Insurance Guide · Last verified: April 24, 2026
By The RX Index Editorial Team · Formulary status cross-checked against CVS Caremark, FDA, and CMS sources within the last seven days · 14-min read
Does CVS Caremark Cover Zepbound?
2026 Coverage, PA & Appeal Guide
Bottom line
The short answer is usually no — at least not on CVS Caremark's three standard employer formularies. Effective July 1, 2025, CVS Caremark removed Zepbound (tirzepatide) from its Standard Control, Advanced Control, and Value formularies for weight management (source: CVS Caremark). CVS Caremark has also stated it is making no new GLP-1 formulary changes for January 2026. But your situation might be one of the scenarios where Zepbound is still covered.
Where CVS Caremark may still cover Zepbound
- Your employer customized the plan. Many self-funded employers chose to keep Zepbound on their plan-specific formulary despite CVS Caremark's standard template changes.
- You meet 7056-A formulary exception criteria. Most often this means documented Wegovy intolerance, inadequate response, or contraindication.
- Your client plan has a weight-management copay tier. CVS Caremark's 2026 GLP-1 Outlook describes a plan-design option that can limit member out-of-pocket cost up to $200/month for weight-management drugs (source: CVS Caremark 2026 GLP-1 Outlook).
- You're on a government plan with separate rules. Medicare Part D excludes weight-loss drugs federally, but the December 2024 Zepbound OSA approval and the upcoming Medicare GLP-1 Bridge program created pathways that don't exist on commercial formularies (source: CMS).
What we actually verified for this page
Verified ✓
- CVS Caremark Standard, Advanced Control, and Value formulary GLP-1 status (caremark.com, business.caremark.com)
- CVS Caremark's own statement on no new GLP-1 changes for January 2026
- The published Zepbound PA criteria (6947-C) and Custom Exception criteria (7056-A) from info.caremark.com
- Eli Lilly Zepbound Savings Card 2026 terms and Self Pay Journey Program pricing (zepbound.lilly.com)
- FDA-approved Zepbound label, indications, contraindications, and warnings
- CMS Medicare GLP-1 Bridge guidance for 2026 and BALANCE model overview
- Active class action lawsuit dockets (SDNY and D.C. federal court)
- Ro and Sesame Care current public pricing and program pages
Not verified — because it's plan-specific or pending
- Your exact employer plan's customizations
- Your specific PA outcome or appeal odds
- Live pharmacy claim adjudications
- Lawsuit outcomes (cases are pending; CVS has filed motions to dismiss)
We re-verify this page quarterly and after any material change. Last refresh: April 24, 2026.
Quick verdict by situation
| If this is your situation | Most likely answer | First move |
|---|---|---|
| Standard CVS Caremark employer formulary, weight management | Zepbound usually not covered | Run Caremark's Check Drug Cost & Coverage tool + ask about Wegovy |
| Custom or self-funded employer plan | Could still be covered | Ask HR whether your employer customized GLP-1 coverage |
| Already on Zepbound, recently denied | Plan switched to Wegovy-preferred | Get the denial reason in writing before doing anything else |
| Moderate-to-severe OSA + obesity | Distinct exception pathway | Submit under the OSA indication with sleep-study documentation |
| Medicare Part D beneficiary | Separate federal rules apply | Check Part D plan + Medicare GLP-1 Bridge eligibility (starts July 1, 2026) |
| New start, never tried Wegovy | Plan-specific PA criteria apply | Check whether your plan uses 6947-C standard PA or 7056-A exception path |
| Hard plan exclusion (employer dropped weight-loss meds) | Coverage unlikely | Compare LillyDirect, Zepbound Savings Card, TrumpRx, or branded telehealth |
Does CVS Caremark cover Zepbound in 2026?
CVS Caremark is a pharmacy benefit manager (PBM) — the middle-layer company that administers prescription benefits on behalf of health insurers and self-funded employers. Whether your employer uses one of CVS Caremark's standard formulary templates or a custom design changes the answer dramatically.
The three standard formulary templates CVS Caremark dropped Zepbound from on July 1, 2025 are:
- Standard Control Formulary
- Advanced Control Formulary
- Value Formulary
In its 2026 client outlook, CVS Caremark stated that more than 95% of members in the weight-loss category had moved to a preferred formulary product after the July change, and that the company is holding steady with no new GLP-1 formulary changes for January 2026 (source).
What this means — and doesn't mean — for you
| Statement | True? | Why it matters |
|---|---|---|
| CVS Caremark's standard formularies removed Zepbound for weight management | Yes | This is the broad default answer for most members |
| No CVS Caremark member can get Zepbound covered | No | Custom plans, exceptions, OSA, and Medicare paths still exist |
| Wegovy is now the preferred GLP-1 alternative | Yes, on standard formularies | This affects your PA, appeal, and switch discussion |
| Cash-pay is your only real option | No | Exception, OSA path, custom plans, and the Medicare Bridge can apply |
| Zepbound and Wegovy are interchangeable | No | Different mechanisms and different FDA-approved indications |
Why CVS Caremark removed Zepbound on July 1, 2025
| Source | What they say | What it changes for you |
|---|---|---|
| CVS Caremark | Formulary strategy uses competition between drug manufacturers to lower list-price pressure and broaden access | Sets the official position you'll see on letters and member portals |
| CVS Caremark spokesman to NPR | High manufacturer list prices are the biggest barrier to patient access; the formulary decision was designed to deliver lower costs | Frames the decision as cost-driven, not clinical |
| Reuters / NPR reporting | The formulary change followed a CVS-Novo Nordisk rebate agreement that took effect just before the July 1 change | Helps you understand the business mechanism, not the medical one |
| Truveta health-data analysis (cited by CNN) | About 1 in 10 Zepbound users switched GLP-1s in July 2025 — roughly 16x typical; more than 8 in 10 of those switched to Wegovy | Confirms the change was implemented quickly and broadly |
| Larkin v. CVS Caremark (S.D.N.Y.) | Alleges the change and subsequent appeal denials violate ERISA medical-necessity standards (allegations only) | Suggests appeal denials may eventually be reviewed; no relief is currently available |
| Hamburger v. CVS Caremark / CareFirst (D.D.C.) | Alleges the OSA exclusion violates ERISA because no formulary alternative is FDA-approved for sleep apnea (allegations only) | Most directly relevant to denied OSA patients; CVS and CareFirst have filed motions to dismiss |
The honest reality you need to accept first
The formulary change isn't reversing in time to help your next refill. CVS Caremark has explicitly stated no new GLP-1 changes for 2026. The lawsuits are pending and could take 1–3+ years; CVS has already moved to dismiss. Even successful ERISA cases typically result in remand-and-review rather than blanket coverage restoration. That means you can stop refreshing news pages and start working the four real paths: exception, switch, self-pay, or branded telehealth with insurance support.
How to verify YOUR exact CVS Caremark Zepbound coverage in 10 minutes
The 5-step coverage verification ladder
- Use Caremark's Check Drug Cost & Coverage tool. Log into caremark.com, search for Zepbound, and enter your specific dose. The answer can vary by formulation — vial vs. KwikPen vs. single-dose pen. Take a screenshot of whatever it tells you.
- Call the member services number on your prescription card. Use this script: "I'm checking coverage for Zepbound for my exact plan. Can you confirm whether it's covered, excluded, non-formulary, or PA-required? If it's denied, what's the specific denial reason and the preferred alternative?"
- Ask HR whether your employer customized coverage. Use this script: "Does our plan use CVS Caremark's standard formulary, or did the employer customize coverage for Zepbound or anti-obesity medications?"
- If you've already gotten a denial, request the written denial, coverage determination, or plan appeal instructions. This is critical because different denial reasons require different responses. The denial reason determines whether you appeal, request a formulary exception, switch drugs, or pay cash.
- Have your pharmacy run the actual claim. A live claim adjudication is the highest-confidence answer. Use this script: "When you process Zepbound for me, what specific rejection reason or note appears in the system? Does it show PA required, non-formulary, plan exclusion, or quantity limit?"
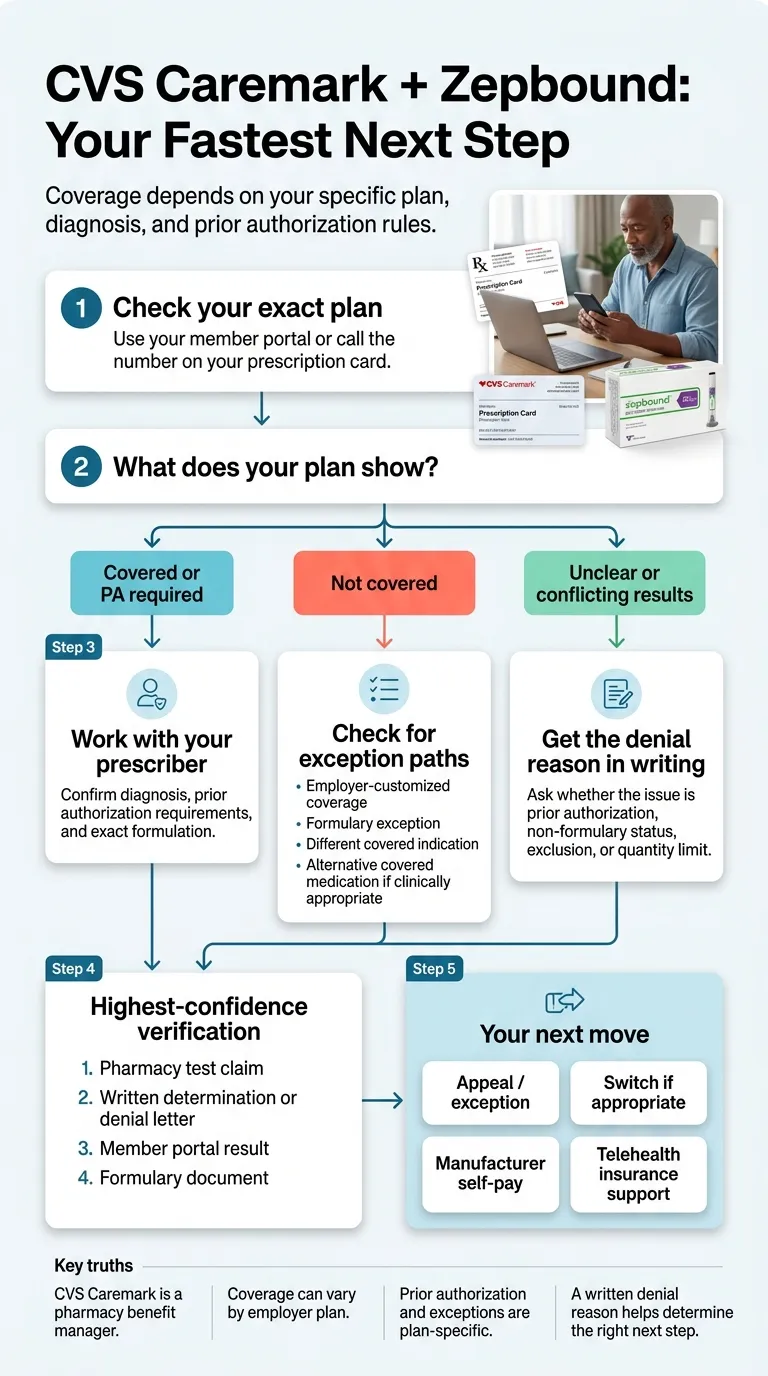
The evidence hierarchy — trust these answers in this order
| Source | Trust level | Why |
|---|---|---|
| Live paid or rejected pharmacy claim | Highest | Shows how your specific plan adjudicates the exact prescription, dose, and formulation |
| Written denial or written approval letter | High | Establishes appeal rights and gives you the official reason in writing |
| Caremark Check Drug Cost & Coverage tool | High | Member- and dose-specific, but doesn't always reflect employer customizations |
| Plan formulary PDF | Medium | Useful but often broad or 30–90 days stale |
| General CVS Caremark news article (including this one) | Low for your specific plan | Explains the trend, not your benefit |
| Reddit, Facebook groups, forum comments | Voice-of-customer only | Useful for understanding the change emotionally, not proof of coverage |
When the formulary says yes but the cost tool says no
| Conflict pattern | What it usually means | What to ask next |
|---|---|---|
| Public formulary lists Zepbound, member tool says not covered | Employer customization or PA-gated coverage | "Has my employer customized this drug? Is PA required?" |
| Listed but cost tool requires PA | Coverage is possible with documentation | "What are the exact PA criteria for my plan?" |
| Listed but excluded for weight management | Coverage tied to specific indication | "Is there a separate PA pathway for OSA?" |
| Different doses show different results | Formulation-specific coverage | "Which Zepbound formulations and doses are covered on my plan?" |
| Formulary PDF outdated | Live system has more recent data | "What does today's adjudication show?" |
When this happens to you: do not pay cash, do not abandon your script, and do not start an appeal yet. Get the written determination first.
Want help running the verification without all the back-and-forth?
If you'd rather not wrangle CVS Caremark yourself, Ro's free GLP-1 insurance check runs your specific plan and, when prior authorization is required, Ro's insurance support team submits the paperwork directly to CVS Caremark. Ro lists Zepbound single-dose pen as an insurance-eligible GLP-1 option and Zepbound KwikPen as a cash-pay option. Ro Body membership is $39 for the first month, then $149/month — or as low as $74/month with annual prepay (source: Ro pricing); medication cost is separate.
We may earn a commission from this referral. Ro cannot guarantee CVS Caremark approval — that decision is the PBM's. The PA process typically takes about 2–3 weeks.
Check your Zepbound coverage with Ro →CVS Caremark's prior authorization criteria for Zepbound
PA criteria vs. exception criteria — the distinction that determines your outcome
| Document | Purpose | What it requires |
|---|---|---|
| 6947-C (Standard PA criteria) | Coverage on plans that include Zepbound on the formulary with PA | FDA-approved indication, BMI documentation, OSA documentation if applicable, comprehensive weight-management program history, continuation response data (source) |
| 7056-A (Custom Exception criteria) | Exception when the plan formulary excludes Zepbound | Documentation that the patient cannot be treated with Wegovy due to inadequate response, intolerance, or contraindication |
| FEP-specific Zepbound form | Federal Employee Program plans | Plan-specific exception criteria (different fields than commercial 7056-A) |
If your plan excluded Zepbound on July 1, 2025, you need 7056-A, not 6947-C. Submitting against the wrong document is the #1 reason exceptions get denied.
Weight management criteria (typical 6947-C requirements)
- Adult diagnosis (18+)
- Documentation of reduced-calorie diet and increased physical activity
- BMI ≥ 30, or BMI ≥ 27 with a weight-related comorbidity (hypertension, type 2 diabetes, dyslipidemia, etc.)
- Documentation of a 6-month comprehensive weight-management program
- Continuation criteria: stable maintenance dose plus documented response (often a 5% baseline body-weight loss or maintained loss)
Obstructive sleep apnea criteria
Zepbound was FDA-approved on December 20, 2024 as the first and only prescription medication for adults with moderate-to-severe obstructive sleep apnea and obesity (source: FDA label). CVS Caremark's OSA-specific PA criteria typically require:
- Confirmed OSA diagnosis with documented Apnea-Hypopnea Index (AHI) on polysomnography or home sleep apnea test
- BMI documentation
- Reduced-calorie diet and increased physical activity context
- Continuation of CPAP or other established sleep-apnea therapy where appropriate
Approval durations and quantity limits
| Indication | Initial approval | Continuation approval | Notes |
|---|---|---|---|
| Obstructive sleep apnea | ~6 months | ~12 months | Requires OSA-specific documentation |
| Weight management | ~8 months | ~12 months | Continuation often requires response/maintenance |
| Quantity limits | Plan-specific | Plan-specific | Varies by dose and formulation |
If you've been denied — the 7-type denial decoder
| Denial reason | What it means | Best first response | Proof that resolves it |
|---|---|---|---|
| Benefit exclusion | Your plan doesn't cover weight-loss drugs at all | Ask HR if a rider/exception exists; otherwise pursue self-pay or alternative | HR confirmation; written exception approval |
| Non-formulary | Drug isn't on plan's preferred list | Request formulary exception (7056-A path) | Letter of Medical Necessity tied to 7056-A criteria |
| PA required (not yet submitted) | Coverage is possible but the prescriber hasn't submitted criteria | Match the 6947-C PA form line by line and submit | Complete 6947-C documentation |
| PA denied (criteria not met) | Documentation didn't satisfy plan criteria | Request denial letter, fix gaps, resubmit or appeal | Specific evidence addressing each unmet criterion |
| Step therapy / preferred alternative required | Plan wants you to try Wegovy (or other) first | Try the alternative or document why you can't | Documented Wegovy trial outcome (intolerance, side effects, inadequate response) |
| Quantity limit | Dose or refill quantity exceeds plan rules | Submit quantity-limit exception with clinical justification | Dosing rationale from prescriber + clinical guidelines |
| Indication mismatch | Plan covers Zepbound for one diagnosis but not another | Confirm diagnosis coding; consider OSA pathway if applicable | Correct ICD-10 coding + indication-appropriate PA submission |
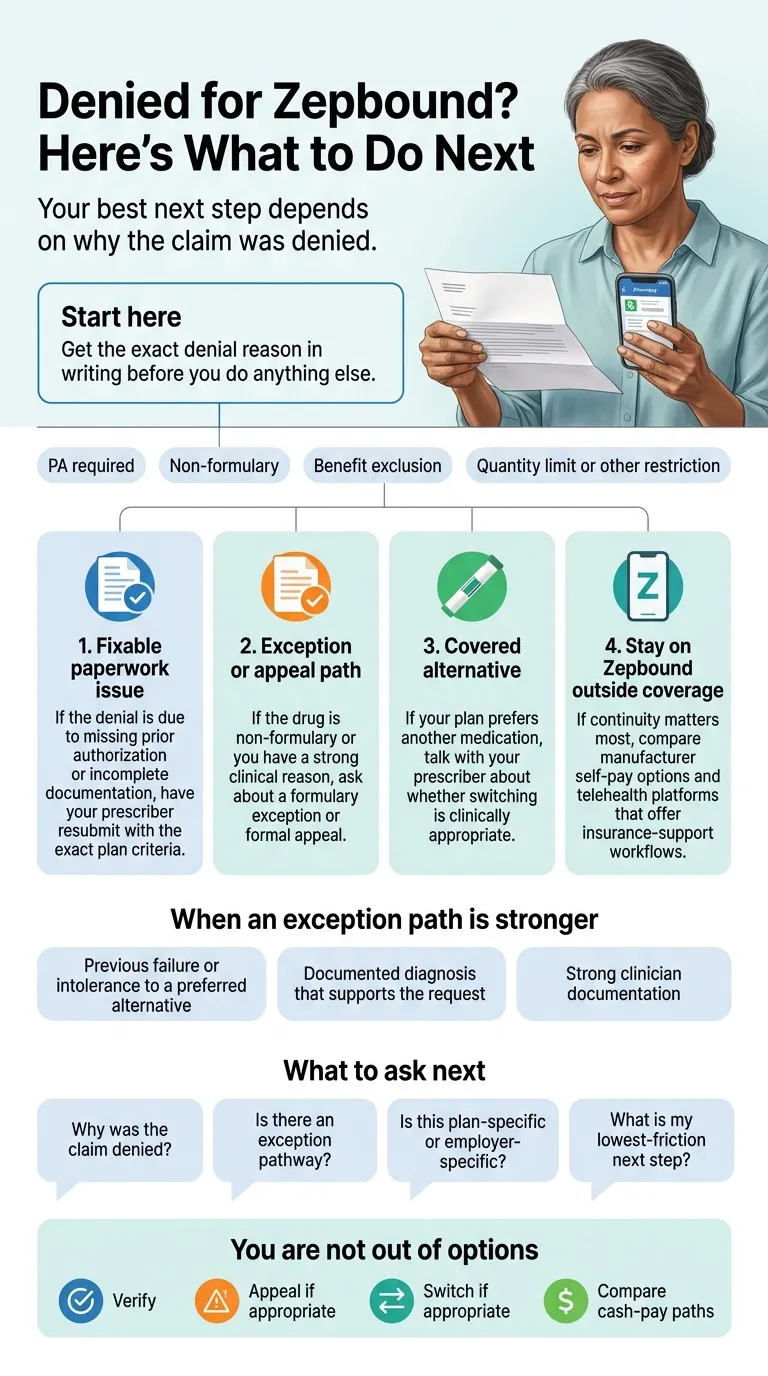
What to do in the first 24 hours after a denial
- Save the denial letter or denial-tracking number. You'll need it for any appeal.
- Call CVS Caremark and ask for the specific denial reason in writing. Use this script: "Can you send me the written denial reason and the exact criteria that were not met? I need to know whether this was a benefit exclusion, PA denial, non-formulary denial, quantity limit, or preferred-alternative requirement."
- Don't pay cash yet. Once you know the denial type, you'll know whether an exception or appeal is realistic.
- Don't refill at retail price. If you need to bridge access while you sort the denial, LillyDirect Self Pay or the Zepbound Savings Card are almost always cheaper than retail.
What not to do
- Don't ask your doctor for a generic "medical necessity" note. CVS Caremark's reviewers want criteria-specific documentation.
- Don't assume someone else's approval predicts yours. Plans differ.
- Don't appeal a benefit exclusion. If your employer chose to exclude weight-loss medications, no appeal will reverse that.
How to appeal a CVS Caremark Zepbound denial
When an appeal is worth pursuing
- ✅ You meet BMI/comorbidity criteria but documentation was missing
- ✅ You have moderate-to-severe OSA with obesity and the request was filed under the wrong indication
- ✅ You've tried Wegovy and have documented intolerance, side effects, or insufficient response (the standard 7056-A path)
- ✅ Continuation criteria were met but not documented
- ✅ Your plan has a formulary exception process and you have a clinical reason Zepbound is appropriate
When an appeal probably isn't worth your time
- ❌ Your plan has a hard exclusion for weight-loss medications
- ❌ You don't meet BMI/OSA documentation criteria and there's no clinical case to make
- ❌ You're asking for a non-covered formulation or quantity outside what the plan allows
- ❌ Your denial reason is "excluded benefit," not missing paperwork
Appeal timing by plan type
| Plan type | Typical appeal timeline | External review available? |
|---|---|---|
| Employer ERISA / commercial (non-grandfathered) | At least 180 days to request internal review per DOL guidance | Yes — denial notice describes external review rights |
| Fully insured state-regulated plan | Plan-specific, typically 180 days | Yes, often through state insurance department |
| Self-funded ERISA employer plan | Plan-specific, typically 180 days | Yes for non-grandfathered plans |
| Medicare Part D | Strict CMS-defined timelines (varies by request type) | Yes — CMS-administered process |
| Medicaid | State-specific timelines and processes | Yes — state-administered |
| Federal Employee Program (FEP) | OPM-defined process; uses FEP-specific Zepbound form | Yes — OPM-administered |
Don't want to do the appeal paperwork yourself?
Ro cannot guarantee that CVS Caremark approves your prior authorization — no one can. What Ro's insurance support team does is file the documentation correctly and handle the back-and-forth that's the #1 reason patients abandon the appeal. Get started for $39 (first month), then as low as $74/month with annual prepay. Medication cost is separate.
We may earn a commission from this referral.
See if you qualify for Ro's GLP-1 insurance support →Should you just switch to Wegovy? An honest comparison
Wegovy contains semaglutide, which acts on the GLP-1 receptor alone. Zepbound contains tirzepatide, which acts on both GIP and GLP-1 receptors. In head-to-head trial data, tirzepatide produced greater average weight loss than semaglutide. Wegovy has a unique advantage: it's the only GLP-1 with FDA approval to reduce major cardiovascular events in patients with established heart disease.
| Path | Best fit | Real tradeoff |
|---|---|---|
| Switch to Wegovy | Plan covers Wegovy and prescriber agrees clinically | Different medication; tolerability and weight-loss response may differ; no FDA OSA indication |
| Stay on Zepbound via formulary exception | Strong clinical reason not to switch (OSA, prior Wegovy failure, established response) | More paperwork; no approval guarantee; can take 1–4 weeks |
| Pay for Zepbound outside coverage | Continuity matters more to you than monthly cost | Higher monthly cost; savings-card eligibility varies |
Where Wegovy may actually fit you better
- You have a cardiovascular history (Wegovy has the FDA-approved CV risk-reduction indication)
- You're early in titration (no established Zepbound response to lose)
- Coverage simplicity is your priority
Where Zepbound is genuinely harder to substitute
- You've established a stable, effective response on tirzepatide
- You have moderate-to-severe OSA — Zepbound is the only FDA-approved GLP-1 for sleep apnea
- You've previously had poor tolerability or insufficient response on semaglutide
The OSA exception path — distinct clinical and coverage territory
Wegovy has shown some research benefit for sleep apnea, but it's not FDA-approved for OSA. Zepbound is. That distinction is a medical-necessity argument no other on-formulary GLP-1 can answer for an OSA patient.
Documentation to bring to the OSA exception request
- Sleep study with documented Apnea-Hypopnea Index (AHI) — moderate is generally AHI 15–29; severe is AHI 30+
- Current BMI documentation
- OSA diagnosis (ICD-10 code G47.33)
- Documentation of CPAP use, intolerance, or insufficient response (strengthens the case)
- Letter of Medical Necessity citing the FDA OSA indication and the absence of an on-formulary alternative with the same indication
- Reduced-calorie diet and increased physical activity context (CVS Caremark criteria still require this)
What to ask CVS Caremark:
"If Zepbound is denied for weight management, does my plan have a separate prior-authorization pathway for moderate-to-severe obstructive sleep apnea with obesity?"
OSA lawsuit docket tracker
| Case | Court | Filed | Current status |
|---|---|---|---|
| Larkin v. CVS Caremark | S.D.N.Y. | September 2025 | Pending; targets broad Zepbound exclusion under ERISA |
| Hamburger v. CVS Caremark / CareFirst BlueCross BlueShield | D.D.C. | September 2025 | Pending; targets OSA exclusion specifically; CVS and CareFirst have filed motions to dismiss |
Allegations only. Outcomes are not guaranteed and these cases should not be treated as a short-term coverage solution. Track classaction.org for updates.
Does Medicare or Medicaid change the answer?
Medicare Part D: the GLP-1 Bridge details
CMS announced the Medicare GLP-1 Bridge to address coverage gaps for anti-obesity medications (source: CMS).
- Start date: July 1, 2026
- End date: December 31, 2027
- Eligibility: Eligible Part D beneficiaries (not all Medicare beneficiaries — verify with your specific Part D plan)
- Drug listed: Zepbound KwikPen for weight reduction
- Copay: $50/month under Bridge terms
- PA requirement: Yes, prior authorization is required
If your Zepbound prescription is for OSA, it's handled under ordinary Part D utilization management — not the Bridge program. The OSA pathway existed before the Bridge announcement because the December 2024 FDA OSA approval gave Zepbound a non-weight-loss indication.
Medicaid and BALANCE
CMS's BALANCE (Better Approaches to Lifestyle and Nutrition for Comprehensive hEalth) model is launching state-by-state in 2026. Some state Medicaid programs may begin offering expanded GLP-1 access through BALANCE participation, but state participation is voluntary. Verify with your specific state Medicaid administrator.
What government-plan readers should do
- Confirm whether your Part D plan participates in the GLP-1 Bridge
- Confirm whether your prescription is being filed for weight loss or for OSA — this changes the pathway
- For Medicaid, verify with your specific state administrator whether BALANCE applies
- Don't rely on commercial CVS Caremark articles for Medicare/Medicaid answers — the rules are entirely different
What Zepbound actually costs if CVS Caremark won't cover it
The full Zepbound cost reality matrix
| Your situation | Path | Realistic monthly cost | Verified |
|---|---|---|---|
| CVS Caremark plan still covers Zepbound | Insurance + Zepbound Savings Card | As little as $25 | Lilly, April 2026 |
| Excluded — successful exception | Insurance + Savings Card at tier 3 copay | Tier 3 copay (varies; often $40–$100) | Plan-specific |
| LillyDirect Self Pay — 2.5 mg vial or KwikPen | LillyDirect | $299/month | Lilly Self Pay Journey, April 2026 |
| LillyDirect Self Pay — 5 mg vial or KwikPen | LillyDirect | $399/month | Lilly Self Pay Journey, April 2026 |
| LillyDirect Self Pay — 7.5 mg, 10 mg, 12.5 mg, 15 mg (with 45-day refill) | LillyDirect Self Pay Journey Program | $449/month | Lilly Self Pay Journey, April 2026 |
| Missed 45-day refill window — 7.5 mg | LillyDirect standard pricing | $499/month | Lilly current terms, April 2026 |
| Missed 45-day refill window — 10 mg, 12.5 mg, 15 mg | LillyDirect standard pricing | $699/month | Lilly current terms, April 2026 |
| Commercial insurance without Zepbound coverage — KwikPen w/ Savings Card | Lilly Savings Card | $299–$449/month based on dose | Lilly, April 2026 |
| TrumpRx | TrumpRx.gov via LillyDirect fulfillment | As low as $299; average $346/month | TrumpRx, April 2026 |
| Switch to Wegovy via CVS Caremark | Insurance + Wegovy Savings Card | As little as $25 | NovoCare, April 2026 |
| Some CVS Caremark plans' weight-management copay tier | Plan benefit | Up to $200/month | CVS Caremark 2026 GLP-1 Outlook |
Branded telehealth options: Ro, Sesame Care, LillyDirect & TrumpRx
| Path | Uses insurance? | PA support? | Membership / visit fee |
|---|---|---|---|
| Ro | Yes — lists Zepbound pen as insurance-eligible | Yes — insurance team submits PA (typically 2–3 weeks) | $39 first month, then $149/mo or as low as $74/mo annual |
| Sesame Care | Program-specific; verify before committing | Program-specific; verify directly | Visit-based pricing varies |
| LillyDirect Self Pay | No — cash-pay only | No PA support | None |
| TrumpRx | No — cash-pay only | No PA support | None |
Compare your branded Zepbound options before you commit
If you want telehealth with insurance support and PA help, Ro is the natural fit — they're already filing this exact paperwork to CVS Caremark every day. If you want transparent cash-pay branded options without going through the appeal process, Sesame Care is worth a look (verify PA support directly for the weight-loss program). If you don't need telehealth at all, LillyDirect is the cheapest direct route.
We may earn commissions from these referrals. Coverage and approval are not guaranteed by any provider; PBM decisions are made by CVS Caremark.
What real CVS Caremark members are saying
Voice-of-customer evidence only — not medical claims, not provider endorsements, not proof of any plan's coverage.
"Is CVS Caremark still covering your Zepbound?"
"It felt like a double punch."
"I guess I can't make it work."
Today, this week, this month — your action plan
Today (60 min)
- ☐Find your prescription card and call the member services number
- ☐Run Zepbound through Caremark's Check Drug Cost & Coverage tool at your exact dose
- ☐Email or message HR about employer customization
- ☐If you have a denial letter, save it (paper and digital)
This week
- ☐Identify your denial type using the decoder table above
- ☐Decide which path you're pursuing: exception, switch, self-pay, or telehealth
- ☐If pursuing exception: contact prescriber to start 6947-C or 7056-A
- ☐If switching to Wegovy: ask prescriber about transition dosing
This month
- ☐Have your Zepbound (or alternative) source in place
- ☐If on LillyDirect, mark calendar for the 45-day refill window on doses 7.5 mg+
- ☐Bookmark this page — we re-verify quarterly and after every major change
The exact scripts to use with CVS Caremark, HR, your prescriber & your pharmacy
To CVS Caremark member services:
"For my exact plan, is Zepbound covered, prior-authorization required, non-formulary, or excluded? If it's denied, what is the specific denial reason and the preferred alternative? Can you send the denial reason in writing?"
To HR / benefits administrator:
"Does our plan use CVS Caremark's standard formulary, or did the employer customize coverage for Zepbound or anti-obesity medications? If standard, has the company considered adding a GLP-1 rider for affected employees?"
To your prescriber:
"Can you review CVS Caremark's current Zepbound prior-authorization criteria (6947-C) and exception criteria (7056-A) before submitting? If the plan prefers Wegovy, can you document whether switching is medically appropriate for me — and if not, can you write a Letter of Medical Necessity tied line-by-line to the relevant criteria?"
To your pharmacy:
"When you process Zepbound for me, what specific rejection reason or note appears in the system? Does it show PA required, non-formulary, plan exclusion, or quantity limit?"
PA and appeal documentation checklist
Print this. Bring it to your prescriber's office. Most appeals fail because something on this list was missing.
For a new Zepbound PA submission
- ☐Member ID and plan name (exactly as printed)
- ☐Exact Zepbound formulation and dose (vial vs. KwikPen vs. single-dose pen)
- ☐Diagnosis and ICD-10 code
- ☐Current and historical BMI
- ☐Weight-related comorbidities (with diagnostic codes)
- ☐Documentation of 6-month comprehensive weight-management program (where required)
- ☐For OSA: sleep study with AHI score, BMI, ICD-10 G47.33
- ☐Documentation of any prior Wegovy / Saxenda / Qsymia trials
- ☐Prescriber Letter of Medical Necessity tied to plan-specific criteria
- ☐Screenshots of CVS Caremark coverage tool result (if relevant)
For a continuation / renewal PA
- ☐Starting weight at Zepbound initiation
- ☐Current weight
- ☐Documented weight loss percentage (5% baseline loss often required)
- ☐Dose history and current dose
- ☐Refill history
- ☐Side-effect / tolerability notes
- ☐Continued lifestyle intervention documentation
- ☐Prior PA approval letter
For a formal appeal after denial
- ☐The denial letter
- ☐All PA submission documents above
- ☐A new Letter of Medical Necessity addressing CVS Caremark's specific denial reason
- ☐Any new clinical evidence not in the original submission
- ☐Member appeal request form (varies by plan)
Safety and medical considerations
Boxed warning
Risk of thyroid C-cell tumors based on rodent studies. Zepbound is contraindicated in patients with a personal or family history of medullary thyroid carcinoma (MTC) or Multiple Endocrine Neoplasia syndrome type 2 (MEN 2). Counsel patients about the risk and symptoms of thyroid tumors.
Other contraindications: Known serious hypersensitivity to tirzepatide or any of the product's excipients.
Major label warnings include: severe gastrointestinal adverse reactions; acute kidney injury related to dehydration; acute gallbladder disease; acute pancreatitis; hypoglycemia (especially with concomitant insulin or sulfonylureas); hypersensitivity reactions including anaphylaxis; diabetic retinopathy complications; pulmonary aspiration during general anesthesia; suicidal behavior and ideation (monitor for new or worsening depression); pregnancy and fetal risk; reduced effectiveness of oral contraceptives.
Key points
- FDA approval does not equal insurance coverage. Plan benefit design and PBM formulary decisions determine what your insurance covers.
- Never stop or switch your GLP-1 without your prescriber.
- Mounjaro contains the same active ingredient (tirzepatide) as Zepbound but is FDA-approved for type 2 diabetes — not chronic weight management. Do not assume Mounjaro is a covered substitute.
For full safety information, see the Zepbound Prescribing Information and Medication Guide.
How we verified this guide
Primary sources we checked directly:
- CVS Caremark's published GLP-1 formulary page (business.caremark.com)
- CVS Caremark's 2026 GLP-1 Outlook and formulary strategy update
- The Zepbound PA criteria document 6947-C and Custom Exception criteria 7056-A (info.caremark.com)
- The FEP-specific Zepbound exception form for federal employees
- Eli Lilly's Zepbound Self Pay Journey Program and Savings Card terms (zepbound.lilly.com)
- The FDA-approved Zepbound label (FDA Access Data)
- CMS guidance on the Medicare GLP-1 Bridge program and BALANCE model
- TrumpRx Zepbound page and pricing
- NovoCare Wegovy Savings Offer
- Ro and Sesame Care current public pricing and program pages
- Court dockets for the SDNY and D.C. federal court class actions
How we make money:
We may earn commissions from telehealth providers we link to, including Ro and Sesame Care. Commissions do not change our coverage analysis or which providers we recommend for your specific situation.
Refresh cadence:
Quarterly minimum, plus immediately after any material change — formulary update, lawsuit ruling, Lilly pricing change, CMS guidance update, or partner provider pricing change. Last verified: April 24, 2026.
Frequently asked questions
Does CVS Caremark cover Zepbound in 2026?
For most CVS Caremark members on a standard employer formulary, no — Zepbound is not covered for weight management as of July 1, 2025, and CVS Caremark has stated no new GLP-1 formulary changes for January 2026. Coverage may still apply through customized employer plans, formulary exceptions (form 7056-A), the up-to-$200/month weight-management copay tier on some client plans, or Medicare Part D when prescribed for OSA.
Why did CVS Caremark stop covering Zepbound?
CVS Caremark says the change is part of a formulary strategy using competition to lower costs, and that more than 95% of weight-loss utilization shifted to a preferred product after the July 2025 change. News reporting and pending lawsuits link the decision to a rebate agreement with Wegovy maker Novo Nordisk. The lawsuits remain pending and CVS has filed motions to dismiss.
Is Zepbound covered by CVS Caremark for sleep apnea?
The categorical exclusion still applies, but obstructive sleep apnea is a distinct exception pathway because Zepbound is the only GLP-1 FDA-approved (December 2024) for moderate-to-severe OSA in adults with obesity. A pending class action lawsuit (Hamburger v. CVS Caremark / CareFirst) targets this issue specifically.
What's the CVS Caremark exception document for Zepbound?
The standard PA criteria document is 6947-C and the exception criteria document is 7056-A. Federal employee plans use a separate FEP-specific Zepbound form. Submission method (ePA, fax, phone, or plan-specific workflow) varies by plan — your prescriber's office can confirm the right channel.
How long does a CVS Caremark Zepbound exception take?
Appeal and PA timing depends on plan type. Many employer health plans give members at least 180 days to request review after a denial under DOL rules. Follow the appeal instructions in your specific denial letter for exact timelines.
How much does Zepbound cost without CVS Caremark coverage?
LillyDirect Self Pay Journey Program pricing is $299/month (2.5 mg), $399/month (5 mg), and $449/month (7.5 mg, 10 mg, 12.5 mg, and 15 mg) when refilled within the 45-day window. Standard prices outside that window are $499/month (7.5 mg) and $699/month (10, 12.5, and 15 mg). TrumpRx lists Zepbound at as low as $299/month with an average around $346/month.
Can I appeal a CVS Caremark Zepbound denial?
Often, yes. Many employer health plans give at least 180 days to file a formal appeal after a denial under DOL rules. After internal appeals are exhausted, external review rights may be available — the specific process depends on plan type. Follow your denial letter for the exact route.
Can I use the Zepbound Savings Card if CVS Caremark denies coverage?
Yes, with conditions. Commercially insured patients whose plans don't cover Zepbound can use current Lilly KwikPen Savings Card terms at $299–$449/month depending on dose, subject to purchase-offer terms and refill timing. Government beneficiaries (Medicare, Medicaid, TRICARE) are excluded.
Will CVS Caremark cover Mounjaro for weight loss instead of Zepbound?
Mounjaro is FDA-approved for type 2 diabetes, not chronic weight management. Do not assume Mounjaro is a covered substitute for Zepbound unless your prescriber and plan confirm that route for your specific diagnosis.
Does CVS Caremark cover Wegovy?
Yes. Wegovy (semaglutide) is the preferred weight-management medication on CVS Caremark's three standard formularies as of July 1, 2025, typically with prior authorization required.
Does Aetna CVS Caremark cover Zepbound?
Aetna plans using CVS Caremark vary by employer and formulary. Use your member drug-cost tool and plan documents rather than assuming the broad CVS Caremark standard-formulary answer applies. Aetna Medicare plans typically exclude weight-loss drugs but may cover Zepbound for OSA under Part D rules.
What if my employer opted out of the CVS Caremark exclusion?
Some self-funded employers negotiated to keep Zepbound on their specific formulary. Ask your HR benefits team directly whether your plan opted out — this isn't always reflected in standard CVS Caremark documentation.
Is there a class action lawsuit I can join?
Two ERISA-based class actions are pending — Larkin v. CVS Caremark in SDNY targeting the broad Zepbound exclusion, and Hamburger v. CVS Caremark / CareFirst BlueCross BlueShield in D.C. federal court targeting the OSA-specific exclusion. Both cases are pending and CVS has filed motions to dismiss. Track classaction.org for updates or consult a benefits attorney about your specific eligibility.
Should I switch to compounded tirzepatide if CVS Caremark denies Zepbound?
This page is about FDA-approved Zepbound coverage. Compounded tirzepatide is a different product made by individual compounding pharmacies — it is not FDA-approved and not equivalent to brand-name Zepbound. Discuss any alternatives with a licensed clinician.
Is CVS Caremark the same as CVS Pharmacy?
No. CVS Caremark is a pharmacy benefit manager that administers prescription benefits for many plans. CVS Pharmacy is the retail pharmacy chain. They share a parent company (CVS Health) but operate as separate entities with different functions.
Still not sure which path is right for you?
Answer a few quick questions about your insurance, denial status, OSA history, and whether you want to appeal, switch, or compare self-pay branded options. You'll get a personalized action plan with the next step that fits your situation — no pitch, just clarity.
Get my personalized GLP-1 action plan →Last verified: April 24, 2026 by The RX Index Editorial Team. The RX Index is a pricing intelligence and comparison resource for GLP-1 telehealth providers. We update this page quarterly and after any material change to CVS Caremark's formulary, Zepbound's pricing or label, CMS Medicare guidance, or partner provider pricing.
This page is for educational purposes only. It is not medical, legal, or insurance advice. Zepbound is prescription-only. Coverage decisions should be verified directly with your plan, prescriber, pharmacist, or benefits administrator.