Wegovy HD Insurance Coverage: Does Insurance Cover the 7.2 mg Dose?
By The RX Index Editorial Team · Last verified:
The RX Index is a pricing intelligence and comparison resource for GLP-1 telehealth providers.
Disclosure: Some links on this page are affiliate links. If you purchase through these links, we may earn a commission at no extra cost to you.

The bottom line on Wegovy HD insurance coverage in 2026
Wegovy HD insurance coverage is limited right now. NovoCare's official coverage checker currently states that no insurance coverage is available for Wegovy injection 7.2 mg, while the verified self-pay price through official channels is $399 per month. The important nuance: NovoCare's savings program already includes Wegovy HD-specific pricing and commercial-insurance language, so coverage may change as plans update their formulary and NDC files. But you should not assume coverage exists today — verify with your plan directly.
Wegovy HD coverage answer at a glance
| Your situation | Likely coverage answer | Best next step |
|---|---|---|
| Commercial insurance, trying to cover Wegovy HD | Currently limited; verify plan-specific HD/NDC coverage | Run a coverage check and ask about NDC 00169-4572-14 |
| Commercial insurance, standard Wegovy is covered | HD may still require a separate check or PA | Ask if the HD NDC is on your formulary |
| No insurance / paying cash | Verified HD self-pay price is $399/month | Compare NovoCare or GoodRx self-pay paths |
| Medicare beneficiary | Medicare GLP-1 Bridge access begins July 1, 2026 for eligible patients | Review Bridge eligibility and PA requirements |
| Medicaid beneficiary | State-dependent; 13 fee-for-service Medicaid programs covered GLP-1s for obesity as of January 2026 | Check your state Medicaid plan and PA rules |
Damaging admission:
Wegovy HD is not the easiest path if your main goal is using insurance today. NovoCare's own coverage checker currently says no insurance coverage is available for Wegovy injection 7.2 mg. That does not mean you are out of options — it means you should verify standard Wegovy, Wegovy pill, or another FDA-approved GLP-1 before committing to the $399/month HD self-pay route.
Check your GLP-1 coverage before paying cash →
Ro's free GLP-1 Insurance Coverage Checker contacts your plan and produces a personalized report for FDA-approved GLP-1 medications — including Wegovy and Zepbound — with prior-authorization detail and cost estimates. Use this before you commit to $399/month cash.
Run Ro's free GLP-1 coverage check →The Wegovy HD Coverage Reality Matrix
Most “Wegovy coverage” pages give you generic answers about standard Wegovy. This matrix isolates the 7.2 mg HD dose specifically and reconciles the contradictions across NovoCare, the FDA, GoodRx, CMS, KFF, and the major payer policies — every row sourced, every cell timestamped. Last verified across all rows: .
| Coverage path | Applies to Wegovy HD 7.2 mg? | Verified cost / copay | What it means for you | Source |
|---|---|---|---|---|
| NovoCare official coverage checker | Yes, HD-specific lookup | Currently states: no insurance coverage available for Wegovy injection 7.2 mg; self-pay remains an option | Strongest available signal that broad insured HD coverage is not in place yet. Do not assume plan coverage without HD-specific verification. | NovoCare |
| NovoCare self-pay / savings program | Yes | $399 / 1 month, $798 / 2 months, $1,197 / 3 months; NDC 00169-4572-14 | If insurance does not cover HD, this is the current official self-pay floor. | NovoCare savings terms |
| Commercial insurance + savings card ($25 path) | Conditional | As low as $25/month with HD savings capped at $100 / 1 month, $200 / 2 months, $300 / 3 months; government beneficiaries excluded | Not proof HD is covered today. The savings card reduces a covered copay; it does not create coverage. | NovoCare savings terms |
| GoodRx self-pay access | Yes | $399/month, $798/2 months, $1,197/3 months | Useful fallback if you have an HD prescription and you're not using insurance. | GoodRx |
| FDA approval status | Yes | FDA-approved March 2026 | Confirms Wegovy HD is an FDA-approved brand medication, not a compounded substitute. | FDA |
| Wegovy prescribing information | Yes | Step-up to 7.2 mg only after tolerating 2.4 mg once weekly for at least 4 weeks and when additional weight reduction is clinically indicated | This is why HD is rarely a “starter” prescription, which affects PA documentation. | Novo Nordisk PI |
| CVS/Caremark public PA criteria | Partially / plan-specific | Adult weight management treated separately; HD excluded from certain non-weight-management pathways | Demonstrates that “Wegovy is covered” does not automatically mean “Wegovy HD is covered.” | CVS Caremark PA |
| Prime / HCSC public PA-QL example | Yes, listed | Wegovy HD 7.2 mg with quantity limit of 4 pens / 28 days | Shows some payer documents already recognize HD in their utilization-management workflows. | Prime / HCSC |
| Medicare GLP-1 Bridge (eligible beneficiaries) | Yes, beginning July 1, 2026 | $50 copay through Humana as centralized processor (BIN/PCN 028918 / MEDDGLP1BR) | Separate pathway from normal Part D. Requires PA criteria. Coupons generally do not stack. | CMS Bridge |
| Medicaid coverage for obesity drugs | State-dependent | 13 state Medicaid FFS programs covered GLP-1s for obesity treatment as of January 2026; PA common | Medicaid readers need a state-specific check, not a national yes/no. | KFF |
This matrix is assembled, source-linked, timestamped analysis pulled from sources a typical reader would otherwise need an hour and 10+ tabs to reconcile.
Why this is confusing for real patients
A typical version of this question posted publicly on GLP-1 community threads reads: “Has anyone been able to get their insurance to cover Wegovy HD, the newer higher dose version.”
Being on standard Wegovy 2.4 mg does not automatically answer whether the 7.2 mg HD dose is covered. The product is new. The NDCs are different. Many payers haven't updated their formularies to address HD specifically. And NovoCare itself is currently saying no insurance coverage is available — while simultaneously publishing HD-specific savings-card terms and self-pay pricing. That mixed signal is the source of most of the confusion.
Does insurance cover Wegovy HD right now?
Short answer: Wegovy HD insurance coverage appears limited right now. NovoCare's official coverage checker currently states no insurance coverage is available for Wegovy injection 7.2 mg. The safest move is to verify the HD-specific NDC with your plan before assuming coverage — even if your plan covers standard Wegovy.
Why “Wegovy is covered” does not automatically mean “Wegovy HD is covered”
A pharmacy benefit decides what's covered at four different levels:
- Drug name — the molecule itself (semaglutide).
- Brand and formulation — Wegovy injection vs Wegovy pill vs Ozempic.
- Dose / strength — the 2.4 mg pen vs the new 7.2 mg HD pen.
- NDC (National Drug Code) — the 11-digit identifier that uniquely tags the SKU at the pharmacy claim level.
A plan can say yes at levels 1 and 2 (semaglutide and Wegovy) while saying no — or “not yet adjudicated” — at levels 3 and 4. When you call your plan, you want them looking at the specific HD NDC, not just “Wegovy.”
The confusing part: why the savings-card terms still mention HD
NovoCare's savings program terms list HD self-pay pricing alongside language that talks about commercially insured patients paying as little as $25/month. That language is present in the terms, but it does not override the current coverage-checker result. Today, in most cases, the $25/month copay path on Wegovy HD is theoretical.
Don't pay cash before verifying what your plan actually covers →
Ro's free GLP-1 Insurance Coverage Checker contacts your plan directly and returns a personalized report across Wegovy, Wegovy pill, Zepbound, and other FDA-approved GLP-1 options.
Run a free GLP-1 coverage check →How much does Wegovy HD cost with and without insurance?
Short answer: The verified self-pay price for Wegovy HD 7.2 mg is $399 for one month, $798 for two months, or $1,197 for three months through verified self-pay channels (NovoCare's program and GoodRx). If a commercial plan eventually covers HD and you qualify for the savings program, eligible patients may pay less — but government beneficiaries are excluded from the savings offer entirely, even when they pay cash.
Verified Wegovy HD self-pay pricing
| Route | 1-month price | Runs through insurance? | Counts toward deductible / OOP max? |
|---|---|---|---|
| NovoCare self-pay program | $399 | No | No |
| GoodRx Wegovy HD access | $399 | No | No |
| Commercial insurance with HD coverage + savings card (eligible patients) | As low as $25 (HD 1-month savings cap: $100) | Yes | Yes (plan-paid portion) |
| Insurance fill without savings card | Plan-specific (deductible / coinsurance applies) | Yes | Yes |
Prices documented on NovoCare's savings/eligibility page and corroborated by GoodRx's Wegovy HD access announcement. Self-pay costs processed outside insurance will not count toward your insurance deductible or out-of-pocket maximum.
What about the $25 Wegovy savings card?
The $25/month savings path applies to:
- Eligible commercially insured patients with coverage for the prescribed Wegovy formulation.
- Patients within program savings caps — for Wegovy HD, NovoCare's published caps are up to $100 in savings on a 1-month prescription, $200 on 2 months, and $300 on 3 months.
- Patients not enrolled in government plans — Medicare, Medicaid, TRICARE, VA, and similar plans are excluded, even when they pay as self-paying patients.
The savings card reduces a covered copay; it does not create coverage where none exists. If your plan does not cover Wegovy HD specifically, savings-card math doesn't apply to HD even if you have great commercial insurance.
What to actually ask your insurer
“I'm asking about Wegovy HD 7.2 mg injection, NDC 00169-4572-14. Is this NDC on my formulary? Does it require prior authorization, step therapy, or a quantity limit? If standard Wegovy is covered on my plan, does that coverage automatically include the 7.2 mg HD dose, or is HD on a separate formulary line?”
Asking by NDC forces a specific answer. Asking “does my plan cover Wegovy” gets you a generic answer that may be wrong for HD.
Skip the call queue →
Ro's free GLP-1 Insurance Coverage Checker contacts your plan for you and returns a personalized coverage and PA report. Use it as your first move, then call your plan only if you need to clarify something.
Run Ro's free GLP-1 coverage check →Who qualifies for Wegovy HD medically?
Short answer: Wegovy HD is not a starter dose. The FDA-approved prescribing information says adults using Wegovy injection for weight reduction may step up to 7.2 mg only after tolerating 2.4 mg once weekly for at least 4 weeks and when additional weight reduction is clinically indicated.
The FDA approved Wegovy HD as a new higher-dose 7.2 mg semaglutide injection in March 2026. It uses the same molecule as standard Wegovy at a higher weekly dose, with its own NDC. It is an FDA-approved brand-name medication from Novo Nordisk — not a compounded preparation.
Why this matters for your insurance
If your plan does cover Wegovy HD, the PA criteria will typically require your prescriber to document:
- That you've already been on standard Wegovy 2.4 mg.
- That you tolerated it at 2.4 mg for an adequate duration.
- That additional weight reduction is clinically indicated — typically a plateau or insufficient response.
- Your BMI / weight history and any qualifying comorbidities the plan considers.
Safety note (read the prescribing information for the full list)
Wegovy carries a boxed warning and is contraindicated in patients with a personal or family history of medullary thyroid carcinoma (MTC) or Multiple Endocrine Neoplasia syndrome type 2 (MEN 2). The most common adverse reactions involve gastrointestinal effects.
The FDA noted that altered skin sensation (dysesthesia) occurred more often at the 7.2 mg dose than at 2.4 mg in clinical studies — approximately 22% at 7.2 mg vs 6% at 2.4 mg vs 0.3% on placebo. Discuss this with your prescriber before stepping up. Review the full prescribing information before starting, switching, or stepping up.
What prior authorization rules are likely for Wegovy HD?
Short answer: Most Wegovy coverage paths require prior authorization, and Wegovy HD should be checked at the dose/NDC level, not just the brand level. The practical move is to ask for the exact PA criteria before assuming coverage.
What prior authorization typically asks for on Wegovy HD
- A covered indication for weight management on your specific plan.
- BMI documentation — usually BMI ≥30, or ≥27 with at least one weight-related comorbidity.
- Weight-related comorbidity documentation (type 2 diabetes, hypertension, dyslipidemia, sleep apnea, cardiovascular disease, etc.).
- Prior weight-management program documentation, where applicable.
- Current Wegovy dose history — what dose, how long, what response.
- Tolerability — that you handled 2.4 mg for at least the labeled period.
- Step therapy — whether the plan wants you to have tried other GLP-1s, other anti-obesity medications, or specific lifestyle programs first.
- Quantity limits — pens per fill, fills per year.
PA Policy Crosswalk: two large public PA documents compared on Wegovy HD
| Item | CVS / Caremark public PA criteria | Prime / HCSC public weight-management PA-QL |
|---|---|---|
| Wegovy HD recognized as separate product? | Yes, with HD-specific language under adult weight management criteria | Yes, listed in policy |
| BMI criteria | BMI ≥30, or ≥27 with comorbidity | BMI ≥30, or ≥27 with comorbidity |
| Lifestyle-program requirement | Documentation of dietary and physical activity counseling typically expected | Documentation of dietary and physical activity counseling typically expected |
| 2.4 mg tolerance prerequisite for HD | Reflected in HD-specific clinical criteria | Reflected in HD-specific clinical criteria |
| Quantity limit | Per published criteria | 4 pens / 28 days for Wegovy HD 7.2 mg |
| Source | CVS Caremark PA document | Prime / HCSC weight-management program summary |
Your “give this to your prescriber” checklist
- Insurance card (front and back) and pharmacy benefit card if separate.
- Pharmacy benefit phone number from the back of the card.
- Current medication list.
- Wegovy dose history with dates (when you started 2.4 mg, current dose, fill history).
- BMI and weight history — measured weights over time, not estimates.
- Relevant diagnoses (ICD-10 codes if you can get them).
- Documentation of any prior weight-management attempts the plan may want to see.
- Any prior denial letter or PA correspondence.
- The exact NDC you want filled: 00169-4572-14.
Get a coverage report you can hand to your prescriber →
Ro's free GLP-1 Insurance Coverage Checker returns a personalized report you can bring to your appointment. Faster than going round and round with your plan on the phone, and useful regardless of whether you ultimately fill through Ro.
Get a personalized coverage report →What if my insurance covers Wegovy but not Wegovy HD?
Short answer: This is one of the most common scenarios right now. A plan can cover standard Wegovy 2.4 mg and still not cover the new 7.2 mg HD dose. Ask your plan to look up the exact Wegovy HD NDC (00169-4572-14) and tell you whether the issue is formulary exclusion, missing prior authorization, a quantity limit, or dose-specific noncoverage — because each leads to a different next step.
Standard Wegovy NDCs differ from HD's NDC. Wegovy HD 7.2 mg: 00169-4572-14. Standard Wegovy doses have their own NDCs by strength. If your plan covers one strength, that does not guarantee they cover all of them.
Your options if Wegovy HD is not covered
- Stay on covered standard Wegovy 2.4 mg if it's still clinically appropriate and you and your prescriber agree HD is not urgent.
- Ask whether Wegovy pill is covered as an alternative. Ro publicly stocks Wegovy pill with insurance concierge support.
- Ask whether another FDA-approved GLP-1 is covered. Zepbound (tirzepatide) is one FDA-approved adult weight-management alternative your plan may list differently from Wegovy.
- Appeal the HD denial with clinical rationale, especially if the denial reason is missing PA documentation rather than a hard formulary exclusion.
- Pay cash at $399/month if HD is genuinely the right fit and you can absorb the cost.
- Recheck coverage every 30–60 days. This is a new product. Formularies update. What's denied today can be approved next quarter.
What should I do if insurance denies Wegovy HD?
Short answer: First, identify why the denial happened. A formulary exclusion, missing PA, step-therapy requirement, non-covered indication, quantity limit, or dose-specific denial each requires a different response. Read the denial letter and match the response to the reason.
The denial-reason map
| Denial reason | What it means | What to do | Evidence to attach |
|---|---|---|---|
| Not on formulary | Plan does not cover Wegovy HD at all | Ask about standard Wegovy, Wegovy pill, Zepbound, or other covered alternatives | Denial letter, formulary printout, list of alternatives you'd accept |
| Prior authorization required | Plan needs documentation before paying | Have your prescriber submit the full PA with the criteria the plan specifies | Plan's PA criteria, BMI documentation, dose history, comorbidity ICD-10s, lifestyle-program records |
| Prior authorization denied | Documentation didn't meet criteria | Request the denial letter and the appeal pathway, then resubmit with what was missing | Denial letter, the specific criteria you didn't meet, prescriber letter of medical necessity |
| Step therapy required | Plan wants other treatment(s) tried first | Ask exactly what satisfies step therapy and document if you've already met it | Fill history of prior therapies, dates tried, tolerability records |
| Quantity limit | Plan limits pens / fills per period | Request a quantity-limit exception with clinical rationale | Prescriber letter justifying QL exception, dosing records |
| Non-covered indication | Plan covers some indications but not weight management | Ask whether any covered indication applies (only if clinically accurate) | Diagnosis documentation, prescriber letter |
| Coupon error on a government plan | Manufacturer copay savings cannot be used | Use the Medicare or Medicaid pathway specific to your plan | Plan ID showing government enrollment, alternate route documentation |
Appeal or exception script
“I received a denial for Wegovy HD 7.2 mg, NDC 00169-4572-14. Please send me: the denial reason in writing, the complete prior authorization criteria, the appeal process and deadline, and confirmation of whether the denial is based on the medication, the indication, the dose, or the specific NDC.”
When not to appeal
If your plan has a hard exclusion on anti-obesity medications across the board, or explicitly excludes Wegovy HD, an appeal is usually not the fastest path. Your time is better spent checking coverage on other FDA-approved GLP-1s, asking HR about open enrollment options, or pricing $399/month self-pay against your timeline.
Does Medicare cover Wegovy HD?
Short answer: Traditional Medicare Part D has historically excluded medications used solely for weight loss. CMS has announced a Medicare GLP-1 Bridge scheduled to run July 1, 2026 through December 31, 2027. Beginning July 1, 2026, all formulations of Wegovy — including Wegovy HD 7.2 mg, NDC 0169-4572-14 — will be available to eligible Part D beneficiaries through the Bridge with a $50 copay, subject to PA criteria.
The Medicare GLP-1 Bridge: eligibility and operational details
| Bridge detail | What CMS says |
|---|---|
| Window | July 1, 2026 through December 31, 2027 |
| Scope | Available nationwide to eligible Part D beneficiaries |
| Wegovy formulations covered | All formulations, including Wegovy HD 7.2 mg, NDC 0169-4572-14 |
| Eligibility — clinical pathways (must meet one) | BMI ≥35; or BMI ≥30 with specified conditions; or BMI ≥27 with specified cardiovascular / prediabetes conditions |
| Additional eligibility | Wegovy must be prescribed for weight reduction with ongoing lifestyle modification |
| Prior authorization | Yes — Bridge access requires meeting PA criteria |
| Claim flow | Centralized through Humana as Bridge processor (BIN/PCN 028918 / MEDDGLP1BR), not your normal Part D plan |
| Patient cost | $50 copay collected at the pharmacy |
| Manufacturer coupon stacking | Generally not allowed on top of the Bridge |
| TrOOP credit | Not counted as a Part D claim |
Source: CMS Medicare GLP-1 Bridge
Why most Medicare readers should not start with a generic provider CTA
Ro explicitly says it cannot help coordinate GLP-1 coverage for government insurance plans (Federal Employee Health Benefits is an exception). The right next step for a Medicare reader is understanding Bridge eligibility and PA documentation.
Find your GLP-1 path based on your coverage type →
The quiz routes Medicare scenarios to Bridge eligibility and Part D context, commercial scenarios to coverage-check options, and uninsured scenarios to verified self-pay paths.
Take the free 60-second matching quiz →Does Medicaid cover Wegovy HD?
Short answer: Medicaid coverage for Wegovy HD is state-dependent and sometimes plan-dependent within a state. As of January 2026, KFF data shows only 13 state Medicaid fee-for-service programs covered GLP-1s for obesity treatment, and prior authorization is common where coverage exists.
The 13 states with Medicaid fee-for-service GLP-1 obesity coverage as of January 2026
DE · KS · MA · MI · MN · MO · MS · NC · RI · TN · UT · VA · WI
Source: KFF Medicaid GLP-1 coverage tracker, as of January 2026
Even if your state appears on this list: your managed-care Medicaid plan inside that state may have its own formulary and PA criteria; your state may cover GLP-1s for obesity but not specifically Wegovy HD until formularies update; and your state may require specific BMI/comorbidity documentation, lifestyle-program participation, or step therapy.
What Medicaid readers should ask
“Does my Medicaid plan cover Wegovy HD 7.2 mg injection, NDC 00169-4572-14, for my diagnosis? Is my coverage through fee-for-service or a managed-care plan? What prior authorization criteria apply? If Wegovy HD is not covered, what GLP-1 medications are covered on this plan?”
Find the coverage path for your insurance type →
Take the free 60-second matching quiz →Is Wegovy HD cheaper through NovoCare, GoodRx, Ro, or a pharmacy?
Short answer: For Wegovy HD self-pay, the verified floor is $399/month through NovoCare's program and GoodRx's HD access program. Ro is most useful for insurance checking and FDA-approved GLP-1 support — Wegovy HD-specific cash-pay routing through Ro was not verified as of .
- If you already have a Wegovy HD prescription and you're paying cash: Compare NovoCare and GoodRx self-pay (both at $399/month) and confirm your pharmacy can dispense the correct NDC.
- If you need help with the insurance side: A coverage-check tool or insurance concierge. Ro's free GLP-1 Insurance Coverage Checker contacts your plan, returns a personalized coverage report with PA detail, and lists Wegovy pill, Wegovy pen, Foundayo, Zepbound pen, and Zepbound KwikPen options. Use the checker before you spend money on cash-pay HD if there's any chance your plan would cover Wegovy, Wegovy pill, Zepbound, or Foundayo.
- If you're not sure HD is right for you: A clinical evaluation through an FDA-approved GLP-1 telehealth program before paying for HD specifically. Don't pay $399/month on assumption.
Provider-fee warning (so you're not surprised)
Telehealth GLP-1 programs typically charge a membership or program fee separate from the medication price. For example, Ro's Body program is publicly listed at: $39 for the first month (intro pricing), $149/month ongoing, or as low as $74/month with annual prepay. Medication is billed separately from the membership.
What documents should I collect before checking Wegovy HD coverage?
Short answer: Collect your insurance card, prescription/pharmacy benefit card, prescriber details, your Wegovy dose history, your BMI/weight history, your relevant diagnoses, and any prior denial letter — before you call your plan. The goal is to keep your plan from giving you a generic “Wegovy” answer when you need a Wegovy HD 7.2 mg-specific answer.
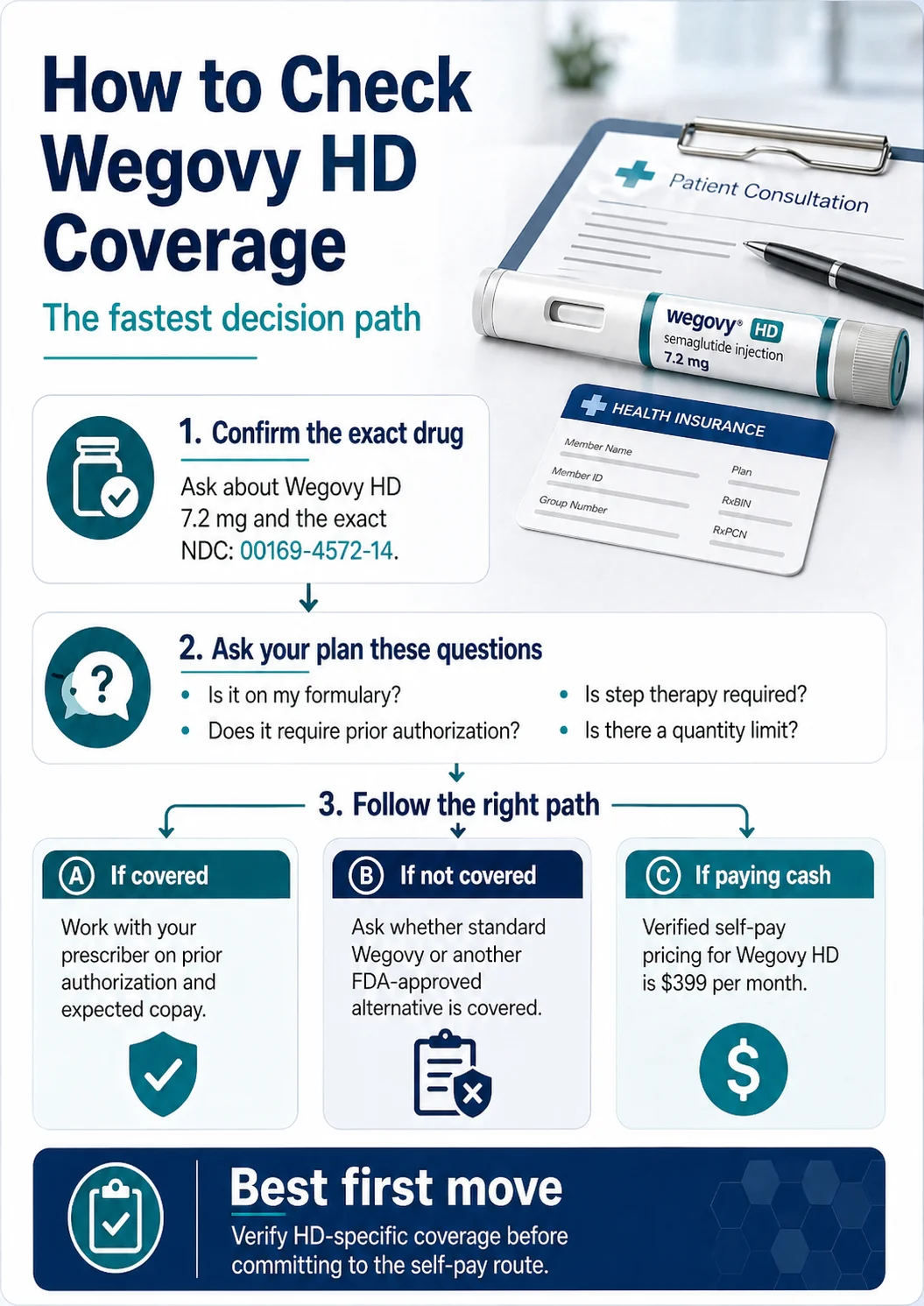
The pre-call checklist
- Insurance card (front and back).
- Pharmacy benefit info: RxBIN, RxPCN, RxGRP, member ID.
- Plan name (commercial group, individual marketplace, Medicare, Medicaid, etc.).
- Pharmacy benefit phone number.
- Your current Wegovy dose and the date you started 2.4 mg.
- Tolerability notes — any side effects you've had, how you handled them.
- Relevant diagnoses (and ICD-10 codes if you can get them).
- BMI and weight history with measured weights, ideally from your prescriber's records.
- Lifestyle-program documentation, if your plan requires evidence of prior effort.
- Prior denial letter, if one exists.
- The exact NDC: 00169-4572-14.
Questions to ask your plan
- Is Wegovy HD 7.2 mg (NDC 00169-4572-14) on my formulary?
- If so, what tier is it on? What's my copay or coinsurance after deductible?
- Is prior authorization required? Can you send me the criteria?
- Is step therapy required? What satisfies it?
- Is there a quantity limit?
- What documents does my prescriber need to submit?
- What's my appeals or exception process if PA is denied?
Find your fastest Wegovy HD path
Match yourself to the closest scenario below for your next move.
| Your scenario | Most likely path | First documents | First call or check |
|---|---|---|---|
| Commercial insurance + on 2.4 mg 4+ weeks + want to use insurance | NDC-specific HD coverage check + PA preparation | Dose history, BMI/weight history, comorbidity ICD-10s, tolerability notes | Run a free coverage check, then book your prescriber for PA submission |
| Commercial insurance + HD already denied | Identify denial reason, then either appeal or pivot | Denial letter, plan PA criteria, prescriber letter of medical necessity | Read the denial letter; appeal if it's a documentation issue, otherwise consider standard Wegovy or Zepbound |
| Commercial insurance + standard Wegovy covered, HD status unknown | NDC-level lookup (HD vs 2.4 mg) | Insurance card, pharmacy benefit phone number, NDC 00169-4572-14 | Call the pharmacy benefit number with the HD NDC |
| Uninsured / paying cash + willing to pay $399 | Verified self-pay channel comparison | HD prescription | Compare NovoCare and GoodRx self-pay; confirm pharmacy can fill the correct NDC |
| Uninsured / paying cash + not sure HD is right | Clinical evaluation before committing to cash | Weight history, current GLP-1 status (if any) | Take the matching quiz to see whether HD or another option fits |
| Medicare beneficiary + obesity indication only | Wait for Bridge (July 1, 2026) and review eligibility now | BMI/weight, comorbidity documentation | Read the Bridge eligibility table above, plan for PA |
| Medicare beneficiary + cardiovascular indication | Possible standard Part D coverage outside Bridge | CV diagnosis documentation | Call your Part D plan with NDC and CV indication code |
| Medicaid beneficiary in a covering FFS state | State-specific check including managed-care plan | Medicaid card, diagnosis, BMI documentation | Call state Medicaid member services with HD NDC |
| Medicaid beneficiary in a non-covering state | Non-obesity indication review or other GLP-1 | Diagnosis documentation | Call member services to confirm what is covered |
| Employer plan with broad anti-obesity exclusion | Skip the appeal, pivot to alternatives | HR plan summary documents | Talk to HR about open enrollment options; price $399/month self-pay |
Want a personalized version? →
Take the free 60-second GLP-1 matching quiz to get a routing recommendation tailored to your insurance type, medical history, and budget.
Take the free 60-second matching quiz →Related guides on The RX Index
- Wegovy HD Prior Authorization — the deeper PA documentation packet, criteria, and appeal-letter workflow
- Wegovy HD vs Wegovy Pill — formulation comparison if you're choosing between the two
- Wegovy Savings Card — how the NovoCare savings program actually works
- Best GLP-1 Providers That Accept Insurance — for readers who want to start with insurance from day one
- GLP-1 Pancreatitis Risk — symptoms, FDA label rates, and red flags
- Find My GLP-1 Path quiz — the personalized routing tool
How we verified this Wegovy HD insurance coverage guide
Last verified: .
What we actually verified:
- FDA approval status and press announcement for the 7.2 mg dose
- The current Wegovy prescribing information, including adult weight-reduction dosing language and the boxed warning
- NovoCare's official Wegovy coverage checker output for the 7.2 mg injection
- NovoCare's self-pay and savings program terms, including HD-specific pricing, per-fill savings caps, and government-beneficiary exclusion language
- GoodRx's Wegovy HD access announcement and self-pay pricing
- CMS's Medicare GLP-1 Bridge page, including covered formulations, Wegovy HD NDC, Humana processor, BIN/PCN, and eligibility clinical pathways
- KFF's Medicaid GLP-1 coverage tracker, including the 13-state fee-for-service obesity-coverage list as of January 2026
- Public CVS/Caremark prior authorization criteria for Wegovy
- Public Prime Therapeutics / HCSC weight-management program summary listing Wegovy HD
What still needs verification on update:
- Whether NovoCare's coverage checker still returns “no insurance coverage available” for Wegovy injection 7.2 mg. If it flips, the headline of this page changes.
- Whether GoodRx still lists Wegovy HD at $399/month.
- Whether Ro has added Wegovy HD-specific cash-pay availability or HD-specific routing through the coverage checker (currently flagged as not verified as of April 28, 2026).
Why we don't recommend compounded providers on this page
Wegovy HD is an FDA-approved brand-name medication from Novo Nordisk. This page covers FDA-approved-brand insurance intent. Compounded semaglutide programs are a different product governed by different regulatory rules. We won't blur those two product categories on this page, on principle.
Published by: The RX Index Editorial Team. This page is not medical, insurance, legal, or benefits advice. Confirm clinical decisions with a licensed clinician. Confirm coverage decisions with your insurer or plan administrator.
Frequently asked questions about Wegovy HD insurance coverage
Is Wegovy HD covered by insurance?
Wegovy HD insurance coverage appears limited right now. NovoCare’s coverage checker currently states that no insurance coverage is available for Wegovy injection 7.2 mg, so verify the HD-specific NDC (00169-4572-14) with your plan before assuming coverage — even if your plan covers standard Wegovy 2.4 mg.
How much does Wegovy HD cost without insurance?
The verified self-pay price for Wegovy HD 7.2 mg is $399 for one month, $798 for two months, or $1,197 for three months through NovoCare’s program and through GoodRx’s HD access announcement, as of the verification date on this page.
Can I get Wegovy HD for $25?
Only with eligible commercial insurance covering Wegovy HD specifically and savings card eligibility. The HD savings cap is up to $100 on a 1-month fill, $200 on 2 months, and $300 on 3 months. Government beneficiaries (Medicare, Medicaid, TRICARE, VA, etc.) are excluded — even when paying cash. Because NovoCare’s checker currently returns no HD insurance coverage available, the $25 path is largely theoretical for HD today.
What is the Wegovy HD NDC?
NovoCare lists the NDC as 00169-4572-14 on its self-pay/savings page. CMS lists the same product as 0169-4572-14 in its Medicare GLP-1 Bridge formulary list (the leading zero is sometimes dropped depending on formatting). Both refer to the same Wegovy HD 7.2 mg injection product.
Does a Wegovy prior authorization automatically cover Wegovy HD?
Not necessarily. Many plans treat Wegovy HD as a separate dose-level or NDC-level coverage decision. Ask your plan to look up Wegovy HD by NDC 00169-4572-14 and confirm whether your existing PA, if any, applies to the 7.2 mg HD dose specifically.
Can I start directly on Wegovy HD?
No. The FDA-approved prescribing information for Wegovy injection used for adult weight reduction supports stepping up to 7.2 mg only after tolerating 2.4 mg once weekly for at least 4 weeks and when additional weight reduction is clinically indicated. Expect insurance pushback on starting at HD with no 2.4 mg history.
Does Medicare cover Wegovy HD?
Through the Medicare GLP-1 Bridge scheduled to run July 1, 2026 through December 31, 2027, all Wegovy formulations including Wegovy HD 7.2 mg will be available to eligible Part D beneficiaries with a $50 copay, subject to prior authorization, processed centrally through Humana. Outside the Bridge, normal Part D rules apply and Part D historically does not cover drugs used solely for weight loss.
Who qualifies for the Medicare GLP-1 Bridge?
Per CMS, eligible Part D beneficiaries must meet one of the published clinical pathways: BMI ≥35; or BMI ≥30 with specified conditions; or BMI ≥27 with specified cardiovascular or prediabetes conditions. Wegovy must be prescribed for weight reduction with ongoing lifestyle modification, and PA criteria must be met before the Bridge will pay.
Does Medicaid cover Wegovy HD?
State-dependent. KFF reported that 13 state Medicaid fee-for-service programs covered GLP-1s for obesity treatment as of January 2026 (DE, KS, MA, MI, MN, MO, MS, NC, RI, TN, UT, VA, WI), with prior authorization common. Even within those states, managed-care plans may have different rules. Call your state Medicaid plan to verify Wegovy HD coverage by NDC.
What if my plan covers standard Wegovy but not HD?
Ask your plan to look up Wegovy HD by NDC and identify whether the issue is formulary exclusion, missing prior authorization, a quantity limit, or a hard exclusion. Depending on the answer, your best move may be to appeal, stay on covered standard Wegovy, switch to another FDA-approved GLP-1 (like Wegovy pill or Zepbound), or pay $399/month cash for HD.
Can Ro check Wegovy HD coverage?
Ro publicly offers a free GLP-1 Insurance Coverage Checker that contacts your plan and returns a personalized report covering FDA-approved GLP-1 medications, with prior-authorization detail and cost estimates. Wegovy HD 7.2 mg-specific routing through Ro was not verified as of April 28, 2026. Ro also cannot help coordinate GLP-1 coverage for government insurance plans (Federal Employee Health Benefits is an exception).
Is Wegovy HD the same as compounded semaglutide?
No. Wegovy HD is an FDA-approved brand-name medication manufactured by Novo Nordisk at the higher 7.2 mg dose. Compounded semaglutide is prepared by 503A or 503B pharmacies and operates under different regulatory rules. The two are different products.
How often should I recheck Wegovy HD coverage?
For Wegovy HD specifically, recheck monthly. The product is new, payer formularies are updating, and what’s denied today can be approved next quarter as plans finish reviewing the HD dose. Set a calendar reminder.
Final word
Wegovy HD is a real FDA-approved option for the right patient, and the coverage picture should improve as more plans finish adjudicating the new dose. But the honest answer in 2026 is that you should not assume Wegovy HD is covered just because Wegovy is. Verify the NDC with your plan. Use a coverage check before paying cash. Know your fallback options across other FDA-approved GLP-1s. And if HD genuinely is the right path and you're paying cash, the floor is $399/month through verified self-pay channels.
Still not sure which GLP-1 program is right for you?
Take our free 60-second matching quiz — it routes Medicare, Medicaid, commercial, and uninsured scenarios to the right next step based on your situation.
Take the free 60-second GLP-1 matching quiz →