GLP-1 Providers That Accept Molina: 2026 Paths [Verified]
Published:
By The RX Index Editorial Team · Next scheduled verification: July 30, 2026
Disclosure: Some links on this page are affiliate links. We may earn a commission if you start a program through them, at no extra cost to you. We listed Molina’s own in-network path first because for most Molina Medicaid members, that’s the path that actually uses your benefits.
The Honest Answer in One Paragraph
The honest answer for GLP-1 providers that accept Molina is this: most online GLP-1 programs do not bill Molina for the visit, and whether your medication gets covered depends on your Molina plan type, state, formulary, and prior authorization. The strongest covered path for Molina Medicaid members is usually an in-network Molina doctor plus a Molina pharmacy, because most online programs are cash-pay memberships that explicitly cannot coordinate coverage with government insurance. If your Molina plan excludes weight-loss GLP-1s — which is most Molina Medicaid plans in 2026 — the fastest realistic route to FDA-approved medication is the cash-pay path through NovoCare (Wegovy oral at $149/month) or LillyDirect (Zepbound at $299–$449/month). For Molina Marketplace and some Medicare Complete plans, a strong prior-authorization workflow (Ro for Marketplace, in-network specialist for Medicaid) changes the math.
What We Actually Verified for This Page
We don’t ask you to take our word for any of this. Every claim below was checked against a primary source on April 30, 2026:
- KFF Medicaid GLP-1 coverage tracker and Pew Research January 2026 update on state Medicaid GLP-1 obesity coverage
- Molina state Medicaid Preferred Drug Lists and coverage policy documents (verified in WA, MI, IL, KY, TX, VA; remaining states marked for direct verification)
- CMS Medicare GLP-1 Bridge FAQ (April 6, 2026 update)
- Ro’s GLP-1 Insurance Coverage Checker, insurance language, and pricing pages
- Sesame Care’s Success by Sesame pricing, medication options, and stated cash prices
- Form Health’s published insurance and Medicaid policy
- Teladoc’s GLP-1 program eligibility statement
- MD Live’s anti-obesity medication policy and state exclusions
- LillyDirect Zepbound Self-Pay Journey terms (including the 45-day refill condition)
- NovoCare Pharmacy Wegovy pricing and savings program terms
- FDA guidance on unapproved/compounded GLP-1 drugs
- FDA Wegovy MASH approval (2025) and Foundayo (orforglipron) approval
State formularies and provider policies change quarterly. The “Last verified” date at the top of this page tells you exactly when it was last checked.
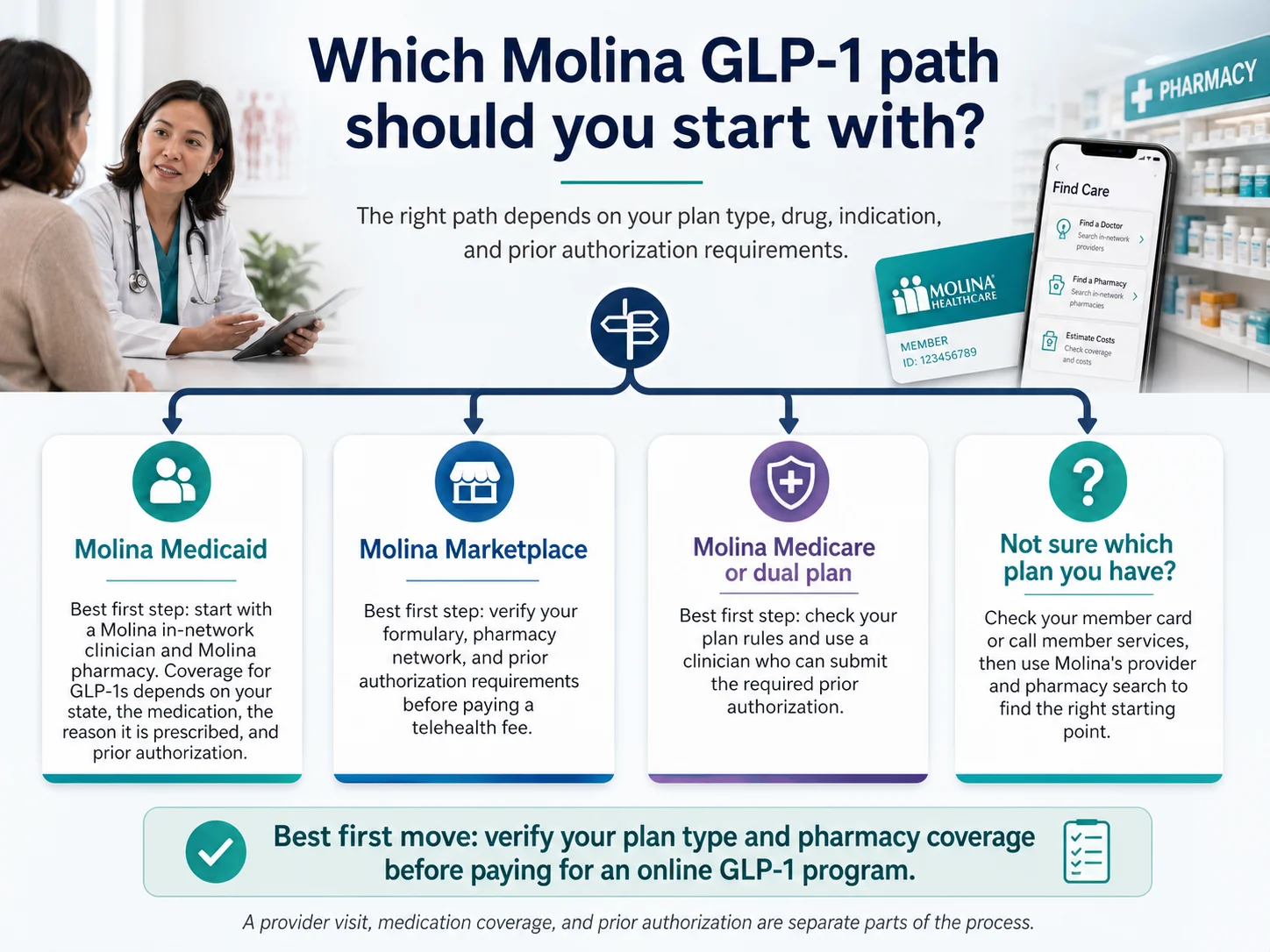
Quick Answer: Which Path Should You Start With?
The path that works for you depends on your Molina plan type and state. Here’s the 30-second answer:
| Your Molina situation | Best first path | Will it use Molina? |
|---|---|---|
| Molina Medicaid in a state that excludes weight-loss GLP-1s (most states in 2026) | Cash-pay through LillyDirect, NovoCare, Ro, or Sesame | No — Molina isn't an option for the medication |
| Molina Medicaid in a state that covers GLP-1s for obesity (per KFF/Pew Jan 2026 data) | In-network Molina doctor + Molina pharmacy | Yes — your Medicaid benefits apply |
| Molina Marketplace (commercial-style ACA plan) | Ro's free coverage checker, then PA filing | Yes, with prior authorization |
| Molina Medicare Complete or Senior Whole Health | Wait for the Medicare GLP-1 Bridge ($50/mo, starts July 1, 2026) | Yes, if you meet eligibility and PA criteria |
| You qualify for an indication pathway (T2D, established CV disease, OSA, MASH) | Standard Molina coverage paths apply | Often yes |
| You were already denied | Read the denial letter, fix what's fixable, or move to cash-pay | Maybe — see denial section |
| You don't know what Molina plan you have | Take our quiz — we identify it in 60 seconds | Depends on plan |
The Damaging Admission We’re Going to Get Out of the Way
We’re an affiliate site. We earn commissions when readers start programs through some of the providers on this page. So you might expect us to push you toward the highest-paying telehealth provider regardless of fit.
We’re not going to do that, and here’s why.
For most Molina Medicaid members in 2026, the best path to a covered GLP-1 isn’t a telehealth membership. It’s an in-network Molina doctor. That doctor doesn’t pay us a commission. We listed them first anyway because if you have Molina Medicaid in a state that covers GLP-1s for obesity, an in-network doctor is the only path that actually uses your Medicaid benefits. Telehealth memberships can’t bill Medicaid for visits, and most explicitly say they cannot coordinate coverage with government insurance plans.
Where the affiliate path makes sense honestly: If you have Molina Marketplace or your Molina Medicaid plan flatly excludes GLP-1s for weight loss (most states), then Ro and Sesame become legitimately useful — Ro for its free coverage checker and PA-filing concierge on commercial plans, Sesame for provider choice and brand-name options. Those are real value-adds, not just affiliate plays. We tell you which bucket you’re in below.
Do GLP-1 Providers That Accept Molina Actually Exist?
Yes — but “accepts Molina” means four different things, and you need different ones depending on what you’re trying to do. Most pages on this topic blur these together, which is why people end up paying telehealth fees and still owing $1,000 at the pharmacy.

Visit billed to Molina
Your telehealth or doctor's office runs the appointment through Molina, and you pay your standard copay (often $0 for Medicaid). Rare in GLP-1 telehealth — Form Health, knownwell, and PlushCare bill some commercial plans, but Form Health does not accept Medicaid for program costs.
Medication covered through Molina
Your Molina plan's drug list covers your GLP-1, and you pay your copay tier. Subject to prior authorization in nearly all cases. This is what most people actually want.
Provider files Molina prior authorization
Almost every Molina-covered GLP-1 requires PA. A strong provider has a workflow for this. Ro's insurance concierge handles this for eligible commercial plans. In-network Molina doctors do this routinely.
Works with Molina government plans
Different from commercial Marketplace. Most consumer telehealth services explicitly limit their PA workflow to commercial plans and cannot coordinate government-plan coverage (Medicaid, Medicare Complete, dual).
First, Which Molina Plan Do You Actually Have?
Molina Healthcare runs three different lines of business: Medicaid, Marketplace, and Medicare Complete. They cover GLP-1s very differently, and most members don’t know which one they have.
Look at your Molina card right now
- State Medicaid name on the card (Apple Health, Healthy Michigan, Passport, MississippiCAN, MMA, STAR, etc.) → You have Molina Medicaid
- “Marketplace” or “Exchange” on the card → You have Molina Marketplace
- “Medicare Complete,” “Part D,” “MAPD,” “Senior Whole Health,” or “Dual Options” on the card → You have Molina Medicare Complete or a dual-eligible plan
- You can’t tell → Call the member services number on the back: “Am I on Medicaid, Marketplace, or Medicare with Molina?” One question, 30 seconds, saves hours.
Molina Medicaid — most restrictive in 2026
This is Molina managing your state Medicaid benefits. Coverage is governed by your state’s Medicaid Preferred Drug List plus Molina’s coverage policy. Federal Medicaid law (Social Security Act §1927) lets states exclude weight-loss medications, and most states do. According to KFF’s tracker (last updated January 2026), only 13 state Medicaid programs cover GLP-1s for obesity treatment under fee-for-service. Even in those states, prior authorization, step therapy, and quantity limits apply.
Molina Marketplace — broadest GLP-1 path
These are commercial-style ACA plans bought through healthcare.gov or your state exchange. Coverage of weight-loss GLP-1s exists on most commercial-style formularies with prior authorization, step therapy, and quantity limits. Worth knowing: CVS Caremark administers some Molina Marketplace plans and removed Zepbound from several standard formularies on July 1, 2025 — verify your specific plan. Ro can run a free coverage check and file your prior authorization for eligible commercial plans.
Molina Medicare Complete — changing on July 1, 2026
These are Medicare Advantage Part D plans. Until July 1, 2026, Medicare did not cover GLP-1s for weight loss alone — only for type 2 diabetes, certain cardiovascular indications, or sleep apnea. Starting July 1, 2026, eligible Medicare beneficiaries can access Wegovy (injection and oral), Zepbound KwikPen, and Foundayo through the Medicare GLP-1 Bridge at a $50/month flat copay. Bridge eligibility is not automatic — you must be enrolled in an eligible Part D plan type and meet CMS clinical criteria submitted through the Bridge’s central processor (not consumer telehealth).
Does Molina Cover GLP-1 Medications?
The answer depends on your plan type, your state, and what you’re using the GLP-1 for. Coverage for diabetes (Ozempic, Mounjaro) is broad. Coverage for weight loss (Wegovy, Zepbound, Foundayo) is heavily restricted, especially on Medicaid.
| Indication | Molina Medicaid | Molina Marketplace | Molina Medicare Complete |
|---|---|---|---|
| Type 2 diabetes (Ozempic, Mounjaro, Rybelsus) | Usually covered with PA | Covered with PA | Covered with PA |
| Weight loss only (Wegovy, Zepbound, Foundayo, Saxenda) | Excluded in most states (13 covered per KFF) | Usually covered with PA + step therapy + QL | Bridge only — $50/month starting July 1, 2026 |
| Cardiovascular risk reduction (Wegovy CV) | Separately covered with documented CV disease + obesity | Covered with PA | Covered with PA (Tier 3+) |
| Sleep apnea (Zepbound OSA) | Separately covered with documented moderate-severe OSA + obesity | Covered with PA | Covered with PA |
| MASH (Wegovy injection) | Coverage being added — verify PDL | Coverage being added — verify formulary | PA required |
Coverage by Specific GLP-1 Medication
Does Molina Cover Wegovy?
Maybe — depends on your plan type and state. Molina Marketplace plans generally cover Wegovy with PA + step therapy. Molina Medicaid covers Wegovy for weight loss only in states with Medicaid GLP-1 obesity coverage. Molina Medicare Complete will cover Wegovy via the Medicare GLP-1 Bridge starting July 1, 2026, at $50/month for eligible members.
Cash-pay through NovoCare: $149/month for Wegovy oral pill (1.5mg and 4mg; 4mg offer expires August 31, 2026, then $199/month). Wegovy pen: $199/month for the first two fills on 0.25mg and 0.5mg (eligible new patients, through June 30, 2026), then $349/month. Wegovy HD 7.2mg: $399/month.
Does Molina Cover Zepbound?
Coverage is tightening. CVS Caremark — which administers some Molina commercial plans — removed Zepbound from its Standard Control, Advanced Control, and Value formularies on July 1, 2025, with Wegovy now preferred. Molina Medicaid coverage of Zepbound for weight loss varies by state. Only the Zepbound KwikPen format is eligible through the Medicare GLP-1 Bridge starting July 2026.
Cash-pay through LillyDirect: $299/month for 2.5mg, $399/month for 5mg, $449/month for 7.5mg–15mg if you meet the 45-day refill requirement. Regular pricing (without offer): $499 for 7.5mg and $699 for 10mg, 12.5mg, and 15mg.
Does Molina Cover Ozempic for weight loss?
No. Ozempic is FDA-approved for type 2 diabetes only. Molina covers Ozempic only for documented T2D with PA. Off-label weight-loss prescriptions are denied. The FDA-approved semaglutide for weight loss is Wegovy.
Does Molina Cover Mounjaro for weight loss?
No. Mounjaro is FDA-approved for type 2 diabetes. Molina covers it for documented T2D with PA, not for off-label weight loss. The FDA-approved tirzepatide for weight loss is Zepbound.
Does Molina Cover Foundayo?
Foundayo (orforglipron) is FDA-approved for chronic weight reduction in adults with obesity, or overweight with at least one weight-related comorbidity. CMS has confirmed Foundayo is eligible under the Medicare GLP-1 Bridge starting July 1, 2026. Molina formulary inclusion is being added on a plan-by-plan basis — verify your specific Marketplace formulary, and don't assume Medicaid coverage in states that exclude weight-loss medications.
Does Molina Cover Rybelsus?
Yes for type 2 diabetes. Rybelsus is an oral semaglutide tablet FDA-approved for T2D. Molina covers it for documented diabetes with PA. Not covered for off-label weight loss.
Does Molina Cover Saxenda?
Same answer as Wegovy — depends on your plan and state. Saxenda (liraglutide) is FDA-approved for chronic weight management. It's covered on a small number of state Medicaid plans, broader on Marketplace, and not eligible under the Medicare GLP-1 Bridge.
The Provider Path Matrix: Who Actually Works with Molina
Below is every realistic provider path, compared across what matters: do they bill Molina for visits, do they file Molina PA, which plan types they handle, and what they charge.
| Provider path | Bills Molina for visit | Files Molina PA | Medicaid | Marketplace | Medicare Complete | Cash-pay backup |
|---|---|---|---|---|---|---|
| In-network Molina doctor (PCP, endo, obesity medicine) | Yes | Yes (best PA route) | Yes | Yes | Yes | N/A |
| Zocdoc filtered for Molina | Provider-dependent | Provider-dependent | Verify | Verify | Verify | N/A |
| Teladoc (if your plan includes it) | When included as benefit | Eligible Weight Mgmt or Diabetes Prevention only | Some plans | Some plans | Some plans | N/A |
| MD Live (if your plan includes it) | When included | Routine Primary Care only; excluded in FL, LA, MS, NJ | Some plans | Some plans | Some plans | N/A |
| Ro | No (cash-pay membership) | Yes — eligible commercial coverage | No (cannot coordinate govt plans) | Yes | No (Bridge uses CMS central processor) | Zepbound $299–$449; Wegovy oral $149+ |
| Sesame Care — Success by Sesame | No (cash-pay membership) | Selected providers may file PA — verify before booking | Verify | Verify | Verify | LillyDirect & NovoCare cash prices |
| Form Health | Yes for major private insurance and Medicare | Yes | No — does not accept Medicaid for program costs | Verify | Verify | Not primary |
| knownwell | In-network with many plans | Yes | Verify | Verify | Verify | Cash-pay options |
| PlushCare | Aetna/BCBS/Anthem/Humana/Medicare confirmed | Yes | Verify | Verify | Verify for visits | LillyDirect referenced |
| MEDVi | No (cash-pay only) | No | No | No | No | Yes — cash path (compounded + branded) |
| Eden | No (cash-pay only) | No | No | No | No | Yes — FDA-approved focus |
| SHED Rx | No (cash-pay only) | No | No | No | No | Yes — compounded; not FDA-approved |
| Hims / Hers | No (cash-pay only) | No | No | No | No | Yes — branded Wegovy/Ozempic via Novo partnership |
The Covered Path: In-Network Doctors and Plan Telehealth
For Molina members in covered states (or with covered indications like T2D, CV disease, or OSA), the strongest path is an in-network Molina doctor. Here’s how to find one and what to ask.
Use Molina’s official provider search first
Log in to your Molina state member portal and search by:
- Specialty: Primary care, endocrinology, obesity medicine, family medicine, or for indication-specific paths — cardiology (CV), sleep medicine (OSA), or hepatology (MASH)
- Location: Within a reasonable distance
- Visit type: Telehealth + in-person, telehealth-only, or in-person-only
Three questions to ask the office before booking
- “Do you submit pharmacy prior authorizations for Wegovy/Zepbound/Foundayo? About how long does it take?”
- “Do you appeal denials when needed?”
- “Do you take new patients for chronic weight management on Molina?”
If the answer is no to any of those for the medication you want, keep searching. Some primary care offices won’t touch GLP-1 PAs. Obesity-medicine specialists almost always will.
Teladoc and MD Live: free for many Molina Medicaid members, but with limits
- Teladoc critical limit: GLP-1 prescribing is not available through general medical or urgent care services. GLP-1 access requires an established Primary360 or Condition Management relationship with eligible Weight Management or Diabetes Prevention program access.
- MD Live critical limit: Can prescribe anti-obesity medications only through Routine Primary Care visits at physician discretion. MD Live does not prescribe anti-obesity medications in Florida, Louisiana, Mississippi, or New Jersey.
Can Ro, Sesame, Teladoc, or MD Live Use Molina Insurance?
Short answer: it depends on which Molina plan you have. The strongest option (Ro) works for Marketplace plans but cannot coordinate coverage on Medicaid or Medicare.
Ro — best for Molina Marketplace and self-pay readers
For Molina Marketplace members or anyone choosing to self-pay, Ro pairs a free GLP-1 Insurance Coverage Checker, an insurance concierge that files prior authorization for eligible commercial coverage, and a cash-pay backup if Marketplace coverage falls through. That combination is the strongest in consumer telehealth.
Sesame Care — provider choice for Marketplace and self-pay
Best secondary online option when you want to pick your own provider from a marketplace, want brand-name access including Foundayo, or want a lower membership fee. Subscription starts at $59/month with annual billing or $99/month month-to-month.
Covers: Foundayo, Wegovy (pill + injection), Zepbound (pen, KwikPen, vial), Ozempic, Mounjaro, Saxenda, Rybelsus, Contrave. Costco members can access discounted brand-name Wegovy and Ozempic through Sesame’s program.
Honest note on Molina: Sesame says insurance is accepted for weight-loss medications, but Molina-specific PA handling is provider-dependent. Verify with the Success by Sesame provider you select before paying.
Form Health, knownwell, PlushCare: visit-billing options
If you specifically want the telehealth visit itself billed to your Molina plan (as opposed to a cash-pay membership), three providers handle visit billing on commercial coverage:
- Form Health — Obesity-medicine specialists, files PA, accepts most major private insurance and Medicare. Form Health says it does not accept Medicaid for program costs. Verify Molina Marketplace and Medicare Complete participation directly.
- knownwell — No membership fee, in-network with many plans. Verify Molina-specific participation.
- PlushCare — In-network with Aetna, BCBS, Anthem, Humana, and Medicare. Molina compatibility varies; confirm before booking.
We don’t earn affiliate commissions from these three. They appear because some Molina readers genuinely need the visit-billing path.
The Cash-Pay Fallback: When Molina Excludes Your GLP-1
If your Molina plan doesn’t cover weight-loss GLP-1s — which is the case for most Molina Medicaid members in 2026 — your realistic options are LillyDirect or NovoCare cash-pay pricing on FDA-approved medication, or a cash-pay telehealth provider.
Cash-pay Path A: FDA-approved brand at LillyDirect / NovoCare prices
| Medication | Cash price | Notes |
|---|---|---|
| Zepbound vials (2.5mg) via LillyDirect | $299/month | 45-day refill offer |
| Zepbound vials (5mg) via LillyDirect | $399/month | 45-day refill offer |
| Zepbound vials/KwikPen (7.5–15mg) via LillyDirect | $449/month | 45-day refill offer; regular: $499–$699 |
| Wegovy oral pill (1.5mg or 4mg) via NovoCare | $149/month | 4mg increases to $199/month after Aug 31, 2026 |
| Wegovy pen (0.25mg/0.5mg) via NovoCare | $199/month first 2 fills | Eligible new patients; through June 30, 2026; then $349/month |
| Wegovy pen (all doses) via NovoCare — standard | $349/month | 0.25–2.4mg doses |
| Wegovy HD 7.2mg via NovoCare | $399/month | Newest formulation |
You still need a prescription from a licensed provider. Manufacturer savings card offers ($25/fill) apply only to commercial insurance and exclude government beneficiaries (Medicare, Medicaid, TRICARE, VA).
Cash-pay Path B: Telehealth providers for branded or compounded GLP-1s
None of these accept Molina — they’re cash-pay only. But they bundle the visit, prescription, and shipping at a single cash price.
MEDVi — Broad cash-pay menu including compounded semaglutide, compounded tirzepatide, and branded Ozempic. HSA/FSA-eligible. Best fit for a deep-menu cash-pay option.
Eden — Emphasizes FDA-approved Wegovy and Zepbound. No membership fees, HSA/FSA eligible. Best fit if you want a mainstream cash-pay service focused on FDA-approved options.
SHED Rx — Specialist in compounded oral and sublingual GLP-1 formulations. Compounded; self-pay; not FDA-approved. Not the path to FDA-approved Foundayo.
Hims and Hers — Following the March 2026 Novo Nordisk partnership, both offer broad access to FDA-approved Wegovy (pill and pen) and Ozempic.
About compounded GLP-1s — what you need to know
Compounded semaglutide and tirzepatide are not FDA-approved and are not the same as Wegovy, Zepbound, Ozempic, Mounjaro, or Foundayo. The FDA has raised concerns about compounded GLP-1 quality, dosing errors, fraudulent products, and adverse-event reports. The safety and effectiveness data from FDA-approved drug trials does not transfer to compounded preparations. Your prescriber can explain the trade-offs. If you want FDA-approved medication only, verify the specific medication on your provider’s checkout page before paying.
How Do I Find Molina’s GLP-1 Prior Authorization Form?
Molina’s GLP-1 prior authorization forms are state-specific. The fastest way to find yours: log in to your Molina state member portal, or ask your prescriber’s office to pull the right form through their provider portal. Most Molina state plans publish PA forms on their public provider page under “Pharmacy” or “Drug Formulary.”
For prescribers, the PA submission usually goes through one of three channels:
- Molina state provider portal (online submission)
- Availity Essentials (multi-payer portal)
- Fax to the state-specific Molina pharmacy PA fax number
State-specific contact lines like Molina Pharmacy Prior Authorization at 1-855-322-4080 (Texas) and 800-364-6331 (CVS Caremark, multiple Molina states) are common entry points published in Molina’s provider materials.
The Molina GLP-1 Prior Authorization Process
Almost every Molina-covered GLP-1 requires prior authorization. Many denials happen because the documentation is incomplete or the wrong indication was used. Here’s what Molina commonly requires and how long it takes.
What goes in a strong Molina GLP-1 PA submission
Bring this checklist to your prescriber. Exact requirements vary by state, plan, and drug.
- ☐Diagnosis with ICD-10 code (E66.x for obesity, E11.x for type 2 diabetes, plus comorbidities)
- ☐Current height, weight, and BMI with measurement dates
- ☐BMI documentation showing ≥30, OR ≥27 with a weight-related condition (hypertension, T2D, OSA, dyslipidemia)
- ☐Documented lifestyle modification attempts (diet + exercise + behavioral)
- ☐No personal or family history of medullary thyroid carcinoma
- ☐No MEN-2 syndrome
- ☐Not currently on another GLP-1 receptor agonist
- ☐For step-therapy plans: documented trial/failure of cheaper alternative (Saxenda before Wegovy, or Contrave/phentermine first)
- ☐Your prescriber's clinical rationale for medical necessity
- ☐For indication-specific pathways: documented CV disease (Wegovy CV), moderate-severe OSA (Zepbound OSA), or MASH (Wegovy MASH)
| Review type | Timeline | Notes |
|---|---|---|
| Standard review | 1–7 business days (some states up to 10) | Submit electronically when possible — faster than fax |
| Urgent review (medically urgent flag) | 24–72 hours | Ask your prescriber to mark as urgent if clinically appropriate |
| Renewal | Varies by plan and medication | Some Molina plans require documented weight-loss outcomes for renewal (e.g., Virginia requires ≥5% weight loss) |
The Molina Call Script
Five minutes on the phone with Molina before you pay anyone for anything saves weeks of paperwork and hundreds of dollars. Call the member services number on the back of your Molina card and read this script:
“Hi, I’m calling to verify GLP-1 medication coverage on my plan.
First — is my plan Medicaid, Marketplace, or Medicare Complete?
Second — is [Wegovy / Zepbound / Foundayo / Ozempic / Mounjaro] covered on my formulary or Preferred Drug List? Is it covered for [weight loss / type 2 diabetes / cardiovascular disease / sleep apnea]?
Third — does it require prior authorization, step therapy, or quantity limits? What documentation does the prior authorization need?
Fourth — which pharmacies are in my network for this medication?
Fifth — if my prior authorization is denied, what’s the appeal process and timeline?
Can you note this call in my file or send a written summary?”
Five questions, five minutes. You’ll know whether your Molina plan can cover what you need before you pay any telehealth fees.
What Happens If Molina Says the Drug Is Excluded?
A “drug is excluded” denial is different from a “PA criteria not met” denial. Resubmitting the same prior authorization usually cannot create coverage for a benefit exclusion. But you still have options.
Step 1: Read the denial letter carefully
| Denial reason | What it means for you |
|---|---|
| "Drug is excluded for weight-loss indication on this plan" | §1927 federal Medicaid exclusion or plan-specific benefit exclusion; PA resubmission usually cannot fix this. Move to indication pathway, formulary exception, or cash-pay. |
| "Insufficient documentation of prior weight-loss attempts" | Fixable with appeal + better paperwork. |
| "BMI not documented in last 30 days" | Fixable with appeal. |
| "Step therapy not satisfied" | Try Saxenda/Contrave/phentermine first, then resubmit. |
| "Off-label use" | Diabetes drug requested for weight loss; switch to FDA-approved indicated drug. |
| "Prior auth criteria not met" | Often fixable with stronger documentation. |
Step 2: File an appeal if the denial is fixable
You typically have 30–60 days from the denial date to file. Standard appeal package:
- Letter of medical necessity from your prescriber
- Updated BMI history with measurement dates
- Detailed documentation of prior weight-loss attempts
- Comorbidity documentation
- Personal letter describing health impact
- Any new clinical evidence
Per KFF’s analysis of ACA Marketplace claims, fewer than 1% of denied claims were appealed in 2024 — and insurers upheld 66% of appealed denials. The denials that get reversed tend to be the ones with stronger paperwork the second time around.
Step 3: Request a formulary exception or alternative indication
- Formulary exception: Your prescriber requests Molina cover a non-formulary drug based on medical necessity. Different from a standard PA.
- Alternative indication pathway: CV disease + obesity → Wegovy CV indication. Moderate-severe OSA + obesity → Zepbound OSA indication. MASH + obesity → Wegovy MASH indication. Type 2 diabetes → Ozempic, Mounjaro, or Rybelsus.
Step 4: Move to cash-pay if all routes are closed
If your plan flatly excludes weight-loss medications and you don’t qualify for an alternative indication:
- Wegovy oral pill through NovoCare: $149/month for 1.5mg or 4mg
- Zepbound vials through LillyDirect: $299–$449/month with 45-day refill
- Wegovy injection through NovoCare: $199/month new-patient intro pricing on lower doses, then $349/month standard
What Molina Members Actually Pay in 2026
The cost of a GLP-1 with Molina ranges from a few dollars per month if you’re a covered Medicaid member to $1,086+ at retail without insurance.
| Your scenario | Out-of-pocket cost per month |
|---|---|
| Molina Medicaid, covered state, PA approved | $0–$5 |
| Molina Marketplace, PA approved + manufacturer commercial savings card (commercial only — govt. beneficiaries excluded) | As low as $25 |
| Molina Marketplace, PA approved, no savings card | $50–$200 |
| Molina Medicare Complete, Bridge eligible (after July 1, 2026) | $50 flat |
| Molina excluded → LillyDirect Zepbound vial (with 45-day refill offer) | $299–$449 |
| Molina excluded → LillyDirect Zepbound (regular pricing without offer) | $499–$699 |
| Molina excluded → NovoCare Wegovy oral pill (1.5mg or 4mg) | $149 |
| Molina excluded → NovoCare Wegovy injection new-patient intro (0.25mg/0.5mg, first 2 fills) | $199 |
| Molina excluded → NovoCare Wegovy injection standard pricing | $349 |
| Molina excluded → retail Zepbound KwikPen | ~$1,086 |
| Molina excluded → Ro membership + cash-pay Zepbound | $39 first / $149 ongoing + $299–$449 medication |
| Molina excluded → compounded semaglutide (not FDA-approved) | $199–$499 |
Does Molina Medicaid Cover GLP-1s in My State?
Most state Medicaid programs don’t cover GLP-1s for weight loss. Per KFF’s January 2026 tracker, only 13 state Medicaid programs cover GLP-1s for obesity treatment under fee-for-service. Even within those states, your Molina managed-care plan may apply additional rules.
| State / plan | Verified observation | Verified date | What it does NOT prove |
|---|---|---|---|
| Washington (Apple Health via Molina) | Wegovy, Zepbound, Foundayo, Saxenda listed as "Carve Out" to Apple Health Fee-for-Service in 2026 PDL | Apr 2026 | Specific dose availability for any individual member; requires WA HCA verification |
| Michigan (Healthy Michigan via Molina) | Zepbound = Preferred with PA, QL 2 mL/28 days, age 18+; Wegovy = Non-Preferred with PA in 2026 | Apr 2026 | That a specific member's PA will be approved |
| California (Medi-Cal Rx) | Wegovy, Zepbound, Saxenda for weight loss = NOT COVERED effective Jan 1, 2026; Wegovy CV indication remains covered with PA | Apr 2026 | Coverage status under non-Medicaid lines of Molina California |
| Texas (Molina TX Medicaid + CHIP) | Molina TX 2026 PA Criteria Guide includes GLP-1 receptor agonists, Ozempic, Mounjaro, Rybelsus, Wegovy, Zepbound PA workflows | Apr 2026 | That weight-loss use will be approved |
| Kentucky (Passport by Molina) | GLP-1 PA criteria limited to T2D diagnosis; weight-loss use excluded | Apr 2026 | Marketplace or other Molina lines |
| Virginia (Molina VA) | Weight-loss SA form includes Wegovy/Zepbound BMI and risk-factor criteria, plus 5% weight-loss renewal threshold | Apr 2026 | Specific approval probability |
| Other Molina-served states | Pull current state PDL or call Molina | — | Anything we haven't verified |
Recent state changes (California, NH, PA, SC eliminating weight-loss coverage Jan 1, 2026; North Carolina suspending then reinstating in late 2025) prove how fast the landscape moves. Before paying any telehealth fee, run the call script above.
How We Picked These Providers
We rank providers based on what actually works for Molina members in different situations, not on affiliate payouts. We applied four filters:
- Plan-type compatibility — Does this provider work with Molina Medicaid, Marketplace, Medicare Complete, or only one of those?
- PA workflow strength — Does the provider’s team file insurance prior authorization on commercial plans, or do they hand you a prescription and hope?
- FDA-approved medication access — For insurance-sensitive readers, FDA-approved brand-name medication is the priority because that’s what insurance covers.
- Honest disqualification — A provider gets ranked lower if their workflow systematically fails certain Molina plan types we know they can’t serve.
This is why Ro is our primary recommendation for Molina Marketplace and self-pay readers, but not for Medicare Complete — Ro’s insurance concierge handles commercial PA filings, but Ro cannot coordinate government-plan coverage. This is why Form Health appears in the matrix despite earning us no commission — for Marketplace and Medicare members who specifically want their visit billed in-network. This is why MEDVi, Eden, SHED, and Hims/Hers appear only as cash-pay fallback — they don’t accept Molina, and saying so honestly is what makes this guide useful.
The RX Index is a pricing intelligence and comparison resource for GLP-1 telehealth providers. We earn affiliate commissions from Ro, Sesame Care, MEDVi, Eden, SHED Rx, Hims, Hers, and other providers when readers start through our links. Affiliate relationships do not change which provider we conclude is the best fit.
Frequently Asked Questions
Do any GLP-1 providers actually accept Molina?
Yes — but 'accepts Molina' means different things. In-network Molina doctors and pharmacies bill Molina directly for visits and medications. Online programs like Ro can file prior authorization for eligible commercial coverage but explicitly cannot coordinate government-plan coverage like Medicaid or Medicare. Cash-pay providers like Eden, MEDVi, SHED, and Hims/Hers don't accept Molina at all.
Does Molina cover Wegovy for weight loss?
It depends on your plan and state. Molina Marketplace plans generally cover Wegovy with prior authorization on commercial-style formularies. Molina Medicaid covers Wegovy for weight loss only in the limited number of states with Medicaid GLP-1 obesity coverage — 13 states under fee-for-service per KFF as of January 2026. Molina Medicare Complete will cover Wegovy through the Medicare GLP-1 Bridge starting July 1, 2026, at $50/month for eligible members.
Does Molina cover Zepbound?
Coverage is tightening. CVS Caremark removed Zepbound from its Standard Control, Advanced Control, and Value formularies in July 2025 with Wegovy now preferred — and CVS Caremark administers some Molina commercial plans. Molina Medicaid coverage of Zepbound for weight loss varies by state. Only the Zepbound KwikPen format is eligible through the Medicare GLP-1 Bridge.
Does Molina cover Ozempic for weight loss?
No. Ozempic is FDA-approved for type 2 diabetes only. Molina covers Ozempic for documented type 2 diabetes with prior authorization, but off-label weight-loss prescriptions are denied. The FDA-approved version of semaglutide for weight loss is Wegovy.
Does Molina cover Mounjaro for weight loss?
No. Mounjaro is FDA-approved for type 2 diabetes. Molina covers it for documented T2D with PA, not for off-label weight loss. The FDA-approved tirzepatide for weight loss is Zepbound.
Does Molina cover Foundayo?
Foundayo (orforglipron) is FDA-approved for chronic weight reduction in adults with obesity, or overweight with at least one weight-related comorbidity. CMS has confirmed Foundayo as an eligible product under the Medicare GLP-1 Bridge starting July 1, 2026. Marketplace and Medicaid coverage is being added plan-by-plan — verify your specific formulary.
Can I use Ro with Molina?
For Molina Marketplace, yes — Ro's free coverage checker contacts your insurance and Ro's concierge files prior authorization. For Molina Medicaid or Molina Medicare Complete, no — Ro is a cash-pay membership and explicitly cannot coordinate coverage with government insurance plans. Government-plan members should use an in-network Molina doctor for Medicaid or the CMS Medicare GLP-1 Bridge through their prescriber for Medicare.
Does Sesame Care accept Molina?
Sesame Care is a cash-pay telehealth marketplace and does not bill Molina for visits. The Success by Sesame subscription is cash-pay. Sesame says insurance is accepted for weight-loss medications, but Molina-specific PA handling is provider-dependent — verify with the Success by Sesame provider you select before paying.
Does Form Health accept Molina?
Form Health says it accepts most major private insurance and Medicare. Form Health does not accept Medicaid for program costs — including Molina Medicaid. For Molina Marketplace or Molina Medicare Complete, verify Molina-specific participation directly with Form Health before booking.
Can Teladoc prescribe GLP-1s through Molina?
Many Molina Medicaid plans include Teladoc at no cost, but Teladoc's general medical and urgent care services do not prescribe GLP-1 medications. GLP-1 access through Teladoc requires an established Primary360 or Condition Management relationship with eligible Weight Management or Diabetes Prevention program access. Call Molina member services to confirm what your plan includes.
Can MD Live prescribe GLP-1s?
MD Live can prescribe anti-obesity medications including GLP-1s only through Routine Primary Care visits at physician discretion. MD Live does not prescribe anti-obesity medications in Florida, Louisiana, Mississippi, or New Jersey. If you're in those states, MD Live is not an option for this use case.
Do I need prior authorization for GLP-1s with Molina?
In nearly all cases, yes. Molina commonly requires PA for Wegovy, Zepbound, Foundayo, Saxenda, Ozempic, Mounjaro, and Rybelsus, though specific PA requirements vary by state, plan type, formulary, drug, and indication. Standard PA review takes 1–7 business days; urgent review takes 24–72 hours.
What states does Molina cover GLP-1s for weight loss?
Per KFF's January 2026 update, only 13 state Medicaid programs cover GLP-1s for obesity treatment under fee-for-service. The list changes — California, New Hampshire, Pennsylvania, and South Carolina eliminated coverage as of January 1, 2026; North Carolina briefly suspended coverage but reinstated it in December 2025. Always verify with your state's current Preferred Drug List and Molina directly.
How do I get Wegovy approved through Molina?
Your prescriber submits a prior authorization documenting your BMI (30 or higher, or 27 or higher with a comorbidity), prior weight-loss attempts, and absence of contraindications. Standard review takes 1–7 business days. Use a provider experienced with insurance PAs — Ro for commercial Marketplace coverage, Form Health for major private insurance and Medicare, or an in-network Molina obesity-medicine specialist for Medicaid.
What if Molina denies my prior authorization?
Read the denial letter for the specific reason. If it's a fixable issue (incomplete documentation, missing BMI, step therapy not met), file an appeal with stronger paperwork — you typically have 30–60 days. If the denial is a benefit exclusion ('drug is excluded for weight-loss indication'), a PA resubmission usually can't create coverage; consider an alternative indication pathway (CV disease, OSA, MASH, T2D), a formulary exception request, or move to cash-pay.
Are compounded GLP-1s covered by Molina?
No. Compounded semaglutide and tirzepatide are not FDA-approved and are not on any Molina formulary. They're cash-pay only. The FDA has raised specific concerns about compounded GLP-1 quality, dosing errors, and fraudulent products — discuss with your prescriber before choosing this path.
What's the cheapest path to a GLP-1 if Molina won't cover it?
For FDA-approved medication: NovoCare Wegovy oral pill at $149/month (1.5mg or 4mg) is the lowest. NovoCare Wegovy pen new-patient intro is $199/month for the first two fills (eligible new patients only). LillyDirect Zepbound vials are $299–$449/month with the 45-day refill offer.
When does Medicare cover GLP-1s for Molina Medicare Complete members?
Starting July 1, 2026, the Medicare GLP-1 Bridge gives eligible Medicare beneficiaries — including those on Molina Medicare Complete in eligible Part D plan types — access to Wegovy (injection and pill), Zepbound KwikPen, and Foundayo at $50/month flat copay through December 31, 2027. Eligibility requires both an eligible Part D plan type and a prescriber-submitted prior authorization through the Bridge's central processor.
Can I appeal a Molina GLP-1 denial?
Yes. Molina allows 30–60 days (state-dependent) to file an appeal. Submit through your Molina state member portal, by fax to the state-specific PA appeal address, or via Availity Essentials provider portal. Appeals succeed most often when the original denial was for documentation deficiency rather than plan exclusion.
The Bottom Line: Your Next Step
The path that works for you depends on your Molina plan type, your state, and which GLP-1 you need.
If you have Molina Marketplace
Start Ro’s free coverage check. If Molina covers it, Ro files PA and you pay a copay at the pharmacy. If Molina denies, Ro’s cash-pay backup is right there.
If you have Molina Medicare Complete
The Medicare GLP-1 Bridge launches July 1, 2026, at $50/month flat for eligible members. Talk to your prescriber about preparing your PA packet for the Bridge’s central processor. Ro and Sesame are cash-pay options for the wait period.
Read our full Medicare GLP-1 Bridge guide →If you have Molina Medicaid in a covered state
Use Molina’s provider directory to find an in-network doctor who handles GLP-1 PAs. Call the office and ask the three questions in our covered-path section. Your Medicaid benefit applies — no telehealth membership fee required.
If you have Molina Medicaid in an excluding state (most states)
Skip the insurance route. Your fastest cash-pay paths are NovoCare Wegovy oral at $149/month or LillyDirect Zepbound vials at $299/month. Or use Ro for a one-stop branded cash-pay experience.
Don’t know what Molina plan you have?
Take our free 60-second quiz. We’ll figure it out and route you to the right path in under a minute.
Find My GLP-1 Path →Related Guides
- Best GLP-1 Providers That Accept Insurance
- Medicare GLP-1 Bridge: Full 2026–2027 Guide
- Best Zepbound Providers That Accept Insurance
- Compounded vs. FDA-Approved GLP-1s
- Does Medicare Cover Wegovy for Weight Loss?
- Does Ro Accept Insurance for GLP-1?
- Sesame Care Reviews
- GLP-1 Providers That Accept Aetna
- GLP-1 Providers That Accept UnitedHealthcare
- GLP-1 Providers That Accept Anthem