Does Cigna Cover Mounjaro? 2026 PA Rules, Real Costs, and What to Do Next
By The RX Index Editorial Team — a pricing intelligence and comparison resource for GLP-1 telehealth providers.
Published: · Last reviewed:
Some links on this page are affiliate links. We may earn a commission if you choose a featured provider, at no extra cost to you. Our coverage facts come from Cigna's published policies, the FDA, Eli Lilly, and the providers we feature. We do not change our recommendations based on payouts.
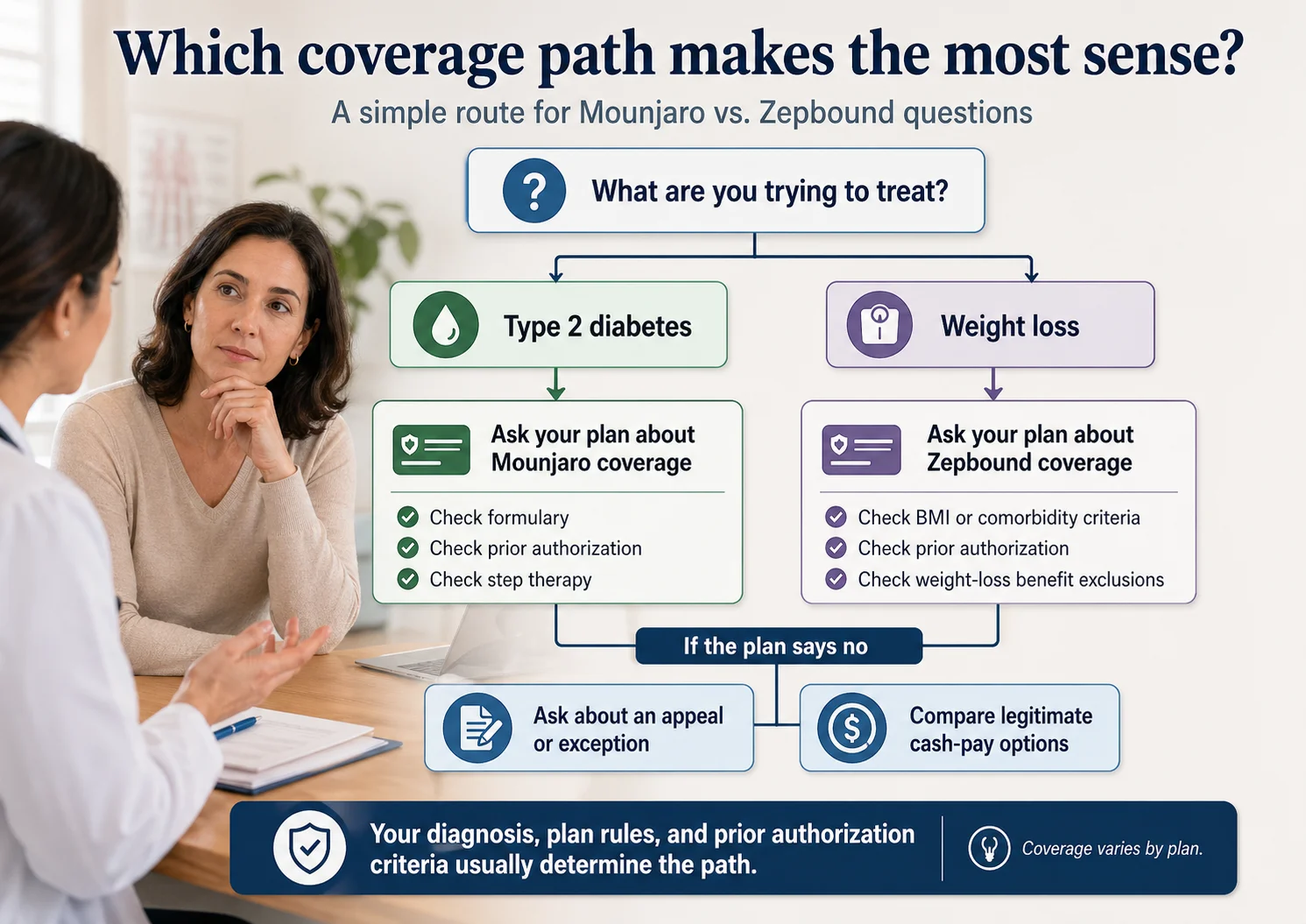
The short answer
Does Cigna cover Mounjaro? Yes for type 2 diabetes when your specific Cigna plan includes it and Cigna's prior authorization criteria are met. Cigna's current GLP-1 coverage policy treats Mounjaro as medically necessary for type 2 diabetes in patients age 10 and older — and not medically necessary for weight loss without type 2 diabetes, type 1 diabetes, prediabetes, or metabolic syndrome.
Here's what most pages won't tell you: if Cigna can see a recent claim for an oral diabetes medication on your record — anything except Rybelsus or single-entity metformin — your Mounjaro claim may clear at the pharmacy without a manual prior authorization review. That's not a guarantee. But it's the path most established type 2 diabetes patients take, and almost nobody explains it. We'll show you when it triggers, when it doesn't, and what to do in both cases.
If your real goal is weight loss and you don't have type 2 diabetes, we'll save you a wasted appointment fee. Cigna's policy is clear on this. We'll show you which Cigna-covered drug is the right question (it's the same active ingredient, different label) and how to check whether your plan covers it.
Find your situation in this table
| Your situation | Cigna's likely answer | What you'll pay |
|---|---|---|
| Type 2 diabetes, age 10+, recent oral diabetes drug on file | Often clears at pharmacy without a manual PA | As low as $25/month with Lilly Savings Card if eligible |
| Type 2 diabetes, age 10+, new diagnosis or no recent oral diabetes med | Manual prior authorization required | As low as $25/month if approved |
| Want Mounjaro for weight loss, no diabetes | Denied — policy excludes this use | Ask about Zepbound instead |
| Prediabetes or PCOS, no type 2 diabetes | Denied under Mounjaro's diabetes policy | Different path needed |
| Existing user, refill suddenly blocked | PA expired, quantity limit, plan year change, or exclusion | Depends on the rejection code |
| Cigna Medicare Part D + type 2 diabetes | Covered for diabetes only — never weight loss on Medicare | Capped by Part D's $2,100 max out-of-pocket in 2026 |
Not sure which row is yours? Take our 60-second Cigna Mounjaro path check. You'll get a personalized answer plus the documents your doctor needs to give Cigna.
Check my Cigna Mounjaro path →What we actually verified
We don't ask you to take our word for this. Here's exactly what we read and when.
| Source | What it tells you |
|---|---|
| Cigna Diabetes – GLP-1 Agonists PA Policy (CNF360, rev. 01/07/2026) | Mounjaro can be approved for type 2 diabetes in patients age 10+ when criteria are met. Lists weight loss without T2D, type 1 diabetes, prediabetes/diabetes prevention, and metabolic syndrome without T2D as not medically necessary uses. |
| Cigna Weight Loss – GLP-1 Agonists PA Policy (CNF684) | A separate policy governing Zepbound, Wegovy, and Saxenda — not Mounjaro. |
| Cigna National Preferred 5-Tier Drug List (starts July 1, 2026) | Mounjaro is listed under Diabetes with PA and QL flags. Plan-specific coverage may differ. |
| FDA Mounjaro prescribing information | FDA-approved as adjunct to diet and exercise to improve glycemic control in adults and pediatric patients age 10+ with type 2 diabetes. Boxed warning for thyroid C-cell tumors. |
| Eli Lilly Mounjaro pricing page | List price $1,112.16 for a 28-day supply. Mounjaro Savings Card may bring cost to as low as $25 per fill with eligible commercial insurance. Terms run through 12/31/2026. |
| Ro Body Program | Ro does not currently offer Mounjaro. Ro carries Zepbound for tirzepatide weight-loss treatment, plus Wegovy and Foundayo where available. |
| Sesame Care | Sesame providers can prescribe Mounjaro when clinically appropriate and can assist with prior authorization paperwork. Prescriptions are at the provider's discretion. |
What we did not verify and you must check yourself: your specific plan's copay, your deductible, your employer's drug exclusions, which pharmacy channel your plan requires, whether your prescriber will submit the PA, and whether any appeal will succeed. We'll show you exactly how to look these up in myCigna in a few minutes.
Does Cigna cover Mounjaro? The 3 questions that decide your answer
Cigna isn't one plan. It's hundreds of plan designs administered through Cigna Healthcare and Evernorth (Cigna's health services arm, which includes Express Scripts as the pharmacy benefit manager and Accredo as one of the specialty pharmacies). What your neighbor's Cigna plan covers may have nothing to do with what yours covers.
So "does Cigna cover Mounjaro" is really three stacked questions:
- Is Mounjaro on my plan's drug formulary at all? Mounjaro appears on Cigna's National Preferred drug list under Diabetes, but plan-specific coverage can differ.
- What does my plan require before it pays? Prior authorization, almost always. Sometimes step therapy. Sometimes a specific pharmacy channel.
- Will I actually meet those requirements? That depends on your diagnosis, your treatment history, and what your prescriber documents.
Most coverage articles answer question 1 and skip 2 and 3. We're going to walk through all three.
Does Cigna cover Mounjaro for type 2 diabetes?
Yes. Cigna covers Mounjaro for type 2 diabetes when prior authorization criteria are met, with approval typically granted for one year at a time. For patients already on an oral diabetes medication, the claim may clear through point-of-service logic without a manual PA review.
The Cigna criteria for Mounjaro and type 2 diabetes
Cigna's current Diabetes – Glucagon-Like Peptide-1 Agonists Prior Authorization Policy (CNF360, selected revision 01/07/2026) lists Mounjaro as covered when prescribed for type 2 diabetes in patients age 10 and older. Approval is typically granted for one year.
The same policy lists four uses as not medically necessary:
- Weight loss in a patient without type 2 diabetes
- Type 1 diabetes
- Prediabetes or diabetes prevention
- Metabolic syndrome without type 2 diabetes
These aren't paperwork you can appeal your way around. These are the lines Cigna drew at the policy level.
The 130-day point-of-service rule almost nobody talks about
Here's the part you won't find on most Cigna Mounjaro pages: Cigna built automation into the policy. If Cigna sees a pharmacy claim on your record for an oral diabetes medication — anything except Rybelsus or single-entity metformin — within the past 130 days, and the age criterion is met, your Mounjaro claim may adjudicate at the pharmacy through point-of-service logic. No manual PA submission required.
What this looks like in practice: if you've been on a sulfonylurea, a DPP-4 inhibitor, an SGLT-2 inhibitor, or a metformin combination drug recently, the pharmacy system can see your prior diabetes claim, see Mounjaro is approved for type 2 diabetes, and pay without your doctor's office sending paperwork.
This is not a guarantee. Plans can have additional edits. Your prior diabetes meds may have been filled outside the lookback window, at a pharmacy not visible to Cigna, or under a different insurance. If the automation doesn't trigger, a manual PA submission is required.
But when it does trigger, you skip the 5-to-10 business day wait. That's the part most readers don't know exists.
What your doctor needs if a manual PA is required
If a manual PA is needed, your prescriber's office will submit through CoverMyMeds, Cigna's provider portal, or EviCore by Evernorth. The documentation that helps your case includes:
- Your name, date of birth, and Cigna member ID
- Type 2 diabetes diagnosis with ICD-10 code (usually E11.x)
- Recent A1c lab value
- Prior diabetes medication history with dates, doses, and outcomes
- Why Mounjaro specifically is being requested (intolerance to alternatives, inadequate glycemic control, etc.)
- The dose and quantity prescribed
Specificity wins. A PA note that says "patient failed metformin" leaves Cigna's reviewer with nothing to verify. A PA note that names the dose, duration, A1c trend, and reason for switching gives the reviewer something concrete to approve.
If you have type 2 diabetes and want a clinician who handles the Mounjaro prescription and prior authorization paperwork, Sesame Care has online providers who can prescribe Mounjaro when clinically appropriate and assist with PA submission. Sesame visits are pay-per-visit — Costco members see $29 virtual primary care pricing through Sesame's partnership. A prescription is not guaranteed and depends on your clinical situation.
See if a Sesame provider can help with my Mounjaro PA → (sponsored affiliate link, opens in a new tab)Does Cigna cover Mounjaro for weight loss?
No. Cigna's diabetes GLP-1 policy lists Mounjaro for weight loss without type 2 diabetes as not medically necessary — regardless of BMI. If weight loss is your goal, the right question for your insurance is whether Cigna covers Zepbound (same active ingredient, different FDA-approved label).

The reality most pages dance around
If you do not have type 2 diabetes, and you ask your doctor to prescribe Mounjaro for weight loss, three things will happen:
- Your doctor can write the prescription. Off-label prescribing is legal.
- You'll hand it to the pharmacy.
- Cigna will reject the claim. The denial reason will say something like "not approved for indication" or "off-label use."
This isn't a paperwork problem you can rewrite your way out of. It's a policy-level exclusion. Cigna's diabetes GLP-1 policy lists this use as not medically necessary, and the appeal pathway for "not medically necessary under our standard policy" is narrow. Some plans allow exception requests, but the realistic next step for almost every reader in this situation is a different drug, not a louder Mounjaro PA letter.
Why this happens — and why it's actually good news
Mounjaro and Zepbound both contain tirzepatide as the active ingredient, are made by Eli Lilly, and come in the same dose strengths. The FDA approved them under different labels: Mounjaro for type 2 diabetes, Zepbound for chronic weight management (and also for moderate-to-severe obstructive sleep apnea in adults with obesity).
Cigna treats them as separate drugs because the FDA-approved indications are different. Mounjaro for weight loss = off-label = denied. Zepbound for weight loss = on-label = potentially covered under Cigna's separate weight-loss GLP-1 policy.
So does Cigna cover Zepbound?
Cigna has a separate policy — Weight Loss – Glucagon-Like Peptide-1 Agonists Prior Authorization (CNF684) — that covers Zepbound, Wegovy, and Saxenda. Two things determine your outcome:
- Your employer plan must not exclude anti-obesity medications. Some employer plans carve out "weight-loss drugs" entirely. If your plan has that exclusion, no medical-necessity argument wins the appeal.
- You'll still need PA. Typical criteria include adult age, BMI ≥30 (or ≥27 with a weight-related condition like high blood pressure, sleep apnea, or dyslipidemia), and documented behavioral modification or diet/exercise efforts.
If weight loss is your real goal, the fastest move is a free Cigna Zepbound check — not a doctor's appointment for Mounjaro.
Ro's GLP-1 Insurance Coverage Checker plugs into your specific plan and shows you which FDA-approved GLP-1 medications your Cigna plan covers. If Zepbound is covered, Ro's insurance concierge handles the prior authorization paperwork. If it's not covered, Ro offers Zepbound as a cash-pay option starting at $299/month for the 2.5 mg starter dose, $399/month for 5 mg, and $449/month for higher doses with on-time refills. Ro Body membership: Get started for $39, then as low as $74/month with annual plan paid upfront. Medication cost is separate.
Check Cigna's Zepbound coverage free with Ro → (sponsored affiliate link, opens in a new tab)How to check your own Cigna Mounjaro coverage in 5 minutes
The only person who can tell you exactly what your plan pays is Cigna. Log into myCigna.com, go to Price a Medication, search Mounjaro, and you'll see your tier, your copay, your prior authorization status, and your quantity limit — for your specific plan.
This is the single most useful five minutes you can spend before your next doctor's appointment.
Log into myCigna.com
If you don't have an account, your member ID and date of birth are enough to create one. The mobile app works the same way.
Find Price a Medication
It’s under the “Prescriptions” tab. On the app, tap “Prescriptions” → “Price a Medication.”
Search “Mounjaro” or “tirzepatide”
Search by either brand name or generic name. Both should return the same result.
Read the result
You'll see: Tier (often Tier 3 non-preferred brand or Tier 4 specialty), PA required, QL (typically 4 pens per 28 days), ST (step therapy if your plan adds it), and your estimated copay — the most useful number.
Screenshot it
Send the screenshot to your prescriber's office. This tells them exactly what your plan requires and saves them a phone call.
What PA, QL, and ST mean in plain English
| Code | What it means |
|---|---|
| PA | Prior Authorization — Cigna must approve the medication before they pay. Your doctor submits documentation. |
| QL | Quantity Limit — Cigna pays for a specific quantity per time period. Fill more than that, you pay the difference. |
| ST | Step Therapy — You must try (and fail or be intolerant to) cheaper covered alternatives before Cigna pays for the more expensive drug. |
Cigna phone script
Call the member services number on the back of your Cigna ID card. Read this:
"Hi, I'm checking pharmacy coverage for Mounjaro — generic name tirzepatide — for type 2 diabetes. Can you tell me: Is it on my formulary? What tier? Is prior authorization required? Is there a quantity limit? Is step therapy required? Does my plan have any exclusion related to weight-loss drugs or GLP-1s? Which pharmacy channel does my plan require — retail, home delivery, or specialty? And what's my estimated copay after deductible?"
Pharmacy script
If you're standing at the counter and the pharmacist says "your insurance is rejecting this," ask:
"Can you tell me the exact rejection code? Is this a prior authorization issue, a quantity limit, a refill-too-soon problem, a plan exclusion, or a coupon-processing issue?"
The pharmacy software shows them a specific code. Knowing which code is rejecting determines your next move.
The Cigna Mounjaro Approval Matrix
This table crosses your medical situation with your plan type and shows what Cigna actually does in each square.
| Your situation | What Cigna does | What you provide | Est. monthly cost if approved |
|---|---|---|---|
| T2D + recent oral diabetes med in claims (last ~130 days) + age 10+ | May clear through point-of-service logic without a manual PA | Active Mounjaro Rx + insurance card | As low as $25 with Lilly Savings Card (commercial insurance, age 18+, FDA-approved use) |
| T2D + newly diagnosed or no recent oral diabetes med | Manual PA required, typically 5–10 business days | A1c, T2D diagnosis (E11.x), clinical rationale | As low as $25 with Lilly Savings Card if approved |
| T2D + plan with step therapy added | PA with documented trial of preferred alternatives required | A1c trend, documented failure or intolerance to required step drugs | As low as $25 with savings card |
| Want Mounjaro for weight loss + no T2D | Denied under Cigna's diabetes GLP-1 policy | Cleaner path is Zepbound — different policy | N/A — pivot to Zepbound |
| Prediabetes only | Denied. Excludes diabetes prevention | N/A | N/A — different approach needed |
| PCOS or insulin resistance, no T2D | Denied under Mounjaro's diabetes policy | Discuss FDA-approved weight-loss path or T2D evaluation | N/A |
| Cigna Medicare Part D + T2D | Covers for diabetes only. PA required for most plans. | A1c, T2D diagnosis | Plan copay; 2026 Part D max out-of-pocket is $2,100 |
| Cigna + Medicaid + T2D | Coverage varies by state Medicaid program | A1c, T2D diagnosis | Medicaid copay (no Lilly Savings Card eligibility) |
| Cigna ACA marketplace plan + T2D | Follows commercial PA pattern | A1c, T2D diagnosis | Plan copay (savings card eligibility depends on plan type) |
| Cigna employer plan with anti-obesity drug exclusion rider | Denies weight-loss intent regardless of medical necessity | Plan exclusion overrides medical-necessity arguments | Cash pay, switch plans, or alternative coverage path |
| Existing user, refill blocked at pharmacy | Depends on the rejection code | Find out the code first — it determines your next move | Varies |
Find your row. Then act on the rightmost two columns.
What Mounjaro actually costs with and without Cigna
With eligible commercial Cigna coverage and the Mounjaro Savings Card, you can pay as little as $25 per fill. Without Cigna coverage, retail cash and coupon prices typically run around $930 to $1,100 per month depending on pharmacy and discount program (verified May 14, 2026). The savings card has a separate tier that can bring cost to $499 per fill even when your commercial plan doesn't cover the drug — but it's never available to anyone on Medicare, Medicaid, TRICARE, or VA benefits.
Your real-world cost ladder
| Path | Monthly cost (verified May 14, 2026) | Who qualifies |
|---|---|---|
| Cigna covers Mounjaro + Lilly Savings Card | As low as $25/fill | Age 18+, commercial Cigna covering Mounjaro, FDA-approved use. Up to $1,950 annual savings, max 13 fills/year. |
| Cigna doesn't cover it + Lilly Savings Card (commercial insurance) | As low as $499/fill | Age 18+, commercial insurance, FDA-approved use, plan doesn't cover Mounjaro. Up to $8,411 annual savings. |
| Cash with SingleCare coupon at major U.S. pharmacies | ~$928–$953 | Anyone |
| Cash with GoodRx coupon | As low as $1,097 | Anyone |
| Manufacturer list price (WAC) | $1,112.16 | Reference price — per 28-day supply (Lilly, current) |
| Cigna Medicare Part D + T2D | Plan copay | Cigna Medicare beneficiaries with T2D; capped by Part D's $2,100 max out-of-pocket for the year |
How the Lilly Mounjaro Savings Card actually works
The card has two tiers, both for commercial drug insurance only:
Tier 1 — commercial insurance that covers Mounjaro
As low as $25 for a 1-month, 2-month, or 3-month fill. Maximum monthly savings of $150 (1-month), $300 (2-month), or $450 (3-month). Annual savings capped at $1,950. Up to 13 fills per calendar year.
Tier 2 — commercial insurance that does NOT cover Mounjaro
As low as $499 for a 1-month fill. Annual savings cap of $8,411.
You must be age 18 or older, your prescription must be for an FDA-approved use, and the savings-card terms currently run through December 31, 2026. Terms can change, so check Lilly's current Mounjaro savings page before relying on the price.
Who's permanently excluded from the card: Medicare, Medicaid, Medigap, DoD, VA, TRICARE, CHAMPUS, or any state pharmaceutical assistance program. Federal anti-kickback rules block savings card use for anyone on a government plan.
Why your price can change after the first fill
A good first month doesn't mean twelve good months. Your cost can shift because of:
- Deductible reset. Most plans reset January 1. On high-deductible plans, your first fill of the year may be retail price until you hit the deductible.
- Plan year change. Employers re-shop pharmacy benefits annually. A plan that covered Mounjaro last year may not next year.
- PA expiration. Your one-year approval ends. If your prescriber doesn't renew on time, the next claim denies.
- Quantity limit overrun. You try to fill early. The plan rejects.
- Savings card annual cap. You hit the $1,950 or $8,411 ceiling.
If your refill suddenly costs more or got rejected, find out why before you pay full price. Our free Cigna Mounjaro Coverage Triage Tool identifies which of the common rejection codes you're hitting and what to do next.
How Cigna may fill your Mounjaro
Don't assume your Mounjaro will come from one specific pharmacy. Cigna and Evernorth (which includes Express Scripts and Accredo) support multiple pharmacy channels depending on your plan: retail in-network, Express Scripts home delivery, or Accredo for specialty medications. Check myCigna for your plan's required or preferred channel before transferring your prescription.
A lot of Mounjaro users don't think about this until they hand the script to a retail pharmacy and the pharmacist says "your plan requires this through another channel."
How to find your required pharmacy channel
In myCigna, your Prescription Drug List details should tell you whether Mounjaro can be filled at a retail pharmacy, requires home delivery, or routes through specialty pharmacy. If you're unsure, call Cigna member services and ask: "For my plan, can Mounjaro be filled at a retail pharmacy, or does it require home delivery through Express Scripts or specialty pharmacy through Accredo?"
If your plan uses Accredo for Mounjaro
- Your prescriber sends the prescription to Accredo (or you call to transfer it).
- Accredo verifies coverage with Cigna. This is when any PA paperwork is pulled.
- You set up an account at MyAccredoPatients.com. First-time setup takes 10–15 minutes.
- Accredo ships the medication in temperature-controlled packaging. Mounjaro pens require refrigeration, so coordinate to be home for delivery.
- Refills come on a schedule. Accredo will check in to verify you're on track for the next fill.
What to do if Cigna denied your Mounjaro
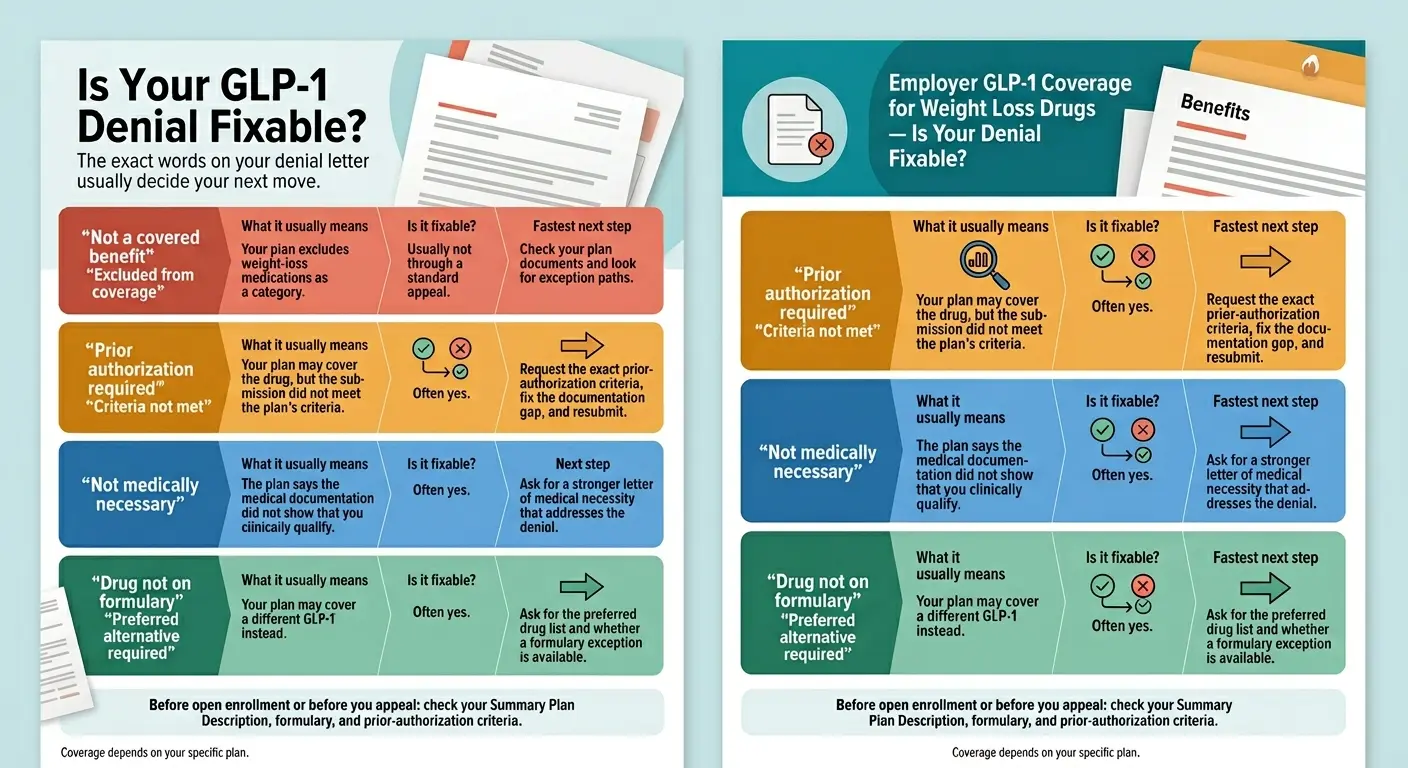
Don't appeal blindly. First, figure out the denial reason. Most Cigna Mounjaro denials are documentation problems — and the fix depends entirely on the denial code.
Pull your denial letter (or call Cigna and have them email it through your member portal). Find the denial reason. Then use this table.
The 7-reason denial decoder
| The denial says… | What it actually means | Your next move |
|---|---|---|
| "Prior authorization required" | The pharmacy claim hit Cigna's system but no PA was on file yet. Common at first fill or after a plan year change. | Your prescriber submits a PA through CoverMyMeds or Cigna's provider portal. Typically 5–10 business days. |
| "Missing information" | A PA was submitted, but key data was missing — usually the A1c value, the diagnosis code, or prior therapy details. | Your prescriber resubmits with the specific missing data. |
| "Not approved for indication" or "Off-label use" | Cigna saw the prescription is for weight loss (or another non-T2D use) without a T2D diagnosis on file. | The practical next step is pivoting to Zepbound if your goal is weight loss. Cigna's diabetes policy is the binding wall here. |
| "Step therapy not met" | Your specific plan requires you to try and fail covered alternatives first. | Your prescriber documents the trial and failure of the required step drugs. |
| "Quantity limit exceeded" | You tried to fill more than the plan covers per period. | Ask the pharmacy to reduce the quantity, or your prescriber submits a QL exception. |
| "Plan exclusion" | Your employer's specific plan excludes this drug category entirely. | Read your Summary Plan Description. If excluded, no medical-necessity appeal will work. Pivot to a covered alternative or different plan at open enrollment. |
| "Authorization expired" | Your one-year PA ended. | Your prescriber submits a renewal — ideally 30–45 days before expiration to prevent a gap. |
How to file the appeal
If your denial is a documentation problem (not a policy exclusion), you have appeal rights:
- Internal appeal: File within the time window listed on your denial letter (often 180 days). Include the denial letter, the corrected PA submission, A1c labs, diagnosis documentation, and prior therapy history.
- Peer-to-peer review: Your prescriber calls Cigna and requests a clinical discussion with a Cigna medical director. Get the number from your denial letter.
- External review: Available after internal appeal denial. Independent physician reviewers decide. The decision is binding on Cigna. Timing and exact rules are on your denial letter.
What not to do
- Don't ask your provider to code a diagnosis you don't have. This is fraud. It can cost your provider their license and trigger a fraud investigation against you.
- Don't assume "denied" means "no Cigna drug will ever work." Most denials of Mounjaro can be redirected to a covered alternative — Zepbound, Wegovy, or a different diabetes drug — that your plan does pay for.
- Don't pay full retail without checking the savings card first. Even if Cigna denies coverage, the Lilly Savings Card Tier 2 may bring your cash cost from $1,112 to $499 if you have other commercial insurance.
If you're staring at a denial letter and want a clinician to review your situation, Sesame Care has providers who can evaluate your Mounjaro request and assist with prior authorization paperwork. Visits are pay-per-visit and a prescription is not guaranteed.
See if a Sesame provider can help with my Mounjaro PA → (sponsored affiliate link, opens in a new tab)If your goal is weight loss and your Mounjaro request was denied, Ro's free GLP-1 Insurance Coverage Checker shows whether Zepbound is covered under the same Cigna plan.
Check Zepbound coverage instead — free with Ro → (sponsored affiliate link, opens in a new tab)Cigna Medicare, Medicaid, Marketplace, and TRICARE: how each one handles Mounjaro
The biggest functional difference across plan types: the Lilly Mounjaro Savings Card is not available to anyone on Medicare, Medicaid, TRICARE, or VA. Coverage rules and copays also differ across Cigna Commercial, Cigna Medicare Advantage, Cigna Medicare Part D, Cigna Medicaid managed care, and Cigna ACA marketplace plans.
Cigna Commercial (employer-sponsored and individual)
The standard PA policy applies. Mounjaro is covered for type 2 diabetes with PA, typically on a higher tier. The Lilly Savings Card is available if you meet the eligibility requirements. This is the most flexible group.
Cigna Medicare Part D and Medicare Advantage
Mounjaro coverage is available for the diabetes indication only — never weight loss, because federal law historically excluded weight-loss drugs from Medicare coverage. Tier, PA status, and copay vary by specific Cigna Medicare plan. Check your plan's 2026 formulary, Evidence of Coverage, or myCigna for your plan-specific details.
The 2026 Medicare Part D out-of-pocket maximum is $2,100 under CMS's Part D redesign. Once you hit that across all covered prescriptions for the year, you pay $0 for the rest of the year for covered Part D drugs. You cannot use the Lilly Mounjaro Savings Card on any Medicare plan.
What changed for Medicare GLP-1 weight-loss coverage in 2026
CMS launched the Medicare GLP-1 Bridge program, which begins July 1, 2026. The Bridge creates a Part D pathway for eligible beneficiaries using listed GLP-1 weight-reduction products including Foundayo, Wegovy, and Zepbound KwikPen — but not Mounjaro. Mounjaro remains covered under Medicare for type 2 diabetes only. If you're on Medicare and your goal is weight loss, the relevant 2026 question is whether you qualify for the GLP-1 Bridge.
Medicare Prescription Payment Plan (M3P)
You can opt into the Medicare Prescription Payment Plan, which spreads your Part D out-of-pocket cost across monthly bills instead of paying a large amount at the pharmacy counter. It helps with cash flow. It does not reduce the total amount you owe.
Cigna Medicaid managed care
Coverage varies by state Medicaid program and managed-care plan. Check your state's Medicaid preferred drug list and your specific Cigna Medicaid plan documents. The Lilly Mounjaro Savings Card is not available to Medicaid beneficiaries. If Mounjaro isn't covered by your state Medicaid program, the pharmacy benefit may cover Trulicity, Ozempic, or another GLP-1 alternative for type 2 diabetes.
Cigna ACA marketplace plans
Most marketplace plans follow the commercial PA pattern. Coverage exists for T2D. Whether the Lilly Savings Card applies depends on whether the plan is structured as commercial insurance — verify with Lilly's eligibility tool before assuming you qualify.
Cigna for TRICARE-eligible members
If you have TRICARE, the Lilly Savings Card is not available regardless of which Cigna plan administers your benefits. TRICARE has its own pharmacy benefit structure and may cover Mounjaro for T2D with PA through its pharmacy network.
What real Cigna members are dealing with
The themes below come from public discussion on r/Mounjaro and other patient communities. We use them only as voice-of-customer language — to show you that the situations you're worried about are situations real people work through. We do not use them as evidence for any medical or policy claim.
Theme 1: New plan year, new problem
A common scenario: members report that on January 1, their Cigna plan suddenly stopped covering Mounjaro — even though it was covered the day before. The fix is checking whether the new plan year removed Mounjaro from the formulary, requires a new PA, or activated a new exclusion. The Tier 2 Lilly Savings Card ($499/month for commercial insurance holders) often becomes relevant here.
Theme 2: PA required after switching insurance
Two-year Mounjaro users hit this when their employer switches insurance or they change jobs. A new insurance means a fresh PA. Your new prescriber submits with your treatment history. You typically don't need to pay a third-party service for this.
Theme 3: Quantity limit confusion
Cigna's QL on Mounjaro is typically 4 pens per 28 days — which is the standard dose. If you're being told the plan won't cover "more," it usually means the plan won't pay for more than four pens at a time, not that they won't cover Mounjaro at all.
If your real goal is weight loss, Zepbound is the right question
Same active ingredient. Different label. Cigna treats them as different drugs. If you don't have type 2 diabetes and you want tirzepatide for weight loss, Zepbound is what to ask your prescriber and your insurance about.
Typical Cigna Zepbound criteria
Under Cigna's Weight Loss – Glucagon-Like Peptide-1 Agonists Prior Authorization Policy, Zepbound coverage typically requires:
- Adult age (18+)
- BMI ≥30, or BMI ≥27 with a weight-related condition (high blood pressure, type 2 diabetes, dyslipidemia, cardiovascular disease, obstructive sleep apnea)
- Documented behavioral modification or reduced-calorie diet
- No contraindications
If your employer plan doesn't have an anti-obesity drug exclusion, this is a reasonable PA path. Confirm your plan's anti-obesity medication benefit before booking an appointment.
Zepbound cash-pay options if your plan excludes weight-loss drugs
- Zepbound through LillyDirect: Starting at $299/month for the 2.5 mg starter dose.
- Zepbound via Ro Body: Cash-pay pricing starts at $299/month for 2.5 mg, $399/month for 5 mg, and $449/month for 7.5–15 mg with on-time refills, plus the Ro Body membership fee.
Here's the cleanest path if weight loss is your real goal:
Use Ro's free GLP-1 Insurance Coverage Checker. It plugs into your specific Cigna plan and shows you whether Zepbound or Wegovy are covered. If Zepbound is covered, Ro's insurance concierge fights for the prior authorization. If it's not covered, Ro offers Zepbound as cash-pay starting at $299/month. Ro Body membership: Get started for $39, then as low as $74/month with annual plan paid upfront. Medication cost is separate.
Check Zepbound coverage free with Ro → (sponsored affiliate link, opens in a new tab)Who can actually help you get Mounjaro through Cigna?
For type 2 diabetes patients seeking Mounjaro coverage, your three best options are your existing primary care doctor or endocrinologist, Sesame Care's online providers, or a diabetes-focused telehealth service. Ro does not currently prescribe Mounjaro — Ro's Body Program is a weight-loss service that prescribes Zepbound and other FDA-approved weight-loss GLP-1 options.
Why Ro is the wrong CTA for Mounjaro (and the right CTA for Zepbound)
Ro's Body Program is for weight management. The GLP-1 medications Ro prescribes are FDA-approved for weight loss: Zepbound (tirzepatide for weight loss), Wegovy (semaglutide), and Foundayo (orforglipron). Mounjaro is FDA-approved for type 2 diabetes, and Ro does not currently offer it. If your goal is Mounjaro for type 2 diabetes, Ro isn't the right answer. If your goal is FDA-approved tirzepatide for weight loss, Ro is one of the strongest paths — they have a free insurance checker, they handle PA paperwork, and they offer cash-pay options when insurance says no.
Option 1: Your existing prescriber (best for established T2D patients)
If you already have a primary care doctor or endocrinologist managing your diabetes, they're often the strongest path for a Mounjaro PA. They have your full medical record, your A1c trend, your prior medication history. The PA submission is mostly clerical work for their office. Schedule a follow-up, hand them the PA checklist, confirm they can submit through CoverMyMeds or Cigna's provider portal, and set a calendar reminder for 11 months from now to renew before the PA expires.
Option 2: Sesame Care (best for online consultation + PA paperwork support)
Sesame Care has online providers who can prescribe Mounjaro when clinically appropriate and can assist with prior authorization paperwork. Costco members see $29 virtual primary care pricing through Sesame. Sesame's honest limitations: visits are pay-per-visit, so this works better for established T2D patients. A prescription is not guaranteed. Sesame's strength: speed and access — if your local options are weeks out, a Sesame provider can usually evaluate you within a few days.
See if a Sesame provider can help with my Mounjaro PA → (sponsored affiliate link, opens in a new tab)Option 3: A diabetes-focused telehealth service
Several telehealth companies specialize in T2D management with online endocrinology, lab review, and ongoing care. These work better than a one-off visit for newly diagnosed patients who need a full diabetes management plan, not just a single Mounjaro prescription. We cover the best options in our GLP-1 Providers That Accept Cigna guide.
A quick note on safety
Mounjaro carries a boxed warning. Insurance approval is not a substitute for a prescriber confirming the drug is right for you. Make sure your provider knows your full medical and family history before starting.
The boxed warning: Tirzepatide caused thyroid C-cell tumors in rats. It is not known whether Mounjaro causes thyroid C-cell tumors, including medullary thyroid carcinoma (MTC), in humans. Do not use Mounjaro if you or any family member has ever had MTC or if you have Multiple Endocrine Neoplasia syndrome type 2 (MEN 2).
Other serious warnings from the FDA label: Pancreatitis; hypoglycemia (especially when combined with insulin or sulfonylureas); hypersensitivity reactions; acute kidney injury; severe gastrointestinal side effects; diabetic retinopathy complications; gallbladder disease; pulmonary aspiration during anesthesia or deep sedation; risk of pen sharing (don't share pens).
Common side effects: Nausea, diarrhea, decreased appetite, vomiting, constipation, indigestion, abdominal pain. Most ease after the first few weeks.
This is not medical advice. Talk to your prescriber. If you experience severe symptoms, call your provider or 911.
What to do next, based on your situation
Pull the bucket that matches you. Each one ends with a specific next action.
Bucket A: You have type 2 diabetes and want to start Mounjaro
- Log into myCigna and confirm Mounjaro is on your formulary with PA/QL status for your specific plan.
- Get a recent A1c lab if you don't have one (within the past six months helps).
- Schedule a visit with your prescriber. Hand them the PA checklist.
- If your prescriber can't see you for weeks, a Sesame Care provider can do an online visit and submit the PA if clinically appropriate.
- Check your Lilly Mounjaro Savings Card eligibility at mounjaro.lilly.com before your first fill.
Bucket B: You want tirzepatide for weight loss (no T2D)
Mounjaro is the wrong drug for Cigna's coverage rules. Zepbound is the right question.
- Use Ro's free GLP-1 Insurance Coverage Checker to see if your Cigna plan covers Zepbound.
- If yes, Ro's insurance concierge handles the PA. Get started for $39, then as low as $74/month for Ro Body membership (medication cost is separate).
- If no, ask your prescriber about Zepbound cash-pay through LillyDirect or Ro's self-pay tirzepatide pricing.
Bucket C: You got a Mounjaro denial and need to figure out what's next
- Read the denial letter. Find the specific denial reason (see the denial decoder table above).
- If it's documentation, your prescriber resubmits with the corrected information.
- If it's a policy exclusion (off-label, plan exclusion), pivot to a covered alternative.
- If you want a clinician to evaluate and help, Sesame Care has providers who can review your case.
Bucket D: You're not sure which bucket you're in
Some readers come here knowing they want tirzepatide but uncertain whether Mounjaro or Zepbound is right for their insurance, diagnosis, and goals.
Find my GLP-1 path — free 60-second quiz →How we built this guide
We don't pretend to interpret your specific plan for you. We separate policy facts from medical facts from commercial facts, and we cite each.
Policy facts
- Cigna Diabetes GLP-1 PA Policy (CNF360, rev. 01/07/2026)
- Cigna Weight Loss GLP-1 PA Policy (CNF684)
- Cigna National Preferred 5-Tier Drug List (July 2026)
- myCigna member tools
- CMS Part D 2026 redesign and Medicare GLP-1 Bridge documentation
Medical facts
- FDA Mounjaro prescribing information (current label)
- Eli Lilly's Mounjaro patient information
Commercial facts
- Lilly Mounjaro pricing and Savings Card terms
- Ro Body Program pricing
- Sesame Care Mounjaro service pages
- GoodRx and SingleCare retail pricing (May 14, 2026)
What we did not verify: your specific plan's copay, your deductible status, your employer's drug exclusions, which pharmacy channel your plan requires, whether your prescriber will submit the PA, or whether any appeal will succeed. Those are yours to check in myCigna or by calling Cigna member services. We do not provide medical advice. We do not interpret your specific plan. We translate published policy into a workflow you can act on.
Frequently asked questions
Is Mounjaro on Cigna's formulary?
Mounjaro appears on Cigna's National Preferred 5-Tier Prescription Drug List under Diabetes with PA (prior authorization) and QL (quantity limit) flags. Whether your specific plan covers it depends on your individual benefit design — check myCigna for your plan-specific status.
Does Cigna require prior authorization for Mounjaro?
Yes, in nearly all Cigna plans. The PA may clear at the pharmacy through point-of-service logic if Cigna sees a recent oral diabetes medication claim (other than Rybelsus or single-entity metformin) within the past ~130 days and the age criterion is met. New diagnoses or no prior diabetes drug history typically trigger manual PA review.
Does Cigna cover Mounjaro for weight loss?
No. Cigna's diabetes GLP-1 policy lists Mounjaro for weight loss without type 2 diabetes as not medically necessary. If your goal is weight loss, the correct Cigna question is whether your plan covers Zepbound (same active ingredient, weight-loss label) or Wegovy.
Does Cigna cover Mounjaro for prediabetes?
No. Cigna's policy explicitly excludes prediabetes and diabetes prevention as covered uses for Mounjaro. If you have prediabetes and your goal is preventing diabetes, the standard first-line therapy is lifestyle modification and metformin.
Does Cigna cover Mounjaro for PCOS?
Not on the basis of PCOS alone. Cigna's diabetes GLP-1 policy doesn't list PCOS as an approved indication. Some PCOS patients with insulin resistance meet type 2 diabetes diagnostic criteria — in that case, they'd qualify under the T2D path. Talk to your prescriber about whether you meet T2D criteria. Never ask anyone to miscode a diagnosis.
How long does Cigna take to approve Mounjaro?
For automated approvals at the pharmacy, the decision is instant. For manual PAs, Cigna says prior authorization decisions are typically made within 5–10 business days after the request is received. Expedited review may be available within 72 hours when your prescriber documents medical urgency.
What's the Cigna Mounjaro prior authorization phone number?
PAs are typically submitted electronically by your prescriber's office through CoverMyMeds, Cigna's provider portal, or EviCore by Evernorth. For provider peer-to-peer review after a denial, the phone number is on your specific denial letter — call that number, since it can vary by plan and region.
Can I use the Mounjaro Savings Card with Cigna?
Yes, if you have commercial Cigna coverage (not Medicare, Medicaid, TRICARE, VA, or any government plan), you're age 18 or older, and your prescription is for an FDA-approved use. With Cigna covering Mounjaro, you may pay as little as $25 per fill. Without Cigna coverage but with commercial insurance, the card's second tier brings cost to $499 per fill. Annual and per-fill caps apply.
Will Cigna Medicare cover Mounjaro?
For type 2 diabetes, most Cigna Medicare Part D and Medicare Advantage plans cover Mounjaro with PA. Federal law historically excluded weight-loss drugs from Medicare, so no Medicare plan covers Mounjaro for weight loss. The 2026 Part D annual out-of-pocket maximum is $2,100. For weight-loss intent on Medicare, the new 2026 Medicare GLP-1 Bridge covers Foundayo, Wegovy, and Zepbound KwikPen — not Mounjaro — beginning July 1, 2026.
Why is my Mounjaro showing 'not covered' on Cigna's formulary check?
Three common reasons: (1) your specific plan doesn't include Mounjaro on its formulary, (2) Mounjaro is on the formulary but requires a PA you haven't filed yet, or (3) your plan has a weight-loss drug exclusion that the system is interpreting as a blanket non-coverage. Call member services for the exact reason.
Is Mounjaro a specialty drug under Cigna?
Some Cigna plans route Mounjaro through Accredo specialty pharmacy; others allow retail or home delivery. Check your plan's required pharmacy channel in myCigna before transferring your prescription.
Does Cigna require step therapy for Mounjaro?
It depends on your specific plan. Cigna's point-of-service logic uses a 130-day oral diabetes medication lookback for many plans. Some plan designs add explicit step therapy requirements. If ST appears in myCigna, ask Cigna which preferred alternatives your specific plan requires before Mounjaro.
What if my plan covered Mounjaro last year and now it doesn't?
Plan formularies change annually. Your options: (1) ask your prescriber to submit a formulary exception request, (2) switch to a covered alternative within the same drug class (Ozempic, Trulicity, or another covered GLP-1), or (3) use the Mounjaro Savings Card's second tier ($499/month for eligible commercial insurance holders without Mounjaro coverage).
Can I get Mounjaro shipped to me?
Yes, depending on your plan. If your plan routes Mounjaro through Accredo or Express Scripts home delivery, your medication ships in temperature-controlled packaging. Mounjaro pens need refrigeration on arrival, so coordinate to be home for delivery.
Why we built this page
We're The RX Index — a pricing intelligence and comparison resource for GLP-1 telehealth providers. We built this page because every "does my insurance cover Mounjaro" article we read either gave a vague "depends on your plan" non-answer or pointed readers toward providers that don't actually prescribe the drug they're asking about.
Cigna's own policy is dense, legalistic, and written for benefits administrators — not patients. So we read it carefully, mapped it against the FDA label and Lilly's pricing, and built the 130-day POS rule explainer, the approval matrix, the verification workflow, and the denial decoder that we wish existed when our team was navigating GLP-1 coverage questions.
If something here saves you an unnecessary appointment, a wasted PA submission, or a $1,000 retail pharmacy fill that you could have avoided, that's the win. If your situation doesn't match anything in our matrix, email us — we'll update the page.
Still not sure which GLP-1 program is right for you?
Take our free 60-second matching quiz. You'll get a personalized answer for your diagnosis, plan, and goals.
Find my GLP-1 path →Last verified: May 14, 2026. The RX Index is a pricing intelligence and comparison resource for GLP-1 telehealth providers. We may earn a commission from some links on this page at no additional cost to you. Our coverage facts come from Cigna's published policies, the FDA, Eli Lilly, Ro, and Sesame Care. We do not change our recommendations based on payout structure. This guide is for educational purposes only and does not constitute medical, legal, or insurance advice. Always consult your healthcare provider about treatment decisions and verify coverage details with Cigna directly.