Insurance Coverage Guide · Last verified: May 14, 2026 · Updated quarterly
Does Blue Cross Cover Mounjaro? 2026 Coverage, Prior Authorization & Costs
Published: · Last reviewed:
By The RX Index Editorial Team
Verified against: FDA Mounjaro label (2026) · Eli Lilly pricing page · FEP Blue 2026 formulary · HCSC/BCBS Texas Basic Drug List (April 2026) · BCBSMA GLP-1 FAQ · BCBSM 2026 Clinical Drug List · Blue Cross NC Medicare Choice 2026 · BCBSMS medical policy (04/01/2026) · Lilly Mounjaro Savings Card terms
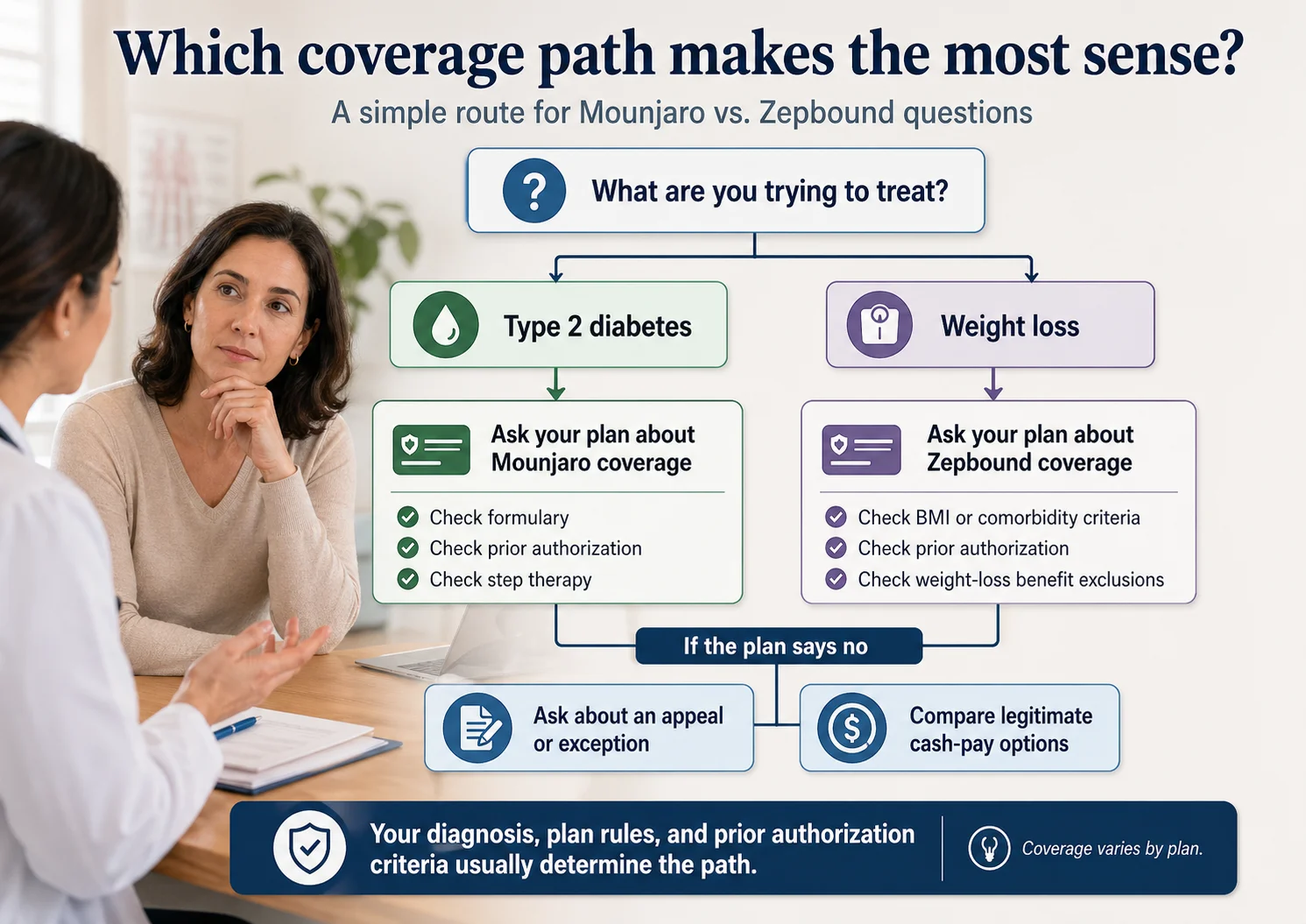
Yes — some Blue Cross plans cover Mounjaro, usually with prior authorization and usually when prescribed for type 2 diabetes — not weight loss. Mounjaro is FDA-approved for glycemic control in adults and children age 10+ with type 2 diabetes. With commercial coverage plus the Mounjaro Savings Card, eligible patients can pay as little as $25 per month. The exact answer depends on which Blue you're on, your diagnosis, and whether your doctor can satisfy the PA rules — details below.
Want to check your exact plan right now?
Ro's free GLP-1 Insurance Coverage Checker contacts your insurer and returns a personalized coverage report — including PA requirements. Takes about 3 minutes.
Does Blue Cross Cover Mounjaro? The Quick Answer
Some Blue Cross plans cover Mounjaro, usually when the prescription is tied to a documented type 2 diabetes diagnosis and the plan's prior authorization rules are satisfied. Coverage almost never works for off-label weight loss. The exact answer is plan-specific and lives in your formulary, not on any generic insurance website.
Blue Cross isn't one company. It's 33 independent, locally operated Blue Cross and Blue Shield companies under the Blue Cross Blue Shield Association — Anthem, Highmark, Excellus, BCBS of Texas, BCBS of Michigan, FEP Blue, Florida Blue, CareFirst, Independence Blue Cross, and others. Each one runs its own formulary, its own prior authorization rules, and its own tier system.
Here's what changes the answer:
| Your situation | Likely Blue Cross answer | What to do next |
|---|---|---|
| You have type 2 diabetes | Often possible — usually with prior authorization (PA), sometimes step therapy (ST) | Check your formulary, then have your doctor submit a PA with diagnosis, A1C, and prior medications |
| You want Mounjaro for weight loss only | Usually denied — Mounjaro is off-label for weight loss; Zepbound is the on-label tirzepatide brand for weight management | Ask your doctor about Zepbound — far more realistic insurance path |
| Mounjaro is listed but pharmacy says no | Could be PA, step therapy, a quantity limit (QL), the wrong pharmacy, or unmet deductible | Ask Blue Cross for the exact rejection code |
| You were already denied | Path forward depends on the type of denial | Use the denial decoder below before paying anyone |
| You have Medicare or Medicaid Blue | Different rules; manufacturer savings card not available | Check your plan's Part D or Medicaid formulary directly |
Mounjaro Coverage by Blue Cross Plan: What We Found in Official Documents
We pulled current formulary documents from six Blue Cross plans across the country and the Federal Employee Program. Mounjaro appears on many of them — but with prior authorization, step therapy, or quantity limits on top of the listing. “Listed” doesn't mean “approved.” Here's what we actually saw, verified May 14, 2026.
Mounjaro across six Blue Cross plans (verified May 14, 2026)
| Plan / source | What the document says | What this does NOT prove |
|---|---|---|
| FDA Mounjaro label (2026) | FDA-approved as an adjunct to diet and exercise to improve glycemic control in adults and pediatric patients age 10+ with type 2 diabetes | Doesn't prove FDA approval for weight loss; off-label use is at the prescriber's discretion |
| Eli Lilly pricing page | $1,112.16 list price per fill; actual cost depends on insurance, pharmacy charges, discounts, and assistance | Doesn't prove your final pharmacy receipt; pharmacies set their own retail markup |
| FEP Blue 2026 abbreviated formulary | Mounjaro listed under diabetes drugs as Tier 2 across BS / BB / BF; marked with the prior-approval symbol | Doesn't prove your specific FEP plan's deductible status or final out-of-pocket |
| HCSC / BCBS Texas Basic Drug List (April 2026) | Mounjaro listed with PA + QL: 2.5 mg = 4 pens / 180 days; 5 mg–15 mg = 4 pens / 28 days. Applies across BCBSIL, BCBSMT, BCBSNM, BCBSOK, BCBSTX | Doesn't prove non-Basic-list plans within the same companies have the same rules |
| BCBS Massachusetts GLP-1 FAQ | Coverage of GLP-1s for type 2 diabetes — Mounjaro included — is not changing; PA required, including documented T2D diagnosis | Doesn't prove BCBSMA's stance on weight-loss GLP-1 coverage, which is handled separately |
| BCBS of Michigan 2026 Clinical Drug List | Mounjaro listed as a preferred brand with step therapy and quantity limit markers | Doesn't tell you which step-therapy medications BCBSM requires for your plan |
| Blue Cross NC Medicare Choice 2026 | Mounjaro listed as Tier 3 with PA and a quantity limit of 4 pens / 28 days | Doesn't prove this tier applies to other Blue Cross Medicare plans — one plan example only |
| BCBS & Blue Shield of Mississippi medical policy (04/01/2026 update) | Mounjaro may be medically necessary when criteria are met: validated T2D documentation (e.g., A1C ≥ 6.5%), no duplicate DPP-4/GLP-1 use, no FDA-labeled contraindications. The 04/01/2026 update removed the prior metformin trial / intolerance requirement | Doesn't mean other Blue Cross plans dropped the metformin requirement — most still have step therapy |
Find your Blue Cross formulary faster
| Your plan | Where to find your formulary | What to search for | Symbols to look for |
|---|---|---|---|
| FEP Blue (federal employees) | fepblue.org → pharmacy → formulary | “Mounjaro” or “tirzepatide” | Diamond / prior-approval symbol |
| Anthem Blue Cross (multi-state) | anthem.com → pharmacy → member drug list | “Mounjaro” or “tirzepatide” | PA, ST, QL, NF flags |
| BCBS Texas / IL / MT / NM / OK (HCSC) | bcbstx.com (or your HCSC state site) → drug lists | “Mounjaro” or “tirzepatide” | PA, QL markers, dose-specific quantity limits |
| BCBS Massachusetts | bluecrossma.com → pharmacy benefits | “Mounjaro” or “tirzepatide” | PA, exclusion flags for weight-loss use |
| BCBS of Michigan | bcbsm.com → pharmacy → drug lists | “Mounjaro” or “tirzepatide” | Preferred brand + ST, QL markers |
| Blue Cross NC (commercial / Medicare) | bluecrossnc.com → pharmacy → formularies | “Mounjaro” or “tirzepatide” | Tier + PA, QL markers |
| BCBS Mississippi | bcbsms.com → medical policy / pharmacy | “Mounjaro” or “GLP-1 agonist” | Medical policy criteria |
| Florida Blue, CareFirst, Highmark, Independence Blue Cross, Excellus | Each company's member portal | “Mounjaro” or “tirzepatide” | Tier, PA, ST, QL flags |
The exact phone script
Copy this and read it on the call. These questions in this order get you the answer fastest.
Follow-up questions worth asking
- “What specific criteria must my doctor document in the PA?”
- “Do the rules differ by dose — for the 2.5 mg starter versus the 5–15 mg maintenance doses?”
- “What's the appeal deadline if it gets denied?”
- “Has my deductible been met for this plan year?”
Don't want to navigate the phone tree?
Ro's free GLP-1 Insurance Coverage Checker contacts your insurer and returns a personalized report including PA requirements. The free checker does not submit treatment requests or write prescriptions.
Does Blue Cross Cover Mounjaro for Type 2 Diabetes?
If you have type 2 diabetes, this is your strongest path. Mounjaro is FDA-approved for type 2 diabetes glycemic control, and most commercial Blue Cross plans list it on their formularies — usually with prior authorization, and sometimes with step therapy or quantity limits. Your odds of approval are real, but your doctor has to submit the right documents.
Why diabetes changes everything
Insurance companies evaluate medications against their FDA-labeled indication and the plan's clinical criteria. Mounjaro's label is type 2 diabetes. So when your prescription says “for type 2 diabetes,” Blue Cross is evaluating a request that matches the drug's approved use. When it says “for weight loss,” they're evaluating an off-label request — and that almost never wins.
Blue Cross Blue Shield of Massachusetts says it plainly in its public GLP-1 FAQ: coverage of GLP-1s approved to treat type 2 diabetes — Mounjaro included — is not changing, but PA is required with documented T2D diagnosis. Blue Cross & Blue Shield of Mississippi's April 2026 policy update spells it out further: validated type 2 diabetes documentation (such as A1C ≥ 6.5%), no duplicate DPP-4 / GLP-1 use, and no FDA-labeled contraindications. Notably, BCBSMS removed the prior metformin trial requirement in that update.

What your doctor probably needs to submit
This is the pattern across Blue Cross plans we've reviewed. Your specific plan may want more, less, or different details — pull your plan's published PA criteria document for the authoritative version.
- ✓Confirmed type 2 diabetes diagnosis — with date of diagnosis
- ✓ICD-10 code — typically the E11.x family for type 2 diabetes mellitus
- ✓Recent A1C or lab confirmation — many plans want labs that establish the diagnosis; BCBSMS accepts A1C ≥ 6.5%
- ✓Medication history — documenting other diabetes meds you've tried
- ✓Step-therapy documentation — if your plan requires it — metformin is common but BCBSMS removed this requirement in April 2026
- ✓"Adjunct to diet and exercise" noted in the chart — the FDA label requires this framing
- ✓Comorbidities documented — if relevant — hypertension I10, dyslipidemia E78.5, obstructive sleep apnea G47.33
- ✓Contraindications ruled out — no personal or family history of medullary thyroid carcinoma (MTC) or Multiple Endocrine Neoplasia syndrome type 2 (MEN 2)
- ✓Letter of medical necessity — from the prescriber explaining specifically why Mounjaro is the right choice for this patient
A letter-of-medical-necessity pattern that works
Roughly, the structure that gets approved looks like this. Your doctor will use their own clinical language:
Specifics win PAs. Vague statements like “patient failed metformin” don't. Your doctor needs the exact A1C, the exact medication, the exact duration, and the exact reason it didn't work.
“Listed” is not the same as “approved”
This trips up a lot of people. You look up Mounjaro on your plan's drug list. It's there. You think you're set. Then the pharmacy hits you with a rejection — because most Blue Cross plans attach markers:
| Symbol | Meaning |
|---|---|
| PA | Prior authorization required — your doctor must submit paperwork before the pharmacy can dispense |
| ST | Step therapy required — you may have to try a different medication first |
| QL | Quantity limit — the plan caps how many pens or how often you can fill |
| NF | Non-formulary — not on the plan's standard drug list; you may need a formulary exception |
A listing with PA + ST + QL means three different conditions to clear. Find those markers next to the drug name on your formulary, and you'll know exactly what to expect.
Need a Mounjaro-capable provider?
Sesame providers can prescribe Mounjaro if appropriate and assist with prior authorization paperwork. Blue Cross still decides coverage — Sesame doesn't override plan rules.
Does Blue Cross Cover Mounjaro for Weight Loss?
Almost never — and we'd rather be straight with you than waste your time. Mounjaro is FDA-approved for type 2 diabetes, not weight management. The tirzepatide brand your insurance fight usually points to for weight loss is Zepbound — same manufacturer (Eli Lilly), same active ingredient (tirzepatide), but FDA-approved for weight management and obstructive sleep apnea. That's the coverage path that actually works for weight loss.

If you don't have type 2 diabetes and your real goal is weight loss, pushing for Mounjaro through Blue Cross is the hard road, and you'll usually lose. Insurers have tightened off-label denials. Some Blue Cross plans now exclude GLP-1s for weight loss entirely. Even when prior authorization is technically available, the criteria require type 2 diabetes documentation that you don't have.
The tirzepatide brand your insurance company is actually willing to evaluate for weight loss is Zepbound — same molecule, different FDA-approved brand, different insurance rules.
Mounjaro vs Zepbound — the difference that matters for your wallet
| Mounjaro | Zepbound | |
|---|---|---|
| Active ingredient | Tirzepatide | Tirzepatide (same molecule) |
| FDA-approved use | Type 2 diabetes glycemic control | Chronic weight management; moderate-to-severe obstructive sleep apnea in adults with obesity |
| Manufacturer | Eli Lilly | Eli Lilly |
| Blue Cross coverage for T2D | Often yes — with PA | Not typically prescribed for T2D |
| Blue Cross coverage for weight loss | Usually denied — off-label | Plan-dependent — more realistic than Mounjaro, but some plans still exclude GLP-1s for weight loss |
| Doses | 2.5, 5, 7.5, 10, 12.5, 15 mg weekly | Same doses, same titration schedule |
| Cash-pay options | List price ~$1,112.16/fill; savings card for eligible commercial patients | Zepbound Self Pay via LillyDirect: $299/mo for 2.5 mg, $399/mo for 5 mg, $449/mo for 7.5–15 mg under program terms |
When you should ask about Zepbound instead
- You don't have a type 2 diabetes diagnosis
- Your goal is weight management
- Your Blue Cross plan denied your Mounjaro request as off-label
- You have moderate-to-severe obstructive sleep apnea with obesity (an FDA-approved Zepbound indication)
- You want the most realistic shot at insurance coverage for tirzepatide
One honest caveat: even Zepbound can be excluded by some plans that block GLP-1s for weight management. Check your formulary or run a free coverage check before assuming Zepbound will be covered.
Pursuing weight loss instead of T2D coverage?
Ro's current program lists Zepbound as a covered GLP-1 path with insurance, and their concierge submits PA paperwork on your behalf. Ro Body: $39 first month, then as low as $74/mo with annual plan — medication billed separately.
What You'll Actually Pay for Mounjaro With Blue Cross in 2026
With commercial Blue Cross coverage that approves Mounjaro for type 2 diabetes plus the Mounjaro Savings Card, eligible patients can pay as little as $25 per month for up to a 3-month fill. Without coverage, eligible commercially insured patients may pay as low as $499 per 1-month fill through the savings card. The cash list price without any program is around $1,112.16 per fill. Government-insured patients can't use the savings card.
| Your situation | Estimated monthly cost | What drives the number |
|---|---|---|
| Commercial Blue Cross covers Mounjaro + savings card eligible | As low as $25 | Lilly Savings Card pulls covered copay to $25 floor; max monthly savings $150/$300/$450 by fill length; annual cap $1,950 |
| Commercial Blue Cross covers Mounjaro, no savings card | $30 – $150+ | Plan-specific Tier 2 or 3 copay or coinsurance |
| Commercial Blue Cross doesn't cover Mounjaro, savings card eligible | As low as $499 | Card reduces non-covered fill; max savings up to $647 per fill, up to $8,411 annual per Lilly's current terms |
| Commercial Blue Cross, no coverage, no card | $1,000 – $1,481+ | Cash list price plus pharmacy markup |
| Blue Cross before deductible met | Often near list price | High-deductible plans can require $2,000–$5,000 spend before coverage activates |
| Medicare Blue Cross Part D, covers Mounjaro | Varies by plan | In 2026, covered Part D drug out-of-pocket spending is capped at $2,100/year; after that, covered Part D drugs are $0 |
| Medicaid Blue Cross | State-dependent; savings card NOT available | Federal anti-kickback rules block the savings card on government-funded plans |
A quick word on the Mounjaro Savings Card
The Mounjaro Savings Card is the single biggest reason eligible patients pay $25 instead of $1,100. Per Lilly's current published terms:
- →If your commercial insurance covers Mounjaro: card pulls your copay down to as little as $25 per 1-, 2-, or 3-month fill, with maximum monthly savings of $150 / $300 / $450 and an annual cap of $1,950
- →If your commercial insurance doesn't cover Mounjaro: eligible commercially insured patients may pay as low as $499 per 1-month fill, with maximum savings up to $647 per fill and annual savings up to $8,411
- →Government insurance excluded: Lilly's terms list Medicaid, Medicare, Medicare Part D, Medicare Advantage, Medigap, DoD, VA, TRICARE/CHAMPUS, and state prescription drug assistance programs. FEHB members should verify directly with Lilly
You must have a Mounjaro prescription for type 2 diabetes, be 18+, and reside in the US or Puerto Rico. Enroll at mounjaro.lilly.com/savings-resources or text MJ to 85099. Verify current terms before each refill — Lilly updates these periodically.
Want a real cost estimate for your specific plan?
Ro's free coverage checker contacts your insurer and returns a personalized cost report — fastest way to find out if you're in the $25/month bucket, the $499/month bucket, or the full-price bucket.
Blue Cross Mounjaro Prior Authorization: What Your Doctor Needs to Submit
Most Blue Cross plans require prior authorization for Mounjaro. Approvals usually hinge on a documented type 2 diabetes diagnosis, lab confirmation of the diagnosis, no duplicate DPP-4 / GLP-1 use, and no FDA-labeled contraindications. Some plans add step therapy on top. Decision turnaround varies by plan and request type.
The PA documentation checklist
This is the pattern we see across the Blue Cross plans we reviewed. Pull your plan's formulary and PA criteria document for the authoritative version.
- ✓Confirmed type 2 diabetes diagnosis with date of diagnosis
- ✓ICD-10 code (typically E11.x for type 2 diabetes mellitus)
- ✓A1C or lab confirmation — BCBSMS accepts A1C ≥ 6.5% per its current policy
- ✓Medication history documenting other diabetes meds tried
- ✓Step-therapy documentation if your plan requires it — read your PA criteria to know which drugs count
- ✓No duplicate DPP-4 / GLP-1 use confirmed
- ✓Chart note confirming "adjunct to diet and exercise" — the FDA label requires this framing
- ✓Comorbidities documented if relevant (hypertension I10, dyslipidemia E78.5, OSA G47.33)
- ✓Contraindications ruled out — no personal or family history of MTC or MEN 2
- ✓Letter of medical necessity explaining specifically why Mounjaro is the right choice for this patient
Step therapy: when it applies
“Step therapy” means the plan wants you to try cheaper or more established medications before approving the expensive one. The exact rule varies by plan:
- BCBS of Michigan's 2026 Clinical Drug List marks Mounjaro with step-therapy flags — typically requiring a designated Step 1 medication first
- BCBS Massachusetts treats Mounjaro as part of a step-up sequence for type 2 diabetes management
- BCBS Mississippi's 04/01/2026 policy update removed the prior metformin trial / intolerance requirement — a notable departure from the step-therapy pattern
Don't assume metformin is universal. Pull your plan's published PA criteria document and read it before guessing.
How long approval takes
| Request type | Typical turnaround |
|---|---|
| Standard PA (commercial) | Many decisions come back within 24–72 hours of complete submission |
| Expedited PA (urgent health concerns) | Typically faster — Medicare and many commercial plans target 24-hour decisions once supporting information is received |
| Medicare formulary exception (standard) | 72 hours once supporting information is received |
| Medicare formulary exception (expedited) | 24 hours once supporting information is received |
Want help running this fight?
Sesame providers can prescribe Mounjaro if appropriate and assist with prior authorization paperwork. Blue Cross still decides coverage; Sesame doesn't override plan rules.
Why Did Blue Cross Deny My Mounjaro? The Denial Decoder
A Blue Cross denial isn't one thing — it's seven different things, and the right fix depends on which kind of “no” you got. Pull out your denial letter — we'll show you exactly what each one means and what to do next.
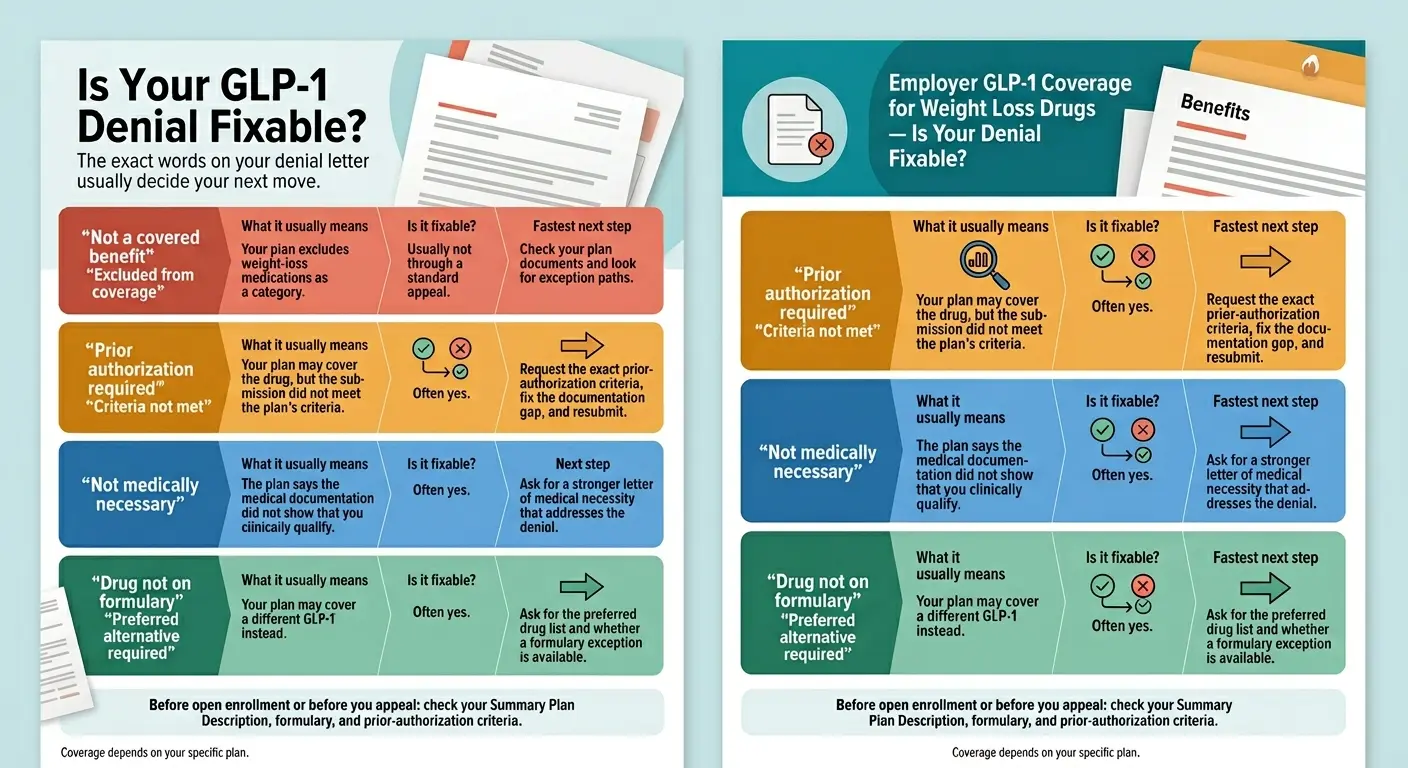
| Denial reason on the letter | What it actually means | Your best next step |
|---|---|---|
| “Prior authorization required” | Blue Cross hasn't reviewed medical necessity yet — your doctor needs to submit the PA | Have your doctor submit the PA with diagnosis, A1C, and medication history |
| “Prior authorization denied” | Blue Cross reviewed but says the criteria weren't met | Get the denial letter, identify the exact missing criterion, and appeal with that gap closed |
| “Step therapy required” | The plan wants you to try a different medication first | Document past trials, or ask for a step-therapy exception with clinical justification |
| “Quantity limit exceeded” | The dose, days-supply, or refill timing doesn't match the plan's limit | Have your doctor or pharmacy adjust days supply, or request a QL exception |
| “Non-formulary” | Mounjaro isn't on your plan's standard drug list | Request a formulary exception with documentation of medical necessity |
| “Benefit excluded” | The plan doesn't cover this drug or category at all | Ask HR about adding an employer rider; consider Zepbound for weight-loss intent; or compare cash-pay paths |
| “Pharmacy not in network” or “specialty pharmacy required” | The drug needs a different pharmacy than the one you used | Ask Blue Cross which pharmacy is required for Mounjaro and transfer your prescription |
What to Do After a Blue Cross Mounjaro Denial
Match your next move to the kind of denial you got. PA denials are appealable with better documentation. Step-therapy denials usually need proof of past trials. Benefit exclusions need a different strategy entirely. Most commercial plans give you 180 days to file an internal appeal.
If it was a PA denial
- Request the denial letter in writing if you don't already have it. The exact denial reason matters.
- Identify the specific criterion that wasn't met. Was it A1C threshold? Step therapy? Missing chart notes?
- Have your doctor request a peer-to-peer (P2P) review. This is a phone call between your prescriber and Blue Cross's medical director. P2P reviews often resolve denials faster than written appeals.
- File a written internal appeal if P2P doesn't work. Typical deadline: 180 days from denial. Include the denial letter, a new letter of medical necessity, any new labs, and a clinical justification that closes the gap from the denial.
- File an external review if the internal appeal fails. Each state runs its own external review process through the Department of Insurance. New York gives you 4 months from the final adverse determination. California runs Independent Medical Review (IMR) through DMHC.
If it was a step-therapy denial
- Ask exactly which medications Blue Cross wants you to try first
- Document any past trials with dose, duration, outcome — same level of specificity as the original PA
- If you can't try the required step (medical contraindication, prior intolerance, drug interaction), request a step-therapy exception with clinical justification
If it was a benefit exclusion
- Ask your HR department whether your employer offers (or could add) a GLP-1 rider — open enrollment is the time to push
- If your goal is weight management, ask your clinician about Zepbound — it's the on-label tirzepatide brand for that use, though some plans still exclude GLP-1s for weight loss
- Compare cash-pay FDA-approved options, including LillyDirect's Zepbound Self Pay program ($299/mo for 2.5 mg, $399/mo for 5 mg, $449/mo for 7.5–15 mg under program terms)
If your pharmacy quoted full price but Blue Cross says it's covered
This is more common than people realize. Run through this checklist:
- Was the PA actually approved? (Many “denials” are PAs not yet submitted.)
- Did the pharmacy run the claim under the correct insurance?
- Is the pharmacy in your plan's network for this drug?
- Is the prescription written for the correct days supply (28 days, typically)?
- Is the dose subject to a quantity limit you're exceeding?
- Has your annual deductible been met?
- Was the savings card applied at the counter?
- Is the pharmacy using the right BIN/PCN/group from your savings card?
Need help re-submitting your PA or appeal?
Sesame providers can write the prescription and assist with the documentation fight. Blue Cross coverage still depends on your specific plan.
How Sesame Can Help With Mounjaro and Blue Cross Prior Authorization
Sesame is the most direct telehealth path for Mounjaro specifically because Sesame's public Mounjaro page states their providers can prescribe Mounjaro if appropriate and assist with prior authorization paperwork. Blue Cross still decides coverage, but Sesame can write the prescription and help with the PA.
When Sesame makes sense for you
- You have type 2 diabetes (or your doctor believes Mounjaro is clinically appropriate)
- You need a Mounjaro prescription sent to your local or preferred pharmacy
- You want help with prior authorization paperwork
- You don't already have an in-person clinician who can or will navigate the PA fight
- You understand that medication coverage is still plan-specific — Sesame can do the clinical work, but they can't override your plan's rules
Provider-stated vs. verified
| Sesame says | Verified? | What this means for you |
|---|---|---|
| Sesame providers can prescribe Mounjaro if appropriate | ✓ Verified on Sesame's public Mounjaro page (May 14, 2026) | Sesame can write the prescription |
| Sesame providers assist with prior authorization paperwork | ✓ Verified on Sesame's public Mounjaro page (May 14, 2026) | Sesame can help with PA documentation |
| Sesame guarantees Blue Cross approval | ✗ Not offered | Blue Cross's plan rules still control coverage |
| Sesame replaces in-person endocrinology care | ✗ Not offered | If you need ongoing complex diabetes care, work with your in-person clinician too |
Real Sesame patient quotes
Pulled from Sesame's public review section. These are service-experience reviews — not evidence of Mounjaro coverage outcomes, medical results, or what your specific Blue Cross plan will approve.
“Sesame is a dream. The doctor they paired me with was kind, empathetic, explained everything thoroughly.”
“The prices are great too. Easy to navigate and fast to get appointments and prescriptions.”
See if a Sesame provider can help with your Mounjaro prescription and PA
Visit cost is transparent — keep your existing pharmacy and insurance.
How Ro Can Help (and Where Ro Can't)
Ro runs a free GLP-1 Insurance Coverage Checker that contacts your insurer and returns a personalized GLP-1 coverage report. The free checker doesn't submit treatment requests or write prescriptions. Ro's published Mounjaro page says Mounjaro is not currently available through Ro — their tirzepatide path is Zepbound for weight management.
When Ro is genuinely useful here
- For a free GLP-1 coverage check: Ro's GLP-1 Insurance Coverage Checker contacts your insurer and returns a report on which GLP-1 medications your plan covers and what PA requirements apply. The free checker does not submit treatment requests or write prescriptions
- For the Zepbound pivot: If you're really after weight loss, Ro's current pricing page lists Zepbound KwikPen (cash-pay) and Zepbound pen (through insurance) as options. Their insurance concierge submits PA paperwork on your behalf for branded GLP-1s and resubmits if denied
- Ro Body membership pricing: $39 for the first month, then as low as $74/month with annual plan paid upfront — otherwise $149/month. Medication is billed separately. Ro Body itself is cash-pay; insurance doesn't pay for the membership
Provider-stated vs. verified
| Ro says | Verified? | What this means for you |
|---|---|---|
| Free GLP-1 Insurance Coverage Checker contacts insurer and returns personalized report | ✓ Verified on ro.co (May 14, 2026) | Free coverage orientation, no commitment |
| Free checker does not submit treatment requests or write prescriptions | ✓ Verified on ro.co (May 14, 2026) | Use the checker for coverage info; separate path needed for a prescription |
| Mounjaro is not currently available through Ro | ✓ Verified on ro.co (May 14, 2026) | If you specifically need a Mounjaro prescription, Ro isn't the path — see Sesame or your prescriber |
| Ro carries Zepbound KwikPen (cash-pay) and Zepbound pen (through insurance) | ✓ Verified on ro.co pricing page (May 14, 2026) | Zepbound is the tirzepatide path through Ro |
When Ro isn't the right tool
- You want Mounjaro specifically prescribed. Ro doesn't prescribe Mounjaro
- You're on Medicare, Medicaid, TRICARE, VA, or IHS. Ro's concierge doesn't coordinate with most government plans for GLP-1 medication coverage
- You want a compounded GLP-1. Ro doesn't lead with compounded, and compounded medications are not FDA-approved finished products
Check my GLP-1 coverage free with Ro
Best if you want a free insurer-contact report on which GLP-1 your plan covers.
Check coverage free → (sponsored affiliate link, opens in a new tab)See Zepbound coverage with Ro
Best if your real goal is weight loss and you want Ro's concierge handling the PA.
See Zepbound with Ro → (sponsored affiliate link, opens in a new tab)Mounjaro vs Zepbound: Which Question Are You Really Asking?
If you have type 2 diabetes, you're asking the Mounjaro question — and your insurance path is real if your plan covers GLP-1s for diabetes (most commercial Blue Cross plans we checked do, with PA). If your real goal is weight loss, you're asking the Zepbound question — same molecule, different FDA-approved brand, different insurance path.
If you're not sure which question is really yours, ask yourself two things:
- Has a clinician diagnosed me with type 2 diabetes, and is my A1C above target despite treatment?
- Or am I trying to lose weight, with or without a weight-related comorbidity?
If yes to #1: pursue Mounjaro. The strongest path is a complete PA submission and (if needed) appeal.
If yes to #2: pursue Zepbound. The strongest path is a clinician who treats obesity, plus a coverage check on your plan's GLP-1-for-weight-loss benefits before you commit.
For diabetes intent
See if a Sesame provider can help with Mounjaro and your PA
See Sesame Mounjaro → (sponsored affiliate link, opens in a new tab)For weight-loss intent
Check Zepbound coverage with Ro — PA concierge included
Check Zepbound with Ro → (sponsored affiliate link, opens in a new tab)Special Situations
Does FEP Blue (Federal Employee Program) cover Mounjaro?
FEP Blue's 2026 abbreviated formulary lists Mounjaro under diabetes drugs as Tier 2 across the BS / BB / BF benefit options, marked with the prior-approval symbol. FEP's own prior-approval rules apply — not the same rules as commercial Blue Cross plans.
Find your FEP Blue formulary at fepblue.org or in your member portal. The standard FEP PA requirements apply: type 2 diabetes documentation, ICD-10 code, lab confirmation, medication history, and any step-therapy criteria specific to your benefit option. The diamond / prior-approval symbol on the formulary is your flag.
Does Blue Cross Medicare Advantage or Part D cover Mounjaro?
Some Medicare Blue Cross plans cover Mounjaro for type 2 diabetes; not all do. The Blue Cross NC Medicare Choice 2026 formulary lists Mounjaro as Tier 3 with PA and a quantity limit of 4 pens / 28 days — but that's one plan example, not a universal Blue Cross Medicare rule. In 2026, covered Part D drug out-of-pocket spending is capped at $2,100 per year. The Mounjaro Savings Card is not available with Medicare.
Check your specific Medicare plan's Annual Notice of Change and formulary. If Mounjaro is non-formulary on your plan, ask about a formulary exception. If the tier puts your copay out of reach early in the year, the $2,100 Part D out-of-pocket cap activates once you hit it — meaning your covered Part D drug spend is capped for the rest of the year.
Does Blue Cross Medicaid cover Mounjaro?
Coverage varies by state. Some state Medicaid programs (often through managed-care Blue Cross plans) cover Mounjaro for type 2 diabetes with PA; weight-loss coverage is rare to none. The manufacturer savings card is not available on Medicaid plans.
Check your state's preferred drug list. If Mounjaro is non-preferred, your prescriber can request a non-preferred drug authorization.
I get Blue Cross through my employer — does my employer affect coverage?
Yes, in part. Many large employer plans are “self-insured,” meaning the employer — not Blue Cross — sets the benefit design and chooses which drug categories to cover. Blue Cross simply administers the plan. Self-insured plans can include or exclude GLP-1s for weight management; your formulary will tell you, and your HR Summary Plan Description (SPD) is the authoritative document.
If your formulary excludes GLP-1s for weight loss, ask HR whether a GLP-1 rider is available for next plan year. Open enrollment is the time to push for it.
What if Blue Cross drops Mounjaro from the formulary mid-year?
For Medicare drug plans, mid-year formulary change notice and transition rules follow Medicare requirements. For commercial and employer plans, notice and transition rights depend on your specific plan documents and applicable law.
Keep the notice, check whether your active PA continues through the change, and ask about a formulary exception or transition fill before you run out.
What Doesn't Work: A Word on Compounded “Mounjaro Alternatives”
Some telehealth providers advertise compounded tirzepatide as a cheaper alternative to Mounjaro. Two things we won't blur for you:
- Compounded tirzepatide is not FDA-approved. Mounjaro is. They are not regulatory equivalents
- The official Blue Cross plan documents we checked do not establish a coverage path for compounded tirzepatide. Compounded GLP-1 cash-pay programs are generally sold outside insurance
If you're looking for a cash-pay path because Blue Cross said no, the more honest comparison is between branded options — Mounjaro through Lilly's savings programs, Zepbound's Self Pay program via LillyDirect ($299/mo for 2.5 mg, $399/mo for 5 mg, $449/mo for 7.5–15 mg under program terms), or other FDA-approved GLP-1s your plan does cover.
How We Built This Page
The RX Index is a pricing intelligence and comparison resource for GLP-1 telehealth providers. For this page, we cross-referenced:
- The official FDA Mounjaro prescribing information (label) updated 2026
- Eli Lilly's published Mounjaro pricing page (pricinginfo.lilly.com) and Mounjaro Savings Card current terms
- Six current Blue Cross plan formulary or coverage documents: FEP Blue 2026 abbreviated formulary; HCSC / BCBS Texas Basic Drug List (April 2026); BCBS Massachusetts GLP-1 FAQ; BCBS of Michigan 2026 Clinical Drug List; Blue Cross NC Medicare Choice 2026 formulary; and BCBS Mississippi medical policy (04/01/2026)
- Ro's public weight-loss program and Mounjaro pages (to verify what Ro actually does and doesn't prescribe)
- Sesame's public Mounjaro page (to verify prescribing scope and PA assistance language)
- CMS's 2026 Medicare Part D out-of-pocket cap
We earn affiliate commissions from some of the providers we mention, including Ro and Sesame. Affiliate compensation does not affect which information we publish. If a provider's marketing claim doesn't match their published policy page, we side with the policy page. If a coverage approach doesn't work for our reader, we say so plainly — even when it costs us a click.
Coverage policies change. We re-verify this page quarterly and immediately after any major label or pricing update. The “last verified” date at the top reflects the most recent check.
Last verified:
Frequently Asked Questions
Does Blue Cross cover Mounjaro?
Some Blue Cross plans cover Mounjaro, usually with prior authorization and usually when prescribed for type 2 diabetes. Coverage for off-label weight loss is rare. Because Blue Cross is 33 independent companies, your specific plan's formulary is the only authoritative answer.
Does Blue Cross cover Mounjaro for weight loss?
Usually no. Mounjaro is FDA-approved for type 2 diabetes, not weight loss. The on-label tirzepatide brand for weight management is Zepbound, which is more likely to be considered for coverage when prescribed for weight loss — though some Blue Cross plans still exclude GLP-1s for weight loss entirely.
How much is Mounjaro with Blue Cross?
With commercial Blue Cross coverage for type 2 diabetes plus the Mounjaro Savings Card, eligible patients can pay as little as $25 per month. If your commercial plan doesn't cover Mounjaro, eligible commercially insured patients may pay as low as $499 per 1-month fill through the savings card. Without coverage and without the card, the cash list price is around $1,112.16 per fill.
Can I use the Mounjaro Savings Card with Blue Cross?
Yes if you have commercial (private) Blue Cross insurance. The card cannot be used with Medicaid, Medicare, Medicare Part D, Medicare Advantage, Medigap, DoD, VA, TRICARE/CHAMPUS, or state prescription drug assistance programs, per Lilly's current terms. FEHB members should verify directly with Lilly and the pharmacy.
What does Blue Cross prior authorization for Mounjaro require?
Most Blue Cross plans want a documented type 2 diabetes diagnosis with ICD-10 code, lab confirmation of the diagnosis (BCBSMS accepts A1C of 6.5% or higher per its current policy), no duplicate DPP-4 or GLP-1 use, and no FDA-labeled contraindications. Some plans add step therapy. The specific PA criteria document for your plan controls.
Why did Blue Cross deny my Mounjaro?
Common reasons include missing prior authorization, PA criteria not met, step therapy required, quantity limit exceeded, non-formulary status, pharmacy network issues, or a benefit exclusion. The denial letter identifies which one applies.
Does FEP Blue cover Mounjaro?
FEP Blue's 2026 abbreviated formulary lists Mounjaro under diabetes drugs as Tier 2 across the BS, BB, and BF benefit options, with the prior-approval symbol. FEP's own prior-approval rules apply.
Does Anthem Blue Cross cover Mounjaro?
Anthem Blue Cross coverage varies by state, employer plan, and pharmacy benefit. Check your Anthem member formulary for Mounjaro or tirzepatide and look for tier, PA, ST, and QL markers. Formulary inclusion does not guarantee the drug is a covered benefit.
Does Blue Cross Blue Shield of Texas cover Mounjaro?
Per the HCSC Basic Drug List (April 2026), Mounjaro is listed with PA and quantity limits: 2.5 mg = 4 pens per 180 days, and 5 mg through 15 mg = 4 pens per 28 days. Coverage applies across BCBSIL, BCBSMT, BCBSNM, BCBSOK, and BCBSTX.
Does Blue Cross Blue Shield of Michigan cover Mounjaro?
BCBSM's 2026 Clinical Drug List lists Mounjaro as a preferred brand with step therapy and quantity limit markers. Verify your specific plan's PA criteria.
Should I ask my doctor for Zepbound instead of Mounjaro?
If your goal is weight management and you don't have type 2 diabetes, ask your clinician whether Zepbound is the more appropriate on-label tirzepatide question. Zepbound is FDA-approved for chronic weight management and for moderate-to-severe obstructive sleep apnea in adults with obesity.
Can Ro prescribe Mounjaro?
No. Ro's published Mounjaro page states Mounjaro is not currently available through Ro. Ro's tirzepatide path is Zepbound for weight management. The free Ro GLP-1 Insurance Coverage Checker does not submit treatment requests or write prescriptions.
Can Sesame prescribe Mounjaro?
Sesame's public Mounjaro page says their providers can prescribe Mounjaro if appropriate and assist with prior authorization paperwork. Blue Cross coverage still depends on the patient's specific plan.
How long does Blue Cross prior authorization take for Mounjaro?
Turnaround depends on the plan and request type. Medicare formulary exceptions commonly use 72 hours for standard decisions and 24 hours for expedited decisions once supporting information is received. Commercial PA timing varies by plan and PBM; many decisions return within 24 to 72 hours.
What if my Blue Cross plan has a benefit exclusion for weight-loss medications?
Then no PA will get Mounjaro covered for weight loss on that plan. Realistic paths: ask HR about adding a GLP-1 rider, ask your clinician about Zepbound (still subject to your plan's GLP-1 exclusion rules), or compare cash-pay FDA-approved options.
Still Not Sure Which GLP-1 Path Is Right for You?
If you've made it this far and you're still trying to figure out whether to fight for Mounjaro, switch to Zepbound, or try a different path entirely — that's normal. Insurance decisions are layered, and the right answer depends on your diagnosis, your plan, your state, and your goals.
Take our free 60-second GLP-1 matching quiz
We'll ask a few questions about your goal, insurance, state, and medical situation, then return a personalized action plan: which medication to ask about, which coverage path to check, and which provider fits your situation. Free to use.