Medicaid GLP-1 Coverage by State (2026): All 50 States, Verified
Only 13 state Medicaid fee-for-service programs cover GLP-1 medications for obesity treatment as of 2026 — and that number dropped from 16 after California, New Hampshire, Pennsylvania, and South Carolina eliminated coverage on January 1. Roughly 80% of adult Medicaid enrollees live in states with no obesity GLP-1 pathway right now.
But "not covered for weight loss" is not the same thing as "no path at all." Every state Medicaid program is federally required to cover GLP-1s prescribed for type 2 diabetes. Since 2024, the rules changed for additional indications — Wegovy for cardiovascular risk reduction, Zepbound for obstructive sleep apnea, Wegovy for MASH. Children under 21 have a separate federal protection (EPSDT) that most pages don't mention.
Sources: KFF Medicaid Coverage of and Spending on GLP-1s (Jan 2026); The RX Index Coverage Reach calculation based on CMS enrollment data; state Medicaid bulletins.
If any of those sound familiar, you're in the right place. The system is genuinely confusing — and it's changing faster than most coverage guides keep up with. That's why we verify this page monthly and publish every source, every change date, and a downloadable dataset you can audit yourself.
Which states cover GLP-1s through Medicaid right now?
As of April 2026, 13 state Medicaid FFS programs cover GLP-1 medications for obesity treatment. Our verification, updated April 7, 2026, breaks that 13 into 10 states with full obesity GLP-1 coverage and 3 with restricted coverage. There are also 7 additional states that cover at least one weight-loss drug — but not any GLP-1 specifically.
The RX Index Coverage Reach
We calculate Coverage Reach using CMS Medicaid enrollment data — because "13 states" doesn't tell you how many people are actually affected:
- 19.7% of adult Medicaid enrollees (~7.8 million out of ~39.5 million adults) live in states with some pathway to obesity GLP-1 coverage
- 80.3% (~31.7 million adults) live in states with no FFS obesity GLP-1 coverage
- ~35% of adult Medicaid enrollees live in states that changed coverage status in the last 12 months
Source: The RX Index Coverage Reach calculation; CMS Medicaid enrollment data; KFF Jan 2026.
50-State Medicaid GLP-1 Coverage Table
The following table reflects our most recent verification as of April 10, 2026. We cross-reference state Medicaid preferred drug lists (PDLs), official policy bulletins, KFF's 50-state survey, and CMS data.
How to read this table: "Obesity GLP-1 status" refers to coverage of GLP-1s when prescribed for obesity or weight management — not diabetes, cardiovascular, or sleep apnea indications, which have different federal rules covered below.
| State | Obesity GLP-1 Status | Drugs Named | Prior Auth? | Key Notes | Recent Change |
|---|---|---|---|---|---|
| Alabama | 🔴 Not covered | — | — | Diabetes GLP-1s covered | — |
| Alaska | 🔴 Not covered | — | — | Diabetes GLP-1s covered | — |
| Arizona | 🔴 Not covered | — | — | Partial managed care notes; verify with AHCCCS | — |
| Arkansas | 🔴 Not covered | — | — | HB 1332 failed to advance | — |
| California | 🔵🔴 Recently cut | — | — | Eliminated all GLP-1 weight loss coverage for adults 21+ effective Jan 1, 2026. Wegovy, Zepbound, Saxenda removed from Medi-Cal Rx CDL for weight loss. Covered for T2D, CVD, OSA, and noncirrhotic MASH with PA. | Jan 1, 2026 |
| Colorado | 🔴 Not covered | — | — | Diabetes GLP-1s covered | — |
| Connecticut | 🟠 Non-GLP-1 only | ⚠️ Verify | — | Reported covering a weight-loss drug but not GLP-1s; proposed ending coverage | ⚠️ Verify |
| Delaware | 🟢 Covered | Wegovy, Zepbound, Saxenda | Yes | — | — |
| Florida | 🔴 Not covered | — | — | Considering expansion per KFF survey | — |
| Georgia | 🔴 Not covered | — | — | Considering expansion per KFF survey | — |
| Hawaii | 🔴 Not covered | — | — | Diabetes GLP-1s covered | — |
| Idaho | 🔴 Not covered | — | — | Diabetes GLP-1s covered | — |
| Illinois | 🔴 Not covered | — | — | State employee plan covers; Medicaid does not | — |
| Indiana | 🔴 Not covered | — | — | Diabetes GLP-1s covered | — |
| Iowa | 🔴 Not covered | — | — | SSB 1138 under review for state employees | — |
| Kansas | 🟡 Restricted | Wegovy, Zepbound, Saxenda | Yes | KanCare PA criteria include severe obesity pathway + separate Wegovy CVD pathway. Not limited to CVD-only. | — |
| Kentucky | 🔴 Not covered | — | — | Diabetes GLP-1s covered | — |
| Louisiana | 🟠 Non-GLP-1 only | Orlistat | — | Covers orlistat but no GLP-1s for obesity | — |
| Maine | 🔴 Not covered | — | — | Diabetes GLP-1s covered | — |
| Maryland | 🔴 Not covered | — | — | Legislation introduced but not advanced | — |
| Massachusetts | 🟡 Restricted | Zepbound (preferred adult); Wegovy for adolescents + CVD | Yes | Adults age 21+ with BMI ≥30 (or ≥27 with comorbidity). MassHealth announced scheduled shift away from ongoing weight-loss GLP-1 coverage effective July 1, 2026. | Restricted Mar 2026; further change Jul 1, 2026 |
| Michigan | 🟡🔵 Restricted + recently changed | Wegovy, Zepbound | Yes | Restricted to morbid obesity only effective Jan 1, 2026. Must have failed other weight loss interventions. | Jan 1, 2026 |
| Minnesota | 🟢 Covered | Wegovy, Zepbound, Saxenda | Yes | — | — |
| Mississippi | 🟢 Covered | Wegovy, Zepbound, Saxenda | Yes | SB 2867 to expand was vetoed by governor due to fiscal concerns, but existing coverage continues | — |
| Missouri | 🟢 Covered | ⚠️ Verify specific drugs | Yes | — | ⚠️ Verify |
| Montana | 🔴 Not covered | — | — | SB 417 did not advance | — |
| Nebraska | 🔴 Not covered | — | — | Diabetes GLP-1s covered | — |
| Nevada | 🔴 Not covered | — | — | Diabetes GLP-1s covered | — |
| New Hampshire | 🔵🔴 Recently cut | — | — | Eliminated weight-loss-only coverage effective Jan 1, 2026. Diabetes and other indications still covered. | Jan 1, 2026 |
| New Jersey | 🔴 Not covered | — | — | Diabetes GLP-1s covered | — |
| New Mexico | 🟠 Non-GLP-1 only | ⚠️ Verify | — | SB 193 did not advance; may cover non-GLP-1 weight-loss drug | ⚠️ Verify |
| New York | 🔴 Not covered | — | — | ⚠️ Some sources list partial coverage; verify with state PDL | ⚠️ Verify |
| North Carolina | 🟢🔵 Covered (reinstated) | Wegovy, Zepbound, Saxenda | Yes | Reinstated Dec 12, 2025 after budget stalemate. Previously cut Oct 2025. | Dec 12, 2025 ✓ |
| North Dakota | 🟠 Non-GLP-1 only | ⚠️ Verify | — | First state to mandate insurance coverage for GLP-1s (Jan 2025), but Medicaid GLP-1 obesity status needs verification | ⚠️ Verify |
| Ohio | 🔴 Not covered | — | — | Considering expansion per KFF survey | — |
| Oklahoma | 🔴 Not covered | — | — | Diabetes GLP-1s covered | — |
| Oregon | 🔴 Not covered | — | — | Diabetes GLP-1s covered | — |
| Pennsylvania | 🔵🔴 Recently cut | — | — | Eliminated for adults 21+ effective Jan 1, 2026. Under-21 still covered under EPSDT. GLP-1 spending grew from $233M (2022) to est. $1.3B (2025) — from 5% to 22% of total drug spending. | Jan 1, 2026 |
| Rhode Island | 🟢 Covered | Wegovy, Zepbound, Saxenda | Yes | Considering new restrictions per Stateline (Nov 2025) | ⚠️ Watch |
| South Carolina | 🔵🔴 Recently cut | — | — | Eliminated Wegovy and Saxenda for obesity effective Jan 1, 2026. | Jan 1, 2026 |
| South Dakota | 🔴 Not covered | — | — | Diabetes GLP-1s covered | — |
| Tennessee | 🟢 Covered | ⚠️ Verify specific drugs | Yes | — | ⚠️ Verify |
| Texas | 🟠 Non-GLP-1 only | ⚠️ Verify | — | HB 2412 did not advance. May have partial non-GLP-1 coverage; considering expansion per KFF | ⚠️ Verify |
| Utah | 🟢 Covered | ⚠️ Verify specific drugs | Yes | — | ⚠️ Verify |
| Vermont | 🟠 Non-GLP-1 only | Wegovy (MACE only) | Yes | Covers Wegovy for cardiovascular risk reduction but NOT for obesity as standalone condition. Ozempic covered for T2D only. | — |
| Virginia | 🟢 Covered | Wegovy, Zepbound, Saxenda | Yes | Requires documented medical necessity, PA, patient eligibility, and budget constraints | — |
| Washington | 🟠 Non-GLP-1 only | ⚠️ Verify | — | HB 1197/SB 5166 requires state agency reports on future coverage | ⚠️ Verify |
| West Virginia | 🔴 Not covered | — | — | HB 2912 introduced. State employee plan pilot paused 2024 ($1.3M/month cost). | — |
| Wisconsin | 🟢 Covered | Wegovy, Zepbound, Saxenda | Yes | Considering new restrictions per Stateline (Nov 2025) | ⚠️ Watch |
| Wyoming | 🔴 Not covered | — | — | Diabetes GLP-1s covered | — |
| Washington, D.C. | 🔴 Not covered | — | — | ⚠️ Verify | ⚠️ Verify |
⚠️ Coverage policies change frequently. We verify this table monthly. Always confirm directly with your state Medicaid program before making medical or financial decisions.
Sources: KFF Medicaid Coverage of and Spending on GLP-1s (Jan 2026); state Medicaid PDLs and pharmacy bulletins; CMS BALANCE Model page; Stateline (Nov 2025); Real Chemistry state analysis (Nov 2024); Pharmacy Times (Mar 2026).
Does Medicaid have to cover Wegovy, Zepbound, or Ozempic in any situation?
Yes — but only for specific indications. Federal law under the Medicaid Drug Rebate Program (42 U.S.C. § 1396r-8) requires state Medicaid programs to cover nearly all FDA-approved drugs for their medically accepted indications. The exception is a narrow category that includes drugs "used for weight loss" — which is why states can exclude GLP-1s when prescribed for obesity.
But here's what most coverage guides get wrong: the same medications have other FDA-approved indications that fall outside the weight-loss exclusion. When prescribed for those indications, Medicaid coverage is mandatory, not optional. This distinction is not a loophole. It's how the law actually works.
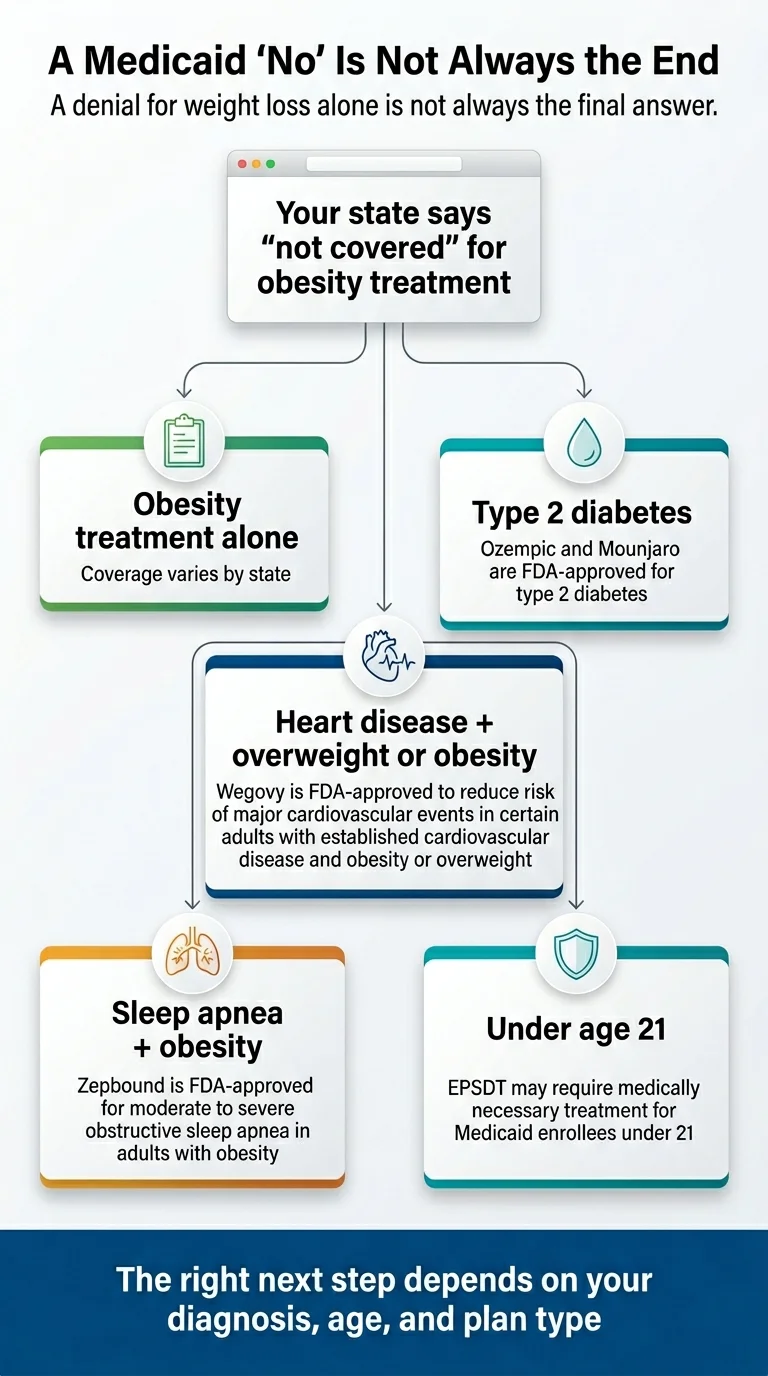
Diagnosis-Path Matrix
This matrix shows when a GLP-1 medication goes from "optional state coverage" to "federally required coverage" based on the FDA-approved indication your doctor prescribes it for.
| Medication | Obesity / Weight Loss | Type 2 Diabetes | Cardiovascular Risk | Sleep Apnea (OSA) | MASH (Liver Disease) | Under 21 (EPSDT) |
|---|---|---|---|---|---|---|
| Wegovy(semaglutide) | ⚪ State optional — only 13 states | N/A (not approved for T2D) | ✅ Required — FDA approved Mar 2024 for CVD risk reduction in adults with BMI ≥27 + established CVD | N/A | ✅ Required — FDA approved Aug 2025 for noncirrhotic MASH with liver fibrosis | ✅ Required if medically necessary |
| Zepbound(tirzepatide) | ⚪ State optional — only 13 states | N/A (Mounjaro is T2D brand) | N/A | ✅ Required — FDA approved Dec 2024 for moderate-to-severe OSA in adults with obesity | N/A | ✅ Required if medically necessary |
| Ozempic(semaglutide) | N/A (not approved for weight loss) | ✅ Required — all 50 states | N/A | N/A | N/A | ✅ Required if medically necessary |
| Mounjaro(tirzepatide) | N/A (not approved for weight loss) | ✅ Required — all 50 states | N/A | N/A | N/A | ✅ Required if medically necessary |
| Saxenda(liraglutide) | ⚪ State optional | N/A | N/A | N/A | N/A | ✅ Required if medically necessary |
What this means practically
If your state Medicaid says "we don't cover GLP-1s for weight loss," ask your doctor whether any of these apply to you:
- Do you have type 2 diabetes? Ozempic and Mounjaro are covered in every state for T2D — and these medications also produce significant weight loss even when prescribed for diabetes.
- Do you have established cardiovascular disease (prior heart attack, stroke, or documented coronary artery disease) and a BMI of 27 or higher? Since March 2024, Wegovy is FDA-approved for cardiovascular risk reduction. Medicaid must cover it for this indication.
- Do you have moderate-to-severe obstructive sleep apnea and obesity? Since December 2024, Zepbound is FDA-approved for moderate-to-severe OSA in adults with obesity — a non-weight-loss indication requiring sleep apnea documentation.
- Have you been diagnosed with MASH with liver fibrosis? Since August 2025, Wegovy is FDA-approved for noncirrhotic MASH. California's Medi-Cal explicitly confirms Wegovy for MASH continues to be covered even after the obesity coverage cut — if the prescriber submits the appropriate diagnosis code.
- Are you under 21? Federal EPSDT law requires Medicaid to cover medically necessary treatments for enrollees under 21 — even when those treatments are excluded for adults. A plan cannot apply a blanket "we don't cover weight loss drugs" exclusion to someone under 21. Pennsylvania's January 2026 coverage change explicitly preserved under-21 GLP-1 access for this reason. If your child has been denied, appeal immediately and cite EPSDT.
We are not suggesting you ask for a prescription under a false indication. We are saying that many Medicaid enrollees have legitimate comorbidities that qualify them for coverage through a different pathway than obesity alone. Your doctor determines which indication is clinically appropriate.
Not sure which path fits your situation?
Our 60-second quiz matches you to the right next step based on your state, diagnosis, and budget. No account required.
Take the free GLP-1 matching quiz →Why your answer may change depending on fee-for-service vs. managed care
About 78% of Medicaid beneficiaries nationally are enrolled in comprehensive managed care (MCOs), not fee-for-service (FFS). The 50-state table above is based on FFS coverage — the baseline policy that each state sets. But your actual coverage may differ depending on which plan you're in.

Fee-for-service means the state Medicaid agency pays providers directly. The state's preferred drug list (PDL) is what determines your coverage.
Managed care means a private insurance company (the MCO) manages your Medicaid benefits under contract with the state. MCOs have their own formularies and prior authorization criteria. In some states, the MCO may cover drugs the FFS program doesn't — or vice versa.
The state-level answer is your starting point, not your final answer. You need to verify with your specific plan.
Don't stop at the state answer — use this checklist
Before you conclude that Medicaid won't cover your GLP-1, verify all five of these:
- Which type of Medicaid do you have? Check your Medicaid card. If it names a company (Aetna Better Health, Anthem MediBlue, Centene, Molina, UnitedHealthcare, etc.), you're in managed care.
- What does your MCO's formulary say? Call the number on the back of your card and ask specifically: "Is [drug name] on your preferred drug list for [your indication]?"
- What indication is your doctor using? "Obesity" vs. "cardiovascular risk reduction" vs. "type 2 diabetes" can produce completely different answers from the same plan.
- Has the formulary been updated recently? MCOs update formularies quarterly. A "no" from six months ago may not be current.
- Is prior authorization required? Even when covered, almost every plan requires PA for GLP-1s. Ask what documentation is needed before your doctor submits.
Here's a script you can use when you call:
Write down the name of the person you speak with, the date, and what they tell you.
Which states changed Medicaid GLP-1 coverage most recently?
Coverage is moving fast — and mostly in the wrong direction. Nine states changed coverage status in the last 12 months, affecting roughly 35% of adult Medicaid enrollees.
❌ CUT
California — Eliminated
Medi-Cal eliminated all GLP-1 weight loss coverage for adults 21 and older. Wegovy, Zepbound, and Saxenda were removed from the Medi-Cal Rx Contract Drugs List for weight loss. Coverage continues for type 2 diabetes, cardiovascular disease, sleep apnea, and noncirrhotic MASH with prior authorization.
Important: California's official Medi-Cal Rx FAQ confirms Wegovy for MASH continues to be covered if the prescriber submits the appropriate diagnosis code — a pathway many enrollees don't know about. The state estimated savings of over $200 million from the change.
❌ CUT
Pennsylvania — Eliminated
Pennsylvania Medicaid stopped covering GLP-1s for weight loss in adults 21 and older. GLP-1 spending exploded from $233 million in 2022 to an estimated $1.3 billion in 2025 — growing from 5% to 22% of total Medicaid drug spending in three years. The state projected $836 million in savings.
Children and young adults under 21 are still covered under EPSDT protections. Adults prescribed GLP-1s for diabetes, CVD, or sleep apnea retain coverage with prior authorization.
✅ REINSTATED
North Carolina — Reinstated
North Carolina eliminated GLP-1 obesity coverage in October 2025 due to a legislative budget stalemate, then reinstated it in December 2025 once funding was resolved. Coverage is now active again through NC Medicaid.
❌ CUT
New Hampshire — Eliminated
New Hampshire ended weight-loss-only GLP-1 coverage. Coverage continues for other medically accepted indications.
❌ CUT
South Carolina — Eliminated
South Carolina removed Wegovy and Saxenda for obesity from its Medicaid formulary.
🟡 RESTRICTED
Michigan — Restricted
Michigan restricted coverage significantly to individuals classified as morbidly obese, with coverage contingent on the failure of other weight loss interventions to prevent higher-cost bariatric surgery. Prior authorization is required for all indications.
🟡 RESTRICTED
Massachusetts — Restricted, further change coming
Massachusetts shifted its preferred adult GLP-1 from Wegovy to Zepbound in October 2024 and further tightened criteria in early 2026. Adults 21+ with BMI ≥30 (or ≥27 with comorbidity) may still qualify. MassHealth announced a scheduled shift away from ongoing weight-loss GLP-1 coverage effective July 1, 2026 — enrollees currently covered should verify their renewal timeline.
States to watch
Rhode Island and Wisconsin were both reported considering new restrictions as of late 2025. Connecticut has proposed ending coverage. We'll update this section as changes are confirmed.
Why are states cutting GLP-1 coverage?
It's not because the drugs don't work. States are cutting coverage because the math broke.
KFF data tells the story clearly: Medicaid GLP-1 prescriptions rose from about 1 million in 2019 to over 8 million in 2024 — an eightfold increase. Gross spending rose from about $1 billion in 2019 to nearly $9 billion in 2024. Even accounting for manufacturer rebates that typically reduce costs by about 40%, that's an enormous budget line that grew faster than almost anyone projected.
GLP-1s went from roughly 0% of all Medicaid prescriptions in 2019 to about 1% in 2024 — a tiny share of total prescriptions — but they now account for over 8% of all Medicaid prescription drug spending before rebates. Pennsylvania's numbers illustrate this at the state level: GLP-1 costs grew from 5% of total Medicaid drug spending in 2022 to 22% in 2025.
This isn't about whether GLP-1s are effective. The evidence is clear that they are. It's about whether state budgets can absorb the cost at current utilization rates — especially with federal Medicaid spending cuts from the 2025 reconciliation law adding additional pressure. Nearly 40% of adults on Medicaid have obesity, which means the potential demand is enormous. That's the core tension.
Sources: KFF Medicaid Coverage of and Spending on GLP-1s (Jan 2026); PA DHS data per Philadelphia Inquirer (April 10, 2026); MACPAC enrollment data.
Will the CMS BALANCE Model change Medicaid GLP-1 coverage in your state?
Possibly — and the timeline is now. But it's not automatic, and it's not a guarantee.
The CMS BALANCE Model
The BALANCE Model (Better Approaches to Lifestyle and Nutrition for Comprehensive hEalth) is a voluntary CMS Innovation Center program that launched for state Medicaid agencies on May 1, 2026. States can apply through July 31, 2026, with all participating states required to have coverage live by January 1, 2027.
- Negotiated drugs: Mounjaro, Ozempic, Rybelsus, Wegovy, Zepbound KwikPen, orforglipron (if approved)
- States that participate adopt standardized coverage criteria — they can be broader but not more restrictive than CMS terms
- All beneficiaries receiving GLP-1s under BALANCE get access to a manufacturer-funded lifestyle program at no cost
- States can start with FFS populations and bring managed care in later
Which states will participate?
As of April 10, 2026, CMS has not published a list of participating states. States that already cover GLP-1s for obesity are natural candidates. States that recently eliminated coverage could rejoin under BALANCE if the negotiated pricing makes it budget-feasible. Several states — including Texas, Florida, Georgia, and Ohio — were reportedly considering expansion in KFF's earlier surveys.
What BALANCE means for you
- If your state joins: You may gain coverage starting as early as May 2026, with standardized PA criteria and a lifestyle support program at no cost.
- If your state doesn't join: Nothing changes. Your current coverage status stays in place.
- If you're already covered: You may see lower out-of-pocket costs and access to the lifestyle program.
The honest assessment: BALANCE is promising but voluntary. States facing budget pressure may not opt in even at lower prices, because the volume of eligible enrollees could still make total spending unmanageable. We'll know more by summer 2026.
Sources: CMS BALANCE Model page (updated Mar 2026); CMS BALANCE RFA (Dec 2025); KFF "What to Know About the BALANCE Model" (Mar 2026). For a deeper breakdown, see our full guide: CMS BALANCE Model GLP-1 Explained.
What do I do if my state Medicaid says no?
A denial is not the end. It's the start of a decision tree. Your next step depends on why you were denied and what your specific situation is.

Get the exact denial reason in writing
Call your Medicaid plan (the number on the back of your card) and request the denial in writing. You need to know exactly which category your denial falls into:
- "Your plan does not cover this drug for weight loss" = Plan exclusion. This is the hardest to overturn through standard appeal.
- "Prior authorization required / not approved" = PA denial. This can often be resolved by resubmitting with better documentation.
- "Not on formulary" = Formulary exclusion. May be resolvable through a coverage exception or formulary alternative.
- "Only covered for certain conditions" = Indication restriction. Another diagnosis pathway may work.
Check whether another indication applies
Revisit the diagnosis-path matrix above. If you have type 2 diabetes, documented cardiovascular disease, diagnosed sleep apnea, or MASH, ask your doctor whether prescribing for that indication is clinically appropriate. See our full guide to getting insurance to cover GLP-1 medications for step-by-step instructions.
Verify FFS vs. managed care
If you're in managed care, your MCO formulary may differ from the state FFS baseline. Use the verification script above to check with your specific plan.
Appeal or request a fair hearing
If your PA was denied, you have the right to appeal. In most states:
- Internal appeal: File within the timeline on your denial letter (usually 30–60 days). Include updated clinical documentation.
- Peer-to-peer review: Your doctor can request a phone call with the plan's medical director to discuss your case.
- State fair hearing: If internal appeals are exhausted, you can request a hearing through your state Medicaid agency.
- For under-21 enrollees: If denied, always appeal citing EPSDT. The plan must evaluate medical necessity individually — they cannot apply a blanket exclusion.
Timing matters: In Pennsylvania, filing an appeal within 15 days of the denial date preserved coverage during the appeal process.
Decide when to pivot
If you've exhausted your Medicaid options, you have a decision to make. The brand-name list price remains $1,000+/month at retail. KFF made this point directly: unless Medicaid covers these drugs, even reduced manufacturer prices are likely prohibitive for people who must have low income to qualify for the program. But there are options that cost a fraction of that — see below.
If Medicaid won't cover it: your best next routes
This section is for readers who've worked through the steps above and determined that Medicaid coverage genuinely isn't available in their situation. We're not going to pretend this is ideal — it's not. But we're also not going to leave you without a path forward.
If you need help with prior authorization or insurance navigation
Sometimes the issue isn't that coverage doesn't exist — it's that the paperwork wasn't done right, or a covered indication wasn't explored.
- → How to Get Insurance to Cover GLP-1 Medications — our full guide to PA strategy, appeal letters, and covered indication routing
- → Best GLP-1 Providers That Help With Prior Authorization — providers that handle PA on your behalf
If you need an affordable cash-pay path
Compounded semaglutide is available through licensed telehealth providers at prices dramatically lower than brand-name medications. These programs don't bill Medicaid — they're cash-pay, so there's no PA, no denial, no appeals process. Compounded medications are prepared by licensed pharmacies but are not FDA-approved products. They are legal when prescribed by a licensed provider and dispensed by a licensed pharmacy — but they are not the same as brand-name Wegovy or Zepbound. Prices typically range from $99–$299/month.
- → GLP-1 Cost Without Insurance: All Your Options — our full pricing breakdown across all major telehealth providers
If you want FDA-approved medication at a lower cash price
Ro offers FDA-approved GLP-1 medications including Wegovy (injectable and pill), Zepbound, and Foundayo (orforglipron) — an oral GLP-1 approved April 2026 for chronic weight management. Their Ro Body membership starts at $39 for the first month, then as low as $74/month with an annual plan paid upfront — medication costs are separate. Ro works with commercial insurance for prior authorization on FDA-approved medications but does not currently coordinate coverage for government insurance plans like Medicaid. For Medicaid enrollees who also have a separate commercial plan, or who want to explore the FDA-approved cash-pay route, Ro is worth checking.
Ro Body — FDA-Approved GLP-1s Starting at $39/month
Wegovy (injectable + pill), Zepbound, and Foundayo available. First month $39, then as low as $74/mo with annual plan. No Medicaid coordination required — this is a cash-pay program. Worth checking if your Medicaid path is closed.
See Ro's current pricing and options →If you're not sure which path is right for you
The people who get stuck are the ones who stop after a single "no." The people who get started are the ones who find the path that actually fits.
Still not sure which GLP-1 program is right for you?
The quiz asks about your state, insurance situation, budget, and medical history, then routes you to the path most likely to work — whether that's Medicaid navigation, a diagnosis-pathway strategy, or a cash-pay provider.
Take the free GLP-1 matching quiz →How we verified every state in this tracker
We built this tracker because we couldn't find one that combined state-level coverage, diagnosis pathway exceptions, recent changes, and actionable next steps in one verified resource.
Source hierarchy
Our verification follows this priority order:
Coverage Reach methodology
Coverage Reach = (adult Medicaid enrollees in states with FFS obesity GLP-1 coverage ÷ total adult Medicaid enrollees nationally) × 100. Using CMS Medicaid enrollment data: ~7.8 million out of ~39.5 million adult Medicaid enrollees = 19.7%.
Limitations
- MCO formularies may differ from FFS in ways we haven't captured for every state and plan
- We verify monthly, not daily — a state could change policy between verification cycles
- BALANCE participation will change the landscape once states begin joining; we'll update as participation is confirmed
- States marked with ⚠️ need additional verification against their current PDL
- We do not have staffed reporters in all 50 states — our verification relies on public documents, official bulletins, and published reporting
Download and audit
We publish the raw data behind this tracker as a downloadable CSV and maintain a public GitHub repository.
Medicaid GLP-1 Coverage by State: FAQ
Does Medicaid cover Wegovy for weight loss?
Only in the 13 states that currently cover GLP-1s for obesity treatment under FFS Medicaid. In all other states, Medicaid can exclude Wegovy when prescribed for weight loss. However, Wegovy is covered in all states when prescribed for cardiovascular risk reduction in patients with established CVD and BMI ≥27, or for noncirrhotic MASH with liver fibrosis — because those are separate FDA-approved indications that fall outside the weight-loss exclusion.
Which states cover Wegovy through Medicaid?
As of April 2026, states with confirmed obesity GLP-1 coverage include Delaware, Kansas (restricted), Massachusetts (restricted), Michigan (restricted — morbid obesity only), Minnesota, Mississippi, Missouri, North Carolina, Rhode Island, Tennessee, Utah, Virginia, and Wisconsin. See the full 50-state table above for details and verification notes.
Does Medicaid cover Zepbound for weight loss?
Only in states that cover GLP-1s for obesity. However, Zepbound is covered in all states when prescribed for moderate-to-severe obstructive sleep apnea in adults with obesity — an indication FDA approved in December 2024.
Does Medicaid cover Zepbound for sleep apnea?
Yes — Zepbound is covered for moderate-to-severe obstructive sleep apnea in adults with obesity, which falls outside the weight-loss exclusion. Prior authorization with sleep study documentation is typically required. Your documentation needs to support the moderate-to-severe OSA diagnosis in adults with obesity.
Does Medicaid cover Ozempic for weight loss?
Ozempic is not FDA-approved for weight loss — it is approved for type 2 diabetes. All state Medicaid programs cover Ozempic for diabetes. Some doctors prescribe it off-label for weight loss, but Medicaid is unlikely to cover off-label use.
Can children get GLP-1s through Medicaid?
Federal EPSDT law requires Medicaid to cover medically necessary treatments for enrollees under 21, even in states that exclude weight-loss drugs for adults. Coverage requires a prior authorization submission demonstrating medical necessity — it is not automatic blanket coverage for every child. But a plan cannot simply apply a blanket "we don't cover weight loss drugs" exclusion to someone under 21. If denied, appeal immediately and cite EPSDT — the plan must evaluate medical necessity individually.
How much do I pay if Medicaid covers it?
Medicaid enrollees pay nominal out-of-pocket amounts for covered prescriptions — often a few dollars or less, depending on the state and plan. Federal rules cap copays for many low-income enrollees. If your state covers GLP-1s for your indication, your cost should be minimal.
Does prior authorization mean I'm approved?
No. Prior authorization is a requirement, not an approval. It means your doctor must submit documentation justifying the prescription before the pharmacy can fill it. PA requests can be approved or denied. Approval rates tend to be higher when documentation is thorough on the first submission.
Can my managed care plan cover it if my state FFS program does not?
Possibly. MCO formularies can differ from state FFS policy. Contact your specific managed care plan to ask — don't assume the FFS answer is your final answer.
What do I do after a Medicaid denial?
Request the denial in writing, identify whether it's a plan exclusion, formulary exclusion, or PA denial, check whether another diagnosis pathway applies, and appeal within the stated timeframe. See our step-by-step denial action plan above.
Will BALANCE make my state cover GLP-1s?
Only if your state voluntarily joins the model. BALANCE launched for Medicaid states May 1, 2026, with applications due July 31, 2026. Participation is voluntary — no state is required to join. We'll update this page as state participation is confirmed.
Are there states that cover weight-loss drugs but not GLP-1s?
Yes — at least 7 states cover a non-GLP-1 weight-loss drug (such as orlistat) but do not cover GLP-1 medications for obesity. These are noted in the 50-state table with the 🟠 Non-GLP-1 only designation.
Does Medicaid cover Wegovy for MASH (liver disease)?
Yes. FDA approved Wegovy for noncirrhotic MASH with liver fibrosis in August 2025. Because MASH is not a weight-loss indication, this falls under mandatory Medicaid drug coverage. California's Medi-Cal has explicitly confirmed this pathway remains available even after the state's obesity coverage cut — if the prescriber submits the appropriate diagnosis code. If you have a MASH diagnosis and have been denied Wegovy, ask your doctor to resubmit under the MASH indication.
Does Medicaid cover compounded semaglutide?
No. Compounded semaglutide is not FDA-approved and is not practically available as a Medicaid benefit for obesity treatment. It is available only through cash-pay telehealth providers.
What is the difference between BALANCE and TrumpRx?
TrumpRx is an online platform where consumers can search for discounted self-pay GLP-1 prices negotiated with manufacturers — it routes users to coupons or purchase channels rather than selling medications directly. BALANCE is a CMS program enabling state Medicaid agencies and Medicare Part D plans to cover GLP-1s at negotiated prices. For Medicaid enrollees, BALANCE is the relevant program — TrumpRx pricing is unlikely to be affordable for most people who qualify for Medicaid.
Does Medicaid cover Foundayo (orforglipron)?
Foundayo (orforglipron) by Eli Lilly is an oral GLP-1 FDA-approved April 1, 2026 for chronic weight management in adults with obesity or overweight plus a weight-related comorbidity. Because it is approved for a weight-loss indication, Medicaid coverage remains optional by state. Foundayo is included in the BALANCE Model's negotiated drugs, so states that join BALANCE may cover it. Outside BALANCE, check your state's current PDL. Foundayo is also available through providers like Ro on a cash-pay basis.
Still not sure which GLP-1 program is right for you?
If you've read this far, you already know more about Medicaid GLP-1 coverage than most people — including most of the people answering phones at insurance companies. The question now is which path actually fits your state, your diagnosis, and your budget. No account required. No commitment. Just clarity on your next step.
Take the free 60-second GLP-1 matching quiz →