The Bottom Line
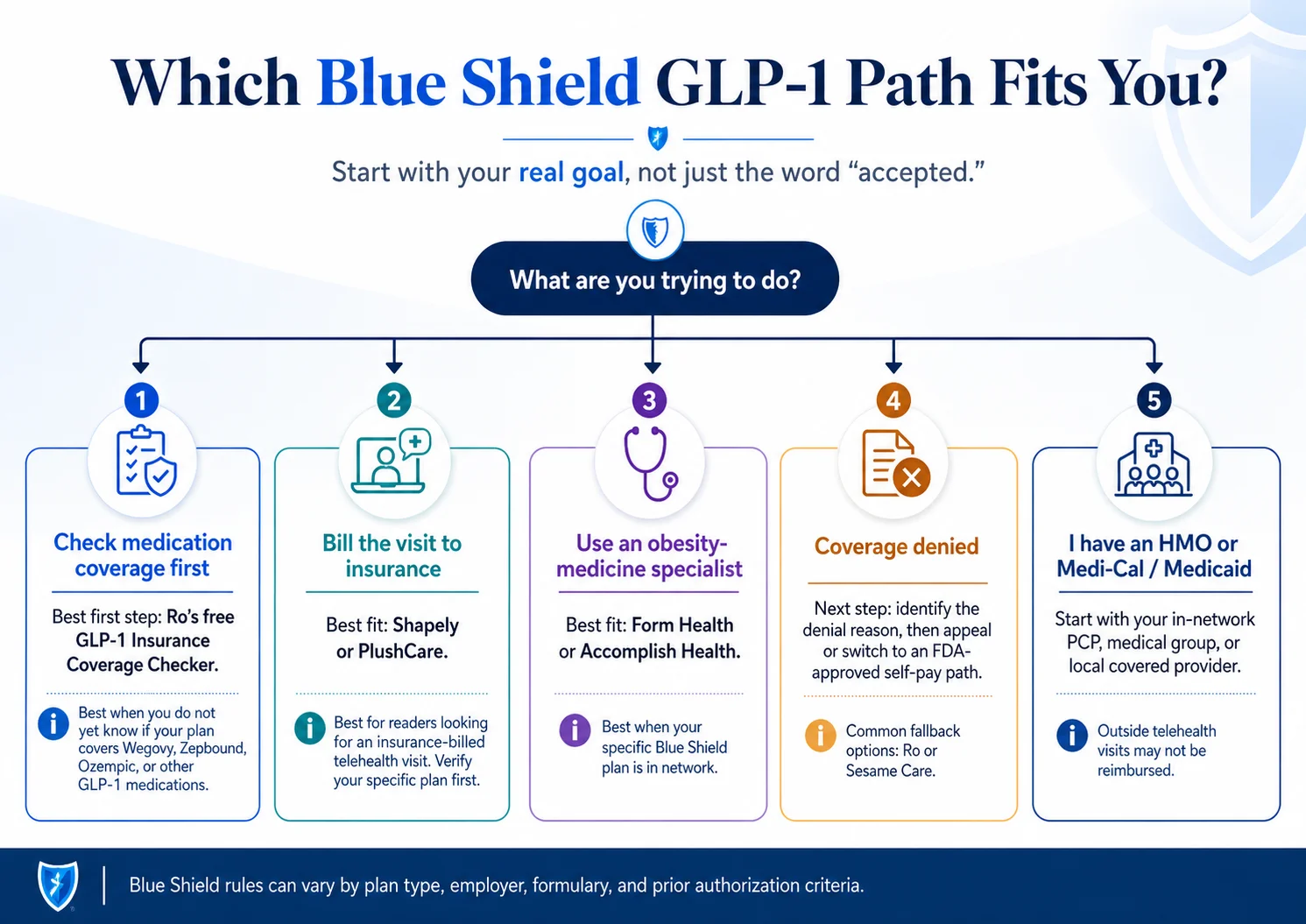
If you're searching for GLP-1 providers that accept Blue Shield, here's the truth most pages skip: “accepts Blue Shield” can mean four different things, and the right move depends on which one you actually need.
For most Blue Shield members, the smartest first step is Ro's free GLP-1 Insurance Coverage Checker. You enter your insurance info, Ro reaches out to your plan, and you get a personalized report back showing whether your plan covers Wegovy, Zepbound, or Ozempic — and whether prior authorization is required. New Ro accounts get a $50 credit for using the checker.
If you'd rather have your telehealth visit billed directly to your Blue Shield PPO, two providers publicly say they accept Blue Shield: Shapely (in California, Florida, New York, and Texas) and PlushCare (most Blue Shield of California plans, with a typical copay around $30). If your plan doesn't cover GLP-1s for weight loss at all — and a growing list of plans don't in 2026 — Ro and Sesame Care match the manufacturers' direct cash-pay prices on FDA-approved options.
Check your Blue Shield GLP-1 coverage with Ro — free
Free coverage report. No Ro account needed up front. New accounts get a $50 credit.
Check My Blue Shield Coverage Free →Quick Match: Find Your Blue Shield Path in 30 Seconds
| Your situation | Best first move | Why |
|---|---|---|
| “I don't even know if my Blue Shield plan covers a GLP-1.” | Ro's free GLP-1 Insurance Coverage Checker | Answers the biggest-dollar question before you pay any membership fee. |
| “I want my telehealth visit itself billed to my Blue Shield PPO.” | Shapely (CA, FL, NY, TX) or PlushCare (broader) | Both publicly state they accept Blue Shield / Blue Shield of California. Shapely is the strongest exact PPO fit; PlushCare runs broader. |
| “I want a real obesity-medicine doctor running my prior auth.” | Form Health or Accomplish Health | Both publicly state they take most major commercial insurance. Confirm your specific plan first. |
| “I have Blue Shield HMO.” | Start with your in-network PCP or medical group | HMO rules usually require a referral inside the medical group. An outside telehealth visit may not be covered. |
| “I have Blue Shield Promise (Medi-Cal).” | Read Medi-Cal Rx 2026 GLP-1 rules first | Medi-Cal Rx limits most GLP-1s to non-weight-loss uses starting Jan 1, 2026. Different rules, different path. |
| “My Blue Shield plan dropped GLP-1 coverage in 2026.” | Cash-pay through Ro or Sesame Care | Both match the manufacturers' direct prices on FDA-approved Wegovy, Zepbound, and Foundayo. |
| “Blue Shield denied my prior authorization.” | Identify the denial type → appeal or pivot | A criteria-based denial, a step-therapy block, and a plan exclusion each need a different next step. |
“Accepts Blue Shield” Means Four Different Things
Most “best Blue Shield GLP-1 providers” pages mash three vague words together: insurance accepted. Before you hand over a credit card, you need to know which of these four things a provider actually does for you:
1. They bill your Blue Shield plan for the telehealth visit itself.
The doctor visit is run through your insurance. You pay a copay — often around $30 — like a normal in-network appointment. Examples on this page: Shapely, PlushCare, Form Health, Accomplish Health.
2. They get the medication covered through your Blue Shield pharmacy benefit.
This is a separate question from the visit. Whether your medication is covered depends on your formulary, your pharmacy benefit manager, your diagnosis, and prior authorization. Ro's insurance concierge — a team that handles insurance work for you — is the strongest example here.
3. They help with prior authorization paperwork.
Most legit providers will at least submit the form. Some go further with appeals and case management. Ro runs a dedicated team. Sesame's Success-by-Sesame providers each handle their own. Form Health's obesity-medicine doctors file PAs all day long. See our full guide to providers that help with prior authorization.
4. They offer a cash-pay backup if Blue Shield says no.
This is not the same as accepting Blue Shield. Cash-pay providers don't bill your insurance — they're a backup when coverage fails. Ro's cash-pay GLP-1 prices match the manufacturers' direct prices through LillyDirect®, NovoCare®, and TrumpRx — currently the lowest published prices for FDA-approved Wegovy, Zepbound, and Foundayo.
A provider can do one, two, three, or all four. The right pick depends on which one matters most to you.
Which GLP-1 Providers Accept Blue Shield in 2026? The Verified Matrix
What we verified on April 30, 2026: each provider's published insurance language, current pricing pages, Blue Shield-specific claims, prior authorization workflows, state availability where listed, and material limitations. What only you can verify: your specific plan's formulary, your employer's pharmacy benefit, your deductible, and whether your specific prior auth gets approved.
| Provider | Bills Blue Shield for visits? | Helps with medication coverage / prior auth? | Membership cost (2026) | FDA-approved cash-pay backup? | Best Blue Shield use case |
|---|---|---|---|---|---|
| Ro | No — Ro Body membership is cash-pay | Yes — dedicated insurance concierge handles benefits checks, prior auth, and post-denial steps. Supports FEHB members. | $39 first month, then $149/month — or as low as $74/month with annual prepay | Yes — matches LillyDirect®, NovoCare®, and TrumpRx pricing on Wegovy, Zepbound, and Foundayo | Best first step if you don't yet know whether Blue Shield will cover your medication |
| Shapely | Yes — provider-stated for most PPO plans including Blue Shield | Yes — team helps handle prior auth and documentation | $49/month membership; meds and labs separate | Compounded self-pay option (compounded drugs are not FDA-approved as finished products) | Best Blue Shield PPO fit in CA, FL, NY, or TX |
| PlushCare | Yes — accepts copays for most Blue Shield of California, BCBS, Anthem, Aetna, Humana, and Medicare plans | Partial — care team can start prior auth; less GLP-1-specialized than Ro or Form | $19.99/month after first month; in-network visits typically $30 or less; uninsured visits $129 | Limited | Best broad nationwide Blue Shield-billed telehealth visit option |
| Sesame Care | No — subscription is cash-pay | Yes — your chosen Success provider files prior auth paperwork | $59/month with annual / $99/month month-to-month | Yes — Wegovy pen $199/mo intro then $349/mo; Zepbound KwikPen $299–$698/mo by dose; Foundayo $149–$349/mo by dose | Best lower-cost provider-choice alternative if Ro's centralized concierge isn't your style |
| Form Health | Generally yes — accepts most major private insurance and Medicare | Yes — care team navigates prior auth as standard practice | $299/month if uninsured or not covered | Yes (FDA-approved only — Form does not prescribe compounded GLP-1s) | Best obesity-medicine specialist team if your specific Blue Shield plan is in-network |
| Accomplish Health | Publicly in-network with Blue Cross Blue Shield (Blue Shield-specific status varies; verify before booking) | Yes — insurance-covered obesity care model | Insurance-billed; cost depends on your plan | N/A — insurance-first model | Best in-network specialist BCBS path. Does not participate with Medicare Advantage or EPO plans. |
Why We Won't Recommend MEDVi, Sprout Health, or Other Compounded GLP-1 Providers on This Page
On March 3, 2026, the FDA announced 30 warning letters to telehealth companies marketing compounded semaglutide and tirzepatide products. MEDVi received its own letter (Letter #721455, dated February 20, 2026). Sprout Health received a separate FDA warning letter (Letter #715879). The FDA cited misleading website language — claims like “same active ingredient as Wegovy” and language implying that compounded products were FDA-approved.
On April 30, 2026 — the day this page was published — the FDA proposed excluding semaglutide, tirzepatide, and liraglutide from the 503B bulks list, finding no clinical need for outsourcing facilities to compound these drugs from bulk substances. Public comments on that proposal are due June 29, 2026.
On a Blue Shield page specifically, none of them are the right answer. We did not verify any Blue Shield formulary that covers compounded GLP-1s — they're all cash-pay. And insurance-sensitive readers deserve insurance-sensitive, FDA-approved answers. If you decide compounded is right for your situation after exhausting FDA-approved options, that's a separate decision and we have a separate guide. On this page, every recommendation routes to FDA-approved options.
Which Blue Shield GLP-1 Provider Should You Pick?
Ro — Best for Coverage Discovery + FDA-Approved Cash-Pay Backup
If you don't know whether your Blue Shield plan covers a GLP-1, Ro's free GLP-1 Insurance Coverage Checker is the highest-leverage thing you can do today. You enter your insurance info. Ro reaches out to your plan. You get back a personalized report showing your coverage status and any prior authorization requirements. New Ro accounts get a $50 credit for using it. You don't have to become a Ro member to run the check.
If you do continue as a Ro Body member, Ro's insurance concierge takes over — the concierge submits your prior auth, coordinates with your pharmacy, and helps with next steps if your plan denies coverage. If one medication gets denied, Ro-affiliated providers can review whether a different GLP-1 is clinically appropriate and resubmit. Ro is the only provider in this comparison that pairs a free pre-check with a dedicated team — separate from your individual prescriber — that runs the back-and-forth with your insurer.
The numbers (verified April 30, 2026):
- Membership: $39 for the first month, then $149/month — or as low as $74/month if you prepay annually
- Medications available: Wegovy® (pen and pill), Zepbound® (KwikPen, pens, and vials), Ozempic® off-label, Mounjaro® off-label, Foundayo™ (FDA-approved April 1, 2026), and Saxenda®
- Cash-pay prices are matched to the manufacturers — Wegovy at NovoCare prices, Zepbound at LillyDirect prices, Foundayo at Lilly's launch pricing. No markup.
- Time to first dose: about a week if paying cash, longer if going through insurance because the prior auth process usually takes 2–3 weeks
- Insurance support: full prior auth workflow plus FEHB. Federal employees with FEHB can join Ro Body and access the insurance concierge.
Free coverage report. No Ro account required up front. New accounts get a $50 credit.
Sesame Care (Success by Sesame) — Best Lower-Cost, Provider-Choice Alternative
Success by Sesame is the better choice if (a) picking your own doctor matters more to you than centralized concierge support, (b) you want a lower subscription cost than Ro, and (c) you're comfortable with a provider-led prior auth process — your chosen Success provider files your paperwork.
The numbers (verified April 30, 2026):
- Subscription: $59/month with an annual plan, or $99/month month-to-month (billed every 28 days)
- Provider choice: browse profiles, reviews, and ratings before booking — no random matching
- Medications: Wegovy, Zepbound, Ozempic, Mounjaro, Saxenda, Rybelsus, Foundayo, Contrave, metformin — 14 prescription weight-loss options
- Cash-pay prices: Wegovy pill $149–$299/mo by dose; Wegovy pen $199/mo intro then $349/mo; Zepbound KwikPen $299–$698/mo by dose; Foundayo $149–$349/mo by dose
- Costco member benefit: 10% off Sesame's weight-loss program
Pick your provider. Run your visit. Get your prior auth filed.
Shapely — Best Direct Blue Shield PPO Visit Billing (Limited States)
If your top priority is having the telehealth visit itself billed to Blue Shield PPO — and you live in California, Florida, New York, or Texas — Shapely is the cleanest exact-fit option we've found. Shapely's public Blue Cross Blue Shield landing page states the program accepts most PPO plans including Blue Shield, and the team helps with prior authorization for medications like Wegovy and Zepbound.
- Membership: $49/month (separate from your visit copay; usually not a covered insurance benefit)
- Visits, labs, and medications: typically billed through your Blue Shield PPO if in-network
- States listed: California, Florida, New York, Texas (verify the current state list before booking)
We don't have a commercial relationship with Shapely. If they fit, you can verify directly:
PlushCare — Best Broad Blue Shield of California Telehealth Visit Option
PlushCare is one of the few consumer telehealth brands that bills commercial insurance for the visit itself in most states. PlushCare's How It Works page states it accepts copays from most Blue Shield of California, Blue Cross Blue Shield, Anthem Blue Cross, Aetna, Humana, and Medicare plans, with most in-network patients paying $30 or less per visit.
- Membership: first month included with first visit, then $19.99/month
- In-network visits: $30 or less for most Blue Shield of California / BCBS members
- Uninsured visits: $129
- Membership fee: generally not a covered insurance benefit (separate from your copay)
- Cost estimates are not guarantees — PlushCare confirms benefits at the visit
Form Health & Accomplish Health — Best Specialist Routes If Your Plan Is In-Network
Form Health publicly states it accepts most major private insurance and Medicare. Visits, labs, and medications can all be billed through your insurance when your plan covers them. The clinical team is built around board-certified obesity-medicine specialists who file prior auths as routine work. If you're uninsured or your plan doesn't cover the program, the self-pay program is $299/month. Form prescribes FDA-approved-only medications — no compounded GLP-1s. Verify your specific Blue Shield plan is in-network before signing up.
Accomplish Health publicly states it is in-network with Blue Cross Blue Shield and offers virtual, insurance-covered obesity care. Blue Shield-specific status varies by state and plan, so verification is required. Accomplish currently does not participate with Medicare Advantage or EPO plans.
For both providers, call the number on the back of your Blue Shield card and ask: “Is [Form Health / Accomplish Health] an in-network provider for my plan?” A 5-minute call now beats a denied claim later.
Find Your Blue Shield Plan Type and Path
Blue Shield of California Commercial PPO
This is the largest single bucket of readers. Your three real questions:
- Did your employer keep GLP-1 weight-loss coverage in 2026? Blue Shield of California's 2026 large-group commercial coverage varies a lot. Some plans require Class III obesity (BMI of 40 or higher) with documented participation in a comprehensive weight-management program. Others may cover at BMI 30, or BMI 27 with related conditions. Some employers may choose no weight-loss drug coverage at all.
- Is the medication on your plan's formulary? Blue Shield's drug formulary tools change over time and vary by plan. Check yours directly through your member portal or the Price Check My Rx tool.
- What's your starting BMI documented as in your medical record? This is the one number Blue Shield will check first.
Best first move: run Ro's free coverage check. If your plan kept weight-loss coverage, Ro's concierge handles the prior auth. If your plan dropped it, you'll know right away — without paying a membership fee — and can switch to the cash-pay or formulary-exception path.
Blue Shield of California HMO
HMO members can usually only see in-network providers. Visits with outside telehealth services typically aren't billed through insurance. Your real first call is your in-network primary care doctor or your medical group's obesity-care pathway, not an outside telehealth brand. A Ro or Sesame visit might still help as a coverage check or a cash-pay path, but don't expect HMO reimbursement for the visit itself.
Blue Shield Promise (Medi-Cal)
Medi-Cal Rx published 2026 GLP-1 changes effective January 1, 2026. Wegovy, Zepbound, Saxenda, Ozempic, Rybelsus, Mounjaro, Victoza, Byetta, Bydureon, and Trulicity are not covered for weight-loss-only use. Some non-weight-loss uses may still be covered by diagnosis code or prior authorization (Type 2 diabetes, certain cardiovascular indications).
Telehealth providers like Ro do not coordinate Medicaid coverage in any state. Your real path is an in-network provider through your Medi-Cal Managed Care Plan, with a covered diagnosis if it fits medically.
Anthem Blue Cross of California (Important: This Is Not Blue Shield)
BlueCard PPO / Out-of-State BCBS
If you have a Blue Shield PPO in one state and you're traveling or living in another, your BlueCard lets you use the local Blue affiliate's network for medical visits. But prescription drug coverage is not the same as medical-network access. A BlueCard visit may go in-network. Your Wegovy prescription still has to clear your home plan's pharmacy benefit and prior auth criteria.
Federal Employee Health Benefits (FEHB) / Blue Cross and Blue Shield Service Benefit Plan
The Office of Personnel Management requires every FEHB carrier — including the BCBS Service Benefit Plan — to cover at least one GLP-1 weight-loss medication. That gives federal employees a coverage floor private plans don't always have. For specific 2026 tier placements and out-of-pocket costs on FEP Blue Standard, FEP Blue Basic, and FEP Blue Focus, check the current FEP formulary directly at fepblue.org.
Ro says FEHB members can join Ro Body and access the insurance concierge. If you're a federal employee, Ro is likely your fastest path because they handle the formulary exception process and prior auth on your behalf.
Does Blue Shield Cover GLP-1 Medications in 2026?
Wegovy (Semaglutide for Weight Loss)
Some Blue Shield commercial plans cover Wegovy with prior authorization in 2026. Common prior auth requirements include BMI of 30 or higher (or BMI of 27 or higher with at least one weight-related condition like Type 2 diabetes, hypertension, sleep apnea, or cardiovascular disease). When covered with a Novo Nordisk savings card stacked on top, eligible commercially-insured members can sometimes pay as little as $25/month.
If your plan denies Wegovy for weight loss, two alternate FDA-approved uses may apply if they fit your situation medically:
- Cardiovascular event reduction in adults with established cardiovascular disease plus obesity or overweight
- MASH (metabolic dysfunction-associated steatohepatitis) with moderate-to-advanced liver fibrosis
Zepbound (Tirzepatide for Weight Loss)
Some Blue Shield plans cover Zepbound with prior auth. Note that CVS Caremark removed Zepbound from its standard formulary in mid-2025 in favor of Wegovy, which affected many Blue Shield plans whose pharmacy benefit is run by CVS Caremark. Two alternate FDA-approved uses worth knowing:
- Obstructive sleep apnea (OSA): Zepbound was FDA-approved December 20, 2024, for moderate-to-severe OSA in adults with obesity
- With a Lilly savings card on top of Blue Shield approval, eligible commercially-insured patients can sometimes pay as low as $25/month
Ozempic and Mounjaro (For Type 2 Diabetes)
Blue Shield broadly continues to cover Ozempic and Mounjaro for Type 2 diabetes in 2026. Prior auth is typically required, with a confirmed Type 2 diabetes diagnosis. Off-label prescribing for weight loss is increasingly limited. If you have both Type 2 diabetes and obesity, prescribing the diabetes-indicated formulation may run into fewer coverage barriers while still delivering weight loss.
Foundayo™ (Orforglipron) — The New Oral GLP-1 Pill
The FDA approved Foundayo (orforglipron) on April 1, 2026, for chronic weight management. What makes Foundayo different: it can be taken any time of day with or without food and water restrictions — unlike oral semaglutide's strict timing rules. As of April 30, 2026, most Blue Shield plans haven't yet published formal formulary placement for Foundayo. The fastest current path is Ro at Lilly-matched pricing ($149 first month, $199–$299/month after).
Saxenda (Liraglutide for Weight Loss)
Daily injectable liraglutide is older and increasingly displaced by weekly Wegovy and Zepbound on Blue Shield formularies. When still covered, prior auth criteria mirror Wegovy.
Blue Shield Prior Authorization: What to Expect
Common Prior Auth Criteria to Check on Your Plan
Blue Shield is part of the broader Blue Cross and Blue Shield Association of 33 independent licensees. Each plan sets its own rules. There is no single “Blue Shield criteria.” What follows is a checklist of common items to ask about — not standard requirements across all plans. See also our guide to getting insurance to cover GLP-1.
- BMI threshold: Many plans use BMI of 30 or higher, or BMI of 27 or higher with at least one weight-related condition. Some Blue Shield plans require BMI 35 or 40 with a comprehensive weight-management program for formulary-level coverage.
- Documented lifestyle effort: Many plans want to see 3 to 6 months of nutrition, exercise, and behavioral change documented in your chart before starting the medication.
- No concurrent GLP-1 use: You can't be on Wegovy and Ozempic at the same time.
- Step therapy (must try other meds first): some plans require it, some don't. Verify with your specific plan.
- Renewal weight loss: some plans want documented weight loss (often 5%) at the 6-month renewal point. Verify with your specific plan.
- Adolescents (age 12 and up): Wegovy coverage typically requires BMI in the 95th percentile or higher.
The single most useful thing you can do is ask your plan for the prior auth criteria document in writing. It's your roadmap.
What Strengthens Your Prior Auth Approval
- Documented BMI at the time the prescription is written (height, weight history, the BMI calculation)
- 3 to 6 months of nutrition, exercise, and behavioral counseling notes in your medical chart
- Diagnosis codes documented for any related conditions (E11.x for Type 2 diabetes, I10 for hypertension, G47.33 for OSA, etc.)
- A failed prior weight-loss medication trial documented in your chart, if your plan requires step therapy
What Gets Prior Auths Denied
- BMI below the threshold
- Missing or thin lifestyle-program documentation
- Concurrent GLP-1 prescription
- Non-formulary tier without an exception request
- Plan-level benefit exclusion — this isn't a denial you can appeal through the standard process. It means your employer didn't buy GLP-1 weight-loss coverage. Different problem, different fix.
What to Ask Before Paying Any Membership Fee
The 7-Question Provider Script
- “Do you bill Blue Shield (or Blue Shield of California) for the visit itself, or is your membership fee separate from insurance?”
- “Do you accept my plan type — PPO, HMO, EPO, POS, Medicare Advantage, Medi-Cal, or FEHB?”
- “Will you submit the GLP-1 prior authorization for me?”
- “If Blue Shield denies the prior auth, will you support the appeal?”
- “Are medication costs included in the membership fee, or paid separately?”
- “Are labs included?”
- “Can I cancel the membership if Blue Shield ultimately won't cover the medication?”
The 7-Question Blue Shield Script (call the number on the back of your card)
Write down the rep's name, the date, and the reference number. Then ask:
- “Is Wegovy covered under my plan, and what tier is it on?”
- “Is Zepbound covered under my plan, and what tier is it on?”
- “Is Ozempic or Mounjaro covered only for Type 2 diabetes, or also for off-label weight-loss use?”
- “Is weight-loss-only GLP-1 use excluded from my plan's pharmacy benefit?”
- “What is the prior authorization criteria document for [medication name]? Can you email it to me?”
- “What's the exact denial reason code I would receive if I don't meet criteria?”
- “Is there a covered alternative — like Saxenda, Contrave, or another weight-loss medication — on my formulary?”
The single most useful sentence in those scripts is #5 to your insurer. Asking for the prior auth criteria document in writing turns a guessing game into a checklist.
What to Do If Blue Shield Denies Your GLP-1 Coverage
Step 1: Identify the Denial Type
| Denial reason | What it actually means | Your next step |
|---|---|---|
| Missing PA | Your provider never submitted, or Blue Shield didn't get it | Call your provider; confirm submission; ask for a copy |
| PA denied — criteria not met | Your documentation didn't satisfy BMI, step therapy, or lifestyle requirements | Request the denial letter and the clinical policy; gather the missing documentation; resubmit or appeal |
| Step therapy required | You must try a less expensive medication first | Discuss with your prescriber; either try the alternate or document a contraindication |
| BMI threshold not met | Plan requires a higher BMI than yours | Ask for medical records confirming your starting BMI; if you're below the threshold, you don't qualify on this indication |
| Lifestyle program requirement | Plan wants documented weight-management program participation | Submit program records; your provider can document concurrent participation |
| Benefit exclusion | Your plan doesn't cover weight-loss GLP-1s as a benefit | Standard appeal won't work. Move to formulary exception, alternate covered diagnosis, or cash-pay |
| Diagnosis mismatch | Medication covered for diabetes / OSA / CVD but not weight loss | Discuss medically appropriate diagnosis coding with your prescriber |
Step 2: Pick the Right Path
If it's a prior auth denial (criteria-based): You generally have 180 days for an internal appeal under most commercial Blue Shield plans. Get the denial letter. Identify the reason code. Ask for the clinical policy. Have your provider submit the missing documentation. Ro Body members get the insurance concierge to do this for them.
If it's a benefit exclusion (your employer dropped coverage): Standard appeals don't apply. Your three real options:
- Formulary exception request. Your provider submits a written argument that the medication is medically necessary and no covered alternative is appropriate.
- Alternate FDA-approved diagnosis (if it fits medically). Wegovy has a covered cardiovascular event reduction indication. Wegovy has a covered MASH indication. Zepbound has a covered OSA indication.
- Cash-pay through Ro or Sesame Care at LillyDirect / NovoCare / TrumpRx-matched pricing.
Step 3: The Honest Cash-Pay Math
FDA-approved options (verified April 30, 2026):
- Wegovy pen: $199/month introductory price for the first 2 monthly fills (NovoCare offer terms apply). Standard doses typically $349/month; Wegovy HD listed at $399/month.
- Wegovy pill (oral semaglutide): $149/month for lower doses (1.5mg, 4mg) or $299/month for higher doses (9mg, 25mg) via Ro at NovoCare-matched pricing.
- Zepbound vials (LillyDirect self-pay): $299/month for 2.5mg, $399/month for 5mg, $449/month for higher approved doses.
- Zepbound KwikPen via Ro: $299 first month. Discounted refill price $449/month for 7.5–15mg only when manufacturer offer terms are met (including a 45-day refill window).
- Foundayo: $149 first month, $199–$299/month after for higher doses (Lilly launch pricing, Ro-matched). Always verify Lilly's current launch terms.
A savings-card-stacked, covered Wegovy or Zepbound at $25/month will always beat any cash-pay option. But if your plan won't cover the medication, $149–$499/month for FDA-approved brand medication is the floor — and Ro is the cleanest cash-pay path because their prices are matched to the manufacturers' lowest published rates with no markup.
Common Mistakes Blue Shield Members Make With GLP-1 Telehealth
Mistake 1: Confusing visit coverage with medication coverage.
A provider can accept your Blue Shield PPO for a $30 visit copay while the medication itself is denied at the pharmacy. Two separate benefits. Two separate approval processes.
Mistake 2: Paying a membership fee before checking the formulary.
If Wegovy isn't on your Blue Shield formulary at all, no telehealth membership creates coverage. Run the free coverage check first.
Mistake 3: Assuming Blue Shield PPO and HMO follow the same rules.
They don't. HMO members usually need to start with an in-network primary care doctor or medical group, not an outside telehealth brand.
Mistake 4: Assuming Ozempic or Mounjaro will be covered for weight loss.
They probably won't be. Both are FDA-approved for Type 2 diabetes. Off-label weight-loss prescribing is getting more restricted, not less.
Mistake 5: Treating a benefit exclusion like a missing form.
A plan-level exclusion can't be appealed through the standard prior auth process. The right move is a formulary exception, an alternate covered diagnosis, or cash-pay.
Mistake 6: Not documenting your starting BMI before treatment begins.
Blue Shield will look at your medical record's BMI at the time the prescription was written. If you've already lost weight before your first visit, document your starting BMI clearly.
Mistake 7: Treating compounded 'alternatives' as a Blue Shield substitute.
They're not covered by Blue Shield. They're not regulatorily equivalent to FDA-approved brands. They belong in a different decision, not in the Blue Shield path.
What Patients Actually Say
“They support you, encourage you, and any question, they have an answer.”— Shapely patient testimonial, published on Shapely's website. Provider-published; testimonials shared with permission. Use as a service-experience signal only.
We could share more quotes from other providers, but we won't include any we can't link to a verifiable, sourced page on the provider's own site. Ro, Sesame Care, Form Health, and Shapely all publish patient stories on their own sites. Read them with the same caution you'd apply to any paid testimonial.
How We Built This Comparison
What we verified on April 30, 2026 (click to expand)
Verified directly:
- Pricing pages for Ro, Sesame Care, Shapely, PlushCare, and Form Health
- Cash-pay GLP-1 prices through LillyDirect, NovoCare, and TrumpRx — confirmed against each manufacturer's published direct-to-patient pricing
- Insurance acceptance language — pulled from each provider's official insurance and how-it-works pages
- Blue Shield of California medical policies — Drug Prior Authorization page, weight-loss medication policy, and 2026 coverage updates
- Medi-Cal Rx 2026 GLP-1 coverage changes (effective Jan 1, 2026)
- FDA-approval status of Wegovy, Zepbound, Ozempic, Mounjaro, Saxenda, and Foundayo — verified through drugs.fda.gov
- FDA enforcement landscape — 30 warning letters March 3, 2026; MEDVi Letter #721455; Sprout Health Letter #715879
- FDA's April 30, 2026 proposal to exclude semaglutide, tirzepatide, and liraglutide from the 503B bulks list
What only you can verify: your specific Blue Shield plan's formulary, your employer's pharmacy benefit, your deductible, and whether your specific prior auth gets approved.
Next scheduled review: July 2026, with monthly spot-checks for Blue Shield CA policy changes, FDA enforcement updates, and Foundayo formulary placement as 2026 coverage decisions roll out.
Frequently Asked Questions
Does Blue Shield cover GLP-1 medications like Wegovy or Zepbound in 2026?
Sometimes — depends on your specific plan, diagnosis, formulary, and prior authorization rules. Some Blue Shield commercial PPO plans cover Wegovy or Zepbound with prior auth for adults with BMI 30 or higher (or 27 or higher with related conditions). Some Blue Shield of California plans limit weight-loss GLP-1 coverage to Class III obesity (BMI 40 or higher) with documented program participation. Coverage for Type 2 diabetes (Ozempic, Mounjaro) remains broad in 2026.
What GLP-1 providers actually accept Blue Shield?
For Blue Shield PPO visit billing, Shapely (in CA, FL, NY, TX) and PlushCare (broader, around $30 copay) are the two providers with public verified Blue Shield acceptance. For medication coverage and prior authorization, Ro runs the most complete insurance concierge and supports FEHB members. Sesame Care's Success program is a lower-cost alternative where your chosen provider files prior auth paperwork.
Does Ro accept Blue Shield?
Ro Body membership is cash-pay — Ro does not bill Blue Shield for the visit itself. But Ro's insurance concierge does work with Blue Shield and most major commercial plans on GLP-1 medication coverage and prior auth, and Ro's free GLP-1 Insurance Coverage Checker reaches out to your Blue Shield plan to confirm coverage before you commit. Ro says FEHB members can join Ro Body and access the insurance concierge.
Does PlushCare accept Blue Shield of California?
Yes. PlushCare's published How It Works page states it accepts copays from most Blue Shield of California, Blue Cross Blue Shield, Anthem Blue Cross, Aetna, Humana, and Medicare plans, with most in-network patients paying $30 or less per visit.
Does Shapely accept Blue Shield?
Yes. Shapely's public Blue Cross Blue Shield page states it accepts most PPO plans including Blue Shield, currently in California, Florida, New York, and Texas, with a $49/month membership fee separate from insurance-billed visits.
How long does Blue Shield prior authorization take for a GLP-1?
Blue Shield of California's published timeline is 24 to 72 hours for a standard review. In real-world practice, expect closer to 1 to 14 business days when you factor in collecting documents and back-and-forth with the insurer. The full benefits-verification and prior auth process — including medication shipment — typically takes 2 to 3 weeks total.
What if my Blue Shield plan dropped GLP-1 coverage in 2026?
Three real options: (1) request a formulary exception in writing, (2) re-route to an alternate FDA-approved diagnosis if it fits medically (Zepbound for moderate-to-severe obstructive sleep apnea, Wegovy for cardiovascular disease or MASH), or (3) use cash-pay through Ro or Sesame Care at LillyDirect / NovoCare / TrumpRx-matched pricing. FDA-approved cash-pay options currently start at $149/month for some doses.
Can I use Blue Shield with a compounded GLP-1 provider?
We did not verify any Blue Shield formulary coverage path for compounded GLP-1s. Compounded medications are not FDA-approved as finished drug products, and the compounded telehealth platforms we reviewed all operate cash-pay. So they don't accept Blue Shield in any meaningful way. The FDA issued 30 warning letters to telehealth platforms in March 2026 over misleading compounded GLP-1 marketing.
Is Blue Shield the same as Blue Cross Blue Shield?
Not exactly. Blue Shield of California is its own separate company, distinct from Anthem Blue Cross of California. Nationally, the Blue Cross Blue Shield Association is a federation of 33 independent licensees, and 'Blue Shield' can refer specifically to Blue Shield of California, the BCBS Federal Employee Program, or other regional Blues. Look at the back of your card to confirm which company actually issues your plan.
Does Medicare or Medicaid through Blue Shield cover GLP-1s?
Differently. Medicare Part D has begun covering Wegovy for some beneficiaries with established cardiovascular disease, but coverage for weight-loss alone is still limited. Medi-Cal (California's Medicaid) restricts most GLP-1s to non-weight-loss indications starting January 1, 2026. Telehealth providers like Ro do not coordinate Medicare or Medicaid for GLP-1 coverage; your real path is an in-network local provider.
What's the cheapest GLP-1 path if Blue Shield denies me?
For FDA-approved brand medication: Foundayo at $149/month first month (Lilly launch pricing, verify current terms), Wegovy pill at $149/month for lower doses, Wegovy pen at $199/month introductory then $349/month, and Zepbound vials at $299–$449/month depending on dose. Ro is the cleanest path because their cash-pay prices are matched to LillyDirect, NovoCare, and TrumpRx — the manufacturers' own direct prices, no markup.
Your Next Step
Three paths, depending on where you actually are right now.
If you don't yet know whether Blue Shield will cover your GLP-1 medication
Ro reaches out to Blue Shield on your behalf and sends you back a personalized coverage report. No Ro account required up front. New accounts get a $50 credit.
Check Your Blue Shield GLP-1 Coverage with Ro — Free →If you'd rather pick your own provider and pay $59/month for a fuller telehealth experience
Browse Success by Sesame providers. Read reviews. Pick the obesity-medicine clinician you want. Run a video visit and let them file your prior auth paperwork.
See Success by Sesame Providers from $59/Month →Still not sure which GLP-1 program is right for you?
Take our free 60-second matching quiz.
Find My GLP-1 Path →If you have an Anthem Blue Cross or other Blue Cross plan instead of Blue Shield, see our companion guide: GLP-1 Providers That Accept Anthem.
Last verified: April 30, 2026. Pricing, provider participation, pharmacy benefits, and prior authorization rules can change. Always verify your specific Blue Shield plan and the provider's current insurance acceptance before enrolling. The RX Index is a pricing intelligence and comparison resource for GLP-1 telehealth providers — we are not a healthcare provider, and this guide is not medical advice. Talk to a licensed clinician before starting any prescription medication.
Affiliate disclosure: Some links on this page are affiliate links. The RX Index may earn a commission when readers sign up through those links. The price you pay is the same whether you use our link or go directly.
