Does Insurance Cover Mounjaro for Weight Loss?2026 Verified Guide
Disclosure: Some links on this page are affiliate links. If you purchase through these links, we may earn a commission at no extra cost to you.
Educational use only — not medical advice. Coverage depends on your specific plan, diagnosis, and prescriber documentation.Does insurance cover Mounjaro for weight loss?
Almost never on its own. Mounjaro is FDA-approved only for type 2 diabetes, so most commercial plans, all standard Medicare Part D plans, and most state Medicaid programs will not cover it when the diagnosis is “weight loss” or “obesity.” The version of tirzepatide built for weight-loss coverage is Zepbound — same active ingredient, same listed dose strengths, made by the same company, but with FDA approval for chronic weight management and for moderate-to-severe obstructive sleep apnea in adults with obesity.
Three paths actually work in 2026: (1) check your plan's Zepbound coverage with Ro's free GLP-1 Insurance Coverage Checker (no prescription needed), (2) get Zepbound direct from Eli Lilly through LillyDirect at $299–$449/month if insurance is a dead end, or (3) appeal a denial — the GAO found that 39%–59% of appealed coverage denials were reversed in states it reviewed.
✓ Find your coverage route — start here
You don't need a prescription, an appointment, or even a phone call. Pick the one that matches your situation:
Want to know if your specific plan covers Zepbound (or Mounjaro)?
Ro's team contacts your insurer by phone and emails a personalized coverage report. No commitment to start treatment. New accounts get a $50 credit if you decide to start later.
Use Ro's free GLP-1 Insurance Coverage Checker →Not sure where to begin?
Take our free 60-second matching quiz →Both options are free. Need to call your insurer right now? Jump to the verbatim phone script ↓
Why insurance won't cover Mounjaro for weight loss
The FDA approves drugs by indication, not just by molecule
Eli Lilly ran two completely separate clinical trial programs and submitted two completely separate FDA applications:
- SURPASS tested tirzepatide for blood sugar control in adults with type 2 diabetes. The FDA approved that version in May 2022 under the brand name Mounjaro.
- SURMOUNT tested tirzepatide for weight loss in adults with obesity or overweight plus a weight-related condition. The FDA approved that version in November 2023 under the brand name Zepbound. Zepbound also received FDA approval in December 2024 for moderate-to-severe obstructive sleep apnea in adults with obesity.
Same active ingredient. Same listed dose strengths. Same manufacturer. Two different brand names. Two different FDA labels. Two different “boxes” your insurer is deciding whether to check.
Why this matters for your wallet
When your prescription comes through with the diagnosis code for type 2 diabetes (E11), your plan's pharmacy benefit manager looks up Mounjaro in your formulary. If it's on the formulary for the diabetes indication, the prescription gets paid.
When the same Mounjaro prescription comes through with a diagnosis code for obesity (E66) or overweight (E66.3), the system flags it. Most plans say no. That's not a glitch — that's the system working as designed.
⚠ Important safety information
Mounjaro and Zepbound carry a boxed warning for risk of thyroid C-cell tumors, including medullary thyroid carcinoma (MTC). They are contraindicated in people with a personal or family history of MTC or Multiple Endocrine Neoplasia syndrome type 2 (MEN 2), and in anyone with a known serious hypersensitivity to tirzepatide. This page is about insurance coverage, not medical fit — your prescriber decides whether tirzepatide is appropriate for you.
Mounjaro vs. Zepbound: same active ingredient, different label, different coverage
This is the move most people miss. They keep asking their insurer about Mounjaro, hit a wall, and assume tirzepatide is just not available to them. Zepbound is the path the system was designed for — many major commercial insurers that cover any weight-loss medication will at least consider Zepbound with prior authorization.
| Mounjaro | Zepbound | |
|---|---|---|
| Active ingredient | Tirzepatide | Tirzepatide |
| Doses available | 2.5 / 5 / 7.5 / 10 / 12.5 / 15 mg | 2.5 / 5 / 7.5 / 10 / 12.5 / 15 mg |
| FDA-approved for | Type 2 diabetes (May 2022) | Chronic weight management (Nov 2023); moderate-to-severe OSA in adults with obesity (Dec 2024) |
| Manufacturer | Eli Lilly | Eli Lilly |
| Insurance pathway for weight loss | Almost never covered | Often covered with prior authorization (varies by plan) |
| Insurance pathway for diabetes | Often covered with prior authorization | Not approved for diabetes |
| List price | $1,112.16/fill | List price varies by formulation |
| Manufacturer savings card | $25/month with T2D diagnosis (commercial insurance) | $25/month for FDA-approved Zepbound use (commercial insurance) |
| Direct-pay option through Lilly | Not available at reduced direct-pay prices | LillyDirect Self Pay: $299–$449/month |
Insurance coverage by payer (verified 2026 snapshot)
The Mounjaro Coverage Route Matrix (2026)
| Your situation | Usually covered for weight loss? | Better question to ask | What to verify |
|---|---|---|---|
| Commercial / employer plan + type 2 diabetes | Often yes (for T2D, not weight loss) | “Is Mounjaro covered for my diabetes diagnosis, and what PA criteria apply?” | Tier, PA, step therapy, A1C, metformin history |
| Commercial / employer plan + weight loss only (no T2D) | Almost never | “Does my plan cover Zepbound, Wegovy, or another obesity-labeled medication?” | Weight-loss benefit, BMI/comorbidity criteria, exclusions |
| Mounjaro is on your formulary | Not enough by itself | “Is Mounjaro covered for my specific diagnosis code?” | Diagnosis restrictions, PA criteria |
| Employer plan excludes weight-loss drugs | Appeal is low-probability | “Is there a medical exception process or alternative covered indication?” | HR benefits doc, exclusion language |
| ACA Marketplace plan | Plan-dependent | “Does this specific plan cover obesity medications?” | Formulary, EHB rules, exclusions |
| Medicare Part D (standard) | No — federal law excludes weight-loss drugs | “Is there an FDA-approved indication my plan does cover?” | Formulary, diagnosis, OSA/CV exceptions |
| Medicare GLP-1 Bridge (July 1, 2026 – Dec 31, 2027) | Mounjaro NOT on eligible products list | “Am I eligible for a Bridge-covered obesity GLP-1?” | BMI/comorbidity criteria, central PA; Bridge covers Foundayo, Wegovy, Zepbound KwikPen only |
| Medicaid | Varies by state | “Does my state’s Medicaid PDL cover obesity GLP-1s?” | State preferred drug list, managed care PA |
| TRICARE | Listed for diabetes, not weight management | “Does my TRICARE plan cover Zepbound or Wegovy for weight management?” | Plan type, PA, exclusion groups |
| No insurance / cash pay | Insurance won’t help | “Should I compare LillyDirect Zepbound before paying retail Mounjaro?” | Coupon eligibility, branded alternatives, direct-pay |
The numbers behind the table (2026 employer reality)
- 36% of U.S. employers cover GLP-1 medications for both diabetes and weight loss in 2025, up from 34% in 2024 (IFEBP 2025 Pulse Survey, reported by SHRM).
- 55% of employers cover GLP-1s for diabetes only.
- GLP-1 medications now represent an average of 10.5% of total annual prescription claims at employers covering them, up from 6.9% in 2023.
2026 commercial payer changes worth knowing
The five denial patterns (memorize this list)
- “Mounjaro is on my formulary” — Formulary listing isn't the same as diagnosis approval. Ask whether coverage is restricted to type 2 diabetes.
- “Prior authorization required” — This isn't a denial yet. Your prescriber needs to submit clinical notes, labs, and treatment history.
- “Step therapy required” — Your plan wants you to try a less-expensive medication first. Document failures or intolerance to overcome this.
- “Plan excludes weight-loss drugs” — A true benefit exclusion. Appeals are low-probability. Switch to LillyDirect or appeal with a different indication if applicable.
- “Quantity limit exceeded” — Usually a pharmacy processing issue. Have your prescriber rewrite the script.
✓ Already know Zepbound is your path? Get started with insurance support
Ro Body's program costs $39 for the first month, then $149/month — or as low as $74/month with annual prepay. Medication billed separately. Ro's insurance concierge handles prior authorization paperwork directly with your plan; if your plan won't cover Zepbound, you can switch to LillyDirect cash pricing through the same membership (Ro matches LillyDirect, NovoCare, and TrumpRx prices on medication).
Honest tradeoff: Ro's insurance concierge generally does not coordinate with most government insurance plans — Medicare, Medicaid, and TRICARE — with Federal Employees Health Benefits (FEHB) as the main exception. See the Medicare and TRICARE sections below if that's your situation.
See if you qualify for Ro Body's GLP-1 program with insurance concierge included →Will insurance cover Mounjaro if I don't have type 2 diabetes?
Including prediabetes, PCOS, insulin resistance
Diagnoses that sometimes (rarely) work for off-label coverage
- Prediabetes (HbA1c 5.7–6.4%) — Some plans recognize this with other risk factors documented. Many won't.
- Polycystic ovarian syndrome (PCOS) with insulin resistance — A handful of plans have PCOS coverage clauses, but it's far from universal.
- Strong cardiovascular risk — Documented hypertension, dyslipidemia, prior cardiovascular events.
- Severe obesity (BMI ≥40) with multiple comorbidities — Some plans treat this as a metabolic disease pathway.
Even with these diagnoses, your plan can deny, your appeal can fail, and you'll have spent weeks chasing it. The cleaner play in almost every situation is to ask your prescriber for Zepbound instead.
Why your prescriber may push back on Mounjaro for weight loss
- Zepbound is FDA-approved for the actual goal. Prescribing within the label is cleaner clinically and from an insurance standpoint.
- Coverage is more likely. Even with prior authorization, Zepbound has a real pathway. Mounjaro for weight loss often doesn't.
- Insurer audit risk. Persistent off-label prescribing of Mounjaro for weight loss can flag a clinic for insurer audits.
“Should I tell my doctor I have diabetes to get Mounjaro covered?”
No. That's healthcare fraud, and it puts both you and your prescriber at risk. The honest path — asking for Zepbound for the actual indication of weight loss — is faster, more likely to succeed, and doesn't put your medical record or your prescriber's license in jeopardy.
The Mounjaro Savings Card and weight loss: read the fine print
Eli Lilly's Mounjaro Savings Card is for eligible commercially insured patients with a type 2 diabetes prescription. Government beneficiaries (Medicare, Medicaid, TRICARE, VA) are not eligible. In practice, some pharmacies process it on off-label weight-loss prescriptions — but this is inconsistent. The honest read: if you don't have type 2 diabetes, plan as though the Mounjaro Savings Card won't work. Use the Zepbound Savings Card instead — eligible commercially insured patients whose plan covers Zepbound single-dose pen may pay as little as $25/fill for an FDA-approved use.
What Mounjaro actually costs without insurance
| Path | Monthly cost | Who qualifies |
|---|---|---|
| Mounjaro retail (no insurance, no card) | ~$1,000–$1,300 | Anyone with a prescription |
| Mounjaro Savings Card (commercial insurance + T2D diagnosis) | As low as $25 | Commercial insurance + T2D + plan covers Mounjaro |
| Zepbound Savings Card (commercial covers Zepbound, FDA-approved use) | As low as $25 | Commercial insurance + plan covers Zepbound |
| LillyDirect Zepbound Self Pay — 2.5 mg vial or KwikPen | $299 | Valid prescription; verify eligibility through LillyDirect |
| LillyDirect Zepbound Self Pay — 5 mg | $399 | Same |
| LillyDirect Zepbound Self Pay — 7.5/10/12.5/15 mg (45-day refill rule) | $449 | Same — must refill within 45 days to keep this price |
| LillyDirect Zepbound KwikPen (off-program / missed refill) | $499–$699 | Price escalates if 45-day window is missed |
The 45-day refill window matters for higher doses. For 7.5 mg, 10 mg, 12.5 mg, and 15 mg, you have to refill within 45 days of your previous delivery to keep the $449/month Self Pay Journey Program price. Set a calendar reminder for day 30–35 after each shipment and this never matters.
Single-dose vials require drawing the medication with a syringe. It's a simple technique your prescriber can show you. The KwikPen is a pre-filled multi-dose pen — simpler, but priced separately. Both deliver the same FDA-approved Zepbound.
Medicare and Medicaid: the rules are different (and changing in July 2026)
Why federal law currently blocks Medicare weight-loss coverage
The Medicare Modernization Act of 2003 explicitly excludes drugs “when used for weight loss” from Part D coverage. That's been the rule for over two decades.
| Drug & indication | Medicare Part D coverage |
|---|---|
| Mounjaro for type 2 diabetes | Covered (subject to formulary, tier, PA, step therapy) |
| Mounjaro for weight loss | Not covered. Period. |
| Zepbound for weight loss alone | Not covered by standard Part D |
| Zepbound for moderate-to-severe OSA in adults with obesity | May be covered when criteria are met (different FDA indication than weight loss) |
| Wegovy for cardiovascular risk reduction in adults with overweight/obesity and established CV disease | May be covered when criteria are met (different FDA indication than weight loss) |
What changes on July 1, 2026: the Medicare GLP-1 Bridge
CMS launched the Medicare GLP-1 Bridge as a short-term demonstration running from July 1, 2026 through December 31, 2027. It operates outside normal Part D payment flow.
- Eligible products: All formulations of Foundayo (orforglipron), all formulations of Wegovy (injection and tablet), and Zepbound KwikPen. Mounjaro is not on the list. Zepbound single-dose vials and pens are not included — KwikPen only.
- Beneficiary copay: $50/month for qualifying beneficiaries.
- Eligibility criteria (plus one):
- BMI ≥35, or
- BMI ≥30 with HFpEF (heart failure with preserved ejection fraction), uncontrolled hypertension despite two antihypertensives, or chronic kidney disease stage 3a or higher, or
- BMI ≥27 with prediabetes, previous heart attack, previous stroke, or symptomatic peripheral artery disease.
Medicaid: 13 states cover obesity GLP-1s (under fee-for-service)
As of January 2026, KFF reported that 13 state Medicaid programs covered GLP-1s for obesity treatment under fee-for-service (KFF BALANCE Model overview). Coverage can differ by state, managed-care arrangement, preferred drug list, and whether a state opts into Medicaid BALANCE participation starting May 2026.
Verbatim script for your state Medicaid pharmacy line:
“Hi, I'd like to verify GLP-1 medication coverage on my Medicaid plan. Specifically: (1) Is Mounjaro on the preferred drug list for type 2 diabetes? (2) Is Zepbound or Wegovy on the preferred drug list for weight management or obesity treatment? (3) What are the prior authorization criteria for each? (4) Is there a difference between fee-for-service and managed care coverage for GLP-1s in this state?”
Does TRICARE cover Mounjaro for weight loss?
Three things to verify on a TRICARE call:
- Plan type: TRICARE Prime, Select, For Life, Reserve Select, Retired Reserve, US Family Health Plan — the rules differ.
- PA criteria: Most weight-loss medications require prior authorization documenting BMI, comorbidities, and prior weight-loss attempts.
- Exclusion language: Some TRICARE coverage groups don't have a weight-loss medication benefit at all, regardless of PA approval.
For 2026, TRICARE Pharmacy Home Delivery brand-name formulary copays are $44 for up to a 90-day supply for most non-active-duty beneficiaries (TRICARE 2026 pharmacy costs). Verify your specific drug's formulary tier before relying on that figure. If your goal is weight loss, the cleanest path on TRICARE is a Zepbound prior authorization, not a Mounjaro one.
How to find out exactly what your plan covers
Step 1 — Find your plan's formulary online
Log in to your insurance member portal. Search for: “tirzepatide”, “Mounjaro”, and “Zepbound”. For each, note:
- Whether it's listed at all
- What tier it's on (Tier 1 is cheapest, Tier 4 / specialty is most expensive)
- Whether it has a “PA” flag (prior authorization required) or “ST” flag (step therapy)
- Any quantity limits
Step 2 — Call member services with this script
“Hi, I'd like to verify coverage for two specific medications. First, Mounjaro — generic name tirzepatide — prescribed for weight loss. Second, Zepbound, also tirzepatide, prescribed for weight loss. For each one, I need to know: (a) is it on my formulary, (b) what tier it's on, (c) does it require prior authorization or step therapy, (d) what my expected copay or coinsurance would be, and (e) is there a quantity limit. I'd also like to know whether my plan has a weight-loss drug exclusion or any specific BMI or comorbidity criteria. Could I get a reference number for this call?”
That last line — the reference number — matters. If you ever need to appeal, you'll cite it.
Step 3 — Use a free third-party coverage checker (highest-value step)
Ro's GLP-1 Insurance Coverage Checker is free. Their team contacts your insurer by phone and sends a personalized coverage report by email telling you exactly which GLP-1 medications your plan covers, whether each requires prior authorization, and the estimated copay. No prescription required. New accounts get a $50 credit if you decide to start treatment later.
✓ Use Ro's free GLP-1 Insurance Coverage Checker →Step 4 — Have your prescriber's office run a benefits check
Most clinics will run a benefits check for free during your appointment. Bring your insurance card and pharmacy benefit ID. Ask specifically about:
- Whether your prescriber's preferred medication (typically Zepbound for weight loss) is on your formulary
- The PA submission window — Ro states its full insurance process can take about 2–3 weeks
- Any forms the office needs to send the insurer
If you're denied: the 4-step appeal playbook
The Mounjaro Denial Decoder
| Denial language on your letter | What it actually means | Best next step |
|---|---|---|
| “Prior authorization required” | Plan needs your prescriber to submit documentation. Not a final denial yet. | Have your prescriber submit the PA with diagnosis, labs, and treatment history. |
| “Not medically necessary” | Specific clinical criteria weren’t documented. | Request the exact criteria in writing; have your prescriber address each one. |
| “Diagnosis not covered” | Plan restricts Mounjaro to type 2 diabetes specifically. | If your goal is weight loss, switch the request to Zepbound and start a new PA. |
| “Step therapy required” | Plan wants you to try a less-expensive medication first. | Document trials of preferred meds (often metformin, Wegovy, or Saxenda) including dates, dosages, and reasons for failure or intolerance. |
| “Weight-loss drugs excluded” | True benefit exclusion in your employer’s plan. | Appeals are low-probability. Ask HR about medical exception process; otherwise consider LillyDirect cash pay. |
| “Quantity limit exceeded” | The prescription quantity exceeds the plan’s per-fill limit. | Have your prescriber rewrite the script with the correct quantity. |
| “Coupon not accepted” | Usually a government-insurance issue — Medicare/Medicaid/TRICARE patients can’t use manufacturer copay cards. | Switch to LillyDirect cash pay or pursue a different coverage pathway. |
Step 1 — Read the denial letter and find your deadline
Every denial letter must include the specific reason, your appeal rights, and the deadline to file. Most commercial plans give you 180 days; some give as few as 60–65. Find the deadline on your specific denial letter and mark it on your calendar today. Missing it means you can't appeal at all.
Step 2 — Gather the right clinical evidence
This is where most appeals win or lose. Have your prescriber provide:
- Current BMI and weight history (specific numbers, not “obesity”)
- Comorbidities with ICD-10 codes — hypertension (I10), dyslipidemia (E78.x), prediabetes (R73.03), sleep apnea (G47.33), PCOS (E28.2), prior cardiovascular events
- Recent lab results — A1C, lipid panel, fasting glucose, blood pressure history
- Medication history — every weight-loss medication or GLP-1 previously tried, with dates, dosages, and outcomes
- Documented diet and exercise history — many plans require evidence of a structured program for at least 6 months prior to GLP-1 prescription
- Clinical notes explaining medical necessity — your prescriber's written argument for why this specific medication is appropriate
Step 3 — Request a peer-to-peer review
A peer-to-peer is a phone call between your prescriber and the insurer's medical reviewer. Often the fastest way to overturn a denial. Have your prescriber prepare a 2–3 sentence summary of medical necessity before the call. Many denials are reversed in under 30 minutes once the prescribing clinician explains the case directly to a reviewer.
Step 4 — Submit a structured appeal letter
Every effective appeal letter includes:
- Patient identification — name, member ID, DOB, plan name, claim/PA reference number
- Reference to the denial — date of denial, exact denial reason as written
- Statement of the requested medication and indication — “Zepbound (tirzepatide) prescribed for chronic weight management”
- Direct response to each denial reason with clinical evidence
- Clinical evidence attached — BMI, comorbidities with ICD-10 codes, labs, prior medication trials, lifestyle history
- Citation of FDA labeling for the requested medication's FDA-approved indication
- Specific request — “I am requesting reconsideration of the denial and approval of Zepbound coverage”
- Prescriber signature and contact information
When the appeal still fails: three fallback paths
- External review. State law requires an independent third-party review for most insurance denials after internal appeals are exhausted. Your denial letter will include instructions. Timelines run 30–60 days.
- Switch to LillyDirect cash pay. $299–$449/month for Zepbound. You can submit an HSA/FSA reimbursement request even though insurance isn't paying.
- Talk to your prescriber about other GLP-1s your plan does cover. Some plans cover Wegovy when they don't cover Zepbound, and vice versa. Saxenda (daily liraglutide injection) is sometimes covered when newer GLP-1s aren't.
The cheaper path: Zepbound through LillyDirect at $299–$449
What you actually get
- Same FDA-approved Zepbound as anything you'd get at retail. Manufactured by Eli Lilly. No compounded substitutes.
- Available as single-dose vials (require drawing the dose with a syringe — a 30-second technique your prescriber can demonstrate) or KwikPen (multi-dose pre-filled pen).
- Shipped to your home — typically 1–4 days from order to delivery.
- HSA and FSA eligible when prescribed by a healthcare provider.
- Available through Ro — Ro matches LillyDirect prices on Zepbound (vial and KwikPen) and adds an insurance concierge if you want to try insurance first.
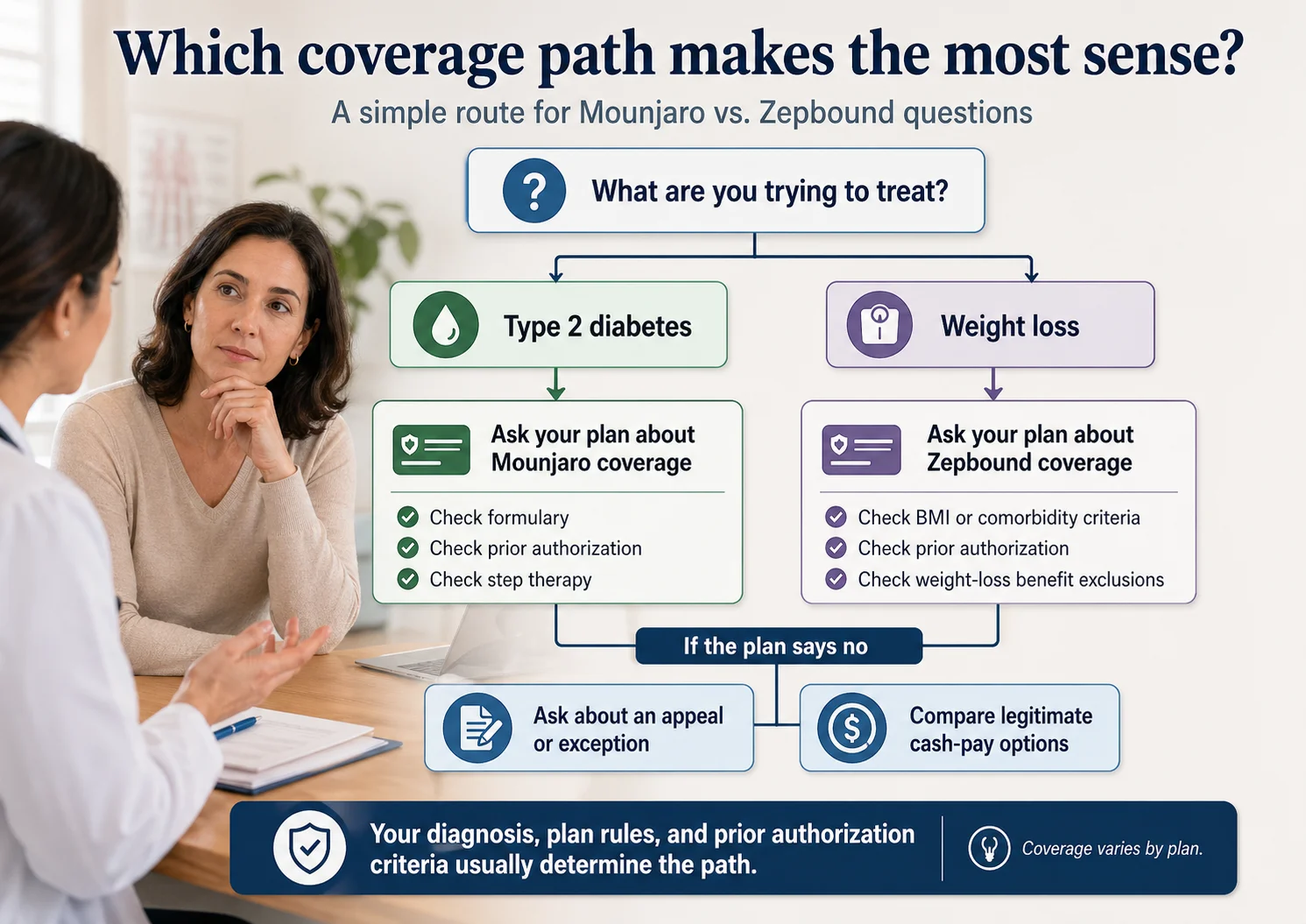
Your diagnosis, plan rules, and prior authorization criteria usually determine the path. Coverage varies by plan.
LillyDirect vs. Ro: which is the right route?
| LillyDirect direct | Ro Body | |
|---|---|---|
| Medication price | $299/$399/$449 (Zepbound, Self Pay Journey terms) | Matches LillyDirect for cash pay |
| Membership/program fee | None | $39 first month, $149/mo or as low as $74/mo with annual prepay |
| Insurance handling | None — cash pay only | Full insurance concierge for commercial insurance (FEHB included; most other government plans not supported) |
| Prior authorization help | None | Yes, handled for you |
| Provider visit | Required (use any prescriber, or LillyDirect can connect to telehealth) | Included in membership |
| Best for | “I just want the medication, cash pay, no fuss” | “I want to try insurance first, with help” |
✓ Three honest tradeoffs before you decide
- Even Zepbound coverage is being narrowed by major payers in 2026, not expanded. BCBS Massachusetts, Independence Blue Cross, and FEP Blue have all tightened criteria. If you have one of those plans, expect the LillyDirect path to matter more than the insurance path.
- The Mounjaro Savings Card officially requires a type 2 diabetes diagnosis. Don't plan as if it'll work for weight-loss patients. Use the Zepbound Savings Card or LillyDirect instead.
- LillyDirect's $299–$449/month is genuinely affordable but it's still a recurring cost. In SURMOUNT-4, participants who switched from tirzepatide to placebo after initial weight loss regained weight, while those who continued tirzepatide maintained their weight loss or lost more (JAMA SURMOUNT-4). Plan for the long term and discuss duration with your prescriber.
What real people get wrong about Mounjaro coverage
“My formulary says Mounjaro is covered, so why was I denied?”
A formulary listing tells you the drug is on the plan’s covered drug list. It doesn’t tell you the plan will cover it for your diagnosis. Most plans restrict Mounjaro coverage to type 2 diabetes through prior authorization. Ask the plan, in writing, what diagnoses Mounjaro is covered for on your specific plan.
“My friend pays $25. Why am I seeing $1,000?”
Five possibilities: (1) they have type 2 diabetes and use the Mounjaro Savings Card; (2) they have a better commercial insurance plan; (3) they’re filling Zepbound, not Mounjaro, with the Zepbound Savings Card; (4) they’re paying through LillyDirect for Zepbound; (5) they have an employer-sponsored plan with expanded obesity coverage. You can’t replicate path 1 without a T2D diagnosis. You can replicate paths 2–5 with the steps in this guide.
“My doctor prescribed it. Doesn’t insurance have to cover it?”
No. Prescribing authority and insurance benefit design are separate systems. A doctor can write any legal prescription; your plan can still deny coverage based on its own written criteria. Your appeal needs to target the plan’s written criteria, not your doctor’s clinical opinion.
“What if my insurance changes mid-year?”
Plans can change formularies any time, but they’re required to give you advance notice of material changes. Watch for letters from your plan around January 1 and July 1. If a covered medication becomes excluded mid-year, “continuity of therapy” exception requests are possible — ask your prescriber to submit one before your supply runs out.
What we actually verified for this guide
Here's exactly what we checked, where, and when. If you find anything outdated, email us at research@therxindex.com and we'll re-verify.
| Fact | Source | Last checked |
|---|---|---|
| Mounjaro FDA label and indication (type 2 diabetes) | FDA Mounjaro label | |
| Zepbound FDA label and indications (weight management; OSA in adults with obesity) | FDA Zepbound label | |
| Mounjaro list price ($1,112.16/fill) | Lilly Mounjaro pricing page | |
| Mounjaro Savings Card terms (T2D required, $25 with commercial coverage, government beneficiaries excluded) | Lilly Mounjaro savings page | |
| Zepbound Savings Card terms ($25 with coverage for FDA-approved use; government beneficiaries excluded) | Lilly Zepbound savings page | |
| LillyDirect Zepbound Self Pay Journey Program prices ($299/$399/$449 with 45-day refill rule) | Lilly Self Pay Journey terms | |
| Medicare GLP-1 Bridge timeline (July 1, 2026 – Dec 31, 2027) and eligible products | CMS Medicare GLP-1 Bridge | |
| Medicaid GLP-1 obesity coverage (13 states under fee-for-service, January 2026) | KFF BALANCE Model overview | |
| TRICARE coverage of Mounjaro (T2D), Zepbound, Wegovy, Saxenda; 2026 Home Delivery copay ($44/90 days) | TRICARE Wegovy/Zepbound FAQ | |
| BCBS Massachusetts 2026 GLP-1 weight-loss exclusion at plan renewal | BCBS Massachusetts GLP-1 update | |
| IBX 2025 weight-loss-only GLP-1 exclusion (still in effect for 2026) | IBX provider communication | |
| Aetna Zepbound PA criteria (6-month comprehensive program) | Aetna Clinical Policy Bulletin 0039 | |
| Employer GLP-1 coverage stats (36% cover both; 55% diabetes only; 10.5% of total claims) | SHRM / IFEBP 2025 Pulse Survey | |
| Internal appeal success rate (39%–59%, GAO 2011 general health insurance data) | GAO report | |
| Ro Body program pricing and coverage checker (free, contacts insurer by phone, $50 credit) | Ro pricing; Ro insurance page | |
| SURMOUNT-4 weight regain after tirzepatide discontinuation | JAMA SURMOUNT-4 |
We re-verify pricing, savings-card terms, and CMS Bridge specifics monthly. Payer policies and employer survey data, quarterly.
Frequently asked questions
Does insurance cover Mounjaro for weight loss in 2026?
Almost never on its own. Mounjaro is FDA-approved only for type 2 diabetes, so most insurance plans won’t cover it for a weight-loss-only diagnosis. The version of tirzepatide that insurance is set up to cover for weight loss is Zepbound, the FDA-approved-for-weight-management brand of the same molecule, made by the same company.
Will insurance cover Mounjaro if I don’t have diabetes?
It’s very rare. A small minority of self-funded employer plans with expanded obesity-care benefits may cover off-label Mounjaro for weight loss with prior authorization. If your goal is weight loss and you don’t have type 2 diabetes, the practical path is to ask your prescriber for Zepbound instead.
What’s the difference between Mounjaro and Zepbound for insurance purposes?
Mounjaro and Zepbound contain the same active ingredient (tirzepatide) at the same listed dose strengths. Mounjaro is FDA-approved for type 2 diabetes; Zepbound is FDA-approved for chronic weight management and for moderate-to-severe obstructive sleep apnea in adults with obesity. Insurance plans cover medications based on FDA-approved indications.
Can I use the Mounjaro Savings Card for weight loss?
Per Eli Lilly’s official terms, the Mounjaro Savings Card requires a type 2 diabetes prescription and excludes government beneficiaries. If you don’t have type 2 diabetes, plan as though the savings card won’t apply. Use the Zepbound Savings Card instead for an FDA-approved Zepbound use.
What BMI do I need for Zepbound to be covered?
Most commercial plans require BMI ≥30 (obesity), or BMI ≥27 with at least one weight-related condition like hypertension, dyslipidemia, prediabetes, or sleep apnea. Some plans set stricter thresholds — certain Blue Shield California 2026 plans limit coverage to Class III obesity (BMI ≥40) plus participation in a structured program. Always verify the exact criteria in writing for your specific plan.
Does Medicare cover Mounjaro for weight loss?
No. Federal law prohibits Medicare Part D from covering drugs used solely for weight loss. Mounjaro is covered by Medicare Part D only for type 2 diabetes. The Medicare GLP-1 Bridge running from July 1, 2026 to December 31, 2027 will cover certain weight-loss GLP-1s at $50/month for qualifying beneficiaries — but Mounjaro is not on the eligible products list (Foundayo, Wegovy, and Zepbound KwikPen are).
What are the Medicare GLP-1 Bridge eligibility criteria?
An adult Medicare beneficiary prescribed an eligible GLP-1 for excess body weight reduction with ongoing lifestyle modification, plus one of these clinical scenarios: BMI ≥35; or BMI ≥30 with HFpEF, uncontrolled hypertension despite two antihypertensives, or chronic kidney disease stage 3a or higher; or BMI ≥27 with prediabetes, previous heart attack, previous stroke, or symptomatic peripheral artery disease.
Does Medicaid cover Mounjaro for weight loss?
It varies by state. Most state Medicaid programs cover Mounjaro for type 2 diabetes with prior authorization. As of January 2026, KFF reports that 13 state Medicaid programs covered GLP-1s for obesity treatment under fee-for-service. Coverage for Mounjaro for weight loss specifically is rare.
How much does Mounjaro cost without insurance in 2026?
The list price is $1,112.16 per fill per Eli Lilly’s pricing page. Retail pharmacy cash prices typically run $1,000–$1,300/month. The cheapest legitimate path for tirzepatide weight loss is Zepbound through LillyDirect at $299/month (2.5 mg), $399/month (5 mg), or $449/month (7.5–15 mg) when Self Pay Journey Program terms are met.
What if my insurance covers Zepbound but not Mounjaro for weight loss?
That’s the expected outcome on most commercial plans, and it’s the correct path. Have your prescriber write the prescription for Zepbound, not Mounjaro. They contain the same active ingredient at the same listed dose strengths; the prior authorization will use your weight-loss indication.
What happens if I stop taking Mounjaro or Zepbound?
In SURMOUNT-4, participants who switched from tirzepatide to placebo after initial weight loss regained weight, while those who continued tirzepatide maintained their weight loss or lost more. Clinical guidelines now treat obesity as a chronic condition that may require long-term medication. Discuss duration of therapy with your prescriber before stopping.
Is there a way to get tirzepatide for less than $299/month legitimately?
For FDA-approved branded tirzepatide (Mounjaro or Zepbound), $299/month for the 2.5 mg starting dose through LillyDirect is the lowest verified legitimate price as of April 2026. Compounded tirzepatide is a separate category with different regulatory status and is outside the scope of this guide.
Final answer + your next step
Bottom line: Insurance almost never covers Mounjaro for weight loss because Mounjaro is FDA-approved only for type 2 diabetes. The version of tirzepatide that insurance is set up to cover for weight loss is Zepbound — same active ingredient, same listed dose strengths, made by the same company, but with the FDA approval insurance plans actually look for. Your fastest next step is to verify your plan's Zepbound coverage (free, via Ro), or get Zepbound direct from Lilly at $299–$449/month if insurance is a dead end.
Three honest paths from here:
1. Verify your Zepbound coverage for free
Ro's team contacts your insurer for you and emails a personalized coverage report. No prescription required.
Use Ro's free GLP-1 Insurance Coverage Checker →2. Skip insurance entirely
LillyDirect Zepbound Self Pay at $299/$399/$449/month. Same FDA-approved Zepbound, direct from Eli Lilly, no PA, no formulary fights.
Go to LillyDirect Zepbound Self Pay →3. Compare all FDA-approved GLP-1 options with provider choice
Sesame Care's weight-loss program starts at $59/month with annual subscription and includes provider visits, labs, and access to FDA-approved branded GLP-1 options including Zepbound, Wegovy, Ozempic, and Foundayo (medication pricing varies by drug, dose, insurance, and cash-pay route).
Compare FDA-approved GLP-1 options on Sesame Care →🎯 Still not sure which GLP-1 program is right for you?
Take our free 60-second matching quiz →