By The RX Index Editorial Team · Last Verified: March 28, 2026 · Sources: KFF 2025, CMS, NovoCare · Our methodology · Updated monthly
INSURANCE COVERAGE GUIDE — 2026
Does Insurance Cover Wegovy for Weight Loss?
Sometimes — but the honest answer is more useful than that.
Whether insurance covers Wegovy for weight loss depends on your plan type, your employer's benefit design, why your doctor prescribed it, and whether Wegovy is on your specific formulary. If you have commercial insurance through an employer and Wegovy is covered, you could pay as little as $25 per month with the manufacturer savings card. But if your plan excludes anti-obesity medications — and many do — no amount of perfect paperwork will change the answer.
Here's what most pages won't tell you: the same Wegovy prescription can be covered for one person and denied for another on the exact same insurance carrier, because your employer picks which drug categories to include. Knowing that one fact can save you weeks of chasing a dead end.
Below, we break down coverage by insurance type, show you exactly how to check in 10 minutes, walk you through what to do if you're denied, and — if insurance isn't going to work — lay out the cash-pay paths that have made FDA-approved Wegovy dramatically more affordable in 2026.
Affiliate disclosure: The RX Index may earn a commission when you visit a partner through links on this page. This never influences our coverage analysis or editorial ratings. Read our full methodology.
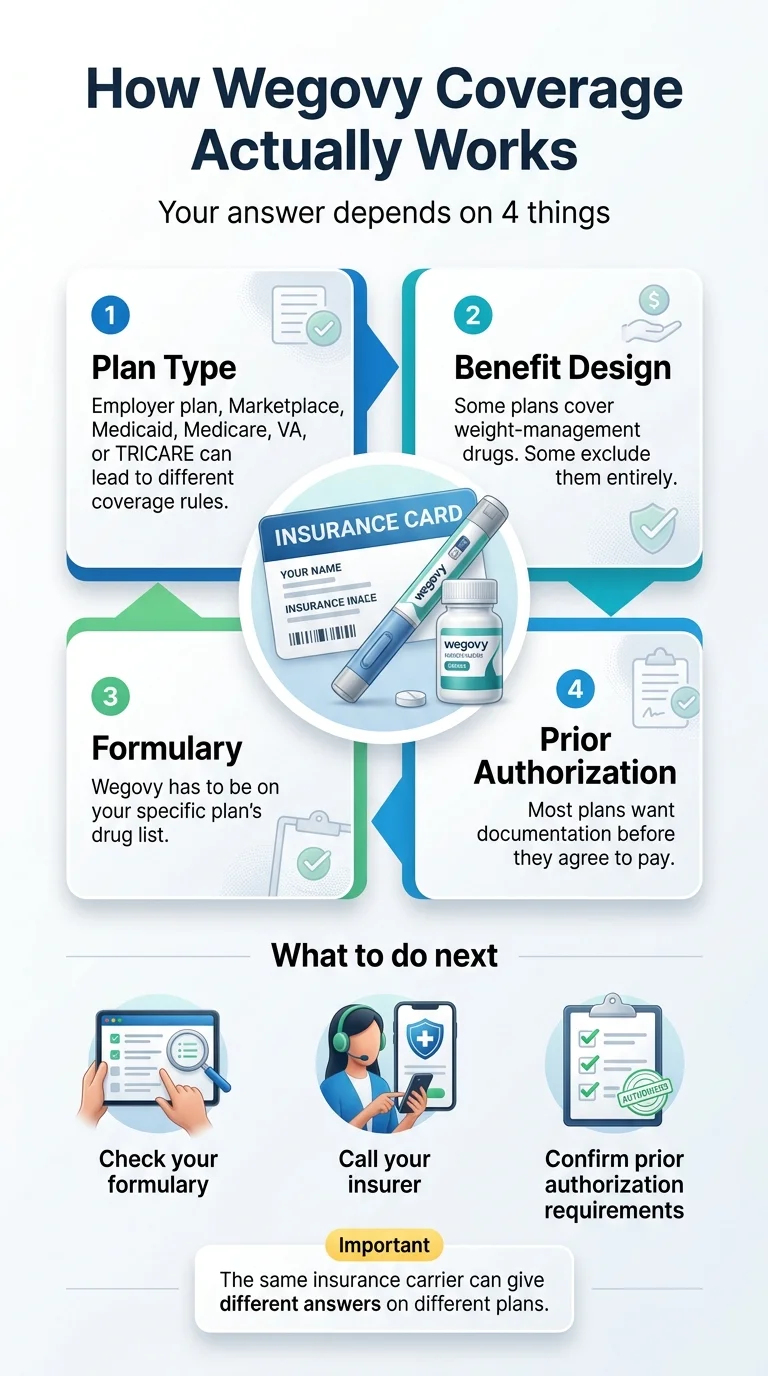
The same insurance carrier gives different answers on different plans — because your employer chose the benefit design. Source: The RX Index, 2026.
Key numbers to know (March 2026)
- Wegovy list price: $1,349/month — but almost nobody pays this
- Commercial insurance + Savings Offer: as low as $25/month (max savings $100/1-mo supply — NovoCare terms)
- NovoCare self-pay Wegovy pill: $149–$299/month
- NovoCare self-pay Wegovy injection: $199–$349/month
- Medicare GLP-1 Bridge (July 1–Dec. 31, 2026): $50/month copay — CMS details
Wegovy Coverage at a Glance: What You'll Likely Pay in 2026
Start here. This table answers the question for most readers based on insurance type.
| Insurance Type | Usually Covered? | What Decides It | Fastest Next Step |
|---|---|---|---|
| Employer-sponsored | Maybe — 43% of large firms (5,000+) cover it; 19% of firms with 200+ workers (KFF 2025) | Your employer's benefit design + plan formulary | Use our phone script |
| ACA Marketplace / individual | Unlikely — ~1% of federal Marketplace plans covered it (KFF 2024) | Plan formulary; ACA does not require obesity drug coverage | Check formulary; self-pay likely your fastest path |
| Medicaid | State-dependent — 13 fee-for-service state programs cover GLP-1s for obesity (KFF, Jan. 2026) | Your state's Medicaid formulary and managed-care plan | Call your managed care plan directly |
| Medicare | Not for weight loss (standard Part D) — but Bridge program July–Dec 2026 at $50/month | Bridge eligibility: BMI criteria + qualifying conditions | See Medicare section |
| TRICARE / VA | Possible with prior authorization; VA covers through MOVE! program | Plan-specific formulary and clinical criteria | Contact TRICARE pharmacy or VA provider |
Your Insurance Type Determines Almost Everything
The single biggest mistake people make is Googling “does Blue Cross cover Wegovy?” as if every BCBS plan gives the same answer. They don't. The same carrier offers hundreds of different plan designs, and your employer — or the Marketplace — picks which drug categories to include. Start with your insurance type instead.
If You Have Employer-Sponsored Insurance
Most common situationIn KFF's 2025 Employer Health Benefits Survey, 19% of firms with 200+ workers said their largest plan covers GLP-1s for weight loss. Among firms with 5,000+ workers, 43% said it does — up from 28% in 2024. Real momentum, but the majority of employer plans still don't cover these medications for weight loss.
What decides it: Your employer's benefit design. When your company set up the plan, they chose which drug categories to include. If they excluded “anti-obesity medications” as a benefit category, Wegovy for weight loss is off the table regardless of your medical case. That's not the insurer being difficult — it's a plan design choice your employer made.
Your fastest move — call and ask these 3 questions:
- “Is Wegovy (semaglutide) on my plan's formulary?”
- “Does my plan cover medications for weight management, or are anti-obesity drugs excluded as a benefit category?”
- “If covered, does Wegovy require prior authorization?”
If question 2 is “excluded,” your best next step is asking HR to add coverage (Novo Nordisk provides a template letter your doctor can use) or exploring self-pay options below.
If You Have an ACA Marketplace or Individual Plan
Coverage is rareCoverage is rare. In KFF's 2024 analysis of federal Marketplace plans, about 1% covered Wegovy. The Affordable Care Act does not require insurers to cover obesity medications, so most individual plans simply don't.
Your fastest move: Check your plan's drug formulary online. If Wegovy isn't listed and anti-obesity drugs are excluded, an appeal is unlikely to succeed. Self-pay is probably your fastest path.
If You’re on Medicaid
State-dependentKFF found 13 fee-for-service state Medicaid programs covering GLP-1s for obesity treatment as of January 2026. Managed-care plan coverage can differ from fee-for-service. California's Medi-Cal stopped covering Wegovy for weight management effective January 1, 2026, while the CMS BALANCE Model may expand Medicaid access starting May 2026.
Your fastest move: Check your state Medicaid formulary or call your managed care plan directly.
If You're on Medicare
Changing fast in 2026Medicare has been legally prohibited from covering weight-loss-only medications since 2003. Standard Medicare Part D does not cover Wegovy for weight loss.
However, Medicare Part D may already cover Wegovy when prescribed for cardiovascular risk reduction (FDA-approved March 2024) or MASH (FDA-approved August 2025, injection only). And the Medicare GLP-1 Bridge launches July 1, 2026 with a $50/month copay.
→ Jump to the full Medicare breakdownFor a deeper dive on insurance across all GLP-1 medications, see: How to Get Insurance to Cover GLP-1 Medications.
What Actually Decides Whether Your Insurance Covers Wegovy
Understanding these five factors will save you more time than anything else on this page.
Your employer’s benefit design matters more than your insurer’s name
“I have Blue Cross” doesn’t mean much by itself. BCBS offers thousands of plan configurations. Your employer chose which drug classes to include. Two people at different companies can both have BCBS and get opposite coverage answers.
Wegovy has to be on your specific plan’s formulary
A formulary is your plan’s approved drug list. Wegovy may be on some formularies and not others — even within the same carrier. If it’s not listed, you may be able to request a non-formulary exception, but success varies.
Nearly every plan requires prior authorization
Prior authorization (PA) means your doctor must submit documentation proving you meet the plan’s clinical criteria before the insurer agrees to pay. This is standard for Wegovy and virtually unavoidable. We walk through exactly what your doctor needs to submit below.
The reason Wegovy was prescribed changes everything
Wegovy has multiple FDA-approved indications, and your coverage may depend on which one applies. If your plan excludes weight-loss medications but your doctor determines you also qualify under the cardiovascular or MASH indication, the same prescription may be coverable under a different diagnosis code. This isn’t a loophole — it’s legitimate medical practice when you genuinely have the qualifying condition.
“Covered” doesn’t always mean affordable
Even when Wegovy is on your formulary, it’s often on a specialty tier (Tier 4+), which can mean 25–33% coinsurance instead of a flat copay. On a $1,349 list price, 25% coinsurance is $337/month before savings programs. That’s where the Wegovy Savings Offer helps — eligible commercially insured patients can bring cost to as low as $25/month. But it cannot be used with Medicare, Medicaid, TRICARE, or other government programs.
Wegovy's FDA Indications — and How They Affect Coverage
| FDA-Approved Use | Who Qualifies | Coverage Impact |
|---|---|---|
| Chronic weight management | Adults with BMI ≥30, or ≥27 with ≥1 weight-related condition; injection also approved ages 12+ | Varies — plan must cover anti-obesity drugs |
| Cardiovascular risk reduction | Adults with established CV disease + obesity or overweight | Higher — many plans cover CV indications even when they exclude weight-loss drugs |
| MASH (injection only) | Adults with moderate-to-advanced liver scarring | Emerging — FDA-approved Aug. 2025; formulary placement still catching up |
Important note: The Wegovy injection and tablets do not have identical FDA-approved indications. The injection is approved for adult and pediatric (12+) weight management, CV risk reduction, and MASH. The tablets are approved for adult weight management and adult CV risk reduction, but not pediatric use and not MASH. Always check for the specific form when verifying coverage.
How to Check If Your Plan Covers Wegovy in 10 Minutes
You don't need to spend hours on hold. Follow these steps in order.

6 steps to verify Wegovy coverage and prior authorization requirements. Source: The RX Index, 2026.
Check your formulary online
Log in to your insurer's website and search “Wegovy” or “semaglutide” in the pharmacy or formulary section. Note whether it’s listed and what tier it’s on.
Look for benefit exclusions
Search your Summary of Benefits and Coverage for language about “anti-obesity medications,” “weight management drugs,” or “weight loss medications.” If excluded, Wegovy for weight loss won’t be covered no matter what else you do.
Call member services
Use the number on the back of your card. Ask: Is Wegovy on my formulary? Are anti-obesity drugs excluded? What tier and cost? Does it require prior authorization? Are there step-therapy requirements? See the full script below.
Ask about prior authorization requirements
If covered, ask: “What clinical criteria does my plan require for prior authorization?” Common requirements: BMI of 30+ (or 27+ with comorbidities), documented diet and exercise history, sometimes step therapy.
Ask the pharmacy to run a test claim
Your pharmacist can submit a test claim to see what your plan will pay before you fill the prescription, revealing your real out-of-pocket cost.
Get everything in writing
Ask for written confirmation or note the call reference number. This protects you if a dispute arises later.
Rather have someone handle this for you?
Ro offers a free GLP-1 Insurance Coverage Checker that contacts your plan directly and sends you a personalized report — coverage details, PA requirements, and cost estimates — without you sitting on hold. If you continue with Ro for treatment, Ro Body membership is $45 for the first month and $145/mo thereafter; medication costs are billed separately.
Get Your Free Wegovy Coverage Report →Exactly What to Say When You Call Your Insurance Company
Many readers call their insurer, ask a vague question, get a vague answer — and are blindsided at the pharmacy. This script prevents that.
The 60-second phone script
“Hi, I'm calling about prescription drug coverage for a specific medication. The drug is Wegovy — W-E-G-O-V-Y — brand name Wegovy, generic name semaglutide. I need five things:
First, is Wegovy on my plan's formulary?
Second, does my plan cover medications for weight management, or are anti-obesity drugs excluded as a benefit category?
Third, if covered, what tier is it on, and what's my copay or coinsurance?
Fourth, does Wegovy require prior authorization?
Fifth, are there step-therapy requirements — meaning, do I need to try a different medication first?”
What the jargon actually means
| They Say | It Means | What to Do |
|---|---|---|
| Not on formulary | Your plan's drug list doesn't include Wegovy | Ask about a non-formulary exception |
| Excluded benefit | Your plan chose not to cover anti-obesity drugs at all | No PA will fix this — pivot to HR exception, another indication, or self-pay |
| Prior authorization required | Doctor must submit documentation proving medical necessity first | Have your doctor submit PA with complete docs (see checklist below) |
| Step therapy required | Try a cheaper drug first and document it didn't work | Ask which drug and for how long |
| Specialty tier | High-cost tier with coinsurance instead of a flat copay | Ask the coinsurance percentage and calculate your real cost |
| Not medically necessary | Insurer says you don't meet clinical criteria | Often fixable with better documentation — see appeal section |
What Your Doctor Needs for Wegovy Prior Authorization
If your plan covers Wegovy and requires PA (nearly all do), your doctor needs to build a strong case. Here's what insurers typically want — and where things break down.

Incomplete documentation is the most common fixable cause of Wegovy prior authorization denials. Source: The RX Index, 2026.
| What the Insurer Wants | Who Provides It | Where It Usually Goes Wrong |
|---|---|---|
| BMI documentation | Doctor’s chart notes | BMI not documented at a recent visit; old records submitted |
| Diagnosis code | Doctor | Wrong ICD-10 code (e.g., “overweight” instead of “obesity with comorbidity”) |
| Comorbidities | Doctor’s records + labs | Comorbidities exist but aren’t in the submitted chart notes |
| Prior weight-loss attempts | Doctor’s notes | No documentation of prior diet, exercise, or behavioral interventions |
| Lab results | Doctor/lab | Labs outdated or missing key markers (A1C, lipid panel, liver function) |
| Step therapy compliance | Doctor/pharmacy records | Plan required trying a cheaper drug first and it wasn’t documented |
| Letter of medical necessity | Doctor | Letter is generic; doesn’t address the plan’s exact criteria |
The most common fixable mistake
Incomplete documentation. A surprising number of PA denials happen not because the patient doesn't qualify, but because the paperwork was missing something. Before your doctor submits, confirm they're including: current BMI with a recent date, all relevant comorbidities with supporting labs, documentation of prior weight-management interventions, and a patient-specific letter of medical necessity addressing the plan's criteria point by point.
Why Wegovy Gets Denied — and What You Can Actually Do About It
Getting a denial feels personal. Understanding why is the fastest way to figure out whether it's worth fighting.

Get the denial reason in writing first — it tells you which path to take. Source: The RX Index, 2026.
| Denial Reason | Fixable? | Your Best Move |
|---|---|---|
| Plan excludes anti-obesity drugs entirely | Usually not through appeal | Ask HR to add coverage; check if another indication applies; explore self-pay |
| Wegovy is not on formulary | Sometimes | Doctor submits non-formulary exception showing medical necessity |
| Don’t meet BMI or comorbidity criteria | Maybe — if documentation was incomplete | Resubmit with complete records |
| PA paperwork was incomplete | Yes — most common fixable denial | Resubmit with full documentation; see checklist above |
| Plan requires step therapy | Yes — but takes time | Try the required first-line treatment, document it, resubmit |
| Plan changed or employer dropped coverage | Not through appeal | Self-pay; new employer plan at next enrollment |
| Prescribed for unrecognized or off-label use | Depends | Work with doctor to align with an FDA-approved use your plan covers |
A pattern we see constantly
Many people get denied and assume it's final. It often isn't — especially when the denial was for incomplete documentation rather than a true plan exclusion. Appeals succeed regularly when you resubmit with better paperwork and a specific letter of medical necessity. But if your plan has a blanket exclusion for anti-obesity drugs, an appeal can't fix a structural benefit-design choice. That's not a paperwork problem — it's a benefit problem.
Get the denial reason in writing first.
That single document tells you whether to fight or pivot. It's the difference between a three-week fix and three months of wasted effort.
How to Appeal a Wegovy Denial
If your denial is fixable — not a blanket benefit exclusion — here's how to fight it.
When to appeal
- • Denial was for incomplete documentation
- • Unmet criteria you can demonstrate with records
- • Step therapy you can complete and document
- • Formulary exception your doctor can medically justify
When to skip the appeal and pivot
- • Plan explicitly excludes anti-obesity medications as a benefit category
- • Better path: ask HR to add benefit
- • Check if another FDA-approved indication applies
- • Move to self-pay
Get the denial in writing with the specific criteria and reason
Gather documentation: current BMI, comorbidities with labs, prior interventions, new clinical info
Doctor writes a patient-specific letter of medical necessity addressing the plan’s denial criteria point by point
File the internal appeal within your plan’s deadline (typically 60–180 days)
If internal appeal denied, request external review — an independent third party that can overturn decisions internal appeals won’t
The HR exception route
If your employer plan excludes weight-loss drugs, your doctor can submit a coverage request directly to HR. Novo Nordisk offers a template letter for this. With growing evidence that obesity treatment reduces long-term healthcare costs, more employers are reconsidering these exclusions every year.
How Much Does Wegovy Cost With Insurance?
Even when insurance says “yes,” the out-of-pocket number catches people off guard.
| Scenario | What You'll Likely Pay | Notes |
|---|---|---|
| Commercial insurance + Savings Offer | As low as $25/month | Max savings $100/1-mo supply. Commercial only. |
| Commercial insurance, no savings offer | $100–$700+/month | Depends on tier, coinsurance, deductible |
| Commercial, high-deductible plan | Full list price until deductible met | You may owe $1,349/month until deductible satisfied |
| Medicare (CV risk or MASH indication) | Varies by Part D plan | Typically Tier 3+; 25–33% coinsurance common |
| Medicare GLP-1 Bridge (July–Dec. 2026) | $50/month | For weight loss; specific criteria required |
When paying cash is actually cheaper than using insurance
If your plan covers Wegovy on a specialty tier with 33% coinsurance, you could owe ~$445/month. Compare that to $149–$299/month for the pill through NovoCare self-pay — going out-of-pocket may save you money, especially before you've met your deductible. The trade-off: self-pay costs don't count toward your deductible or out-of-pocket maximum.
For a full pricing breakdown across all GLP-1 medications, see: Cheapest GLP-1 Without Insurance (2026).
Wegovy Pill vs. Injection: Does It Affect Coverage?
Since the Wegovy pill launched in late 2025, this is one of the most common questions. The pill and injection do not have identical FDA-approved indications — which matters for coverage.
| Wegovy Pill | Wegovy Injection | |
|---|---|---|
| Format | Daily tablet | Weekly self-injection |
| FDA-approved indications | Adult weight management, adult CV risk reduction | Adult + pediatric (12+) weight management, CV risk reduction, MASH |
| NovoCare self-pay (starter) | $149/mo | $199/mo intro through June 30, 2026 |
| NovoCare self-pay (maintenance) | $299/mo | $349/mo |
| Refrigeration | No | Yes (before first use) |
| Mean weight loss (FDA label) | 13.6% at week 64 | 14.9% at week 68 |
Our take: If you're paying cash, the pill is the better deal — cheaper at every dose, no needles, no refrigeration. If you have insurance with a good copay, it's personal preference. Always check your formulary for the specific form prescribed.
Wegovy HD (7.2 mg injection, FDA-approved March 2026) is for patients who've tolerated 2.4 mg for 4+ weeks and need additional weight loss. More on the pill: How to Get the Wegovy Pill Online.
What If Insurance Won't Cover Wegovy?
If you've confirmed your plan won't cover Wegovy for weight loss, you have real options. And they're more affordable than even a year ago.
Check if another indication changes the answer
If you have established cardiovascular disease, your doctor may prescribe Wegovy for CV risk reduction — covered by many plans even when they exclude weight-loss drugs. If you have MASH (moderate-to-advanced liver scarring), that’s another coverable indication. These aren’t workarounds — they’re legitimate medical uses when you have the qualifying condition.
Manufacturer self-pay through NovoCare
Novo Nordisk's NovoCare Pharmacy offers reduced pricing for eligible self-pay patients not enrolled in Medicare, Medicaid, VA, DOD/TRICARE, or similar government programs.
Wegovy pill:
- Starter (1.5 mg): $149/month
- 4 mg: $149/mo through April 15, 2026
- Maintenance (9 mg, 25 mg): $299/month
Wegovy injection:
- Starter: $199/mo intro through June 30, 2026
- All other doses: $349/month
Government-program beneficiaries: NovoCare self-pay terms explicitly exclude government-program enrollees. Ask your pharmacist about cash pricing available to you specifically.
Ask HR to add coverage
If your employer plan is the barrier, this is worth trying. More employers are adding GLP-1 coverage every year, and the cost argument is in your favor — treating obesity reduces long-term spending on diabetes, cardiovascular disease, and joint problems.
Use HSA or FSA funds
Wegovy may qualify for HSA/FSA reimbursement when prescribed to treat a diagnosed condition such as obesity, subject to IRS rules and your plan administrator's documentation requirements. See our guides: Can I Use HSA for GLP-1? and Can I Use FSA for GLP-1?
A note on compounded semaglutide
You'll see compounded semaglutide advertised for less. We want to be straightforward: compounded semaglutide is not FDA-approved and is not the same product as brand-name Wegovy. The FDA has flagged safety and consistency concerns with some compounded products. With FDA-approved Wegovy pill now available from $149/month through NovoCare, the price gap has narrowed significantly. If budget is your primary constraint and you've discussed the tradeoffs with a doctor, some providers prescribe compounded semaglutide through licensed pharmacies. Compare options on our provider guide.
Insurance said no and you're ready to move forward?
Ro checks your coverage for free — and if coverage doesn't pan out, connects you directly with FDA-approved Wegovy at competitive self-pay pricing. Ro Body membership is $45 for the first month and $145/mo thereafter; medication is billed separately.
See Your Wegovy Coverage and Pricing Options on Ro →Does Medicare Cover Wegovy for Weight Loss?
This section is changing fast. Here's exactly where things stand as of March 2026.
Current rules (as of March 2026)
- Standard Medicare Part D: Does NOT cover Wegovy for weight loss — legally prohibited since 2003. The Wegovy Savings Offer also cannot be used with Medicare.
- Medicare Part D for CV risk reduction: MAY cover Wegovy — FDA-approved March 2024. Coverage depends on your specific Part D plan's formulary.
- Medicare Part D for MASH: MAY cover Wegovy injection — FDA-approved August 2025. Formulary placement still developing.
The Medicare GLP-1 Bridge (July 1 – December 31, 2026)
CMS released detailed FAQs on March 3, 2026 confirming this temporary program:
- Covers: Wegovy (injection and tablets) and Zepbound for weight reduction
- Your cost: $50/month copay
- Eligibility: Medicare Part D enrollees with BMI ≥35 or BMI ≥30 with HFpEF/uncontrolled HTN/CKD stage 3a+ or BMI ≥27 with prediabetes/prior MI/prior stroke/symptomatic PAD
- How it works: Doctor submits PA to a CMS central processor (Humana), not your Part D plan
- Key detail: The $50 copay does not count toward your Part D deductible or out-of-pocket cap
- Duration: July 1–December 31, 2026 only. Transitions to the voluntary BALANCE Model in January 2027
Might qualify for the Bridge?
Talk to your doctor now about documenting your BMI and qualifying conditions so paperwork is ready when the program launches July 1, 2026.
Can't wait until July?
Ask your pharmacist about current cash pricing available to Medicare beneficiaries. Pricing may differ from manufacturer promotional programs depending on your eligibility status.
Wegovy vs. Other GLP-1s: Which Is Easiest to Get Covered?
If Wegovy coverage looks difficult, here's how alternatives compare.
| Medication | FDA-Approved For | Coverage for Weight Loss | Typical Self-Pay |
|---|---|---|---|
| Wegovy (semaglutide) | Weight loss, CV risk, MASH | Moderate — strongest with CV or MASH indication | Pill: $149–$299/mo · Injection: $199–$349/mo |
| Zepbound (tirzepatide) | Weight loss, sleep apnea | Mixed — CVS Caremark dropped it mid-2025, directing to Wegovy | Vials: $299–$449/mo via LillyDirect |
| Ozempic (semaglutide) | Type 2 diabetes | High for diabetes; very low for weight loss (not approved for it) | $199–$349/mo via NovoCare |
| Mounjaro (tirzepatide) | Type 2 diabetes | High for diabetes; low for weight loss (not approved for it) | ~$549/mo via LillyDirect |
Wegovy has more FDA-approved indications relevant to insurance than any other GLP-1 for weight loss — three distinct coverage pathways. And CVS Caremark chose Wegovy over Zepbound as its preferred weight-loss GLP-1, giving it favorable formulary placement for many employer plans.
The Real Talk: Is Fighting Insurance Worth It?
A perfect prior authorization does not override a true plan exclusion. If your employer chose a benefit design that excludes anti-obesity drugs, no paperwork fixes that. But spotting that early saves you weeks — and tells you to pivot to an HR exception request, a different FDA-approved indication, or self-pay instead of chasing a dead end.
If your plan covers Wegovy but requires PA
Fight for it. With complete documentation, PA approvals are common.
If your plan excludes anti-obesity drugs entirely
Don’t chase a PA that can’t work. Check whether you qualify under the CV or MASH indication. If not, self-pay through NovoCare or an authorized partner is your fastest path.
If you’re on Medicare
Prepare for the GLP-1 Bridge in July 2026. If you can’t wait, ask your pharmacist about available cash pricing.
Three Real-World Scenarios
These are composites based on common situations across our readership.
Jamie, employer-sponsored BCBS. BMI 34 with documented hypertension and prediabetes. Called insurer — Wegovy on formulary at Tier 3. Doctor submitted PA with current BMI, labs, and diet history. Approved in 8 business days. With Savings Offer: $25/month.
Time to first dose: ~3 weeks.
David, employer UnitedHealthcare. BMI 32 with sleep apnea. First PA denied — documentation of prior weight-management attempts was thin. Doctor resubmitted with two years of supervised diet counseling notes plus updated labs. Internal appeal approved. Pays $25/month with savings card.
Time to first dose: ~7 weeks. The fix was better paperwork.
Rachel, ACA Marketplace plan. Wegovy not on formulary, anti-obesity drugs excluded. Rather than chase an appeal that couldn’t succeed, she started the Wegovy pill through NovoCare at $149/month. Now on maintenance at $299/month.
Time from decision to first dose: 4 days. Sometimes the fastest path is the one that doesn’t involve insurance at all.
What to Expect When You Start Wegovy
Dose schedule — injection
Dose schedule — pill
Pill: $149/mo starter, $299/mo maintenance (NovoCare self-pay)
Realistic weight-loss expectations
Per FDA labeling: Wegovy injection 2.4 mg produced mean 14.9% body-weight reduction at 68 weeks. Wegovy tablets 25 mg produced mean 13.6% at 64 weeks. For someone at 250 lbs, that's roughly 34–37 pounds. Most people see modest changes during dose escalation and more significant results at maintenance dose.
Plan for cost increases: If paying cash, your cost rises with your dose. Budget for month 4, not just month 1.
Your 3-Minute Decision Framework
Employer-sponsored insurance
- Call insurer → use our script (5 min)
- Covered → doctor submits PA → enroll in Savings Offer ($25/mo)
- Excluded → ask HR to add coverage + explore self-pay
- PA denied → appeal with better docs OR pivot to self-pay
ACA Marketplace / Medicaid / no insurance
- Check formulary (2 min online)
- Not covered → explore NovoCare self-pay from $149/mo
- Income qualifies → ask about financial assistance programs
Medicare
- Check if you qualify under CV risk or MASH through Part D
- If not → prepare for GLP-1 Bridge (July 2026, $50/mo)
- Can’t wait → ask pharmacist about available cash pricing
The $1,349 list price that drove you to search this question does not reflect what most commercially insured or eligible self-pay patients actually pay. Between insurance and savings programs, manufacturer self-pay, and the upcoming Medicare Bridge, there are more paths to affordable Wegovy than ever before. The people who get the best results pick a path and start.
One starting point — every path covered
Ro checks your insurance for free. Covered? Their team handles prior authorization. Not covered? They connect you with competitive self-pay pricing for FDA-approved Wegovy. Ro Body membership: $45 first month, $145/mo thereafter; medication is billed separately.
Check Your Wegovy Options on Ro →Not sure which GLP-1 fits you? Take the free 60-second quiz →How We Verified This Information
Sources checked for this guide: FDA labeling for Wegovy injection and tablets, CMS Medicare GLP-1 Bridge FAQs (March 3, 2026), KFF 2025 Employer Health Benefits Survey, NovoCare savings and self-pay terms (verified March 2026), IRS medical expense guidance, Novo Nordisk press releases on pricing and Wegovy HD approval.
Changes most often: Employer formularies, savings-card terms, state Medicaid formularies, Medicare Part D placements. Last verified: March 28, 2026. Reviewed monthly.
Medical disclaimer: This content is for informational purposes only and does not constitute medical or insurance advice. Coverage decisions are made by your individual insurance plan. Always consult your healthcare provider and insurance company for guidance specific to your situation.
Frequently Asked Questions
Does insurance cover Wegovy for weight loss?
Sometimes. In KFF’s 2025 survey, 43% of firms with 5,000+ workers said their largest plan covers GLP-1s for weight loss; among firms with 200+ workers, 19%. ACA Marketplace and Medicaid coverage is much rarer — about 1% of federal Marketplace plans covered Wegovy in KFF’s 2024 analysis.
What insurance covers Wegovy?
Major commercial carriers — BCBS, Aetna, Cigna, UnitedHealthcare — offer plans that include Wegovy. But coverage is plan-specific, not carrier-wide. Two people with the same carrier at different employers can get opposite coverage answers because their employers chose different benefit designs.
How do I get insurance to cover Wegovy?
Check your formulary, confirm anti-obesity drugs aren’t excluded as a benefit category, and have your doctor submit prior authorization with your current BMI, comorbidities, prior weight-management interventions, and a patient-specific letter of medical necessity.
How much does Wegovy cost with insurance?
With commercial insurance and the Wegovy Savings Offer: as low as $25/month (maximum savings $100 per 1-month supply). Without the savings offer: $100–$700+ depending on your plan’s tier structure and coinsurance rate. The savings offer cannot be used with Medicare, Medicaid, or other government programs.
Does Medicare cover Wegovy for weight loss?
Not under standard Medicare Part D. However, a temporary CMS GLP-1 Bridge program runs July 1–December 31, 2026 at a $50/month copay for eligible beneficiaries (BMI ≥35, or ≥30 with HFpEF/uncontrolled HTN/CKD 3a+, or ≥27 with prediabetes/prior MI/prior stroke/symptomatic PAD). Medicare Part D may cover Wegovy prescribed for cardiovascular risk reduction or MASH depending on your Part D plan’s formulary.
Does Medicaid cover Wegovy?
State-dependent. KFF found 13 fee-for-service state Medicaid programs covering GLP-1s for obesity as of January 2026. Managed-care plans within a state may differ from fee-for-service. California’s Medi-Cal stopped covering Wegovy for weight management effective January 1, 2026.
Can Wegovy be covered for cardiovascular risk instead of weight loss?
Yes. Wegovy was FDA-approved for cardiovascular risk reduction in March 2024. Many plans cover it for this indication even when they exclude weight-loss drugs. If you have established cardiovascular disease plus obesity or overweight, ask your doctor whether the CV indication applies to your clinical situation.
Can Wegovy be covered for MASH?
Potentially. The Wegovy injection was FDA-approved for moderate-to-advanced MASH (liver scarring) in August 2025. Formulary placement for this indication is still developing across plans as of March 2026. Coverage depends on your specific Part D or commercial plan.
Why was my Wegovy prior authorization denied?
Common reasons: plan excludes anti-obesity drugs as a benefit category (unfixable through PA), incomplete documentation (most common fixable reason), unmet BMI or comorbidity criteria, step therapy required, or the wrong FDA indication was used. Get the specific denial reason in writing before deciding whether to appeal.
Is the Wegovy pill covered the same as the Wegovy injection?
Not necessarily. The pill and injection share some but not all FDA-approved indications — the injection covers adult and pediatric (12+) weight management, CV risk reduction, and MASH; the tablets cover adult weight management and adult CV risk reduction only. Plans may also tier them differently, which changes your copay.
Does the Wegovy savings card work without insurance?
With different terms. Commercially insured patients without coverage can access reduced self-pay pricing. Government-program beneficiaries (Medicare, Medicaid, VA, TRICARE) are not eligible for the NovoCare savings offer, even if they elect to pay out of pocket.
Is Wegovy covered by Blue Cross Blue Shield?
Some BCBS plans cover it; others don’t. BCBS is a network of independent local plans, each offering hundreds of plan designs. The answer depends on your specific plan and employer’s benefit choices — not the BCBS name itself. Call the number on your insurance card and ask the three questions in our phone script above.
What’s the cheapest way to get Wegovy?
For commercially insured patients: insurance coverage plus the Wegovy Savings Offer can bring monthly cost to $25. For self-pay patients not on government programs: NovoCare pharmacy offers the Wegovy pill starting at $149/month for starter doses and $299/month for maintenance, and the injection starting at $199/month intro (through June 30, 2026) and $349/month for other doses.
Is Wegovy HSA/FSA eligible?
It may qualify when prescribed for a diagnosed condition like obesity, subject to IRS rules and your plan administrator’s documentation requirements. Confirm with your HSA/FSA administrator before assuming eligibility. For full detail, see our guides on HSA and FSA eligibility for GLP-1 medications.
Will insurance cover Wegovy for prediabetes?
Wegovy isn’t FDA-approved specifically for prediabetes. But prediabetes alongside qualifying obesity (BMI 30+, or 27+ with conditions) can strengthen your prior authorization as a documented comorbidity. If you also have established cardiovascular disease, the CV risk reduction indication may open a stronger coverage path.
Affiliate disclosure: The RX Index may earn a commission when you visit a partner through links on this page. This never influences our coverage analysis or editorial ratings. Read our full editorial policy.
© 2026 The RX Index. This page is for informational purposes only and does not constitute medical or insurance advice.
By The RX Index Editorial Team · Last updated March 28, 2026 · More GLP-1 Guides →
Related Guides