Affiliate disclosure: The RX Index earns a commission when you sign up with some of the providers mentioned on this page. It does not affect what you pay, and it never determines our rankings or which providers we cover. Read the full disclosure.
Foundayo Prior Authorization: What Insurers Ask For and How to Get Approved Faster
Published: · Last updated:
By The RX Index Editorial Team · Last verified:
Disclosure: Some links on this page are affiliate links. If you purchase through these links, we may earn a commission at no extra cost to you.
Foundayo prior authorization is likely required on many commercial insurance plans before they'll cover orforglipron — and because Foundayo was just FDA-approved on April 1, 2026, coverage policies are still forming at most insurers. Lilly's own guidance to prescribers says they will “likely need to complete a Prior Authorization request” before insurance covers Foundayo, and the approval typically comes down to documented BMI, diagnosis, prior weight-loss attempts, and how well your chart supports medical necessity.
Here's the short version: if you have commercial insurance and want the least paperwork friction, Ro is the strongest starting point — they check your coverage, tell you whether PA is required, and submit the paperwork on your behalf. If your plan excludes weight-loss drugs or you'd rather skip insurance, LillyDirect starts at $149/month for the starter dose with no prior authorization needed.
The rest of this page exists for one purpose: make sure you don't waste weeks on an incomplete submission, get blindsided by a denial, or miss a faster path you didn't know about. We built the documentation checklist, the access-path comparison, and the denial-recovery workflow so you have one page instead of twelve tabs.
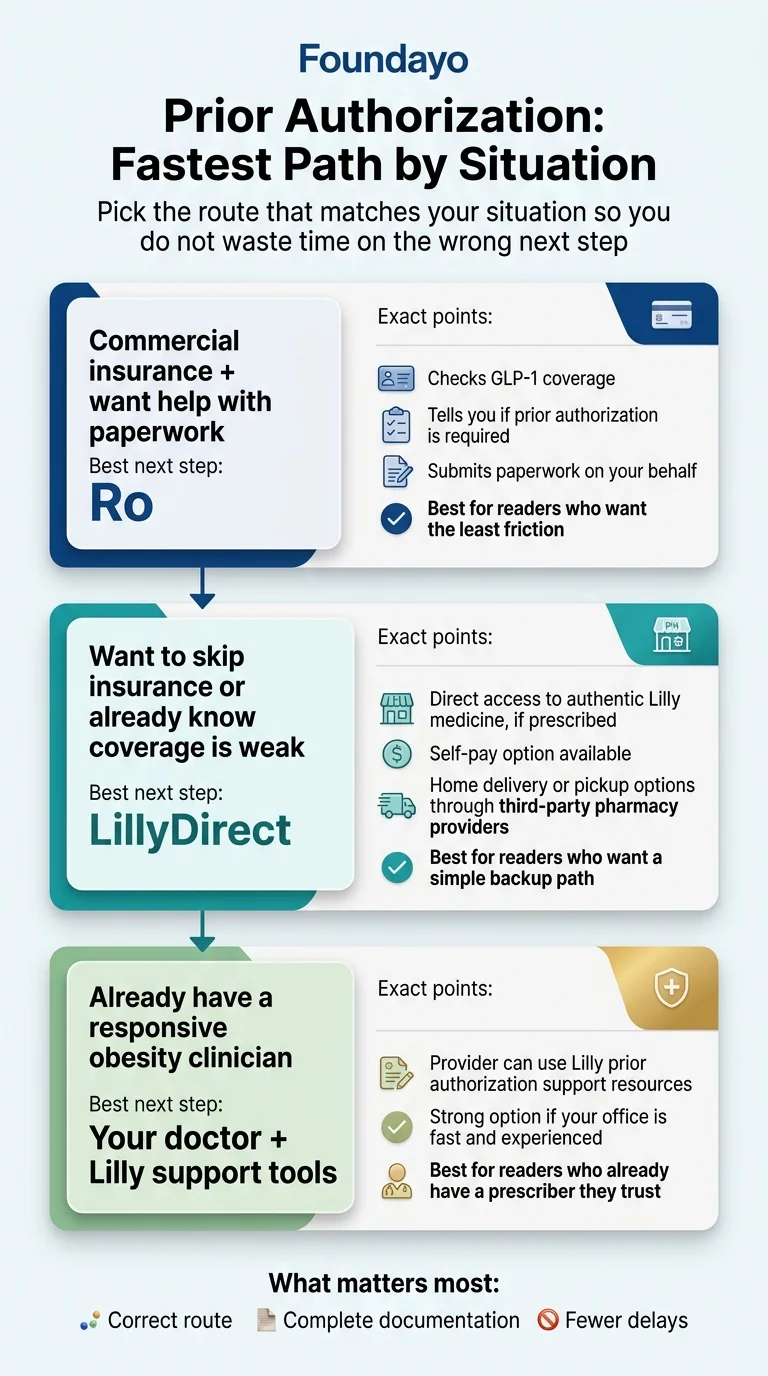
Your best next step depends on your situation
| Your situation | Fastest path | Why |
|---|---|---|
| Commercial insurance + want someone to handle PA | Ro | Checks coverage, submits PA, handles insurer back-and-forth — ~2–3 weeks total |
| Know your plan won't cover it / want to skip insurance | LillyDirect | $149–$349/month, ships after checkout, no PA required |
| Want clinic-style care with insurance support | Knownwell | Authorization team helps with benefit verification and next steps |
| Already have a responsive obesity clinician | Your doctor + Lilly's PA tools | Lilly publishes a PA guide and letter-of-medical-necessity template for providers |
| Medicare Part D beneficiary | GLP-1 Bridge (July 2026–Dec 2027, 18 months) | $50/month if eligible — PA submitted to CMS central processor, not your Part D plan |
Want Ro to check whether your plan requires prior authorization for Foundayo?
Ro checks your insurance, tells you if PA is required, and submits the paperwork for you. About 2–3 weeks for the insurance path.
Check your Foundayo coverage and eligibility on Ro → (sponsored affiliate link, opens in a new tab)What we actually verified
We didn't summarize other affiliate pages and call it a guide. Here's what we checked against primary sources:
Does Foundayo require prior authorization?
Often, yes — if you're using commercial insurance. Lilly's PA guide tells prescribers they will likely need to submit for prior authorization before insurance covers Foundayo. Ro's coverage checker explicitly reports whether a specific user's plan requires PA. Self-pay routes through LillyDirect bypass insurance approval entirely.
It's a brand-name GLP-1 for weight loss
That puts it in the most scrutinized drug class in pharmacy benefits right now. GLP-1 medications are expensive, widely prescribed, and insurers are actively managing access. That's the environment Foundayo is entering.
Coverage policies are still forming
Foundayo was FDA-approved on April 1, 2026. While at least one insurer — Excellus BCBS — has already added orforglipron to its weight-management policy (last reviewed April 13, 2026), many plans haven't published Foundayo-specific criteria yet. Lilly's own guidance recommends beginning the PA process as soon as the prescribing decision is made.
What Excellus already requires (a live example)
Their current policy covers Foundayo for Class III obesity (BMI ≥40) or Class II obesity (BMI 35–39.9) with at least one comorbidity, plus documentation of current enrollment in a comprehensive weight-management program for at least 3 consecutive months, with proof of participation. This gives you a realistic preview of what other commercial plans will likely require.
When self-pay bypasses the issue entirely
If you go through LillyDirect or a telehealth provider offering cash-pay pricing, prior authorization isn't part of the equation. You get a prescription, you pay the published price, and your medication ships.
What insurers usually ask for in a Foundayo prior authorization
The documentation pattern across GLP-1 prior authorizations is well-established, and Lilly's own PA guide confirms what Foundayo submissions need. A successful PA packet will typically require: a qualifying diagnosis with documented BMI, weight-related comorbidities, evidence of prior weight-loss efforts, complete chart notes, and correct coding. Missing any single item is the most common cause of delays and denials according to Lilly's guide.
This checklist is designed to be printed or saved. Bring it to your next appointment or send it to your provider's office before they submit the PA.

Foundayo Prior Authorization Readiness Matrix
| Document you need | Why it matters | What to gather before your visit | How to strengthen it |
|---|---|---|---|
| Qualifying diagnosis | Foundayo's FDA label is for adults with obesity, or adults with overweight with at least one weight-related comorbidity. If the diagnosis doesn't match, the case is weak from the start. | Active diagnosis on your chart, problem list showing comorbidities, clinician note tying treatment to weight management. | Make sure your provider documents the specific FDA-approved indication language — not just 'patient wants to lose weight.' |
| Current BMI with a date | BMI is the single most referenced criterion in every PA framework reviewed — Lilly's guide, CMS Bridge criteria, and Excellus's live policy all start here. | Height, weight, BMI calculated and recorded at a recent visit. If continuing therapy, bring your BMI from when treatment started. | Excellus requires Class II (BMI 35–39.9 with comorbidity) or Class III (BMI ≥40). Ask your insurer for their specific threshold. |
| Weight-related comorbidities | For patients who don't meet the highest BMI tier alone, comorbidities make the difference between approval and denial. | Documented diagnoses: hypertension, type 2 diabetes or prediabetes, dyslipidemia, obstructive sleep apnea, PCOS, cardiovascular disease, CKD, NASH/MASH, osteoarthritis. | List every qualifying condition, not just the primary one. Ask your doctor: 'Are there other weight-related conditions in my chart we should include?' |
| Prior weight-loss medication history | Lilly's PA guide asks for prior medications, therapies tried, and reasons for discontinuation. Some plans require step therapy. | Names of prior medications (phentermine, Contrave, Saxenda, Qsymia, etc.), dates used, why you stopped. | If you previously tried injectable GLP-1s and had adherence issues or injection aversion, document that explicitly. Foundayo's oral format is a distinguishing clinical factor. |
| Lifestyle program participation | Lilly's guide asks for prior attempts and chart support. Excellus's live policy requires at least 3 consecutive months in a comprehensive weight-management program. | WW records, nutritionist visit notes, dietitian referrals, gym membership records, food diary logs, app data, counseling notes. | If your lifestyle efforts weren't formally documented, ask your doctor to add a chart note about weight-management counseling. |
| Complete chart notes | Lilly's guide specifically calls for chart notes and medical records. Incomplete notes are a common documentation problem. | Most recent office visit note, weight history over time, treatment plan, counseling documentation. | Ask your provider's office: 'Will you include my full weight history in the PA submission?' A single recent visit note often isn't sufficient. |
| Correct ICD-10 codes and benefit routing | Wrong codes or wrong submission channel can delay or derail the request. For the Medicare GLP-1 Bridge, PA goes to a CMS central processor — not your Part D plan. | E66.01 (morbid/severe obesity), E66.09 (other obesity), E66.3 (overweight) + relevant comorbidity codes. Confirm with your provider's billing staff. | Triple-check before submission. Incorrect codes can result in automatic rejection. |
| Reauthorization documentation | Lilly's guide notes that initial authorization typically lasts approximately 6–8 months, and reauthorization will likely be required. | Updated weight measurements, refill history showing adherence, visit notes documenting continued treatment. | Document your baseline weight at treatment start and keep it accessible. Reauthorization denials are common when patients can't demonstrate continued progress. |
Checklist cross-referenced from: Lilly's Foundayo PA Guide, CMS Medicare GLP-1 Bridge criteria, and Excellus BCBS live policy (verified April 2026).
Want to skip the paperwork?
Ro checks your coverage, tells you if PA is required, and submits it for you. Start for $39 the first month.
See if Ro can handle your Foundayo prior authorization → (sponsored affiliate link, opens in a new tab)The fastest ways to get Foundayo approved or access it, compared
For most commercially insured readers who want the least friction, Ro is the best starting point. It combines coverage checking, PA submission, insurer follow-up, and cash-pay fallback in one workflow — and publishes a realistic timeline. LillyDirect is the cleanest self-pay path when insurance won't cooperate. Medicare readers have a separate branch entirely.
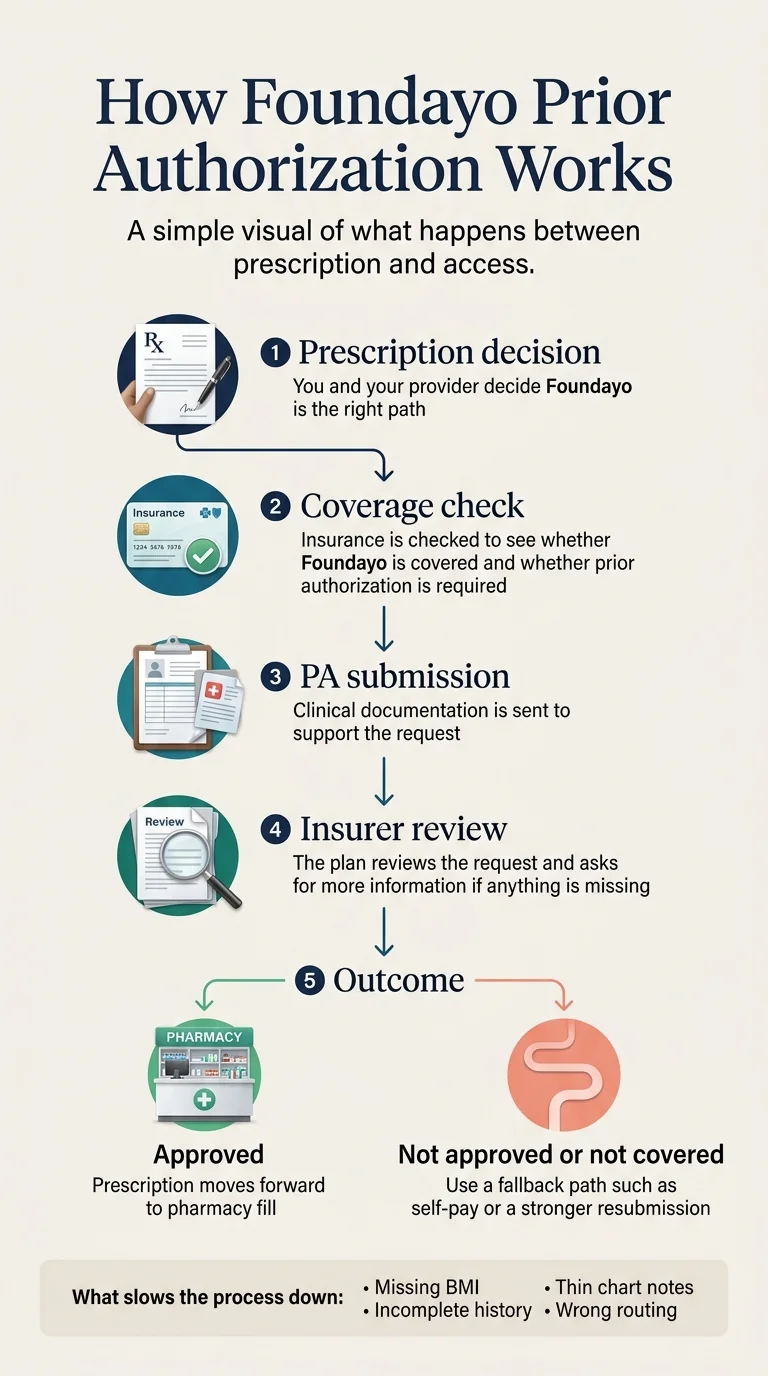
Foundayo Access Path Comparison — Verified April 2026
| Path | What they do for PA | Timeline | Current pricing | Best for | Biggest drawback |
|---|---|---|---|---|---|
| RoRecommended | Checks insurance coverage, reports whether PA is required, submits all paperwork, handles insurer back-and-forth | ~2–3 weeks for PA; insurer review 2–9 days after submission | Membership: $39 first month, then as low as $74/mo (annual). Foundayo: $149–$349/mo depending on dose | Commercially insured readers who want someone else to handle paperwork | Membership fee applies even while PA is pending; cannot coordinate government insurance |
| LillyDirect | Checks insurance, applies savings when eligible, supports patients if PA is needed | No specific end-to-end PA timeline published | $149 (0.8mg), $199 (2.5mg), $299 (5.5/9mg), $299–$349 for higher doses | Self-pay with no PA hassle, or clean backup when insurance fails | Less public evidence of hands-on PA concierge than Ro |
| Knownwell | Authorization team helps with benefit verification, insurance navigation, and next steps | No clear public PA timeline | Foundayo starts at $149/month; doses up to ~$399/month per their page (see pricing note below) | Readers who want clinic-style care with insurance help | Pricing language appears less current than LillyDirect's official page |
| Your doctor + Lilly PA tools | Lilly publishes a PA guide and letter-of-medical-necessity template clinicians can use | Depends on the office | Visit costs vary; medication cost depends on pharmacy/savings route | Readers who already have a responsive, experienced obesity clinician | Great if your office is efficient; frustrating if they're slow or inexperienced |
| Medicare GLP-1 Bridge | Provider submits PA + prescription to CMS central processor for eligible uses | CMS hasn't published specific turnaround time | $50/month if eligible, July 1, 2026 – December 31, 2027 (18 months) | Eligible Medicare Part D beneficiaries | Temporary demonstration with strict eligibility criteria; not permanent Part D coverage |
Pricing verification note
We found a discrepancy between Knownwell's Foundayo page and LillyDirect's live pricing as of April 14, 2026. Knownwell states self-pay doses can cost “up to $399 per month.” LillyDirect's official price ladder tops out at $349 for the 14.5mg and 17.2mg doses when the 45-day refill window is missed — and drops to $299 if you refill on time. We recommend using LillyDirect's pricing as the source of truth, since Lilly sets the price and LillyDirect is their direct channel.
Ro: why it's the strongest path for most commercially insured readers
Our editorial verdict: Ro is the best first step for this specific search intent — not because of commission priority, but because it's the clearest published solution to the exact problem this reader has. A person searching “Foundayo prior authorization” wants someone to handle paperwork, reduce uncertainty, and give them a timeline. Ro addresses all three.
Here's what Ro says it does, specifically:
- ✓Checks your insurance to determine whether GLP-1 coverage is available
- ✓Tells you if prior authorization is required for your plan
- ✓Submits all PA paperwork on your behalf through its insurance concierge
- ✓Handles back-and-forth with your insurer during the review process
- ✓If coverage fails, your Ro provider suggests alternative FDA-approved cash-pay options
- ✓Publishes a timeline: roughly 2–3 weeks for the insurance path, or less than a week for cash-pay
What you'll pay: Get started for $39 for the first month, then as low as $74/month with the annual plan paid upfront. Foundayo medication cost is separate — either through your insurance (as low as $25/month with the Foundayo Savings Card if your plan covers it) or at LillyDirect's self-pay pricing ($149–$349/month depending on dose).
What to know about the membership fee: Ro does NOT waive its membership fee while your PA is pending. If you already have an obesity specialist who handles PA submissions efficiently, a local prescriber plus Lilly's free PA tools could cost less on the service side.
Who Ro is NOT for on the insurance side:
Ro cannot coordinate GLP-1 coverage for government insurance plans. People with Medicare, Medicare supplement, or TRICARE can still join Ro Body and pay cash. People with Medicaid or certain government-funded plans cannot join. People with Federal Employee Health Benefits (FEHB) can use Ro's insurance concierge — FEHB is treated as commercial insurance. If you're on Medicare and want coverage, the GLP-1 Bridge ($50/month starting July 1) is the right path.
“They've done two PAs for me with no issues.” — Reddit user, r/RoBody
Ro checks your coverage, submits PA, and offers cash-pay alternatives if insurance won't cover Foundayo. Start for $39 the first month.
See if you qualify for Foundayo through Ro → (sponsored affiliate link, opens in a new tab)How long does Foundayo prior authorization take?
The clearest published patient-facing timeline comes from Ro: approximately 2–3 weeks for the full process, with insurer review typically taking 2–9 days once the submission is in. Your experience will depend on your insurer's workload, the completeness of your documentation, and whether additional information is requested.
Missing documentation is the #1 cause of slow PA. If the submission is missing your BMI, doesn't include comorbidity documentation, or has incorrect diagnosis codes, the insurer will request additional information — adding days or weeks. This is why we built the readiness matrix above: submit everything the first time.
The motivation gap is real. Every week of PA delay is a week where momentum fades. If your PA is going to take two or more weeks, consider starting on LillyDirect's $149/month starter dose while you wait. If insurance approves later, you can switch to covered pricing.
Reauthorization is part of the picture. Lilly's PA guide says initial authorization typically lasts approximately 6–8 months, and reauthorization will likely be required. Plans may ask for updated BMI, adherence records, continued program participation, and evidence of benefit such as at least 5% weight loss from your baseline weight. Document your starting weight when you begin treatment and keep records of every refill.
The most common reasons Foundayo prior authorization gets denied
Most denials trace back to documentation gaps, not medical-necessity disagreements. Lilly's PA guide and the Excellus live policy both point to the same patterns: missing BMI or comorbidity evidence, insufficient prior-attempt documentation, thin chart notes, or incorrect coding and routing.
| Denial reason | What it usually means | What to do |
|---|---|---|
| Not covered / plan exclusion | Plan design excludes weight-loss drugs — no PA can fix this | Self-pay through LillyDirect ($149–$349/mo) or pursue a formulary exception |
| Medical necessity not demonstrated | Documentation was incomplete or didn't meet insurer criteria | Resubmit with gaps filled; use the readiness matrix above |
| Missing BMI or comorbidity proof | 'Patient is obese' without recorded BMI, date, and comorbidity codes is weak | Update chart with specific BMI, date, and all qualifying diagnoses |
| Missing prior-attempt documentation | Plan requires evidence of lifestyle modification or prior medications | Ask provider to add chart notes covering prior weight-loss efforts |
| Incorrect codes or wrong benefit channel | Lilly's PA guide emphasizes correct routing — wrong codes can auto-reject | Triple-check ICD-10 codes; Medicare Bridge PA goes to CMS central processor |
“Stuck in this awful limbo” while waiting for a PA decision on a GLP-1 — a frustration that's largely avoidable when documentation is complete from the start. — Reddit, r/antidietglp1
What to do if Foundayo prior authorization is denied
A denial isn't necessarily the end — and it's often not even a reflection of your medical eligibility. KFF analysis of CMS data found that in 2024, only 11.5% of denied Medicare Advantage prior authorization requests were appealed, but 80.7% of those appeals were at least partially overturned. Most people who fight back win. Most people don't fight back.
Get the denial reason in writing
Request the Explanation of Benefits (EOB) with the specific denial code and reason. Common reasons: not covered by plan (plan exclusion — different fix than documentation gap), medical necessity not demonstrated (documentation problem), step therapy requirements not met (prior medications required), or missing clinical information.
Match your response to the denial reason
If “medical necessity not demonstrated”: Resubmit with the gaps filled. Use the readiness matrix above as your checklist. Ask your provider to write a letter of medical necessity — Lilly publishes a letter of medical necessity guide specifically for this on their HCP portal.
File an internal appeal
Every insurance plan is required to offer an appeal process. Your appeal should include the specific denial reason you're addressing, updated documentation filling the identified gap, a letter of medical necessity from your provider, relevant clinical evidence (ATTAIN-1 trial data: 12.4% average weight loss at the highest dose over 72 weeks), and your full weight and comorbidity history.
Request external review if internal appeal fails
Under ACA and applicable state rules, insurers must offer an external review process. An independent third party reviews your case. Standard external review takes up to 45 days; expedited external review is available for urgent situations and takes up to 72 hours. Source: HealthCare.gov
Don't lose treatment time
LillyDirect's self-pay pricing starts at $149/month for the 0.8mg starter dose, and Ro offers cash-pay options alongside its insurance concierge. Starting treatment while an appeal processes means you don't lose months of health outcomes to paperwork.
Ro checks your coverage, submits PA, and offers cash-pay alternatives if insurance won't cover Foundayo.
See if you qualify for Foundayo through Ro → (sponsored affiliate link, opens in a new tab)Medicare, Part D, and the GLP-1 Bridge
Medicare Part D does not cover Foundayo for weight loss — that's federal law, not a plan decision. But starting July 1, 2026, the CMS Medicare GLP-1 Bridge changes the picture for eligible beneficiaries.
An 18-month demonstration program running July 1, 2026 through December 31, 2027, operating outside of normal Part D coverage. BALANCE will not launch for Medicare Part D in 2027 — CMS extended the Bridge. CMS administers the entire program through a central processor (Humana, BIN 028918 / PCN MEDDGLP1BR) — Part D sponsors aren't directly involved.
Foundayo (all formulations), Wegovy (injection and tablets), and Zepbound (KwikPen formulation only). CMS updated the eligible drug list on April 6, 2026 to include Foundayo following FDA approval.
$50/month if eligible.
Who qualifies — three eligibility tiers (you only need to meet one)
| Tier | BMI threshold | Required diagnosis |
|---|---|---|
| Tier 1 | BMI ≥35 | None beyond the FDA indication |
| Tier 2 | BMI ≥30 | At least one of: heart failure with preserved ejection fraction (HFpEF), uncontrolled hypertension (systolic >140 or diastolic >90 on 2+ antihypertensives), or chronic kidney disease stage 3a or above |
| Tier 3 | BMI ≥27 | At least one of: prediabetes (ADA guidelines), previous myocardial infarction, previous stroke, or symptomatic peripheral artery disease |
Source: CMS.gov Medicare GLP-1 Bridge FAQ
Important: BMI is measured at the time of initiating GLP-1 therapy, not at the time of the PA request. If you started at BMI 37 and are now at BMI 34, your provider can attest to the initiating BMI.
Why Ro isn't the right path for Medicare: Ro cannot coordinate GLP-1 coverage for government insurance. If you're a Medicare beneficiary interested in Foundayo through the GLP-1 Bridge, work with your own clinician and the CMS central processor. If you can't wait until July, LillyDirect self-pay ($149+/month) is available now. See our Medicare GLP-1 Bridge program guide.
Not sure which path fits your situation? Take our free 60-second GLP-1 matching quiz for a personalized action plan.
Get your personalized GLP-1 action plan →Safety and practical issues that can affect PA candidacy
Several items from Foundayo's prescribing label materially affect whether you're a candidate, what your provider needs to discuss with you, and whether PA is the right immediate step.

How we chose the recommended path
This recommendation is editorial, but not arbitrary. We ranked access paths by: published evidence of coverage checking and PA support, published timeline specificity, pricing transparency verified against official sources, fallback clarity when insurance fails, and match to the specific job this reader needs done.
Ro scored highest because it's the only path we found that bundles coverage checking, PA submission, insurer follow-up, timeline publication, and cash-pay fallback in one workflow with a dedicated insurance concierge. LillyDirect scored highest for self-pay pricing clarity and directness. Knownwell scored well for clinical care but lower for public PA documentation.
We have affiliate relationships with some providers on this page. That's disclosed at the top. Our recommendation is based on which provider solves this reader's specific problem most completely — and if the evidence changed, the recommendation would change with it.
Frequently asked questions
Does Foundayo always require prior authorization?
Not always, but PA is likely required on many commercial plans for GLP-1 weight-loss medications, and Foundayo will be no exception for most carriers. Self-pay routes through LillyDirect bypass PA entirely. Lilly's PA guide tells prescribers to begin the process as soon as the prescribing decision is made.
How do I know if my specific plan covers Foundayo?
Call the member services number on your insurance card and ask: 'Is Foundayo, generic name orforglipron, on your formulary? What tier? Is prior authorization required? What are the PA criteria?' Ro's coverage checker can also determine this for you as part of the onboarding process.
What BMI do I need for Foundayo coverage?
Foundayo's FDA-approved label is for adults with obesity, or adults with overweight plus at least one weight-related comorbidity. Live insurer criteria vary — Excellus BCBS requires BMI 40+ or BMI 35–39.9 with comorbidity. The Medicare GLP-1 Bridge has three tiers: BMI 35+, BMI 30+ with specific conditions, or BMI 27+ with specific conditions.
Can Ro do Foundayo prior authorization for me?
Yes. Ro checks your insurance coverage, tells you whether PA is required, submits all paperwork through its insurance concierge, and handles insurer back-and-forth. If coverage fails, your Ro provider suggests cash-pay alternatives. The process takes approximately 2–3 weeks.
What if my plan excludes weight-loss drugs entirely?
PA won't help if the medication category is excluded from your plan design. Your options are: self-pay through LillyDirect ($149–$349/month depending on dose), cash-pay through Ro or another telehealth provider, or pursuing a plan-design exception (difficult but not impossible).
Does Medicare cover Foundayo?
Not through standard Part D — weight-loss drugs are excluded by federal law. The Medicare GLP-1 Bridge covers Foundayo for eligible Part D beneficiaries at $50/month through a CMS central processor. The Bridge runs July 1, 2026–December 31, 2027 (18 months). BALANCE will not launch for Medicare Part D in 2027 — CMS extended the Bridge.
Is there a Foundayo savings card?
Yes. If your commercial plan covers Foundayo, the savings card reduces copays to as low as $25/month. If your commercial plan does not cover Foundayo, the card still offers reduced pricing at LillyDirect levels ($149–$299 depending on dose). Government insurance beneficiaries are not eligible. Card expires December 31, 2026.
What if my Foundayo prior authorization is denied?
Get the denial reason in writing, address the specific documentation gap, file an internal appeal with a letter of medical necessity, and request external review if the internal appeal fails. KFF data shows over 80% of Medicare Advantage PA appeals are at least partially overturned. You can start Foundayo self-pay at $149/month through LillyDirect while appeals process.
What happens when Foundayo prior authorization expires?
Reauthorization is likely. Lilly's PA guide says initial authorization typically lasts approximately 6–8 months. Plans may request updated BMI, adherence records, refill history, and evidence of continued benefit such as at least 5% weight loss from baseline.
Can I start Foundayo while waiting for PA approval?
Yes. LillyDirect self-pay starts at $149/month for the 0.8mg starter dose, and Ro offers cash-pay medication options. If insurance approves later, you can switch to covered pricing going forward.
Still not sure which GLP-1 program is right for you?
Take our free 60-second matching quiz. You'll get a personalized action plan based on your insurance situation, medication preferences, and whether Foundayo, an injectable, or a different option is actually the best fit.
Take the quiz — get your personalized GLP-1 action plan →