Best GLP-1 Providers That Accept Insurance in 2026
By The RX Index Editorial Team · Last verified: April 2, 2026 · Affiliate disclosure
The best GLP-1 provider that accepts insurance for most people is Ro. After reviewing insurance processes across a dozen telehealth platforms, Ro’s dedicated insurance concierge checks your coverage, submits prior-authorization paperwork, and helps navigate denials — all for FDA-approved GLP-1 options like Wegovy and Zepbound. In Ro’s own Insurance Coverage Checker dataset, half of covered patients had a copay of $50/month or less.
But here’s what most comparison sites won’t tell you: “accepts insurance” means three different things depending on the provider. Some bill your visits to insurance. Some help get your medication covered. Some do both. And some are cash-pay memberships that still do a better job fighting for prior authorization than going through your regular doctor’s office alone. We reviewed exactly what each provider does — and doesn’t do — so you can pick the right one for your situation.
No payment · No commitment to check coverage

Best GLP-1 Providers That Accept Insurance: Quick Comparison
Every number in this table was verified from each provider’s official pricing, FAQ, and terms pages in April 2026. “Prior Auth Help” means the provider’s team submits PA paperwork on your behalf — not just that they hand you a form.
| Provider | Visits Billed? | Prior Auth Help? | Program Cost | ||
|---|---|---|---|---|---|
| Ro ★ | ❌ Membership cash-pay | ✅ Full concierge | $45 mo1 · $145/mo | ||
| Form Health | ✅ Most plans + Medicare | ✅ Team advocates | $299/mo self-pay | ||
| WW Clinic | ⚠️ Varies by plan | ✅ Coordinators (commercial) | $25 mo1 · $74/mo (12-mo) | ||
| PlushCare | ✅ Most major commercial | ✅ Team reaches out | ~$129/visit or copay | ||
| Knownwell | ✅ Most plans + Medicare | ✅ Yes | $0 signup · $299 first visit | ||
| Found | ✅ Some commercial plans | ✅ Supports documentation | $39/mo (in-network) | ||
| Check Your GLP-1 Insurance Coverage on Ro — Free → | |||||
“Accepts Insurance” Means Three Different Things — Know Which Before You Choose
This is the single most important distinction in GLP-1 telehealth, and it’s why people waste weeks picking the wrong provider.
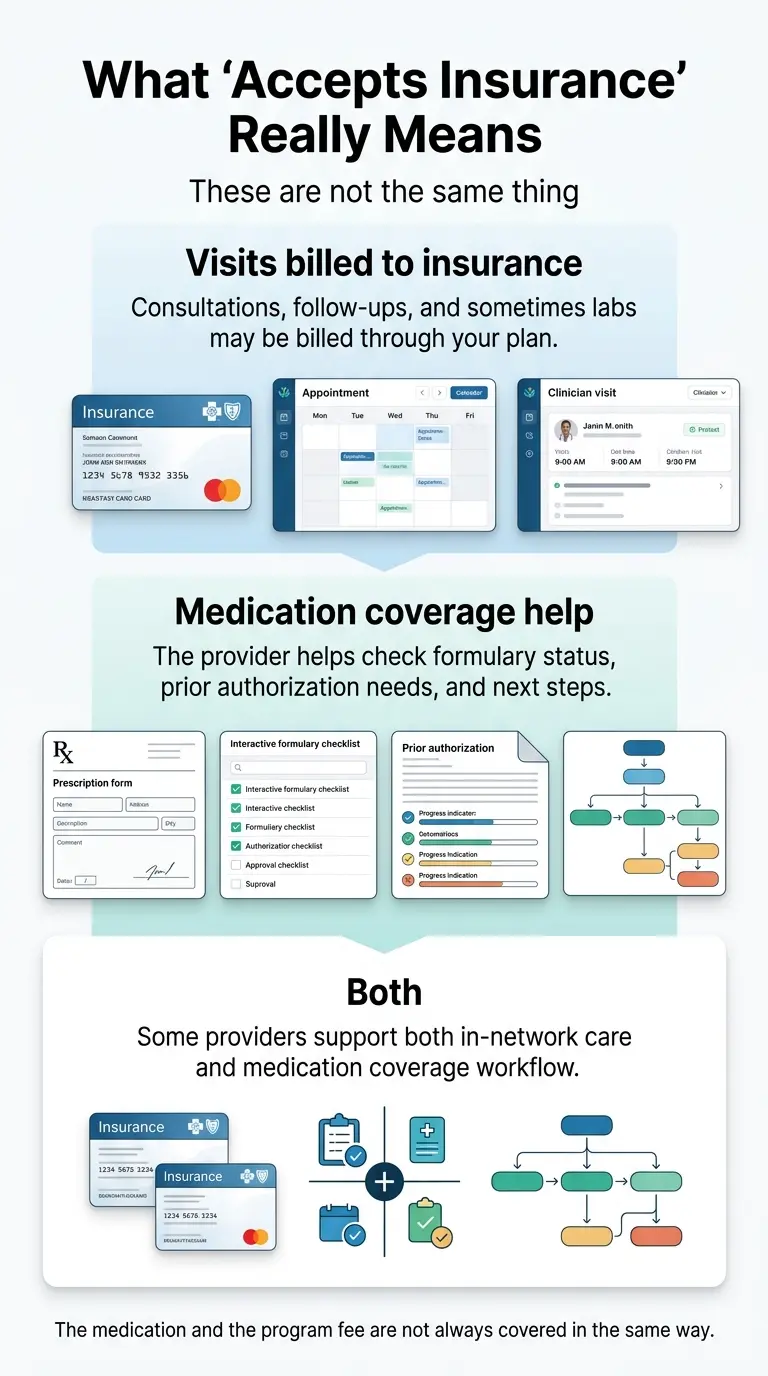
Level 1 — Visits billed to insurance
The provider is in-network with your insurer, so your consultations, check-ins, and possibly lab work are billed through your plan. Form Health, PlushCare, and Knownwell work this way. You still need separate coverage for the medication itself.
Level 2 — Medication coverage help
The provider’s team actively works with your insurer to determine whether your GLP-1 prescription will be covered and handles the prior authorization process. Ro does this exceptionally well. Your visits aren’t billed to insurance, but the medication might be — and that’s where the real money is.
Level 3 — Both
A handful of providers bill visits to insurance AND help with medication coverage. Form Health and Knownwell come closest to this model.
Why does this matter? Because medication is by far the largest expense. A telehealth visit might run $50–$150. Brand-name Wegovy without insurance is listed around $1,350/month. The provider that’s best at getting your medication covered saves you dramatically more than one that merely bills your visits.
That’s why Ro tops our list despite its cash-pay membership: it’s focused on the part that actually costs the most — getting the medication covered.
Which Provider Is Right for Your Insurance Situation?
Not every provider fits every plan. Here’s how to find yours fast.
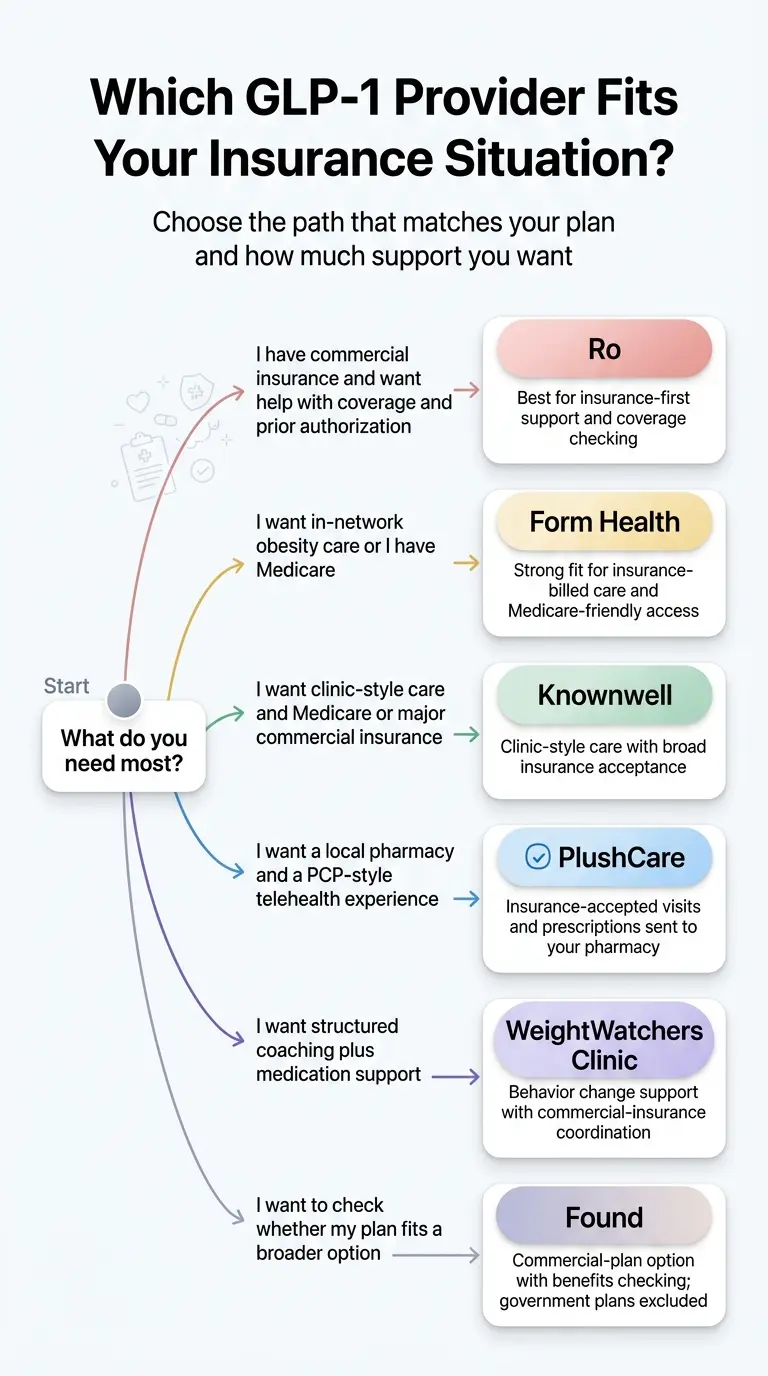
You have commercial insurance through an employer →
Best fit: Ro
Their concierge checks coverage, submits PA paperwork, and navigates denials. If your medication is covered, you'll likely pay just a copay. If not, Ro can pivot you to cash-pay FDA-approved options.
You want visits AND medication billed in-network →
Best fit: Form Health or Knownwell
Both accept most major commercial insurers, and Form Health also accepts Medicare.
You have Medicare →
Best fit: Form Health or Knownwell
Ro cannot coordinate most government-plan coverage. Form Health and Knownwell both accept Medicare now. The Medicare GLP-1 Bridge launching July 2026 will add a $50/month path for eligible Part D beneficiaries.
You want medication + a structured lifestyle coaching program →
Best fit: WeightWatchers Clinic
Their care team includes insurance coordinators for commercial plans, and the behavioral program has decades of evidence behind it.
You prefer a traditional doctor-and-pharmacy model →
Best fit: PlushCare
In-network with most major commercial insurers, prescriptions go to your local pharmacy, and their team helps with PA.
Your plan excludes weight-loss drugs entirely →
Best fit: Cash-pay options
Skip to our 'What to Do When Insurance Says No' section below. You have better options than you think.
#1. Ro — Best Overall for Insurance Coverage
Ro wins this list because its insurance concierge does the thing that actually matters: helping commercially insured patients get FDA-approved GLP-1 medication covered, and handling the paperwork that stops most people cold.
Verified from Ro’s official pages (April 2026):
- ✓Insurance concierge included with the $145/mo Ro Body membership ($45 first month)
- ✓Concierge helps determine coverage, submits prior-authorization paperwork, and navigates appeals
- ✓Prescribes FDA-approved GLP-1 options: Wegovy (injection and pill) and Zepbound; Ozempic may be prescribed off-label when clinically appropriate
- ✓Metabolic lab testing at Quest locations included if your provider orders it; at-home kit $75 if Quest isn't in your state
- ✓LegitScript certified
- ✓In Ro's Coverage Checker data: 43% of users had GLP-1 coverage, and among covered patients, half had a copay of $50/month or less
- ✓Cash-pay backup: FDA-approved options from $149/mo (Wegovy pill, starting dose)
- ✓Prepay & Save option for additional cash-pay savings
What makes Ro’s insurance concierge different
When you join, your provider determines which GLP-1 is clinically appropriate. Then Ro’s concierge team takes over the insurance side — checking your formulary, preparing and submitting the prior-authorization package, and following up. If it gets denied, they help with the appeal.
The PA process is where most people get stuck, because insurers deny incomplete submissions automatically. Having a team that does this daily is a meaningful advantage over asking your general practitioner to handle it.
What you’ll actually pay through Ro
| Scenario | Monthly Total |
|---|---|
| Membership only (month 1) | $45 |
| Membership ongoing | $145/month |
| With insurance + savings card (medication as low as) | $145 + $25 = ~$170/mo |
| Cash-pay: Wegovy pill starting dose | $145 + $149 = ~$294/mo |
| Cash-pay: Wegovy injection 12-mo sub | $145 + $249 = ~$394/mo |
The honest tradeoff
Ro’s membership does NOT accept insurance. You’ll pay $145/month for the program regardless of your coverage. If having every visit billed in-network is your non-negotiable, Form Health or PlushCare is the better fit.
But consider the math: when Ro’s concierge gets your medication covered and you stack a manufacturer savings card, your total monthly cost is $145 (membership) plus your copay — which is often well under $100. Compare that to $349–$1,350/month for the medication alone without coverage.
“Easy upfront pricing and interaction. Also good value.” — Verified Ro patient, Trustpilot
Built for:
- ✓You have commercial insurance through an employer
- ✓You want someone else handling the insurance paperwork
- ✓You want FDA-approved medications only
- ✓You want a fallback plan if insurance says no
Look elsewhere if:
- ✗You have Medicare or Medicaid → see Form Health or Knownwell
- ✗You need visits billed in-network → see Form Health or PlushCare
- ✗You want compounded GLP-1s → see our cash-pay comparison
Ready to let someone else handle the insurance headache?
Ro's concierge checks coverage, submits prior auth, and navigates appeals — included in your membership.
Check Your Insurance Coverage on Ro — Free →#2. Form Health — Best for In-Network Care and Medicare
If you want your entire weight-loss program — visits, labs, medication — billed through insurance, Form Health is the provider to evaluate first.
Form Health operates more like a traditional obesity medicine clinic than a consumer telehealth subscription. Their clinical team includes obesity-trained physicians, and they structure care around ongoing clinical relationships with regular check-ins, lab monitoring, and treatment adjustments.
Verified from Form Health’s official pages (April 2026):
- ✓Visits, labs, and medication costs covered by most major private insurance and Medicare, subject to patient responsibility
- ✓Team reviews coverage, submits prior authorizations, and advocates for patients
- ✓Requires an ongoing PCP relationship and meeting BMI criteria
- ✓Self-pay option: $299/month if insurance doesn't cover the program
- ✓FDA-approved medications only
- ✓Members can cancel at any time and receive a transition plan
- ✓Available virtually in most U.S. states
The real value here: Form Health doesn’t just help with paperwork — they actually bill your visits to your insurance plan. For people with solid insurance that includes obesity care, the total out-of-pocket can be remarkably low because consultations, lab work, and clinical management may all be covered.
Built for:
- ✓You want comprehensive obesity medicine, not just a prescription
- ✓You want visits AND medication billed to insurance
- ✓You have Medicare
- ✓You have a PCP who will coordinate with your Form clinician
Look elsewhere if:
- ✗You want the cheapest entry point → Ro's first month is $45 vs Form's $299 self-pay
- ✗You want a quick, lightweight process → Form is more thorough but also more clinical
External link · Not an affiliate
#3. WeightWatchers Clinic — Best for Lower Monthly Fee and Lifestyle Coaching
WeightWatchers Clinic is the right choice if you want medication paired with a structured behavioral program — and you want insurance help baked in at a lower monthly program fee.
Their care team includes insurance coordinators who work with commercial insurance plans to help maximize your medication coverage. The clinical program prescribes FDA-approved GLP-1 options including Wegovy (pen and pill), Zepbound, and other approved medications depending on clinical fit. In a study of 3,250 WW Clinic patients, members prescribed a GLP-1 lost an average of 21% of their body weight at 12 months.
Verified from WeightWatchers’ official pages (April 2026):
- ✓Care team includes insurance coordinators for commercial plans
- ✓$25 first month with 12-month Med+ plan, then $74/month (GLP-1 cost separate)
- ✓FDA-approved medications: Wegovy pen, Wegovy pill, Zepbound, and other clinically appropriate options
- ✓Medication delivered to your door or sent to pharmacy of choice
- ✓Includes WW app, coaching, community, and meal tracking
- ✓Non-GLP-1 medications may be included with membership if clinically appropriate
Built for:
- ✓You want medication AND a behavior-change program
- ✓You have commercial insurance
- ✓You want a lower monthly program fee ($74/mo vs $145 at Ro)
- ✓You plan to maintain your weight loss long-term
Look elsewhere if:
- ✗You want month-to-month flexibility → Ro has no annual commitment
- ✗You have Medicare → Form Health or Knownwell
- ✗You just want the medication without lifestyle coaching → Ro or PlushCare
#4. PlushCare — Best for Local Pharmacy and PCP-Style Telehealth
PlushCare is the right pick if you want the experience of visiting a regular doctor — just virtually — with your prescription sent to your local pharmacy.
PlushCare is in-network with most major commercial insurers. Their physician/care team reaches out to insurers for prior authorization on your behalf. Because prescriptions go to a retail pharmacy you choose, you can use manufacturer savings cards directly at the counter.
Verified from PlushCare’s official pages (April 2026):
- ✓In-network with most major commercial insurers
- ✓Care team reaches out for prior auth on your behalf
- ✓Self-pay visit: ~$129 or your insurance copay
- ✓Prescriptions sent to your local pharmacy of choice
- ✓General telehealth platform (not obesity-specific)
- ✓FDA-approved medications
The honest tradeoff: PlushCare is a broad telehealth platform, not a weight-loss specialty service. You’ll get a real doctor and real insurance support, but not the dedicated concierge experience Ro provides or the obesity-focused clinical depth of Form Health. Think of it as your virtual PCP who can also prescribe GLP-1s — reliable, but not specialized.
Built for:
- ✓You prefer picking up prescriptions at your local pharmacy
- ✓You want a PCP-style relationship with insurance billing
- ✓You have commercial insurance
Look elsewhere if:
- ✗You have Medicare Part B (no longer accepted as of Jan 2026)
- ✗You want specialized obesity medicine → Form Health
- ✗You want maximum PA support → Ro's concierge is more dedicated
#5. Knownwell — Best Clinic-Style Care Without a Subscription Fee
Knownwell is the strongest option if you want real clinic-style obesity care without a recurring subscription.
They accept Medicare and most major commercial insurance plans, offer nationwide virtual care, and charge no sign-up fees or membership dues. You pay per visit — $299 for the first visit and $149 for follow-ups if self-paying — or your insurance copay if covered.
What we confirmed from Knownwell (April 2026):
- ✓Accepts Medicare and most major commercial insurance
- ✓No sign-up fees or membership dues
- ✓Self-pay: $299 first visit / $149 follow-ups
- ✓Virtual care available nationwide
- ✓FDA-approved medications only
- ✓Prior authorization support included
Built for:
- ✓You want clinic-quality care without a monthly subscription
- ✓You have Medicare and want a provider that actually accepts it
- ✓You prefer paying per visit, not per month
Look elsewhere if:
- ✗You want maximum insurance concierge support → Ro does that better
- ✗You want a full lifestyle coaching program → WW Clinic is more comprehensive
#6. Found — Worth Checking If Your Plan Is In Their Network
Found is worth a look if your commercial insurer happens to be in their network and you want flexibility across medication types.
Found says it offers in-network pricing for eligible commercial insurance plans. Their insurance specialists check coverage on your behalf and deliver a personalized report. The medication mix is broader than most providers listed here — Found offers both FDA-approved and compounded options.
What we confirmed from Found’s official pages (April 2026):
- ·In-network pricing for some commercial insurance plans
- ·Insurance specialists check coverage and deliver a free report
- ·Both FDA-approved and compounded medication options
- ·Insurance option starts at $39/month or $199/year; self-pay plans higher
- ·Board-certified obesity medicine clinicians
- ·Free GLP-1 Insurance Checker tool
Only choose Found if your commercial plan is confirmed in their network
How Much Will You Actually Pay? Full Cost Breakdown
This is the question that sends people back to Bing. Let’s close it.
Program Fees (Before Medication)
| Provider | First Month | Ongoing Monthly |
|---|---|---|
| Ro | $45 | $145 |
| Form Health | Covered by insurance or $299 | Same |
| WW Clinic | $25 | $74 |
| PlushCare | Insurance copay or ~$129 | Per visit |
| Knownwell | Insurance copay or $299 | $149/visit self-pay |
| Found | $39 (insurance) or higher | Same |
Medication Costs (With and Without Insurance)
| Scenario | Wegovy Pen | Wegovy Pill |
|---|---|---|
| Commercial insurance + savings card | As low as $25/mo | As low as $25/mo |
| Cash-pay (manufacturer direct) | $199 first 2 mo, then $349+/mo | $149 starting, $299/mo higher doses |
Prices as of April 2026. Government insurance beneficiaries (Medicare, Medicaid) are generally not eligible for manufacturer savings cards. Verify current pricing directly.
No payment required to check coverage
GLP-1 Insurance Coverage Is Getting Harder in 2026
You need to understand the landscape you’re walking into. GLP-1 insurance coverage got harder for many people this year, and that’s exactly why choosing the right provider matters more now than a year ago.
42% more people lost Wegovy coverage in 2026
GoodRx reported that the number of people with no commercial insurance coverage for Wegovy increased 42% in 2026 compared to 2025 — leaving over 41 million people uncovered.
Zepbound coverage also dropped significantly
Over 109 million Americans now lack Zepbound coverage. CVS Caremark removed Zepbound from its standard formulary in mid-2025.
Prior authorization still required for most
Even for people who do have coverage, over 88% still face prior authorization requirements before their insurer will pay.
Only ~19% of large employers cover GLP-1s for weight loss
The KFF Employer Health Benefits Survey found only about 19% of large employer plans cover GLP-1 medications when used primarily for weight loss.
But here’s the counter-trend working in your favor: Manufacturer cash-pay pricing has dropped dramatically. Wegovy pill and Lilly’s new Foundayo pill both start at $149/month for self-pay patients — a fraction of the old retail price. Medicare coverage is coming through the GLP-1 Bridge in July 2026. And providers like Ro have built dedicated insurance concierge teams that navigate PA processes at scale.
The bottom line: if your insurance might cover GLP-1s, you need a provider that fights for every dollar you’re entitled to. If it won’t, you need a provider with affordable backup options. The providers on this page do one or both.
How GLP-1 Insurance Coverage Actually Works (Step by Step)
Understanding the process removes the mystery — and helps you pick the right provider.

Step 1: Check if your plan covers weight-loss medication
Key question: Is any GLP-1 on your formulary specifically for weight management, or only for type 2 diabetes? That distinction determines whether you’ll face an uphill fight or a straightforward approval.
Step 2: Understand prior authorization
Missing any single element — an outdated BMI measurement, incomplete lab results, missing documentation of prior diet attempts — can trigger a denial. This is exactly why providers with dedicated insurance teams tend to have better outcomes.
Step 3: Wait for the decision (1–3 weeks)
Step 4: If approved — stack your savings
- ·Wegovy/Ozempic (Novo Nordisk): Eligible commercially insured patients may pay as low as $25/month with the savings card
- ·Zepbound (Eli Lilly): Savings card can bring costs as low as $25/month with commercial coverage
- ·Foundayo (Eli Lilly): Eligible commercially insured patients may pay as low as $25/month
Government insurance beneficiaries (Medicare, Medicaid) are generally not eligible for manufacturer savings cards.
Step 5: If denied — don't stop here
The denial letter tells you why, and the reason determines your strategy:
- ·“Not medically necessary” → Appeal with additional clinical documentation (updated BMI, comorbidity records, physician letter of necessity)
- ·“Formulary exclusion” → Request a formulary exception with clinical rationale for why alternatives aren’t appropriate for you
- ·“Step therapy required” → Document that you’ve tried lower-cost alternatives without adequate results
- ·“Plan excludes weight-loss drugs” → Go through HR if employer-sponsored; some employers add coverage when employees request it. Otherwise, cash-pay is your best path.
Don't want to navigate this alone?
Ro's concierge handles PA submissions AND appeals — included in the $145/month membership.
Get Started with Ro →What to Do When Insurance Says No
Let’s say you’ve exhausted the insurance path. Your plan excludes weight-loss drugs, the appeal didn’t work, or you simply don’t want to wait weeks while your motivation is high. You still have strong options.
First: Make sure it’s really a “no”
Not all denials are final. If it’s a paperwork issue (missing documentation, wrong diagnosis code), your provider can resubmit. If it’s a step therapy requirement, documenting a clinical reason to skip that step may satisfy it. If it’s a formulary exclusion, request a formulary exception — insurers are legally required to have a process for this.
Only if your plan categorically excludes weight-loss medication is it a true dead end on the insurance path.
Option 1: FDA-approved medications at manufacturer direct pricing
Both Novo Nordisk and Eli Lilly now sell directly to consumers at prices dramatically lower than retail:
Option 2: Compounded GLP-1s as a clearly labeled fallback
If FDA-approved options are still out of reach, compounded semaglutide and tirzepatide are available at lower prices. Important: Compounded medications are not FDA-approved and are not covered by insurance plans. For a detailed comparison including both FDA-approved and compounded options, see our cash-pay GLP-1 comparison guide.
Option 3: Use HSA/FSA to reduce your costs
If you have a Health Savings Account or Flexible Spending Account, GLP-1 medications prescribed for a medical condition (obesity, type 2 diabetes) are generally eligible expenses. Most providers accept HSA/FSA cards for medication costs, and some accept them for membership fees too. Using pre-tax dollars effectively reduces your cost by your marginal tax rate — often 20–35%.
Do Any Online GLP-1 Providers Take Medicare?
Yes — but only some, and the landscape is changing fast.
Current Medicare status by provider (April 2026):
Starting July 1, 2026 — the Medicare GLP-1 Bridge
CMS is launching the Medicare GLP-1 Bridge, a short-term demonstration running through December 31, 2026. Eligible Medicare Part D beneficiaries will be able to access Wegovy (injection and tablets) and Zepbound with a $50/month copay. Prior authorization goes through a central CMS processor — not your individual Part D plan. Manufacturer savings cards and discount programs cannot be applied to Bridge claims.
Bridge eligibility criteria (per CMS):
- ·BMI ≥35, OR BMI ≥30 with one or more qualifying conditions (type 2 diabetes, cardiovascular disease, hypertension, chronic kidney disease, heart failure, others per CMS criteria), OR BMI ≥27 with other specified conditions
- ·Must be enrolled in an eligible Medicare Part D plan
- ·Provider submits prior authorization to the CMS central processor
If you’re on Medicare — what to do now:
- 1.Talk to your doctor. Get BMI and qualifying conditions documented.
- 2.Ask your provider to prepare PA documentation for when the Bridge opens in July.
- 3.Consider Form Health or Knownwell for immediate access before July.
- 4.During Medicare open enrollment this fall (Oct 15 – Dec 7), check whether your Part D plan will join the permanent BALANCE Model starting January 2027.
What About the New GLP-1 Pills?
Two oral GLP-1 options are now FDA-approved for weight loss — and both are relevant to the insurance question.
Wegovy Pill (Novo Nordisk)
Approved December 2025
- Average weight loss: 16.6% at highest dose
- Self-pay starting: $149/month (NovoCare)
- With insurance + card: As low as $25/month
- Dosing: Daily, 30 min before food, with small amount of water
Foundayo / orforglipron (Eli Lilly)
Approved April 1, 2026
- Average weight loss: 12.4% at highest dose
- Self-pay starting: $149/month (LillyDirect)
- With insurance + card: As low as $25/month
- Dosing: Daily, no food or water restrictions
Why pills matter for the insurance conversation: Oral GLP-1s have lower manufacturer cash-pay pricing than injectables, which gives you a more affordable fallback if insurance coverage is denied. They also eliminate the needle barrier that stops some people from starting treatment altogether.
Why Every Provider on This List Is FDA-Approved First
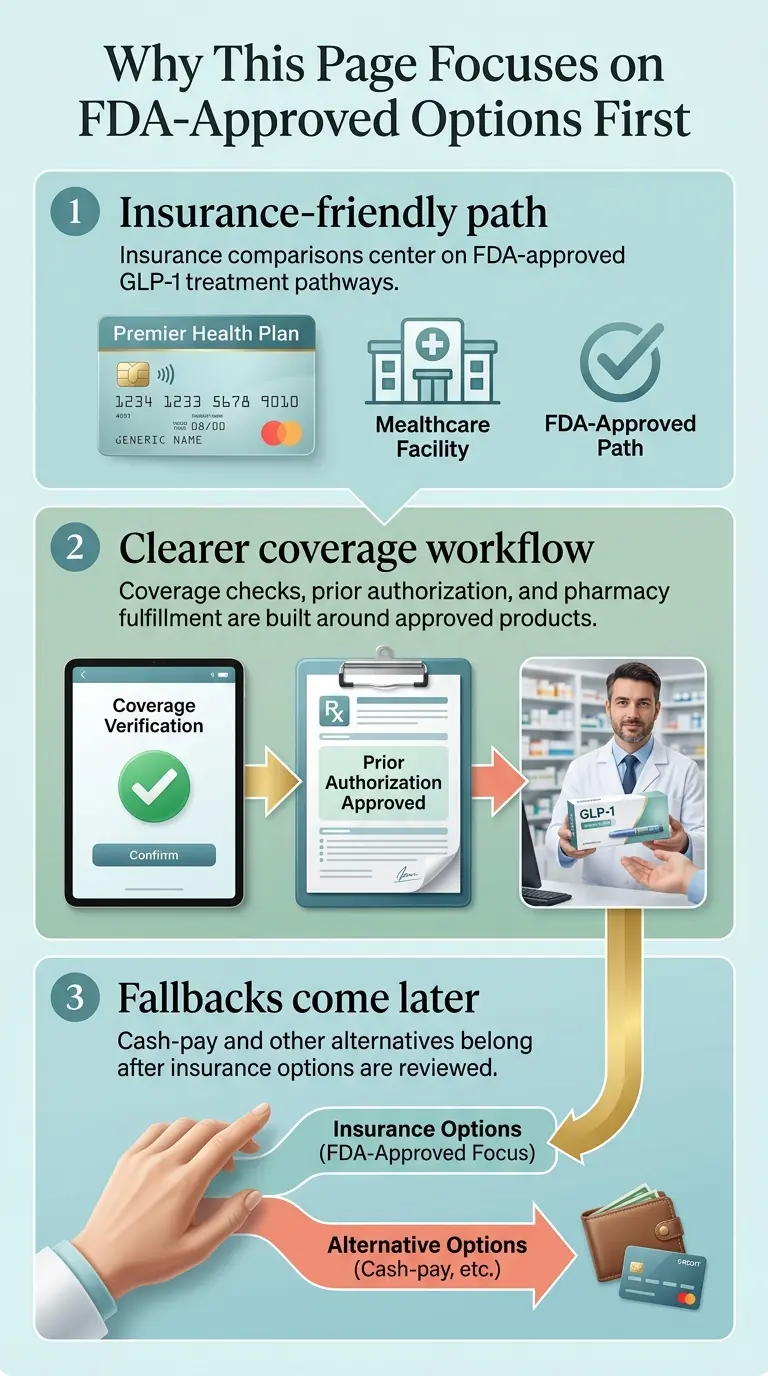
Every provider in our main comparison prescribes FDA-approved GLP-1 medications. That’s deliberate.
If you’re searching for providers that accept insurance, you need FDA-approved drugs. Insurance coverage pathways — formulary listings, prior authorization, manufacturer savings cards — are built around FDA-approved products, not compounded copies.
In March 2026, the FDA issued warning letters to 30 telehealth companies over misleading marketing of compounded GLP-1s. The agency reinforced that compounded copies are permitted only under limited conditions and have not undergone FDA review for safety, effectiveness, or quality.
We include compounded options as a clearly labeled fallback in our cash-pay comparison guide for readers whose insurance path doesn’t work out. But on this page — which exists to help you navigate insurance — FDA-approved is the starting point.
How Hard Is It to Cancel or Switch Providers?
Most comparison pages avoid this section. We don’t.
| Provider | Flexibility | Notes |
|---|---|---|
| Ro | ⭐⭐⭐ Most flexible | Month-to-month, cancel anytime before renewal |
| Knownwell | ⭐⭐⭐ Most flexible | No subscription — nothing to cancel |
| PlushCare | ⭐⭐⭐ | Per-visit model; no subscription to cancel |
| Form Health | ⭐⭐ Moderate | Cancel anytime with transition plan provided |
| Found | ⭐⭐ Moderate | Monthly subscription; some users report friction with cancellation timing |
| WeightWatchers | ⭐ Longest commitment | 12-month plan, auto-renews; may owe remaining balance if you cancel early |
If you switch providers mid-treatment: Your new provider will need your medical records, current dosage, and recent lab results. Most platforms can request records on your behalf. The bigger question is insurance: if your new provider handles PA differently, you may need to restart the authorization process. Ask before switching.
Our recommendation: Start with a month-to-month provider (Ro, Knownwell) so you can evaluate the insurance process without risk. Once you’re confident in the fit, a longer-term commitment can save money.
How We Reviewed and Ranked These Providers
Every provider on this page was evaluated against the same criteria:
| Criterion | Weight |
|---|---|
| Insurance workflow quality | 30% |
| Cost clarity | 20% |
| Clinical credibility | 15% |
| Plan-type fit | 15% |
| Cancellation flexibility | 10% |
| State availability & fulfillment | 10% |
All claims are sourced from each provider’s official website, manufacturer pricing pages, CMS publications, or peer-reviewed data as of April 2026.
Frequently Asked Questions
What is the best GLP-1 provider that accepts insurance?
Ro is the best choice for most commercially insured adults. Their insurance concierge helps with coverage checks, prior authorizations, and appeals for FDA-approved GLP-1s like Wegovy and Zepbound. If you need in-network visits or Medicare support, Form Health or Knownwell are stronger fits.
Do any online GLP-1 providers take Medicare?
Form Health and Knownwell both accept Medicare. The Medicare GLP-1 Bridge program launching July 2026 will provide eligible Part D beneficiaries access to Wegovy and Zepbound at a $50/month copay.
Do I need prior authorization for Wegovy or Zepbound?
Almost always. Over 88% of people with GLP-1 coverage face additional requirements like prior authorization. Choosing a provider that handles PA on your behalf makes a meaningful difference.
Do any online GLP-1 providers actually bill insurance for visits?
Yes. Form Health, PlushCare, and Knownwell bill visits directly to insurance. Ro's membership is cash-pay, but its concierge focuses on getting your medication covered through your insurer.
Will insurance cover Wegovy for weight loss?
It depends on your specific plan. About 40–50% of commercial plans offer some form of GLP-1 coverage for weight loss, often with prior authorization required. Coverage is more common when prescribed alongside a qualifying condition like type 2 diabetes, cardiovascular disease, or sleep apnea.
What if my insurance denies my GLP-1 prescription?
Read the denial letter, identify the specific reason, and consider appealing. Fewer than 1% of denials are appealed, but a meaningful percentage succeed when they are. Ro handles appeals as part of their concierge. If your plan excludes weight-loss drugs entirely, cash-pay options start at $149/month through manufacturer programs.
Can I use HSA or FSA for GLP-1 programs?
Yes. GLP-1 medications prescribed for a diagnosed medical condition such as obesity or type 2 diabetes are generally HSA/FSA eligible. Most providers accept HSA/FSA cards for medication costs.
Which online provider is best for prior authorization help?
Ro's insurance concierge is the most dedicated PA support system among the providers we reviewed. Form Health's clinical team also advocates directly with insurers.
How long does prior authorization for GLP-1s usually take?
Ro says coverage determination typically takes 1–3 weeks. PlushCare reports needing 3–7 business days to compile the PA, with insurers taking 7–14 additional days to respond.
Are compounded GLP-1s covered by insurance?
No. Insurance coverage pathways apply to FDA-approved medications. Compounded semaglutide and tirzepatide are cash-pay only, though HSA/FSA funds may apply.
What is the fastest insurance-friendly path to Wegovy online?
Ro. Complete the online health assessment in about 10 minutes, and Ro begins insurance verification. If covered and no PA is needed, medication can reach you in under a week. If PA is required, expect 1–3 weeks.
Can I switch providers without restarting my dose?
Yes, but your new provider will need your medical records and current dosage. Insurance coverage may need to be re-verified. Ask about the transition process before switching.
Still Not Sure Which GLP-1 Program Is Right for You?
Take our free 60-second matching quiz. Answer 5 questions about your insurance type, budget, and preferences — and we’ll recommend the best provider for your specific situation. No email required, no commitment.
No email required · 60 seconds · No commitment
Have commercial insurance?
Ro’s concierge handles coverage checks, prior authorizations, and appeals — so you don’t have to. $45 first month. Cancel anytime.
Check Your GLP-1 Insurance Coverage on Ro — Free →Related guides
- Does Insurance Cover Zepbound for Weight Loss? (April 2026)
- GLP-1 Providers That Take HSA: 7 Verified Picks (2026)
- Best Online Wegovy Provider: 7 Legit Options (2026)
- Best Telehealth for Wegovy: Full Provider Breakdown
- How to Appeal a GLP-1 Insurance Denial (Step-by-Step)
- Does Medicare Cover Wegovy for Weight Loss?
- Cheapest GLP-1 Without Insurance: Full Cash-Pay Comparison
Sources
- Ro Body Membership
- Ro Weight Loss Pricing
- Ro 2025 GLP-1 Insurance Coverage Checker Report
- Form Health FAQs
- WeightWatchers Weight Loss Medication
- PlushCare Weight Loss
- PlushCare Medicare Coverage
- Knownwell Insurance
- Found Benefits Verification
- NovoCare Wegovy Pricing
- Zepbound Access & Coverage
- CMS Medicare GLP-1 Bridge FAQ
- GoodRx Insurance Coverage Tracking 2026
- KFF Employer Health Benefits Survey
- KFF Claims Denials and Appeals 2024
- FDA Warns 30 Telehealth Companies (March 2026)
Affiliate disclosure: We may earn commissions from Ro, Found, and PlushCare links on this page. Rankings are based on our verified methodology above — not commission rates. Full disclosure →
Medical disclaimer: Content is for informational purposes only and does not constitute medical advice. GLP-1 medications require a prescription from a licensed healthcare provider.