Last verified: April 22, 2026 · Formulary documents reviewed · Lilly pricing confirmed · Ro workflow confirmed
Insurance Coverage Guide · April 22, 2026
Does Blue Cross Cover Foundayo? (2026 BCBS Coverage, Costs & Next Steps)
Published:
By The RX Index Editorial Team · Last verified: April 22, 2026
The short answer, before you scroll
Sometimes — and it depends entirely on which Blue Cross plan you actually have. “Blue Cross” is not one company. Blue Cross Blue Shield is an association of 34 independent, locally operated BCBS companies, and in 2026 they’ve split into four very different camps on whether they’ll cover Foundayo (orforglipron), the once-daily oral GLP-1 pill that received FDA approval on April 1, 2026.
- FEP Blue (federal employee/postal): weight-loss drugs are coverable for eligible members with prior approval, and a formulary-exception path exists for non-listed drugs.
- Excellus BCBS (upstate NY): their drug policy was updated April 13, 2026 and explicitly names Foundayo in the weight-management criteria — the best public signal in the Blue system.
- BCBS Massachusetts “Focused” formulary: obesity GLP-1s are flatly excluded with no medical-necessity review available. Foundayo will almost certainly not be covered.
- Employer-elected plans (Premera, BCBSND large-group, most Anthem commercial, HCSC): your employer’s benefit election often decides the answer before anyone looks at the drug.
If your plan does cover it, you may pay as low as $25/month using the Foundayo Savings Card. If it doesn’t, self-pay through Ro or LillyDirect starts at $149/month for the 0.8 mg starting dose — a real change from the four-figure monthly tags that defined branded GLP-1s for years.
Your fastest next step (commercial BCBS and FEP members)
The cleanest way to find out whether your specific Blue Cross plan covers Foundayo — without a doctor visit, without a 40-minute hold queue — is Ro’s free GLP-1 Insurance Coverage Checker. Ro contacts your insurer on your behalf and emails you a personalized GLP-1 coverage report showing coverage status and prior-authorization requirements. No charge, no obligation.
Check your Blue Cross Foundayo coverage free with Ro → (sponsored affiliate link, opens in a new tab)For commercial Blue Cross and FEP Blue members. Medicare Advantage/Part D members: see the Medicare section below.
Blue Cross Foundayo quick verdict table
| Your Blue Cross situation | Likely Foundayo outcome in 2026 |
|---|---|
| FEP Blue (federal employee / postal) | Coverable for eligible members with prior approval; formulary-exception path available |
| Excellus BCBS (upstate NY) | Strongest public Foundayo signal — drug is named in the weight-management policy |
| BCBSMA Focused Formulary | Excluded; no medical-necessity review available |
| Employer-elected plan (most Anthem, Premera, HCSC, BCBSND large-group) | Depends on whether your employer bought the GLP-1 benefit |
| Blue Cross Medicare Advantage / Part D | Not now, but July 1, 2026: CMS Medicare GLP-1 Bridge launches ($50/month fixed — see below) |
Last verified April 22, 2026. Formularies change monthly; we update this page on the same cadence.
Does Blue Cross cover Foundayo? The four-bucket answer
Four buckets cover almost every BCBS member. Figure out which bucket you’re in before you do anything else — it changes the next step entirely.

Bottom line: Blue Cross coverage for Foundayo depends on your affiliate, formulary, and employer benefit design. Best next step: verify your specific plan before assuming yes or no.
Bucket 1: FEP Blue (federal and postal employees)
If your card says “Federal Employee Program,” “FEP Blue Standard,” “FEP Blue Basic,” or “FEP Blue Focus,” you’re in the strongest general-coverage camp for obesity GLP-1s in the Blue system.
FEP Blue publicly states that weight-loss drug prescriptions are coverable for eligible members who obtain prior approval, and excluded or not-covered weight-loss GLP-1s can still move through a formulary-exception process. That language matters: it’s not “weight-loss drugs are excluded full stop” — it’s “most weight-loss drugs need pre-approval, and even the ones that aren’t on the list have a documented way in.”
Tier context: Wegovy is listed at Tier 3 for FEP Blue Standard and Basic, and is not covered on FEP Blue Focus (base formulary). Approved-exception Zepbound sits at Tier 3 for Standard/Basic; approved-exception Wegovy and Zepbound sit at Tier 2 Preferred for Focus. Foundayo-specific tier placement is not yet visible in the 2026 FEP Blue abbreviated formulary as of April 22, 2026 [NEEDS VERIFICATION] — that’s not unusual for a drug approved three weeks ago.
Practical read: don’t assume no. Your plan has both a standard coverage path and an exception path. If Foundayo isn’t formally listed when you check, your prescriber can submit a non-formulary exception request.
Bucket 2: Excellus BCBS (upstate New York)
Excellus BCBS — serving Rochester, Syracuse, Utica, and Binghamton — has the strongest public Foundayo signal we’ve found from any Blue affiliate. Their weight-management drug policy, updated April 13, 2026 — twelve days after FDA approval — explicitly names Foundayo alongside Wegovy, Zepbound, Saxenda, and Qsymia.
The Excellus criteria are clinically strict: Class III obesity (BMI ≥40) or Class II obesity (BMI 35–39.9) with at least one qualifying comorbidity. Initial coverage runs seven months, and recertification requires documented 5% weight loss. Foundayo specifically is limited to fourteen 30-day supplies or five 90-day supplies on approved therapy.
Practical read: this is probably the cleanest Foundayo coverage path in the Blue system right now. Your criteria are strict, but the drug is explicitly in scope.
Bucket 3: BCBSMA on the Focused Formulary (and similar explicit exclusions)
BCBSMA operates two commercial formularies. The standard BCBSMA formulary includes GLP-1 coverage per obesity medical policy 572 where employer benefit design includes anti-obesity drugs. The BCBSMA Focused Formulary excludes FDA-approved GLP-1 and GLP-1/GIP medications used for weight loss — and states plainly that the medical-necessity review process is not available for these excluded weight-loss GLP-1s.
That’s the meaningful detail. It’s not “submit an appeal and we might say yes.” It’s “the exception route doesn’t exist for this category under this formulary.”
Practical read: check which formulary your plan uses first. If it’s the standard formulary and your employer elected weight-loss drug coverage, you have a path via policy 572. If it’s Focused, Foundayo is almost certainly a commercial cash-pay decision.
Similar category-level exclusions exist at:
- BCBS North Dakota — fully-insured non-grandfathered large-group plans removed weight-loss drug coverage effective January 1, 2026.
- Blue Cross Blue Shield of Michigan — ended GLP-1 weight-loss coverage for fully-insured large-group commercial members in 2025.
- Blue Shield of California — weight-loss drugs excluded since January 1, 2025, except for Class III (morbid) obesity with documented criteria.
- California Medi-Cal (including Anthem managed care) — removed Wegovy, Zepbound, and Saxenda from the Contract Drugs List effective January 1, 2026.
Already know you’re in a true exclusion bucket? Take our 60-second GLP-1 matching quiz if you want a personalized path to an oral or injectable GLP-1 program that fits your situation.
Bucket 4: Employer-elected plans
This is the large commercial bucket where the Blue name on your card matters least. If you have an Anthem plan (14 states), a Premera plan (WA, AK), an HCSC plan (IL, TX, OK, NM, MT), Highmark (PA, DE, WV), Florida Blue, Blue Cross NC, or most other mid-size regional Blues — your employer’s benefit election is the deciding factor.
Premera states the rule most clearly: when an employer has elected the obesity GLP-1 benefit, FDA-approved weight-loss GLP-1s are coverable with prior authorization. When the employer has not elected it, obesity GLP-1s are not covered. Same insurer, same card, totally different answer.
Practical read: call your HR or benefits team and ask two questions:
- 1. “Does our plan include weight-loss / obesity drug coverage as part of the pharmacy benefit?”
- 2. “If yes, has the benefit been updated to include newly-approved GLP-1 medications like Foundayo for 2026?”
Don’t know which bucket you’re in? Ro’s GLP-1 Insurance Coverage Checker will sort you into the right one by calling your specific plan directly.
Sort your BCBS plan into the right bucket — check coverage free → (sponsored affiliate link, opens in a new tab)The RX Index Blue Cross × Foundayo coverage matrix
Every row is sourced to a public policy document or official plan bulletin, with dates. Items marked [NEEDS VERIFICATION] remain under active review and will be updated when a Foundayo-specific policy is published.
| BCBS affiliate / plan type | Public Foundayo signal | 2026 obesity GLP-1 posture | Exception / PA path | What this means for you |
|---|---|---|---|---|
| FEP Blue (Standard, Basic, Focus) | Tier placement not yet visible in 2026 Abbreviated Formulary [NEEDS VERIFICATION] | Coverable for eligible members with prior approval | Yes — formulary exception available | Don’t assume no; verify directly |
| Excellus BCBS (upstate NY) | Named in policy updated April 13, 2026 | Covered with strict PA: Class III or Class II + comorbidity | Yes — standard PA | Best public Foundayo signal in the Blue system |
| BCBSMA (standard formulary) | Governed by medical policy 572; Foundayo-specific listing [NEEDS VERIFICATION] | Covered with PA where employer elected anti-obesity benefit | PA via policy 572 | Check whether employer elected the benefit |
| BCBSMA Focused Formulary | Excluded by category rule | Obesity GLP-1s excluded | No medical-necessity review available | Real dead-end at the formulary level |
| Premera Blue Cross / Blue Shield (WA, AK) | Employer election dependent [NEEDS VERIFICATION] | Coverable only if employer elected the benefit | PA when benefit is active | Employer decision overrides Blue branding |
| BCBS North Dakota | Large-group fully-insured removes GLP-1s + oral meds Jan 1, 2026 | Excluded for fully-insured large-group | PA only where benefit remains | Group type decides first |
| BCBS Michigan (fully-insured large group) | Ended weight-loss GLP-1 coverage in 2025 | Excluded for fully-insured large group | Appeals + exception limited | Cash-pay likely if fully-insured |
| Blue Shield of California | Weight-loss excluded since Jan 1, 2025 except Class III | Excluded in most cases | Path exists for Class III documented obesity | Cash-pay likely unless Class III |
| Anthem (14 states, employer-elected) | Varies by state + employer [NEEDS VERIFICATION] | Most commercial plans exclude by default | Varies by state | Ask HR before calling Anthem |
| HCSC (IL, TX, OK, NM, MT) | Lookup-only; portal-dependent [NEEDS VERIFICATION] | Varies by employer | Varies | Must check via member portal |
| Blue Cross Medicare Advantage / Blue MedicareRx Part D | Bridge coverage opens via CMS central processor | Not covered for weight loss today; Bridge starts July 1, 2026 ($50/month) | Central processor handles PA (not your Part D plan) | See dedicated Medicare section below |
The fastest way to check your specific Blue Cross plan for Foundayo
A drug can be “on the formulary” and still not be covered for your specific employer’s benefit design. A drug can be off the formulary and still get approved through an exception. You have three real options, in order from fastest to most accurate.
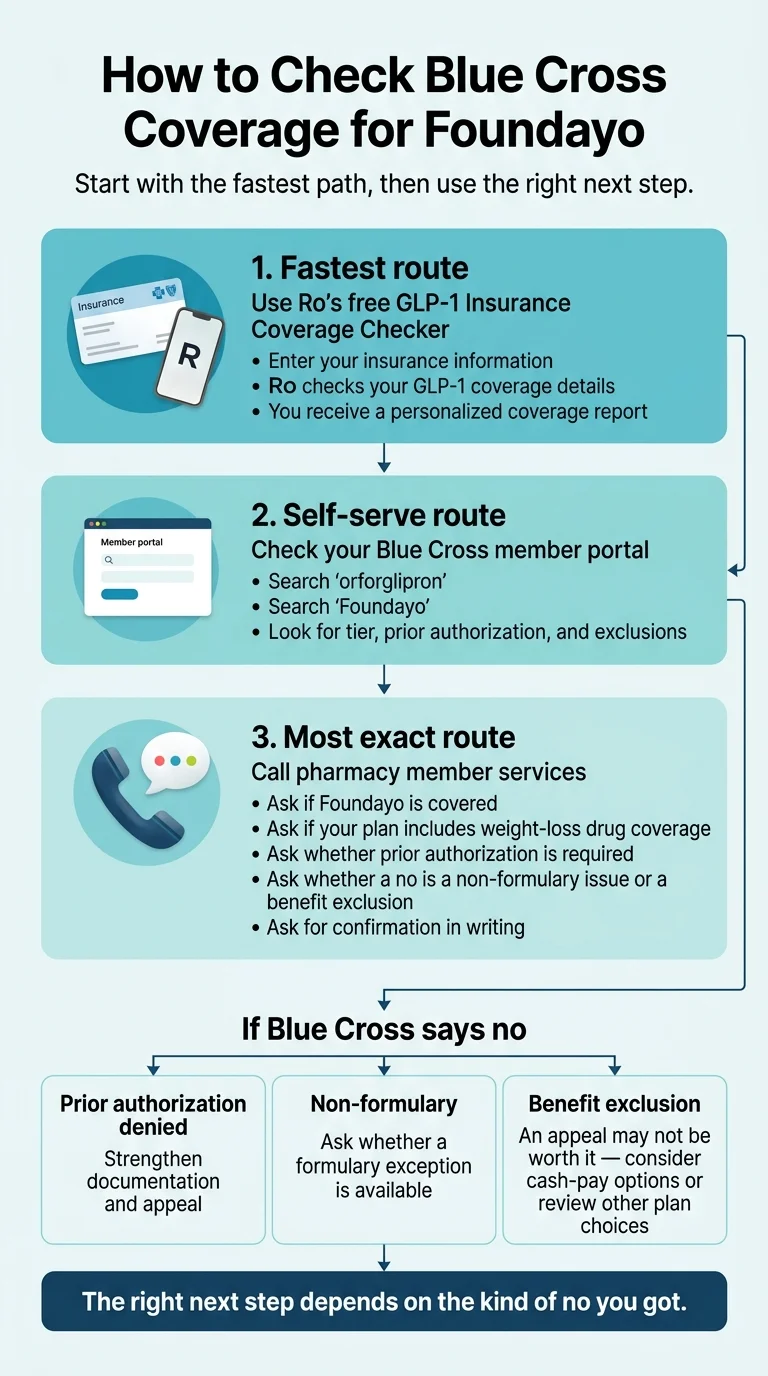
The right next step depends on the kind of no you got.
Option 1: Ro’s free GLP-1 Insurance Coverage Checker (easiest)
You enter your insurance card info and basic eligibility details, and Ro’s insurance specialists contact your plan directly on your behalf. Ro then emails you a personalized GLP-1 coverage report showing coverage status and whether prior authorization is required. No charge, no obligation to become a Ro patient, and the checker itself does not submit treatment requests or write prescriptions.
Why this is the cleanest first click:
- Answers the actual question (“will my Blue Cross cover Foundayo?”) rather than the generic one
- Handles the hold queue for you
- If you end up wanting to fill a prescription, Ro’s insurance concierge handles the prior-auth paperwork
- If your plan excludes it, Ro offers the cash-pay Foundayo path starting at $149/month
Timing note: set expectations at “days for the checker report, a few weeks for the full insurance-to-PA-to-fill process” — not hours. Forbes Health’s independent tester noted the insurance verification process “dragged on for weeks.” Ro’s insurance concierge is thorough, but it isn’t instantaneous.
Medicare caveat: Ro currently cannot help coordinate coverage for government-insurance plans (Medicare, Medicaid, TRICARE, VA). FEP/FEHB Blue is supported. If you have Blue Cross Medicare Advantage or Part D, see the Medicare section below.
Start the free Blue Cross coverage check → (sponsored affiliate link, opens in a new tab)Option 2: Your BCBS member portal (~5 minutes)
Log in to your specific BCBS plan’s member portal. Find the pharmacy or prescription-drug section. Search the formulary for both “orforglipron” (the generic name — formulary tools often index by generic) and “Foundayo” (the brand name — double-check both).
What to note:
- Is the drug listed?
- What tier is it on (Tier 2, Tier 3, Specialty)?
- Is prior authorization required?
- Is there a quantity limit?
- Is it flagged as excluded for weight-loss use?
Key limitation: the member portal shows your plan’s standard formulary. It usually doesn’t tell you whether your specific employer opted out of weight-loss coverage at the benefit-design level. That’s why option 3 matters.
Option 3: Call your plan directly (most accurate, 20–40 minutes)
Flip your card over. Call the pharmacy member-services number. Ask these five questions in order:
- 1. “Is Foundayo — spelled F-O-U-N-D-A-Y-O, generic name orforglipron — covered under my pharmacy benefit?”
- 2. “Does my specific plan include weight-loss or obesity drug coverage in the pharmacy benefit?” (This gets at the employer-election question directly.)
- 3. “If it’s covered, is prior authorization required, and what are the clinical criteria?”
- 4. “If it’s not on the formulary, is there a formulary-exception process?”
- 5. “If it’s excluded, is that a non-formulary exclusion or a benefit exclusion?” (The answer changes what you do next entirely.)
Ask for a reference number and the representative’s name at the end of the call. If your plan later disputes coverage, having that reference is your documentation.
Does Blue Cross require prior authorization for Foundayo?
Short answer: In every Blue Cross policy we verified that covers obesity GLP-1s, prior authorization is standard. The criteria are remarkably consistent across Blue affiliates: BMI threshold, comorbidity documentation, and evidence of prior lifestyle-modification attempts.
Typical Blue Cross Foundayo PA criteria
| Criterion | What your plan typically wants to see |
|---|---|
| BMI threshold | BMI ≥30 (obesity) or BMI ≥27 with at least one weight-related comorbid condition. Excellus BCBS applies stricter criteria: BMI ≥35 (Class II + comorbidity) or BMI ≥40 (Class III). |
| Weight and BMI documentation | Current, dated height and weight measurements from a recent clinical visit. Stale documentation (2+ years old) is a common denial trigger. |
| Comorbidity documentation | ICD-10 coded diagnoses for qualifying conditions: type 2 diabetes, hypertension, dyslipidemia, cardiovascular disease, obstructive sleep apnea. Verbal descriptions without coding are frequently rejected. |
| Prior attempts | Record of prior weight-management attempts: nutrition programs, physical activity programs, prior pharmacotherapy. Generic “diet and exercise” without specifics is often insufficient. |
| Clinical rationale for Foundayo specifically | Why oral GLP-1, why this drug (e.g., injection-averse, prior injectable GLP-1 intolerance). Plans offering formulary exceptions require this rationale. |
| Age requirement | Age 18+ — most commercial obesity-drug policies are adult-only. |
| Dose alignment | Dosing must align with the FDA-approved maintenance dose after titration. Off-label dosing is typically not covered. |
What your prescriber actually submits
A strong Foundayo prior-auth packet from a prescriber’s office typically includes:
- Current height, weight, and BMI
- Weight trend over the past 6–12 months
- Documented comorbidities with ICD-10 codes
- Record of prior weight-loss attempts: nutrition programs, physical activity programs, prior pharmacotherapy
- Clinical rationale for Foundayo specifically (why oral, why this drug)
- Plan for follow-up and side-effect monitoring
- Attestation of FDA-approved use (weight management, not off-label)
If your prescriber’s office isn’t used to submitting BCBS weight-loss drug PAs, Ro’s insurance concierge handles the prior-auth paperwork for you — no additional cost beyond the Ro Body membership.
See how Ro handles Blue Cross prior authorization → (sponsored affiliate link, opens in a new tab)Renewal reviews (typically 6–12 months into therapy) generally require documented 5%+ weight loss to continue coverage. Excellus BCBS sets this threshold explicitly; other Blue plans use similar recertification windows.
For a full prior-authorization walkthrough, see our dedicated guide: Foundayo prior authorization: how to get approved.
What will Foundayo actually cost you?
Short answer: This is where Foundayo breaks new ground for branded GLP-1s. Every scenario below is verified against Eli Lilly’s published terms at foundayo.lilly.com and Ro’s published pricing as of April 22, 2026.
The four real cost scenarios
| Your situation | Monthly cost | What it requires |
|---|---|---|
| Blue Cross covers Foundayo + Foundayo Savings Card | As low as $25/mo | Commercial BCBS plan with GLP-1 weight-loss coverage, approved PA, enrolled Savings Card (expires Dec 31, 2026) |
| Blue Cross covers Foundayo, Savings Card doesn’t fully stack | Varies by plan | Typical commercial specialty copay or coinsurance after PA approval |
| Blue Cross doesn’t cover weight-loss GLP-1s (self-pay path) | $149–$299/mo | No insurance approval needed; pay through LillyDirect or Ro |
| Medicare Part D via CMS GLP-1 Bridge | $50/mo fixed | Eligible beneficiary + meets Bridge clinical criteria; starts July 1, 2026 |
Self-pay dose-by-dose pricing — verified April 22, 2026
| Dose | Monthly price | Notes |
|---|---|---|
| 0.8 mg (starter) | $149/mo | Starting dose; no refill timing restriction |
| 2.5 mg | $199/mo | — |
| 5.5 mg | $299/mo | — |
| 9 mg | $299/mo | — |
| 14.5 mg | $299/mo | 45-day refill rule applies |
| 17.2 mg | $299/mo | 45-day refill rule applies; reverts to $349 if missed |
The 45-day catch most people miss: at 14.5 mg and 17.2 mg, the $299 price only holds if you refill within 45 days of your previous fill. Miss that window, and pricing reverts to $349/month for those two highest doses. If you’re climbing the dose ladder, plan your refills around this rule.
Ro Body membership: what Ro adds on top of medication cost
If you fill Foundayo through Ro rather than LillyDirect, the medication price follows Lilly’s published tiers above. Ro Body (Ro’s weight-loss membership that includes the provider visit, ongoing clinical support, and insurance coordination) is a separate fee:
- $39 for the first month
- $149/month ongoing, or as low as $74/month with annual plan paid upfront
Ro vs. LillyDirect in one sentence: Ro’s value is the clinical visit, ongoing provider relationship, insurance concierge, and PA handling. LillyDirect’s value is rock-bottom cost with no membership. Neither is strictly better; they’re different products.
Can I use the Foundayo Savings Card if Blue Cross says no?
Yes. The Foundayo Savings Card works in two ways depending on your situation:
- Commercially insured with Foundayo coverage: copay as low as $25/month, subject to monthly and annual limits
- Commercially insured without coverage, or self-pay: caps out-of-pocket at $149 (starter dose) through $299–$349 (higher doses)
Government beneficiaries are excluded. If you have Medicare, Medicaid, TRICARE, VA, or any other federal or state-funded coverage, you cannot use the commercial Savings Card. The card expires December 31, 2026.
If your Blue Cross plan covers Foundayo, the Ro checker will tell you your estimated copay before you commit to anything. If it doesn’t, Ro’s cash-pay Foundayo path starts at $149 for the 0.8 mg dose.
See Foundayo pricing on Ro → (sponsored affiliate link, opens in a new tab)Disclosure: The RX Index may earn a commission when readers sign up via affiliate links. Commissions never influence clinical guidance.
What if Blue Cross says no?
A Blue Cross “no” is not one thing. There are three kinds, and the right next step is completely different for each. Get the type wrong and you’ll waste weeks appealing a wall that was never going to move.
Type 1: Prior-authorization denial (worth appealing)
This is when your plan covers obesity GLP-1s, but your PA packet didn’t satisfy the clinical criteria. Maybe BMI documentation was old. Maybe the comorbidity wasn’t coded properly. Maybe the prior-attempt documentation was thin.
This “no” is appealable and often winnable.
Work with your prescriber to:
- Pull current, dated BMI and weight measurements
- Get proper ICD-10 coded comorbidity documentation
- Document prior weight-management attempts with specific programs and dates
- Submit an internal appeal with strengthened documentation (check your denial letter for the appeal window)
- If the internal appeal fails, request external review through your state insurance department
Type 2: Non-formulary / formulary exception (sometimes worth appealing)
This is when Foundayo isn’t on your plan’s formulary at all, but your plan does cover the obesity GLP-1 category in general.
FEP Blue explicitly allows formulary exception requests for excluded or not-covered weight-loss drugs. Many employer-elected plans have similar paths. Success depends on whether you can show a clinical reason Foundayo specifically is needed — documented intolerance to injectables, documented issues with other oral GLP-1s’ food/water restrictions, etc.
For a step-by-step walkthrough, see our Foundayo prior authorization guide.
Type 3: True benefit exclusion (not worth appealing)
This is the BCBSMA Focused Formulary situation, or BCBSND large-group, or a Premera employer group that hasn’t elected the obesity GLP-1 benefit. The exclusion is at the contract level, not the clinical criteria level. No clinical documentation will change the answer.
Appealing wastes time. Move directly to your real options:
- Cash-pay through LillyDirect or Ro ($149/month at the starting dose)
- Check whether you qualify for the Foundayo Savings Card
- Re-evaluate coverage at open enrollment — and ask HR if they’ll add the obesity GLP-1 benefit for the next plan year
Is Ro really the right next step for Blue Cross members?
Here’s our honest take, and we’re going to say something Ro’s marketing team wouldn’t.
Ro does NOT become your cheapest Foundayo option just because it helps with insurance. If your priority is the absolute lowest cash-pay path after a confirmed benefit exclusion, Eli Lilly’s direct self-pay pricing through LillyDirect is the cleaner benchmark — no separate membership fee, same published Foundayo medication pricing, shipping from Lilly-partnered pharmacies (Amazon Pharmacy, Walmart, Prescryptive).
But because Ro checks your Blue Cross plan for free, handles the prior-auth paperwork when coverage exists, and bundles the clinical relationship for ongoing support, it’s still the best first click for most commercial Blue Cross and FEP members who want an FDA-approved Foundayo path.
Use Ro first if:
- You have commercial BCBS or FEP Blue and don’t know whether weight-loss drugs are covered
- You want someone else to handle the PA paperwork
- You want an ongoing clinical relationship for dose titration
- You’re comfortable paying the Ro Body membership fee
Skip Ro and go to LillyDirect if:
- You already know your Blue Cross plan excludes weight-loss GLP-1s and you’re not appealing
- You already have a prescriber relationship and just need a pharmacy
- You want the absolute lowest floor cost with no membership
Skip Ro entirely if: you have Blue Cross Medicare Advantage or a Blue MedicareRx Part D plan — Ro doesn’t coordinate government insurance coverage. Your path is the CMS Medicare GLP-1 Bridge starting July 1, 2026.
Blue Cross Medicare Advantage and Foundayo: the July 1, 2026 GLP-1 Bridge
A major coverage shift is coming July 1, 2026 — but it’s structured differently from how most readers assume. The CMS Medicare GLP-1 Bridge operates outside the normal Medicare Part D benefit.
For two decades, traditional Medicare Part D didn’t cover any weight-loss medication. The GLP-1 Bridge doesn’t change that Part D rule. Instead, CMS created a separate demonstration program that provides access to eligible GLP-1 drugs through a single central processor, regardless of which Part D plan you’re in.
- Eligible beneficiaries access the Bridge through a CMS central processor, not through their Part D plan. Your provider submits the prior-authorization request to the central processor, not to your Blue Cross Medicare Advantage plan.
- The copay is a fixed $50/month for covered Bridge drugs.
- Part D plan sponsors don’t have to opt in. Eligible beneficiaries enrolled in eligible plan types get access through the central processor regardless.
- Foundayo is explicitly included per CMS’s April 6, 2026 update, alongside all formulations of Wegovy and the Zepbound KwikPen.
Bridge eligibility criteria (verified against CMS April 6, 2026)
| Criterion | Detail |
|---|---|
| Purpose of use | Prescribed for excess body weight reduction and maintenance, combined with ongoing lifestyle modification consistent with the FDA label |
| Age | 18+ |
| BMI threshold (one of two criteria) | BMI ≥35 at initiation, OR |
| BMI + comorbidity (second criteria) | BMI ≥27 at initiation with at least one of: prediabetes, previous myocardial infarction, previous stroke, or symptomatic peripheral artery disease |
| Pre-July 2026 initiators | The prescribing provider attests that you met the BMI criterion at the time of initiation, even if your current BMI is lower |
Practical timeline for Blue Cross Medicare Advantage members
- Now through June 2026: Foundayo is not covered for weight loss under any BCBS Medicare Advantage or Blue MedicareRx Part D plan.
- July 1, 2026: the CMS Medicare GLP-1 Bridge launches. Work with your prescriber to understand how to submit PAs to the central processor. CMS said it will publish additional information on PA processes in Spring 2026.
- Your cost if eligible: $50/month fixed, for the duration of the Bridge demonstration.
Medicare members: Ro currently cannot help coordinate coverage for government-insurance plans. Talk to your prescriber about Bridge eligibility starting June 2026. For broader Medicare + GLP-1 education, see our Medicare GLP-1 Bridge walkthrough.
Frequently asked questions about Blue Cross and Foundayo
Does Blue Cross cover Foundayo?
It depends on your specific BCBS affiliate, plan type, and employer benefit design. In 2026, FEP Blue covers weight-loss drugs for eligible members with prior approval and allows formulary-exception requests for non-covered weight-loss GLP-1s. Excellus BCBS has updated its weight-management policy to explicitly name Foundayo as of April 13, 2026. BCBSMA’s Focused Formulary excludes obesity GLP-1s with no medical-necessity review available. Most employer-elected plans depend on whether your employer bought the weight-loss benefit. Use Ro’s free GLP-1 Insurance Coverage Checker or call your plan directly to verify your specific coverage.
Does FEP Blue cover Foundayo?
FEP Blue covers weight-loss drugs for eligible members who obtain prior approval, and excluded or not-covered weight-loss GLP-1s can still be submitted through a formulary-exception process. Foundayo-specific tier placement was not visible in the 2026 FEP Blue abbreviated formulary as of April 22, 2026. Verify directly at fepblue.org or call FEP pharmacy member services before assuming a tier.
Does Blue Cross require prior authorization for Foundayo?
In the Blue Cross policies we verified that cover obesity GLP-1s, prior authorization is standard. Typical criteria include BMI ≥30 (or ≥27 with a qualifying comorbidity), documented weight and BMI history, comorbidity documentation, and evidence of prior lifestyle-modification attempts. Some Blue plans apply stricter criteria — Excellus BCBS requires BMI ≥35 (Class II with comorbidity) or ≥40 (Class III).
What if my Blue Cross plan excludes weight-loss drugs?
First, determine which kind of no you got. If it’s a prior-auth denial, strengthen documentation and appeal. If it’s a non-formulary issue, ask your prescriber to submit a formulary-exception request. If it’s a true benefit exclusion — like BCBSMA Focused Formulary — the exception path doesn’t exist and appealing wastes time. Move directly to cash-pay through Ro or LillyDirect ($149/month starting dose), or re-evaluate at open enrollment.
How much does Foundayo cost without insurance?
Self-pay starts at $149/month for 0.8 mg, $199/month for 2.5 mg, and $299/month for 5.5 mg through 17.2 mg under the Foundayo Self-Pay Journey Program, with pricing through LillyDirect or Ro. At the 14.5 mg and 17.2 mg doses, the $299 price only holds if you refill within 45 days; miss the window and it reverts to $349/month for those two doses.
Can I use the Foundayo Savings Card if Blue Cross doesn’t cover it?
Yes, if you have commercial insurance that doesn’t cover Foundayo, the Savings Card caps your out-of-pocket cost at $149 for the 0.8 mg starter dose, $199 for 2.5 mg, and $299–$349 for higher doses. Government beneficiaries (Medicare, Medicaid, TRICARE, VA) are excluded from the commercial Savings Card. The card expires December 31, 2026.
Does Blue Cross Medicare cover Foundayo?
Not today, but this changes July 1, 2026 when the CMS Medicare GLP-1 Bridge launches. The Bridge runs outside the normal Medicare Part D benefit: eligible beneficiaries access Foundayo and other included GLP-1s through a CMS central processor at a fixed $50/month copay, regardless of which Part D plan they’re enrolled in. Eligibility requires BMI ≥35 at initiation, or BMI ≥27 with prediabetes, previous myocardial infarction, previous stroke, or symptomatic peripheral artery disease.
Is Foundayo covered on BCBS Massachusetts?
It depends on which BCBSMA formulary your plan uses. On the standard Blue Cross Blue Shield of Massachusetts Formulary, GLP-1 coverage for anti-obesity use is governed by medical policy 572 and requires prior authorization. On the BCBSMA Focused Formulary, obesity GLP-1s are excluded with no medical-necessity review available. Log in to your MyBlue account to see which formulary your plan uses.
What is the BMI requirement for Foundayo?
The FDA-approved prescribing label requires BMI ≥30 (obesity) or BMI ≥27 with at least one weight-related comorbid condition such as type 2 diabetes, hypertension, dyslipidemia, cardiovascular disease, or obstructive sleep apnea. Some Blue Cross plans apply stricter criteria for prior-authorization approval — Excellus BCBS requires BMI ≥35 or BMI ≥40 depending on class of obesity and comorbidity status.
What’s the fastest way to check my specific Blue Cross plan?
For commercial BCBS or FEP Blue, Ro’s free GLP-1 Insurance Coverage Checker contacts your insurer on your behalf and emails a personalized report. It’s faster than your member portal and avoids the 20–40-minute hold queue. Ro currently does not coordinate Medicare, Medicaid, TRICARE, or VA coverage — Medicare beneficiaries should work through their prescriber and the CMS Medicare GLP-1 Bridge central processor starting July 1, 2026.
What we actually verified for this page
Every claim traces to one of the primary sources below. Items marked [NEEDS VERIFICATION] remain under active review and will be updated when a Foundayo-specific policy is published.
- 1 FDA press announcement on Foundayo (orforglipron) approval, dated April 1, 2026 — fda.gov
- 2 Foundayo prescribing information and Medication Guide (Eli Lilly, April 2026)
- 3 foundayo.lilly.com/coverage-savings — official Lilly coverage and savings terms, verified April 22, 2026
- 4 ro.co/weight-loss/foundayo/ — Ro pricing and coverage checker workflow, verified April 22, 2026
- 5 FEP Blue 2026 Abbreviated Formulary PDF (fepblue.org)
- 6 Excellus BCBS weight-management drug policy, updated April 13, 2026 (provider.excellusbcbs.com)
- 7 BCBSMA medical policy 572 — GLP-1 and GLP-1/GIP Agonist Drugs for Anti-Obesity Management (bluecrossma.org)
- 8 BCBS North Dakota coverage change bulletin (bcbsnd.com)
- 9 BCBS Michigan Clinical Drug List and pharmacy policy, 2026 (bcbsm.com)
- 10 Premera 2026 prescription drug document (premera.com)
- 11 Blue Shield of California drug formulary pages (blueshieldca.com)
- 12 cms.gov/medicare/coverage/prescription-drug-coverage/medicare-glp-1-bridge, updated April 6, 2026
- 13 Forbes Health Ro Body weight-loss medication review
- 14 Trustpilot Ro review page, accessed April 22, 2026
All non-[NEEDS VERIFICATION] claims were rechecked against the primary sources above on April 22, 2026. We update this page monthly for the first 90 days after publish, and within 7 days of any formulary change or pricing update.
Related pages on The RX Index
Ready to find out where you stand?
For commercial Blue Cross and FEP Blue members: Ro’s free GLP-1 Insurance Coverage Checker contacts your insurer on your behalf and emails you a personalized report — no charge, no obligation to become a patient.
Check your Blue Cross Foundayo coverage with Ro — free → (sponsored affiliate link, opens in a new tab)For commercial Blue Cross and FEP Blue members only. Medicare Advantage/Part D members: see the Medicare section above.
Written by The RX Index Editorial Team. The RX Index is a pricing intelligence and comparison resource for GLP-1 telehealth providers. This article is informational and does not constitute medical advice. Speak with a licensed healthcare provider before starting, changing, or stopping any prescription medication. Last verified: April 22, 2026.