GLP-1 Providers That Accept Medicaid: 2026 Verified Paths
Published: · Last reviewed:
By The RX Index Editorial Team · Last verified: May 13, 2026 · Sources: KFF, CMS, FDA, state Medicaid bulletins, individual provider terms · Methodology ↓ · Affiliate disclosure ↓
If you searched for GLP-1 providers that accept Medicaid, here's the honest answer:
Almost no famous GLP-1 telehealth brand accepts Medicaid. Not Hims. Not Hers. Not Ro. Not Sesame. Not Eden. Not MEDVi. They're cash-pay businesses.
The two consumer telehealth names we've verified that do bill Medicaid for GLP-1 care are knownwell (which says it accepts Medicare and Medicaid in some states — MassHealth confirmed on its insurance page; verify availability for your exact plan at intake) and Accomplish Health (which lists New York Medicaid and SoonerCare — Oklahoma Medicaid; Accomplish communications indicate it has joined forces with knownwell, so verify at intake whether your application still routes through Accomplish or now through knownwell).
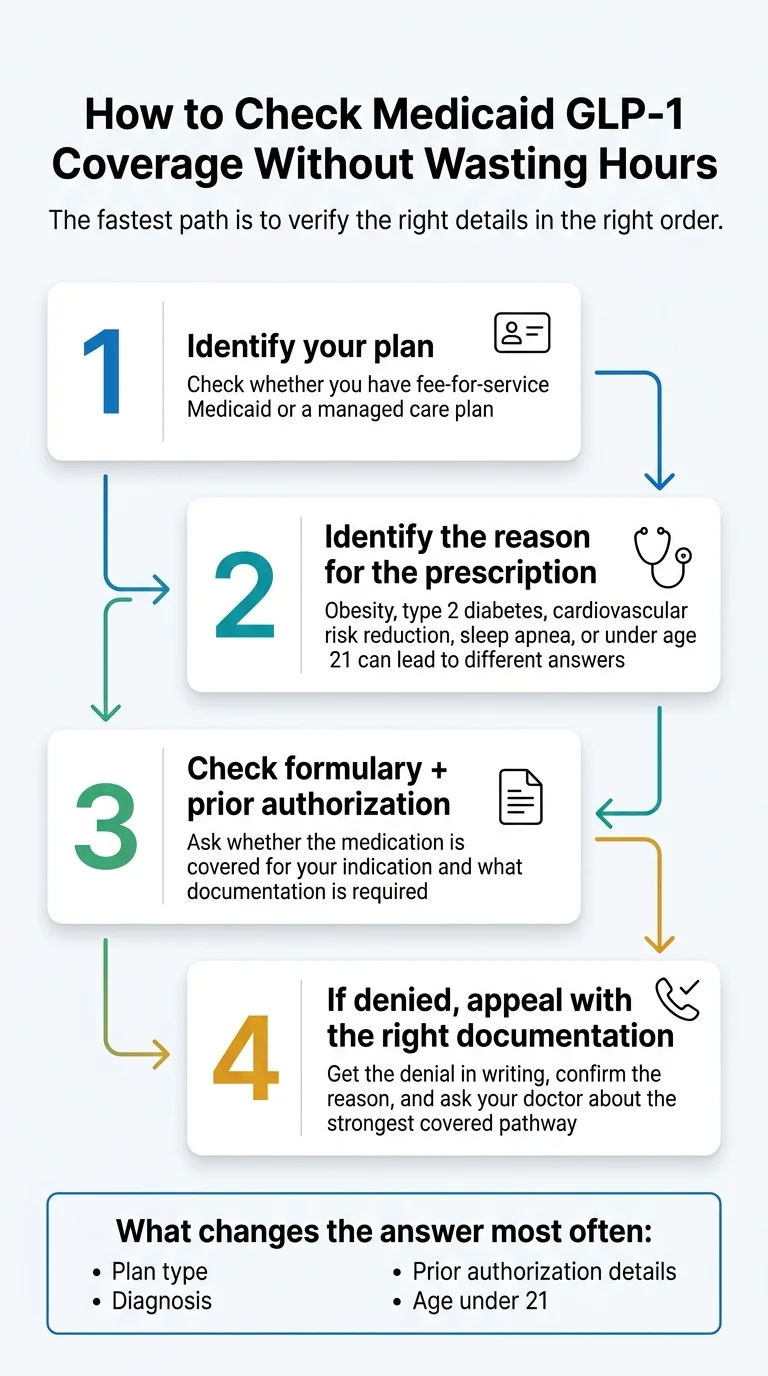
For most people on Medicaid, the cleanest route isn't a national telehealth brand at all. It's your existing primary care doctor, a community health center, or a specialist in your Medicaid network — plus a prior authorization for the medication. What changes the answer: your state, your diagnosis, and your age.
Find your Medicaid GLP-1 route in 60 seconds
4 questions. Personalized 3-step action plan based on your state, diagnosis, and plan type. No email required to see results.
→ Run the Medicaid GLP-1 Route FinderWhat this page does (and doesn't) do
If you came here looking for a slick “best telehealth brand for Medicaid” list, you won't find one — because the list is almost empty. Pretending otherwise would waste your time and burn your week on intake forms that can't bill your plan.
Here's what you will find:
- ✓A verified list of GLP-1 providers that actually accept Medicaid right now
- ✓A clear way to check whether your state and your specific plan will cover the medication
- ✓The diagnosis pathways that can unlock Medicaid coverage even when obesity is excluded
- ✓A step-by-step plan for what to do this week
- ✓Honest cash-pay options for readers who are no longer on Medicaid
First-screen decision table
| If you're in this situation… | Your best first move |
|---|---|
| You want an online provider that bills Medicaid | Check knownwell availability in your state and plan at intake. If knownwell doesn't cover you, use the local-doctor route below. |
| You already have a primary care doctor who takes your Medicaid | Book a visit and ask them to evaluate you for a GLP-1 and submit prior authorization. This is the cleanest route for most people. |
| You're in a state that doesn't cover GLP-1s for weight loss | Ask whether you have a documented covered indication (type 2 diabetes, established cardiovascular disease with overweight or obesity, moderate-to-severe sleep apnea with obesity, or MASH with moderate-to-advanced fibrosis). |
| You're under 21 on Medicaid | EPSDT (a federal Medicaid medical-necessity rule for kids and teens) requires your plan to evaluate medical necessity even when adult obesity coverage is excluded. |
| You just got dropped (California, New Hampshire, Pennsylvania, South Carolina) | Check the appeal deadline on your denial letter immediately. Then ask your doctor about a covered indication. |
| You've checked everything and Medicaid genuinely won't cover you | Skip to the cash-pay section below -- clearly labeled, not Medicaid billing. |
Which GLP-1 providers that accept Medicaid can you actually use in 2026?
Answer in two sentences
As of May 2026, the two consumer telehealth brands we've verified that bill Medicaid for GLP-1 care are knownwell (which states it accepts Medicare and Medicaid in some states, with MassHealth options listed on its insurance page) and Accomplish Health (which lists New York Medicaid and SoonerCare, with intake likely routing through knownwell following a partnership). Every other major direct-to-consumer GLP-1 brand — including Hims, Hers, Ro, Sesame, Eden, MEDVi, SHED, Found, Lemonaid — does not accept Medicaid.
The verified Medicaid provider matrix
Built from each provider's own terms, insurance pages, and intake disclosures verified between May 1 and May 13, 2026. Verification log below.
| Provider | Bills Medicaid for GLP-1 care? | What we verified | What to do |
|---|---|---|---|
| knownwell | In some states. | knownwell.co states it accepts Medicare and Medicaid in some states; ABOM-certified obesity medicine clinicians; in-house prior authorization team that knownwell reports has an 80% success rate. Insurance page lists Massachusetts/MassHealth. Start page lists new patients in MA, NH, RI. | Confirm your state and your specific Medicaid plan at intake before scheduling. |
| Accomplish Health | Lists New York Medicaid and SoonerCare (Oklahoma Medicaid). Likely now routing through knownwell. | Accomplish's insurance page lists NY Medicaid and SoonerCare. Public communications indicate the knownwell partnership. | Start on knownwell.co; confirm whether your application still routes through Accomplish or now through knownwell. |
| Your in-network PCP, FQHC, or specialist | Yes, if they're in your Medicaid plan's network. | In-network status verified via your Medicaid card and MCO directory; FQHCs are expected to participate in Medicaid and CHIP, but individual sites still need to take your specific plan. | This is the cleanest route for most people. See the 5-step plan below. |
| Hims | No -- cash-pay only. | Hims support page states it is unable to accept insurance for its programs. The March 2026 Novo Nordisk partnership added Wegovy pill, Wegovy pen, and Ozempic to its cash-pay menu. | Not a Medicaid option. |
| Hers | No -- cash-pay only. | Same as Hims following the Novo Nordisk partnership. | Not a Medicaid option. |
| Ro | No -- Medicaid users excluded. | Ro's insurance policy explicitly states that Medicaid (and other government-funded plan) members cannot join Ro Body or pay out of pocket through Ro. | Not a Medicaid option. Listed in the cash-pay section below only for readers no longer enrolled in Medicaid. |
| Sesame Care | No -- Sesame does not accept Medicare, Medicaid, or other third-party insurance for its services. | Sesame's terms of service exclude government and third-party insurance for the Sesame service itself. | Not a Medicaid-billing option. |
| Eden | No -- cash-pay only. | Eden runs a cash-pay/HSA-FSA model. | Not a Medicaid option. |
| MEDVi | No -- cash-pay only. | Cash-pay model. Not featured as a recommendation on this page due to the FDA's February 20, 2026 warning letter regarding false or misleading claims about its compounded semaglutide and tirzepatide products. | Not recommended on this page. |
| Found | Some commercial insurance carriers; Medicaid not a listed payer. | Found's site says it partners with commercial carriers in some states. | Not a reliable Medicaid route. |
| LifeMD | Some commercial insurance support; Medicaid not a standard payer. | LifeMD's weight management program supports some commercial PAs. | Not a reliable Medicaid route. |
| Walgreens Weight Management | Cash-pay or commercial; Novo/Lilly savings programs through Walgreens explicitly exclude Medicaid. | Walgreens disclosures exclude government-insured patients from manufacturer savings pricing. | Visit may be covered through some plans; medication savings not available to Medicaid enrollees. |
| Walmart Better Care / Curai | Cash-pay; promotional offers exclude Medicare/Medicaid. | Walmart's April 2026 announcement states promotional free visits are not available to Medicare/Medicaid enrollees. | Not a Medicaid option for GLP-1 medication. |
| Teladoc Weight Management | Only via employer or health plan sponsorship. | Teladoc's program is for sponsored members; not retail Medicaid. | Check whether your Medicaid MCO includes Teladoc as a benefit. |
| Lemonaid | No -- cash-pay only. | Lemonaid's weight-loss program is explicitly cash-pay only. | Not a Medicaid option. |
The damaging admission (and why we're telling you anyway)
The honest truth: the GLP-1 affiliate ecosystem mostly exists for people with commercial insurance or cash. Medicaid users are the underserved corner of this market. If that's frustrating to hear, we hear you. Here's the upside — most people on Medicaid have a cleaner path than they think, and it doesn't run through a flashy telehealth app. It runs through the doctor or clinic that already takes their card. We'll walk you through it.
Verification log (provider matrix sources) ↓
knownwell — knownwell.co/referral, knownwell.co/start, and knownwell.co insurance pages. Checked May 13, 2026. Verified: Medicare and Medicaid accepted in some states; MassHealth on insurance page; new patients in MA/NH/RI on start page; 80% PA team success rate stated on referral page.
Accomplish Health — accomplish.health/insurance. Checked May 13, 2026. Verified: New York Medicaid and SoonerCare listed.
Ro — ro.co/weight-loss/insurance, ro.co/weight-loss/pricing. Checked May 13, 2026.
Sesame Care — sesamecare.com/terms-of-service, sesamecare.com/service/online-weight-loss-program. Checked May 13, 2026.
Hims — support.hims.com (insurance acceptance), hims.com/glp-1 (program pricing). Checked May 13, 2026.
MEDVi — FDA warning letter dated February 20, 2026 (fda.gov inspections/compliance/warning-letters).
Found, Lemonaid, LifeMD, Walgreens, Walmart Better Care, Teladoc — provider terms, FAQ pages, and insurance disclosures. Checked May 1-13, 2026.
Why Medicaid GLP-1 access depends on provider billing, state coverage, and prior authorization
Answer in three sentences
Getting a GLP-1 covered by Medicaid is not one question — it's three. Layer one is whether the provider can bill your specific Medicaid plan. Layer two is whether the state Medicaid program or your MCO lists the medication on its formulary for your diagnosis. Layer three is the prior authorization paperwork that proves you meet the plan's medical criteria.
Does your state's Medicaid cover GLP-1s for weight loss?
Answer in two sentences
Thirteen states cover GLP-1s for obesity treatment under fee-for-service Medicaid as of January 2026, down from 16 in 2025. Medicaid must cover nearly all FDA-approved GLP-1s from participating manufacturers for medically accepted non-obesity indications (like type 2 diabetes), subject to formulary rules and prior authorization.
The 13 states that currently cover GLP-1s for obesity (FFS, January 2026)
Source: KFF Medicaid Coverage of and Spending on GLP-1s, January 2026; Stateline, April 2026.
| Region | States covering GLP-1s for obesity |
|---|---|
| Midwest | Kansas, Michigan (restricted to morbid obesity), Minnesota, Missouri, Wisconsin |
| South | Delaware, Mississippi, North Carolina (reinstated December 2025), Tennessee, Virginia |
| Northeast | Massachusetts (Zepbound preferred; under FY2028 budget review), Rhode Island (under legislative review) |
| West | Utah |
States that dropped coverage on January 1, 2026
California, New Hampshire, Pennsylvania (adults 21 and over), and South Carolina eliminated GLP-1 coverage for obesity on January 1, 2026, citing state budget pressures. If you were previously on a covered GLP-1 in one of these states, see the recent-drop action plan below.
North Carolina briefly dropped coverage in October 2025 and reinstated it in December 2025 after public pressure. Michigan restricted coverage to patients classified as morbidly obese. Massachusetts and Rhode Island are under active legislative review.
Medicaid copays when covered
Medicaid prescription copays are federally capped at low amounts — typically $0 to $8 per fill, depending on your state and income tier. That's dramatically cheaper than cash-pay ($349 to $1,400+ per month). The catch is getting the coverage in the first place.

FFS vs MCO — why your specific plan can answer differently
About 78% of Medicaid enrollees nationally are in managed care plans (MCOs), not fee-for-service. Your MCO might cover something your state's FFS doesn't, or vice versa.
How to check your specific plan in one phone call:
- 1Find your Medicaid card. The MCO name is usually on the front (Molina, Centene, Amerigroup, UnitedHealthcare Community Plan, etc.).
- 2Call the member services number on the back.
- 3Ask: "Is this medication on my formulary?"
- 4Ask: "Which diagnosis codes are covered for this drug?"
- 5Ask: "Is the medication preferred or nonpreferred?"
- 6Ask: "What prior authorization form does my prescriber need?"
- 7Ask: "Does my plan require step therapy?"
- 8Ask: "Which local prescribers are in network for obesity medicine, endocrinology, cardiology, sleep medicine, or hepatology?"
What diagnosis pathways can unlock Medicaid GLP-1 coverage when obesity is excluded?
Answer in two sentences
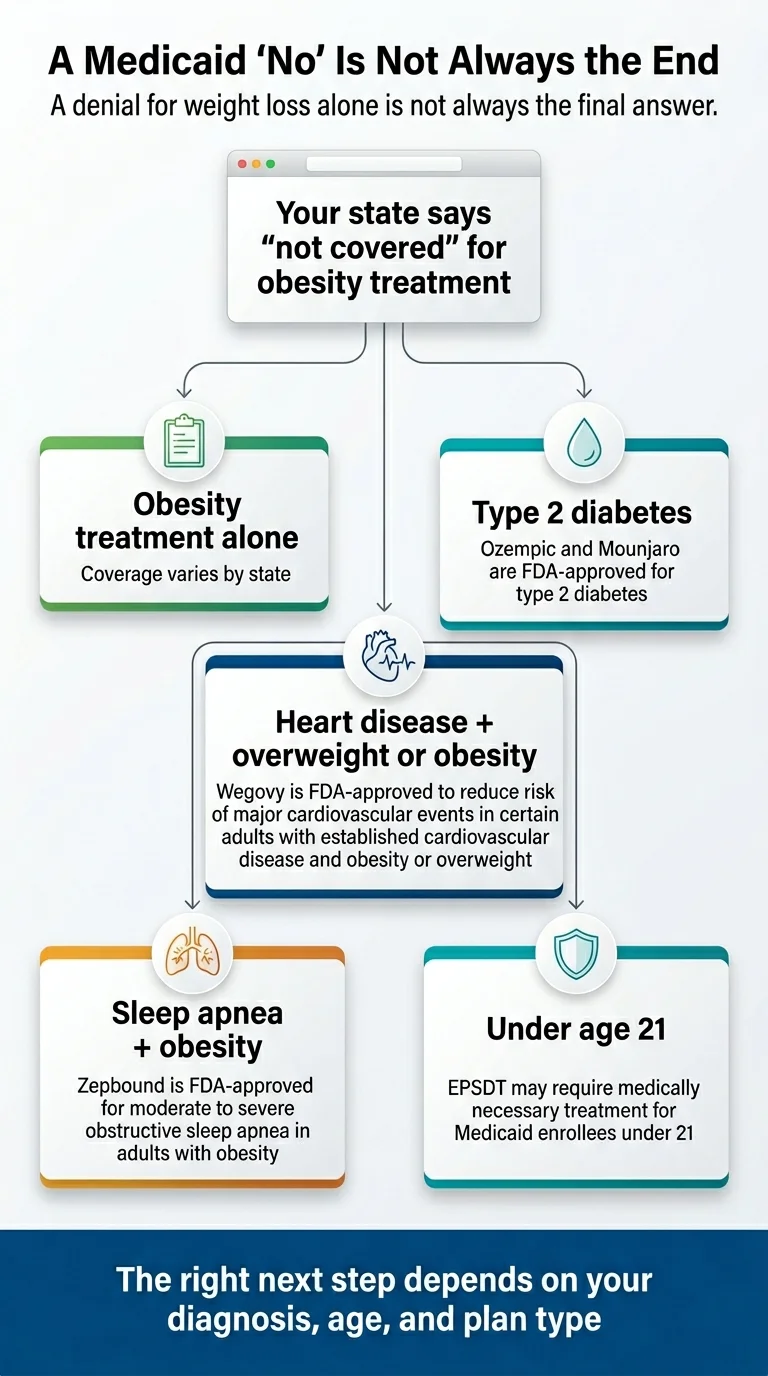
Federal Medicaid law (the Medicaid Drug Rebate Program) requires every state Medicaid program to cover FDA-approved drugs from participating manufacturers for medically accepted indications — with weight-loss drugs as a specific exception states can opt out of. That means GLP-1s prescribed for type 2 diabetes, cardiovascular risk reduction (Wegovy injection), sleep apnea (Zepbound), or MASH (Wegovy injection) create a coverage pathway in every state Medicaid program, though approval still depends on documentation, formulary rules, and prior authorization.
The federally protected pathways
| Diagnosis | Eligible GLP-1 medications | FDA indication | Coverage basis |
|---|---|---|---|
| Type 2 diabetes | Ozempic, Mounjaro, Rybelsus, Trulicity, Victoza (when on state formulary) | Diabetes management | Medically accepted FDA indication; coverage pathway in every state, subject to formulary and PA |
| Cardiovascular event risk reduction (adults with cardiovascular disease + overweight or obesity) | Wegovy injection | FDA approval March 2024 | Medically accepted FDA indication; coverage pathway in every state |
| Moderate-to-severe obstructive sleep apnea + obesity (adults) | Zepbound | FDA approval December 2024 | Medically accepted FDA indication; coverage pathway in every state |
| MASH with moderate-to-advanced fibrosis | Wegovy injection | FDA accelerated approval August 2025 | Medically accepted FDA indication; coverage pathway in every state |
| Obesity alone (no qualifying comorbidity) | Wegovy, Zepbound, Saxenda | Chronic weight management | Optional for states -- 13 states currently cover; the rest can opt out |
What this looks like in practice (if your state dropped obesity coverage)
If you live in California, Pennsylvania, New Hampshire, or South Carolina — the four states that dropped obesity coverage on January 1, 2026 — Medicaid still has a coverage pathway for you in many cases:
- ✓Established cardiovascular disease + overweight or obesity? Wegovy injection has a federally required indication for CVD event risk reduction.
- ✓Moderate-to-severe sleep apnea documented in a sleep study + obesity? Zepbound has a federally required indication for that.
- ✓Type 2 diabetes? A different GLP-1 like Ozempic or Mounjaro can be prescribed under the diabetes indication.
- ✓MASH with moderate-to-advanced fibrosis confirmed on imaging or biopsy? Wegovy injection has an indication for that.
A non-negotiable honesty note
These pathways only work if you actually have one of those diagnoses, documented in your medical record. Do not ask a clinician to label you with a condition you don't have. That would be insurance fraud, and it can cost your prescriber their license. The right move, if you suspect you have an undiagnosed condition (sleep apnea in particular is under-diagnosed in people with obesity), is to ask for the diagnostic workup. A documented sleep study is the most powerful unlock most readers have never thought of.
How to use this with your doctor
Bring this list to your appointment. Ask:
- ›"Do I have any of these diagnoses already documented in my chart?"
- ›"If we suspect I might have sleep apnea, can you order a sleep study?"
- ›"Could you submit the PA under the CVD or OSA indication instead of obesity?"
Your prescriber's experience with Medicaid will vary. Some won't know about the OSA pathway because Zepbound's sleep apnea indication is only about 18 months old. Sharing this information isn't pushy — it's helpful.
How do you find a Medicaid doctor who can prescribe GLP-1s?
Answer in two sentences
Your fastest paths are your existing primary care doctor (if in-network), a community health center / FQHC, or your Medicaid MCO's online provider directory filtered for endocrinology, cardiology, sleep medicine, or obesity medicine. Most national direct-to-consumer telehealth brands are not realistic options for Medicaid coverage.
The provider-type matrix
| Provider type | Likely accepts Medicaid? | Best for | How to find one |
|---|---|---|---|
| Your existing primary care doctor | Yes, if in your Medicaid network | Most people -- the cleanest first stop | Call member services on the back of your Medicaid card |
| Community health center / FQHC | Often yes, but verify the specific site | Readers without a current PCP; underserved areas | findahealthcenter.hrsa.gov, then call to confirm Medicaid plan and GLP-1 prescribing |
| ABOM-certified obesity medicine specialist | Sometimes -- varies by individual practice | Complex cases; PA expertise needed | abom.org diplomate search + call to confirm Medicaid |
| Endocrinologist | Often yes | Type 2 diabetes pathway | Medicaid MCO directory; Zocdoc with Medicaid filter |
| Cardiologist | Often yes | Wegovy CVD pathway | MCO directory; hospital cardiology referral |
| Sleep medicine specialist | Often yes | Zepbound OSA pathway (sleep study needed) | MCO directory; ask PCP for referral |
| Hepatologist or GI specialist | Often yes | MASH pathway | MCO directory; referral usually required |
| knownwell (covered states) | Yes, where Medicaid is accepted | Online care where available | knownwell.co -- verify state and plan at intake |
| Accomplish Health (NY Medicaid, SoonerCare) | Listed -- verify at intake | NY and OK Medicaid users | accomplish.health -- likely now routing through knownwell |
| Hospital-affiliated weight clinic | Often yes -- confirm the specific group | BMI 35+, comorbidities, specialist team | Hospital website + insurance verification call |
| Retail clinic (CVS MinuteClinic, etc.) | Varies; many accept Medicaid for visits but may not prescribe GLP-1s | Limited -- most refer out | Call the specific location |
| National direct-to-consumer telehealth | No -- cash-pay or commercial only | Only if you've decided to leave Medicaid | N/A for Medicaid |
Your 5-step plan for this week
Confirm your plan details.
Pull out your Medicaid card. Note the MCO name (if any). Call the member services number and ask for your formulary lookup tool and the prior authorization criteria for GLP-1 medications.
Try your existing PCP first.
If you have a doctor you already see, schedule a visit and bring the diagnosis pathway list from this page. Ask whether you qualify under any covered indication.
Find a specialist if your PCP can't help.
Use your MCO's online provider directory. Filter for endocrinology (diabetes pathway), cardiology (CVD pathway), sleep medicine (OSA pathway), hepatology (MASH pathway), or obesity medicine.
Try knownwell if you want telehealth.
If you're in a state where knownwell accepts your Medicaid plan, this is the cleanest online option we've verified. Check availability and your plan on their site before booking.
Try a community health center if you don't have a PCP.
Find your nearest Federally Qualified Health Center at findahealthcenter.hrsa.gov. These centers are expected to participate in Medicaid and serve uninsured patients on a sliding scale, but verify the specific site takes your Medicaid plan and prescribes GLP-1s.
What to bring to your appointment

Walking in prepared makes your prior authorization go faster:
- ›Your Medicaid card and MCO name
- ›A printout or screenshot of your plan's formulary for GLP-1s
- ›BMI history (current and historical -- most PAs want at least 6 months)
- ›A list of any qualifying diagnoses: type 2 diabetes (A1c lab values), heart disease, sleep apnea (sleep study results), MASH (liver imaging or biopsy), and supporting comorbidities like hypertension, high cholesterol, or prediabetes
- ›Documented weight-loss attempts: diets you've tried, exercise programs, any weight-loss medications you've taken
- ›Your current medication list
- ›Any previous denial letters
Under 21 on Medicaid? EPSDT gives you a separate federal pathway
Answer in two sentences
Federal Medicaid law (EPSDT — Early and Periodic Screening, Diagnostic, and Treatment) requires every state Medicaid program to evaluate medically necessary services for enrollees under 21 based on the child's individual needs. EPSDT does not guarantee automatic GLP-1 approval, but a Medicaid plan cannot rely solely on an adult obesity-drug exclusion when reviewing a request for a child or teen — it has to evaluate whether the medication is medically necessary for that specific patient.
This protection is real and it's older than the GLP-1 era. Most state Medicaid pages don't highlight it because the medication-level rules feel separate. They aren't.
What EPSDT actually does
When a child under 21 needs a medical service to correct or improve a condition, the state Medicaid plan has to evaluate medical necessity rather than apply an adult policy exclusion as a category bar. CMS guidance specifically lists prescribed drugs among services that can be covered under EPSDT when medically necessary, even when the state has otherwise opted out of coverage.
Pennsylvania real-world example
Pennsylvania Medicaid eliminated adult GLP-1 coverage for overweight and obesity on January 1, 2026. Pennsylvania DHS guidance explicitly states that for under-21 enrollees, the plan cannot deny solely because the medication is prescribed for obesity or overweight — it must evaluate EPSDT medical necessity. A 15-year-old with documented obesity has an EPSDT pathway. Their 22-year-old sibling, on the same Medicaid plan, does not.
What to put in the PA for an EPSDT request:
- ›Age and FDA-approved age indication for the medication (Wegovy and Saxenda are FDA-approved for adolescents 12 and older)
- ›BMI and BMI percentile for age
- ›Growth and weight history
- ›Documented comorbidities
- ›Prior treatment attempts (lifestyle counseling, dietitian, other interventions)
- ›Clinical rationale for why the requested medication is medically appropriate
- ›An explicit note that adult obesity-drug exclusion should not be applied categorically
Under 21 and denied?
If your child's PA was denied citing an adult exclusion, that's worth challenging through an EPSDT-specific appeal. Every state Medicaid program has an appeal process. Ask the plan specifically whether filing by the appeal deadline keeps current coverage active during review.
What should you do if you just lost coverage in California, NH, PA, or SC?
Answer in two sentences
California, New Hampshire, Pennsylvania (adults 21 and over), and South Carolina eliminated adult GLP-1 coverage for obesity on January 1, 2026, due to state budget pressures. Your immediate steps are checking your appeal deadline, exploring the diagnosis pathway with your doctor, and (if applicable) invoking EPSDT for under-21 enrollees.

The 5-day action plan if you got a denial letter
Read the denial letter for the appeal deadline.
State Medicaid appeal windows vary. Pennsylvania DHS uses a 15-day window in which appealing keeps existing coverage running during review. Other states use different deadlines and continuation rules. Do not assume your state matches Pennsylvania's window.
Request the reason in writing if it's not already specified.
Ask your plan: "Was this a category exclusion, a missing-documentation issue, a step-therapy requirement, or a non-preferred-drug issue?" The answers lead to different fixes.
Talk to your prescriber.
Ask whether you have a documented covered indication -- type 2 diabetes, established cardiovascular disease with overweight or obesity, moderate-to-severe sleep apnea with obesity, or MASH with moderate-to-advanced fibrosis. If yes, request a new PA under that indication.
File the appeal.
Most states have a member services phone number and an online appeal form. Submit before the deadline. Ask your plan specifically whether filing by that deadline keeps your current coverage active during review.
If you're under 21, request a separate EPSDT review.
State default denial decisions often apply adult policy and miss EPSDT. This is worth raising explicitly.
State-specific notes
- ›Pennsylvania: Adult overweight/obesity GLP-1 coverage ended January 1, 2026. Other medically accepted indications (diabetes, CVD, OSA, MASH) can still be covered with PA. Under-21 enrollees must be evaluated under EPSDT.
- ›California, New Hampshire, South Carolina: Adult coverage ended cleanly on January 1, 2026. EPSDT remains a federal floor for under-21 enrollees regardless of what the state announced.
- ›All four states: Coverage for non-obesity FDA-approved indications still works through the same federally required pathway as other states.
Can you use GLP-1 savings cards if you have Medicaid?
Answer in two sentences
Generally no. Manufacturer savings programs from Novo Nordisk (NovoCare for Wegovy and Saxenda) and Eli Lilly (LillyDirect for Zepbound) are designed for eligible commercially insured or cash-pay patients and commonly exclude Medicaid, Medicare, TRICARE, VA, and other government-funded insurance beneficiaries from their cash-pay savings pricing. This is a federal anti-kickback rule, not a marketing choice.
| Program | Medicaid eligible? |
|---|---|
| NovoCare Pharmacy (Wegovy injection, Wegovy oral, Saxenda direct-to-consumer pricing) | No -- Medicaid enrollees not eligible for the discounted pricing |
| LillyDirect / Lilly Self Pay (Zepbound vial and KwikPen pricing) | No -- Medicaid enrollees not eligible |
| TrumpRx (direct-to-consumer pricing on multiple manufacturer GLP-1s) | No -- Medicaid enrollees generally excluded |
| Drug-specific copay cards from Novo Nordisk and Lilly for Wegovy or Zepbound | No -- explicitly exclude government-insured patients |
Your pathway as a Medicaid enrollee is through your state's Medicaid pharmacy benefit, not through a manufacturer coupon or direct-to-consumer program.
Will the CMS BALANCE Model change Medicaid GLP-1 access in 2026 or 2027?
Answer in two sentences
The BALANCE Model is a voluntary CMS Innovation Center demonstration starting in May 2026 that lets state Medicaid programs opt in to negotiated lower GLP-1 prices. It doesn't change what Medicaid is required to cover federally — it gives participating states a cheaper way to add or restore obesity coverage if they choose to.
What BALANCE actually does
CMS negotiates lower wholesale prices for the major GLP-1s — including Mounjaro, Ozempic, Rybelsus, Wegovy, the KwikPen formulation of Zepbound, and Foundayo — for state Medicaid programs that opt in. Participating states commit to standardized clinical eligibility criteria and lifestyle support programs. The net price for state Medicaid programs is not public.
What BALANCE doesn't do (yet)
- !It does not require any state to participate. Participation is voluntary.
- !It does not change federally required coverage pathways for diabetes, CVD risk reduction, sleep apnea, or MASH indications.
- !It does not turn cash-pay telehealth brands into Medicaid providers.
- !It covers specified FDA-approved GLP-1 drugs and formulations -- not compounded GLP-1 products.
Timeline
| May 2026 | Medicaid component of BALANCE begins; state opt-in opens. |
| July 31, 2026 | Deadline for state Medicaid agencies to apply for the model. |
| July 1, 2026 – December 31, 2027 | Separate Medicare GLP-1 Bridge program runs (Medicare-only, $50 monthly copay for eligible Part D enrollees on Wegovy, Zepbound KwikPen, or Foundayo). |
| December 31, 2031 | BALANCE Model scheduled to end. |
What cash-pay GLP-1 options exist if Medicaid genuinely will not cover you?
Important boundary
This section is for readers who are no longer enrolled in Medicaid (you've aged out, your eligibility ended, you got commercial insurance, or you've genuinely worked through every pathway above). The providers featured below explicitly do not accept active Medicaid enrollees. None of them are a Medicaid workaround.
You're a candidate for the cash-pay path if all of the following are true:
- ✓You've verified your state Medicaid genuinely won't cover any GLP-1 for any indication you qualify for
- ✓EPSDT doesn't apply (you're 21 or over)
- ✓Your appeal pathway has been exhausted
- ✓You are no longer enrolled in Medicaid (or you've confirmed eligibility directly with the cash-pay provider before signing up)
- ✓You can sustain the monthly cost without putting other essentials at risk
Option 1: Ro Body — FDA-approved brand-name
Not for active Medicaid enrolleesIf you are no longer enrolled in Medicaid, Ro carries the broadest FDA-approved GLP-1 menu among the consumer telehealth brands we've reviewed. Current cash-pay medication options include the Wegovy pill, Foundayo pill, Zepbound KwikPen, Wegovy pen, and Ozempic. Ro also offers an insurance concierge that handles prior authorization paperwork (useful as you transition to commercial insurance), and a free GLP-1 Insurance Coverage Checker.
Pricing (verified May 2026)
- Ro Body membership: $39 first month; then $74/month with annual prepay or $149/month monthly
- Wegovy pill: from $149 first month, then $199–$299/month
- Foundayo pill: from $149 first month, then $199–$299/month
- Zepbound KwikPen: from $299 first month, then $399–$449/month
- Wegovy pen: from $199 first month, then $199–$399/month
Only for readers no longer enrolled in Medicaid. Medication requires clinician approval and a valid prescription.
Option 2: Sesame Care — FDA-approved, provider-choice model
Not for active Medicaid enrollees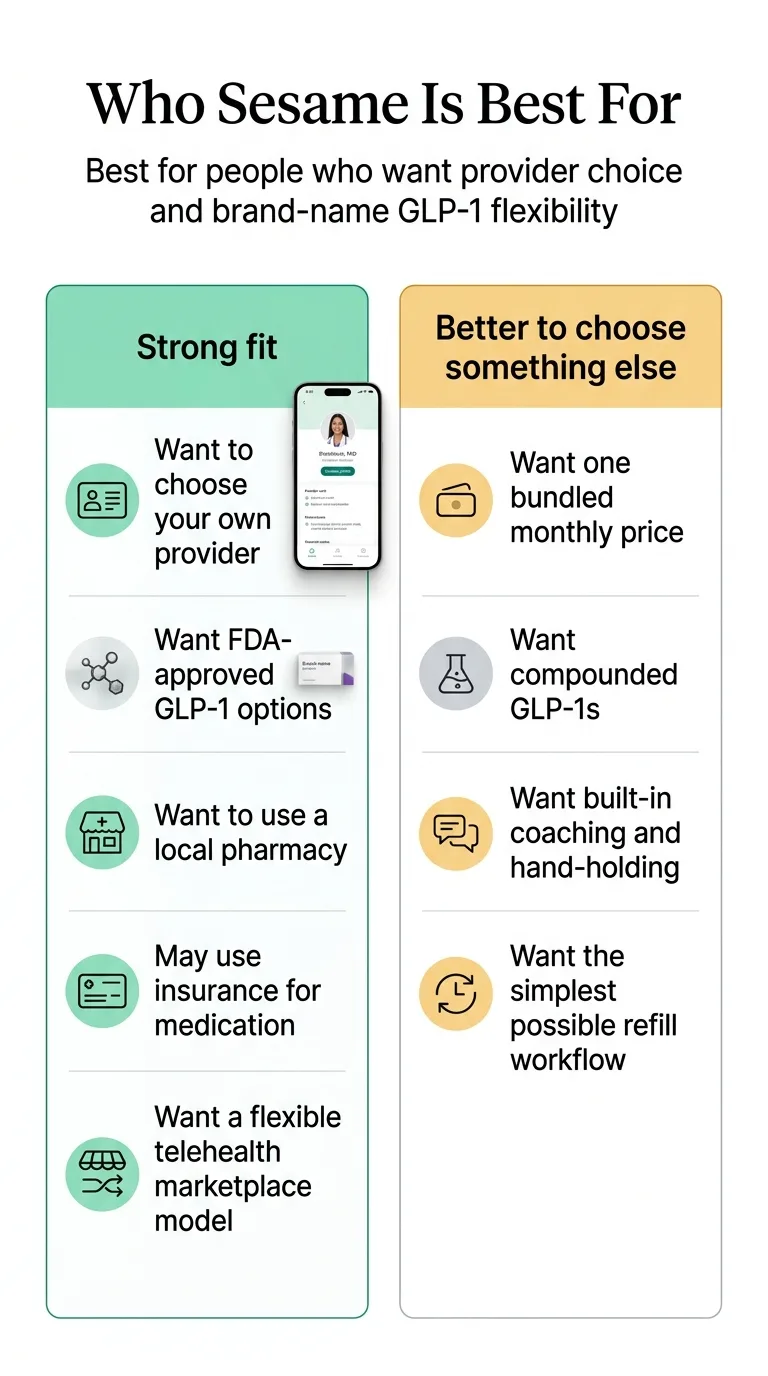
If you are no longer enrolled in Medicaid, Sesame offers a provider-choice model where you pick the clinician you want. Medication menu includes Wegovy pill, Wegovy pen, Zepbound KwikPen, Zepbound vial, Zepbound pen, Foundayo, Ozempic, and other GLP-1 options.
Pricing
Subscriptions from $59/month with an annual plan. Medication cost billed separately based on selection and pharmacy.
Use Sesame instead of Ro when: you want explicit provider choice, you specifically want the Zepbound vial or other formulations Ro doesn't carry, or your situation calls for a less subscription-heavy model.
Only for readers who understand Sesame does not accept Medicaid. Verify at checkout.
What about compounded GLP-1s?
- !Compounded GLP-1 medications are not FDA-approved finished products. They have not gone through FDA's premarket review for safety, effectiveness, or quality control.
- !Compounded medications are not generic equivalents of Wegovy, Zepbound, Ozempic, or Mounjaro. They are separate products.
- !As of FDA's April 2026 update, semaglutide and tirzepatide do not currently appear on the 503B bulks list or FDA's drug shortage list.
- !On April 30, 2026, FDA proposed to exclude semaglutide, tirzepatide, and liraglutide from the 503B bulks list.
- !The FDA issued a February 20, 2026 warning letter to MEDVi regarding false or misleading claims about its compounded semaglutide and tirzepatide products. We are not featuring MEDVi as a recommendation on this page.
- !Compounded GLP-1s are cash-pay. They are not billable to Medicaid in any state under the Medicaid Drug Rebate Program, which applies only to FDA-approved drugs.
If you've worked through everything else and want to compare compounded options as a cash-pay path, we maintain a separate compounded-specific comparison page with current pricing, regulatory disclosures, and provider-by-provider documentation.
Real patient experience signal
We don't fabricate testimonials. The two quotes below are published on knownwell's own site (knownwell.co) and are used to give you a sense of patient experience with the one consumer telehealth brand we've verified as a Medicaid-billing option. They are not RX Index first-party reviews and we don't apply review schema to them.
“I feel so grateful that I found knownwell. I have never had such a positive experience with medical professionals. I feel listened to and seen and like I am really cared for, not just another number.”
— Taylor S., knownwell patient (published on knownwell.co)
“Everyone is so friendly and you can tell they actively listen to you. I also like that they goal plan with you vs. just telling you what you're going to do.”
— Sofia F., knownwell patient (published on knownwell.co)
Frequently asked questions
Do any online GLP-1 providers accept Medicaid?
Yes, but very few. As of May 2026, the consumer telehealth brands we have verified that bill Medicaid for GLP-1 care are knownwell (which states it accepts Medicare and Medicaid in some states; MassHealth listed on its insurance page) and Accomplish Health (which lists New York Medicaid and SoonerCare, with intake likely now routed through knownwell). Most other major direct-to-consumer GLP-1 brands -- Hims, Hers, Ro, Sesame, Eden, MEDVi, SHED, Found, Lemonaid -- are cash-pay or commercial-insurance-only.
Does knownwell accept Medicaid?
knownwell states on its referral and insurance pages that it accepts Medicare and Medicaid in some states, with ABOM-certified obesity-medicine clinicians and an in-house prior authorization team that knownwell reports has an 80% success rate. Its insurance page lists Massachusetts/MassHealth options; its start page lists new patients in Massachusetts, New Hampshire, and Rhode Island. Verify your specific state and Medicaid plan availability at intake on knownwell.co before booking.
Does Accomplish Health accept Medicaid?
Accomplish Health's insurance page lists New York Medicaid and SoonerCare (Oklahoma Medicaid) as accepted plans. Public Accomplish communications indicate Accomplish has joined forces with knownwell, so verify at intake whether your application still routes through Accomplish or now through knownwell.
Does Ro accept Medicaid for GLP-1s?
No. Ro's insurance policy explicitly states that Medicaid (and other government-funded plan) members cannot join Ro Body or pay out of pocket through Ro. Ro is cash-pay or commercial-insurance only and is not a Medicaid workaround for currently enrolled Medicaid users.
Does Sesame Care accept Medicaid?
No. Sesame Care's terms of service state Sesame does not accept Medicare, Medicaid, or other third-party insurance for its services. Sesame is not a Medicaid-billing provider.
Does Hims or Hers accept Medicaid?
No. Hims support says it is unable to accept insurance for its programs. Both Hims and Hers operate cash-pay GLP-1 programs. Following the March 2026 Novo Nordisk partnership, both brands offer FDA-approved Wegovy pill, Wegovy pen, and Ozempic -- but neither accepts Medicaid as a payment method.
Does Medicaid cover Wegovy?
It depends on your state and your diagnosis. Wegovy injection has FDA-approved indications that create a Medicaid coverage pathway in every state for cardiovascular event risk reduction in adults with cardiovascular disease and overweight or obesity, and for MASH with moderate-to-advanced fibrosis. Coverage for Wegovy when prescribed for weight loss alone is optional for states -- 13 state Medicaid programs cover it as of January 2026.
Does Medicaid cover Zepbound?
It depends on your state and your diagnosis. Zepbound has an FDA-approved indication that creates a Medicaid coverage pathway in every state for moderate-to-severe obstructive sleep apnea in adults with obesity (FDA approval December 2024). Coverage for Zepbound when prescribed for obesity alone is optional for states.
Does Medicaid cover Ozempic for weight loss?
Almost never. Ozempic is FDA-approved for type 2 diabetes, not weight loss. Most state Medicaid programs cover Ozempic for the diabetes indication with prior authorization, but they generally do not cover it for off-label use in non-diabetic patients seeking weight loss.
Does Medicaid cover Mounjaro?
Mounjaro is FDA-approved for type 2 diabetes. Most state Medicaid programs cover Mounjaro for the diabetes indication with prior authorization, often as a nonpreferred drug requiring stricter PA criteria. Coverage for off-label weight loss in non-diabetic patients is generally not provided.
Does Medicaid cover Saxenda?
Coverage varies. Saxenda (liraglutide) is FDA-approved for chronic weight management in adults and adolescents 12 and older. Some state Medicaid programs with restricted GLP-1 obesity coverage still list Saxenda as preferred because it is the lowest-cost FDA-approved weight management injectable.
Does Medicaid cover compounded semaglutide?
No. Compounded semaglutide is not FDA-approved and is not covered by Medicaid pharmacy benefits in any state. The Medicaid Drug Rebate Program covers only FDA-approved drugs from participating manufacturers.
What states cover GLP-1 medications through Medicaid for obesity?
As of January 2026, 13 states cover GLP-1s for obesity under fee-for-service Medicaid: Delaware, Kansas, Massachusetts (restricted), Michigan (restricted to morbid obesity), Minnesota, Mississippi, Missouri, North Carolina (reinstated December 2025), Rhode Island, Tennessee, Utah, Virginia, and Wisconsin. California, New Hampshire, Pennsylvania (adults 21 and over), and South Carolina dropped coverage on January 1, 2026. Coverage for type 2 diabetes, cardiovascular risk reduction, sleep apnea, and MASH creates a coverage pathway in every state through Medicaid Drug Rebate Program rules, subject to formulary and prior authorization.
Can I get Wegovy or Zepbound on Medicaid if my state only covers diabetes GLP-1s?
Possibly, through a covered indication other than obesity. Wegovy injection has a federally recognized coverage pathway for cardiovascular event risk reduction in adults with established CVD and overweight or obesity, and for MASH with moderate-to-advanced fibrosis. Zepbound has a federally recognized pathway for moderate-to-severe obstructive sleep apnea in adults with obesity. If you have one of those documented diagnoses, your prescriber can submit a prior authorization under that indication.
Can my child on Medicaid get a GLP-1 for obesity?
EPSDT gives under-21 enrollees a separate federal medical-necessity pathway in every state. It does not guarantee automatic approval, but a Medicaid plan cannot deny solely because the medication is prescribed for obesity or overweight in an adult-policy context -- it has to evaluate whether the medication is medically necessary for the child or teen. Wegovy and Saxenda are FDA-approved for adolescents 12 and older.
What is a Medicaid MCO?
A Medicaid Managed Care Organization (MCO) is a private insurance company contracted by your state to manage your Medicaid benefits. Common Medicaid MCO names include Molina, Centene, Amerigroup, UnitedHealthcare Community Plan, and Aetna Better Health. About 78% of Medicaid enrollees nationally are in MCOs rather than direct fee-for-service Medicaid. Your MCO has its own formulary and prior authorization criteria that can differ from your state's fee-for-service preferred drug list.
Can I use a manufacturer savings card with Medicaid?
Generally no. Manufacturer savings programs from Novo Nordisk (NovoCare for Wegovy and Saxenda) and Eli Lilly (LillyDirect for Zepbound) explicitly exclude patients enrolled in Medicaid, Medicare, TRICARE, VA, and other government-funded insurance from their cash-pay savings pricing. Your pathway as a Medicaid enrollee is through your state's Medicaid pharmacy benefit, not these programs.
What documents do I need for prior authorization?
Most state Medicaid plans require a documented diagnosis, BMI history (often at least 6 months), evidence of qualifying comorbidities if applicable, documented prior weight-loss attempts, current medication list, and any relevant lab values (A1c for diabetes, recent blood pressure, sleep study results, liver imaging or biopsy for MASH). Your prescriber's office handles the actual submission, but bringing this information to your appointment speeds the process.
What if my Medicaid GLP-1 prior authorization is denied?
Read the denial letter for the reason -- was it a documentation issue, a non-preferred-drug requirement, a step-therapy requirement, or a category exclusion? Documentation issues can be fixed by resubmitting with additional records. Category exclusions require an appeal or a switch to a covered indication. Every state Medicaid program has an appeal process; deadlines vary by state. Ask your plan specifically whether filing by the appeal deadline keeps your current coverage active during review.
Will the BALANCE Model make GLP-1s available in every state?
No. BALANCE is voluntary for states. The model starts for Medicaid in May 2026 and gives participating state Medicaid programs access to lower negotiated GLP-1 prices from Novo Nordisk and Eli Lilly. State participation is optional and the full participating-state list is not yet public. BALANCE does not change federally required coverage pathways for diabetes, CVD, sleep apnea, or MASH indications.
Can I pay cash for a GLP-1 if I have Medicaid?
It depends on the provider, and the answer for the major cash-pay telehealth brands is mostly no. Ro explicitly excludes Medicaid enrollees from joining Ro Body or paying out of pocket through Ro. Manufacturer savings programs (NovoCare, LillyDirect, TrumpRx) exclude Medicaid enrollees from cash-pay pricing. If you remain enrolled in Medicaid, cash-pay through national telehealth brands is largely closed; the practical cash-pay options open up only when you are no longer enrolled in Medicaid.
What's the cheapest option if Medicaid won't cover it?
For readers no longer enrolled in Medicaid who want FDA-approved brand-name medication, Ro's listed cash-pay medication prices currently start at $149/month for the lower-dose Wegovy pill or Foundayo pill, $299/month for starting-dose Zepbound KwikPen, and higher amounts by medication and dose (with $39 first-month membership and $74-$149/month ongoing membership billed separately). Compounded medications are advertised at lower price points by some providers but are a separate regulatory category and not interchangeable with brand-name drugs.
Take the matching quiz to find your exact path
Still not sure which GLP-1 path fits your state, your diagnosis, your plan type, and your situation? We built a free 60-second matching quiz that asks 4 questions and gives you a personalized 3-step action plan — including whether your state covers your indication, which provider type to call first, and what to bring to your appointment.
Take the free 60-second Medicaid GLP-1 matching quiz
No account required. Email optional. We'll never share your information.
→ Find My Medicaid GLP-1 PathRelated guides on The RX Index
- State-by-State Medicaid GLP-1 Coverage Tracker (2026)
- GLP-1 Providers That Accept Medicare Advantage: 4 Paths [2026]
- Best GLP-1 Providers That Accept Insurance (2026)
- GLP-1 Providers That Accept CHAMPVA: 4 Coverage Paths (2026)
- GLP-1 Providers That Accept TRICARE (2026): Coverage Paths and PA Guide
- GLP-1 Providers That Accept Centene / Ambetter (2026)
How we verified this page (methodology)
Provider Medicaid billing
- ✓knownwell -- Verified May 13, 2026, via knownwell.co/referral, knownwell.co/start, and knownwell.co insurance pages. Medicare and Medicaid accepted in some states; MassHealth on insurance page; new patients in MA/NH/RI; 80% PA success rate stated.
- ✓Accomplish Health -- Verified via accomplish.health/insurance. Lists New York Medicaid and SoonerCare. Knownwell partnership noted in public communications.
- ✓Ro -- Verified via ro.co/weight-loss/insurance (Medicaid users excluded from Ro Body and out-of-pocket payment) and ro.co/weight-loss/pricing.
- ✓Sesame Care -- Verified via sesamecare.com/terms-of-service (no Medicare, Medicaid, or other third-party insurance for Sesame services).
- ✓MEDVi -- FDA warning letter dated February 20, 2026. Excluded from recommendations.
- ✓All other major brands -- Verified May 1-13, 2026, via each brand's own terms, insurance, or FAQ pages.
State Medicaid coverage
- ✓KFF 'Medicaid Coverage of and Spending on GLP-1s' (January 2026 brief) and 'What to Know About the BALANCE Model' (May 2026 update)
- ✓Stateline (April 2026 reporting)
- ✓Pennsylvania DHS Medical Assistance Bulletin (November 2025)
- ✓State Medicaid PDLs and agency announcements
Federal policy and FDA indications
- ✓Medicaid Drug Rebate Program: 42 U.S.C. § 1396r-8
- ✓Wegovy CVD indication: FDA press announcement, March 2024
- ✓Zepbound OSA indication: FDA press announcement, December 2024
- ✓Wegovy MASH indication: FDA news release, August 2025
- ✓EPSDT protections: 42 U.S.C. § 1396d(r); Medicaid.gov EPSDT guidance; PHLP guidance
- ✓BALANCE Model: CMS Innovation Center; KFF May 2026 analysis
- ✓FDA April 2026 compounded GLP-1 policy and April 30, 2026 503B bulks list proposal
Author: The RX Index Editorial Team · Last verified: May 13, 2026 · Next scheduled update: June 2026
What changed in this update (May 13, 2026): Added Accomplish Health verification (NY Medicaid and SoonerCare; knownwell partnership noted). Added Wegovy MASH indication detail (FDA accelerated approval, August 2025). Updated Ro section to reflect that active Medicaid enrollees cannot join Ro Body or pay cash through Ro. Added Sesame service-vs-medication insurance distinction. Added FDA April 2026 compounded GLP-1 policy update and April 30, 2026 503B bulks list proposal. Tightened EPSDT framing to match CMS and PHLP medical-necessity language. Added BALANCE Model state participation note. Added manufacturer savings-card section.
Last verified: May 13, 2026. The RX Index Editorial Team. This page is on a monthly verification cycle and is updated within 30 days of any announced CMS, FDA, or major state Medicaid policy change.
This page is editorial guidance compiled from primary sources (FDA, CMS, KFF, state Medicaid bulletins, and individual provider terms) and does not constitute medical advice or insurance counseling. Verify your specific situation directly with your state Medicaid agency, your MCO, or a licensed healthcare provider before making medical or financial decisions. Methodology · Editorial Standards
