GLP-1 Providers That Accept UnitedHealthcare: What Actually Works in 2026
The most important thing to know first
“Accepts UnitedHealthcare” means three completely different things depending on who says it. Some providers bill UHC directly for your visits. Others only help you use UHC to cover the medication at the pharmacy. And others don't touch your insurance at all. The wrong choice costs you months and potentially hundreds of dollars.
We checked each provider against UHC's own network resources, their public insurance claims, and their terms of service. Here's what we found:
True UHC in-network online program
Shapely is the clearest publicly documented in-network option for commercial UHC PPO members — $49/month membership plus copays, currently in CA, FL, NY, and TX. Accomplish Health also claims UHC in-network status (announcement September 2023 — confirm current status directly).
Help getting UHC to cover brand-name Wegovy or Zepbound
Ro has the strongest insurance concierge — they call UHC on your behalf, for free, and handle prior authorization paperwork. WeightWatchers Clinic and Noom also offer insurance coordination as part of their programs.
UHC excludes weight-loss drugs on your plan
Compounded GLP-1 programs like MEDVi and Eden offer medication-included pricing with no insurance needed. Compounded medications are not FDA-approved as finished products.
The key constraint: Many UHC employer plans exclude anti-obesity GLP-1 medications entirely unless your employer specifically opted in. That's the single most important thing to check before choosing a provider — and we'll show you how to check in under 10 minutes.
Jump to: Full comparison · What “accepts” means · Which route fits you · UHC coverage policy · How to check your plan · If UHC says no · Cash-pay options · FAQ

GLP-1 Providers That Accept UnitedHealthcare: The Full Comparison
We split every provider into one of three categories based on what they actually do with your UHC card. This is the distinction that saves you from wasting weeks on the wrong program.
Sources cited per row. Rows marked NEEDS VERIFICATION should be confirmed directly with the provider. Provider-stated claims are labeled; independently confirmed claims are noted separately.
Category 1 — True UHC In-Network Options
These providers bill UnitedHealthcare directly for your visits
| Provider | UHC Status | Prior Auth Help | Starting Fee | States |
|---|---|---|---|---|
| Shapely | In-network UHC PPO (provider-stated, current) | Yes | $49/mo + copays | CA, FL, NY, TX |
| Accomplish HealthNEEDS VERIFICATION | Claims UHC in-network (Sept. 2023 — confirm directly) | Yes | Needs verification | Needs verification |
| UHC Provider Directory | In-network by definition | Varies by provider | Copay only | All states |
Shapely source: getshapely.com/weightloss/insurance/unitedhealthcare. Accomplish source: accomplish.health/uhcannouncement (dated Sept. 25, 2023). UHC directory: uhc.com/find-a-doctor.
Category 2 — Insurance Navigation Programs
Cash-pay program fee, but they help you use UHC for the medication
| Provider | How UHC Is Used | Prior Auth Help | Program Fee |
|---|---|---|---|
| Ro | Insurance concierge calls UHC, submits PA, handles denials. Membership is cash-pay. | Yes — strongest PA handling | $45 first mo, then $145/mo |
| WeightWatchers Clinic | Insurance coordinators work with commercial plans for medication coverage | Yes | $25 first mo, then $74/mo (Med+) |
| Noom ⚠️ | Prescriptions go to your pharmacy; you use insurance there | Yes — care team assists (up to 14 days per Noom). Not available in AL or VA. | Needs verification — check noom.com |
| Sesame | Program is cash-pay; insurance accepted for medications at pharmacy | Limited | $59/mo with annual plan |
Sources: ro.co/weight-loss/pricing; weightwatchers.com/us/weight-loss-medication; noom.com branded meds FAQ; sesamecare.com.
Category 3 — Cash-Pay Fallback Programs
No UHC interaction — for members whose plans exclude weight-loss GLP-1s
| Provider | Starting Price | Meds Included? | Med Type |
|---|---|---|---|
| MEDVi | Confirm at medvi.org (certain states only) | Yes | Compounded semaglutide + tirzepatide |
| Eden | $149 first mo, $249/mo ongoing | Yes | Compounded semaglutide + tirzepatide |
| TrimRX | ~$199/mo | Yes | Compounded semaglutide |
| SkinnyRx ⚠️ | Needs verification — check skinnyrx.com | Yes | Compounded semaglutide |
Sources: medvi.org terms of service; tryeden.com terms; TrimRX pricing guide. Compounded medications are not FDA-approved as finished products. MEDVi available in certain states only — confirm before enrolling.
What these tables tell you that no other page does
The difference between “accepts UnitedHealthcare” and “helps you use UnitedHealthcare” is potentially hundreds of dollars per month. Shapely bills UHC for your visits. Ro charges a cash membership but fights to get UHC to cover the medication. MEDVi doesn't interact with your insurance at all. Knowing which bucket you're in before you sign up is the whole game.
What Does “Accepts UnitedHealthcare” Actually Mean?
When a GLP-1 telehealth provider says it “accepts insurance” or “takes UnitedHealthcare,” it could mean any of three things — and most pages presenting these interchangeably are doing you a disservice.
In-network visit billing
The provider has a contract with UHC. Your telehealth visits and clinical services are billed to UHC at negotiated rates. You pay a copay. This is what most people assume "accepts insurance" means. For GLP-1 telehealth, Shapely and Accomplish Health are the publicly documented examples for UHC commercial members.
Prior-authorization and coverage navigation
The provider charges you a cash membership for their program, but they help you get UHC to pay for the actual medication at the pharmacy. This is what Ro, WeightWatchers Clinic, and Noom do. You're paying two separate bills: a program fee (out of pocket) and a medication cost (hopefully covered by UHC after prior authorization). The program fee is never covered by insurance.
Cash-pay fallback
The provider has zero interaction with UHC. You pay for everything out of pocket. This is MEDVi, Eden, and TrimRX. These providers exist for the reader whose UHC plan excludes weight-loss medications — which is more common than most people expect.
Our classification method: We label a provider “UHC in-network” only if it publicly claims UHC network status on its own website or appears in UHC's provider directory. Programs that only help with medication coverage are labeled “insurance navigation.” Anything else is “cash-pay fallback.” Where claims were unclear, contradictory, or dated, we flagged the row with NEEDS VERIFICATION.
Which Route Is Best for Your Situation?
The right answer depends on what you need resolved first: in-network visit billing, the best shot at brand-name coverage, or the fastest workable fallback.

Best if You Want a True UHC In-Network Online Option
Start with Shapely if you're in CA, FL, NY, or TX and have a commercial UHC PPO plan.
Shapely is the clearest publicly documented in-network online GLP-1 program for UnitedHealthcare PPO members. Their UHC insurance page explicitly states in-network status, and their pricing reflects it: $49/month membership plus your standard copays and deductibles for visits. Medication is not included — it's billed separately through your insurance at the pharmacy.
Membership
$49/mo + standard copays
Visits
Monthly video with dedicated provider
Prior auth
Handled by Shapely's team
States
CA, FL, NY, TX
Medication
Billed separately via insurance
Compounded fallback
Sema from $99/mo if insurance denies
Shapely does NOT operate nationwide. If you're outside CA, FL, NY, or TX, Accomplish Health or the UHC provider directory are your next in-network options.
Shapely is not an affiliate — this is a direct editorial link
Accomplish Health — Second In-Network Option
Accomplish Health's announcement explicitly claims UHC in-network status and says they can accommodate most UHC plans. The announcement dates to September 2023, so confirm current network status, pricing, and geographic availability directly before enrolling.
Best if You Want FDA-Approved Medication and Strong Insurance Paperwork Help
Start with Ro if you're pursuing brand-name Wegovy, Zepbound, or Ozempic and want someone to handle the UHC bureaucracy.
Ro has the most robust insurance navigation system in the GLP-1 telehealth space. Their free Insurance Coverage Checker contacts UHC directly on your behalf and delivers a personalized coverage report. If you move forward, their insurance concierge handles prior authorization submissions, denial responses, and all the paperwork you'd rather not deal with.
Membership
$45 first mo, $145/mo ongoing
Medication (with UHC)
Your plan's copay
Coverage check
Free — Ro contacts UHC for you
Prior auth
Handled by Ro's concierge
If UHC denies
Cash-pay options from $149/mo
Limitations
Cannot coordinate Medicare/Medicaid/TRICARE
The honest tradeoff
Ro does not bill its program fee to insurance. If in-network visit billing is your top priority, Shapely is the better fit. But because Ro focuses on the medication-coverage side — the part that actually costs $800–$1,300/month at retail — the membership fee is relatively small for having someone fight for your drug coverage. And if insurance fails, Ro gives you cash-pay options without starting over with a new provider.
“Easy to get started, they walk you through the starting process and even did the paperwork for the pre-authorization for my insurance.”
— Ro member via Trustpilot

Ro contacts UHC on your behalf. No prescription, no commitment — just answers.
WeightWatchers Clinic, Noom, and Sesame
WeightWatchers Clinic / Med+
WW's care team works with commercial insurance to minimize out-of-pocket medication costs. The Med+ program starts at $25 for the first month, then $74/month. WW's registered dietitian service lists UnitedHealthcare among 600+ accepted insurance plans.
"Since starting Mounjaro and the GLP-1 Success Program, I feel like I've gotten my life back." — WW memberEstimate Your GLP-1 Cost with WeightWatchers →
Noom
Good fit for members who want psychology-based coaching and prefer picking up medication at their local pharmacy. Prescriptions go to your preferred pharmacy where you use your UHC insurance. Noom's care team assists with prior authorization (up to 14 days per Noom's documentation). NOT available in Alabama or Virginia.
Check Your Noom Coverage Path →Sesame
Takes a hybrid approach — program is cash-pay, but they accept insurance for weight-loss medications at the pharmacy level. Annual subscriptions start at $59/month. Useful for members who want a low-cost entry point for visits and are comfortable using UHC solely for the prescription.
See Sesame Medication Options →A note on LifeMD and PlushCare
LifeMD's public insurance messaging is contradictory — one page says certain plans may cover care, another says LifeMD doesn't accept insurance for GLP-1 programs. PlushCare is broadly in-network with Cigna, Humana, Aetna, and BCBS, but we could not confirm current UHC in-network status — Reddit reports from 2024 describe UHC/PlushCare network changes. Confirm directly with either provider before enrolling.
Does UnitedHealthcare Cover GLP-1 Medications for Weight Loss?
Sometimes — but far less often than most people assume. UHC's 2026 commercial weight-loss medication criteria (Program 2025 P 1114-19, effective February 1, 2026) make the structure clear: weight-loss drug coverage is an optional program that employers elect into. If your employer didn't opt in, no amount of prior authorization paperwork changes that.
UHC Employer-Sponsored / Commercial Plans
If your employer opted into weight-loss drug coverage, you may be eligible for Wegovy, Zepbound, or other FDA-approved anti-obesity medications with prior authorization. UHC's 2026 commercial criteria require:
BMI ≥ 30, or BMI ≥ 27 with at least one weight-related comorbidity (type 2 diabetes, hypertension, dyslipidemia, obstructive sleep apnea, or cardiovascular disease)
Documentation of prior weight-loss efforts (lifestyle interventions, dietary changes, exercise programs)
Proper diagnosis coding — ICD-10 codes for obesity or specific comorbidities
Initial authorization: 5 months for Wegovy, 6 months for Zepbound in UHC's commercial weight-loss program
Reauthorization: generally 12 months, requires documented treatment response
Source: UHC PA Notification: Weight Loss, Program 2025 P 1114-19, effective 2/1/2026 (uhcprovider.com).
State regulatory note
California, New Mexico, North Dakota (essential health benefits plans), and New York have state requirements that may affect UHC's coverage obligations regardless of employer opt-in.
If your employer did NOT opt in, weight-loss medications are excluded from your formulary. No prior authorization will override a plan exclusion. But check the exception paths — even with a weight-loss exclusion, your plan may still cover:
Wegovy
Non-formulary pathway for cardiovascular risk reduction (requires established CVD) or MASH (metabolic dysfunction-associated steatohepatitis)
Source: UHC Non-Formulary Wegovy criteria
Zepbound
Non-formulary pathway for obesity with obstructive sleep apnea (requires sleep study documentation)
Source: UHC Non-Formulary Zepbound criteria
Ozempic or Mounjaro
Standard formulary with prior authorization for type 2 diabetes diagnosis — these are FDA-approved for T2D
Source: UHC PA Notification Diabetes Medications GLP-1 Receptor Agonists, effective 7/1/2025
Drug-by-Drug UHC Coverage Summary
| Drug | FDA-Approved For | UHC Weight-Loss Path | Exception Paths |
|---|---|---|---|
| Wegovy (semaglutide) | Chronic weight management; CV risk reduction | Covered if employer opted in; 5-month initial PA | CV risk reduction; MASH (non-formulary pathways) |
| Zepbound (tirzepatide) | Chronic weight management; OSA | Covered if employer opted in; 6-month initial PA | Obesity with OSA (non-formulary pathway — requires sleep study) |
| Ozempic (semaglutide) | Type 2 diabetes only | Not applicable — T2D only | T2D standard formulary with PA |
| Mounjaro (tirzepatide) | Type 2 diabetes only | Not applicable — T2D only | T2D standard formulary with PA |
Sources: UHC PA Notification Weight Loss Program 2025 P 1114-19, effective 2/1/2026; UHC PA Notification Diabetes Medications GLP-1 Receptor Agonists, effective 7/1/2025; UHC Non-Formulary Wegovy and Zepbound criteria.
UHC Medicare Advantage
UHC Medicare Advantage plans generally do not cover GLP-1s for weight loss as of early 2026. Coverage exists for type 2 diabetes (with prior authorization) and potentially for obstructive sleep apnea (Zepbound) or cardiovascular risk reduction (Wegovy) depending on your specific MA-PD plan's formulary.
CMS has announced the Medicare GLP-1 Bridge program, which may make certain GLP-1 medications available to eligible Medicare Part D beneficiaries by July 2026, with a broader BALANCE program beginning January 2027.
For detailed workarounds, see our Medicare GLP-1 coverage guide.
UHC Community Plan / Medicaid
Coverage varies entirely by state. According to KFF's January 2026 tracker, 13 state Medicaid fee-for-service programs have a coverage path for GLP-1 medications for obesity. UHC administers Medicaid in many states, but formulary decisions are made at the state level. Check your state's Medicaid formulary or call the number on your UHC Community Plan card.
Ro contacts UHC directly and sends you a personalized drug-by-drug coverage report
How to Check Your Exact UnitedHealthcare GLP-1 Coverage
Don't sign up for any provider before you know what your plan actually covers. This takes under 10 minutes and prevents the most common — and most expensive — mistake: joining a program that doesn't match your coverage reality.
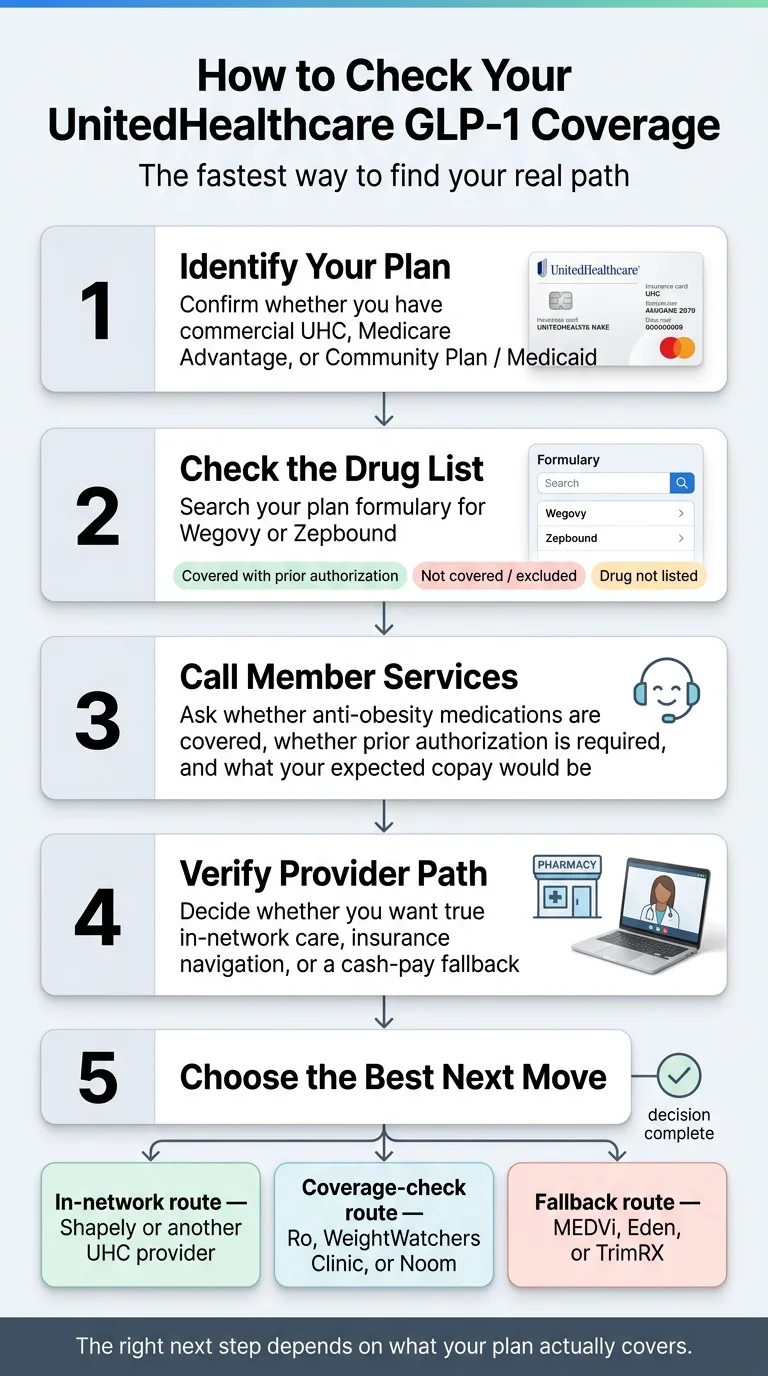
Identify Your UHC Plan Type
Look at your insurance card. Is this employer-sponsored commercial (PPO or HMO), individual marketplace, Medicare Advantage, or Community/Medicaid? The rules are completely different for each.
Check Whether Weight-Loss Drugs Are Covered
Log into member.uhc.com/myuhc → Pharmacy Benefits → Prescription Drug List. Search for 'Wegovy' or 'Zepbound.' You're looking for: 'Covered with prior authorization' (your plan includes it), 'Not covered' or 'Excluded' (employer didn't opt in — check exception paths), or 'Drug not listed' (also likely excluded — confirm with member services).
Call UHC Member Services
Call the number on the back of your card. Ask: (1) 'Does my plan include coverage for anti-obesity medications?' (2) 'Is Wegovy or Zepbound on my plan's formulary?' (3) 'What are the prior authorization requirements?' (4) 'Is there a step therapy requirement?' (5) 'What is my expected copay if the PA is approved?' Write down the reference number for the call.
Verify Provider Network Status
If your plan covers the drug, check whether your preferred provider is in-network using UHC's Find a Doctor tool at uhc.com/find-a-doctor. For Shapely, their UHC page confirms PPO in-network status in their available states.
Use a Provider-Side Coverage Tool
Ro's GLP-1 Insurance Coverage Checker is free — Ro's team calls UHC, gets your drug-by-drug coverage details, and sends you a personalized report. No prescription submitted, no obligation. WeightWatchers and Noom also have coverage estimators built into their enrollment flows.
No prescription, no commitment. Just a personalized coverage report from Ro's insurance concierge.
What If UnitedHealthcare Says No?
A UHC “no” doesn't always mean the same thing. Understanding why you were denied determines what you do next — and whether it's worth fighting or faster to pivot.

Denied Because Weight-Loss Drugs Are Excluded From Your Plan
This is the most common scenario and the hardest to reverse. If your employer didn't opt into weight-loss drug coverage, the exclusion applies regardless of your BMI, comorbidities, or documentation. No prior authorization will override a benefit design choice your employer made.
But check the exception paths first:
Wegovy for cardiovascular risk reduction (requires established CVD) or MASH
Zepbound for obesity with obstructive sleep apnea (requires sleep study)
Ozempic or Mounjaro if you have a type 2 diabetes diagnosis
If none of these apply, the plan exclusion is real. Cash-pay is your most practical path forward.
Denied Because the Prior Authorization Was Incomplete
This is fixable — and it happens more often than it should. Common reasons UHC denies a PA:
Wrong or missing diagnosis coding
ICD-10 code matters enormously. E66.01 (morbid obesity due to excess calories) is stronger than a vague obesity code.
Insufficient documentation of prior weight-loss attempts
Your provider needs documented history of lifestyle interventions — diet modifications, exercise, behavioral counseling. It needs to be in your chart.
BMI not clearly documented
Your most recent BMI must be in your medical records before the PA is submitted.
Wrong drug for the indication
Ozempic is only FDA-approved for T2D — submitting a PA for Ozempic for weight loss will be denied.
The fix: Have your provider resubmit with complete documentation. If denied again, request a peer-to-peer review — a phone call between your doctor and UHC's medical reviewer. Peer-to-peer reviews resolve many initial denials based on documentation gaps rather than true clinical ineligibility.
Should You Appeal or Move On?
If it's a plan exclusion → Move on
Appeals cannot override a benefit design choice your employer made. Your path is cash-pay or exception indications.
If it's an incomplete PA → Appeal
You have the right to a formal appeal and, after that, an external review through your state insurance commissioner.
You don't have to wait while you appeal. There's no rule that says you can't begin treatment through a cash-pay program while your insurance appeal is in process.
For a detailed appeal walkthrough, see our complete guide to getting insurance to cover GLP-1 medications.
Cash-Pay Fallback Options When UHC Excludes Weight-Loss GLP-1s
These providers are not “UnitedHealthcare-accepting” in any sense. They're here because a significant percentage of UHC members discover their plan simply doesn't pay for anti-obesity GLP-1 treatment. For those members, this is the backup plan that gets you started without waiting for insurance to change its mind.
Important: compounded vs. brand-name medications
Compounded GLP-1 medications are not FDA-approved. They are prescribed by licensed providers and dispensed by licensed US pharmacies, but they have not been evaluated by the FDA for safety, effectiveness, or manufacturing quality in the same way as brand-name drugs like Wegovy or Zepbound. We present compounded options as a distinct category — not as interchangeable with brand-name medications. (Source: FDA warning on compounded GLP-1 marketing, March 2026)
MEDVi — Simplest All-In Cash-Pay Option
Medication included · No insurance interaction · Month-to-month
MEDVi is the most streamlined cash-pay option for UHC members whose plans exclude weight-loss drugs. Medication is included in the price — no separate pharmacy bill, no insurance coordination, no surprises. They offer both compounded semaglutide (injectable and oral) and compounded tirzepatide.
Insurance status
Out-of-network per terms of service
Pricing
Confirm at medvi.org (medication included)
Billing
Month-to-month, no long-term commitment
Clinical oversight
Licensed providers via OpenLoop Health
Labs
Ordered if medically necessary via Quest
Availability
Certain states only — confirm before enrolling
Who this is for
UHC members who checked their coverage, discovered it doesn't include weight-loss GLP-1s, and want to start treatment without insurance headaches. All-inclusive pricing means no second bill at the pharmacy, no PA denials, no waiting.
Compounded medications are not FDA-approved as finished products. Source: medvi.org terms of service.
Eden — Clinical Feel, Transparent Cash-Pay Pricing
Eden is a cash-pay-only GLP-1 provider with a clinical aesthetic, licensed providers, and transparent pricing. Compounded semaglutide starts at $149 for the first month, then $249/month. Eden does not accept commercial insurance per its terms of service. Offers clinical tools (BMI, BMR, TDEE calculators) and provider-led educational content.
Who this fits: UHC members who want a provider that feels more “medical practice” than “telehealth startup.”
See Eden Availability and Pricing →Compounded medications are not FDA-approved as finished products. Source: tryeden.com terms of service.
TrimRX — Budget-Focused Compounded Option
Straightforward cash-pay compounded GLP-1 provider. Public pricing puts compounded semaglutide around $199/month. A useful budget fallback after a UHC denial.
Review TrimRX Pricing →Compounded medications are not FDA-approved as finished products. Source: TrimRX pricing guide.
SkinnyRx NEEDS VERIFICATION
SkinnyRx offers quick-access compounded GLP-1s without insurance. We could not verify current pricing from a directly parseable product page at the time of review. Check skinnyrx.com for current rates before enrolling.
Medication included · No insurance needed · Confirm state availability at medvi.org · Compounded = not FDA-approved as finished product
Can You Use HSA or FSA for Cash-Pay GLP-1 Programs?
In many cases, yes. IRS guidance allows HSA/FSA reimbursement for weight-loss expenses when they are for the treatment of a specific disease diagnosed by a physician. GLP-1 prescription medications prescribed by a licensed provider for a diagnosed condition generally qualify. However, program/membership fees may or may not be reimbursable depending on your plan administrator's rules.
Practical takeaway
The medication portion of a cash-pay GLP-1 program is likely HSA/FSA eligible with a valid prescription. Check with your plan administrator for program fees. Pre-tax savings effectively reduce your out-of-pocket cost by 20–35% depending on your tax bracket.
For a deeper dive, see our guide to using HSA/FSA for GLP-1 medications.
How We Classified Each Provider on This Page
Trust is what separates this page from every other “GLP-1 + insurance” list. Here's exactly how we decided which bucket each provider belongs in — so you can verify our work.
"True UHC in-network"
Provider publicly claims UHC network status on its own website, or appears in UHC's provider directory. Shapely met this standard with a current, active UHC-specific page. Accomplish Health met it with a public announcement (September 2023 — should be re-confirmed).
"Insurance navigation"
Provider charges a cash program fee but actively helps members use UHC benefits for medication coverage through insurance concierge services, prior authorization assistance, or pharmacy-level insurance billing. Ro, WeightWatchers Clinic, Noom, and Sesame met this standard.
"Cash-pay fallback"
Provider operates entirely on a cash-pay basis with no UHC interaction. MEDVi (out-of-network per terms), Eden (cash-pay only per terms), and TrimRX fell here.
NEEDS VERIFICATION
Provider's claims were unclear, contradictory, dated, or could not be confirmed from current public sources. Accomplish Health (announcement age), LifeMD (contradictory insurance pages), PlushCare (Reddit reports of UHC network changes), SkinnyRx (pricing not verifiable), and Noom (program fee not confirmed at time of review) carry this flag.
UHC criteria sources: UHC PA Notification Weight Loss Program 2025 P 1114-19 (effective 2/1/2026); UHC PA Notification Diabetes Medications GLP-1 Receptor Agonists (effective 7/1/2025); UHC Non-Formulary Wegovy criteria; UHC Non-Formulary Zepbound criteria; uhc.com member resources. We review provider claims and UHC policies on a monthly cycle.
Frequently Asked Questions
Does UnitedHealthcare cover Wegovy for weight loss?
Only if your specific plan includes weight-loss drug coverage, which is an optional employer add-on. If covered, UHC requires prior authorization with documented BMI, comorbidities, and prior weight-loss attempts. Initial authorization covers 5 months. Wegovy may also be covered through non-formulary pathways for cardiovascular risk reduction or MASH.
Does UnitedHealthcare cover Zepbound?
Same framework as Wegovy: only if your employer opted into weight-loss drug coverage. Initial authorization covers 6 months. Zepbound also has a non-formulary pathway for obesity with obstructive sleep apnea, which may apply even when weight-loss drugs are excluded.
Which online GLP-1 provider takes UnitedHealthcare?
For true in-network visit billing: Shapely (CA, FL, NY, TX for UHC PPO) and Accomplish Health (confirm current status). For medication coverage navigation with cash-pay membership: Ro, WeightWatchers Clinic, and Noom. For cash-pay fallback when plans exclude weight-loss drugs: MEDVi, Eden, and TrimRX.
Does Ro accept insurance?
Partially. Ro's Body Program membership is cash-pay only ($45 first month, $145/month). But Ro's insurance concierge actively helps members get UHC to cover medication costs at the pharmacy, and offers a free GLP-1 Insurance Coverage Checker that contacts your insurer on your behalf.
Does WeightWatchers Clinic take insurance?
WW's insurance coordinators work with commercial insurance plans to help cover medication costs. The Med+ program fee ($25 first month, $74/month) is separate. WW's registered dietitian service lists UnitedHealthcare among 600+ accepted plans.
Does Noom take UnitedHealthcare?
Noom's branded medications program sends prescriptions to your preferred pharmacy, where you use your insurance. Their care team assists with prior authorization. Noom's branded meds program is not available in Alabama or Virginia.
Does PlushCare take UnitedHealthcare?
We could not confirm current UHC in-network status from PlushCare's own public documentation. PlushCare is in-network with several major insurers, but Reddit reports from 2024 suggest UHC network changes. Confirm directly with PlushCare before enrolling.
What if my UHC plan excludes weight-loss medications?
Check non-weight-loss indication pathways first: Wegovy for cardiovascular risk reduction, Zepbound for OSA, Ozempic/Mounjaro for type 2 diabetes. If none apply, cash-pay programs like MEDVi and Eden offer medication-included pricing with no insurance needed.
How long does UHC prior authorization take?
UHC's general standard for non-urgent prior authorization requests is a decision within 15 calendar days. Actual timing varies by plan, product line, and completeness of the submission.
What about UHC Medicare Advantage?
UHC Medicare Advantage generally does not cover GLP-1s for weight loss. Coverage may exist for type 2 diabetes, OSA (Zepbound), or cardiovascular risk reduction (Wegovy). CMS has announced a Medicare GLP-1 Bridge program with initial access for eligible Part D beneficiaries expected by July 2026.
What about UHC Community Plan (Medicaid)?
Coverage varies by state. As of January 2026, 13 state Medicaid fee-for-service programs have a coverage path for GLP-1 medications for obesity per KFF's tracker. Check your state's Medicaid formulary directly.
Does UHC cover compounded GLP-1 medications?
Compounded medications are generally not standard formulary items on UHC plans. Cash-pay compounded providers like MEDVi, Eden, and TrimRX operate entirely outside the insurance system.
Can I use my HSA or FSA for cash-pay GLP-1 programs?
GLP-1 prescription medications prescribed for a diagnosed condition generally qualify for HSA/FSA reimbursement. Program and membership fees may or may not qualify depending on your plan administrator. Check with your HSA/FSA administrator for specifics.
Still Not Sure Which GLP-1 Program Is Right for You?
If you've read this far and still aren't certain which path fits your situation, take our free 60-second matching quiz. We'll ask about your insurance situation, what you've already tried, and what matters most to you — then tell you exactly where to start.
Take the free 60-second matching quiz
We ask about your insurance, budget, and goals — then give a matched recommendation. No email required.
Take the Free 60-Second Matching Quiz →No email required · No signup · Personalized recommendation in under a minute
Or, if you already know your route:
This page is published by The RX Index, an independent comparison resource for GLP-1 telehealth providers. We check provider claims, insurance criteria, and pricing using publicly available documentation and review this page monthly. We may earn a commission when you use affiliate links on this page; this never influences our editorial recommendations. Compounded medications are not FDA-approved as finished products. Always consult a licensed healthcare provider before starting any GLP-1 treatment. Last verified: April 9, 2026.
Related guides
The RX Index is an independent editorial publisher covering GLP-1 medications and telehealth providers. We may earn a commission if you visit a provider through our affiliate links. This never influences our editorial analysis or recommendations. If you find outdated information, contact us and we'll update within 48 hours.