Affiliate disclosure: The RX Index earns a commission when you sign up with some of the providers mentioned on this page. It does not affect what you pay, and it never determines our rankings or which providers we cover. Read the full disclosure.
GLP-1 Providers That Accept TRICARE: What Actually Works in 2026
Published: · Last reviewed:
By The RX Index Editorial Team · Updated when DHA or Express Scripts publishes changes

Affiliate disclosure: Some links on this page are affiliate links. If you sign up, we may earn a commission at no extra cost to you. Affiliate relationships do not influence rankings. Read the full disclosure.
Medical disclaimer: This guide covers coverage and access information only. It is not medical advice. Talk to a licensed clinician before starting, changing, or stopping any prescription medication.
The short answer most people don't want to hear
“GLP-1 providers that accept TRICARE” is almost the wrong question. TRICARE doesn't pay a telehealth app — it pays through Express Scripts, the company that runs the TRICARE Pharmacy Program. Your real goal isn't to find a flashy online clinic that “takes TRICARE.” It's to find a TRICARE-authorized prescriber who'll write the right script, submit the prior authorization (PA), and let Express Scripts fill it. The guide below shows you exactly which path fits your plan.
Your TRICARE plan, your fastest first move
| Your TRICARE Plan | Fastest First Move | Realistic Cost |
|---|---|---|
| Active Duty (Prime / Prime Remote) | Your PCM at an MTF | $0 |
| TRICARE Prime / Select (dependents & retirees) | PCM or any TRICARE-network civilian doctor | Visit cost-share + $44 for a 90-day Wegovy or Zepbound supply via Home Delivery |
| Reserve Select, Young Adult, Retired Reserve, CHCBP | Same as Prime/Select | Same as above |
| TRICARE For Life (Medicare-eligible retirees) | Weight-loss GLP-1 coverage ended Aug 31, 2025. Diabetes GLP-1s for type 2 diabetes are still covered. For weight loss, you're now on a cash-pay path. | Cash-pay platform pricing (see cash-pay section below) |
| US Family Health Plan (USFHP) | USFHP runs its own pharmacy plan — verify directly with your USFHP site | Plan-specific |
| Direct Care Only | TRICARE no longer covers weight-loss drugs for direct-care-only beneficiaries. Talk to your MTF about diabetes-route options if applicable. | Full cost off-base |
Not sure which plan you have, or what to do if your PCM said no?
Take our free 60-second TRICARE GLP-1 Path Finder. Answer a few questions, get your exact next step — no provider recommendation until we know whether TRICARE coverage is realistic for your situation.
→ Check My TRICARE GLP-1 PathDo any GLP-1 providers actually accept TRICARE?
Quick answer
Yes — but probably not the way you're picturing it. TRICARE coverage runs through three separate gates: a prescriber, an approved prior authorization (PA), and a TRICARE pharmacy. A telehealth provider “accepts TRICARE” only when its visit is billed to TRICARE and it can plug into all three gates. Most cash-pay GLP-1 apps don't.

The three-component TRICARE system, in plain English
1. The prescriber
For a Wegovy or Zepbound weight-loss prescription that TRICARE will cover, the cleanest path is an MTF provider or a TRICARE Network provider who has billed TRICARE for professional services and can complete the Express Scripts PA. A telehealth provider who can't confirm network status and PA support is effectively cash-pay for the visit — even if they say they “accept insurance.”
2. The prior authorization (PA)
This is the paperwork TRICARE requires before it will cover Wegovy, Zepbound, Saxenda, or the diabetes GLP-1s. The prescriber fills it out. Express Scripts approves or denies it. The exact form requirements are covered in the PA section below.
3. The pharmacy benefit
Once your PA is approved, the medication gets filled at one of three places: TRICARE Pharmacy Home Delivery (mail-order, the cheapest non-MTF option), a TRICARE network retail pharmacy (like an in-network CVS or Walgreens), or an MTF pharmacy if your base stocks it. This step is run by Express Scripts.
The damaging admission (because trust matters more than a click)
We could send you straight to a telehealth checkout and earn a commission on the click. That's not the right first move if your real goal is TRICARE coverage. TRICARE's covered path runs through a network or authorized prescriber, a real PA, and a TRICARE pharmacy — not just a slick telehealth checkout flow. Cash-pay telehealth is a fine fallback. It's a bad first move when TRICARE will pay $0 to $44 instead of the $300+/month you'd spend cash.
What “accepts TRICARE” really means, in a checklist
Before you book any provider visit, ask these five questions:
- 1Does this provider bill TRICARE for the visit?
- 2Is this provider a TRICARE Network provider (or MTF) who has billed TRICARE for professional services?
- 3Will this provider complete the Express Scripts/TRICARE prior authorization form for my GLP-1?
- 4Will they document the things the PA form actually asks for — my BMI, my comorbid conditions, my six months of lifestyle changes, and any older weight-loss medications I tried?
- 5Can they send the prescription to TRICARE Pharmacy Home Delivery, a TRICARE network retail pharmacy, or my MTF pharmacy?
If you get a clear “yes” on all five, that's a real TRICARE GLP-1 provider. If you get vague answers — especially on PA paperwork — that's a cash-pay program in disguise.
How do you find a TRICARE network provider for GLP-1 care?
Quick answer
Start with your PCM, your local MTF, or your regional TRICARE contractor's online provider directory. Filter for primary care, endocrinology, obesity medicine, or weight-management experience. Before booking, ask three questions: do you bill TRICARE, are you in-network, and do you complete Express Scripts PA forms for Wegovy or Zepbound? If the answer to any is no, keep looking.
The five-step provider search
- 1.Start with your PCM. If you're on Prime, your PCM is your assigned doctor. They're already TRICARE-network. Book the visit. This is the easiest path.
- 2.If your PCM is slow or said no, request a referral. On Prime, ask for a referral to obesity medicine or endocrinology. On Select, you have more flexibility to self-refer to any TRICARE-network specialist.
- 3.Use your regional TRICARE provider directory. TRICARE East (Humana Military) and TRICARE West (TriWest) both maintain online provider directories. Search by specialty (primary care, internal medicine, endocrinology, family medicine, obesity medicine) and verify in-network status before booking.
- 4.Call before you book. When you find a candidate provider, ask: “Are you TRICARE-network for [your region], do you bill TRICARE directly for visits, and do you complete Express Scripts prior authorization forms for Wegovy or Zepbound?” If the front desk says yes to all three, you're good.
- 5.Bring documentation to your first visit. We'll show you exactly what to bring in the PA section below.
Which TRICARE plans still cover GLP-1 medications in 2026?
Quick answer
TRICARE Prime, Prime Remote, Select, Reserve Select, Young Adult, Retired Reserve, CHCBP, and the US Family Health Plan still cover Wegovy, Zepbound, and Saxenda for weight management when you meet clinical criteria and get an approved prior authorization. TRICARE For Life beneficiaries lost weight-loss GLP-1 coverage on August 31, 2025. Diabetes GLP-1 coverage (Ozempic, Mounjaro, Trulicity, Victoza for type 2 diabetes) remains available across most plans when prescribed for that specific FDA-approved indication.
Plans that still have a weight-loss GLP-1 path
| Plan | Weight-Loss GLP-1 Coverage? | Notes |
|---|---|---|
| TRICARE Prime | ✓ Yes, if criteria are met | Active duty: $0. Dependents/retirees: copay applies. |
| TRICARE Prime Remote | ✓ Yes, if criteria are met | Active-duty family members on Prime Remote have $0 Home Delivery/network retail copays starting Feb 28, 2026 |
| US Family Health Plan | ⚠ Plan-specific | USFHP runs its own pharmacy plan — verify with your USFHP site |
| TRICARE Select | ✓ Yes, if criteria are met | More provider flexibility |
| TRICARE Young Adult | ✓ Yes, if criteria are met | Listed by TRICARE as eligible |
| TRICARE Reserve Select | ✓ Yes, if criteria are met | Same PA path as Prime/Select |
| TRICARE Retired Reserve | ✓ Yes, if criteria are met | Same PA path as Prime/Select |
| CHCBP | ✓ Yes, if criteria are met | Premium-based; same PA path |
Plans where the weight-loss GLP-1 path is closed
| Plan | Weight-Loss GLP-1 Coverage? | What's Still Covered |
|---|---|---|
| TRICARE For Life | ✗ Coverage ended Aug 31, 2025 | Diabetes GLP-1s for type 2 diabetes remain covered |
| Direct Care Only | ✗ No weight-loss drug coverage | MTF-dependent diabetes coverage; full cost off-base |
| NATO / Partnership for Peace | ✗ Not covered | Limited coverage; verify with sponsoring agreement |
What changed on August 31, 2025 — and why TFL beneficiaries are angry
On August 31, 2025, the Defense Health Agency (DHA) put new controls on TRICARE's weight-loss medication coverage. If you were a TRICARE For Life beneficiary getting Wegovy, Zepbound, or Saxenda through your benefit, your coverage ended that day. Even if you had a prior authorization approved before Aug 31, it's no longer valid for weight loss.
The Military Officers Association of America (MOAA) has been pushing back on it publicly. In MOAA's October 2025 advocacy update, members described the impact: one wrote, “I just don't understand why a person that served 21 years and deployed in wartime is suddenly being treated like a second-class citizen.” MOAA and other military advocacy organizations are actively working to reverse the policy.
If you're TFL, here's where things stand:
- Diabetes GLP-1s (Ozempic, Mounjaro, Trulicity, Victoza) for type 2 diabetes are still covered when prescribed for that diagnosis and PA/medical-necessity criteria are met.
- Weight-loss GLP-1s (Wegovy, Zepbound, Saxenda) are now full cash-pay for you. Your options are in the cash-pay section below.
Active duty: extra rules to know
Active-duty service members on Prime or Prime Remote have the cleanest path — covered drugs are $0 at MTF pharmacies, network retail, and TRICARE Home Delivery in 2026. But your service branch may have its own weight-management program rules. The Air Force, Army, Navy, Marines, and Space Force each have body composition and weight-management standards that interact with GLP-1 prescribing decisions. Talk to your unit medical staff and your PCM before pursuing an external telehealth GLP-1 path — it can affect readiness reviews and fitness assessments.
Which GLP-1 medications does TRICARE actually cover?
Quick answer
TRICARE covers Wegovy, Zepbound, and Saxenda for chronic weight management when you meet criteria. It covers Ozempic, Mounjaro, Trulicity, and Victoza for type 2 diabetes when prescribed for that diagnosis. The trap most people fall into: asking for Ozempic or Mounjaro when what they actually need is Wegovy or Zepbound. TRICARE lists those drugs under diabetes coverage, not weight management, so the request gets denied.
Track 1 — Weight Management (FDA-approved for chronic weight management)
| Medication | Active Ingredient | What It Treats | TRICARE Status |
|---|---|---|---|
| Wegovy (injection) | semaglutide | Chronic weight management | Covered for eligible plans with PA + step therapy |
| Wegovy pill (oral) | semaglutide | Chronic weight management | FDA-approved Dec 22, 2025; launched Jan 2026. Covered on current March 12, 2026 PA form for adults; not covered for ages 12–17. Verify adult formulary status. |
| Zepbound | tirzepatide | Chronic weight management + obstructive sleep apnea (OSA) | Covered with PA + step therapy for weight; OSA pathway is separate |
| Saxenda | liraglutide | Chronic weight management | Covered with PA + medical necessity form |
Track 2 — Type 2 Diabetes (FDA-approved for blood sugar control)
| Medication | Active Ingredient | What It Treats | TRICARE Status |
|---|---|---|---|
| Ozempic | semaglutide | Type 2 diabetes | Covered with PA + medical necessity form |
| Mounjaro | tirzepatide | Type 2 diabetes | Covered with PA + medical necessity form |
| Trulicity | dulaglutide | Type 2 diabetes | Covered with PA; often the step comparator |
| Victoza | liraglutide | Type 2 diabetes | Covered with PA + medical necessity form |
The mistake to avoid
If you want a GLP-1 for weight loss and your doctor writes Ozempic or Mounjaro, TRICARE lists those drugs under type 2 diabetes coverage, not weight management — the request gets denied. If you have diabetes, use one of the diabetes-route drugs. If you want weight loss, ask for Wegovy or Zepbound.
The Zepbound OSA exception worth knowing
Zepbound has a separate prior authorization pathway for obstructive sleep apnea (OSA). It requires adults 18 or older with a BMI of 30 or higher and an apnea-hypopnea index (AHI) of 15 or higher, plus six months of documented behavioral modification and dietary restriction. The OSA path doesn't require the older-weight-loss-medication step therapy. If you have diagnosed OSA, this could be a faster route.
What about Foundayo (orforglipron)?
Foundayo is FDA-approved April 1, 2026 for chronic weight management. As of May 12, 2026, the DoD Pharmacy & Therapeutics Committee hasn't publicly added Foundayo to the TRICARE formulary. The committee typically reviews new medications within 6 to 12 months of FDA approval, so a coverage decision is expected in 2026. Until then, Foundayo is cash-pay only. Verify current TRICARE formulary status via the TRICARE Formulary Search Tool before assuming.
Compounded GLP-1s and TRICARE: a clear word
Compounded semaglutide and compounded tirzepatide are not the same as Wegovy, Ozempic, Zepbound, or Mounjaro. That matters for TRICARE in three concrete ways:
- TRICARE doesn't cover compounded GLP-1s for weight loss.
- You can't fill a compounded GLP-1 at TRICARE Pharmacy Home Delivery. Express Scripts won't process it.
- Compounded GLP-1s are a separate cash-pay, non-FDA-approved category — not generic equivalents.
Regulatory note: On February 20, 2026, the FDA issued a warning letter to MEDVi, LLC (letter #721455) citing claims like “Same active ingredient as Wegovy® and Ozempic®” as false or misleading misbranding. In March 2026, the FDA issued similar warning letters to more than 30 telehealth companies marketing compounded GLP-1 products. If a telehealth platform tells you they can use your TRICARE for compounded semaglutide, that's a red flag.
Which telehealth providers actually work with TRICARE for GLP-1?
Quick answer
Most household-name telehealth GLP-1 brands don't “accept TRICARE” the way you're imagining. Most are cash-pay. A few accept insurance for the visit and help with PA paperwork, but verifying TRICARE network status directly with the provider is required before you assume the path will work.
The RX Index is a pricing intelligence and comparison resource for GLP-1 telehealth providers. The table below was built from primary sources because the existing pages leave readers guessing.
| Provider / Pathway | Bills TRICARE for Visit? | Helps with PA? | Rx Can Route to TRICARE Pharmacy? | Best Fit For |
|---|---|---|---|---|
| Your PCM (military or civilian network) | ✓ Yes | ✓ Yes — most natural PA submitter | ✓ Yes | Almost every Prime/Select beneficiary pursuing a covered weight-loss or diabetes GLP-1 path |
| MTF provider | ✓ Yes (direct care) | ✓ Yes — handled inside the MTF | ✓ Yes, including MTF pharmacy at $0 | Active duty and dependents living near an MTF |
| Teladoc (TRICARE virtual health partner) | ✓ Yes — listed as TRICARE virtual health partner | ⚠ Limited — TRICARE lists Teladoc under urgent care, behavioral health, and dermatology access. A TRICARE-covered Teladoc GLP-1 prescribing pathway is not verified — confirm directly. | Depends on prescriber | Anyone who wants a TRICARE-billed urgent telehealth visit; not a verified GLP-1 path until confirmed |
| Your TRICARE-network civilian PCP's telehealth | ✓ Yes (if doctor is TRICARE-network) | ✓ Yes | ✓ Yes | Anyone with a TRICARE-network civilian PCP offering telehealth |
| PlushCare | ⚠ Accepts most major insurance plans for visits; confirm TRICARE compatibility directly during sign-up before assuming the visit will be billed | ⚠ Care team handles PA paperwork generally; TRICARE-specific PA support should be verified | ✓ Sends Rx to your pharmacy of choice — including TRICARE Pharmacy Home Delivery, network retail, or MTF | TRICARE beneficiaries who want a fast telehealth visit and PA help — after verifying TRICARE compatibility with PlushCare directly |
| Sesame Care (sponsored affiliate link, opens in a new tab) | ✗ Cash subscription, does not bill health insurance | ⚠ Providers may help with PA generally; TRICARE-specific PA support not independently verified | ✓ Once Rx is issued, you can fill at TRICARE pharmacies if PA is approved | Cash-pay speed seekers who want flat-fee visit access and may also be working a TRICARE PA elsewhere |
| Ro Body Program | ✗ No | ✗ Does NOT coordinate insurance for government plans | Ro's own mail-order pharmacy for cash-pay; not TRICARE-coordinated | Important: Ro's published GLP-1 policy currently states patients with government healthcare coverage are not eligible for the Ro Body Program. Verify directly with Ro support before paying. |
| Hims | ✗ No | ✗ No insurance navigation for GLP-1 | Hims's own mail-order; not TRICARE-coordinated | Cash-pay FDA-approved branded GLP-1s |
| Hers | ✗ No | ✗ No insurance navigation for GLP-1 | Hers's own mail-order; not TRICARE-coordinated | Cash-pay FDA-approved branded GLP-1s |
| Eden | ✗ No | ✗ No PA navigation | Eden's mail-order; not TRICARE-coordinated | TFL or denied-PA users who want a clean cash-pay path to FDA-approved Wegovy and Zepbound at LillyDirect/NovoCare-matched pricing, with no membership fee |
| MEDVi | ✗ No | ✗ No PA navigation | Compounded fills; not TRICARE-coordinated | FDA warning letter issued February 20, 2026 (letter #721455) for false/misleading claims about compounded semaglutide/tirzepatide. Not recommended until remediation is verified. |
Last verified May 12, 2026. Sources: Express Scripts TRICARE Pharmacy FAQ, TRICARE.mil Wegovy/Ozempic/Mounjaro FAQ, DHA Newsroom Q&A (Aug 2025, Sept 2025), MOAA TRICARE Guide, TRICARE Virtual Health Partners directory, each provider's published insurance/eligibility policy, FDA Warning Letter #721455 (MEDVi, 02/20/2026).
If your TRICARE plan covers GLP-1s and you want it filled through TRICARE pharmacy
This is the cheapest path. Period. Most beneficiaries end up paying between $0 (active duty) and $44 for a 90-day Wegovy or Zepbound supply via Home Delivery — compared to $1,300+/month retail.
- 1Get a TRICARE Network or MTF prescriber. Your PCM, an MTF provider, a TRICARE-network specialist, or a telehealth platform that can confirm TRICARE network status and PA support before you pay.
- 2Bring documentation to the appointment. Covered in the PA checklist section below.
- 3Wait for PA approval. Traditional TRICARE pharmacy PA approval takes roughly 10 days after Express Scripts receives the request. Electronic prior authorization (ePA) can be much faster -- sometimes within hours when the prescriber uses ePA correctly.
- 4Fill at TRICARE Pharmacy Home Delivery, a network retail pharmacy, or your MTF. Home Delivery is typically cheapest and easiest for non-active-duty beneficiaries.
Want telehealth speed without accidentally breaking the TRICARE path?
Use our 60-second Path Finder first. If a telehealth provider can't confirm TRICARE network status and PA support, you'll know to treat that visit as cash-pay before you enter payment information.
→ Check My TRICARE GLP-1 PathIf you want fast access without waiting on prior authorization
For some readers, speed matters more than cost. Maybe you've been waiting weeks on a PA. Maybe your PCM is dragging their feet. This is where cash-pay branded telehealth makes legitimate sense.
For TRICARE beneficiaries, the cleanest cash-pay path to FDA-approved branded GLP-1s is Eden. Eden carries FDA-approved Wegovy and Zepbound, flags them as HSA/FSA eligible, charges no membership fee, and prices branded medication at LillyDirect/NovoCare-matched rates. Because Eden doesn't coordinate insurance for GLP-1s, there's no eligibility verification step that conflicts with your TRICARE status.
Ro is also worth knowing about, but with an important caveat: Ro's published GLP-1 policy currently states patients with government healthcare coverage — including TRICARE — are not eligible for the Ro Body Program. Different Ro pages have stated different things historically, so verify directly with Ro support before entering payment information.
Sesame Care (sponsored affiliate link, opens in a new tab) is a third option — flat-fee subscription ($59/month with annual plan, $99/month month-to-month), one of the broadest branded formularies (Wegovy, Zepbound, Ozempic, Mounjaro, Foundayo, Saxenda), and providers who can help with PA paperwork generally.
Want fast cash-pay access to FDA-approved Wegovy or Zepbound — at manufacturer-matched pricing, no membership fee?
Eden carries FDA-approved branded GLP-1s, no eligibility verification required, and prices match LillyDirect/NovoCare.
→ See Eden Pricing & AvailabilityIf you have TRICARE For Life or your PA was denied
The August 31, 2025 change was real, and you didn't do anything wrong. MOAA is still fighting to reverse it. For weight-loss GLP-1s, the TRICARE benefit no longer applies to TFL beneficiaries. You have three honest paths:
Path 1 — FDA-approved branded cash-pay
The cleanest option is Eden (no eligibility verification step, LillyDirect/NovoCare-matched pricing, no membership fee) or direct manufacturer programs (NovoCare for Wegovy, LillyDirect for Zepbound and Foundayo). Ro and Sesame (sponsored affiliate link, opens in a new tab) are alternatives — see the Ro caveat above.
Path 2 — Cash-pay compounded GLP-1s
A separate cash-pay, non-FDA-approved category, at lower prices than branded. Before choosing, read each provider's current regulatory status. The FDA issued more than 30 warning letters to compounded GLP-1 providers in early 2026, including the February 20, 2026 letter to MEDVi (letter #721455). We have a separate compounded GLP-1 guide for readers who want to dig in.
Path 3 — Secondary commercial insurance
If your spouse has employer-sponsored commercial insurance, that plan can serve as primary or secondary for GLP-1s. But don't assume you'll qualify for manufacturer copay cards — manufacturer savings-card terms commonly exclude patients enrolled in any government program, even when the government plan is secondary. Check the drug-specific current terms before relying on a copay card.
TFL beneficiary who lost coverage and wants to stay on FDA-approved Wegovy or Zepbound at manufacturer-matched pricing?
Eden carries FDA-approved branded GLP-1s with HSA/FSA eligibility and no membership fee — and skips the government-insurance eligibility check entirely.
→ See Eden's Current PricingWhat does the TRICARE prior authorization process actually look like?
Quick answer
TRICARE's weight-loss GLP-1 prior authorization form requires your prescriber to document four things: your BMI (30+, or 27+ with a weight-related condition), at least six months of behavioral and dietary modification, a three-month trial of an older generic weight-loss medication (or a documented reason you can't take one), and that none of the hard-stop exclusions apply. Approval typically takes about 10 days after Express Scripts receives the request, faster with electronic PA.

Adult BMI criteria
The TRICARE weight-loss GLP-1 PA form (current version dated March 12, 2026 per the TRICARE Formulary Search Tool) asks the prescriber to confirm one of these:
- BMI of 30 or higher (clinical obesity), OR
- BMI of 27 or higher combined with at least one weight-related condition: type 2 diabetes, impaired glucose tolerance, dyslipidemia (high cholesterol), hypertension (high blood pressure), or sleep apnea
If your BMI is between 27 and 29.9, you absolutely need one of those conditions documented in your medical record. This is the most common reason BMI-borderline patients get denied: the comorbid condition wasn't documented.
Six months of behavioral and dietary modification
The PA form asks whether you've engaged in behavioral modification and dietary restriction for at least six months and failed to achieve your desired weight loss. Documentation that strengthens the PA includes:
- A nutrition or weight-management program (the military's MOVE! program counts; WW counts; a documented diet plan from a registered dietitian counts)
- Tracked food intake or exercise logs over six months
- Notes in your medical chart from prior visits showing weight discussions and lifestyle counseling
Step therapy: the three-month older-medication trial
The form asks whether you've tried (and failed to lose at least 5% of baseline body weight after three months of) generic phentermine, benzphetamine, diethylpropion, or phendimetrazine — or whether you have a documented contraindication or adverse reaction to those drugs.
Important: Contrave or Qsymia trials don't satisfy this requirement. The form is specific about those four agents. If your records show Contrave or Qsymia but not one of the listed step drugs, your PA can be denied for “step therapy not met.”
The fix: your prescriber can document a contraindication or adverse reaction to phentermine and the other step agents. Common contraindications include uncontrolled hypertension, cardiovascular disease, hyperthyroidism, glaucoma, history of substance use disorder, or a documented adverse reaction.
Hard-stop exclusions
These will get an immediate denial, no exceptions:
- Pregnancy. GLP-1s aren't approved for use during pregnancy.
- Use with another GLP-1 receptor agonist. You can't be on two GLP-1s at the same time.
- Personal or family history of medullary thyroid carcinoma (MTC) or Multiple Endocrine Neoplasia syndrome type 2 (MEN2). This is a black-box warning on Wegovy, Zepbound, Ozempic, and Mounjaro.
Renewal is not automatic
Renewal under the current PA form generally requires documented evidence the medication is working:
- Adults on Wegovy or Zepbound for weight management: at least 5% baseline weight loss after full titration
- Adolescents on Wegovy injection: at least 4% baseline weight loss
- Zepbound for OSA: documented improvement in OSA symptoms based on AHI improvement
Your TRICARE GLP-1 appointment checklist
Bring these to your visit. Print them if you have to:
| What to Bring | Why It Matters |
|---|---|
| Current height, weight, and BMI | The PA form requires it |
| List of weight-related conditions (diabetes, prediabetes, hypertension, high cholesterol, sleep apnea) | Critical if your BMI is 27–29.9 |
| Documentation of six months of lifestyle changes (food logs, MOVE! attendance, dietitian notes, fitness tracking) | The PA form requires it |
| List of weight-loss medications tried (especially phentermine, benzphetamine, diethylpropion, phendimetrazine — or reasons you can't take them) | Step therapy is the most common denial reason |
| List of current medications and any thyroid history | Hard-stop exclusions |
| Your preferred pharmacy (TRICARE Home Delivery, network retail, MTF) | Speeds up the fill |
| The medication you want (Wegovy for weight loss, NOT Ozempic) | Avoids the wrong-drug denial |
Want this checklist on paper, plus a personalized list of questions to ask your TRICARE-network provider?
Take our 60-second TRICARE GLP-1 Path Finder and we'll give you a printable plan based on your specific plan and situation.
→ Get My TRICARE GLP-1 ChecklistWhere can you fill a TRICARE-covered GLP-1 prescription?
Quick answer
A TRICARE-covered GLP-1 prescription can be filled through TRICARE Pharmacy Home Delivery, a TRICARE network retail pharmacy, or a military treatment facility (MTF) pharmacy when the drug is stocked. Home Delivery is typically the cheapest and easiest for non-active-duty beneficiaries. Call the MTF pharmacy first before assuming they have the medication — stock varies.
| Pharmacy Type | How It Works | Best For |
|---|---|---|
| TRICARE Pharmacy Home Delivery | Mail-order through Express Scripts; up to 90-day supply | Most non-active-duty beneficiaries — cheapest copay for brand-name formulary drugs |
| TRICARE Network Retail Pharmacy | In-network CVS, Walgreens, or other retail; up to 30-day supply | When you need the medication sooner than mail-order can deliver |
| MTF Pharmacy | Military pharmacy at your base; call ahead to confirm availability | Active duty and dependents living near an MTF — $0 copay |
Non-network pharmacy fills generally require paying full price up front and filing a claim afterward. Stick with the three options above whenever possible.
What will GLP-1 medications cost with TRICARE in 2026?
Quick answer
Active-duty service members pay $0 for covered GLP-1s at military pharmacies, TRICARE Pharmacy Home Delivery, and TRICARE retail network pharmacies in 2026. For most other beneficiaries, 2026–2027 brand-name formulary copays are $44 through Home Delivery (up to 90-day supply) and $48 at retail network pharmacies (up to 30-day supply). Non-covered drugs cost full price.
2026–2027 TRICARE pharmacy cost table
| Beneficiary / Pharmacy Type | Brand-Name Formulary GLP-1 Cost |
|---|---|
| Active duty service member at MTF, Home Delivery, or network retail | $0 |
| Active-duty family members on Prime Remote (starting Feb 28, 2026) at Home Delivery or network retail | $0 |
| Other beneficiaries at military pharmacy | $0 |
| Other beneficiaries via TRICARE Pharmacy Home Delivery (up to 90-day supply) | $44 |
| Other beneficiaries at retail network pharmacy (up to 30-day supply) | $48 |
| Non-network pharmacy or non-covered drug | Full retail (often $1,000+/month for branded GLP-1s) |
Rates from TRICARE.mil/Costs/PharmacyCosts (2026–2027 table). Medically retired sponsors, their family members, and certain survivors may have frozen lower copays. Confirm exact current copay for your specific drug via the TRICARE Formulary Search Tool.
Cash-pay landscape: what GLP-1s cost without TRICARE
If your TRICARE doesn't cover the medication (TFL, denied PA, or non-formulary situation), here's what you're realistically paying in 2026:
| Medication | Cash-Pay Starting Price (2026) | Notes |
|---|---|---|
| Wegovy pill (oral semaglutide) | NovoCare self-pay: $149/month for 1.5 mg and 4 mg; $299/month for higher doses | FDA-approved December 22, 2025; new oral form |
| Foundayo (orforglipron) | LillyDirect self-pay: $149 (0.8 mg), $199 (2.5 mg), $299 (5.5–9 mg), $349 (14.5–17.2 mg) | FDA-approved April 1, 2026 |
| Wegovy pen (injectable) | NovoCare: $199/month for 0.25 mg and 0.5 mg through June 30, 2026, then $349/month; $399/month for Wegovy HD 7.2 mg | Manufacturer direct-to-consumer pricing |
| Zepbound | LillyDirect self-pay: $299 (2.5 mg), $399 (5 mg), $499 (7.5 mg), $699 (10–15 mg) | Journey-program offers can lower some doses |
| Compounded semaglutide | ~$99–$299/month | Not FDA-approved; sold by various telehealth platforms (read each platform's current regulatory status) |
| Compounded tirzepatide | ~$125–$399/month | Not FDA-approved; same caveats apply |
The price gap between brand-name and compounded has narrowed in 2026. With the Wegovy pill and Foundayo both starting at $149/month at manufacturer pricing, the cash-pay branded path is much closer to compounded pricing than it was in 2024.
The federal program copay card trap
Manufacturer copay cards for Wegovy, Zepbound, Ozempic, and Mounjaro are not available to TRICARE-only beneficiaries. Federal law prohibits manufacturer copay assistance for patients enrolled in federal program drug coverage. The often-cited workaround — using a spouse's commercial insurance as secondary — is not a guaranteed unlock. Manufacturer savings-card terms commonly exclude any patient enrolled in a government program, even when the government plan is secondary. Check the drug-specific current terms before assuming a copay card will work.
What if your TRICARE prior authorization is denied?
Quick answer
Most TRICARE GLP-1 denials fall into one of five categories — wrong drug for the indication, missing step-therapy documentation, BMI or comorbidity documentation gap, plan-type ineligibility (TFL after Aug 31, 2025), or wrong PA pathway. Each has a different fix. You have 90 calendar days from the denial date to file a TRICARE pharmacy appeal.
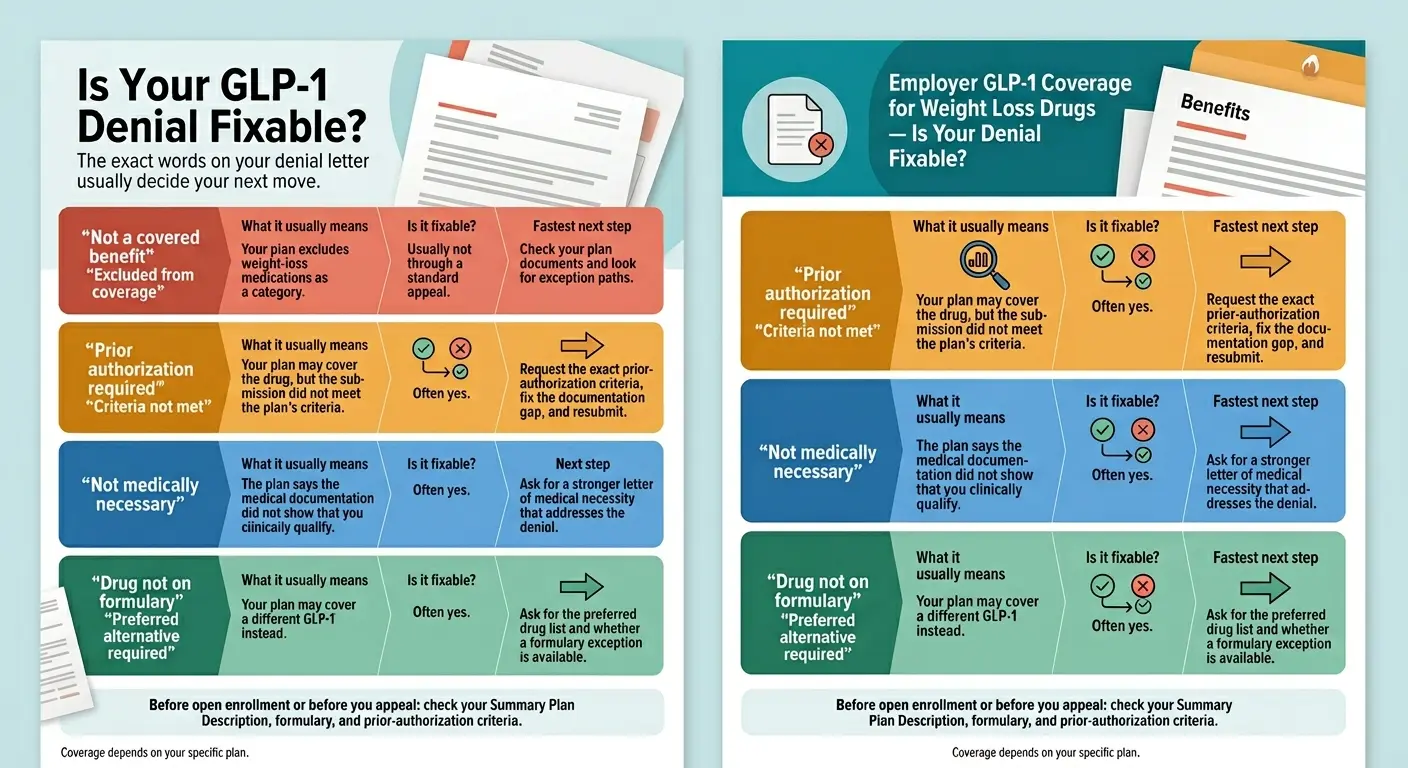
The five denial branches and what to do about each one
Branch 1: Wrong drug for the wrong indication
What happened: Your prescriber asked for Ozempic or Mounjaro for weight loss. TRICARE lists those drugs under type 2 diabetes coverage, not weight management.
The fix: Ask your prescriber to switch the request to Wegovy or Zepbound for the weight-management pathway. Resubmit.
Branch 2: Step therapy not met
What happened: Your records don't show a three-month trial of phentermine, benzphetamine, diethylpropion, or phendimetrazine -- or a documented contraindication or adverse reaction.
The fix: Your prescriber documents a contraindication or adverse reaction to those drugs (uncontrolled hypertension, cardiovascular disease, hyperthyroidism, glaucoma, history of substance use disorder). Or trial one agent for three months and resubmit. The contraindication route is usually faster.
Branch 3: BMI or comorbidity gap
What happened: Your BMI is between 27 and 29.9 and the weight-related condition wasn't documented in your chart.
The fix: Your prescriber updates the medical record to clearly document the comorbid condition (hypertension, dyslipidemia, prediabetes, sleep apnea, etc.) and the BMI. Resubmit.
Branch 4: Plan ineligible (TFL)
What happened: You're a TRICARE For Life beneficiary and the August 31, 2025 change ended your weight-loss GLP-1 coverage.
The fix: There's no fix inside TRICARE for the weight-loss pathway. Your options are the cash-pay paths above, secondary commercial insurance if available, or -- if you have type 2 diabetes -- the diabetes-route GLP-1s which remain covered for TFL when prescribed for that diagnosis.
Branch 5: Zepbound denied for weight; OSA path might fit
What happened: Your Zepbound PA was denied on the weight-loss pathway.
The fix: If you have a diagnosis of obstructive sleep apnea with a BMI of 30+ and an AHI of 15+, plus six months of documented behavioral modification, ask your prescriber to resubmit under the Zepbound OSA pathway. That pathway doesn't require the older-weight-loss-medication step therapy.
How to file the appeal
If the fix doesn't resolve it on resubmission, you have 90 calendar days from the date of the denial notice to file a TRICARE pharmacy appeal. Submit the appeal in writing to Express Scripts with a copy of the denial decision and any supporting documentation. Include BMI, comorbid conditions, six months of lifestyle modification, prior medication history, and a clear medical-necessity letter from your prescriber. Your prescriber's office usually handles the paperwork on your behalf if you ask.
Got denied and not sure why?
Take our 60-second TRICARE GLP-1 Path Finder and answer a few questions about your situation. We'll tell you which of the five denial branches you're likely in and what specifically to ask your prescriber to fix.
→ Diagnose My TRICARE DenialWhen does cash-pay GLP-1 actually make sense for TRICARE beneficiaries?
Quick answer
Cash-pay GLP-1 telehealth makes sense in exactly three situations: you're a TRICARE For Life beneficiary who lost coverage on August 31, 2025; you've been denied a TRICARE PA after exhausting the fix paths above; or you've decided the wait and paperwork of the TRICARE route isn't worth it for your situation. If none of those apply, cash-pay is usually the wrong first move.
Scenario 1
TRICARE For Life beneficiary, weight loss
Your TRICARE benefit no longer covers this. Diabetes-route GLP-1s remain covered if you have T2D. For weight loss, you're cash-pay now.
Scenario 2
Denied PA, all fixes exhausted
You ran through the denial branches, tried the fixes, appealed, and TRICARE still won't approve. Cash-pay is a reasonable next step.
Scenario 3
Chosen speed over the TRICARE process
Some readers don't want to wait 10+ days for PA review, or want to start this week. Cash-pay telehealth is a legitimate choice -- just know what you're paying for.
Where cash-pay is the wrong move
If you're on TRICARE Prime or Select with a covered weight-loss path, paying $300+/month cash for what would cost $44 for a 90-day supply through TRICARE is generally a bad decision. Work the TRICARE path first — it's worth a few weeks of patience for most beneficiaries.
One real beneficiary's experience (sourced from a public r/Zepbound thread)
In a public Reddit thread titled “Tricare will cover wegovy/zepbound, let me tell you how” on r/Zepbound, the original poster — a TRICARE Prime beneficiary — wrote that the “tricky part” of the process was “getting a base doctor to prescribe” the medication. Their advice: come to appointments with BMI, comorbidity documentation, and prior medication history already organized. The thread generated dozens of replies from other military beneficiaries describing similar workflows.
We share this because it captures the most common friction in the TRICARE GLP-1 journey: the prescriber conversation, not the medication or pharmacy step. Every beneficiary's situation is different.
How we verified this guide
Built from primary-source documents: TRICARE.mil's coverage pages, the Express Scripts militaryrx GLP-1 pages, the current Wegovy/Zepbound prior authorization form (dated March 12, 2026 per the TRICARE Formulary Search Tool), TRICARE Newsroom and DHA articles on the August 2025 weight-loss medication policy change, MOAA's TRICARE coverage advocacy updates, FDA guidance on compounded GLP-1s including the February 20, 2026 warning letter to MEDVi, and each telehealth provider's published insurance and eligibility policy.
What we verified
- TRICARE plan eligibility, including Aug 31, 2025 TFL coverage cessation
- Drugs listed for weight management (Wegovy, Zepbound, Saxenda) and type 2 diabetes (Ozempic, Mounjaro, Trulicity, Victoza)
- TRICARE Network and MTF prescription requirements
- PA process timing and current March 12, 2026 PA form requirements
- The four step-therapy agents and 5% weight-loss benchmark for failure
- Pharmacy fill routes and 2026–2027 TRICARE pharmacy cost rates
- 90-day pharmacy appeal deadline per TRICARE.mil
- Zepbound OSA pathway requirements (BMI ≥30, AHI ≥15, six months behavioral modification)
- Wegovy pill FDA approval (December 22, 2025) and January 2026 launch
- Foundayo FDA approval (April 1, 2026)
- Cash-pay pricing from NovoCare and LillyDirect direct-to-consumer programs
- Ro Body Program government-insurance eligibility language
- FDA Warning Letter #721455 to MEDVi (02/20/2026) verified via FDA.gov
Items flagged for direct verification
- Foundayo TRICARE formulary status — pending DoD P&T Committee review
- Wegovy pill adult formulary status — included on current PA form for adults but not adolescents; confirm before assuming
- PlushCare TRICARE network status — accepts most major insurance plans generally; confirm TRICARE-specific compatibility directly
- Teladoc GLP-1 prescribing under the TRICARE virtual health partnership — confirm directly with Teladoc before assuming GLP-1 access is available
We update this page when DHA, Express Scripts, the FDA, or any cited provider publishes a material change. The “Last verified” date above reflects our most recent direct check.
Frequently asked questions
Does TRICARE cover Wegovy in 2026?
Yes, TRICARE covers Wegovy for chronic weight management if you are enrolled in TRICARE Prime, Prime Remote, Select, Reserve Select, Young Adult, Retired Reserve, CHCBP, or the US Family Health Plan, you meet the clinical criteria, you have a prescription from a TRICARE Network or MTF provider, and you have an approved prior authorization. TRICARE For Life beneficiaries lost Wegovy coverage on August 31, 2025.
Does TRICARE cover Zepbound in 2026?
Yes, TRICARE covers Zepbound under the same plan eligibility and prior authorization rules as Wegovy for chronic weight management. Zepbound also has a separate prior authorization pathway for obstructive sleep apnea (BMI 30 or higher, AHI 15 or higher, plus six months of documented behavioral modification) that does not require the older-weight-loss-medication step therapy. TRICARE For Life beneficiaries lost Zepbound coverage on August 31, 2025 for weight management.
Does TRICARE cover Ozempic for weight loss?
No. TRICARE lists Ozempic under type 2 diabetes coverage. Ozempic is FDA-approved for type 2 diabetes, not weight loss, so a request for Ozempic on the weight-management pathway will be denied. If your goal is weight loss, ask your prescriber for Wegovy or Zepbound instead.
Does TRICARE cover Mounjaro for weight loss?
No. Like Ozempic, Mounjaro is FDA-approved for type 2 diabetes only. TRICARE lists Mounjaro under diabetes coverage with a prior authorization. For weight loss, ask for Zepbound -- which has the same active ingredient (tirzepatide) but is FDA-approved for chronic weight management.
Does Ro accept TRICARE?
Ro does not coordinate GLP-1 insurance coverage for government-funded plans. Ro's published GLP-1 policy currently states patients with government healthcare coverage -- including TRICARE -- are not eligible for the Ro Body Program. Because Ro has had conflicting language across different pages, verify directly with Ro support before paying.
Does Sesame Care accept TRICARE?
Sesame Care does not bill TRICARE for visits -- it operates on a flat-fee subscription ($59/month with annual plan, $99/month month-to-month). Sesame providers can write prescriptions and may help with prior authorization paperwork generally, but TRICARE-specific Wegovy/Zepbound PA support should be verified before assuming the path will work. Manufacturer copay promotions are not available to TRICARE-only beneficiaries.
Does PlushCare accept TRICARE?
PlushCare accepts most major insurance plans for visits, which has included TRICARE for many beneficiaries. Their care team handles prior authorization paperwork generally, and prescriptions are sent to your pharmacy of choice -- including TRICARE Pharmacy Home Delivery, network retail, or MTF. Confirm TRICARE-specific compatibility during PlushCare sign-up before assuming the visit will be billed.
Can active-duty service members use telehealth for GLP-1s?
Active-duty service members can use telehealth, but referrals are typically required for non-MTF care, and weight-management GLP-1 prescriptions usually originate from MTF providers under your service branch's weight-management program rules. Talk to your unit medical staff and your PCM before pursuing external telehealth GLP-1 prescribing. Active-duty pays $0 for covered drugs at MTF pharmacies, TRICARE Pharmacy Home Delivery, and TRICARE retail network pharmacies in 2026.
What happened to TRICARE For Life GLP-1 coverage in August 2025?
On August 31, 2025, the Defense Health Agency ended TRICARE For Life coverage of weight-loss medications, including Wegovy, Zepbound, Saxenda, Contrave, Qsymia, and phentermine. Direct-care-only and NATO/Partnership for Peace beneficiaries also lost coverage. Diabetes-route GLP-1s (Ozempic, Mounjaro, Trulicity, Victoza for type 2 diabetes) remained covered for these groups when prescribed for that diagnosis. MOAA and other military advocacy organizations are actively challenging the policy change.
Can I fill a TRICARE GLP-1 prescription at a non-network pharmacy?
You can, but you will generally pay full price up front and file a claim afterward, with reimbursement subject to plan status, deductibles, point-of-service rules, and TRICARE's non-network cost-share rules. For most beneficiaries, this is a bad financial decision. Use TRICARE Pharmacy Home Delivery (typically the cheapest), a TRICARE network retail pharmacy, or your MTF pharmacy.
How long does TRICARE prior authorization take?
Traditional TRICARE pharmacy prior authorization approval takes about 10 days after Express Scripts receives the provider's request. Electronic prior authorization (ePA) -- used by more prescribers each year -- can be much faster, sometimes within hours or even minutes when submitted correctly. The most efficient path: complete the appointment checklist in this guide, give your prescriber organized documentation, and ask whether they can submit ePA.
Can I appeal a TRICARE GLP-1 denial?
Yes. You have 90 calendar days from the date of the denial notice to file a TRICARE pharmacy appeal. Submit the appeal in writing to Express Scripts with a copy of the denial decision and any supporting documentation. Your prescriber's office usually handles the paperwork on your behalf if you ask. Include BMI, comorbidities, lifestyle documentation, prior medication history, and a clear medical-necessity letter to give Express Scripts the specific facts it needs to reconsider.
Does TRICARE cover the Wegovy pill (oral semaglutide)?
The Wegovy pill was FDA-approved December 22, 2025 and launched in January 2026. The current TRICARE Wegovy/Zepbound PA form includes semaglutide tablets and injections for adults; Wegovy tablets are not covered for ages 12 to 17 on the current form. Verify adult formulary status and current PA requirements via the TRICARE Formulary Search Tool before assuming coverage.
Does TRICARE cover Foundayo (orforglipron)?
Foundayo, Eli Lilly's once-daily oral GLP-1, was FDA-approved on April 1, 2026 for chronic weight management. As of May 12, 2026, the DoD Pharmacy & Therapeutics Committee has not publicly confirmed Foundayo on the TRICARE formulary. The committee typically reviews new medications within 6 to 12 months of FDA approval, so a decision is expected by late 2026 or early 2027. Until coverage is confirmed, Foundayo is cash-pay only.
Does TRICARE cover compounded semaglutide or tirzepatide?
No. TRICARE's covered formulary includes FDA-approved medications. Compounded GLP-1s are a separate cash-pay, non-FDA-approved category and are not generic equivalents. TRICARE Pharmacy Home Delivery, network retail pharmacies, and MTF pharmacies do not process compounded GLP-1 prescriptions through the TRICARE benefit. The FDA issued warning letters in 2026 to more than 30 telehealth companies -- including a February 20, 2026 letter to MEDVi (letter #721455) -- for misleading claims about compounded GLP-1 products.
Related guides on The RX Index
Still not sure which GLP-1 program is right for you?
TRICARE is genuinely complicated, and the right answer depends on your specific plan, your specific situation, and what matters most to you right now. Take our free 60-second matching quiz — we'll give you a personalized next step, whether that's the cheapest TRICARE-covered path, the fastest cash-pay route, or a clear answer about what won't work for you.
→ Find My GLP-1 PathThe RX Index is a pricing intelligence and comparison resource for GLP-1 telehealth providers. We track current pricing, coverage rules, and provider policies so you don't have to. This guide is not medical advice. It covers coverage and access information only. Talk to a licensed clinician before starting, changing, or stopping any prescription medication.
Last verified: May 12, 2026. Next scheduled review: June 2026.