The quick version:
- →If your commercial insurance covers Zepbound or Mounjaro, Eli Lilly's savings card drops your cost to as low as $25/month (Zepbound Savings).
- →If you're denied, appeal it. In Medicare Advantage alone, KFF found that more than 8 in 10 appealed prior-authorization denials were overturned each year from 2019–2024 (KFF).
- →If insurance isn't an option, FDA-approved Zepbound vials start at $299/month through providers like Ro — no insurance needed, shipped to your door (Ro Pricing).

Jump to your situation
Your Best Coverage Path, Based on Your Situation
Before we go deep, here's the decision at a glance. Find your row and you'll know your next move in 30 seconds.
| Your Situation | Best Brand | Best Online Next Step |
|---|---|---|
| Type 2 diabetes | Mounjaro | Ask your doctor for Mounjaro; use savings card ($25/mo) |
| Obesity (BMI 30+) | Zepbound | Ro's insurance concierge checks coverage and submits PA |
| Overweight (BMI 27+) + health condition | Zepbound | Ro handles commercially insured patients |
| Obesity + sleep apnea Strongest angle | Zepbound | Lead with OSA — may qualify even under plans that exclude weight-loss drugs |
| PCOS (no diabetes) | Zepbound | Ro or your PCP can submit PA citing obesity with PCOS as supporting evidence |
| Medicare Part D | Depends on diagnosis | Check Part D formulary; cash-pay Zepbound vials ($299–$449/mo) as fallback |
| Medicaid | Depends on state | Check your state's preferred drug list |
| Plan excludes weight-loss drugs | — | Switch plans at open enrollment, pursue OSA/T2D angle, or go cash-pay at $299/mo |
Last verified: March 20, 2026. Coverage changes frequently — always confirm with your specific plan.
The Five Things That Actually Determine Whether You're Covered
Before we walk through each path, here's the framework that simplifies the entire page. Coverage for tirzepatide comes down to five factors. Get all five right and your odds are excellent. Miss one and you'll likely hit a wall.
The right FDA-approved brand for the right diagnosis.
Mounjaro for diabetes. Zepbound for weight loss or sleep apnea. Wrong brand + wrong diagnosis = automatic denial.
The right insurance bucket.
Commercial employer plans have the best coverage rates, though KFF's 2025 survey found only about 19% of large firms cover GLP-1s for weight loss, while 57% do not and 24% were unsure. Medicare is opening up in 2026. Medicaid varies wildly by state.
Complete paperwork.
Even when you have coverage, over 88% of people with GLP-1 weight-loss coverage still face additional requirements like prior authorization, according to GoodRx. Documentation wins the game.
A provider who actually does the insurance work.
Some providers write a prescription and send you on your way. Others — like Ro — check your benefits, submit prior authorization, and fight denials on your behalf. That difference matters.
Persistence after denial.
A denial is not the end. Appeals have high overturn rates — in Medicare Advantage, KFF reports that more than 8 in 10 appealed denials were overturned each year from 2019 to 2024. The people who get covered are often the ones who simply don’t give up after the first “no.”
Coverage odds = right brand × right diagnosis × right plan × right paperwork × right follow-through.
Keep that formula in mind as you read the rest of this guide. Everything below maps to one of those five factors.
Does Your Insurance Cover Tirzepatide? (How to Find Out in 15 Minutes)
This is the first question everyone asks, and there's a reason most pages just say “call your insurance company.” The answer genuinely depends on your specific plan. But we can make the process a lot faster.
The Mounjaro vs. Zepbound Distinction That Changes Everything
This is the single most important thing to understand, and it's where people get tripped up constantly.
Mounjaro and Zepbound are the same medication — both contain tirzepatide, made by Eli Lilly, at the exact same doses. But the FDA approved them for different conditions, and that distinction determines whether your insurance says yes or no.
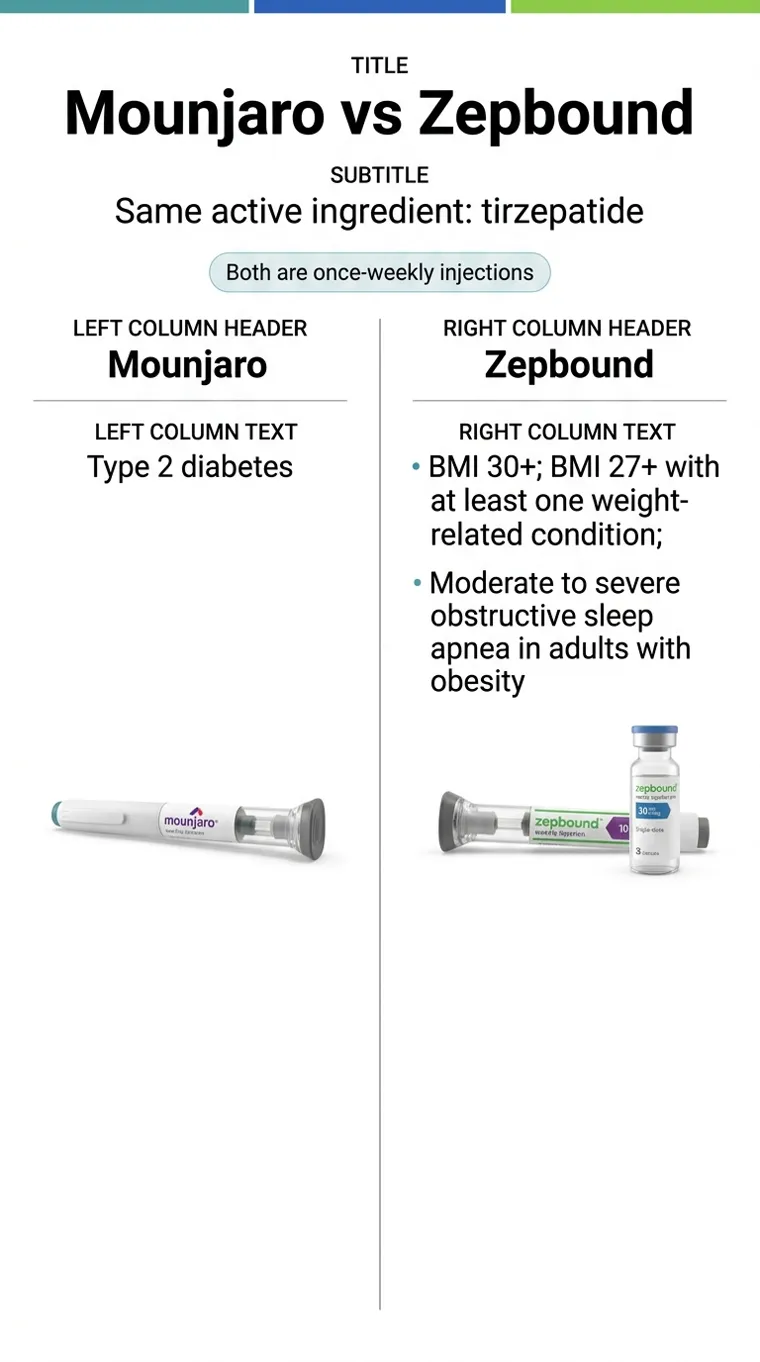
Mounjaro
FDA-approved for: Type 2 diabetes (glycemic control)
Coverage is much more common for diabetes. If you have T2D, this is almost always the easier path.
FDA label ↗Zepbound
FDA-approved for: Chronic weight management (BMI ≥30, or ≥27 with a weight-related condition) AND moderate-to-severe obstructive sleep apnea in adults with obesity
Weight-loss coverage is less consistent. OSA is the strongest coverage angle if you qualify.
FDA label ↗Why this matters: If your doctor writes “Mounjaro for weight loss,” your insurer will likely deny it — that's off-label use. The wrong brand is one of the most common avoidable denial reasons.
Three Ways to Check Your Coverage
Method 1: Check your formulary online. Log into your insurance portal and search the drug formulary for “tirzepatide,” “Zepbound,” or “Mounjaro.” The formulary will tell you if it's covered, what tier it's on, and whether prior authorization is required.
Method 2: Call your insurer. Use the number on the back of your insurance card. Here's exactly what to say:
Phone Script — What to Say When You Call
“Hi, I'm calling to check prescription drug coverage. My member ID is [NUMBER].”
Ask these five questions and write down the answers:
- “Is Zepbound — that's tirzepatide — on my plan's formulary for chronic weight management?”
- “Is prior authorization required? If so, what clinical criteria need to be met?”
- “Is there a step therapy requirement — do I need to try another medication first?”
- “What tier is it on, and what's my estimated copay or coinsurance?”
- “If it's not covered, is there a formulary exception or appeals process?”
Write down the representative's name and any reference number. Verbal confirmations aren't binding, but documentation helps if there's a dispute later.
Method 3: Use a free coverage checker. Ro (sponsored affiliate link, opens in a new tab) offers a free GLP-1 Insurance Coverage Checker — you enter your insurance information and they send back a personalized coverage report based on a conversation with your plan. It takes a few minutes and costs nothing.
Insurance Coverage Snapshot (2026)
Coverage varies enormously by plan, employer, and state. Rather than make blanket claims, here's what we can verify from official sources:
| Plan Type | What's Verifiable |
|---|---|
| CVS Caremark | Removed Zepbound from Standard Control, Advanced Control, and Value formularies effective July 1, 2025. Wegovy remains preferred. Formulary exception criteria exist for some formularies. |
| TRICARE | TRICARE Prime and Select beneficiaries can have weight-loss medications covered with approved prior authorization; rules vary by program. |
| Medicare Part D | Weight-loss-only use excluded by law. Mounjaro covered for T2D. Zepbound may be covered for OSA. Medicare GLP-1 Bridge launches July 2026 for weight loss ($50/mo copay). |
| Medicaid | 13 state FFS programs cover GLP-1s for obesity as of Jan 2026. BALANCE model expanding access May 2026. |
| Employer/Commercial (BCBS, UHC, Aetna, Cigna) | Coverage varies widely by employer and plan. KFF found 19% of large firms cover GLP-1s for weight loss; 57% do not. Always check your specific formulary. |
Last verified: March 2026. Always confirm with your specific plan before making decisions.
Want someone to check for you?
Ro's insurance concierge team will verify your coverage, submit prior authorization paperwork, and fight denials on your behalf — all included in their membership. If you're commercially insured and want someone in your corner, it's one of the best deals in the GLP-1 space.
Check Your Tirzepatide Coverage Through Ro → (sponsored affiliate link, opens in a new tab)Free for commercially insured patients. $39 first month if you enroll.
How Prior Authorization Works for Tirzepatide (And How to Get It Approved)
If your plan covers tirzepatide, you're probably not done yet. GoodRx research found that among people with insurance coverage for GLP-1 weight-loss medications, over 88% still face additional requirements like prior authorization before the pharmacy will fill the prescription (GoodRx).
Don't let that discourage you. Prior authorization sounds intimidating, but it's really just a documentation exercise. Your doctor submits paperwork proving you medically need this medication. The insurer reviews it.
Timelines vary by plan type. ACA-regulated plans must generally respond to pre-service requests within 15 days (72 hours for urgent cases) (HealthCare.gov). Medicare drug-plan timelines follow different rules. Ro says its overall insurance workflow typically takes about 2–3 weeks.
What Your Doctor Needs to Submit
Think of this as a checklist. The more boxes your doctor checks, the higher your approval odds:
Diagnosis code — E66.01 (Obesity), E11.x (T2D), G47.33 (OSA), or overweight with comorbidity
Current BMI — documented ≥30, or ≥27 with at least one weight-related condition
Weight-related comorbidities — hypertension, T2D, high cholesterol, sleep apnea, PCOS, fatty liver, cardiovascular disease
Previous weight-management attempts — at least 6 months of supervised diet, exercise, or behavioral modification
Step therapy compliance — if required, document prior medications tried and why they were insufficient
Letter of medical necessity — detailed letter from provider explaining the clinical rationale for tirzepatide specifically
Lab results — A1C, lipid panel, liver function, and sleep study results if applicable
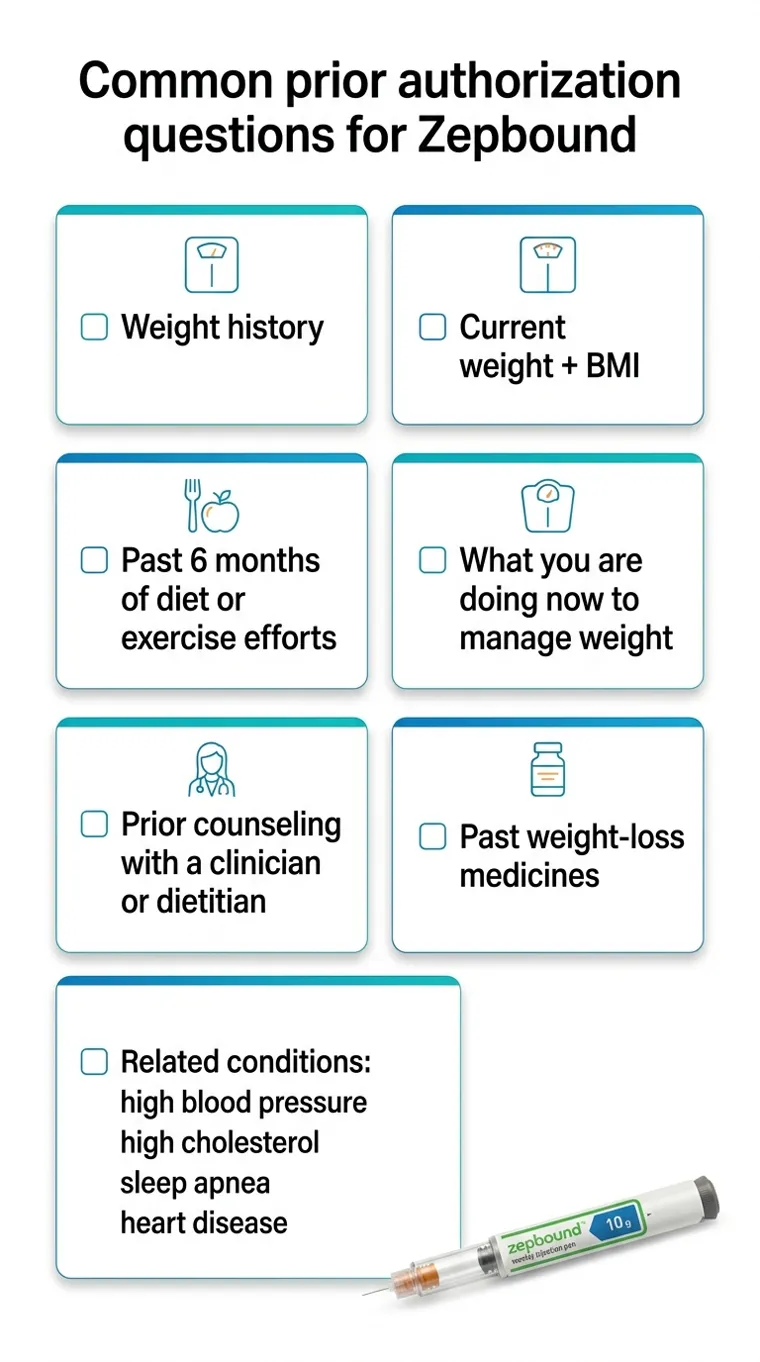
Eli Lilly publishes a Prior Authorization Resource Guide specifically for Zepbound (Zepbound Access), and the Obesity Action Coalition offers free PA letter templates (OAC). Both are worth downloading before your appointment.
Step-by-Step: The Prior Authorization Timeline
Here's what the process actually looks like from start to finish, so nothing catches you off guard:
Doctor prescribes and submits PA
Your doctor prescribes tirzepatide (Zepbound or Mounjaro) and submits a prior authorization form to your insurance company with your diagnosis, BMI, medical history, and clinical justification.
Insurance reviews
A clinical pharmacist or medical director evaluates whether you meet their plan's coverage criteria. ACA plans have up to 15 days for standard requests, 72 hours for urgent.
Approval, denial, or more info requested
You receive a decision via your pharmacy, prescriber, or insurer. If approved, use the Lilly Savings Card. If denied, move to appeal. If more info requested, your doctor resubmits — which resets the review clock.
1–3 weeks for smooth approval
For denials requiring appeal, add another 2–4 weeks. Using Ro, which handles all the paperwork, significantly reduces friction.
How to Increase Your Approval Odds
Submit the letter of medical necessity WITH the initial PA.
Many doctors submit the basic form first and only write the letter after a denial. Submitting everything upfront avoids a round trip that wastes weeks.
Lead with the strongest diagnosis.
If you have both obesity and obstructive sleep apnea, lead with OSA. Zepbound's OSA indication opens doors that 'chronic weight management' sometimes can't — especially with plans that have blanket exclusions for weight-loss drugs.
Document everything you've tried.
Every failed diet, every gym membership, every medication that didn't work or caused side effects. Insurers want to see that tirzepatide isn't the first thing you tried.
Have your doctor submit the PA proactively.
Don't wait for the pharmacy to trigger a rejection. Your doctor's office can submit PA paperwork directly, which starts the clock sooner.
Ro checks your coverage, submits PA paperwork, and fights denials on your behalf.
What to Do If Your Insurance Denies Tirzepatide
A denial is round one, not the final answer.
In Medicare Advantage, KFF found that more than 8 in 10 appealed prior-authorization denials were fully or partially overturned — consistently, each year from 2019 to 2024 (KFF). The AMA reported a similar 81.7% overturn rate for Medicare Advantage PA appeals. Commercial plan overturn rates vary, but the data strongly favors persistence.
Why Denials Happen (Most Are Fixable)
Problem: The PA wasn't submitted yet
Fix: The pharmacy flagged a PA requirement, but your doctor hasn't filed. Fix: have your doctor submit the PA.
Problem: Missing documentation
Fix: The insurer didn't get enough evidence of medical necessity. Resubmit with a stronger letter of medical necessity, additional lab results, or comorbidity documentation.
Problem: Step therapy required
Fix: Your plan requires trying another medication first (often Wegovy or Contrave). If you've tried them, document the results. If not, you may need to try first.
Problem: Not on formulary
Fix: Request a formulary exception — a formal process where your doctor argues your specific case. GoodRx confirms you can request a formulary exception for Zepbound and appeal if denied.
Problem: Plan excludes weight-loss drugs entirely
Fix: A blanket anti-obesity exclusion blocks the weight-loss pathway but does not automatically rule out coverage under T2D (Mounjaro) or OSA (Zepbound) if you qualify. Cash-pay is also an option.
How the Appeal Process Works
Commercial / ACA Marketplace Plans
- → 180 days to file an internal appeal after denial
- → If internal appeal denied: request external review within 4 months
- → Independent reviewer evaluates; insurer must comply
- HealthCare.gov guide ↗
Medicare Part D Plans
- → First appeal (redetermination): within 60 days of denial notice
- → Multiple further appeal levels exist after redetermination
- → Independent review organization evaluates at higher levels
- Medicare.gov appeals guide ↗
Your Appeal Playbook
Resubmit with stronger documentation
Your doctor writes a detailed Letter of Medical Necessity. Include relevant clinical trial data — the SURMOUNT trials showed tirzepatide produced 15–21% body weight loss at 72 weeks. Lilly publishes appeal resources specifically for Zepbound.
Zepbound appeal resources ↗Request a peer-to-peer review
Your doctor speaks directly with the insurance company's medical director. Emphasize your specific clinical need, what you've already tried, and what happens to your health without treatment.
Request external review
If the internal process fails, request an independent external review through your state insurance commissioner. Available in most states.
Ro's insurance concierge manages appeals so you don't have to sit on hold.
What Tirzepatide Actually Costs in 2026 (Every Scenario)
Let's cut through the confusion. Here's every realistic pricing scenario, ranked from cheapest to most expensive:
| Scenario | Monthly Cost |
|---|---|
| Insurance + Lilly Savings Card Best case | As low as $25/mo |
| Clinical trials | $0/mo |
| Medicare GLP-1 Bridge (July 2026–Dec 2027) | $50/mo copay |
| Ro: Zepbound vials (2.5mg) | $299/mo + $149/mo membership |
| Ro: Zepbound vials (5mg) | $399/mo + $149/mo membership |
| Ro: Zepbound vials (7.5–15mg) | $449/mo + $149/mo membership |
| Commercial insurance (no coverage) + Savings Card | As low as $499/mo |
| Retail pharmacy (no discounts) | ~$1,086/mo |
Prices verified March 2026. Costs vary by pharmacy, dose, and plan.
The Zepbound Savings Card — Who Gets It and How
If your commercial insurance covers Zepbound, Eli Lilly's savings card can bring your cost to as low as $25 per fill (up to a 3-month supply). The savings cap is $150 per 28-day supply, or $1,800 per year (Zepbound Savings).
If your commercial insurance does not cover Zepbound, the savings card can still help — eligible patients may pay as low as $499 for a 1-month supply.
Who can't use it: Medicare, Medicaid, TRICARE, VA, or other government-funded insurance beneficiaries. That's a federal regulation. Register at zepbound.lilly.com/coverage-savings.
LillyDirect Vials — The Cash-Pay Game Changer
In 2024, Eli Lilly launched single-dose vials specifically to make tirzepatide accessible for people paying out of pocket. These are FDA-approved Zepbound — just delivered in a vial you draw with a syringe instead of a prefilled autoinjector.
Starting prices: $299/month (2.5mg), $399/month (5mg), $449/month (7.5mg and up with timely refill). Available directly through LillyDirect or through Ro (sponsored affiliate link, opens in a new tab) (same pricing, plus clinical support).
Don't Forget Your HSA/FSA
Tirzepatide prescribed for a medical condition — obesity, type 2 diabetes, OSA — is eligible for Health Savings Account and Flexible Spending Account dollars. That effectively saves you 20–30% depending on your tax bracket. It may also be tax-deductible as a medical expense if you itemize deductions (above the 7.5% AGI threshold).
When Cash-Pay Makes More Sense Than Insurance
→ Your plan excludes weight-loss drugs.
No amount of PA paperwork will override a blanket weight-loss exclusion. Cash-pay gets you started immediately instead of wasting weeks on a guaranteed denial.
→ Your deductible is sky-high.
If you have a $5,000 or $8,000 deductible and haven't met it, you're paying out of pocket either way. Zepbound vials at $299–$449/month through Ro may actually be cheaper than your 'covered' price until you hit that deductible.
→ You want to start treatment NOW.
The insurance path takes 1–3 weeks minimum. Cash-pay through Ro means your first dose ships in under a week. Some people start cash-pay and then switch to insurance once their PA is approved — best of both worlds.
→ Your copay is higher than cash-pay pricing.
Some plans put GLP-1s on specialty tiers with 30–40% coinsurance. At a list price of $1,086, that's $325–$434/month before any savings card. Zepbound vials at $299/month could be less.
→ You're between jobs or switching plans.
Don't let a coverage gap derail your treatment. Cash-pay keeps continuity while you sort out your next plan.
The point isn't that insurance doesn't matter — it absolutely does, and $25/month beats $299/month every time. The point is that waiting for a coverage decision you're not confident about shouldn't stop you from starting a medication that could change your health trajectory.
Medicare, Medicaid, and Government Plans in 2026
If you're on a government insurance plan, the rules are different — and they're changing fast. This section has the latest.
Medicare: What's Covered Right Now
Federal law (the Medicare Modernization Act of 2003) currently prohibits Medicare Part D from covering medications prescribed solely for weight loss. That means:
Covered
- → Mounjaro for type 2 diabetes (most Part D plans)
- → Zepbound for obstructive sleep apnea (some plans)
- → Wegovy for cardiovascular risk reduction (beneficiaries with cardiovascular disease + overweight/obesity)
Not covered (yet)
- → Zepbound for weight loss only (federal prohibition)
- → Changes July 2026 via GLP-1 Bridge program
The Medicare GLP-1 Bridge — Launching July 2026
Biggest Medicare development in years
The Medicare GLP-1 Bridge begins July 1, 2026 and runs through December 31, 2027 (18 months) for eligible Part D beneficiaries. It covers Zepbound KwikPen, Wegovy, and Foundayo used for weight reduction, outside the normal Part D payment flow, with a $50 copay. BALANCE will not launch for Medicare Part D in 2027 — CMS extended the Bridge instead. Humana processes claims (BIN 028918 / PCN MEDDGLP1BR) (CMS ↗).
In November 2025, Eli Lilly also announced that Medicare beneficiaries will pay no more than $50 per month for Zepbound (in a new multi-dose pen format), pending FDA approval (Eli Lilly ↗).
Important nuance: The Bridge program does not apply when the drug is being used for an indication already coverable under basic Part D. If Zepbound is prescribed for OSA, it goes through the regular Part D formulary — not the Bridge.
Bottom line for Medicare beneficiaries:
The landscape is changing rapidly. If you've been told “Medicare doesn't cover weight-loss drugs,” the Bridge has changed that through December 2027. BALANCE did not launch for Medicare Part D in 2027 — CMS extended the Bridge instead. Check for BALANCE 2028 participation during fall 2027 open enrollment. The BALANCE model may still launch in Medicaid in states that opt in.
Medicaid: State by State
Only 13 state Medicaid fee-for-service programs cover GLP-1 medications for obesity as of early 2026, according to KFF (KFF). Coverage varies widely by state. Note that as of January 1, 2026, Medi-Cal (California's Medicaid program) no longer covers GLP-1s for weight loss, though prior authorization requests may still be considered for Zepbound when used for obstructive sleep apnea (Medi-Cal Rx ↗).
The BALANCE model is expected to expand Medicaid access starting May 2026, but participation is voluntary for states.
VA and TRICARE
The VA may cover tirzepatide through the MOVE! Weight Management Program — talk to your VA benefits coordinator. TRICARE Prime and Select beneficiaries can have weight-loss medications covered with approved prior authorization, though rules vary by program (MilitaryRx ↗). Government plan beneficiaries are not eligible for Eli Lilly's manufacturer savings cards, but cash-pay options through LillyDirect or Ro (sponsored affiliate link, opens in a new tab) remain available.
How to Get Tirzepatide Online Without Insurance (Or Without the Wait)
Let's be honest about something: the insurance path works, but it's slow. Prior authorization takes 1–3 weeks. Appeals can take longer. And if you've been thinking about this for months, another month of waiting feels like forever.
That's why a growing number of people are choosing to pay cash — even some who have insurance. They start treatment while the insurance process runs in the background. First dose in under a week vs. first dose in three weeks is a real consideration when you're ready to begin.
What to Look For in a Legitimate Online Provider
Not all telehealth weight-loss services are created equal. Before you hand over your credit card, check these boxes:
Prescribes FDA-approved medications (Zepbound, Wegovy, Ozempic — not unverified alternatives)
Licensed physicians review your health history and prescribe treatment
Transparent pricing — no hidden consultation fees, no bait-and-switch
Ongoing clinical support — monthly check-ins, side-effect management, dose adjustments
Clear medication sourcing — from licensed pharmacies or directly from the manufacturer
Insurance support if you want to pursue coverage simultaneously
Easy cancellation — no long-term contracts or cancellation penalties
Why We Recommend Ro for Most People
We've reviewed a dozen telehealth GLP-1 providers. For this specific search — how to get tirzepatide covered by insurance online — Ro (sponsored affiliate link, opens in a new tab) stands out because it's built around the exact problem you're trying to solve.
Insurance concierge.
Ro's team checks your insurance coverage, submits prior authorization paperwork, and fights denials on your behalf. That's not a common offering. Most telehealth providers send you a prescription and wish you luck. Ro actually gets in the trenches with your insurer.
FDA-approved brand-name medications.
Through a direct integration with LillyDirect, Ro offers Zepbound vials ($299–$449/month) plus Wegovy in both injection and the new oral pill form. These are the real, FDA-approved medications — not compounded alternatives.
Dual path: insurance AND cash-pay.
If your insurance covers tirzepatide, great — Ro helps you get it at your copay. If it doesn't, they seamlessly pivot you to the most affordable cash-pay option. You don't have to start over somewhere else.
Clinical support that goes beyond a prescription.
Monthly check-ins with board-certified providers. Unlimited messaging. Side-effect guidance. Dose titration management. A full curriculum of nutrition, sleep, and exercise content.
Available in all 50 states
And Washington D.C. (though specific service availability may vary by state).
What it costs: $39 for the first month, then $149/month for the Ro Body membership. Medication is billed separately — costs depend on your treatment plan and insurance situation (Ro Pricing ↗).
What Real People Are Saying
“My experience with Ro has been so very positive. The care and communication has been second to none. The results I have seen since beginning Zepbound have given me a new sense of confidence and happiness that I did not know that I was missing.”
— Billy S., Ro member
“From the team at Ro literally handling all the insurance — I'd never heard of a prior authorization much less knew how to get one — to tracking down medication so I never had to miss a dose... I highly recommend advocating for your own health and having Ro as your provider has been such a relief.”
— Colleen B., Ro member
“Zepbound was different. The weight started to come off that first week, and continues to do so. I can now climb stairs without having to stop and catch my breath. I can just move my body more, and I feel really good doing so.”
— Stephanie, Ro member on Zepbound — lost 74 pounds in approximately eight months
Note: Ro members were compensated for their testimonials. (Ro Reviews ↗)
In clinical trials, people taking tirzepatide (with diet and exercise) lost an average of 15–21% of their body weight over 72 weeks, depending on dose — roughly 35 to 52 pounds. At the highest dose (15mg), average weight loss was approximately 20.9% at 72 weeks (SURMOUNT-1, NEJM ↗). That's not a marginal difference. For many people, it's life-changing.
You've done the research. You know the paths. The only step left is starting.
See If You're Eligible Through Ro
Ro checks your insurance, fights for coverage if you have it, and connects you with the most affordable FDA-approved option if you don't — all in one place.
10-minute online visit. Options within 2 days. Cancel anytime.
See If You're Eligible Through Ro — $39 First Month → (sponsored affiliate link, opens in a new tab)$39 first month, then $149/mo. Medication billed separately based on your plan.
The CVS Caremark Situation: What Changed and What to Do Now
If you're here because CVS Caremark dropped Zepbound from its formulary in 2025, you're not alone. This caught a lot of people off guard.
What happened: On CVS Caremark's Standard Control, Advanced Control, and Value formularies, Zepbound was removed effective July 1, 2025. Wegovy remains the preferred GLP-1 for weight loss. This was a PBM formulary decision — contract negotiations between pharmacy benefit managers and drug manufacturers — not a clinical one (CVS Caremark ↗).
What it means for you:
- If you're currently on Zepbound through CVS Caremark, your existing prior authorization will transition to Wegovy. You won't need a new PA for Wegovy.
- If you've tried Wegovy and it didn't work (or caused intolerable side effects), you can request a formulary exception for tirzepatide. Exception criteria exist for some CVS Caremark formularies, and approved exceptions have resulted in Mounjaro coverage even for patients without type 2 diabetes.
- The exception process: submit a PA for Zepbound → receive a denial (this is expected and necessary) → submit a Letter of Medical Necessity with documentation of Wegovy failure → exception review → potential approval for Mounjaro.
It's bureaucratic and frustrating. But there are documented paths through it. Your doctor or a service like Ro's insurance concierge (sponsored affiliate link, opens in a new tab) can navigate this process for you.
Tirzepatide Coverage for Specific Conditions
Can You Get Tirzepatide Covered Without Diabetes?
Yes. Zepbound is FDA-approved specifically for weight management — diabetes is not required (FDA label ↗). The coverage criteria center on BMI (≥30, or ≥27 with a weight-related comorbidity), not on having diabetes. Your doctor prescribes Zepbound (not Mounjaro), and the PA documentation focuses on your weight, comorbidities, and prior weight-management efforts.
That said, coverage rates for weight-loss indications are lower than for diabetes. Be prepared to appeal if needed.
Can You Get Tirzepatide Covered for Sleep Apnea?

This is one of the strongest coverage angles available right now.
In December 2024, the FDA approved Zepbound for moderate-to-severe obstructive sleep apnea in adults with obesity (FDA announcement ↗). Clinical trials showed significant reductions in sleep apnea severity.
Why this matters for coverage: Some insurance plans that exclude “weight-loss medications” will still cover medications prescribed for sleep apnea — because OSA is a recognized medical condition, not a “lifestyle” concern. If you have both obesity and moderate-to-severe sleep apnea, leading with the OSA diagnosis may unlock coverage that would otherwise be denied.
Even some Medicare Part D plans cover Zepbound for OSA, despite the federal prohibition on covering weight-loss drugs.
Can You Get Tirzepatide Covered for PCOS?
PCOS is not an FDA-approved tirzepatide indication. Coverage is more plausible when you independently meet Zepbound's obesity or overweight criteria (BMI ≥30, or ≥27 with a comorbidity). Some payer policies do explicitly list PCOS among acceptable weight-related comorbidities, but others do not. If PCOS is the only diagnosis without meeting BMI thresholds, coverage is much less likely.
Work with your doctor to frame the PA around your BMI and qualifying comorbidities, with PCOS and any insulin resistance listed as supporting evidence.
What Is Tirzepatide and Why Does It Work So Well?
If you're reading this section, you probably already know tirzepatide works. But understanding the science helps — both for your own confidence and because it strengthens your prior authorization case.
The short version: Tirzepatide is a dual GIP/GLP-1 receptor agonist. That's a technical way of saying it mimics two hormones your body naturally produces — GLP-1 and GIP — that regulate appetite, blood sugar, and digestion. By activating both hormones (instead of just GLP-1, like semaglutide), tirzepatide produces stronger appetite suppression and greater weight loss.
What the Clinical Trials Showed
16–22.5%
Average body weight loss at 72 weeks in SURMOUNT-1 (highest dose: ~20.9%)
Source: SURMOUNT-1, NEJM
94%
Reduction in risk of progressing from prediabetes to type 2 diabetes in adults with obesity (3-year study)
Source: SURMOUNT-4
3 indications
FDA-approved for weight loss (Zepbound), type 2 diabetes (Mounjaro), and moderate-to-severe OSA (Zepbound)
Source: FDA
Common side effects include nausea, diarrhea, decreased appetite, and constipation — mostly during dose increases. They typically improve as your body adjusts. Serious side effects are rare but include a boxed warning about thyroid tumors (do not use if you or your family have a history of medullary thyroid carcinoma or MEN 2), pancreatitis, and gallbladder problems.
Tirzepatide is a once-weekly injection. It's a prescription medication — you'll need a licensed provider to determine if it's right for you.
What NOT to Do If You Want Legitimate Coverage
Don't ask your doctor to code inaccurately.
Submitting a diabetes diagnosis code when you don't have diabetes is fraud. It's also unnecessary — Zepbound is FDA-approved for weight loss. Use the correct diagnosis and build a strong PA case.
Don't assume a 'coverage checker' is a guarantee.
Coverage checkers (including Ro's) give you a report based on what your plan says. Actual coverage still depends on your specific PA and clinical documentation.
Don't skip the appeal.
A denial feels final. It usually isn't. The overturn rates speak for themselves.
Don't confuse compounded tirzepatide with the insurance path.
Insurance rarely covers compounded medications. The FDA has raised safety concerns about unapproved compounded GLP-1 products and determined that the tirzepatide shortage is resolved — meaning compounding pharmacies face restrictions. For the insurance coverage path, stick with FDA-approved Zepbound or Mounjaro.
Don't pay full retail without checking alternatives first.
Nobody should pay $1,086/month when $299/month Zepbound vials exist. Check savings cards, manufacturer programs, and telehealth cash-pay options before accepting the sticker price.
How We Research and Verify This Guide
- •Pricing and coverage data are verified monthly against manufacturer websites (Eli Lilly, LillyDirect), insurance formulary databases, and official CMS publications.
- •Policy changes are tracked through CMS announcements, insurer bulletins, state Medicaid updates, and published federal rules.
- •Clinical data references FDA prescribing information (Mounjaro label, Zepbound label), published clinical trials (SURMOUNT-1), and peer-reviewed journal articles.
- •Real user experiences are reviewed across Reddit, Trustpilot, and patient forums to identify real-world coverage challenges.
- •Every claim is sourced. Where we cite statistics, we link to the primary source. If we can't verify something, we say so. Coverage rules change — always confirm with your specific plan.
- •Affiliate relationships never influence our coverage analysis. We recommend the same paths we'd recommend to our own family. Our disclosure is at the top of every page.
Related Guides
Frequently Asked Questions
Is tirzepatide covered by insurance?
It depends on your plan, the brand prescribed, and the diagnosis. Coverage is much more common for type 2 diabetes (Mounjaro) than for weight loss (Zepbound). KFF found only about 19% of large firms cover GLP-1s specifically for weight loss. Call your insurer or use a free coverage checker like Ro's to find out your specific situation.
How much does tirzepatide cost with insurance?
With commercial insurance coverage and the Eli Lilly savings card: as low as $25/month. Without the savings card, copays vary widely by plan tier and cost-sharing structure.
How much does tirzepatide cost without insurance?
FDA-approved Zepbound single-dose vials start at $299/month through LillyDirect or providers like Ro (plus Ro's $149/mo membership). Full retail for brand-name pens is approximately $1,086/month — but savings programs and telehealth options mean almost nobody needs to pay that.
Does Medicare cover tirzepatide for weight loss?
Not as a standard Part D benefit under current law. However, the Medicare GLP-1 Bridge demonstration program launches July 2026 and will cover Zepbound for weight loss at a $50/month copay for eligible beneficiaries. Medicare currently covers Mounjaro for diabetes and Zepbound for obstructive sleep apnea through standard Part D formularies.
What is prior authorization for tirzepatide?
Prior authorization is a documentation process where your doctor submits evidence to your insurance company proving you medically need tirzepatide. It typically requires BMI documentation, comorbidities, records of previous weight-management attempts, and sometimes a letter of medical necessity. Timelines vary by plan type.
What should I do if my insurance denied tirzepatide?
Appeal. KFF found that in Medicare Advantage, more than 8 in 10 appealed PA denials were overturned each year from 2019–2024. Commercial plan overturn rates vary but tend to favor persistence. Your doctor can file a Letter of Medical Necessity. For commercial/ACA plans you generally have 180 days; for Medicare Part D, the first appeal is due within 60 days.
Can I get tirzepatide online?
Yes. Telehealth providers like Ro prescribe FDA-approved tirzepatide (Zepbound) through online consultations. If paying cash, Zepbound vials ship directly to your door in under a week. If using insurance, Ro's concierge handles the coverage process.
What's the difference between Zepbound and Mounjaro?
Same medication (tirzepatide), same doses, same manufacturer (Eli Lilly). Mounjaro is FDA-approved for type 2 diabetes. Zepbound is approved for weight loss and obstructive sleep apnea. The brand your doctor prescribes affects your insurance coverage, not the medication itself.
Is Mounjaro easier to get covered than Zepbound?
Generally, yes — for patients with type 2 diabetes. Diabetes coverage is far more common than weight-loss coverage. If you have both diabetes and obesity, Mounjaro may be the smoother path.
How long does tirzepatide prior authorization take?
Timelines vary. ACA plans generally have up to 15 days for standard requests, 72 hours for urgent. Medicare drug plans follow different timelines. Ro says its overall insurance workflow typically takes about 2–3 weeks.
Can I use an HSA or FSA to pay for tirzepatide?
Yes. Tirzepatide prescribed for a medical condition (obesity, diabetes, OSA) is eligible for HSA and FSA funds, effectively saving you 20–30% depending on your tax bracket.
Is compounded tirzepatide covered by insurance?
Almost never. Insurance plans rarely cover compounded medications. The FDA has also restricted compounding of tirzepatide now that the brand-name shortage is resolved, and has warned about safety risks with unapproved compounded versions.
Does Ro help with prior authorization?
Yes. Ro's insurance concierge checks your coverage, submits PA paperwork on your behalf, and helps fight denials. This is included in the Ro Body membership ($39 first month, then $149/month). Medication costs are separate.
What insurance covers Zepbound in 2026?
Coverage varies by insurer and specific plan. Some employer plans through BCBS, UnitedHealthcare, Aetna, and Cigna cover it. CVS Caremark removed Zepbound from certain formularies in 2025 but allows exceptions. Medicare is launching a $50/month program in July 2026. Always check your specific formulary.
What if my plan excludes weight-loss drugs entirely?
A blanket anti-obesity exclusion usually blocks the weight-loss pathway, but it does not automatically rule out coverage under a different indication — such as type 2 diabetes (Mounjaro) or obstructive sleep apnea (Zepbound) — if you qualify. Other options: switch to a plan that covers GLP-1s during open enrollment, ask your employer's HR about adding coverage, or use cash-pay options (Zepbound vials starting at $299/month through Ro or LillyDirect).
Your Next Step
You now know more about tirzepatide insurance coverage than most people who've spent hours searching. Every path is mapped. Every scenario is covered. Every follow-up question is answered.
The only thing left is starting.
If you want a team that checks your insurance, fights for coverage, and gives you the most affordable FDA-approved option — whether you're covered or not — Ro does all of that in one place.
$39 first month. 10-minute online visit. Know your options in 2 days. Cancel anytime.
Sources Cited in This Article
- Mounjaro (tirzepatide) FDA prescribing information, 2025
- Zepbound (tirzepatide) FDA prescribing information, 2026
- SURMOUNT-1: Jastreboff AM et al., “Tirzepatide Once Weekly for the Treatment of Obesity,” NEJM 2022
- KFF: Medicare Advantage Prior Authorization Determinations, 2024
- KFF: 2025 Employer Health Benefits Survey
- KFF: Medicaid Coverage of and Spending on GLP-1s
- GoodRx: Tracking Insurance Coverage for Weight Loss Medications
- CMS: Medicare GLP-1 Bridge Demonstration Program
- FDA: Approval of Zepbound for Obstructive Sleep Apnea, December 2024
- Eli Lilly: Zepbound Savings Card Program
- HealthCare.gov: Internal Appeals for Insurance Coverage Denials
- AMA: Prior Authorization Overturn Rates, Medicare Advantage
- CVS Caremark: GLP-1 Formulary Changes, 2025
- Medi-Cal Rx: GLP-1 Coverage Changes, January 2026
- Eli Lilly: Medicare Zepbound Access Announcement, November 2025
- Eli Lilly: Zepbound List Price Information
- FDA: Concerns about Unapproved GLP-1 Drugs Used for Weight Loss