost always the cheapest path.
If You're Uninsured or Self-Paying
Through NovoCare Pharmacy:
- $199/month for the first 2 fills of 0.25 mg or 0.5 mg (introductory offer valid through June 30, 2026 for new patients)
- $349/month ongoing for 0.25 mg, 0.5 mg, or 1 mg doses
- $499/month for the 2 mg dose
These prices include home delivery through NovoCare Pharmacy. Have your doctor send your prescription directly to NovoCare.
If You Want a Clinician Managing the Whole Transition
Ro provides telehealth prescribing support, insurance navigation, and ongoing clinical oversight. The membership costs $45 for the first month, then $145/month — medication is separate and billed through your pharmacy or NovoCare.
For Ozempic specifically, Ro's value is not a special medication discount. It's the clinical infrastructure: a prescriber who manages GLP-1 transitions daily, an insurance concierge that checks your coverage and handles prior authorization, and ongoing provider access through the app.
Think about what that insurance concierge is worth: if they get Ozempic covered at $25/month instead of $349+, you recoup the membership fee many times over.
If You Qualify for Patient Assistance (Free Ozempic)
Novo Nordisk offers a Patient Assistance Program that may provide Ozempic at no cost for qualifying patients with type 2 diabetes who are uninsured or on Medicare. Eligibility criteria are product- and coverage-specific and can change — check current requirements directly at NovoCare.com or call 1-888-809-3942.
If you think you might qualify, apply now. Processing typically takes 2–4 weeks, so don't wait until you run out.
Which Pathway Fits You?
Have employer insurance? → Check if Ozempic is covered first. With the savings card, you could pay as little as $25/month — less than most people were paying for compounded.
Uninsured? → NovoCare self-pay at $349/month is the most straightforward option. The intro pricing ($199/mo) makes the first two months more manageable.
Need a prescriber who handles this daily? → Ro gives you the clinician, insurance check, and pharmacy coordination in one place.
Low income or on Medicare? → Apply for the Patient Assistance Program at NovoCare.com. Don't assume you don't qualify — check.
When Should You Take Your First Ozempic Dose?
Your prescriber should determine the start date. Here's the general framework:
If Your compounded semaglutide was weekly
Clinicians often center the conversation around the next scheduled weekly dose — typically about one week after your last compounded injection. But this is still individualized based on your specific situation.
If Your compounded semaglutide was daily or sublingual
Daily formulations clear your system faster than weekly injectables. Your clinician will determine appropriate timing.
If You've already had a 1–2 week gap
You can likely start Ozempic now, generally at the 0.25 mg initiation dose. Bring your records and confirm with your provider.
If You've been off semaglutide for more than 2 weeks
A longer gap changes the conversation. GI tolerance can reset after an extended break, so your clinician will likely treat this closer to a brand-new start — 0.25 mg weekly for 4 weeks, then titrate up. Don't try to jump back to your previous dose.
What to Watch For in the First Month After Switching
The First 1–2 Weeks
Some people experience a return of mild nausea or decreased appetite — even though they've been on a semaglutide product before. This happens because Ozempic is a different formulation with different absorption characteristics, and because your clinician is likely starting you on a lower dose and re-titrating.
Eat smaller, protein-rich meals. Stay hydrated. Avoid greasy or heavy foods for the first few days. These GI effects are typically transient and less intense than when you first started compounded semaglutide — your body already has some adaptation to the drug class.
Weeks 3–4
If you started at 0.25 mg, your provider may increase to 0.5 mg at the 4-week mark. Appetite control tends to become more predictable as you reach a therapeutic dose. This is also a good time to check in with your provider about how the transition is going.
Month 2+
At your target dose, treatment effects stabilize. Schedule ongoing check-ins with your provider every 4–8 weeks to discuss progress and any dose adjustments.
When to contact your provider immediately
- Severe, persistent abdominal pain (potential sign of pancreatitis)
- Vision changes (particularly if you have diabetes)
- Signs of an allergic reaction (rash, swelling, difficulty breathing)
- Severe nausea or vomiting that could lead to dehydration
Who should be extra cautious
- Personal or family history of medullary thyroid carcinoma (MTC) or MEN2 syndrome — Ozempic carries a boxed warning
- History of pancreatitis — requires careful clinician evaluation
- Taking insulin or sulfonylureas — may increase hypoglycemia risk; your clinician may adjust other diabetes medications
- Severe gastroparesis — GLP-1 receptor agonists slow gastric emptying and may worsen this condition
Ozempic vs. Wegovy: Which One Should You Actually Ask For?
Many people type “Ozempic” when what they really mean is “brand-name semaglutide.” The two brands contain the same active ingredient but are approved for different purposes.
| Ozempic | Wegovy (injection) | |
|---|---|---|
| Active ingredient | Semaglutide | Semaglutide |
| FDA-approved for | Adults with type 2 diabetes; CV event reduction in T2D | Weight management; CV event reduction in obesity/overweight |
| Max labeled dose | 2 mg/week | 2.4 mg/week |
| Form | Weekly injection (pen) | Weekly injection (pen) |
| Self-pay cost | $349–$499/mo via NovoCare | $349/mo via NovoCare |
| Insurance coverage | Broad (for diabetes) | Growing (for weight management) |
You have type 2 diabetes → Start the Ozempic conversation. Insurance coverage is strongest here.
Primary goal is weight loss, no diabetes → Wegovy is the FDA-labeled option and may be easier to get approved by insurance.
Insurance covers one but not the other → Go with whichever is covered. Same active ingredient, same mechanism.
You want a pill, not an injection → Wegovy pill (FDA-approved December 2025) is now available starting at $149/month for certain doses.
On Medicare? → The temporary Medicare GLP-1 Bridge beginning July 2026 covers Wegovy (injection and tablets) and Zepbound — not Ozempic. For Ozempic specifically, coverage depends on your Part D plan and indication.
What to Bring to Your Switching Appointment
Prepared patients get better transitions. The more specific your documentation, the less guesswork for your clinician.
Your pre-switch checklist
Bringing this to your appointment turns a 30-minute conversation into a 10-minute one. Your clinician can focus on choosing the right starting dose instead of trying to reconstruct what you were taking.
How to Verify Your Ozempic and Pharmacy Are Legitimate
The compounded-to-brand switch is exactly the moment bad actors target. You're in a hurry, you're vulnerable, and there are online sources happy to sell you something that isn't what it claims.
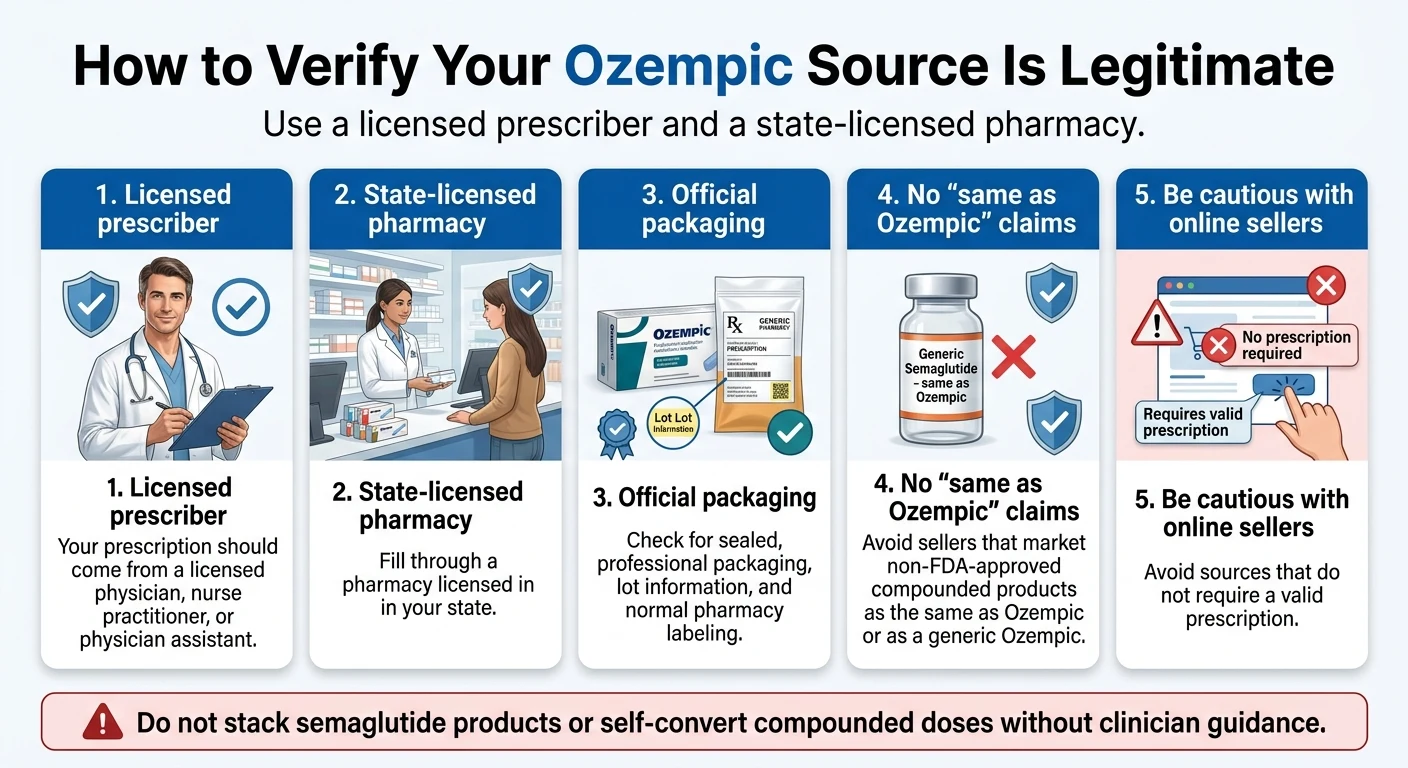
State-licensed pharmacy
NovoCare Pharmacy, major retail chains (CVS, Walgreens, Costco), and Ro's partner pharmacies all meet this standard.
Licensed prescriber
The person writing your prescription should be a licensed physician, PA, or NP practicing in your state.
Official packaging
Ozempic comes in a branded Novo Nordisk pen with specific labeling, lot numbers, and expiration dates. If what you receive doesn't match the images on Ozempic.com, contact Novo Nordisk.
No 'same as Ozempic' marketing
The FDA has warned companies against marketing compounded products as equivalent to FDA-approved drugs. There is no generic Ozempic. If a source claims otherwise, walk away.
Use BeSafeRx
The FDA's BeSafeRx program verifies online pharmacies. Check any online source at FDA.gov/BeSafeRx.
The Best Way to Get Ozempic: Your Doctor, Ro, or Another Path?
You've resolved the medical questions. Now the practical one: who handles the prescription?
| Path | Best For |
|---|---|
| Your own doctor + local pharmacy | People with an existing PCP or endocrinologist |
| Ro (telehealth) | People who need a prescriber + insurance navigation + ongoing support |
| NovoCare Pharmacy direct | People who already have a prescription |
The cheapest path: Your own doctor + insurance. If Ozempic is covered and you activate the savings card, you could pay $25/month. Nothing beats that.
The most practical path for people losing their compounded provider: This is where Ro earns its place. When your compounded telehealth provider exits semaglutide (many have), you need a new clinician, a new prescription, insurance verification, and a pharmacy — all at once. That's the specific problem Ro solves.
If insurance denies Ozempic
Don't stop there. A denial for one product is not a dead end — it's a redirect. Your options:
- Ask about Wegovy — different insurance pathway, same active ingredient
- NovoCare self-pay — $349/month bypasses insurance entirely
- Patient Assistance Program — check current eligibility at NovoCare.com
- Wegovy pill — starting at $149/month for certain doses, no injection required
- Explore tirzepatide (Zepbound) — dual mechanism, self-pay vials start at $299/month for 2.5 mg
Methodology: How We Verified This Page
We take accuracy on medical topics seriously. Here's what we checked and when.
Pricing data (verified April 2026)
- NovoCare.com — Ozempic list price, self-pay pricing, PAP eligibility
- Ozempic.com — savings card terms and eligibility
- Ro.co/weight-loss/pricing — membership cost, medication cost structure
- CMS.gov — Medicare GLP-1 Bridge eligibility
Clinical information sourced from
- Ozempic prescribing information — dosing, indications, warnings
- FDA Drug Safety Communications — compounded GLP-1 concerns
- FDA compounding policy guidance — shortage resolution timeline
- Published clinical guidance on GLP-1 switching (PMC)
What we did NOT do
We did not publish a “dose conversion chart” — no validated one exists. We did not claim compounded semaglutide is “the same” as Ozempic. We did not use fake reviews or schema for content that doesn't exist on the page.
Frequently Asked Questions
Is compounded semaglutide the same as Ozempic?
No. Ozempic is an FDA-approved semaglutide product manufactured by Novo Nordisk with standardized dosing and quality controls. Compounded semaglutide is not FDA-approved, may use different salt forms, and has not undergone the same clinical testing. The FDA warns against treating them as interchangeable.
Can I switch from compounded semaglutide to Ozempic without a gap in treatment?
In many cases, yes. Your prescriber will determine the best timing based on your last dose date, the specific product you were using, and your tolerance history. For people on weekly compounded products, clinicians often center the conversation around the next scheduled weekly dose.
Will I gain weight during the transition to Ozempic?
Continuity of treatment matters. A seamless switch with proper clinician guidance and no extended gap helps maintain your progress. Some mild fluctuation is possible during dose re-titration, but staying in contact with your provider and maintaining your dietary habits helps minimize any disruption.
What dose of Ozempic should I start on after compounded semaglutide?
Ozempic’s labeled initiation is 0.25 mg once weekly for 4 weeks, then 0.5 mg weekly. But switching from compounded semaglutide should be individualized — your clinician will consider your documented prior regimen, any treatment gap, and your GI tolerance to choose the right starting point.
How much does Ozempic cost without insurance in 2026?
Ozempic’s list price is $1,027.51 per pen. Through NovoCare Pharmacy, new self-pay patients currently pay $199 for each of the first 2 monthly fills of 0.25 mg or 0.5 mg (through June 30, 2026). After that, self-pay pricing is $349/month for 0.25–1 mg doses and $499/month for 2 mg.
Is Ozempic covered by insurance for weight loss?
Ozempic is FDA-approved for type 2 diabetes, and most commercial plans cover it for that indication. For weight loss specifically, Wegovy — which contains the same active ingredient — is the FDA-labeled option and has growing but variable coverage. If insurance denies Ozempic for weight loss, asking about Wegovy is usually the next step.
Should I switch to Ozempic or Wegovy?
If you have type 2 diabetes or want the branded Ozempic pen, Ozempic is the right conversation. If your primary goal is weight loss and you do not have diabetes, Wegovy is the more appropriate FDA-labeled option. Both contain semaglutide. Your insurance coverage may also determine which is easier to access.
What if my compounded semaglutide label says semaglutide sodium or semaglutide acetate?
Bring that label to your clinician. The FDA has stated that semaglutide sodium and semaglutide acetate are different active ingredients than the semaglutide base form in Ozempic. This distinction affects how your provider approaches the transition.
Can I take compounded semaglutide and Ozempic at the same time?
No. Do not overlap or stack semaglutide products without explicit clinician direction. The switch should be a clean transition — stop one, start the other — with your provider determining the timing.
What if I have been off semaglutide for more than 2 weeks?
A longer gap usually means a more conservative restart. Your clinician will likely start you at the lowest Ozempic dose (0.25 mg) and re-titrate from there, regardless of what your previous compounded dose was. GI tolerance can reset during extended breaks.
Can I take Ozempic and insulin together?
In some cases — but it requires clinician management because the combination can increase hypoglycemia risk. Your provider may need to adjust your insulin dose when adding Ozempic.
What if Ozempic feels weaker or different after the switch?
This is common and usually reflects differences in formulation, absorption, or dosing between compounded products and the standardized pen. Don’t self-adjust your dose — bring this to your prescriber. It’s one of the most common conversations they have during transitions.
Still Not Sure Which GLP-1 Program Is Right for You?
Tell us your insurance status, budget, and health goals — and we'll show you the most affordable FDA-approved pathway for your specific situation. No spam. No obligations.
Take the Free 60-Second GLP-1 Matching Quiz →Related guides
The RX Index is an independent research platform. We may earn a commission from providers linked on this page. Our editorial recommendations are based on independent research, verified pricing, and clinical accuracy — not compensation. Full affiliate disclosure →
This page was last verified against primary sources on April 1, 2026. The RX Index is not a pharmacy, prescriber, or insurance company. Always consult a licensed healthcare provider before starting or switching any medication.