Does Insurance Cover Zepbound for Weight Loss?
By The RX Index Research Team · April 3, 2026 · Affiliate disclosure · Editorial standards
Does insurance cover Zepbound for weight loss? Some plans do — but coverage is far from universal, and the landscape shifted in 2026. GoodRx estimates that 56% of commercially insured people now have no coverage for Zepbound, leaving over 109 million without access through their plan. Even when plans do cover GLP-1s for weight loss, over 88% impose restrictions like prior authorization or step therapy.
Here’s what matters more than those numbers: if your plan covers Zepbound, you can pay as little as $25/month with Eli Lilly’s savings card. If it doesn’t, Lilly’s self-pay pricing through LillyDirect starts at $299–$449/month depending on dose. And if you’re on Medicare, a temporary $50/month program launches July 1, 2026 — the first route Medicare has ever opened for weight-loss prescriptions.
So the real question isn’t whether insurance ever covers Zepbound. It’s which path gets you Zepbound at the lowest cost based on your insurance type, denial reason, and budget. That’s what this page answers — every scenario, every price, every next step.
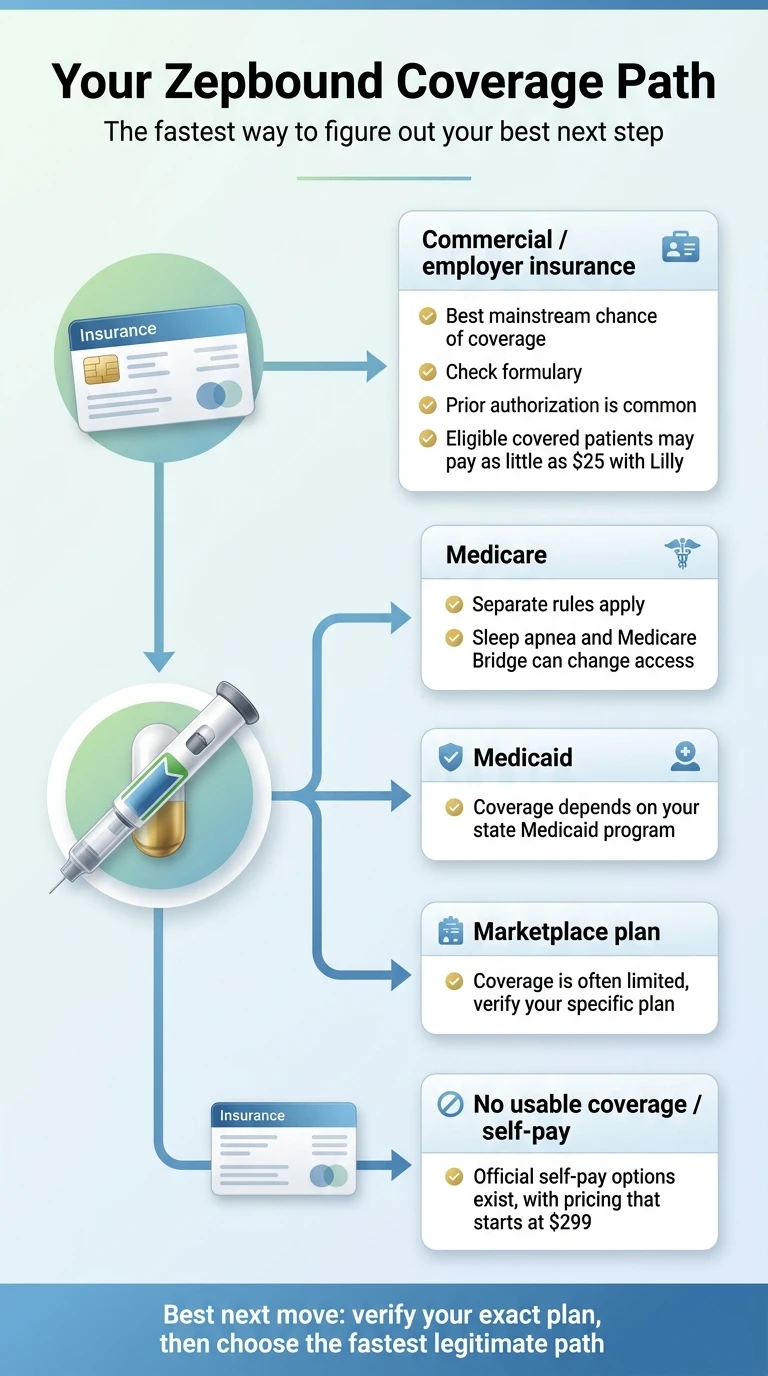
Your Real Zepbound Cost by Access Path (April 2026)
We verified each price directly from Eli Lilly, CMS, and GoodRx. This table covers every legitimate way to access Zepbound right now.
| Access Path | Monthly Cost | Who This Is For |
|---|---|---|
| Commercial insurance + Lilly savings card | As low as $25 | Employer/individual plan that covers Zepbound single-dose pens |
| Commercial insurance, NOT covered (KwikPen via savings card) | $299–$449/mo | Have commercial insurance that doesn't cover Zepbound |
| Commercial insurance, NOT covered (pen via savings card) | As low as $499 | Same — but using the single-dose pen instead of KwikPen |
| LillyDirect self-pay — vials or KwikPen | $299–$449/mo | Anyone with a valid Rx, no insurance needed or used |
| Medicare GLP-1 Bridge (July–Dec 2026) | $50 copay | Eligible Medicare Part D enrollees — operates outside normal Part D benefit |
| Medicaid (13 states) | Varies by state | Residents of states that cover GLP-1s for obesity treatment |
| Full retail, no savings | ~$1,086 | Nobody should pay this if they've read this page |
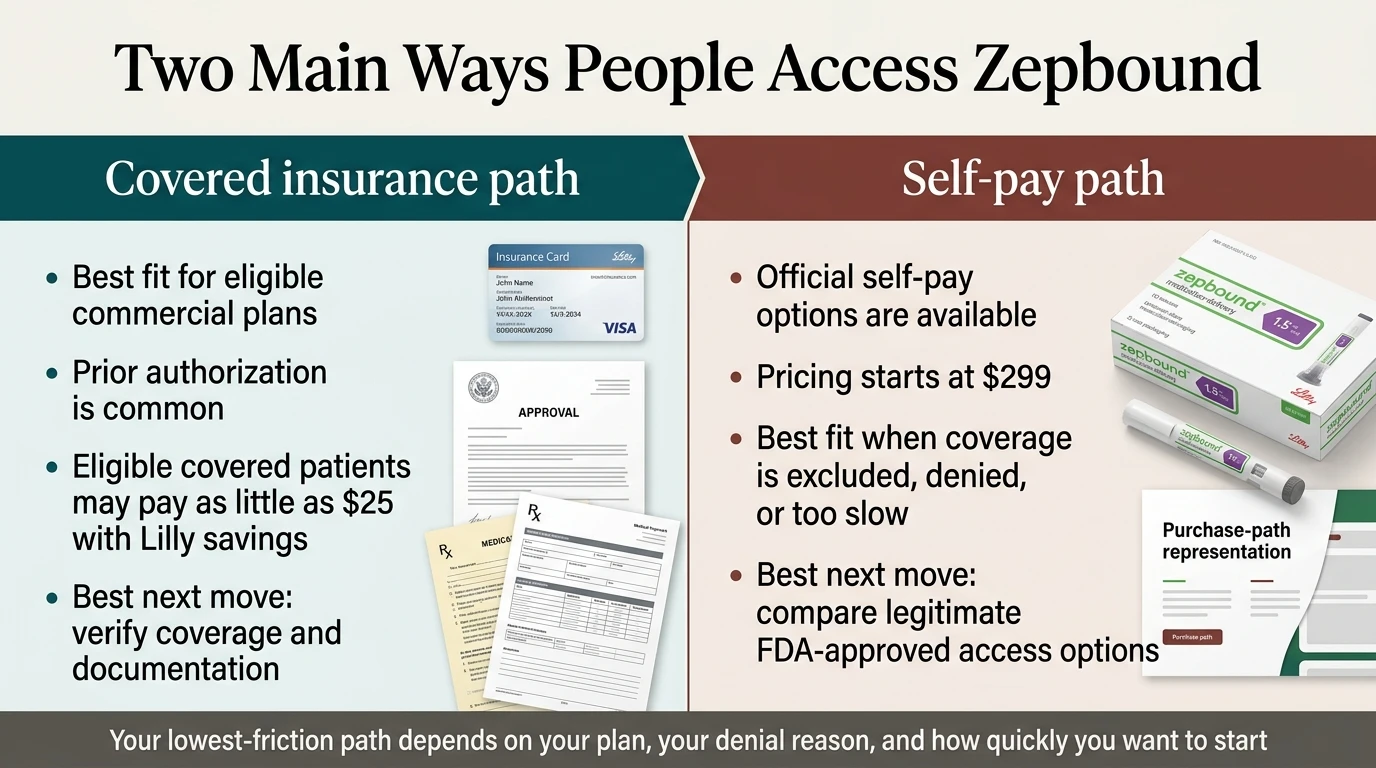
The $25/month path requires two things
Both insurance coverage AND the Lilly savings card — you need both pieces. The card provides up to $100/month in savings, with a $1,300 annual cap, and expires December 31, 2026. Government insurance (Medicare, Medicaid, VA, TRICARE) cannot use this card.
The $449 price requires on-time refills
For KwikPen and vial doses of 7.5 mg and above, the $449 purchase offer requires refilling within 45 days of your previous delivery. Miss that window and you pay the regular price for that fill. The KwikPen (launched February 2026) holds all four weekly doses in one pen — no syringes or measuring needed.
The KwikPen is almost always the better deal
For non-covered patients, KwikPen at $299–$449/month vs. $499+ for the single-dose pen. The math isn’t close.
If you already know your plan covers Zepbound and you want help with the prior authorization process, Ro’s clinical team handles PA submissions across all major insurers — including an insurance concierge that manages the paperwork if your approval gets complicated.
Free coverage check · PA support if you move forward
How Coverage Changes by Insurance Type
This is where most pages fail you. They say “coverage varies” and stop. Your odds change dramatically based on what type of insurance you carry — and the insurer name on your card matters less than you think.
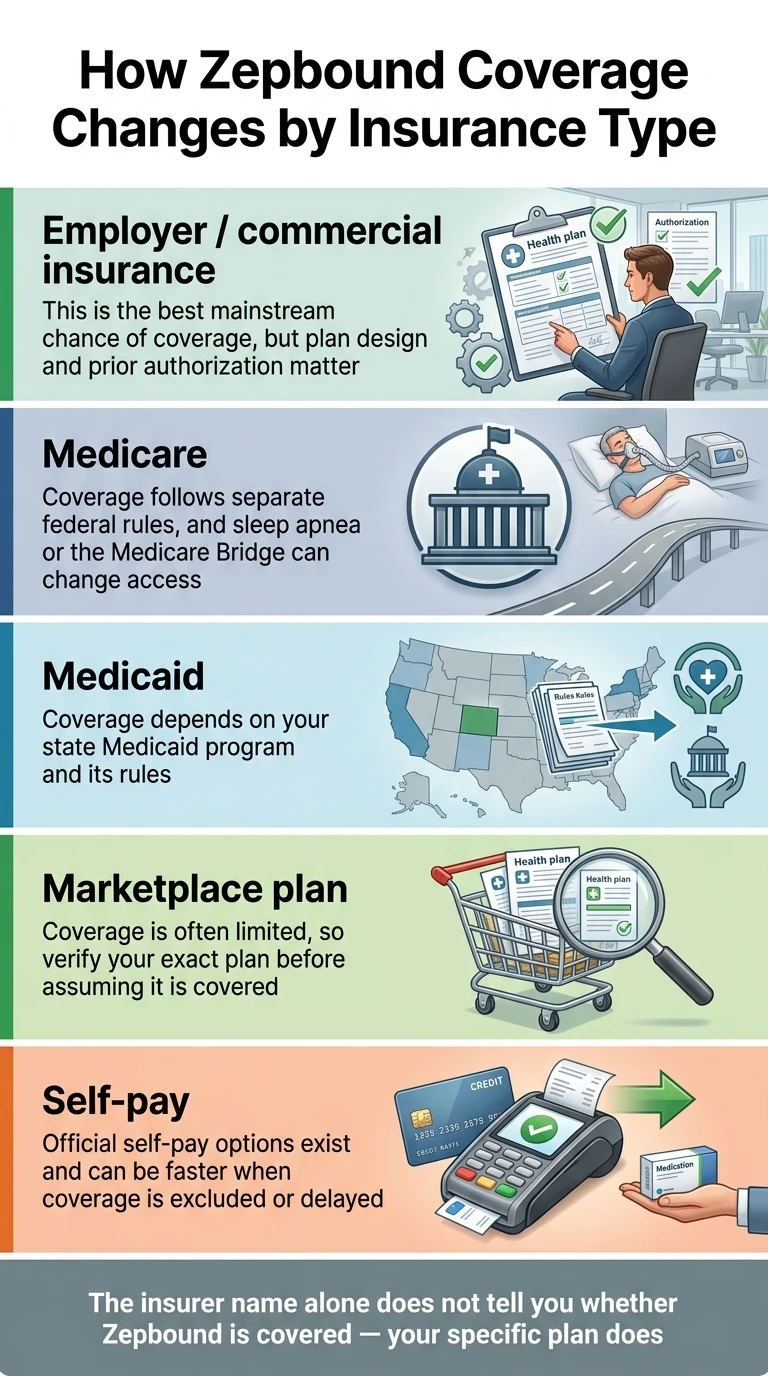
Employer / Commercial Plans — Your Best Mainstream Shot
KFF found that in 2025, GLP-1 drugs used primarily for weight loss were covered by 16% of firms with 200–999 workers, 30% of firms with 1,000–4,999 workers, and 43% of firms with 5,000+ workers. The bigger your employer, the better your odds — but even at large companies, coverage is far from guaranteed.
If your employer-sponsored plan does include anti-obesity medication benefits, Zepbound will almost certainly require prior authorization. Your doctor submits documentation, the insurer reviews it, and you typically hear back within a week or two. This is normal and expected — not a denial.
CVS Caremark watch-out
CVS Caremark — one of the largest pharmacy benefit managers — removed Zepbound from its standard formulary in July 2025, pushing Wegovy as the preferred option. That single decision affected millions of people overnight, even though their “insurer” hadn’t changed. You can request a formulary exception, but you’ll need documentation.
ACA Marketplace Plans — Usually Poor Odds
Marketplace coverage of GLP-1s for weight loss has historically been rare. KFF found Wegovy was covered by just 1% of Marketplace prescription drug plans in 2024. Zepbound coverage should be verified plan-by-plan rather than assumed.
If you’re on a Marketplace plan that excludes weight-loss drugs, the self-pay paths in the table above ($299–$449/month through LillyDirect) are likely your most realistic option.
Medicaid — State by State, and Shrinking
KFF reports that 13 state Medicaid fee-for-service programs cover GLP-1s for obesity treatment as of January 2026, down from 16 in 2025. Even in covered states, access is subject to prior authorization and other utilization controls.
The CMS BALANCE Model can expand Medicaid access beginning as early as May 2026 for states that choose to participate, but individual coverage still depends on state participation and program rules.
Medicare Part D — Historically Blocked, but 2026 Opens a Door
Since 2003, federal law has prohibited Medicare from covering drugs prescribed specifically for weight loss. That left millions of seniors paying over $1,000/month out of pocket — or going without.
The Medicare GLP-1 Bridge launches July 1, 2026
This temporary program gives eligible Part D enrollees access to Zepbound at a flat $50/month copay through December 31, 2026. It operates outside the normal Part D benefit — meaning Part D plans don’t need to opt in.
Eligibility requires meeting one of three tiers (from the CMS March 2026 FAQ):
BMI ≥35 at treatment initiation (no additional conditions required)
BMI ≥30 with heart failure with preserved ejection fraction, uncontrolled hypertension (on 2+ antihypertensive medications), or chronic kidney disease stage 3a or above
BMI ≥27 with pre-diabetes (per ADA guidelines), prior myocardial infarction, prior stroke, or symptomatic peripheral artery disease
Important caveats:
· The $50 copay does NOT count toward your Part D deductible or $2,100 out-of-pocket cap
· Low-Income Subsidy benefits don’t apply to Bridge prescriptions
· If you already get Zepbound through Part D for sleep apnea, you stay on Part D — the Bridge is only for the weight-loss indication
· To maintain access after December 2026, enroll in a Part D plan participating in the BALANCE Model during fall 2026 open enrollment
The sleep apnea shortcut: Zepbound received FDA approval for moderate-to-severe OSA in December 2024. If you have sleep apnea, Medicare Part D may already cover Zepbound under the OSA indication — separate from the Bridge program with normal Part D cost-sharing. See our full Medicare Zepbound guide →
Does the Insurance Company Matter — or Does the Plan Matter More?
The plan matters more than the logo on the card. This is the single most important thing to understand, and it’s why insurer-name coverage tables are misleading.
Two people with Blue Cross Blue Shield cards can have completely opposite answers. One works for a large self-insured employer that includes anti-obesity medications. The other works for a smaller company whose plan specifically excludes them. Same logo. Different answer.
Self-insured employer plans
These cover the majority of people with employer-sponsored insurance. The employer decides what’s covered — not the insurer. Your HR department has more influence over your Zepbound coverage than UnitedHealthcare or Aetna does.
The pharmacy benefit manager (PBM) layer
Your insurer might be Cigna, but your drug benefits might be managed by CVS Caremark, Express Scripts, or OptumRx. The PBM controls the formulary. When CVS Caremark removed Zepbound in July 2025, millions lost coverage overnight even though their “insurer” hadn’t changed anything.
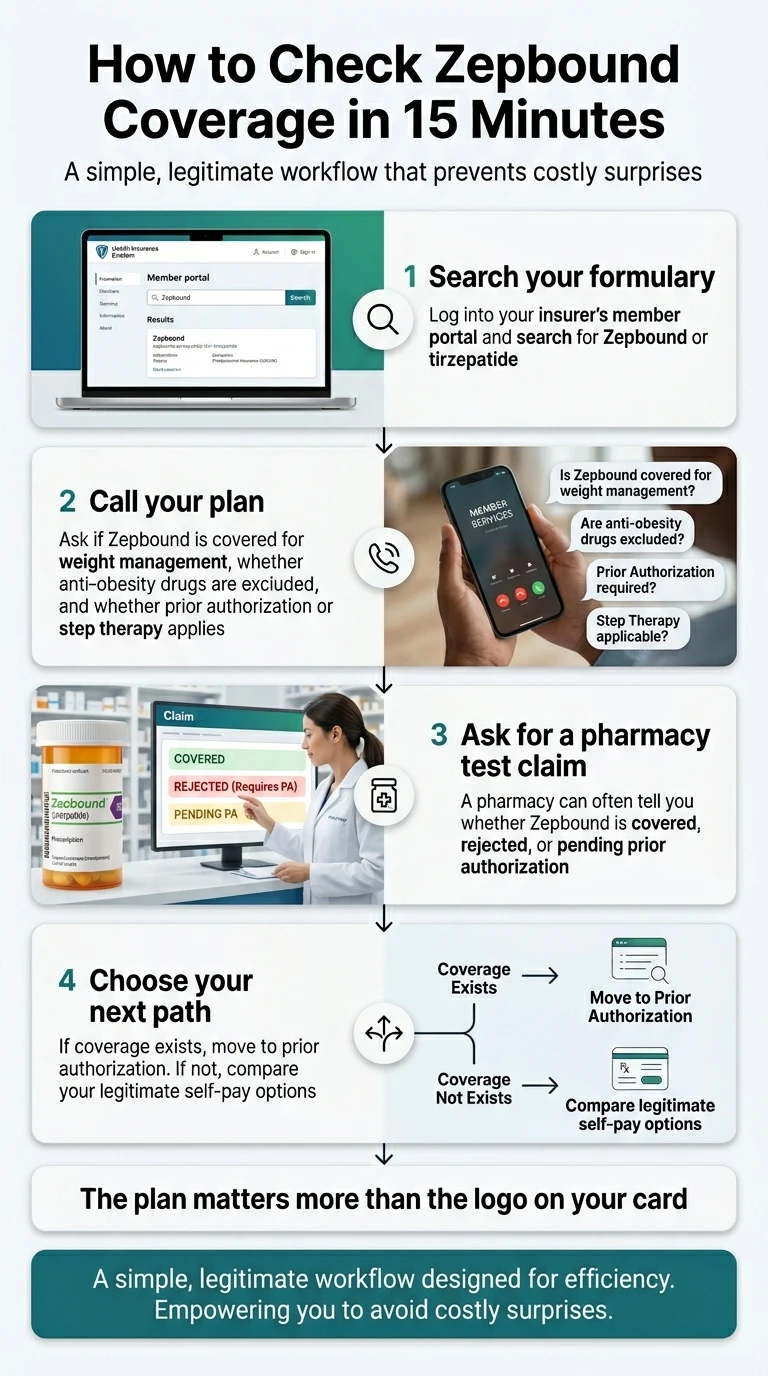
How to Check If Your Plan Covers Zepbound in 15 Minutes
Most people start this process backwards — they ask their doctor for a prescription, show up at the pharmacy, get quoted $1,086, and then try to figure out coverage after the fact. Here’s the faster sequence.
Search Your Plan’s Formulary Online
Log into your insurer’s member portal. Navigate to pharmacy benefits → formulary search. Search for “tirzepatide” or “Zepbound.” If it’s listed, note the tier. If it says “PA required,” that’s normal — proceed to step 2.
Call Your Insurance — Use This Script
Call the member services number on the back of your card. Ask these exact questions:
Script:
“I’d like to verify coverage for tirzepatide, brand name Zepbound, for chronic weight management. Can you tell me:
- Is Zepbound on my pharmacy formulary for weight management?
- Are anti-obesity medications excluded as a benefit category under my plan?
- If covered, what is my estimated copay or coinsurance?
- Is prior authorization required? What are the specific criteria?
- Is step therapy required — do I need to try another medication first?
- Can you send me the written coverage policy or criteria document?
”
Write down the representative’s name and any reference number. Verbal confirmations aren’t binding, but documentation helps if there’s a dispute later.
Ask the Pharmacy to Run a Test Claim
Your pharmacist can often run a test claim without a full prescription. This shows in real time whether Zepbound is covered, requires PA, or is rejected. Takes a few minutes and gives you a definitive answer.
Try Lilly’s Coverage Checker
Eli Lilly offers an online coverage checker at zepbound.lilly.com that walks through your insurance type and matches you with savings programs. Useful as a quick screen, but not a guarantee of coverage — your plan documents are the final word.
Don’t want to manage this yourself? Ro offers a free GLP-1 insurance check that returns a personalized coverage report. If you decide to move forward, their insurance concierge handles the prior authorization from start to finish.
Free coverage check · PA support if covered · Self-pay option if not
What Your Doctor Needs for Prior Authorization — and How to Get It Right the First Time
Prior authorization is the most common reason coverage gets delayed — and the most common reason for denial is incomplete documentation. Not that you don’t qualify. That the paperwork was thin.
One patient on Reddit put it plainly: “The most common reason for denial is incomplete info — most notably, missing your starting BMI.”
A strong PA submission includes:
1. Exact FDA-approved indication language
Zepbound is indicated as an adjunct to a reduced-calorie diet and increased physical activity for chronic weight management in adults with obesity (BMI ≥30) or overweight (BMI ≥27) with at least one weight-related comorbidity. Your doctor should use this specific framing.
2. Current BMI with supporting measurement
Sounds obvious — but outdated or missing BMI is among the most frequently cited denial reasons.
3. Documented weight-related comorbidities
Hypertension, type 2 diabetes or prediabetes, obstructive sleep apnea, PCOS, NAFLD, hyperlipidemia. Include supporting labs: A1C, lipid panel, blood pressure readings.
4. Documentation of previous weight loss attempts
Most insurers want evidence you've tried diet, exercise, and sometimes other medications before Zepbound. Some require 3–6 months of documented lifestyle modification. Weight Watchers, dietitian visits, structured exercise, phentermine, Contrave — document it all.
5. Letter of Medical Necessity
Your doctor explains why Zepbound is specifically appropriate given your clinical history. The Obesity Action Coalition (obesityaction.org) provides free sample letters.
6. For renewals: documented treatment response
Some plans require proof of at least 5% body weight loss to continue coverage.
Ro’s clinical team specializes in GLP-1 prior authorization — they know what each major insurer asks for and how to document it. If your PA gets denied, they handle the appeal.
PA submission + appeal handling if needed
Insurance Denied Zepbound — Here’s What to Do Based on Why
Getting denied feels final. It’s usually not — but the right response depends entirely on why you were denied. Most advice online lumps all denials together and gives you generic tips. That wastes time.
First: get your denial letter. Not a phone summary — the actual written denial. It contains language that tells you which of two fundamentally different problems you’re facing.
Type 1: Plan-Design Denial — “Your Plan Excludes This”
Key phrases in the letter:
“not a covered benefit,” “excluded benefit category,” “anti-obesity medications are excluded”
This means the problem isn’t your documentation — it’s the plan itself. Your employer (for self-insured plans) or insurer (for fully-insured plans) chose to exclude weight-loss medications entirely.
The honest truth: If your plan explicitly excludes all anti-obesity medications, filing a medical necessity appeal is usually not productive. Most pages soften this too much, and people waste months fighting a structural wall.
What actually works:
Talk to HR
For self-insured employers, HR can advocate for adding coverage at the next plan renewal. The Obesity Action Coalition offers sample request letters. Get coworkers to make the same request — numbers matter.
Check the sleep apnea route
If you have or suspect OSA, Zepbound may be covered under a completely different benefit category. At-home sleep studies are widely available and typically covered by insurance.
Switch plans at open enrollment
If your employer offers multiple options, compare formularies.
Go self-pay
LillyDirect KwikPens at $299–$449/month may be your fastest path. Same FDA-approved Zepbound at roughly 60% off list price with free home delivery.
Type 2: Criteria / Documentation Denial — “You Don’t Meet the Requirements”
Key phrases:
“criteria not met,” “prior authorization denied,” “step therapy required,” “insufficient documentation”
This is the fixable denial. Something was missing, incomplete, or incorrectly submitted. Patient advocacy firms that specialize in GLP-1 appeals report that well-documented appeals succeed the majority of the time. The bigger problem: fewer than 1% of denied claims are ever appealed. Most people give up before they start.
| Denial Reason | What Happened | Fastest Fix |
|---|---|---|
| Criteria not met | BMI, comorbidities, or lifestyle documentation didn't meet requirements | Get written criteria, gather exactly what they ask for, resubmit |
| Incomplete documentation | Missing BMI, labs, or chart notes | Doctor adds missing data and resubmits — often resolved quickly |
| Step therapy required | Insurer wants Wegovy, Saxenda, or Contrave first | Complete step therapy OR request a clinical exception |
| Not medically necessary | Insurer needs stronger justification | Doctor submits detailed Letter of Medical Necessity with full clinical history |
| Wrong indication / coding | Claim submitted with incorrect diagnosis codes | Prescriber's office corrects the code and resubmits |
The appeal process:
Get the written denial with the specific reason
Request the insurer's coverage criteria document
Gather complete documentation addressing the specific deficiency
Your doctor submits an appeal with a Letter of Medical Necessity
If denied again, request a peer-to-peer review (your doctor speaks directly with the insurer's medical director)
If still denied, file for external review with your state insurance department
“My doctor didn’t even try to appeal when Zepbound was originally denied. After getting help with the appeal letter, we submitted and got approved within 48 hours.”
— Patient experience shared in GLP-1 community forum
Full Zepbound appeal guide
Decode your denial type, choose the right response — corrected PA, formulary exception, or internal appeal — build the exact documentation packet, and hit your deadline. Covers the CVS Caremark scenario, the OSA coverage pathway, and what to do if the appeal fails.
How to Appeal a Zepbound Denial: 7 Steps That Work (2026) →About CVS Caremark specifically
Zepbound was removed from CVS Caremark’s standard formulary in July 2025, with Wegovy as the preferred alternative. You can request a formulary exception, but you’ll need documentation showing either that Wegovy wasn’t effective or tolerable for you, or that you’re already on Zepbound and have achieved at least 5% body weight loss. Lilly provides a downloadable appeals guide at zepbound.lilly.com/access.
What If Your Insurance Only Covers Wegovy?
Increasingly common — especially on CVS Caremark plans. And not necessarily bad news.
Wegovy (semaglutide) is a legitimate, FDA-approved weight-loss medication. It produced 12–17% average weight loss in clinical trials. Zepbound (tirzepatide) targets both GLP-1 and GIP receptors and produced 15–21% average loss. Zepbound is more effective on average, but Wegovy works well for many people.
The strategic play
Starting Wegovy gives you one of two outcomes. Either it works well (great, you’re losing weight), or it doesn’t work well enough — which gives you documented evidence for a Zepbound formulary exception later. Either way, you’re moving forward instead of stuck.
Oral Wegovy (a pill, not an injection) was FDA-approved in December 2025. If needles are a barrier, this opens another option. MEDVi offers FDA-approved GLP-1 options including Wegovy and Zepbound at transparent pricing — helpful if you want to compare paths side by side.
Transparent pricing · FDA-approved medications · Clinical support
When to Stop Fighting Insurance and Choose a Self-Pay Path
We want to be direct here, because most pages won’t be.
Stop fighting. Pivot to self-pay if:
- ✗Your plan explicitly excludes all anti-obesity medications — an appeal can't fix a benefit that doesn't exist
- ✗You've been in the appeal cycle for weeks with no progress — every month without treatment is a month without results
- ✗Your insurance copay is nearly as much as self-pay — if your copay exceeds $400/month, LillyDirect with free delivery might be the better deal
Keep fighting if:
- ✓Your denial was for incomplete documentation — most common and easiest to fix
- ✓Your plan covers Zepbound but requires step therapy — a defined path to eventual coverage
- ✓You have sleep apnea that hasn't been evaluated — the OSA indication opens doors the weight-loss indication can't
Ro cannot overturn an employer benefit exclusion. No provider can. If your plan flat-out excludes weight-loss drugs, a cash-pay path is faster than fighting a structural wall. But if your plan leaves the door open and you need someone to handle the PA and manage appeals, that’s exactly what Ro’s insurance concierge does. And if insurance isn’t happening, Ro also connects you with FDA-approved Zepbound through legitimate self-pay — same medication, clinical support included.
Free coverage check · PA handling · Self-pay available if insurance isn't an option
The Zepbound Savings Card: How It Actually Works
Eli Lilly’s savings program is one of the most generous in pharma — but the rules are specific.
If your commercial insurance covers Zepbound
✓ EligibleAs low as $25/month
For the single-dose pen. Up to $100 in savings per monthly fill, $1,300 max per calendar year. Up to 13 fills. Card expires December 31, 2026.
If your commercial insurance does NOT cover Zepbound
✓ Eligible$299–$449/mo (KwikPen) or $499+ (pen)
KwikPen: $299 (2.5 mg), $399 (5 mg), $449 (7.5–15 mg). Single-dose pen: as low as $499. The KwikPen is almost always the better value for non-covered patients.
Who cannot use the savings card
✗ ExcludedMedicare GLP-1 Bridge = $50/mo
Anyone with government insurance: Medicare, Medicaid, VA, TRICARE, CHIP. No exceptions. If you're on Medicare, the $50/month GLP-1 Bridge (July 2026) is your equivalent.
The 45-Day Refill Rule
For KwikPen and vial doses of 7.5 mg, 10 mg, 12.5 mg, and 15 mg, the $449 purchase offer requires refilling within 45 days of your previous delivery. Miss that window and you pay regular pricing for that fill. Set a calendar reminder the day your medication arrives.
HSA and FSA
Prescription weight-loss treatment may be HSA/FSA-eligible when used to treat a diagnosed disease such as obesity, but IRS rules are more limited than many people assume. If you use Lilly’s savings card, the card terms state that the savings amount cannot be submitted to an HSA/FSA for reimbursement. Your out-of-pocket portion may still be eligible — consult your plan administrator or tax advisor.
See our complete guide on GLP-1 providers that take FSA and GLP-1 providers that take HSA for details on which platforms accept pre-tax accounts.
Does Sleep Apnea Change Zepbound Coverage?
Yes — meaningfully. Zepbound received FDA approval for moderate-to-severe obstructive sleep apnea in adults with obesity in December 2024. This created an entirely separate coverage pathway.
Plans that explicitly exclude weight-loss medications may still cover Zepbound for OSA — different benefit category, different formulary rules. Medicare Part D already covers Zepbound for OSA outside the Bridge program. The diagnosis coding your prescriber uses can make or break coverage.
If you haven’t been tested
OSA is common in adults with obesity. If you snore heavily, wake up tired despite sleeping 7+ hours, or your partner has noticed you stop breathing during sleep — ask your doctor about a sleep study. At-home studies are widely available and typically covered by insurance.
Getting diagnosed with OSA doesn’t mean your treatment becomes about sleep apnea instead of weight loss. It means you have a clinical condition that broadens your coverage options.
How to Ask Your Employer to Add Zepbound Coverage
If your employer’s plan excludes weight-loss medications, you have more leverage than you think — especially at companies with self-insured health plans.
Talk to HR. Frame it around these points:
The AMA classifies obesity as a chronic disease requiring medical treatment
GLP-1 medications reduce downstream healthcare costs — fewer cardiovascular events, fewer diabetes diagnoses, fewer joint replacements
A large and growing share of peer employers already cover these medications
Employees are asking for this — you probably aren't the only one
The Obesity Action Coalition at obesityaction.org provides sample letters for both employees and employers. Get coworkers to make the same request. One person asking is anecdotal. Ten people asking gets it on the benefits committee agenda.
What’s Changing for Zepbound Coverage in 2026
2026 is the most consequential year for Zepbound access since the drug’s approval. Here’s what happened, what’s coming, and what it means for you.
| Date | What Changed | What It Means |
|---|---|---|
| Dec 2024 | FDA approves Zepbound for OSA | New coverage pathway through Medicare Part D and many commercial plans |
| July 2025 | CVS Caremark removes Zepbound from formulary | Millions lose coverage; Wegovy becomes preferred; exception process available |
| Dec 2025 | Lilly cuts LillyDirect vial prices to $299–$449/mo | Self-pay becomes significantly more accessible |
| Jan 2026 | Some commercial insurers drop GLP-1 coverage entirely | Coverage landscape tightens for select plans |
| Feb 2026 | Lilly launches KwikPen at same pricing as vials | Simpler self-pay option — one pen per month, no syringes |
| Mar 2026 | CMS releases Medicare GLP-1 Bridge FAQ | $50/month eligibility details become real and specific |
| May 2026 | Medicaid BALANCE Model opens for opt-in states | State Medicaid programs can expand GLP-1 access |
| July 2026 | Medicare GLP-1 Bridge launches | $50/month Zepbound for eligible Part D enrollees |
| Jan 2027 | Full BALANCE Model launches for Part D plans | Long-term Medicare/Medicaid GLP-1 coverage structure |
Best Next Step Based on Your Situation
Find your row. Do that thing.
I have employer insurance and I'm not sure if Zepbound is covered
Run a free coverage check on Ro
My plan covers Zepbound but I need prior authorization
Let Ro handle the PA
My PA was denied for documentation issues
Gather missing documentation and resubmit — it works more often than you'd expect
My employer excludes all weight-loss medications
Talk to HR, check the OSA route, or go self-pay through LillyDirect ($299–$449/mo)
CVS Caremark removed Zepbound from my formulary
Request a formulary exception; document why Wegovy isn't right for you
I have Medicare and want Zepbound for weight loss
Prepare for the July 2026 GLP-1 Bridge ($50/mo) — document BMI and comorbidities now
I have Medicare + sleep apnea
Ask your doctor about Part D coverage under the OSA indication — may already be covered
I have Medicaid
Contact your state Medicaid program directly — only 13 states cover it
I have a Marketplace plan
Most exclude it — self-pay via LillyDirect is likely your best path
Insurance isn't an option and I want FDA-approved Zepbound
Get started through Ro at $299–$449/month — clinical support included
How We Verified This Page
Employer coverage statistics
Commercial coverage tracker
Update cadence: This page is reviewed monthly. Major developments (formulary changes, price changes, new programs) are updated within 48 hours. Last full audit: April 3, 2026.
Frequently Asked Questions
How much does Zepbound cost with insurance?
If your commercial plan covers Zepbound single-dose pens and you use Lilly's savings card, your cost can be as low as $25/month. Without the savings card, your out-of-pocket cost depends on your plan's tier, deductible, and coinsurance structure — call your insurer for your specific number.
How much does Zepbound cost without insurance?
Official self-pay pricing through LillyDirect starts at $299/month for 2.5 mg, $399 for 5 mg, and $449 for 7.5–15 mg under Lilly's purchase-offer terms. The full retail list price is approximately $1,086/month, but multiple savings paths exist to bring that down significantly.
Is there a generic version of Zepbound?
No. Zepbound is patent-protected and no generic exists. Tirzepatide no longer appears on FDA's drug shortage list, which means compounded tirzepatide is no longer broadly available in the same way it was during the shortage period.
Can I use the Zepbound savings card with Medicare or Medicaid?
No. Lilly's savings card terms explicitly exclude government insurance beneficiaries including Medicare, Medicaid, VA, TRICARE, and CHIP.
Does Medicare cover Zepbound for weight loss?
The temporary Medicare GLP-1 Bridge launches July 1, 2026, offering Zepbound at a $50/month copay for eligible Part D beneficiaries. This operates outside the normal Part D benefit and runs through December 31, 2026. The longer-term BALANCE Model for Part D plans begins January 2027.
Does Medicaid cover Zepbound?
As of January 2026, 13 state Medicaid fee-for-service programs cover GLP-1s for obesity treatment. Coverage varies by state and is subject to prior authorization and utilization controls.
Does sleep apnea help with Zepbound coverage?
Yes. Zepbound is FDA-approved for moderate-to-severe obstructive sleep apnea in adults with obesity. Many plans that exclude weight-loss medications still cover Zepbound for OSA, including Medicare Part D.
Why did my Zepbound prior authorization get denied?
The most common reason is incomplete documentation — missing BMI measurements, insufficient comorbidity records, or undocumented lifestyle modification efforts. Get the written denial, identify the specific deficiency, and have your doctor resubmit with complete documentation.
What if my employer excludes weight-loss drugs entirely?
Three options: advocate for coverage through HR at the next plan renewal, check whether the OSA indication opens a separate coverage path, or go self-pay through LillyDirect at $299–$449/month.
When will Medicare cover Zepbound for weight loss?
The temporary Medicare GLP-1 Bridge launches July 1, 2026, offering a $50/month copay for eligible Part D beneficiaries. The longer-term BALANCE Model for Part D plans begins January 2027.
Still Not Sure Which GLP-1 Program Is Right for You?
Take our free 60-second matching quiz. Tell us your insurance type, budget, and goals — we’ll show you the most affordable path personalized to your exact situation.
Not sure which path fits your situation?
Insurance check, PA help, or self-pay — we’ll map your exact next step in 60 seconds.
Take the Free GLP-1 Matching Quiz →No email required · 60 seconds · Personalized path
Related guides
- Ozempic vs Zepbound: Which Is Better in 2026? (Real Prices)
- Cheapest Zepbound Without Insurance: Real 2026 Prices ($299/Mo Path)
- Does Medicare Cover Zepbound? 2026 Coverage Guide
- Best Way to Get Zepbound Online: Verified Providers (2026)
- Best GLP-1 Providers That Accept Insurance (2026)
- How to Get Tirzepatide Covered by Insurance Online (2026)
- GLP-1 Providers That Take FSA: 8 Verified Picks (2026)
- GLP-1 Providers That Take HSA: 7 Verified Picks (2026)
- Cheapest GLP-1 Without Insurance: All Options Compared (2026)
- Cheapest Wegovy Without Insurance in 2026
- Wegovy vs. Zepbound vs. Saxenda: Full 2026 Comparison
Sources
- Zepbound.lilly.com — Savings & Access
- Lilly Self Pay Journey Program Full Terms
- CMS Medicare GLP-1 Bridge FAQ (March 2026)
- KFF 2025 Employer Health Benefits Survey
- GoodRx Commercial Coverage Tracker
- FDA — Zepbound Prescribing Information (Dec 2024)
- Obesity Action Coalition — PA Resources
Affiliate disclosure: Some links on this page go to partner providers including Ro and MEDVi. We earn a commission if you use these services. This doesn’t change our analysis — if we removed every link, the information would be identical. We recommend Ro for readers navigating insurance because their free coverage checker and PA support directly serve this page’s intent. We recommend MEDVi for readers comparing FDA-approved GLP-1 options. Full disclosure →
Medical disclaimer: This page is for informational purposes only and does not constitute medical advice. Always consult a licensed healthcare provider before starting any medication. Zepbound® is a registered trademark of Eli Lilly and Company. The RX Index is not affiliated with Eli Lilly.
Last updated: April 3, 2026 · By The RX Index Research Team
Free coverage check · PA support · Self-pay option if insurance isn’t available