GLP-1 Providers That Accept Ambetter in 2026: The Honest, Verified Guide
Published:
By The RX Index Editorial Team · Last verified May 1, 2026
Disclosure: The RX Index earns commissions when readers click certain provider links. Affiliate relationships do not change which providers we feature or how we describe them.
Not sure if Ambetter covers your GLP-1 yet?
Ro contacts your plan and sends a personalized report on whether Wegovy, Zepbound, Ozempic, or Mounjaro may be covered, plus copay estimates. Free checker only; no prescription written.
Bottom Line First
What We Actually Verified for This Guide
Every fact below comes from a primary source we read and dated:
- ✅Ambetter's official policy notice: "GLP-1 Medications: Coverage Exclusions for Weight Loss Treatment," published November 21, 2025 by Ambetter from Arkansas Health & Wellness
- ✅The 2026 Ambetter Formulary (Mississippi, document AMB25-AHS-C-00023-MS, effective January 1, 2026, updated May 2026) — pulled directly from ambetterhealth.com
- ✅Centene Clinical Policy CP.PMN.295 (Wegovy) — including the weight management exclusion language and separate criteria for cardiovascular event prevention and MASH
- ✅Centene Clinical Policy HIM.PA.53 (GLP-1 Receptor Agonists) — including type 2 diabetes criteria and the non-preferred GLP-1 RA criteria that govern Mounjaro
- ✅Ambetter Indiana's 2025 prior authorization statistics — published publicly on ambetter.mhsindiana.com
- ✅Ro's pricing and insurance concierge scope (ro.co/weight-loss/pricing, ro.co/weight-loss/glp1-insurance-checker, ro.co/weight-loss/how-it-works)
- ✅knownwell's state-by-state insurance coverage page (knownwell.co/insurance) confirming Ambetter participation in Dallas/Fort Worth and Atlanta
- ✅Sesame Care's pricing and Costco partnership (sesamecare.com)
- ✅FDA's February 20, 2026 warning letter to MEDVi and FDA's published concerns about unapproved GLP-1 products
- ✅FDA approval letter for Foundayo (orforglipron), dated April 2026
What we did not verify: every state Ambetter formulary, every individual plan’s exact coverage, or whether your specific PA will be approved. Coverage rules vary by state and plan. Always confirm yours before relying on this page.
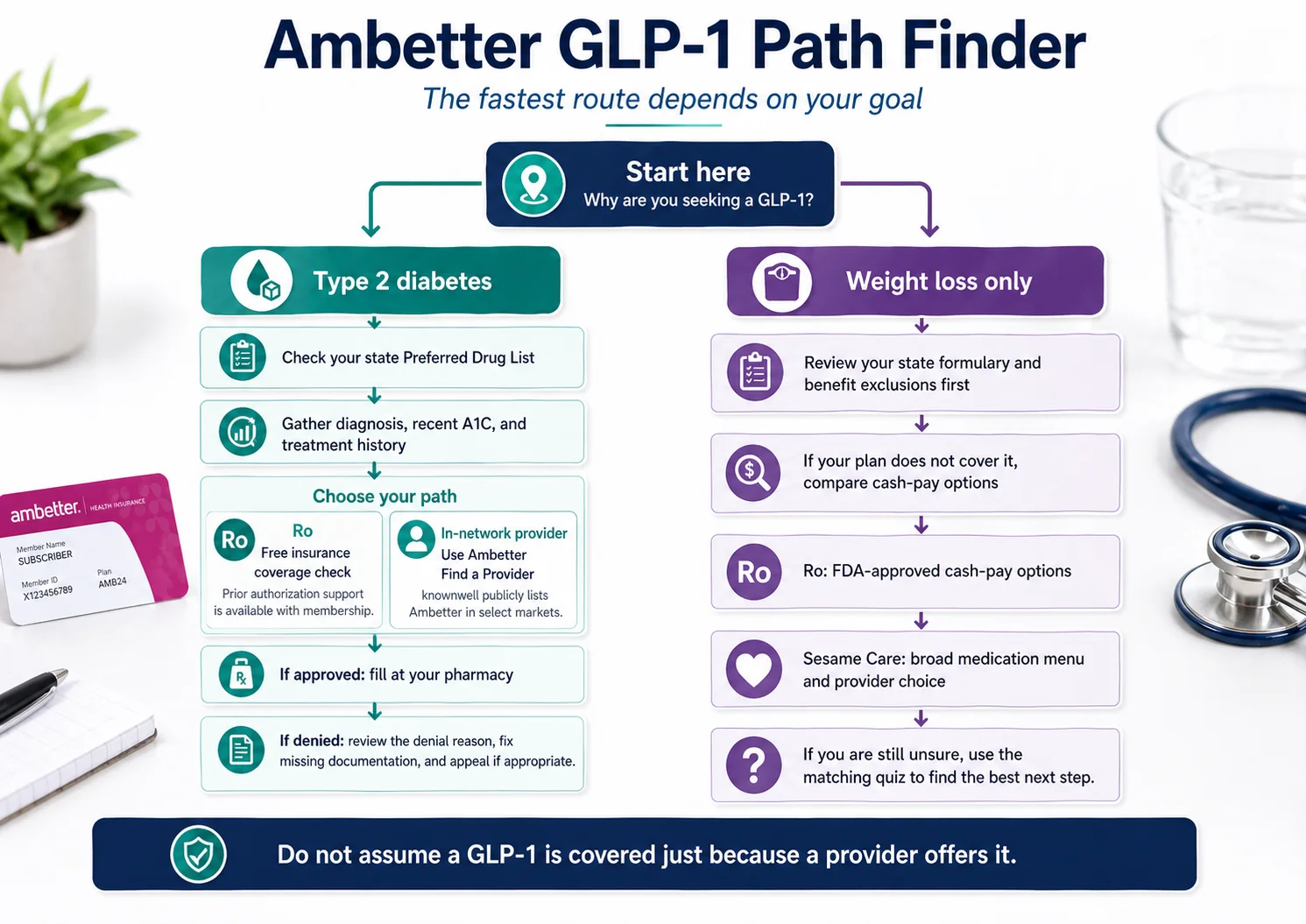
The 30-Second Decision Matrix
| Your situation | Best first move | Why |
|---|---|---|
| Not sure if Ambetter covers your GLP-1 | Ro free coverage check | Ro contacts your plan and sends a real coverage report — no payment to check |
| Want the doctor visit billed to Ambetter | knownwell (Dallas/Fort Worth or Atlanta) or Ambetter Find a Provider | True in-network billing for the visit itself |
| Have type 2 diabetes and want Ozempic, Rybelsus, or Trulicity | Ro for commercial Ambetter plans, or your in-network PCP | These are on the formulary with PA — the path exists |
| Want a GLP-1 only for weight loss | Cash-pay path (Ro for branded; Sesame for choice and Costco pricing) | Ambetter weight-management criteria point to denial |
| Have CV disease, MASH, or sleep apnea | Talk to your prescriber about the indication-specific criteria | Wegovy and Zepbound have separate non-weight-management indications worth pursuing |
| Already got denied | Read the denial letter, fix what's missing, then appeal — or pivot to cash-pay | Many Ambetter denials are documentation problems, not flat refusals |
That’s the whole picture in one table. The rest of this guide explains every line.
Why “GLP-1 Providers That Accept Ambetter” Is the Wrong Question (and the Right One)
“Accept Ambetter” sounds simple, but it splits into two questions that have totally different answers — does the provider bill Ambetter for the visit, and does Ambetter cover the medication they prescribe? The medication is the four-figure problem, not the visit.
Layer 1 — The Visit
Some providers (like knownwell, in certain states) actually bill your visit to Ambetter as in-network medical care. You pay your normal copay or deductible like a regular doctor’s appointment. Other providers (like Ro and Sesame Care) charge a flat membership fee you pay yourself. That fee isn’t billable to insurance — but the membership unlocks the support.
Layer 2 — The Medication
This is the part that costs $1,000+ a month at retail. Ambetter pays for medications based on your plan’s formulary, the diagnosis on the prescription, and whether prior authorization is approved. The provider can help or hurt you here, but the rules belong to Ambetter — not the telehealth company.
Does Ambetter Cover Wegovy, Zepbound, Ozempic, or Mounjaro?
It depends on the medication, the indication, your state’s formulary, and your specific plan. The Mississippi 2026 Ambetter formulary we verified lists Ozempic, Rybelsus, Trulicity, and generic liraglutide for type 2 diabetes — most with quantity limits and prior authorization. Wegovy, Zepbound, Mounjaro, Saxenda, and Foundayo did not appear in that specific state formulary.
Does Ambetter Cover Ozempic?
Yes — for type 2 diabetes with PA
Ozempic (semaglutide injection) is on the Mississippi 2026 Ambetter formulary at Tier 2, with quantity limits and prior authorization required. Ozempic tablets (1.5 mg, 4 mg, 9 mg) are listed separately at Tier 2 with quantity limits and PA. Ambetter's PA criteria require type 2 diabetes documentation. Hoping to get Ozempic for weight loss alone? Expect denial.
Does Ambetter Cover Wegovy?
Generally no for weight loss; possibly yes for CV risk or MASH
Wegovy did not appear in the Mississippi 2026 formulary we verified. The Centene Wegovy policy lists weight management as a benefit exclusion. However, that same policy includes separate criteria for cardiovascular event prevention (adults with established CV disease and overweight/obesity) and MASH. If you have documented CV disease or a MASH diagnosis, this is worth raising with your prescriber.
Does Ambetter Cover Zepbound?
Generally no for weight loss; possibly yes for OSA
Zepbound did not appear in the Mississippi 2026 formulary we verified. Like Wegovy, it would be excluded for weight management on most Ambetter plans. But Zepbound has a separate FDA approval for moderate-to-severe obstructive sleep apnea in adults with obesity. If you have a documented sleep study showing OSA, this is a different conversation. Your prescriber can submit a PA tied to the OSA indication.
Does Ambetter Cover Mounjaro?
In Centene's PA policy as non-preferred for type 2 diabetes
Mounjaro did not appear in the Mississippi 2026 formulary we verified. Don't take that as a national result. Centene's GLP-1 receptor agonist clinical policy (HIM.PA.53) includes Mounjaro under non-preferred type 2 diabetes criteria — coverage is plan- and formulary-specific. A PA submission for diabetes use is possible on plans that include it.
Does Ambetter Cover Rybelsus, Trulicity, and generic liraglutide?
Yes — for type 2 diabetes
The Mississippi 2026 formulary lists Rybelsus (Tier 2, quantity limit, PA required), Trulicity (Tier 2, quantity limit, PA required), and generic liraglutide (Tier 1B, quantity limit — the lowest-tier GLP-1 we verified on the formulary).
Does Ambetter Cover Foundayo?
Not yet on this formulary
Foundayo (orforglipron) was FDA-approved in April 2026 for chronic weight reduction in adults with obesity. It did not appear on the Mississippi 2026 formulary we verified. Available through Ro and Sesame Cash-pay from $149/month.
The Verified Ambetter Formulary in One Table
Numbers below are from the Mississippi 2026 Ambetter formulary specifically. Other state formularies can differ. Always pull your state’s PDL before relying on coverage information.
| Medication / formulation | Indication | Tier | Restrictions | Covered for weight loss? |
|---|---|---|---|---|
| Ozempic (injection, multiple doses) | Type 2 diabetes | Tier 2 | Quantity limit, PA required | No |
| Ozempic tablets (1.5 / 4 / 9 mg) | Type 2 diabetes | Tier 2 | Quantity limit, PA required | No |
| Rybelsus (oral tablet) | Type 2 diabetes | Tier 2 | Quantity limit, PA required | No |
| Trulicity (injection) | Type 2 diabetes | Tier 2 | Quantity limit, PA required | No |
| Liraglutide (generic) | Type 2 diabetes | Tier 1B | Quantity limit | No |
| Wegovy (injection or pill) | Weight management / CV / MASH | Not on this formulary | — | Weight management excluded; CV/MASH have separate criteria |
| Zepbound (pen, KwikPen, vials) | Weight management / OSA | Not on this formulary | — | Weight management excluded; OSA has separate criteria |
| Mounjaro (injection) | Type 2 diabetes | Not on this formulary | — | In Centene PA policy as non-preferred for diabetes |
| Saxenda (injection) | Weight management | Not on this formulary | — | Excluded |
| Foundayo (oral, FDA-approved April 2026) | Weight management | Not on this formulary | — | New medication; not yet on this formulary |
What Ambetter says in plain English
Ambetter from Arkansas published a member notice on November 21, 2025 titled “GLP-1 Medications: Coverage Exclusions for Weight Loss Treatment.” It says directly: “Ambetter does not currently cover GLP-1s when prescribed solely for weight management.” It warns that if you take a GLP-1 for weight loss anyway, “you may be responsible for the full cost out of pocket.” Some providers and pharmacy reps will tell you “it depends on your plan” and “let’s submit and see.” That’s not wrong — but it’s not the most likely outcome for weight-loss-only requests. Ambetter has already told you what they’re going to do. Believe them. Plan accordingly.
Real Numbers from a Real Ambetter Market
Ambetter’s Indiana plan publishes its 2025 prior authorization statistics. This is the most useful number on this entire page — almost every guide on the internet is vague about your real odds. Here is the actual data, cited as published on ambetter.mhsindiana.com:
| Metric | Number | Percent (as published) |
|---|---|---|
| Pharmacy PA requests received | 48,942 | — |
| Fully approved | 30,060 | 54.1% |
| Adverse determinations (denied) | 18,882 | 45.9% |
| Partial approvals | 0 | 0% |
| Average time from submission to response | 0.73 days | — |
The key takeaway
Even taking the most favorable read, somewhere between four and five out of every ten Ambetter Indiana pharmacy PA requests don’t get fully approved on the first pass. The top requested GLP-1 medications were Ozempic, Zepbound, Mounjaro, Wegovy, and Trulicity — five of the seven top medications are GLP-1s.
| Appeal metric | Number | Context |
|---|---|---|
| Total appeals received | 2,044 | Across all categories |
| Appeals fully approved | 782 (~38%) | Best-case for documentation-fixable denials |
| Appeals denied | 1,262 (~62%) | — |
| Average appeal response time | 22.75 days | vs. 0.73 days for initial PA |
| Top reason for denial | Medical Necessity Not Evident | Translation: paperwork didn't make a strong enough case — often fixable |
The response time for an initial PA averaged 0.73 days. The response time for an appeal averaged 22.75 days. If you can get the first PA right, you save three weeks.
The Provider Paths That Actually Work for Ambetter Members
Three providers are worth your attention if you have Ambetter, and each one solves a different problem. Pick the one that matches what you actually need.
Ro — Best for Coverage Checking and Commercial PA Support
Ro doesn’t bill Ambetter for the membership — that’s cash-pay — but Ro’s free coverage checker contacts your Ambetter plan, and Ro’s paid Body membership includes an insurance concierge that submits prior authorization paperwork on your behalf for commercial Ambetter plans. That’s the answer most pages get wrong.
knownwell — Best for True Ambetter In-Network Visits
knownwell is a primary care and weight management clinic with physical locations and nationwide virtual care. Their public insurance page lists the exact Ambetter plans they accept by region.
Verified Ambetter participation as published on knownwell.co/insurance (May 2026):
- Texas / Dallas-Fort Worth area: Centene — Ambetter-TX — Superior HealthPlan (PPO)
- Georgia / Atlanta area: Ambetter (HMO) and Ambetter (EPO)
If you live in those markets, knownwell can bill the visit directly to your Ambetter plan — you might pay only your copay or coinsurance for the appointment itself. Cash-pay backstop: $299 first visit and $149 follow-up visits in most states (Illinois follow-ups are $49).
Where knownwell falls short: it doesn’t have its own pharmacy or compounded drug option, and outside Texas and Atlanta, your Ambetter plan may not be accepted at all. Always check your specific state listing on their site before booking.
Sesame Care — Best for Medication Choice and Costco Pricing
If you want a wide selection of GLP-1 options, the ability to pick your own clinician, and (if you’re a Costco member) a meaningful cash-pay discount on branded GLP-1s, Sesame Care is a strong fit.
Other Paths to Know
- Ambetter’s own provider directory at findaprovider.ambetterhealth.com — the safest route for in-network PCPs who bill your visit to Ambetter the traditional way. Downside: many PCPs aren’t enthusiastic about handling GLP-1 PA paperwork and some submit half-completed forms that get denied for “Medical Necessity Not Evident.”
- PlushCare and Form Health — both work with insurance for some plans. Neither publishes a state-by-state Ambetter participation list as cleanly as knownwell does. Call before booking and ask: “Are you in-network for Ambetter [your plan name] in [your state]?” Get the answers in writing.
- Meto.co — runs a directory page for “Doctors for GLP-1 Therapy Accepting Centene (Ambetter, WellCare).” It’s a directory, not a clinic. Useful for finding actual doctors who participate in Ambetter.
If You Have Type 2 Diabetes: The Fastest Path to Coverage
If you have a confirmed type 2 diabetes diagnosis, Ozempic, Rybelsus, Trulicity, or generic liraglutide is the path with the highest approval odds on Ambetter. Ambetter Indiana’s average pharmacy PA response time in 2025 was 0.73 days. Three steps.
Step 1: Get your diagnosis paperwork in order
Ambetter’s PA team needs to see specific things. Have your records ready before your appointment:
- ☐Confirmed type 2 diabetes diagnosis (your doctor will use ICD-10 code E11.x)
- ☐Most recent A1C result — if you don't have a recent A1C, ask your provider to order one before submitting a PA
- ☐Weight history and current BMI
- ☐List of diabetes medications you've already tried — most plans want to see metformin first (step therapy)
- ☐Confirmation that you don't have a personal or family history of medullary thyroid carcinoma or MEN 2
Step 2: Pick who submits the PA
Step 3: Track the response and confirm coverage
Ambetter Indiana’s 2025 average pharmacy PA response was 0.73 days. The Mississippi formulary commits to 24 hours for urgent requests and 72 hours for non-urgent unless state law is faster. If approved, your cost depends on the medication’s tier, your deductible, and your plan’s pharmacy benefit design. If denied, read the denial letter carefully.
If Your Goal Is Weight Loss Only: The Realistic Cash-Pay Path
For weight-loss-only use, the Ambetter and Centene materials we reviewed point to denial. If you walked into this with no diabetes, no major comorbidity, the Ambetter materials say no. The only realistic insurance paths here are a different covered indication (CV disease, MASH, OSA, or T2D — and you can’t fake those) or going cash-pay.
Here’s the better news: branded GLP-1 cash-pay prices in 2026 are dramatically lower than two years ago. Drug companies started competing seriously, and self-pay programs through the manufacturers cut prices roughly in half from 2024 levels.
Important safety information
GLP-1 medications are not for everyone. Wegovy, Zepbound, Ozempic, Mounjaro, and similar GLP-1s carry boxed warnings or warnings about thyroid C-cell tumors and should not be used by people with a personal or family history of medullary thyroid carcinoma or MEN 2. FDA-listed warnings include pancreatitis, gallbladder problems, low blood sugar, acute kidney injury, severe allergic reactions, diabetic retinopathy, increased heart rate, and reports of suicidal behavior or thinking. Zepbound’s OSA approval materials add a warning for pulmonary aspiration risk during anesthesia or deep sedation. Talk to your prescribing provider about your full medical history before starting any GLP-1 medication.
| Medication | Starting cash price | Notes |
|---|---|---|
| Wegovy pill (oral semaglutide, lower doses) | From $149/month | Through Ro and Sesame promo pricing reflected on their pages |
| Foundayo (oral orforglipron) | From $149/month | FDA-approved April 2026; available through Ro |
| Wegovy injection | $199/month for first 2 fills, then $349/month | NovoCare manufacturer self-pay; Sesame Costco price is $349/mo from day one for Costco members |
| Zepbound vials (you load the syringe yourself) | From $299/month for 2.5 mg dose | LillyDirect self-pay; available through Ro/Sesame |
| Zepbound KwikPen (cash-pay) | Starts at $299 first month; later doses $399–$449 | Verify current Ro/Sesame/LillyDirect pricing before you commit |
| Zepbound pre-filled pen at retail pharmacy | Often $1,000+/month at standard retail | Manufacturer-direct cash-pay options can be much lower — don't pay retail without checking |
| Compounded semaglutide or tirzepatide | Pricing varies by provider | Separate regulatory category — not FDA-approved; see compounded section below |
Why “off-label Ozempic for weight loss” doesn’t save you money on Ambetter
A clinician may prescribe Ozempic off-label when clinically appropriate — that’s a normal part of medicine. But Ambetter’s PA team needs to see a type 2 diabetes diagnosis to approve Ozempic. If your prescription is submitted with a weight-loss-only indication, expect denial. So an off-label Ozempic prescription for weight loss generally means full cash-pay, even though you “have insurance.”
How to Appeal an Ambetter GLP-1 Denial
A denial isn’t always the end. About 38% of Ambetter Indiana pharmacy appeals were approved in the most recent published data. The trick is figuring out which kind of denial you have.
The five reasons Ambetter denies a GLP-1 PA
| Denial reason | What it means | Fixable? |
|---|---|---|
| Medical Necessity Not Evident | Top reason per Indiana data — paperwork didn't strongly establish why you need this drug | Often yes — strengthen the documentation |
| Wrong diagnosis on the prescription | You can't get Ozempic covered with a weight-loss-only indication; you can with a T2D indication. Sometimes a prescriber writes the wrong code. | Yes — prescriber resubmits with correct code |
| Missing step therapy documentation | Plan requires you to try metformin first and there's no record of it in the submission | Yes — document metformin trial and resubmit |
| Drug not on formulary | Wegovy or Zepbound for weight management — structural reason that usually can't be appealed unless you have CV disease, MASH, or OSA documentation | Hard — pursue indication pathway or cash-pay |
| Submission errors | PA forms with missing fields, wrong NPI numbers, or wrong member IDs — boring but common | Yes — resubmit with correct information |
What to do, in order
- 1Get the denial letter and read it carefully. It will name the specific reason, the appeal deadline, and the address or fax number for appeals. The deadline matters — miss it and you lose your internal appeal rights.
- 2Decide if it’s worth appealing. Documentation problem → fix it and appeal. Wrong diagnosis → ask prescriber to resubmit, not appeal. Plan exclusion (weight-loss-only GLP-1) → very tough; start cash-pay in parallel. Step therapy not met → fix documentation and resubmit.
- 3Build the appeal packet: the denial letter (reference number), a letter of medical necessity from your prescriber, recent labs (A1C, lipid panel, relevant results), comorbidity documentation, prior medication trial records, and your prescriber’s contact info.
- 4Ask whether peer-to-peer review is available. This is when your prescribing doctor talks directly to an Ambetter medical director by phone. Some plans offer it. Ask.
- 5External review if internal appeal fails. Federal rules generally give ACA marketplace plan members the right to ask an independent third party to review the decision. Your specific deadlines and process are in your plan’s Evidence of Coverage and the second denial letter.
State-by-State Notes: Ambetter Is Not the Same Everywhere
Ambetter operates in many states under different Centene subsidiaries, and the formulary, in-network telehealth options, and PA criteria can differ. Always pull your specific state’s Preferred Drug List from ambetterhealth.com before relying on coverage information.
| State / region | What we verified | What you should do |
|---|---|---|
| Texas — Dallas/Fort Worth area | knownwell is in-network with Centene — Ambetter-TX — Superior HealthPlan (PPO) | If your plan matches, knownwell can bill Ambetter for visits |
| Georgia — Atlanta area | knownwell is in-network with Ambetter (HMO) and Ambetter (EPO) | Confirm your specific plan letter (HMO vs EPO) before booking |
| Indiana (Coordinated Care Corporation) | Publishes 2025 PA stats; top requested medications include Ozempic, Zepbound, Mounjaro, Wegovy, and Trulicity | Use the published criteria as your benchmark for what to expect |
| Arkansas | Ambetter from AR Health & Wellness publicly stated GLP-1 weight-loss exclusion (Nov 2025) | Don't expect weight-loss coverage; pursue diabetes path or cash-pay |
| Mississippi | 2026 Ambetter formulary AMB25-AHS-C-00023-MS lists Ozempic, Rybelsus, Trulicity, and generic liraglutide (all PA except liraglutide with QL) | Use this as your reference if you're in MS; verify your plan |
| Other states | Each Ambetter state subsidiary publishes its own PDL | Pull your state's formulary at ambetterhealth.com/select-your-state-enroll/coverage-area.html |
How to verify your specific Ambetter state and plan in under five minutes:
- Go to ambetterhealth.com
- Click your state from the coverage map
- Open the Pharmacy Resources or Drug Coverage page
- Download the current Preferred Drug List PDF
- Use Ctrl+F (Cmd+F on Mac) to search for “Ozempic,” “Wegovy,” “Zepbound,” “Mounjaro,” “Trulicity,” and “liraglutide”
- Note the tier and any restrictions (PA, QL for quantity limit, ST for step therapy)
That five-minute exercise will tell you more about your real coverage than any blog post.
A Note on Compounded GLP-1 Telehealth
Compounded GLP-1s are a separate regulatory category. Here’s what they are and aren’t.
What they are:
Medications prepared by a licensed compounding pharmacy under sections 503A or 503B of federal drug law, based on a prescription from a licensed prescriber.
What they aren’t:
FDA-approved drug products. The FDA has not reviewed compounded GLP-1s for safety or effectiveness the way it reviewed Wegovy, Zepbound, Ozempic, or Mounjaro.
The FDA issued a warning letter to MEDVi on February 20, 2026 for marketing claims like “Same active ingredient as Wegovy® and Ozempic®” — the agency views those claims as misbranding because they imply FDA approval the products don’t have.
The FDA has also warned that some compounded products marketed as “semaglutide” actually contain semaglutide salt forms (such as semaglutide sodium or semaglutide acetate) that are different active ingredients than what’s in the FDA-approved Wegovy and Ozempic.
For Ambetter members: Ambetter does not cover compounded GLP-1s. Compounded telehealth platforms are cash-pay only. Compounded GLP-1 spending generally does not count toward your Ambetter deductible.
We don’t feature any compounded provider as a winner on this page — partly because of the regulatory environment, partly because this guide is written for Ambetter members where the question is real insurance and FDA-approved branded medication. See our compounded vs. FDA-approved GLP-1 comparison if you’ve decided that path anyway.
What Real Ambetter Members Run Into
The most common Ambetter member experience with GLP-1s is a denial or a long PA delay — which is what the published Indiana data confirms. Members who use a provider with insurance concierge support consistently report a smoother experience than those who navigate the PA process alone.
“I was not expecting insurance help. Usually patients are their own advocate, so I was thrilled to not have to fight for my coverage.”
— Hannah, Ro member (paid testimonial; published on ro.co)
Disclosure: Ro members were compensated for this testimonial. The experience it describes — not having to fight your insurance plan alone — matches what Ambetter members consistently say is the most stressful part. Individual results vary. Coverage outcomes depend on your specific plan, diagnosis, and submitted documentation. Testimonials do not constitute medical advice.
If you’d rather hear from members who fought the PA process themselves, the Ambetter Indiana data is the most useful proxy: the published 2025 stats show somewhere between 4 and 5 in 10 Ambetter Indiana pharmacy PA requests didn’t get fully approved on the first pass. That’s why outsourcing the PA paperwork to a provider that handles it routinely tends to be the highest-leverage move.
Frequently Asked Questions about GLP-1 Providers That Accept Ambetter
1. Are there GLP-1 providers that accept Ambetter?
Yes, but the question splits into two. For visit billing, knownwell accepts Ambetter in Dallas/Fort Worth and the Atlanta area, and Ambetter's own provider directory lists in-network PCPs and specialists nationwide. For medication coverage support, Ro's insurance concierge handles prior authorization with commercial Ambetter plans, and Sesame Care providers will assist with PA paperwork. No single provider does all three perfectly.
2. Does Ambetter cover Wegovy?
Generally no for weight-loss-only use — the Centene Wegovy policy we reviewed lists weight management as a benefit exclusion, and Wegovy did not appear on the Mississippi 2026 formulary we verified. The same policy includes separate criteria for cardiovascular event prevention and MASH (metabolic dysfunction-associated steatohepatitis), so the answer for those indications depends on your diagnosis, documentation, and plan rules.
3. Will Ambetter cover Wegovy if I have cardiovascular disease or MASH?
Possibly, on appeal. Wegovy has FDA approvals for cardiovascular event reduction in adults with established CV disease and overweight or obesity, and for MASH. The Centene Wegovy policy includes separate criteria for those indications. An Ambetter plan that excludes Wegovy for weight management may still consider an exception for a different covered indication when documentation is strong. Talk to your prescriber about the specific indication being submitted.
4. Does Ambetter cover Ozempic?
Yes — for type 2 diabetes only, with prior authorization. Ozempic injections and Ozempic tablets are both on Tier 2 of the Mississippi 2026 formulary we verified, with quantity limits and prior authorization required. Ambetter will not cover Ozempic prescribed off-label for weight loss; the PA criteria require type 2 diabetes documentation.
5. Does Ambetter cover Zepbound?
Zepbound did not appear on the Mississippi 2026 formulary we verified, and Zepbound for weight management is not on the path most Ambetter plans cover. Zepbound has a separate FDA approval for moderate-to-severe obstructive sleep apnea in adults with obesity — so if you have a documented sleep study, that's a different conversation. Ask your prescriber about the OSA-specific criteria.
6. Will Ambetter cover Zepbound if I have obstructive sleep apnea?
Possibly. Zepbound's OSA approval is real and the criteria are policy-based, not a flat exclusion. Coverage still depends on your documented sleep study, your plan's specific rules, and prior authorization. Bring a recent sleep study to your prescriber and ask them to submit a PA tied to the OSA indication.
7. Does Ambetter cover Mounjaro?
Mounjaro did not appear on the Mississippi 2026 formulary we verified. Don't take that as a national result — Centene's GLP-1 PA policy includes Mounjaro under non-preferred type 2 diabetes criteria. Coverage is plan- and formulary-specific. If you're seeking Mounjaro for type 2 diabetes, ask your prescriber to check your specific state plan and submit a prior authorization. Off-label weight-loss requests will be denied under the criteria we reviewed.
8. What is prior authorization, and why does Ambetter require it for GLP-1s?
Prior authorization is when your insurance plan requires your prescriber to send clinical paperwork before the prescription will be covered. Ambetter requires PA for GLP-1s because the medications are expensive and the plan wants to confirm the use matches its coverage criteria. The Mississippi formulary commits to 24 hours for urgent requests and 72 hours for non-urgent requests unless state law is faster.
9. What documents do I need for an Ambetter GLP-1 prior authorization?
For a type 2 diabetes-indicated GLP-1: confirmed diagnosis with ICD-10 code E11.x, most recent A1C result, BMI and weight history, documented prior diabetes treatments (commonly metformin first), and confirmation that contraindications like medullary thyroid carcinoma history or MEN 2 have been ruled out.
10. Can a telehealth provider submit prior authorization to Ambetter?
Yes. Ro's insurance concierge submits PAs for commercial Ambetter plans. Sesame Care providers will submit PA paperwork as part of their subscription. Some PCPs through other telehealth platforms also handle PA paperwork — confirm before booking.
11. What if Ambetter says the drug is covered but the pharmacy says denied?
This usually means the PA was not completed, the criteria were not met, or the prescription was written with the wrong indication. Call Ambetter's pharmacy benefits number on the back of your card with your prescription number and ask exactly what step is missing. Ask them to email or fax the PA criteria so you can give them to your prescriber.
12. Will cash-pay GLP-1 spending count toward my Ambetter deductible?
Generally no. If Ambetter isn't paying any portion, it usually doesn't count toward your deductible or out-of-pocket maximum. Some plans will count expenses if a service is denied as 'non-covered' with specific reasoning, but this is rare for elective medication choices. Read your plan documents or ask Ambetter directly.
13. Can I use HSA or FSA funds if Ambetter denies my GLP-1?
It depends. IRS guidance generally treats weight-loss programs as reimbursable from HSA/FSA only when treating a specific disease diagnosed by a physician — for example, obesity, diabetes, hypertension, or heart disease. Ask your HSA/FSA administrator what documentation they require before you spend the money.
14. Is Ro the same as having Ambetter cover my GLP-1?
No. Ro's Body membership is cash-pay (Ambetter doesn't pay for it), and the medication is billed separately. What Ro adds is an insurance concierge that fights for coverage on the medication side. If Ambetter approves your GLP-1 prescription with Ro's help, you pay your normal pharmacy copay or coinsurance for the drug — but you also pay Ro's membership fee on top.
15. Does knownwell accept all Ambetter plans nationwide?
No. As of May 2026, knownwell's public insurance page lists Ambetter network participation in Texas (Centene–Ambetter-TX–Superior HealthPlan PPO) and the Atlanta area (Ambetter HMO and EPO). For other states, knownwell may accept other major insurers but not Ambetter specifically. Check your state on their insurance page before booking.
16. What if my doctor refuses to submit a prior authorization?
You have three options: find a different in-network provider on Ambetter who will submit; use Ro's insurance concierge or a Sesame Care provider to handle the paperwork; or ask your current doctor if there's a specific clinical issue you can address. Don't argue endlessly with a doctor who won't help — go to a provider who routinely does this work.
17. How often will Ambetter make me renew a GLP-1 prior authorization?
Renewal timing depends on the medication, indication, and policy. The Centene policies we reviewed include both 6-month and 12-month approval durations depending on the request type. Your prescriber will typically need to document continued medical necessity at renewal — current A1C or other relevant labs, current weight, ongoing tolerance, and continued treatment plan.
18. Are compounded GLP-1 medications the same as Wegovy or Zepbound?
No. Compounded GLP-1s are not FDA-approved drug products. They are prepared by compounding pharmacies under specific federal rules and represent a separate regulatory category from FDA-approved branded medications. The FDA has issued warning letters to compounded GLP-1 marketers for claims implying equivalence to FDA-approved drugs, and has separately warned that some compounded products marketed as 'semaglutide' actually contain semaglutide salt forms that are different active ingredients than what's in Wegovy or Ozempic.
19. If I qualify for Ozempic through diabetes, can I just lose weight on it?
Many people experience weight loss on Ozempic prescribed for diabetes. The PA was approved based on your diabetes management, and continued coverage depends on your prescriber documenting that the medication is helping with that. It's not a workaround for weight-loss-only use; it's a legitimate diabetes medication that may have weight loss as a side benefit when prescribed appropriately.
20. What's the fastest way to check my Ambetter GLP-1 coverage?
Run Ro's free GLP-1 Insurance Coverage Checker. Ro contacts your plan and sends a personalized report on which GLP-1s may be covered, copay estimates, and whether prior authorization is required. The free check doesn't write a prescription or submit a treatment request, and there's no obligation to join Ro's program afterward.
How We Built This Guide and How Often We Update It
We’re The RX Index — a pricing intelligence and comparison resource for GLP-1 telehealth providers. We built this guide by reviewing Ambetter’s pharmacy program materials, the 2026 state formulary PDFs, Centene’s clinical policies (CP.PMN.295 for Wegovy and HIM.PA.53 for the GLP-1 receptor agonist class), the Ambetter Indiana published PA statistics, FDA approval letters and warning letters, and the public insurance pages of every telehealth provider mentioned.
- Ro pricing and insurance concierge scope: monthly
- Sesame Care pricing and Costco partnership: monthly
- knownwell state and Ambetter network listings: monthly
- Ambetter state formularies: quarterly
- Centene clinical policies: quarterly, or immediately on revision
- Ambetter PA statistics: quarterly when new data is published
- FDA compounded GLP-1 actions and warning letters: monthly
Affiliate disclosure: The RX Index earns commissions when readers click certain provider links and complete actions like signing up for a coverage check or membership. Affiliate relationships do not change which providers we feature or how we describe them.
Still Not Sure Which Path Is Right for You?
Ambetter coverage is plan-specific, state-specific, diagnosis-specific, and constantly changing. Take our free 60-second GLP-1 matching quiz. We’ll ask about your Ambetter plan, your state, your goal, and whether you’ve already been denied — then route you to the most realistic next step with a personalized action plan.
Take Our Free 60-Second GLP-1 Matching Quiz
Coverage check, in-network provider, PA help, appeal pathway, or cash-pay alternative — we’ll route you to the right move. No spam. No obligation.
Find My GLP-1 Path →Related Guides
- Best GLP-1 Providers That Accept Insurance
- GLP-1 Providers That Accept Aetna
- GLP-1 Providers That Accept Cigna
- GLP-1 Providers That Accept Anthem
- GLP-1 Providers That Accept UnitedHealthcare
- GLP-1 Providers That Accept Oscar
- GLP-1 Providers That Accept Molina
- Does Ro Accept Insurance for GLP-1?
- Sesame Care Reviews
- Compounded vs. FDA-Approved GLP-1s