Does Marketplace Insurance Cover Wegovy? (2026 Coverage Guide)
Published: · Last reviewed:
By The RX Index Editorial Team · Published: May 14, 2026 · Last verified: May 14, 2026
Sources: KFF · HealthCare.gov · CMS · RWJF · HAP · BCBS North Dakota · Ambetter/Centene · Fallon Health · NovoCare · Ro.co
Does Marketplace insurance cover Wegovy? Usually no for weight loss.
KFF's 2024 analysis of federally facilitated Marketplace formularies found Wegovy on just 1% of Marketplace prescription drug plans, while Ozempic — a different FDA-approved product with the same active ingredient, approved for diabetes — appeared on 82%. Every plan that covered Wegovy required prior authorization.
The newer RWJF-funded 2026 carrier review found GLP-1 obesity coverage in only 26 of 300 state-plus-carrier offerings, concentrated in 9 states. Coverage is real but rare, plan-specific, and always gated by prior authorization.
What we actually verified for this page
- ✓KFF's 2024 federal Marketplace formulary analysis -- 1% Wegovy coverage on HealthCare.gov plans (historical benchmark)
- ✓RWJF-funded 2026 carrier review -- 26 of 300 state-plus-carrier Marketplace offerings cover GLP-1s for obesity across 9 states
- ✓Four real 2026 plan examples (HAP, BCBS North Dakota, Ambetter/Centene, Fallon Health) -- current formulary and policy status
- ✓HealthCare.gov rules for prescription drug verification and appeals
- ✓Ro's published GLP-1 Insurance Coverage Checker, insurance concierge process, and pricing -- verified May 14, 2026
- ✓NovoCare cash-pay pricing for Wegovy injection, pill, and HD -- verified May 14, 2026
- ⚠We did not call every insurer in every state. We spot-checked four plans. Coverage changes mid-year. We re-verify quarterly and monthly during Open Enrollment.
Why This Guide Exists
Most “Does insurance cover Wegovy?” articles mash Medicare, Medicaid, employer plans, and Marketplace plans into one big blur — and Marketplace shoppers get hurt the most by that. Marketplace plans are the most restrictive segment for Wegovy. If you're shopping a plan, already enrolled in one, or staring at a denial letter, you need the Marketplace-specific answer.
This page gives you real plan examples from 2026, the mechanics of prior authorization, the cardiovascular indication door that some plans treat differently, and your cash-pay backup if Medicare and Medigap aren't your situation.
The First Decision: Which Path Applies to You?
| Your Situation | The Honest Answer | Where to Go Next |
|---|---|---|
| Shopping a Marketplace plan for 2027 coverage | Maybe -- depends on state and carrier | Jump to: How to check before you enroll |
| Already have a Marketplace plan | Usually no, but verify | Jump to: Check your plan in 10 minutes |
| Have established heart disease + obesity/overweight | A separate coverage pathway may exist -- still plan-specific | Jump to: The cardiovascular door |
| Already got denied | Appeals are real | Jump to: How to appeal a denial |
| Plan says "excluded" | Bigger problem than a denial | Jump to: Your options if your plan excludes Wegovy |
| Want someone to check for you | Free option exists | Ro's free coverage checker below |
Want someone to check your plan for free?
Ro's GLP-1 Insurance Coverage Checker contacts your insurer, confirms whether Wegovy is on your drug list, and tells you whether prior authorization is required — before you pay or commit to anything. No prescription, no obligation, no charge.
Run a free Ro Wegovy coverage check →Sponsored affiliate linkDoes Marketplace Insurance Cover Wegovy?
Almost never for weight loss, sometimes for cardiovascular risk reduction, and always with prior authorization when it is covered. Only about 1% of HealthCare.gov plans included Wegovy on formulary for obesity in KFF's 2024 federal Marketplace analysis. The newer RWJF-funded 2026 carrier review found Marketplace GLP-1 obesity coverage in nine states — California, Delaware, Georgia, North Dakota, New York, Pennsylvania, Rhode Island, Vermont, and West Virginia — across 26 of 300 offerings.
What “Marketplace” means and doesn't mean
ACA Marketplace plans are the individual health insurance plans you buy on HealthCare.gov or a state-run site like Covered California, NY State of Health, or Pennie. They're not employer plans, not Medicare, not Medicaid. They're called “Marketplace” plans because you shop them on a government-run marketplace, and sometimes called “ACA plans” or “Obamacare plans.”
The ACA requires these plans to cover prescription drugs as one of ten Essential Health Benefits. But “prescription drugs are covered” doesn't mean “every drug is covered.” Each plan picks its own formulary — the list of specific drugs the plan will pay for. And weight-loss drugs sit in a category the federal rules don't require to be covered.
So most plans don't cover them. That's not an accident. It's the system working as designed.
Here's the catch that flips the answer: Wegovy isn't just a weight-loss drug anymore. The FDA has approved it for three different uses:
- 1Chronic weight management (June 2021) — The original approval.
- 2Cardiovascular risk reduction (March 2024) — For adults with established cardiovascular disease plus obesity or overweight.
- 3Noncirrhotic MASH with moderate-to-advanced liver fibrosis (August 15, 2025) — Wegovy injection 2.4 mg, under accelerated approval.
Some current insurer policies create separate pathways for Wegovy when it is requested for cardiovascular risk reduction or MASH instead of weight management. That can change the coverage path, but it still has to be verified against your exact plan's formulary and prior authorization policy.
Does HealthCare.gov Cover Wegovy?
HealthCare.gov doesn't “cover” anything — it's a shopping platform, not an insurer.
The plans sold on HealthCare.gov are issued by private insurance companies, and each plan decides whether to include Wegovy on its drug list. Among those plans, only about 1% covered Wegovy for weight loss in KFF's 2024 analysis, and every plan that did required prior authorization.
If you're on HealthCare.gov shopping plans right now, the prescription drug filter is your most important tool. Add Wegovy to your prescription list before comparing plans, and the platform will show which plans include the drug on formulary. (It doesn't show whether the prior authorization will actually be approved — that's a separate step.)
The state-based marketplaces — Covered California, NY State of Health, MNsure, Pennie, Connect for Health Colorado, and others — have their own equivalent prescription filters. Coverage rates can differ because state-run marketplaces sometimes have stronger formulary inclusion, especially in California and New York.
Does Obamacare Cover Wegovy?
“Obamacare” is shorthand for the ACA and the Marketplace plans created under it. ACA Marketplace plans cover prescription drugs as an Essential Health Benefit, but coverage of any specific medication — including Wegovy — depends on the plan's formulary, prior authorization rules, and benefit design. Most Obamacare plans don't cover Wegovy for weight loss.
The reason comes down to one rule. ACA-compliant plans must cover at least one drug in each major drug category, using categories set by the United States Pharmacopeia (USP). CMS has confirmed the USP categories that count for ACA compliance don't include drugs for “anorexia, weight loss, or weight gain.” The states that have moved beyond the federal floor did it through their Essential Health Benefits benchmark plan.
State EHB Benchmark Plans That Include Weight-Loss Medication
| State | When It Took Effect | What the Benchmark Includes |
|---|---|---|
| New Mexico | 2022 plan year | Anti-obesity medications as part of medically necessary treatment of morbid obesity and obesity |
| North Dakota | 2025 plan year | Weight-loss drugs, including GLP-1s, for treatment of morbid obesity |
| North Carolina | Pre-existing | Some anti-obesity medications (e.g., phentermine) for long-term use; the benchmark plan excludes drugs for "short-term treatment of clinical obesity" |
Outside those states, weight-loss drug coverage is purely optional — each insurer decides for itself, plan by plan.
Why Most Marketplace Plans Don't Cover Wegovy
The ACA requires Marketplace plans to cover prescription drugs as an Essential Health Benefit, but federal rules specifically exclude drugs used only for weight loss from that requirement. That's why coverage decisions get made state-by-state, plan-by-plan, and most plans say no.
Here's something most articles skip. A drug being on the formulary doesn't mean you walk into the pharmacy and pay $25. There are four other things in the way:
Tier placement
Wegovy, when covered, is almost always on a specialty or preferred-brand tier with a high copay or coinsurance.
Prior authorization
Every Marketplace plan that covered Wegovy in KFF's federal dataset required this -- your prescriber must submit paperwork first.
Step therapy
Some plans make you try cheaper drugs first before they'll approve Wegovy.
Quantity limits
Caps on how much medication the plan will pay for each month.
“Covered” can still mean $200+ per month after insurance. The path from “on formulary” to “$25 at the pharmacy” usually requires a successful prior authorization, the manufacturer Savings Offer, and a plan that doesn't have an accumulator program eating up manufacturer discounts.
Which 2026 Marketplace States or Carriers Cover Wegovy?
The RWJF-funded 2026 Marketplace carrier review found GLP-1 obesity coverage concentrated in nine states across 26 of 300 state-plus-carrier offerings. California and North Dakota were the only two states where every carrier in the review offered plans covering GLP-1s for obesity. Being in one of these states does not guarantee your plan covers Wegovy — it just means coverage exists somewhere in that state.
| State | Marketplace Type | Coverage Pattern in 2026 Carrier Review |
|---|---|---|
| California | State-based (Covered California) | Coverage found across carriers in the review |
| Delaware | Federally facilitated | At least one carrier covers GLP-1s for obesity |
| Georgia | State-based (Georgia Access) | At least one carrier covers GLP-1s for obesity |
| North Dakota | Federally facilitated | Coverage found across carriers in the review; EHB benchmark added weight-loss meds in 2025 |
| New York | State-based (NY State of Health) | At least one carrier covers GLP-1s for obesity |
| Pennsylvania | State-based (Pennie) | At least one carrier covers GLP-1s for obesity |
| Rhode Island | State-based (HealthSource RI) | At least one carrier covers GLP-1s for obesity |
| Vermont | State-based (Vermont Health Connect) | At least one carrier covers GLP-1s for obesity |
| West Virginia | Federally facilitated | At least one carrier covers GLP-1s for obesity |
Source: RWJF-funded 2026 Marketplace carrier review. For historical context, RWJF's 2024 Marketplace Pulse identified 13 states with at least one plan covering Wegovy for obesity — the 2026 nine-state list is narrower, reflecting carrier changes. If your state isn't on this list, coverage is rare but not impossible; verify your plan's formulary.
Real 2026 Marketplace Plan Examples (Verified May 14, 2026)
Marketplace Wegovy coverage in 2026 looks nothing like a single national rate. We pulled four real, current plan documents to show you what the actual decisions look like — not 2024 averages, not “it varies,” but the language insurers are using right now.
The Marketplace Wegovy Coverage Reality Matrix
| Issuer / Source | Market Segment | What We Found | Status | Plan Year | What It Proves |
|---|---|---|---|---|---|
| HAP (Health Alliance Plan) — 2026 QHP Drug Formulary PDF | Marketplace Qualified Health Plan | Wegovy HD, Wegovy oral tablets, and Wegovy injection pens all listed as "Not Covered – Excluded" | Hard exclusion | 2026 | A plan can technically have drug benefits and still exclude Wegovy in every form. Verify before you enroll. |
| BCBS North Dakota — provider pharmacy update | Health Insurance Marketplace / NetResults formularies | Wegovy oral tablets added effective February 1, 2026 | Preferred brand tier, PA required | 2026 | Marketplace formularies aren't frozen. A plan that didn't cover Wegovy last quarter can add it. But "added" still means prior authorization. |
| Ambetter (Centene) — clinical policy CP.PMN.295 | Marketplace + Medicaid policy | Policy covers FDA-approved indications but states Wegovy "for weight management" is a benefit exclusion and will not be authorized | Indication-based exclusion | 2026 | "Excluded for weight management" doesn't always mean excluded for every use. The CV and MASH pathways may be handled differently. |
| Fallon Health Community Care — 2026 plan policy update | Marketplace plan | Weight-loss drugs including Wegovy not covered starting January 1, 2026; GLP-1s remain covered for diagnosed type 2 diabetes | 2026 renewal exclusion | 2026 | Plans can drop weight-loss coverage at the new plan year even if they covered it before. Check the current plan year, not when you first enrolled. |
| KFF analysis (federal Marketplace, 2024 dataset) | All HealthCare.gov plans | 1% of plans covered Wegovy for weight loss; 82% covered Ozempic | Historical benchmark | 2024 | The base rate is rare. Specific 2026 plans may differ -- verify yours. |
| RWJF-funded 2026 carrier review | 300 state-plus-carrier Marketplace offerings | 26 of 300 offerings cover GLP-1s for obesity across 9 states | Current 2026 evidence | 2026 | Coverage is real but concentrated. New England, CA, NY, and ND lead. |
What this matrix proves — three things, in order of importance:
- 1.You cannot guess your coverage from your insurance company's name. A "BCBS plan" doesn't tell you anything until you read the formulary.
- 2.The label matters. "Excluded," "not covered," "non-formulary," and "covered with prior authorization" are four different problems with four different solutions.
- 3.The medically accurate FDA-approved indication matters. Some plan policies treat weight management, cardiovascular risk reduction, and MASH as separate coverage pathways with different criteria.
Stop guessing — have Ro check your specific plan for free
Ro's GLP-1 Insurance Coverage Checker contacts your insurer, confirms whether Wegovy is on your drug list, and tells you whether prior authorization is required — before you commit to anything.
Run free Ro coverage check →Sponsored affiliate linkDoes Marketplace Insurance Cover Wegovy for Heart Disease or MASH?
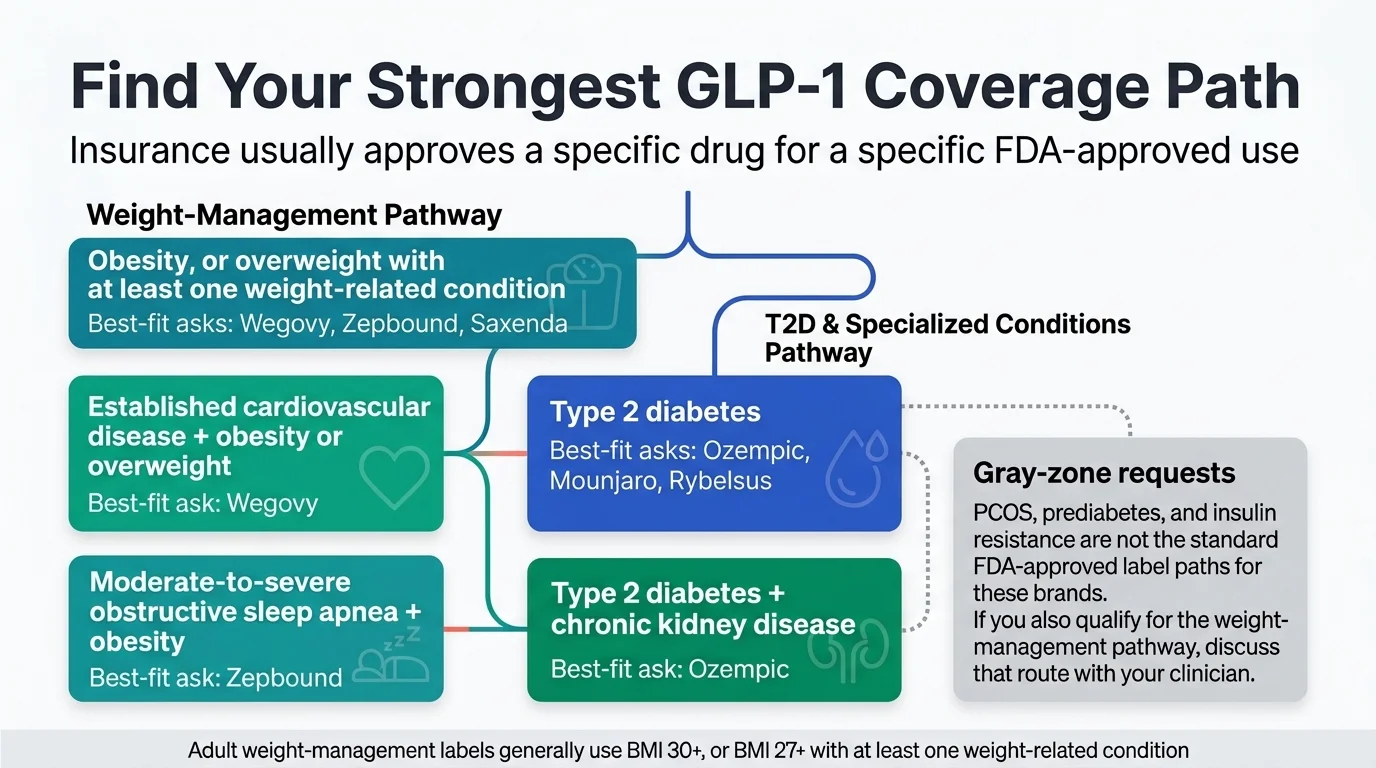
Wegovy has FDA-approved indications beyond weight management: cardiovascular risk reduction in adults with established heart disease plus obesity or overweight, and noncirrhotic MASH with moderate-to-advanced liver fibrosis. Some insurer policies create separate coverage pathways for these indications, with different criteria from weight-management requests. Coverage still depends on your plan's formulary and prior authorization policy.
Who actually qualifies for the cardiovascular indication
Your clinician decides whether the indication is medically appropriate. Your insurer decides whether the submitted documentation satisfies coverage criteria.
- ✓Established cardiovascular disease (previous heart attack, stroke, or peripheral artery disease)
- ✓AND body mass index of 27 or higher (overweight) or 30 or higher (obesity)
- ✓AND you're an adult
The SELECT clinical trial (March 2024 FDA approval) showed Wegovy reduced major cardiovascular events by about 20% in this population. That's the data insurer policies respond to. See our GLP-1 adverse event rates guide for the full trial data.
Weight-Loss Exclusion vs CV/MASH Pathway — Verified Policy Examples
| Source | Weight-Management Coverage | Non-Weight-Management Indication |
|---|---|---|
| Ambetter/Centene policy CP.PMN.295 | Excluded for weight management; will not be authorized | Policy addresses FDA-approved indications separately |
| Fallon Health Community Care 2026 | Weight-loss drugs not covered starting Jan 1, 2026 | GLP-1s remain covered for diagnosed type 2 diabetes |
How the prescription wording affects coverage
The medically accurate FDA-approved indication matters because it determines which plan criteria apply. If you genuinely meet the cardiovascular criteria, the question worth asking your clinician is: “Given my full health history, is the cardiovascular indication medically appropriate to use for the prescription?” That single question is worth asking before an appeal. The CV indication isn't a cheat code — you still need PA, and some plans still deny it. And if you don't have established cardiovascular disease, the indication can't ethically be used just to get coverage.
How to Check Your Specific Marketplace Plan in 10 Minutes
The fastest way to confirm whether your Marketplace plan covers Wegovy is to (1) find your plan's formulary, (2) search for “Wegovy” or “semaglutide,” (3) read the symbols next to it, and (4) call your insurer to verify. There are two paths below: the 6-step self-check and Ro's free coverage checker that skips steps 2 through 5.

Method A: The 6-Step Self-Check (10 minutes)
Find your exact plan name
Don't search by insurance company alone. Find the full plan name, metal level (Bronze/Silver/Gold/Platinum), year, and state. It's on your insurance card, your HealthCare.gov dashboard, or your enrollment paperwork.
Open the formulary, not the marketing page
Search Google for "[your plan name] 2026 formulary PDF" or look in your member portal under "Prescription drugs" or "Drug list." Plans publish a real PDF that lists every covered medication.
Search the formulary three ways
Press Ctrl-F (or Cmd-F on Mac) and search for: Wegovy, semaglutide, and weight (to catch exclusion language).
Read the symbols
See the decoder table below. "Covered" and "covered with PA" are four completely different problems.
Call your insurer with the exact script below
The number is on the back of your insurance card. Write down the date, time, and the rep's name and reference number.
Save proof
Screenshot the formulary page. Save the PDF. Note the date you accessed it. Formularies change mid-year, and the version you confirmed coverage on is your strongest documentation if anything gets disputed later.
Formulary Symbol Decoder
| Symbol or Label | What It Means in Plain English |
|---|---|
| Covered | The plan pays. Check the tier for your copay. |
| PA (prior authorization) | Your clinician has to submit paperwork before the plan pays. Possible coverage, not guaranteed. |
| ST (step therapy) | You have to try a cheaper drug first. |
| QL (quantity limit) | The plan caps how much you can get per month. |
| NF or non-formulary | Not on the standard drug list. You can request an exception. |
| Not covered | The plan won't pay for it today. Some exceptions possible. |
| Excluded | The plan's benefit design specifically blocks it. Hardest to overcome. |
Step 5 call script — read this word for word to your insurer
“Hi, I'm calling about coverage for Wegovy under my plan. My member ID is [____]. Can you confirm four things?
One — is Wegovy on my plan's formulary, and if so, what tier?
Two — does my plan require prior authorization or step therapy for Wegovy?
Three — does my plan handle the cardiovascular risk reduction or MASH indications differently from weight management?
Four — if Wegovy is not covered or is denied, what's the formulary exception process and the timeline?”
Write down the answer, the date, the time, and the representative's name and reference number. If you ever need to appeal, this call is evidence.
Method B: Free Ro Coverage Check (5 minutes)

If you don't want to call insurance companies or read drug list PDFs, Ro has a free Insurance Coverage Checker that handles steps 2 through 5 for you.
Here's what Ro says happens when you use it:
- 1.You enter your insurance details (no prescription, no payment)
- 2.Ro's team contacts your insurer
- 3.They pull your formulary status, prior authorization requirements, and estimated cost
- 4.They send you a personalized coverage report
No commitment. No obligation to use Ro after. You walk away with the answer.
We feature Ro for this specific job because Ro is a verified telehealth platform with a published GLP-1 insurance checker and insurance concierge process, and it works with FDA-approved Wegovy (both the pen and the oral tablet) — not compounded semaglutide.
Run your free Wegovy coverage check on Ro →sponsored affiliate linkWhat “Covered with Prior Authorization” Really Means for Wegovy
Prior authorization (PA) is a process where your clinician must submit paperwork to your insurance company showing the medication is medically necessary, before the plan will pay. In KFF's 2024 federal Marketplace dataset, every Marketplace plan that covered Wegovy required PA. PA isn't a denial — it's a gate. Ro says its GLP-1 prior authorization process usually takes 2–3 weeks and can take longer if the initial request is denied.

What Marketplace PA forms typically ask for
- •Diagnosis and FDA-approved indication (weight management, CV risk reduction, MASH)
- •BMI -- usually 30+, or 27+ with at least one weight-related condition
- •Weight-related conditions (high BP, sleep apnea, prediabetes, established CVD)
- •Documentation of past weight-loss attempts (diet, exercise, counseling -- with dates)
- •Medical history and contraindications
- •Current medications
Top 5 PA friction points insurers flag
- 1.Missing weight-loss attempt documentation -- "tried diet" without dates or details
- 2.BMI documentation gaps -- no recent BMI on file
- 3.Indication mismatch -- generic "obesity" coding when patient might qualify for CV indication
- 4.Step therapy not satisfied -- plan required trying a different drug first
- 5.Insufficient comorbidity documentation -- conditions listed without supporting records

Or skip the work and let Ro's concierge handle it
Ro says its insurance concierge checks coverage, handles paperwork, submits PA requests, and continues working if the insurer denies the initial request — including exploring additional information, other clinically appropriate GLP-1 options, or cash-pay options.
Ro Body starts at $39 for the first month, then $149/month ongoing, or as low as $74/month with annual plan paid upfront. The membership is separate from medication cost, and insurance doesn't cover the membership.
Wegovy Coverage by Insurance Type: How Marketplace Compares
Marketplace is the most restrictive segment for Wegovy coverage. For reference, here's how other insurance types compare.
| Insurance Type | Wegovy Coverage for Weight Loss | Best Resource |
|---|---|---|
| ACA Marketplace (HealthCare.gov) | ~1% of plans in KFF 2024 federal dataset | This page |
| ACA Marketplace (state-run) | More common in CA, NY; still plan-specific | This page |
| Large-employer commercial | 19% of firms with 200+ workers; 43% of firms with 5,000+ workers (KFF 2025) | Best GLP-1 Providers That Accept Insurance |
| Self-funded employer | Plan-by-plan | Your benefits administrator |
| Medicaid | 13 state FFS programs covered GLP-1s for obesity as of January 2026 | GLP-1 providers that accept Medicaid |
| Medicare Part D | Not routinely for weight loss; possible for cardiovascular indication | Does Medigap Cover Wegovy? |
| Medicare GLP-1 Bridge | $50/month for eligible Part D beneficiaries, July 1 – Dec 31, 2027 | Medigap + Bridge guide |
| TRICARE | Possible with PA | Provider-specific |
What Real Marketplace Patients Are Dealing With
KFF's 2025 GLP-1 polling was blunt: 56% of adults who had taken GLP-1 medications said they were difficult to afford, and 22% said insurance covered the full cost.
“I was not expecting insurance help. Usually patients are their own advocate, so I was thrilled to not have to fight for my coverage.”
— Ro member, published patient testimonial. Individual experience; not a coverage guarantee.
We're including this not to imply Ro will get every reader covered — they won't. But the insurance navigation work is real and verifiable on Ro's public pages. If you've ever spent an afternoon on hold with a Marketplace insurer, the value of someone else handling it is immediate.
How to Actually Move Forward Today
Pick the description that fits you and follow the path.
I have a Marketplace plan and I don't know if it covers Wegovy.
Do the 6-step self-check, OR let Ro's free coverage checker do it for you. Either way, get the answer before you spend money.
Run free Ro coverage check →sponsoredMy Marketplace plan covers Wegovy but requires prior authorization.
Work with your existing prescriber to submit a complete PA, or let Ro's insurance concierge handle the paperwork as part of Ro Body membership ($39 first month, then $149/month, or as low as $74/month with annual plan paid upfront).
See if Ro can support your PA paperwork →sponsoredMy Marketplace plan denied my Wegovy PA.
File an internal appeal within 180 days of receiving notice. If you have established cardiovascular disease and obesity/overweight, ask your clinician about the CV indication. Ro's concierge continues working when insurers deny the initial request.
Check whether Ro can support your coverage paperwork →sponsoredMy Marketplace plan excludes Wegovy entirely.
You have two realistic moves: (1) pay cash through NovoCare or Ro at manufacturer-matched prices, or (2) switch plans at the next Open Enrollment if a better-covered plan exists in your state. Cash-pay through Ro starts at $199/month for starting doses (through June 30, 2026).
See current Wegovy cash-pay pricing on Ro →sponsoredI want provider choice and a lower ongoing program fee.
Sesame Care is the secondary FDA-approved option here -- providers can prescribe Wegovy and evaluate insurance-covered options and preauthorization paperwork. Good fit if you want a licensed provider evaluation without a $149/month membership.
See Wegovy options on Sesame →sponsoredI'm not sure where I fit yet.
That's what the quiz is for. It takes 60 seconds and gives you a personalized plan based on your insurance, state, and goals.
Take the free 60-second matching quiz →
Frequently Asked Questions
Does Obamacare cover Wegovy?
"Obamacare" usually means ACA Marketplace plans. Most Marketplace plans don't cover Wegovy for weight loss -- only about 1% in KFF's 2024 federal dataset did. Coverage is more common in some state-run marketplaces (especially California, New York, and North Dakota) and may follow a separate pathway for the cardiovascular or MASH indications.
Does HealthCare.gov cover Wegovy?
HealthCare.gov is a shopping platform, not an insurer. It sells plans from many insurance companies. Among those plans in KFF's 2024 federal analysis, only about 1% covered Wegovy for weight loss, and every plan that did required prior authorization. Use the prescription drug filter on HealthCare.gov when comparing plans to find which ones include Wegovy on formulary.
Does the ACA require coverage for weight-loss drugs?
No. The Affordable Care Act requires Marketplace plans to cover prescription drugs as an Essential Health Benefit, but CMS has confirmed that the required drug categories don't include medications for "anorexia, weight loss, or weight gain." Coverage is decided state-by-state through each state's Essential Health Benefits benchmark plan. Only New Mexico, North Dakota, and North Carolina (partially) have added weight-loss drugs to their state benchmark.
Why does my plan cover Ozempic but not Wegovy?
Ozempic is a different FDA-approved product with the same active ingredient as Wegovy (semaglutide), approved for type 2 diabetes -- not weight management. Wegovy is FDA-approved for weight management, cardiovascular risk reduction, and MASH. Many Marketplace plans cover GLP-1 drugs for diabetes (about 82% of plans covered Ozempic in KFF's 2024 federal dataset) but exclude them for weight loss. Coverage follows the FDA indication and the plan's benefit design.
Can I get Wegovy covered for a cardiovascular condition on a Marketplace plan?
Some plans may treat the cardiovascular indication separately from weight-loss exclusions, but coverage still depends on the plan's prior authorization policy. Wegovy is FDA-approved to reduce major cardiovascular events in adults with established heart disease plus obesity or overweight. Talk to your clinician about whether the indication applies to your full health picture -- and ask your plan specifically about CV indication coverage before assuming a blanket exclusion applies.
Does Wegovy require prior authorization on Marketplace plans?
In KFF's 2024 federal Marketplace analysis, every plan that covered Wegovy required prior authorization. The paperwork is filled out by your prescriber and typically includes BMI documentation, weight-related conditions, prior weight-loss attempts, and the FDA-approved indication being treated.
How much is Wegovy with Marketplace insurance?
If covered with the Wegovy Savings Offer applied, eligible commercial-insurance patients may pay as little as $25 per month -- verify the current maximum savings and terms directly on NovoCare. Without insurance coverage, cash-pay through NovoCare or Ro starts at $199 per month for starting injection doses (through June 30, 2026), then $349/month for maintenance injection doses, $399/month for Wegovy HD, and $149-$299/month for the Wegovy pill depending on dose.
Can I appeal a Wegovy denial?
Yes. You must file your internal appeal within 180 days (6 months) of receiving notice that your claim was denied. If that fails, you have the right to a free federal external review, or a state/independent review process where any fee cannot exceed $25. Most legitimate denials based on documentation gaps get reversed on appeal when the PA is resubmitted with complete records.
Should I switch Marketplace plans just to get Wegovy covered?
Maybe -- but don't switch based on drug coverage alone. Compare total annual cost: premium, deductible, copay, and network. A higher-premium plan that covers Wegovy can beat a cheaper plan that excludes it, but only if the math works out. Use HealthCare.gov's prescription drug filter to find plans that include Wegovy before Open Enrollment ends.
Does the Wegovy pill have the same Marketplace coverage as the injection?
Not necessarily. In a May 2026 spot check, BCBS North Dakota added Wegovy oral tablets with prior authorization effective February 1, 2026, while HAP's 2026 QHP formulary listed Wegovy oral tablets as Not Covered-Excluded. Coverage decisions for the pill are made separately from the injection in each plan's formulary. Verify your exact plan.
Does Wegovy HD have Marketplace coverage?
In a May 2026 spot check, HAP's 2026 QHP formulary listed Wegovy HD 7.2 mg (FDA approved March 2026) as Not Covered-Excluded. NovoCare lists Wegovy HD cash-pay at $399/month. Verify your specific plan's formulary -- HAP's status does not predict your plan.
Is the Medicare GLP-1 Bridge for Marketplace plan holders?
No. The Medicare GLP-1 Bridge is exclusively for eligible Medicare Part D beneficiaries. It runs from July 1, 2026 through December 31, 2027 and offers covered GLP-1s at a flat $50/month copay. Marketplace plan holders are not eligible for the Bridge.
Is compounded semaglutide covered by Marketplace insurance?
Compounded semaglutide is not FDA-approved as a finished drug product. Most Marketplace plans do not cover compounded medications as a substitute for brand-name Wegovy, and the plans that exclude Wegovy for weight loss typically exclude compounded semaglutide as well. Check your plan documents before assuming any compounded medication is covered.
What's the fastest way to know if my plan covers Wegovy?
Two options: (1) Find your plan's formulary PDF, search for "Wegovy" or "semaglutide," read the tier and PA symbols, and call your plan's member services to confirm -- about 10 minutes. (2) Use Ro's free GLP-1 Insurance Coverage Checker -- Ro says it contacts your insurer and emails you the coverage report.
How We Verified This Page (and What We Didn't)
Sources used:
- ✓HealthCare.gov Marketplace benefit, prescription-drug, internal appeals, and external review pages
- ✓KFF analysis of federal Marketplace formularies -- Wegovy coverage in 2024
- ✓KFF 2025 Employer Health Benefits Survey
- ✓KFF Medicaid GLP-1 coverage and spending update (January 2026)
- ✓KFF 2025 GLP-1 polling
- ✓Robert Wood Johnson Foundation Marketplace Pulse (2024 state-level coverage tracking)
- ✓RWJF-funded 2026 carrier review (current Marketplace GLP-1 obesity coverage)
- ✓Health Alliance Plan (HAP) 2026 QHP formulary PDF
- ✓BCBS North Dakota pharmacy update for Wegovy oral tablets
- ✓Ambetter/Centene clinical policy CP.PMN.295 (Semaglutide for Wegovy)
- ✓Fallon Health Community Care 2026 plan policy update
- ✓FDA approval announcements for Wegovy MASH indication (August 15, 2025) and Wegovy HD (March 19, 2026)
- ✓Novo Nordisk press release on the Wegovy pill FDA approval (December 22, 2025)
- ✓NovoCare published pricing for Wegovy injection, Wegovy HD, and Wegovy pill
- ✓Ro's published GLP-1 Insurance Coverage Checker, pricing, and insurance concierge pages
- ✓Sesame Care's published Wegovy and online weight-loss program pages
- ✓CMS Medicare GLP-1 Bridge official page
Related Guides on The RX Index
- Best GLP-1 Providers That Accept Insurance
- Does Medigap Cover Wegovy? No -- Here's Why and What Actually Does (2026)
- GLP-1 Providers That Accept Medicaid (2026)
- GLP-1 Providers That Accept Medicare Advantage (2026)
- Does COBRA Cover Wegovy? 2026 Rules and What Actually Pays
- GLP-1 FDA Indication vs Off-Label Use: The Real Difference
- Cheapest Wegovy Without Insurance
- Wegovy Savings Card: Qualify, Cost & Enroll
- Best Telehealth for Wegovy
- Does Medicare Cover Wegovy for Weight Loss?
- GLP-1 Path Quiz -- Find the Option That Fits Your Situation
Still Not Sure Which GLP-1 Path Is Right for You?
Take our free 60-second matching quiz and get a personalized plan based on your insurance, your state, your goals, and whether you're looking at brand-name Wegovy or another GLP-1. No sign-up to see your match.
Take the Free 60-Second Matching Quiz →If your plan excludes Wegovy and you can't wait for Open Enrollment, Ro is the most direct cash-pay path to FDA-approved Wegovy right now.
See current Ro Wegovy pricing →sponsored affiliate link — see disclosureLast verified: May 14, 2026. Next scheduled verification: quarterly (monthly during Open Enrollment). The RX Index Editorial Team.
The RX Index is a pricing intelligence and comparison resource for GLP-1 telehealth providers. We don't sell health insurance plans, prescribe medications, or accept payment from providers to feature their offers more prominently. When we link to an affiliate provider, we mark the link clearly and the commission doesn't change what you pay.
Medical disclaimer: This is informational content, not medical advice. Wegovy requires evaluation and prescription by a licensed healthcare provider. Insurance coverage decisions are made by your specific plan based on your specific medical situation. Always verify with your plan before relying on any coverage information.
Wegovy® is a registered trademark of Novo Nordisk. This page is not affiliated with Novo Nordisk, Ro, Sesame Care, or any health insurance plan.