Does Aetna Cover Mounjaro? 2026 Coverage, PA Rules, Cost, and Next Steps
Published: · Last reviewed:
By The RX Index Editorial Team · Last verified: May 14, 2026
Sources: Aetna Clinical Policy Bulletin 5468-C · Aetna 2026 Drug Guides · Lilly pricinginfo.lilly.com · CMS Medicare GLP-1 Bridge FAQ · Aetna Better Health Medicaid Policy
Does Aetna cover Mounjaro?
Yes — Aetna may cover Mounjaro for type 2 diabetes when your specific pharmacy plan includes it and prior authorization (PA) is approved.
No — do not assume Aetna will cover Mounjaro for weight loss. Mounjaro is FDA-approved for type 2 diabetes only. If your goal is weight loss, the right next move is usually to check whether your plan covers Zepbound, Wegovy, or another antiobesity medication under your plan’s weight-management benefit.
That’s the bottom line. But “covered” hides five separate gates, and which one you’re stuck at decides what to do in the next ten minutes. This page is the map.
Does Aetna cover Mounjaro? Find your row.
| If this sounds like you | The bottom line |
|---|---|
| Type 2 diabetes + Aetna commercial coverage | Mounjaro is potentially covered with prior authorization if your exact plan includes it and your documentation matches Aetna’s criteria. Cost is plan-specific — check your member portal. |
| You want Mounjaro for weight loss only | Aetna’s public Mounjaro policy is for type 2 diabetes. Ask your doctor about Zepbound (same active ingredient, different FDA label) or another antiobesity medication under your plan’s weight-management benefit. |
| Aetna Medicare (Part D / MA-PD) + type 2 diabetes | Mounjaro may be covered under standard Part D with PA. Mounjaro is not in the new Medicare GLP-1 Bridge program — that program covers weight-loss drugs only. |
| Aetna Better Health (Medicaid) | State-specific. Coverage exists in some states with PA; rules vary. Check your state’s Aetna Better Health pharmacy benefit. |
| Your pharmacy said “PA required” | This is not a denial. Aetna wants documentation before paying. Most fixable PAs go through. |
| You already got denied | Read your denial letter for your appeal deadline. Many denials due to missing documentation are fixable. |
Skip the guesswork. Get a free, personalized coverage report for your exact plan.
Ro’s free GLP-1 Insurance Coverage Checker contacts your insurer to create a personalized report showing coverage for GLP-1 medications, including whether prior authorization is required. It does not submit prescriptions or PAs — it tells you what your plan covers so you walk into your doctor’s appointment informed.
Check your GLP-1 coverage in 60 seconds with Ro →We earn a commission if you use this link, at no cost to you.
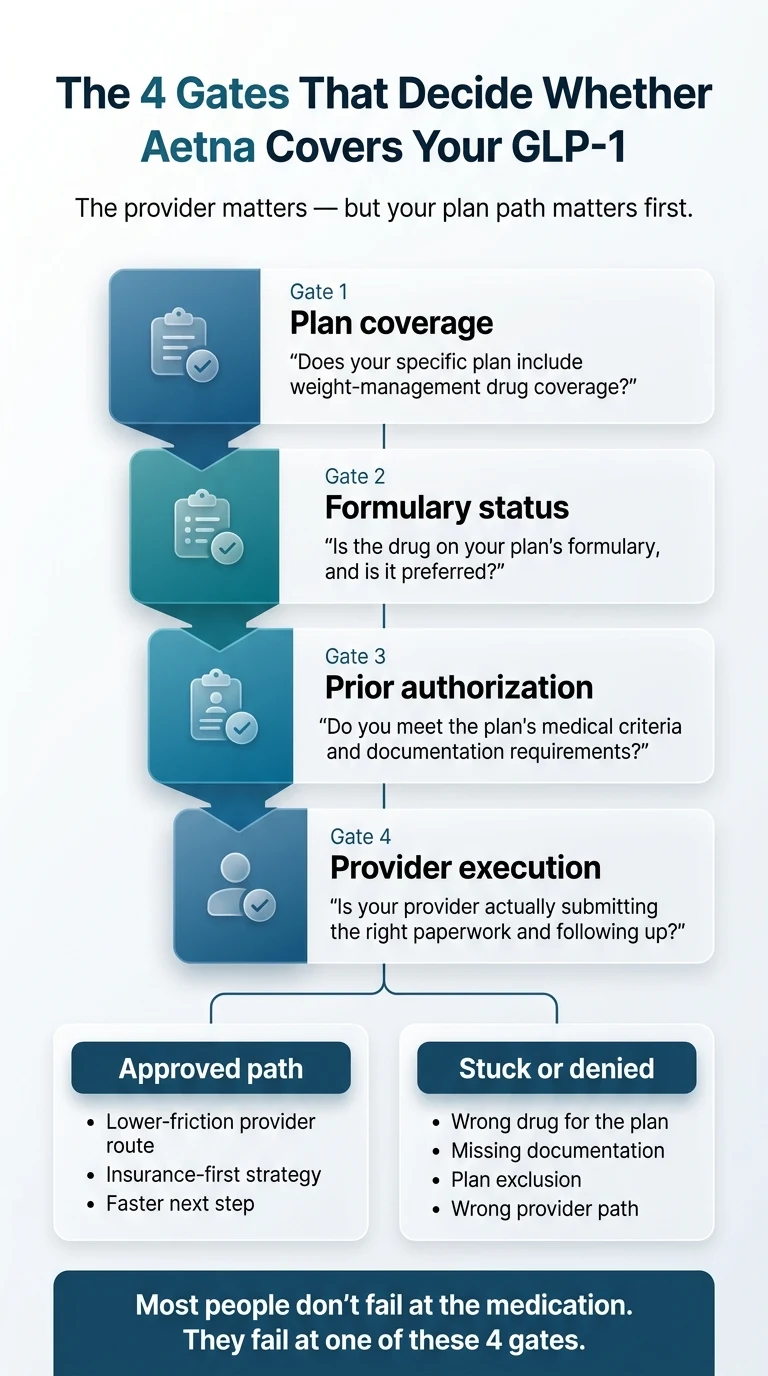
What “covered” actually means: the 5 gates
A drug being “on the formulary” is not the same as your plan paying for it. Coverage runs through five separate gates. One failed gate stops the claim cold.
When someone says “Aetna covers Mounjaro,” they usually mean gate #1. Real coverage means clearing all five:
- 1
Formulary listing. Mounjaro shows up on your plan's drug list. (Mounjaro appears in Aetna's 2026 Standard Plan Pharmacy Drug Guide under antidiabetic / incretin mimetic agents — but Aetna says appearing in the guide does not guarantee coverage for every member.)
- 2
Diagnosis match. Your prescription's reason for use matches what Aetna covers Mounjaro for — which is type 2 diabetes.
- 3
Prior authorization. Aetna requires documentation before paying. PA = prior authorization, the paperwork your doctor sends to prove medical necessity.
- 4
Step therapy or quantity limits. Some plans require you to try metformin first. Most plans cap how many pens per fill.
- 5
Pharmacy and fill match. Your prescription lands at an in-network pharmacy, mail-order option, or specialty channel allowed by your plan, in the right quantity, for the right days' supply.
Two people on “the same Aetna plan” can get different answers because they’re stuck at different gates. The fastest way to find your gate: log into Aetna’s member portal and search “Mounjaro.” Your screen shows your tier, PA flag, step therapy flag, and any quantity limits for your exact plan.
The Aetna Mounjaro Coverage Path Matrix
Assembled from Aetna’s public clinical policy bulletins, 2025 and 2026 Aetna drug guides, Aetna Medicare cost estimator examples, Aetna Better Health Medicaid policy guidelines, CMS Medicare GLP-1 Bridge documentation, and Lilly’s current pricing page. Verified May 14, 2026.
| Your Situation | Likely Aetna Outcome | What Has To Be True | Best Next Step |
|---|---|---|---|
| Aetna Commercial + Type 2 Diabetes | Potentially covered with PA | Plan includes Mounjaro; T2D diagnosis documented (ICD-10 E11.x); metformin trial documented, intolerance, or contraindication — or combination therapy with A1C ≥7.5% | Confirm formulary, then submit PA with full documentation |
| Aetna Commercial + Weight Loss Only | Aetna's public Mounjaro policy is for T2D, not weight loss | Off-label use; not Aetna's Mounjaro pathway | Ask whether your plan covers Zepbound, Wegovy, or another antiobesity medication |
| Aetna Commercial + Obesity + Sleep Apnea | Mounjaro: no path here. Zepbound: separate OSA PA exists | For Zepbound OSA: AHI ≥15 on PSG or HSAT, BMI ≥30, with documentation, per Aetna Policy 6947-C | Ask about Zepbound for moderate-to-severe OSA, not Mounjaro |
| Aetna Medicare (MA-PD or Part D) + T2D | Potentially covered under standard Part D with PA | T2D diagnosis + PA criteria met | Standard Part D rules apply. Mounjaro is NOT in the 2026 Medicare GLP-1 Bridge |
| Aetna Medicare + Weight Loss | Mounjaro: no Medicare path. Some weight-loss GLP-1s available via the Bridge from July 1, 2026 | Medicare GLP-1 Bridge eligibility for Wegovy, Foundayo, or Zepbound KwikPen | Talk to your doctor about Bridge-eligible drugs if weight loss is your indication |
| Aetna Better Health (Medicaid) + T2D | State-specific. Coverage with PA exists in some states. | Verified for Maryland, Florida Kids, Pennsylvania Kids — does NOT apply to Illinois, Florida, New Jersey, Michigan, or Virginia | Check your specific state's Aetna Better Health pharmacy benefit |
| Aetna Federal Employee Plan (FEHB) + T2D | Plan-specific; typically follows commercial PA rules | Standard PA criteria per your FEHB plan | Check your FEHB plan documentation or call Aetna federal member services |
| Plan excludes anti-obesity drugs (employer carve-out) | No GLP-1 weight-loss coverage at all | Employer chose to exclude antiobesity meds | Self-pay branded path, manufacturer savings cards, or talk to HR about open enrollment |
Sources: Aetna Pharmacy Clinical Policy Bulletin 5468-C (Mounjaro PA with Limit, UDR 05-2024); Aetna Pharmacy Clinical Policy Bulletin 6947-C (Zepbound PA with Limit, P04-2025); 2025 and 2026 Aetna Standard Plan and Advanced Control Plan Pharmacy Drug Guides; Aetna Better Health Medicaid policy guideline for Mounjaro (effective 2/3/2025); CMS Medicare GLP-1 Bridge FAQ; Lilly pricinginfo.lilly.com.
What we verified vs. what it proves
Insurance writing online tends to mash verified facts together with generalizations until you can’t tell which is which. We separate them here.
| Source we checked | Exact thing verified | What it proves | What it does not prove |
|---|---|---|---|
| Aetna Pharmacy Clinical Policy Bulletin 5468-C | Non-Medicare PA criteria for Mounjaro + quantity limits | Aetna has a published PA-with-limit policy for Mounjaro covering type 2 diabetes | That every Aetna plan covers Mounjaro |
| Aetna 2026 Standard Plan Pharmacy Drug Guide | Mounjaro appears in antidiabetic/incretin mimetic section | Mounjaro is on Aetna's reference drug list | Member-specific coverage on every plan |
| Aetna 2026 Formulary Exclusions Drug List | Some plans list Zepbound with preferred alternatives | Some Aetna plans exclude weight-loss GLP-1s in favor of specific alternatives | Zepbound is always excluded or always preferred |
| Aetna Better Health Mounjaro Medicaid Policy | T2D coverage criteria for Maryland, Florida Kids, Pennsylvania Kids | Medicaid coverage path exists in those plans/states | National Medicaid coverage |
| CMS Medicare GLP-1 Bridge FAQ | Bridge covers Foundayo, Wegovy injection/tablets, Zepbound KwikPen for weight reduction starting July 1, 2026 | What products are in the Bridge | That Mounjaro is in the Bridge — it is not |
| Lilly pricinginfo.lilly.com | Current Mounjaro list price $1,112.16 per fill | Lilly's current published list price | Pharmacy retail price, which varies |
Does Aetna cover Mounjaro for type 2 diabetes?
Yes, Aetna may cover Mounjaro for type 2 diabetes when your specific plan includes Mounjaro on its formulary and prior authorization criteria are met. Aetna has a published PA-with-limit policy (Pharmacy Clinical Policy Bulletin 5468-C) that lays out the criteria. Mounjaro is listed in Aetna’s 2026 Standard Plan and Advanced Control Plan drug guides. Approval typically comes down to three things: a documented type 2 diabetes diagnosis, A1C lab evidence, and proof of a metformin trial, intolerance, or contraindication.
What Aetna’s published policy actually says
Aetna’s Pharmacy Clinical Policy Bulletin 5468-C is the policy controlling Mounjaro PA decisions on non-Medicare plans. In plain language, it approves Mounjaro for type 2 diabetes when:
- •You haven’t been on a stable maintenance dose of Mounjaro for at least 3 months (this is the initial PA), AND one of these is true:
- –You had an inadequate response to metformin, can’t tolerate metformin, or have a contraindication to it, OR
- –You need combination therapy and your A1C is 7.5% or higher
For continuation (refill) PAs, Aetna looks at whether you’ve been stable on Mounjaro for 3+ months and whether your A1C has improved from baseline. Aetna’s policy also sets quantity limits: 4 pens (2 mL) per 21 days, or 12 pens (6 mL) per 63 days. If your doctor writes for more, the claim rejects on quantity even if everything else is approved.
The Aetna Mounjaro PA documentation checklist
This is what your doctor’s office needs to send. The more of this they include up front, the higher your approval odds and the faster the decision.
Type 2 diabetes diagnosis with ICD-10 code E11.x. Aetna's policy states Mounjaro is not indicated for type 1 diabetes (E10.x), so a type 1 code on the PA will trigger a denial.
Recent A1C lab result. Aetna's policy uses A1C ≥7.5% specifically in the combination therapy pathway. For continuation PAs, A1C reduction from baseline matters — include both the original (high) A1C and the current value.
Metformin history. Dates, dose, response, and either: it didn't work, you couldn't tolerate it, or you have a contraindication. Send whatever metformin records you can get — old prescriptions, prior provider notes, pharmacy fill history.
If skipping metformin: combination therapy plan with A1C ≥7.5%.
Time-on-therapy detail. For new PAs: confirmation you haven't been on Mounjaro for 3+ months already. For continuation: dose, start date, and current A1C.
Prescriber NPI and signature on the Aetna Specialty Medication Precertification Request form, or submitted via Aetna's electronic PA portal (faster).
The most common reasons Aetna PAs get denied
The same denial patterns repeat. The fixes are usually simple — the problem is your doctor’s office often doesn’t know to include them up front.
- 1
Wrong primary indication code. Doctor put an obesity code (E66.x) on the script instead of, or in front of, the type 2 diabetes code (E11.x). Aetna's auto-adjudication catches this and denies.
- 2
No metformin trial in the chart. Even if you took metformin years ago, if the medical record doesn't say so, Aetna assumes you didn't. Pull old prescription records from any past pharmacy or insurer.
- 3
Missing A1C documentation. Aetna wants a recent lab result with a number. "Patient has diabetes" is not enough.
- 4
Continuation PA missing baseline data. If you've been on Mounjaro for a year and your A1C is now 6.0% (great!), Aetna's reviewer may not see the original A1C that justified treatment. Submit both.
- 5
Quantity limits exceeded. Doctor wrote for more pens than the plan allows in the days-supply window. The fix is usually a script that fits the limit or a quantity exception request.
A useful next step before your doctor submits the PA
Check what your specific plan covers and what your PA will need to include. Ro offers a free GLP-1 Insurance Coverage Checker that contacts your insurer and creates a personalized report showing whether prior authorization is required for your plan. You walk into your doctor’s appointment knowing what to ask for — and what to bring.
Check what your Aetna plan covers before your doctor submits the PA →Does Aetna cover Mounjaro for weight loss?
Aetna’s public Mounjaro policy is for type 2 diabetes — not for weight loss. Mounjaro is FDA-approved for type 2 diabetes only. If your goal is weight loss, the cleaner path is usually to ask your doctor about Zepbound (the tirzepatide brand with FDA approval for chronic weight management), Wegovy, or another antiobesity medication under your plan’s weight-management benefit.
We’ve seen too many readers spend weeks fighting an off-label Mounjaro denial when a clean Zepbound PA would have been the right path from day one.
Why Aetna says no to Mounjaro for weight loss
Insurance plans cover medications for their FDA-approved indications. Mounjaro is FDA-approved for type 2 diabetes. Lilly’s own prescribing information indicates Mounjaro for glycemic control in type 2 diabetes — not weight management. From Aetna’s perspective, paying $1,100+/month for off-label Mounjaro when FDA-approved tirzepatide for weight loss (Zepbound) exists is unnecessary cost. So they generally don’t.
There’s a separate question of whether your plan covers any weight-loss GLP-1s at all. Aetna says many of its benefit plans exclude weight-reduction medications entirely. Other plans cover weight-loss GLP-1s under specific clinical policies. Aetna’s published BMI-based weight-loss GLP-1 policy applies to Saxenda, Wegovy, and Zepbound — not Mounjaro.
The Zepbound pivot: same active ingredient, different FDA label
Zepbound contains tirzepatide — the same active ingredient as Mounjaro — at the same dose strengths. The difference is the FDA label. Zepbound is FDA-approved for chronic weight management in adults with obesity (BMI ≥30) or overweight (BMI ≥27) with at least one weight-related comorbidity. Some Aetna plans cover Zepbound when PA criteria are met. Zepbound is also FDA-approved for moderate-to-severe obstructive sleep apnea (OSA) in adults with obesity, and Aetna’s published Zepbound policy (Bulletin 6947-C) has a specific OSA pathway: AHI ≥15 on a PSG or HSAT, plus BMI ≥30.
Mounjaro vs. Zepbound: side-by-side for Aetna members
| Detail | Mounjaro | Zepbound |
|---|---|---|
| Active ingredient | Tirzepatide | Tirzepatide (same) |
| FDA-approved for | Type 2 diabetes (adults and pediatric 10+) | Chronic weight management; moderate-to-severe OSA in adults with obesity |
| Aetna PA pathway | Non-Medicare Policy 5468-C: T2D + step therapy or combination therapy with A1C ≥7.5% | Policy 6947-C: weight reduction pathway, separate OSA pathway with AHI ≥15 + BMI ≥30 |
| Aetna formulary status (2026) | Listed in Standard Plan and Advanced Control Plan drug guides | Plan-dependent. Some Aetna plans list Zepbound with preferred alternatives; others cover it under weight-management benefits |
| Lilly Savings Card | Eligible commercially insured patients with Mounjaro coverage can pay as low as $25 for up to a 3-month prescription (terms apply) | Separate Zepbound Savings Card with similar structure |
| Medicare coverage | Standard Part D for T2D — NOT in the 2026 Medicare GLP-1 Bridge | KwikPen formulation included in the 2026 Medicare GLP-1 Bridge ($50/month copay for eligible beneficiaries) |
Honest caveat: Not every Aetna plan covers weight-loss medications. Some employer plans carve antiobesity drugs out entirely — meaning even Zepbound won’t be covered. If that’s your situation, your realistic options are the Lilly Zepbound Savings Card (for commercially insured eligible patients), LillyDirect self-pay vials, or a transparent telehealth program for FDA-approved tirzepatide. Ro carries Zepbound and Foundayo (Lilly’s newest oral GLP-1, FDA-approved April 2026) on a transparent monthly program: get started for $39, then as low as $74/month with annual plan paid upfront. Ro matches LillyDirect, NovoCare, and TrumpRx pricing on medication.
Check whether your plan covers Zepbound or another FDA-approved weight-management option →Does Aetna cover Mounjaro without diabetes?
Generally no through Aetna’s public Mounjaro PA path. Aetna’s Mounjaro coverage policy (Bulletin 5468-C) is built around type 2 diabetes criteria. If you don’t have a type 2 diabetes diagnosis, the cleaner next move is to check what your plan covers for your actual condition — Zepbound or Wegovy for weight loss, Zepbound for OSA with obesity, or another antiobesity medication under your plan’s weight-management benefit. Some Aetna plans allow medical exception requests for non-formulary or off-label use, but the success rate is low and the process is slow.
If you’re prediabetic, have insulin resistance, or have PCOS and you’re considering Mounjaro: most of these conditions don’t fit Aetna’s Mounjaro PA criteria. Your prescriber may have other options that match your plan’s coverage rules better.
How much Mounjaro costs with Aetna in 2026
With Aetna coverage and PA approved, members commonly pay copays or coinsurance in the range typical for a Preferred Brand or Specialty tier drug — but actual cost depends entirely on your plan’s deductible, copay, coinsurance, and your Savings Card eligibility. Without Aetna coverage, Lilly’s current list price is $1,112.16 per fill, and retail cash prices range from approximately $1,080 to $1,300 per month depending on pharmacy.
Same medication, $25 to $1,200+ depending on your situation. Here’s what actually moves the price.
What moves your Mounjaro cost
| Scenario | Likely cost behavior |
|---|---|
| Aetna commercial + PA approved + Preferred Brand tier + Savings Card eligible | Could be as low as $25/month per Lilly's Savings Card terms |
| Aetna commercial + PA approved + deductible not met | You pay closer to the negotiated price until the deductible is met |
| Aetna commercial + PA approved + Specialty tier | Coinsurance-based, often 20–40% of the negotiated drug cost |
| Aetna Medicare Part D | Plan-specific copay; Savings Card not allowed (federal law prohibits manufacturer cards on government plans); 2026 Part D out-of-pocket cap is $2,100 |
| Aetna Medicaid / Better Health | Often $0 with PA approval (state-specific) |
| Aetna plan exclusion | No coverage; retail or savings-card pathways apply |
| No Aetna coverage (retail cash) | Lilly list price $1,112.16/fill; retail pharmacy range typically $1,080–$1,300/month |
Source notes: Lilly list price from pricinginfo.lilly.com (verified May 14, 2026). Retail pharmacy range from Sesame Care’s published Mounjaro page (pharmacy-dependent). Medicare Part D out-of-pocket cap from current CMS Part D program rules.
The Mounjaro Savings Card with Aetna
The Lilly Mounjaro Savings Card is what people mean when they say “$25 Mounjaro.” It works like this:
- ✓You have commercial Aetna insurance covering Mounjaro AND your PA is approved: Eligible commercially insured patients can pay as little as $25 for up to a 3-month prescription, terms apply. Lilly can change card terms at any time — confirm at the pharmacy or at startlilly.com.
- ✗You have Aetna Medicare, Aetna Better Health/Medicaid, Tricare, VA, or any government-funded plan: Federal law prohibits manufacturer savings cards on government insurance. You can’t use it.
- ~Your commercial Aetna plan doesn’t cover Mounjaro: The card has separate (limited) cash-pay terms with much smaller savings.
What Mounjaro costs when Aetna won’t cover it
The hard scenario: your PA was denied, you don’t have commercial coverage, or your plan excludes the drug entirely. Real options:
- 1
Lilly Cares Foundation (patient assistance): Free Mounjaro for qualifying low-income, uninsured patients. Income at or below 400% of federal poverty level (approximately $60,000/year for an individual in 2026). Application takes 2–4 weeks. Apply at lillycares.com.
- 2
Pharmacy shopping at retail: Costco and Sam's Club consistently offer some of the lowest cash prices (no membership required for pharmacy services). Walgreens and CVS retail are typically higher.
- 3
Transparent telehealth pricing for FDA-approved GLP-1s: Sesame's weight-loss program lists transparent cash-pay pricing for FDA-approved options including Wegovy pen, Wegovy pill, Zepbound KwikPen, Zepbound vial, Foundayo, and Ozempic. Sesame providers can also assist with prior authorization paperwork. Mounjaro pens range $1,080–$1,300/month depending on pharmacy without insurance.
Compare self-pay FDA-approved GLP-1 options on Sesame Care
Sesame providers can help with prior authorization paperwork for Mounjaro. Sesame does not override your Aetna plan rules — but if Aetna says no, Sesame is a way forward.
Compare self-pay FDA-approved GLP-1 options on Sesame Care →How Aetna’s prior authorization actually works
Pharmacy PA decisions are typically completed within 30–45 days for standard requests and within 72 hours for expedited cases (timing varies by plan and request type). Electronic submission (ePA) through Aetna’s provider portal is the fastest path. Your doctor submits — not you.
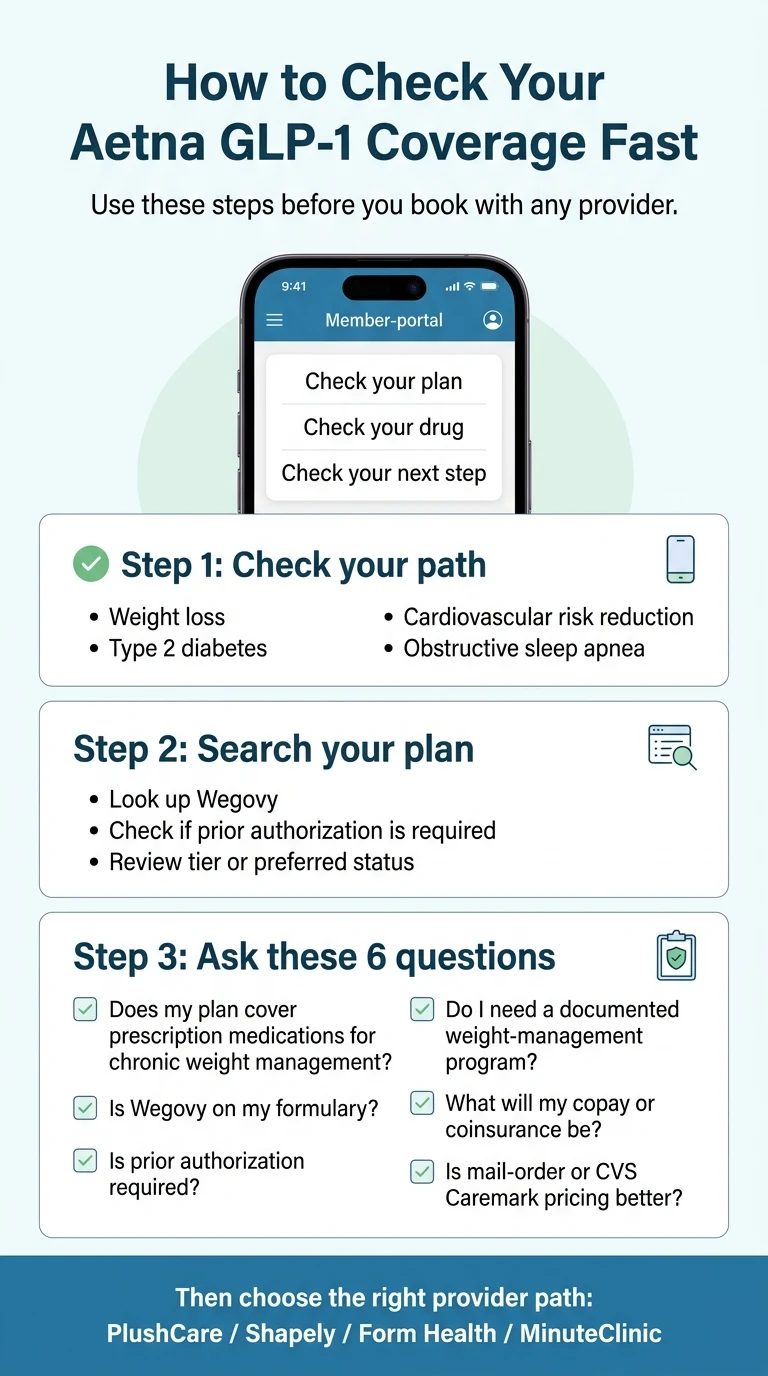
The 6-step Aetna PA process
- 1
Confirm Mounjaro needs PA on your plan.
Log into Aetna's member portal → Find a Medication → search "Mounjaro" or "tirzepatide." Look for PA, ST, QL flags. (PA = Prior Authorization. ST = Step Therapy. QL = Quantity Limit. Mounjaro typically shows PA.)
- 2
Gather documentation with your doctor:
type 2 diabetes diagnosis with ICD-10 code E11.x, recent A1C lab result, metformin history, any contraindications, current medication list.
- 3
Your doctor submits the PA.
Best path: electronic PA (ePA) through Aetna's provider portal. Backup: fax the Aetna Specialty Medication Precertification Request form.
- 4
You wait.
Standard pharmacy PA decisions typically come within 30–45 days. Expedited review (when your doctor certifies delay would seriously jeopardize your health) is faster — often 72 hours.
- 5
Outcome.
Approval → your prescription is filled through your plan's in-network pharmacy or specialty channel. Denial → you get a denial letter with appeal rights and deadlines.
- 6
Continuation PA.
Most plans require it annually. Your doctor documents response (A1C improvement, dose stability, tolerability).
The 5-minute Aetna call script
Skip the portal hunt. Call the number on the back of your Aetna member ID card and read this. Have a pen ready.
“Hi, I’m calling about coverage for Mounjaro under my pharmacy benefit. Can you tell me:
- Is Mounjaro on my plan’s formulary?
- What tier is it on?
- Does it require prior authorization, step therapy, or have a quantity limit?
- Is coverage limited to type 2 diabetes only on my plan?
- If it’s not covered for my situation, what alternatives are covered — Zepbound, Wegovy, Ozempic, Rybelsus, or something else?
- What pharmacy channel does my plan use to fill Mounjaro — retail, mail-order, or specialty?
- Can you email me the prior authorization criteria my doctor needs to meet?”
Write down each answer. If the rep says “I don’t know,” ask for the pharmacy benefit team or a supervisor. The call typically takes 5–10 minutes.
Why the pharmacy still matters after PA approval
A PA approval does not automatically mean every pharmacy will process the claim the same way. On some Aetna plans, Mounjaro is filled through a specialty pharmacy channel (often via mail order with onboarding by a specialty pharmacist). On others, it’s a retail or mail-order fill at your usual pharmacy. If your local pharmacy says “we can’t fill this on your Aetna plan” or the claim rejects even with PA approved, the pharmacy channel is often the reason. Call Aetna and ask: “What pharmacy channel does my plan use to fill Mounjaro?”
What if Aetna denied your Mounjaro?
A denial is not the end. Read your denial letter carefully — it states your appeal deadline (commercial plans typically allow 60 to 180 days, varies by plan type) and the specific reason for the denial. Many denials due to missing documentation are fixable. If the internal appeal fails, you have the right to an independent external review through your state, and the external review decision is binding on the insurer.
Take a breath. Denials with terrifying language (“Not medically necessary”) get overturned in one round with one piece of paper all the time — an old A1C lab from a different doctor, a metformin prescription from a previous insurer, an indication code corrected from E66 to E11.
Aetna denial decoder: what they mean vs. what to do
Match the exact phrase from your denial letter to what it actually means and your real next step.
| Aetna’s denial language | What it actually means | Your best next step |
|---|---|---|
| "Prior authorization required" | Not a denial. Aetna wants documentation before paying. | Have your doctor submit the PA with the checklist above. |
| "Not medically necessary" | A PA criterion was not met or not documented. | Call Aetna and ask: "Which specific criterion was not met?" Then fix that. |
| "Diagnosis not covered" | Off-label use (usually weight loss for Mounjaro). | Switch to Zepbound (FDA-approved for weight loss) or appeal with stronger T2D documentation if applicable. |
| "Step therapy required" | Aetna wants proof you tried metformin (or another first-line drug) first. | Submit your metformin history — any insurer's records count when documented. |
| "Plan exclusion" | Your plan doesn't cover this benefit at all. | Appeals rarely overturn exclusions. Look at savings cards or self-pay paths. |
| "Quantity limit exceeded" | Your prescribed dose/fill exceeds the plan's quantity rule (4 pens/21 days or 12 pens/63 days for Mounjaro). | Have your doctor write a script that fits the quantity limit, or submit a quantity exception request. |
| "Continuation denied" | Aetna doesn't see evidence the medication is still working. | Submit baseline A1C, current A1C, current dose, start date. Show the response. |
| "Non-formulary" | Mounjaro isn't on your plan's drug list at all. | Request a formulary exception with documentation of why alternatives aren't appropriate. |
Step 1: Read your denial letter carefully
The letter states Aetna’s specific reason and the deadline for your internal appeal. Find the policy reference number (often something like “Policy 5468-C” for Mounjaro PA decisions). That number tells you exactly what criteria Aetna applied. Use the decoder above to match the language to the fix.
Step 2: Internal appeal — within the deadline shown on your letter
Internal appeal windows vary by plan type. Many commercial Aetna plans allow up to 180 days; some Medicare appeal windows are tighter. Your denial letter shows your deadline — use it.
Work with your doctor on a medical necessity letter that includes:
- •Your A1C trend over time (not just one value — show inadequate control over months)
- •Your complete metformin history with dates, doses, response, and any intolerance
- •Any other GLP-1 trials (Trulicity, Victoza, Ozempic, etc.) with outcomes
- •The clinical rationale for Mounjaro specifically
Submit through Aetna’s appeals portal or by fax. Expedited internal appeals can be decided much faster when your doctor certifies delay would seriously jeopardize your health.
Step 3: External review — if Aetna upholds the denial
If Aetna denies your internal appeal, you can request an independent external review through your state’s Department of Insurance or Department of Financial Services. The external reviewer is an independent organization unrelated to Aetna. Their decision is binding — if they overturn the denial, Aetna must provide coverage. External review is free to you. Filing windows and timelines vary by state.
Three pro tips from real appeals
- 1
Use A1C trend data, not single values. Multiple A1C readings showing inadequate control over months are more persuasive than one number.
- 2
Pull metformin records from any past insurer. Old prescription records, prior provider notes, and pharmacy fill histories all count when documented.
- 3
If your real goal is weight loss, don't appeal a Mounjaro denial. The policy isn't on your side. Switch to Zepbound — different PA criteria, much higher approval rate when the criteria fit.
Bridge option while you appeal
Appeals can take weeks even when you do everything right. If you have diabetes and need to start medication, paying out-of-pocket through a licensed telehealth provider is a legitimate stopgap. Sesame providers can help with prior authorization paperwork and list pharmacy-dependent pricing for Mounjaro pens at $1,080–$1,300/month.
See Sesame Care’s Mounjaro path and self-pay options →Aetna Medicare and the 2026 GLP-1 Bridge
Aetna Medicare plans may cover Mounjaro for type 2 diabetes under standard Part D with prior authorization. Mounjaro is NOT included in the new Medicare GLP-1 Bridge program — the Bridge covers GLP-1 drugs when used to reduce excess body weight and maintain weight reduction, and CMS currently lists Foundayo, Wegovy injection and tablets, and the KwikPen formulation of Zepbound. Mounjaro for diabetes stays under standard Part D coverage with your plan’s normal PA rules.
This is one of the most confusing areas in GLP-1 coverage right now. We get questions like “Is Mounjaro $50/month under Medicare now?” — no, it’s not. Here’s why.
What Aetna Medicare covers for Mounjaro
If you have an Aetna Medicare Advantage Prescription Drug plan (MA-PD), an Aetna Medicare Part D standalone, or an Aetna Medicare Supplement plus a separate Part D — Mounjaro can be covered for type 2 diabetes when your plan’s formulary includes Mounjaro, PA criteria are met, and you haven’t exceeded quantity limits. The 2026 Medicare Part D out-of-pocket cap is $2,100 — once you hit that, your plan pays 100% of covered drug costs for the rest of the year.
Important: The Mounjaro Savings Card does NOT work with Medicare. Federal law prohibits manufacturer assistance on government insurance. Don’t fall for sites claiming you can stack the card with Medicare — you can’t.
The 2026 Medicare GLP-1 Bridge: what’s actually changing
On July 1, 2026, CMS launches the Medicare GLP-1 Bridge — a short-term demonstration program giving eligible Medicare Part D beneficiaries access to certain GLP-1 medications for $50/month copay. The Bridge runs through December 31, 2027. Humana will serve as the central processor for the program, handling prior authorizations, claims, and payments.
✓ Drugs covered under the Bridge
- • All formulations of Foundayo
- • All formulations of Wegovy (injection and tablets)
- • KwikPen formulation of Zepbound
For weight reduction only. $50/month copay.
✗ Drugs NOT covered under the Bridge
- • Mounjaro
- • Ozempic
- • Rybelsus
- • Zepbound single-dose vials/pens
- • Compounded GLP-1s
If you have Aetna Medicare and want a GLP-1 for weight loss starting July 1, 2026, the Bridge gives you a path — talk to your doctor about Wegovy, Foundayo, or Zepbound KwikPen. The Bridge requires PA through Humana as the central processor and includes specific BMI thresholds plus a comorbidity such as heart failure, hypertension, chronic kidney disease, prediabetes, or established cardiovascular disease.
Aetna Medicare call script for GLP-1 coverage
“I’m calling about GLP-1 medication coverage. Can you tell me:
- Is my Mounjaro request for type 2 diabetes being processed under standard Part D?
- If I’m interested in a weight-loss GLP-1, am I eligible for the Medicare GLP-1 Bridge?
- Which Bridge drugs are available — Wegovy, Foundayo, or Zepbound KwikPen?
- What documentation does my doctor need to submit for each option?”
Aetna Better Health (Medicaid) and Aetna Federal Employee plans
Aetna Better Health (Medicaid) — state-scoped reality
Aetna Better Health is Aetna’s Medicaid plan brand. Coverage of Mounjaro varies significantly by state.
We verified one Aetna Better Health Mounjaro policy (effective February 3, 2025) that applies to Maryland, Florida Kids, and Pennsylvania Kids. That policy requires type 2 diabetes documentation and diabetic lab history, including A1C ≥6.5% or qualifying fasting plasma glucose ≥126 mg/dL after an 8-hour fast, plus criteria tied to metformin response or combination therapy with A1C ≥7.5%. The same policy document explicitly states it does not apply to Aetna Better Health plans in Illinois, Florida, New Jersey, Michigan, or Virginia.
Aetna Federal Employee Plan (FEHB)
Aetna FEHB plans generally follow commercial plan rules: Mounjaro may be covered for type 2 diabetes with PA. Tier placement and exact PA criteria vary by specific FEHB plan. Check your FEHB plan documentation or call Aetna’s federal member services line.
The Aetna Mounjaro Coverage Checker
Find your exact next step. We built this for the readers who shouldn’t have to scroll 8,000 words to figure out what to do.
Answer these 5 questions, then take the action below your match:
- What kind of Aetna plan do you have? (Commercial / Medicare / Better Health (Medicaid) / Federal / Don’t know)
- What’s your reason for taking Mounjaro? (Type 2 diabetes / Weight loss / Both / Other)
- Has your doctor diagnosed you with type 2 diabetes? (Yes / No / Prediabetes)
- Have you tried metformin? (Yes, currently / Yes, in past / No / Contraindicated)
- What’s your most recent A1C? (Under 6.5% / 6.5–7.4% / 7.5% or higher / Don’t know)
The tool is educational — not medical or coverage advice, and not a guarantee of Aetna’s decision. We don’t store your inputs.
Get your personalized GLP-1 coverage report from Ro →Still not sure which GLP-1 path fits your insurance, diagnosis, and goal? Take our free 60-second GLP-1 matching quiz →
Safety: coverage is not medical clearance
Coverage is not medical clearance. Mounjaro and Zepbound are not right for everyone. Mounjaro’s prescribing information includes a boxed warning for risk of thyroid C-cell tumors and states it is contraindicated in people with a personal or family history of medullary thyroid carcinoma (MTC) or multiple endocrine neoplasia syndrome type 2 (MEN2). Warnings and precautions include pancreatitis, hypoglycemia when used with insulin or sulfonylureas, acute kidney injury, severe gastrointestinal adverse reactions, diabetic retinopathy complications, and acute gallbladder disease.
Talk to a licensed clinician about your personal or family history of thyroid cancer or MEN2, any pancreatitis history, kidney issues, gallbladder problems, severe GI symptoms, pregnancy plans, hypoglycemia risk if you’re using insulin or sulfonylureas, and whether you’re using another GLP-1 or tirzepatide product. Do not combine tirzepatide products unless a clinician specifically directs a safe transition.
What this page can’t do for you
We can't run your prior authorization. Only your prescriber can submit a PA to Aetna. We can hand you the checklist of what Aetna needs; getting the form in is on your doctor's office.
We can't guarantee approval. Aetna's clinical reviewers make case-by-case calls. The PA criteria above reflect Aetna's published policy, but individual decisions vary based on documentation quality and your specific plan.
Coverage rules change. Aetna updates its formulary the first week of every month. We re-verify this page quarterly. Always confirm your specific plan's current formulary before filling.
We have affiliate relationships. Ro and Sesame Care are providers we may earn a commission from. We recommend them because they fit specific situations on this page — Ro for insurance navigation and the Zepbound/Foundayo path, Sesame for transparent FDA-approved GLP-1 program pricing and Mounjaro PA help. Our editorial test: if every affiliate link were removed, would this still be the best page on the topic? We think yes.
How we verified this page
Every commercial, clinical, and regulatory claim is sourced. Here’s what we actually checked, when, and where.
- –Aetna Mounjaro PA criteria (Type 2 diabetes), quantity limits (4 pens/21 days or 12 pens/63 days): verified against Aetna Pharmacy Clinical Policy Bulletin 5468-C (Mounjaro PA with Limit, UDR 05-2024).
- –Aetna Zepbound PA criteria (weight management pathway, OSA pathway with AHI ≥15 and BMI ≥30): verified against Aetna Pharmacy Clinical Policy Bulletin 6947-C (Zepbound PA with Limit, P04-2025).
- –Aetna Standard Plan and Advanced Control Plan drug guide listing of Mounjaro: verified against the 2025 and 2026 Aetna Pharmacy Drug Guides.
- –Aetna Better Health Mounjaro Medicaid policy criteria and state scope (applies to Maryland, Florida Kids, Pennsylvania Kids; does not apply to Illinois, Florida, New Jersey, Michigan, Virginia): verified against Aetna Better Health published policy guideline for Mounjaro, effective February 3, 2025.
- –Mounjaro list price ($1,112.16 per fill): verified against pricinginfo.lilly.com.
- –Mounjaro Savings Card terms ($25 for up to a 3-month prescription, eligible commercially insured patients): verified against startlilly.com. Terms subject to change.
- –Mounjaro FDA-approved indication (type 2 diabetes, adults and pediatric patients 10 years and older): verified against Lilly Mounjaro prescribing information.
- –Medicare GLP-1 Bridge program details (July 1, 2026 launch; $50/month copay; covers Foundayo, Wegovy injection/tablets, Zepbound KwikPen; Humana as central processor; Mounjaro not included): verified against cms.gov Medicare GLP-1 Bridge FAQ.
- –2026 Medicare Part D out-of-pocket cap ($2,100): verified against current CMS Part D program rules.
- –Ro GLP-1 Insurance Coverage Checker functionality and Ro Body program pricing ($39 first month, ~$149/month ongoing, or as low as $74/month with annual plan paid upfront): verified against ro.co.
- –Sesame Care Mounjaro page (provider PA assistance; Mounjaro pens range $1,080–$1,300/month pharmacy-dependent without insurance): verified against sesamecare.com/medication/mounjaro.
Last verified: May 14, 2026. We update this page when Aetna policies, Lilly terms, CMS guidance, or provider pricing changes. Aetna formularies update the first week of each month.
Frequently asked questions
Does Aetna cover Mounjaro?
Aetna may cover Mounjaro for type 2 diabetes when your specific pharmacy plan includes it and prior authorization criteria are met. Aetna's public Mounjaro policy is for type 2 diabetes — Aetna rarely covers Mounjaro for weight loss because it's an off-label use. Confirm your specific plan's coverage through the Aetna member portal or by calling the number on your member ID card.
Does Aetna require prior authorization for Mounjaro?
Many Aetna plan designs require prior authorization for Mounjaro. Aetna's public non-Medicare Mounjaro policy is a PA-with-limit policy, and Aetna's plan pages direct members to log in for personalized coverage details.
How much does Mounjaro cost with Aetna?
Cost depends on your plan's tier, deductible, copay or coinsurance, pharmacy channel, and Savings Card eligibility. Eligible commercially insured patients with Mounjaro coverage can pay as little as $25 for up to a 3-month prescription through Lilly's Savings Card (terms apply). Without coverage, Lilly's list price is $1,112.16 per fill and retail pharmacy prices typically run $1,080–$1,300 per month.
Will Aetna cover Mounjaro for weight loss?
Aetna's public Mounjaro policy is for type 2 diabetes. If the request is for weight management, ask whether your plan covers Zepbound, Wegovy, or another antiobesity medication under your weight-management benefit instead of assuming Mounjaro can be approved off-label.
Does Aetna cover Mounjaro without diabetes?
Generally no through Aetna's public Mounjaro PA path, which is built around type 2 diabetes criteria. If you don't have a type 2 diabetes diagnosis, the cleaner next move is to check what your plan covers for your actual indication — Zepbound or Wegovy for weight management, Zepbound for OSA with obesity, or another covered alternative.
Why was my Mounjaro denied by Aetna?
The most common reasons are missing metformin trial documentation, an off-label weight-loss prescription, missing A1C lab results, wrong ICD-10 code, or quantity limits exceeded. Read your denial letter for the specific reason and your appeal deadline.
Does the Mounjaro Savings Card work with Aetna?
The card works for eligible commercially insured Aetna members when Aetna approves the PA. The card is NOT available for Aetna Medicare, Aetna Better Health (Medicaid), Tricare, VA, or any government-funded plan. Federal law prohibits manufacturer assistance on government insurance.
Does Aetna Medicare cover Mounjaro?
Aetna Medicare plans may cover Mounjaro for type 2 diabetes under standard Part D with PA. Mounjaro is not in the 2026 Medicare GLP-1 Bridge program — Mounjaro for diabetes stays under standard Part D coverage. The Bridge program covers Foundayo, Wegovy injection and tablets, and Zepbound KwikPen for weight reduction.
Does Aetna Better Health (Medicaid) cover Mounjaro?
Coverage is state-specific. The Aetna Better Health Mounjaro policy we verified applies to Maryland, Florida Kids, and Pennsylvania Kids — and explicitly does not apply to Illinois, Florida, New Jersey, Michigan, or Virginia. Other states need their own pharmacy-benefit lookup. Coverage typically requires PA with type 2 diabetes documentation.
How long does Aetna's prior authorization take?
Standard pharmacy PA decisions are typically completed within 30–45 days. Expedited reviews are faster, often within 72 hours when your doctor certifies delay would seriously jeopardize your health. Electronic submission through Aetna's provider portal is the fastest path. Check your specific plan documents for exact timelines.
Can I appeal an Aetna Mounjaro denial?
Yes. Your denial letter shows your specific appeal deadline (commercial plans often allow up to 180 days; some Medicare plans have tighter windows). After internal appeals are exhausted, you can request an independent external review through your state's Department of Insurance, and the external reviewer's decision is binding on Aetna.
Your next step
You came here because Aetna and Mounjaro don’t fit together as cleanly as anyone wants. Now you know exactly why, and exactly what to do.
If you have type 2 diabetes and Aetna commercial coverage: gather your A1C and metformin history, hand your doctor the PA checklist, then follow up through your plan's preferred pharmacy when approved.
If you want Mounjaro for weight loss: stop trying to get Aetna to cover Mounjaro. Talk to your doctor about Zepbound — same active ingredient, different FDA label, designed for chronic weight management.
If you have Aetna Medicare: standard Part D rules apply for diabetes. The Bridge isn't your path for Mounjaro — it's the path for Wegovy, Foundayo, or Zepbound KwikPen when you're seeking weight management coverage.
If you were denied: read your denial letter, match it to the decoder, fix what's missing, and appeal within your letter's deadline.
Still not sure which GLP-1 program is right for you?
Take our free 60-second matching quiz. We route you to the right path based on your plan type, diagnosis, and goal.
Take the quiz →Related guides
- →Does Aetna Cover Foundayo in 2026?
- →Does CVS Caremark Cover Mounjaro? PA Criteria & Costs
- →Does Medicare Cover Mounjaro for Weight Loss?
- →Mounjaro Cost Without Insurance: Real 2026 Prices
- →Does Marketplace Insurance Cover Wegovy?
- →GLP-1 Providers That Accept Medicare Advantage
- →The 60-Second GLP-1 Matching Quiz
About The RX Index: The RX Index is a pricing intelligence and comparison resource for GLP-1 telehealth providers. We verify pricing, formulary placement, and coverage rules across major insurers and telehealth providers quarterly. We do not provide medical advice. For treatment decisions, talk to your prescriber. For specific coverage questions, contact Aetna using the number on the back of your member ID card.
Editorial standards: We disclose all affiliate relationships visibly. We do not fabricate authors or medical credentials. We cite primary sources for every clinical, regulatory, and commercial claim. We update pages when source data changes.
Affiliate disclosure: Some links on this page are affiliate links. We may earn a commission if you sign up through them, at no cost to you. We only recommend providers we’ve independently verified. Full disclosure.
This guide is for educational and informational purposes only. It is not medical advice and is not a substitute for consultation with a qualified healthcare provider. Always confirm coverage details directly with Aetna and discuss treatment decisions with your prescriber.