Insurance & Coverage — 2026 Verified Guide
Does Express Scripts Cover Foundayo? 2026 Coverage Check
Published:
Last verified: May 1, 2026 · Next review: June 2026, then monthly
By The RX Index editorial team · Sources: Express Scripts NPF, CMS, DailyMed, KFF, Foundayo.lilly.com · Editorial standards
Does Express Scripts cover Foundayo? Maybe — and “maybe” is the honest answer.
Express Scripts is a pharmacy benefit manager (PBM), not a single insurance plan. It serves more than 85 million Americans across thousands of different employer, Medicare, and TRICARE plans — each with its own rules. As of May 1, 2026, Foundayo (orforglipron) does not appear by name in the public Express Scripts 2026 National Preferred Formulary or its exclusions PDF. That is not a “no.” It's also not a “yes.” Your specific plan decides.
- ✅ With coverage + commercial insurance + Savings Card: as low as $25/month
- ✅ Without coverage, LillyDirect self-pay: $149/month (0.8 mg starter dose)
- ✅ Medicare Part D via GLP-1 Bridge starting July 1, 2026: $50/fill
Want help cutting through the paperwork?
Ro's free GLP-1 Insurance Coverage Checker contacts your insurer and sends you a personalized coverage report — including whether prior authorization is required and your real cost. No charge to use the checker.
Run Ro's free GLP-1 Insurance Coverage Checker →Ro Body: $39 first month, then as low as $74/month with annual plan. Medication billed separately. Government plans (Medicare/Medicaid/TRICARE/VA) excluded; FEHB may be eligible.
What we actually verified
We pulled this from primary sources, not summaries.
- ✅Express Scripts 2026 National Preferred Formulary PDF (express-scripts.com)
- ✅Express Scripts 2026 NPF Exclusions PDF (express-scripts.com)
- ✅Express Scripts GLP-1 coverage and prior-auth FAQ pages
- ✅Express Scripts EncircleRx Patient FAQ
- ✅TRICARE Prior Authorization Form for semaglutide/tirzepatide (militaryrx.express-scripts.com)
- ✅TRICARE 2026 Pharmacy Costs (tricare.mil)
- ✅CMS Medicare GLP-1 Bridge official page and FAQ (cms.gov)
- ✅Foundayo manufacturer pricing and Savings Card terms (foundayo.lilly.com)
- ✅LillyDirect Foundayo product page (lilly.com)
- ✅FDA-approved Foundayo prescribing information (accessdata.fda.gov)
- ✅Eli Lilly's FDA approval press release with ATTAIN-1 trial results
- ✅NovoCare current Wegovy savings offers (novocare.com)
- ✅KFF 2025 Employer Health Benefits Survey for GLP-1 coverage rates (kff.org)
- ✅Ro Body pricing and Foundayo product page (ro.co)
What we did not verify: Your specific plan's coverage. The deciding answer is in your Express Scripts member portal — not in any guide, ours included. This page exists to help you get the real answer faster.
Why “it depends” is the only honest answer
This is the part most coverage articles get wrong. They give you a yes-or-no answer when the structure of the question doesn't allow one.
Here's what's actually happening behind your ID card:
- Cigna's parent company is The Cigna Group. Evernorth Health Services is a Cigna Group division, and Express Scripts is the PBM inside Evernorth. Express Scripts also serves TRICARE and many non-Cigna employer plans.
- Express Scripts publishes a National Preferred Formulary (NPF) — a baseline list of preferred drugs.
- Your employer or plan sponsor can customize the formulary. They can add coverage. They can exclude classes of drugs. They can layer on a program like EncircleRx that requires you to enroll in a lifestyle app to get GLP-1 coverage.
That's why three coworkers at three different companies, all carrying Express Scripts cards, can get three different answers about Foundayo. None of them are wrong. Their plans just made different choices. The published NPF is a starting point — not the verdict. The verdict is in your member account.
Is Foundayo on the Express Scripts National Preferred Formulary?
Short answer: Not by name, as of May 1, 2026. We searched the public Express Scripts 2026 NPF PDF and the 2026 exclusions PDF for both “Foundayo” and “orforglipron” and found neither term. That doesn't prove your plan won't cover it. The NPF is abbreviated, subject to change, and not a coverage guarantee — your member account is the deciding source.
| Drug / Form | What we found in the public 2026 documents | What it proves |
|---|---|---|
| Foundayo (orforglipron) | Not found by name in either PDF we checked | Public document is silent. Not the same as “excluded.” |
| Wegovy injection | Listed as a preferred alternative in the 2026 exclusions document | Express Scripts treats Wegovy injection as a preferred path |
| Wegovy tablets | Listed as a preferred alternative in the 2026 exclusions document | Same |
| Zepbound pens | Listed as a preferred alternative in the 2026 exclusions document | Pens are the preferred form |
| Zepbound vials | Listed as excluded | Pens are the preferred form |
| Liraglutide (generic Saxenda) | Listed as a preferred alternative | Older weight-loss GLP-1 |
The most important sentence on this whole page
“Not found” is an evidence status, not a denial.
- Your plan doesn't cover Foundayo (real “no”)
- Foundayo hasn't been loaded into your plan's database yet (timing lag for a new drug)
- You searched the brand name only — try “orforglipron” too
- Your plan covers it but routes it through specialty pharmacy
Don't accept “I don't see it” as the final answer. Push for the real status.

The 4 Express Scripts coverage scenarios for Foundayo
Short answer: Coverage falls into one of four scenarios depending on your plan type and design. Find yours below and you'll know your real next step.
This table cross-checks the Express Scripts published formulary, the EncircleRx program documentation, the CMS Medicare GLP-1 Bridge announcement, and the TRICARE PA form — all verified May 1, 2026.
| Your situation | Foundayo coverage status | What you'll likely pay | Next step |
|---|---|---|---|
| 1. Commercial plan + employer covers GLP-1s for weight loss + plan uses NPF | Not in the public 2026 NPF by name. Coverage on individual plans is not publicly confirmed. | If covered + commercial insurance + Foundayo Savings Card: as low as $25/month, subject to monthly and annual savings limits | Verify with the call script below. Ask whether prior authorization is required and whether your plan uses EncircleRx or Omada engagement rules. |
| 2. Commercial plan + employer excludes weight-loss medications | Not covered for weight management. Per KFF's 2025 survey, only 43% of firms with 5,000+ workers covered GLP-1s primarily for weight loss; among firms with 200+ workers, only 19% did. | Self-pay through LillyDirect: $149–$349/month depending on dose. Savings Card has a separate dose-based offer for commercially insured patients whose plan doesn't cover Foundayo. | Compare LillyDirect, Ro, and covered alternatives (Wegovy, Zepbound). Medical necessity appeals usually can't override a plan exclusion. |
| 3. Medicare Part D administered by Express Scripts/Cigna | Standard Part D excludes weight-loss drugs. All Foundayo formulations confirmed eligible under the new CMS Medicare GLP-1 Bridge starting July 1, 2026. | $50 copay per fill through the Bridge (program runs through December 31, 2027). Bridge copay does not count toward your Part D true out-of-pocket limit. | Your prescriber submits the Bridge prior authorization centrally to CMS — separate from your Part D plan. See Medicare Bridge section → |
| 4. TRICARE (Express Scripts is the DoD pharmacy contractor) | The current TRICARE PA form for weight-loss GLP-1s names Wegovy and Zepbound. Foundayo is not yet specifically named on that form as of May 1, 2026. | Standard TRICARE pharmacy copay — see TRICARE section for 2026 numbers | Verify with TRICARE Formulary Search before assuming coverage. PA submission via 1-866-684-4488. |
How to check your specific plan in 90 seconds
Short answer: Three options. Fastest: log into your Express Scripts account and use “Price a Medication.” Most accurate: call the member services number on the back of your ID card. Easiest: let Ro's free coverage checker contact your insurer for you.
Option 1 — Express Scripts member portal (fastest, free, you do it)
- Go to express-scripts.com and log in
- Click Prescriptions → Price a Medication
- Search “Foundayo” first
- If nothing comes up, search “orforglipron” (the generic name)
- Look at the result — it will tell you covered status, copay, and whether prior authorization is required
Option 2 — Call member services (most accurate for new drugs)
The number is on the back of your prescription ID card. Have your member ID and date of birth ready. Use this exact 6-question script:
- “I want to confirm coverage for Foundayo, also called orforglipron. It was FDA-approved April 1, 2026, by Eli Lilly.”
- “Is Foundayo currently on my plan's formulary? If yes, what tier?”
- “Does Foundayo require prior authorization on my plan? If yes, what are the criteria?”
- “Is my plan enrolled in EncircleRx or another GLP-1 engagement program? If yes, do I need to enroll in Omada or a different lifestyle program to be eligible for GLP-1 coverage?”
- “Does my plan exclude weight-loss medications entirely? If yes, please confirm — that means medical necessity appeals usually won't change the answer.”
- “If Foundayo isn't covered, are Wegovy or Zepbound covered as alternatives, and would I need step therapy first?”
Save your answer — use this template:
Date called: ___ · Rep name: ___ · Call reference #: ___ · Brand searched: Foundayo · Generic searched: orforglipron · Result label: ___ · PA criteria (if any): ___ · Preferred alternatives: ___ · Next deadline (if any): ___Option 3 — Let someone else handle the call
Ro's free GLP-1 Insurance Coverage Checker does the work for you. You enter your insurance info; Ro's specialists contact your insurer, pull your coverage details, and send you a written report — including whether prior authorization is needed and what your actual cost will be. Ro openly carries Foundayo and Zepbound and can handle the prior authorization process if you decide to move forward.
What your coverage result actually means
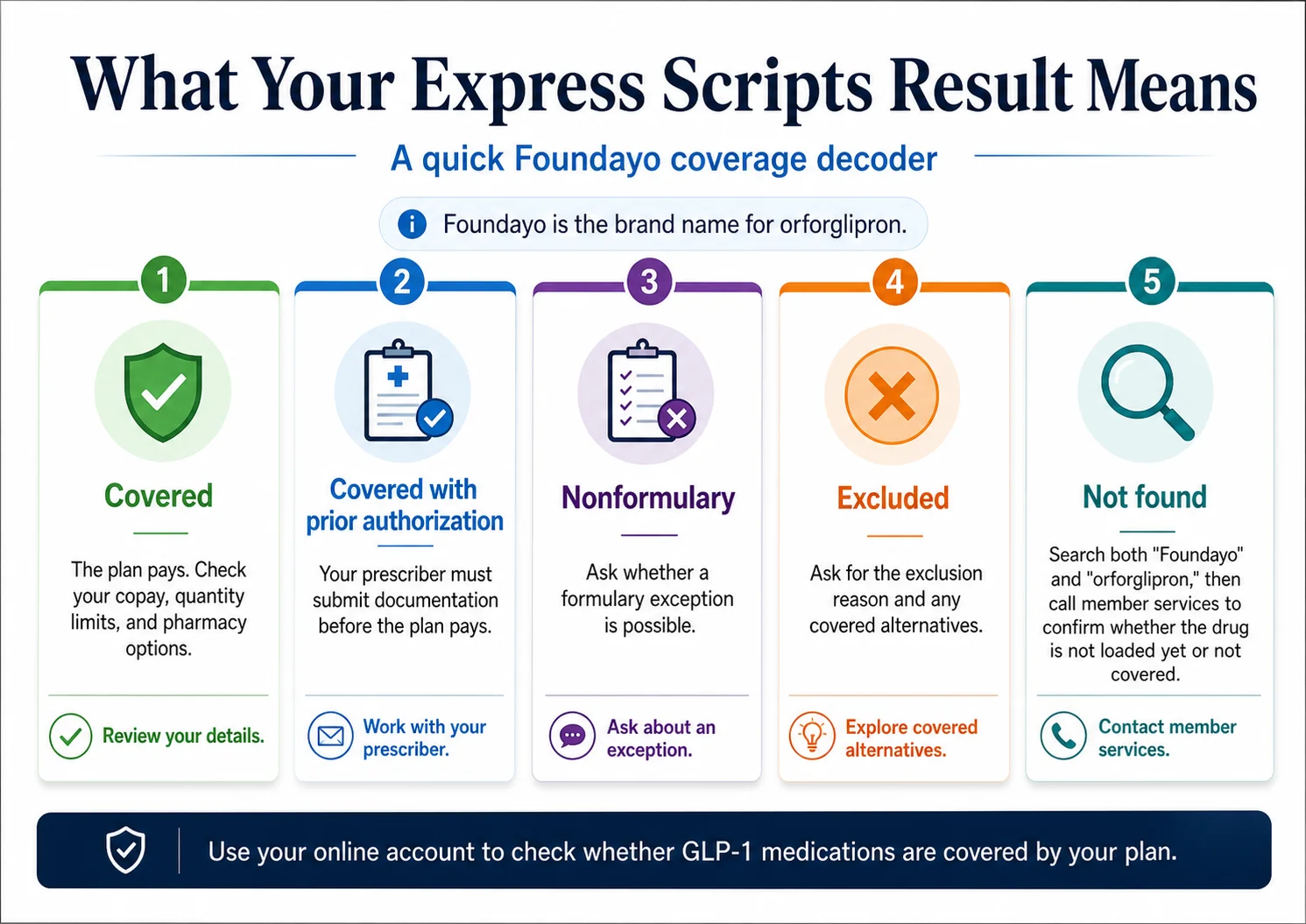
Short answer: Express Scripts coverage results come back in five flavors — each one means something different and has a different next step. “Not covered” is not the same as “excluded.” “Not found” is not the same as either.
| Result you see | What it actually means | What to do next |
|---|---|---|
| Covered | Plan will pay. Check the copay and any quantity limit. | Confirm prior authorization requirement. Ask about the Foundayo Savings Card. |
| Covered with prior authorization | Plan will pay if your prescriber submits documentation that meets the criteria. | Have your prescriber submit PA. See the PA section below. |
| Nonformulary | Not on the preferred list, but a coverage exception may be possible. | Ask your prescriber about a formulary exception request. |
| Excluded | Plan has formally chosen not to cover this drug class or this drug. | Get the exclusion language in writing. Medical-necessity appeals usually won't reverse a plan exclusion. Look at self-pay or covered alternatives. |
| Not found | The drug isn't loaded in the plan's database. Could be timing — not necessarily a coverage decision. | Search both names. Call to confirm whether it's “not loaded yet” versus actually not covered. |
The most important distinction: excluded vs. not found
“Excluded” is a final decision your employer made. You can ask HR to add it next plan year, but appeals rarely reverse an exclusion.
“Not found” often means the system hasn't caught up. Foundayo just launched in April 2026. Many plans take weeks or months to load new drugs. If the answer is “not found,” call. Don't pay cash yet.
How Express Scripts prior authorization works for Foundayo
Short answer: Express Scripts has not published Foundayo-specific public PA criteria yet. Existing weight-loss GLP-1 PA criteria for Wegovy and Zepbound on Express Scripts plans require BMI of 30 or higher, OR BMI of 27 or higher with at least one weight-related condition. Plans that use EncircleRx may also require enrollment in Omada. Express Scripts says nearly all coverage reviews are completed within two days.
What documentation usually belongs in a Foundayo PA packet
- Current BMI (and starting BMI if this is continuation of therapy)
- Weight history going back 6–12 months
- At least one weight-related condition if your BMI is 27–29.9 (hypertension, dyslipidemia, type 2 diabetes, sleep apnea, PCOS, cardiovascular disease)
- Documentation of prior lifestyle attempts — diet program, exercise plan, behavioral counseling, or previous medications
- Letter of Medical Necessity from your prescriber (Eli Lilly publishes a Letter of Medical Necessity template at foundayo.lilly.com for prescribers)
The EncircleRx and Omada engagement rule (the part most people miss)
If your employer's plan uses EncircleRx — Express Scripts' weight management program — getting prior authorization for any weight-loss GLP-1 may require you to enroll in Omada or another assigned lifestyle program. Plans set their own engagement requirements. Miss them and your PA can be denied or your renewal blocked, even if you meet every BMI and comorbidity criterion.
Use question #4 in the call script above to find out whether your plan participates in EncircleRx and what engagement rules apply.
How long PA takes
Express Scripts says nearly all coverage reviews are completed within two days after the prescriber sends complete information. Electronic prior authorization (ePA) determinations can come back within minutes. You can track status in your Express Scripts account under Prescriptions → Prior Authorizations.
Want someone else to handle the prior auth paperwork?
Ro's insurance concierge can submit the PA for you if you qualify — they pull your records, write the letter of medical necessity, and follow up with Express Scripts directly.
See if Ro can handle your PA →Ro Body $39 first month, then as low as $74/month with annual plan. Medication billed separately. Government plans (Medicare/Medicaid/TRICARE/VA) excluded; FEHB may be eligible.
What you'll actually pay for Foundayo (4 cost paths)
Short answer: With commercial insurance that covers Foundayo plus the Foundayo Savings Card, your cost can be as low as $25/month. Without coverage, LillyDirect self-pay starts at $149/month for the 0.8 mg dose. Medicare Bridge enrollees pay $50/fill starting July 1, 2026.
Prices pulled directly from the manufacturer's published pricing pages, verified May 1, 2026.
| Your situation | Foundayo dose | Monthly cost | What you need |
|---|---|---|---|
| Commercial insurance + plan covers + Savings Card | Any | As low as $25 | Commercial drug insurance (not government). Foundayo Savings Card from foundayo.lilly.com. Max $100/mo, $1,000/calendar year, up to 10 fills, expires 12/31/2026. |
| Commercial insurance + plan does NOT cover + Savings Card | 0.8 mg | $149/mo | Commercial insurance (not government). Separate dose-based offer. Expires 12/31/2026. |
| Commercial insurance + plan does NOT cover + Savings Card | 2.5 mg | $199/mo | Same as above. |
| Commercial insurance + plan does NOT cover + Savings Card | 5.5 mg / 9 mg / 14.5 mg / 17.2 mg | $299/mo | Same. 14.5 mg and 17.2 mg subject to Purchase Offer terms. |
| LillyDirect self-pay (no insurance) | 0.8 mg | $149/mo | Prescription routed to LillyDirect Pharmacy. |
| LillyDirect self-pay | 2.5 mg | $199/mo | Same. |
| LillyDirect self-pay | 5.5 mg / 9 mg | $299/mo | Same. |
| LillyDirect self-pay (Self-Pay Journey Program) | 14.5 mg / 17.2 mg | $299/mo (on time) · $349/mo (refill >45 days late) | Stay on schedule. |
| Medicare Part D + Bridge (from July 1, 2026) | Any (all six Foundayo NDCs eligible) | $50/fill | Eligible Part D plan + meet PA criteria. Bridge runs through December 31, 2027. Copay does not count toward Part D TROOP. |
| TRICARE | Any | See TRICARE section for 2026 copays | TRICARE Formulary Search + PA via Express Scripts. |
Important caveats nobody else flags clearly
- Government insurance beneficiaries cannot use the Foundayo Savings Card. Lilly's terms exclude Medicare, Medicare Part D, Medicare Advantage, Medigap, Medicaid, VA, DoD, and TRICARE/CHAMPUS.
- The $25/month commercial copay is the maximum benefit, not a guarantee. Your plan's tier placement, the savings card's monthly and annual limits, and your plan-year deductible all affect what you actually pay.
- The $299 high-dose self-pay price requires you to refill on time. Miss the 45-day refill window and the price jumps to $349.
- Verify with the official source before paying. Foundayo savings card terms are published at foundayo.lilly.com/coverage-savings and can change.
No coverage and want to start anyway? Ro lists Foundayo at the same medication pricing as LillyDirect, with clinical support and insurance help included in the Body membership.
See current Foundayo pricing on Ro →Ro Body $39 first month, then as low as $74/month. Medication billed separately.A note on Ro (the part most coverage articles won't tell you)
Ro is not the cheapest path if all you need is to log into your Express Scripts account and read your own coverage result. The Ro Body membership is separate from the cost of medication. You can run the verification yourself for free with the call script above.
But — if your real problem is not knowing whether you're covered, what prior authorization will require, or how to handle a denial, that's exactly what Ro's insurance concierge is built for. Ro openly carries Foundayo and Zepbound. Ro's specialists contact your insurer directly, run the GLP-1 Insurance Coverage Checker, and produce a personalized report. If you qualify and want to start treatment, they can handle the prior authorization paperwork.
- Ro currently can't coordinate GLP-1 coverage for most government insurance plans (Medicare, Medicaid, TRICARE, VA). FEHB members may be eligible to use Ro Body and the insurance concierge — verify when you sign up.
- The Body membership is separate from medication cost. Foundayo on Ro is the same medication price as LillyDirect; the membership pays for clinical care, monitoring, and insurance help.
If your only goal is the absolute cheapest manufacturer-direct path and you don't mind doing the insurance work yourself, LillyDirect is the manufacturer's direct channel at the prices above. If you want clinical guidance and someone to handle the insurance maze for you, that's where Ro earns its place on this page.
If your plan doesn't cover Foundayo: 4 real options
Short answer: You have four real moves: (1) appeal the decision if it's based on medical necessity, (2) request a formulary exception, (3) self-pay through LillyDirect, Ro, or Hims/Hers, or (4) switch to a covered alternative like Wegovy or Zepbound.
Option 1 — Appeal (only works for medical-necessity denials)
If Express Scripts denied your PA because your documentation didn't meet the criteria — not because your plan excludes weight-loss meds — you can appeal.
- Get the denial reason in writing. Your denial letter will state the specific reason and your appeal deadline.
- Submit a Letter of Medical Necessity from your prescriber with full BMI history, comorbidity records, and prior weight management attempts.
- Ask whether your plan offers peer-to-peer review — your prescriber speaks directly with the Express Scripts medical reviewer.
- If internal appeal denied: ask about external review through your state insurance department.
Option 2 — Formulary exception
Even if Foundayo isn't on your plan's formulary, your prescriber can request a formulary exception when there's a genuine medical reason Foundayo specifically is appropriate — for example, severe injection aversion, intolerance to other GLP-1s, or a need for the oral dosing flexibility Foundayo offers.
Option 3 — Self-pay through verified channels
- LillyDirect: $149–$299/month depending on dose. Free home delivery. The manufacturer-direct verified self-pay path.
- Ro: Carries Foundayo and Zepbound at the same medication pricing as LillyDirect, plus clinical support and insurance help. Ro Body membership is separate from medication cost.
- Hims and Hers: Now publicly list Foundayo among their FDA-approved GLP-1 medication options.
Option 4 — Switch to a covered alternative
If Wegovy or Zepbound is already a preferred alternative on your Express Scripts plan (both appear in the public 2026 exclusions document), this is the path of least resistance. Honest tradeoff: Wegovy and Zepbound are mainly injections — Foundayo's oral form has no food or water timing rules. If injection isn't a dealbreaker and your plan already covers Wegovy or Zepbound, the medication your insurance will actually approve may be the smartest move.
The damaging admission you need to hear
If your employer chose a plan that explicitly excludes weight-loss medications, no amount of appeal paperwork will change that. KFF's 2025 Employer Health Benefits Survey found that only 43% of firms with 5,000+ workers covered GLP-1s primarily for weight loss — meaning 57% of those very large firms did not. Among firms with 200+ workers, only 19% covered them. The fastest answer for an excluded plan is self-pay or a switch at open enrollment. That's a structural problem with your plan, not with you or your medication.
Plan won't cover it and you want to start now? Same medication pricing as LillyDirect, plus a clinical team that monitors your progress.
Get Foundayo through Ro →Medicare and the GLP-1 Bridge ($50/month from July 1, 2026)
Short answer: Standard Medicare Part D doesn't cover GLP-1s for weight loss. That changes July 1, 2026: the new CMS Medicare GLP-1 Bridge will give eligible Medicare Part D members access to all Foundayo formulations for $50 per fill, separate from your normal Part D plan. The Bridge runs through December 31, 2027.
Who qualifies
- Enrolled in a standalone Part D plan (PDP) or Medicare Advantage with Part D (MA-PD)
- Special Needs Plans (SNPs), Employer Group Waiver Plans (EGWPs), and the LI NET program also eligible
- Dually-eligible (Medicare + Medicaid) members in eligible Part D plans qualify
- Not eligible: Private fee-for-service plans, Section 1876 cost contracts, Section 1833 prepayment plans, PACE organizations, fallback plans, and religious fraternal benefit plans — unless they also have a separate eligible PDP
Clinical criteria (CMS Bridge)
CMS Bridge prior authorization criteria, evaluated at the time GLP-1 therapy is initiated, require lifestyle modification plus one of the following:
- BMI ≥ 35, OR
- BMI ≥ 30 with HFpEF, uncontrolled hypertension, or chronic kidney disease (CKD) stage 3a or worse, OR
- BMI ≥ 27 with prediabetes, previous myocardial infarction, previous stroke, or symptomatic peripheral artery disease
How the payment works
Bridge claims are processed centrally — Humana administers the program through the LI NET infrastructure, separate from your Part D plan. The pharmacy collects your $50 copay and submits the rest to the central processor. Your Part D plan doesn't bear the cost. The $50 Bridge copay does not count toward your normal Part D true out-of-pocket limit.
Foundayo is confirmed eligible
CMS has explicitly listed all Foundayo formulations in the Bridge with these NDC numbers: 0002-4178-31, 0002-4503-31, 0002-4794-31, 0002-4803-31, 0002-4839-31, and 0002-4953-31. Bring this list if your pharmacy can't find Foundayo in the Bridge system.
April 2026 update
On April 21, 2026, CMS announced that the full BALANCE Model — originally planned for January 2027 in Medicare Part D — will not launch in Part D in 2027 as planned. The Bridge has been extended through December 31, 2027 to provide continuous access while CMS reassesses.
Warning for Medicare members
Do not use the commercial Foundayo Savings Card. It explicitly excludes anyone enrolled in Medicare, Medicaid, VA, TRICARE, and DoD beneficiaries. The Bridge is your path. The $50 per fill through the Bridge is your price.
TRICARE coverage for Foundayo
Short answer: TRICARE's pharmacy benefit is administered by Express Scripts as the Department of Defense's contractor. The current TRICARE PA form for weight-loss GLP-1s names Wegovy and Zepbound. Foundayo is not yet specifically named on that form as of May 1, 2026 — verify TRICARE Formulary Search before assuming coverage.
TRICARE 2026 pharmacy copays
For most beneficiaries — verify your specific category at tricare.mil/Costs:
| Pharmacy | Generic | Formulary brand | Nonformulary |
|---|---|---|---|
| Military pharmacy | $0 (when available) | $0 (when available) | $0 (when available) |
| Home delivery | (verify category) | $44 | $85 |
| Retail network | (verify category) | $48 | $85 |
Medically retired/survivor rates differ. TFL beneficiaries and direct-care-only categories have specific eligibility rules — verify at tricare.mil/Costs/PharmacyCosts.
Submitting a PA
Until TRICARE updates its PA form to include Foundayo specifically, your prescriber should reference the existing weight-loss GLP-1 criteria when submitting.
TRICARE PA contact: 1-866-684-4488 (phone) or 1-866-684-4477 (fax). For Active Duty Service Members, the PA form must still be initially submitted even if coverage won't be approved; reconsideration is available at the Military Treatment Facility per Military Department-specific policies.
Foundayo vs. Wegovy vs. Zepbound on Express Scripts
Short answer: On Express Scripts plans, Wegovy injection, Wegovy tablets, and Zepbound pens already appear as preferred alternatives in the public 2026 exclusions document. Foundayo (FDA-approved April 1, 2026) is the new option and isn't yet listed by name.
| Foundayo (orforglipron) | Wegovy (semaglutide) | Zepbound (tirzepatide) | |
|---|---|---|---|
| FDA approval for weight loss | April 1, 2026 | June 2021 (injection); Dec 2025 (pill) | November 2023 |
| Form | Oral pill, once daily, no food/water timing | Weekly injection or daily pill | Weekly injection (KwikPen, single-dose pens, vials) |
| Average weight loss in trials | ~11.1% (ATTAIN-1, highest dose treatment-regimen estimand) | ~15% (injection, STEP-1) | ~21% (SURMOUNT-1, highest dose completers) |
| 2026 ES NPF status | Not in public NPF or exclusions PDF by name | Listed as preferred alternative in exclusions PDF | Pens: preferred alternative · Vials: excluded |
| Manufacturer-direct self-pay starting price | $149/mo (LillyDirect, 0.8 mg) | $149/mo (NovoCare, Wegovy pill) | $299/mo (LillyDirect Journey, 2.5 mg) |
| Manufacturer savings card with commercial coverage | As low as $25/mo | As low as $0/mo for eligible patients | As low as $25/mo |
| Medicare Bridge eligible (July 1, 2026) | All formulations ✅ | All formulations ✅ | KwikPen only |
Cross-trial comparison only. These efficacy numbers come from different Phase III trials with different study populations, durations, and designs. They are not head-to-head trial results, and direct comparisons should be interpreted with caution. Talk to a clinician about which medication fits your situation.
Is Foundayo medically right for you just because Express Scripts covers it?
No. Insurance coverage answers payment, not medical fit.
Foundayo's FDA label includes specific contraindications and warnings every patient should review with a clinician before starting. A coverage page that hides safety limitations is a sales page, not a trustworthy resource.
Foundayo is contraindicated in patients with:
- Personal or family history of medullary thyroid carcinoma (MTC) or Multiple Endocrine Neoplasia syndrome type 2 (MEN 2)
- Serious hypersensitivity to orforglipron or any of the product's components
Warnings and precautions on the FDA label include:
- Risk of thyroid C-cell tumors (boxed warning)
- Acute pancreatitis
- Severe gastrointestinal disease
- Acute kidney injury related to volume depletion (from severe nausea, vomiting, or diarrhea)
- Hypoglycemia when used with insulin or insulin secretagogues
- Acute gallbladder disease
- Pulmonary aspiration during anesthesia or deep sedation
- Reduced effectiveness of oral hormonal contraceptives
- Diabetic retinopathy complications in patients with type 2 diabetes
- Suicidal behavior and ideation (general class warning for weight-management products)
- Not recommended in patients with severe hepatic impairment
This page is not medical advice. Talk to a licensed clinician before starting any GLP-1 medication.
Frequently asked questions
Does Express Scripts cover Foundayo?
It depends on your specific plan. Express Scripts is a pharmacy benefit manager that administers thousands of distinct employer, Medicare, and TRICARE plans, each with its own formulary. As of May 1, 2026, Foundayo is not on the public 2026 Express Scripts National Preferred Formulary or its exclusions PDF by name. That's not a confirmation of coverage and not a confirmation of denial — verify in your member portal or by calling the number on your ID card.
Why isn't Foundayo showing up in my Express Scripts account?
Foundayo just launched in April 2026, so a "not found" result often means the drug isn't yet loaded in the plan's database — not necessarily that your plan won't cover it. Search both "Foundayo" and "orforglipron" (the generic name). If neither shows results, call member services and ask whether the drug is "not loaded yet" versus excluded.
How much does Foundayo cost with Express Scripts insurance?
If your plan covers Foundayo and you have commercial insurance, the Foundayo Savings Card can bring your cost to as low as $25/month, subject to monthly and annual savings limits. If your plan doesn't cover it, LillyDirect self-pay is $149/month for the 0.8 mg starter dose, $199 for 2.5 mg, $299 for 5.5 mg or 9 mg, and either $299 (with the 45-day refill offer) or $349 for 14.5 mg or 17.2 mg. Medicare Bridge enrollees pay $50 per fill starting July 1, 2026.
Does Express Scripts require prior authorization for Foundayo?
It may. Express Scripts has not published Foundayo-specific public PA criteria. If your plan covers Foundayo, it will likely apply criteria similar to its existing weight-loss GLP-1 PA rules, which typically require BMI of 30 or higher (or 27 with at least one weight-related condition), documentation of prior lifestyle attempts, and a Letter of Medical Necessity from the prescriber.
What is EncircleRx and do I have to enroll in Omada?
EncircleRx is Express Scripts' weight management program that pairs GLP-1 medications with a lifestyle coaching component, often Omada. If your employer's plan participates in EncircleRx, enrolling in Omada (or another assigned engagement program) may be required to get prior authorization approval for any weight-loss GLP-1, including Foundayo. Engagement rules vary by plan — ask member services.
Does Cigna cover Foundayo?
Cigna members should verify coverage in myCigna and on their ID card. The Cigna Group includes Evernorth Health Services, which includes Express Scripts as its PBM, but the PBM and drug list shown on your specific ID card determine your benefits. Use the call script in this guide to confirm.
Does TRICARE cover Foundayo?
TRICARE's public FAQ lists eligible weight-loss medication coverage categories including Prime, Prime Remote, US Family Health Plan, Select, Young Adult, Reserve Select, Retired Reserve, and Continued Health Care Benefit Program. The current TRICARE PA form names Wegovy and Zepbound; Foundayo is not yet specifically named on that form as of May 1, 2026. Verify TRICARE Formulary Search before assuming coverage.
What if Express Scripts denies my Foundayo prior authorization?
Your denial letter will state the specific reason and your appeal deadline. Submit a Letter of Medical Necessity from your prescriber with full BMI history and documentation of weight-related conditions. Ask whether your plan offers peer-to-peer review. If the denial is based on a plan exclusion (your employer chose not to cover weight-loss meds), medical necessity appeals usually won't reverse it — self-pay or switching plans at open enrollment become your real options.
Can I use the Foundayo Savings Card with Medicare?
No. The Foundayo Savings Card explicitly excludes anyone enrolled in Medicare, Medicare Part D, Medicare Advantage, Medigap, Medicaid, VA, DoD, or TRICARE/CHAMPUS. Medicare members can access Foundayo at $50 per fill through the Medicare GLP-1 Bridge starting July 1, 2026.
How long does Express Scripts prior authorization take for Foundayo?
Express Scripts says nearly all coverage reviews are completed within two days after the prescriber sends complete information. Electronic prior authorization (ePA) determinations can come back within minutes for some requests. Faster processing can be requested if your prescriber considers the situation urgent.
Where can I get Foundayo if my insurance doesn't cover it?
The manufacturer-direct path is LillyDirect at $149/month for the starter dose, rising by dose. Telehealth providers offering Foundayo include Ro and Hims/Hers, both of which now publicly list Foundayo among their FDA-approved GLP-1 options. Use official or verifiable pharmacy channels.
Your next move
If you want to do the verification yourself for free: log into Express Scripts and run the call script in the How to check your specific plan section above. Total cost: a phone call.
If you want help cutting through the insurance maze: Ro's free GLP-1 Insurance Coverage Checker contacts your insurer for you, sends a written report, and handles the prior authorization paperwork if you decide to start treatment. Foundayo and Zepbound are both available through Ro.
If your plan won't cover it and you want to start anyway: LillyDirect is the manufacturer-direct verified self-pay path at $149/month for the starter dose. Ro pairs the same medication price with clinical support and insurance help.
If you're a Medicare member: mark July 1, 2026 on your calendar — that's the Bridge launch date. Confirm with your prescriber that you meet the CMS Bridge BMI and condition criteria, and have them ready to submit the Bridge PA on day one.
If you're a TRICARE member: verify TRICARE Formulary Search for Foundayo before paying cash, and have your prescriber submit PA referencing the existing weight-loss GLP-1 criteria.
Free to use. Ro Body $39 for the first month if you start, then as low as $74/month with annual plan paid upfront. Medication billed separately. Government plans (Medicare/Medicaid/TRICARE/VA) excluded; FEHB may be eligible.
What we verified, what we didn't, and when this gets updated
Sources we cross-checked: Express Scripts 2026 National Preferred Formulary PDF, Express Scripts 2026 NPF Exclusions PDF, Express Scripts coverage-review and prior-authorization FAQ, Express Scripts EncircleRx Patient FAQ, TRICARE Prior Authorization Form for semaglutide/tirzepatide, TRICARE 2026 Pharmacy Costs page, CMS Medicare GLP-1 Bridge official page and FAQ, Foundayo manufacturer pricing and Savings Card terms (foundayo.lilly.com), LillyDirect Foundayo product page (lilly.com), FDA-approved Foundayo prescribing information, Eli Lilly's Foundayo FDA approval press release with ATTAIN-1 results, NovoCare Wegovy savings offers, KFF 2025 Employer Health Benefits Survey, and Ro / Hims / Hers public Foundayo pages.
What we did not verify: Any specific member's plan coverage. The deciding answer for your coverage is in your member portal — not in any guide. This page exists to help you find your answer faster.
Published:
Last verified: May 1, 2026 · Next review: June 2026 (monthly through December 2026, quarterly thereafter)
Why monthly: Foundayo's formulary status is changing plan by plan as Express Scripts catches up to the April 2026 launch.
Related guides
About this guide. The RX Index is a pricing intelligence and comparison resource for GLP-1 telehealth providers. We are not a medical practice. This content is educational and is not medical advice. Always talk to a licensed clinician before starting any GLP-1 medication. We earn affiliate commissions on some partner links — they don't change our verification process or our recommendations. See our editorial standards.