GLP-1 Providers That Accept Medicare Advantage in 2026 (Verified List + Bridge Program Path)
Published: · Last reviewed:
By The RX Index Editorial Team · Last verified May 13, 2026
If you have Medicare Advantage and you're hunting for GLP-1 providers that accept Medicare Advantage, here's the truth most pages won't lead with. The best provider for most readers is not the telehealth ad you saw on social media — it's an in-network Medicare Advantage doctor. The handful of telehealth platforms that genuinely work with Medicare are worth knowing, and that's what this page is for.
Find my Medicare Advantage GLP-1 path — free 60-second quiz
Six questions about your plan, diagnosis, and goal. Get your route, your provider shortlist, and a printable doctor visit script — no email required.
→ Find My Medicare Advantage GLP-1 PathThe fastest answer: best GLP-1 path by your situation
This table is the verdict. The rest of the page is why, how, and what to do next.
| If this is you… | Best first move | What to verify yourself |
|---|---|---|
| Want GLP-1 for weight loss only; your BMI and conditions may meet Bridge criteria | In-network MA prescriber + Medicare GLP-1 Bridge prior authorization (starts July 1, 2026) | Your exact plan type and BMI/qualifying conditions against CMS Bridge eligibility criteria |
| Have type 2 diabetes | Your PCP or endocrinologist + your MA-PD plan's Part D benefit | Whether your specific GLP-1 (Ozempic, Mounjaro, Rybelsus) is on your plan's Drug List and what PA documents are required |
| Have heart disease + obesity or overweight | Your cardiologist or PCP + Wegovy through Part D | Whether Wegovy is on your plan's formulary for the cardiovascular indication |
| Have moderate-to-severe sleep apnea + obesity | Your sleep-medicine doctor or PCP + Zepbound through Part D | Whether Zepbound (covered formulation) is on your plan's formulary for OSA |
| Want a virtual obesity clinic that may bill your MA plan | Verify Form Health, knownwell, Shapely, or One Medical Seniors against your exact plan first | Each provider's current network status for your specific Medicare Advantage plan and your ZIP code |
| Your plan denied the medication | Use the denial decoder below before paying cash | The exact denial reason on your notice and your redetermination deadline |
| Can't get coverage and just want to start | Cash-pay FDA-approved through Ro, Sesame, NovoCare, LillyDirect, or TrumpRx | Live cash price, what's included in any membership, and Medicare eligibility rules at checkout |
One thing to flag right up front.
Most online programs that say “we accept insurance” do not actually bill Medicare Advantage for the medical visit, do not coordinate government-plan drug coverage, and have not publicly shown they'll submit Medicare GLP-1 Bridge prior authorizations to Humana once the program opens. That's not cynicism — it's just how these companies are built. If we lump them in with the four real options, we're wasting your time and your money.
The three questions hiding inside “accepts Medicare Advantage”
Answer capsule
“Accepts Medicare Advantage” actually means three different things: (1) can the provider bill your Medicare Advantage medical benefit for the visit, (2) will they write the prescription for an FDA-approved GLP-1, and (3) will your MA-PD pharmacy benefit, the Medicare GLP-1 Bridge, or an appeal actually pay for the medication. A provider can pass test #2 and fail tests #1 and #3 — that's most cash-pay telehealth GLP-1 platforms.
Most pages today blur all three. That's how readers end up paying a $149/month membership and finding out the membership doesn't include the medication, the medication isn't on their plan's formulary, and the program can't submit a prior authorization to their MA-PD plan's processor.
Which GLP-1 providers accept Medicare Advantage in 2026?
Answer capsule
Four telehealth or hybrid clinics have the strongest Medicare and Medicare Advantage signals: Form Health (national, says it's covered by major insurance and Medicare), knownwell (no membership fee, accepts Medicare and most major commercial plans), Shapely (in-network with Medicare and most MA PPO plans in CA, FL, NY, and TX), and One Medical Seniors(Medicare-participating + select MA plans). Most other platforms are cash-pay only.
The Medicare Advantage GLP-1 Provider Matrix
Last verified May 13, 2026. Source links are inline.
| Provider | What they say about Medicare | Visit billing | Plan PA help today | Bridge PA readiness (publicly verified) | Cash-pay backstop |
|---|---|---|---|---|---|
| Your in-network PCP / obesity medicine / endocrinology / cardiology / sleep medicine | Bills Medicare directly | Standard MA medical billing | ✅ Yes — submits PA through your plan | Best practical starting path; ask whether the office will submit the Bridge PA to Humana | You can still self-pay separately for cash-pay channels |
| Form Health | Says it's 'covered by national health insurance plans, including Medicare,' with PA support for FDA-approved meds. | Insurance-billed when in network | ✅ Yes — Care Team submits PA | [Needs verification after Humana Bridge PA process is live] | $299/mo self-pay covers visits, dietitian, messaging (labs and meds extra) |
| knownwell | Says obesity care is covered by Aetna, Cigna, BCBS, United, and Medicare with no membership fee. Medicare patients may need to fill through NovoCare or LillyDirect to receive manufacturer discounts. | Insurance-billed when in network; no recurring membership | ✅ Yes — insurance advocacy team | [Needs verification after Humana Bridge PA process is live] | $299 first visit / $149 per follow-up self-pay |
| Shapely | Says it's in-network with Medicare and most Medicare Advantage PPO plans; currently CA, FL, NY, TX. | Insurance-billed when in network; $49/mo membership + copays | ✅ Yes | [Needs verification after Humana Bridge PA process is live] | Membership + medication cost; medication not included |
| One Medical Seniors / Amazon One Medical | Says it's Medicare-participating and accepts Original Medicare and select MA plans (by location). Insurance can be used for medications prescribed through One Medical services. | Insurance-billed when in network | ✅ Yes — integrated with primary care | [Needs verification after Humana Bridge PA process is live] | Plan/pharmacy-dependent; copays/deductibles apply |
| WeightWatchers Clinic | Care team works with insurance; cost estimator includes a Medicare-related bucket. Exact MA visit billing not universally confirmed. | Subscription + insurance navigation | ⚠️ Commercial-focused; MA-specific support unclear | [Needs verification] | $25 first month then $74/mo on annual plan; medication separate |
| LifeMD | Accepts Medicare for select services; weight-management membership generally not insurance-covered. | Mixed — depends on service | ⚠️ Limited for MA | [Needs verification] | From $75/mo, medication separate |
| PlushCare | No longer accepts Medicare Part B as of Jan 1, 2026; may accept some Medicare Part C / MA plans at booking. | Subscription + insurance | ⚠️ Plan-dependent | [Needs verification] | $99/mo membership |
| Sesame | Says it does not bill health insurance for the program; medication can still be filled through your plan or a manufacturer pharmacy for covered indications. | Cash-pay subscription | ⚠️ Provider may assist with medication PA; Sesame does not bill insurance | [Needs verification] | Subscriptions from $59/mo on annual plan |
| Ro | Says it cannot coordinate GLP-1 coverage for government insurance plans; Medicare users may join and pay out of pocket for cash-pay medication options. | Cash-pay membership | ❌ Not for government plans | [Needs verification] | $39 first month, then as low as $74/month with annual plan; medication separate |
| Hims / Hers | Cash-pay GLP-1 program | Subscription + cash-pay medication | ❌ Not for government plans | [Needs verification] | Plan-based pricing |
| Compounded telehealth providers (MEDVi, Eden, SHED, Trim Rx, SkinnyRx) | Not a Medicare Advantage-billed path | Cash-pay subscription | ❌ Not Medicare-covered | Not Bridge-eligible — Bridge covers only FDA-approved Wegovy, Zepbound KwikPen, and Foundayo | Cash-pay is the model |
What this table is telling you:
- › A real “accepts Medicare Advantage” answer requires a clear public statement plus your exact plan in their network.
- › The Bridge PA readiness column is honest: as of May 2026, no specific telehealth provider has publicly shown its Bridge PA workflow with Humana.
- › Compounded providers are not a Medicare-covered path and are not eligible for the Bridge program.
Does Medicare Advantage cover GLP-1 medications for weight loss in 2026?
Answer capsule
Standard Medicare Advantage with prescription drug coverage (MA-PD) does not cover GLP-1 medications when used only for weight loss — that's the law for now. It does cover them for FDA-approved non-weight-loss uses. For weight-loss-only use, your real path is the Medicare GLP-1 Bridge, which launches July 1, 2026 and covers Wegovy, Zepbound KwikPen, and Foundayo at $50/month for eligible enrollees.
What your MA-PD plan can cover today
| Drug | May be covered for… | Typical MA-PD treatment |
|---|---|---|
| Ozempic (semaglutide injection) | Type 2 diabetes | May be on the plan formulary; tier, prior authorization, step therapy, and quantity limits vary by plan |
| Mounjaro (tirzepatide injection) | Type 2 diabetes | May be covered if it's on your plan's Drug List and you meet plan criteria; not covered for weight loss alone |
| Rybelsus (semaglutide oral tablet) | Type 2 diabetes | May be on the plan formulary with prior authorization |
| Trulicity, Victoza | Type 2 diabetes | May be on the plan formulary with prior authorization |
| Wegovy (semaglutide) | Cardiovascular risk reduction in adults with established heart disease plus obesity or overweight; MASH liver disease where plan criteria are met | Coverage possible only under the non-weight-loss indication; not for weight loss alone |
| Zepbound (tirzepatide) | Moderate-to-severe OSA in adults with obesity | Coverage possible only under the OSA indication; not for weight loss alone |
| Foundayo (orforglipron oral tablet) | FDA-approved for weight management | Not covered through standard MA-PD Part D; available through the Bridge starting July 1, 2026 |
| Compounded semaglutide or tirzepatide | Not FDA-approved | Not Medicare-covered; not Bridge-eligible |
About compounded GLP-1s:
Compounded drugs are not FDA-approved, and the FDA does not review them for safety, effectiveness, or quality before they're sold. For Medicare Advantage members, this matters because compounded GLP-1s are not a route to insurance coverage, are not eligible for the Bridge program, and switching from compounded to Bridge-eligible brand-name later means starting paperwork from scratch. Source — FDA
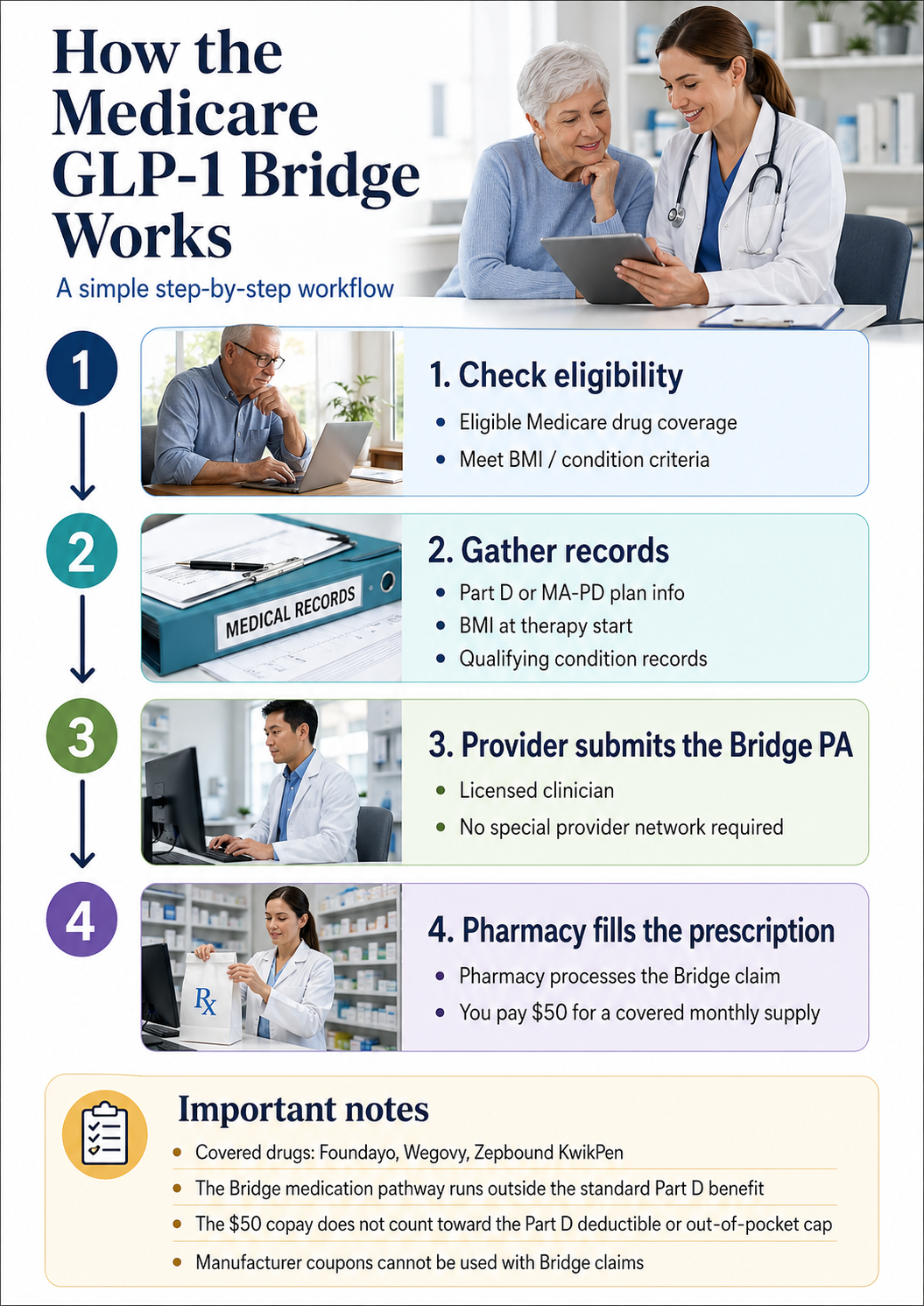
How the $50 Medicare GLP-1 Bridge actually works
Answer capsule
The Medicare GLP-1 Bridge is a CMS demonstration program that gives eligible Medicare Part D and MA-PD beneficiaries access to Wegovy, Zepbound KwikPen, or Foundayo for $50 per month from July 1, 2026 through December 31, 2027. It runs separately from your Part D plan, uses Humana as the central processor, and requires your prescriber to submit specific clinical documentation. The $50 copay does not count toward your Part D out-of-pocket maximum.
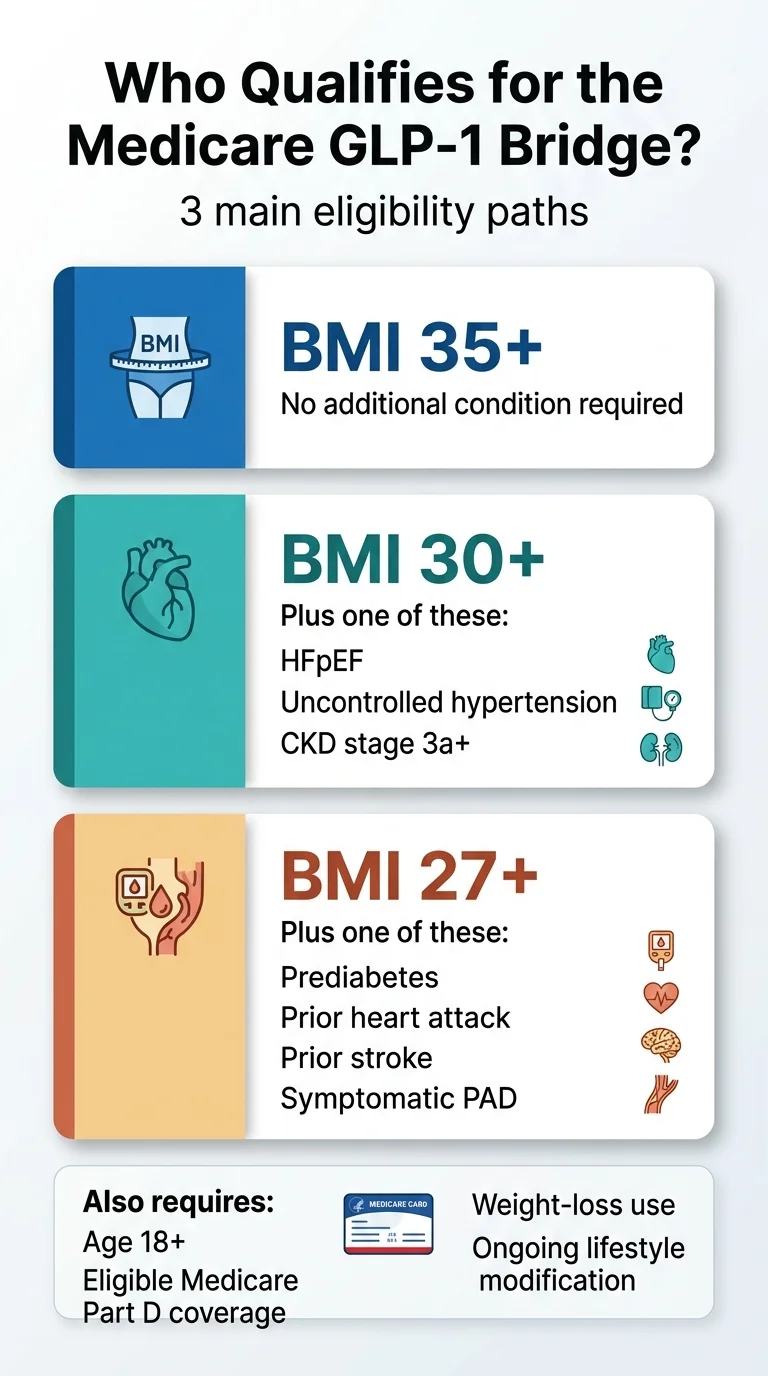
Who qualifies: the three clinical pathways
You must be 18 or older, prescribed for weight reduction and ongoing maintenance with lifestyle changes, and meet one of these:
Which plan types qualify
Eligible plan types
- ✓Standalone Medicare Part D plans (PDP)
- ✓Medicare Advantage with prescription drug coverage (MA-PD) — HMO, HMOPOS, Local PPO, Regional PPO
- ✓Special Needs Plans (SNPs)
- ✓Employer/union group waiver plans that offer Part D (EGWPs)
- ✓LI NET (Limited Income Newly Eligible Transition)
Not eligible (unless also enrolled in a standalone PDP)
- ✗Private fee-for-service plans
- ✗PACE programs
- ✗Cost contract plans (Sections 1876 and 1833)
- ✗Fallback plans
- ✗Religious fraternal benefit plans
Which drugs are covered by the Bridge

Foundayo
All formulations
Wegovy
All formulations (injection and tablets)
Zepbound KwikPen only
Single-dose vials and single-dose pens are NOT in the Bridge
The mechanics most articles skip
| Central processor | Humana — not your Part D plan |
| How PA is submitted | Your prescriber submits a prior authorization directly to Humana |
| BIN / PCN | BIN 028918 / PCN MEDDGLP1BR (Source: CMS) |
| Primary payer | The Bridge is the primary payer — it does not coordinate with your Part D benefit |
| $50 copay treatment | Does NOT count toward your Part D deductible or your $2,100 out-of-pocket cap (rising to $2,400 in 2027) |
| Manufacturer coupons | Cannot be applied to Bridge claims |
| Low-Income Subsidy (Extra Help) | Does not apply to the Bridge — you pay $50 either way |
| Prescriber requirement | Your prescriber does NOT need to be Medicare-enrolled — they just must not be on the CMS Preclusion List |

What the Bridge means for your provider choice
Even cash-pay telehealth platforms could theoretically have their prescribers submit a Bridge PA to Humana once the program goes live, because CMS doesn't require the prescriber to be Medicare-enrolled. The Bridge doesn't care who your prescriber is — it cares whether your clinical paperwork is right.
That said, the providers most likely to actually do this well on day one are the ones already running insurance-billed obesity care: Form Health, knownwell, Shapely, your endocrinologist, your obesity-medicine specialist. They live in this paperwork. As of May 2026, no specific cash-pay telehealth platform has publicly committed to a Humana Bridge PA workflow.
Check your Bridge eligibility — free 60-second quiz
Three questions: plan type, BMI and conditions, and your goal. Get a personalized eligibility readout and exactly what to bring to your doctor.
→ Check My Bridge Eligibility
Sources: CMS Medicare GLP-1 Bridge page (page last modified May 12, 2026); KFF BALANCE Model brief (updated May 11, 2026).
Which path fits your indication?
Answer capsule
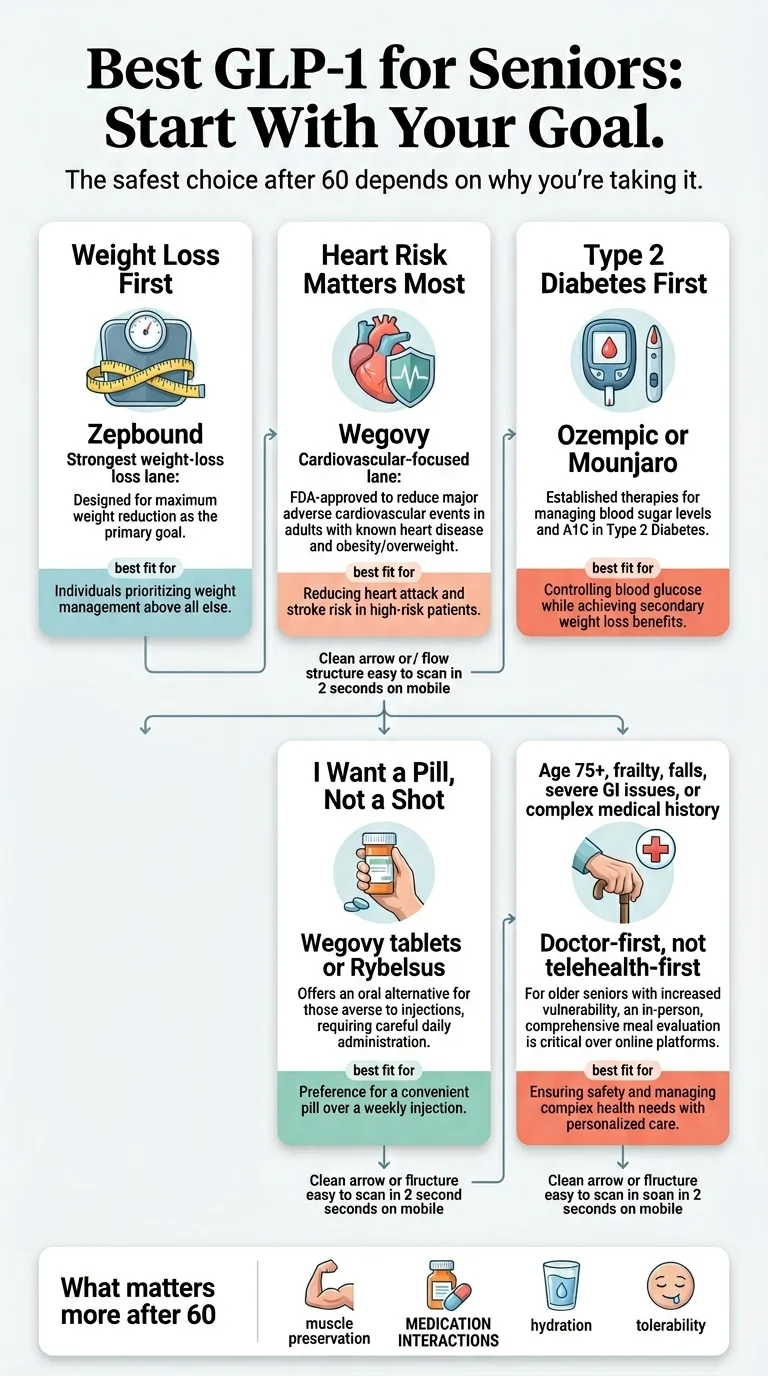
Your indication — the reason you're taking a GLP-1 — decides which Medicare path you use. Type 2 diabetes routes through regular MA-PD. Cardiovascular risk + obesity may unlock Wegovy. Sleep apnea + obesity may unlock Zepbound. Weight loss alone routes through the Bridge (July 1, 2026 onward) or cash-pay until then.
| Start with | Your endocrinologist or your PCP |
| Drugs that may be covered | Ozempic, Mounjaro, Rybelsus, Trulicity, Victoza |
| Expect | Prior authorization documenting your A1C, your current medications, and what you've tried before. Some plans require step therapy first. |
| Telehealth fit | Form Health, knownwell, or any in-network virtual diabetes clinic. Almost any MA-billed clinician can prescribe. |
| Start with | Your cardiologist or your PCP |
| Drug to ask about | Wegovy (under the FDA-approved cardiovascular-risk indication for adults with established cardiovascular disease) |
| Expect | Prior authorization documenting your cardiac history (prior MI, prior stroke, established cardiovascular disease) and your BMI |
| Telehealth fit | Form Health and knownwell both handle this; your in-network cardiologist is usually faster |
| Start with | Your sleep doctor or your PCP |
| Drug to ask about | Zepbound (under the FDA-approved obstructive sleep apnea indication for adults with obesity) |
| Expect | Prior authorization documenting your sleep study results (AHI score), your BMI, and your CPAP history |
| Telehealth fit | Most virtual obesity clinics won't have a sleep doctor on staff. Get the OSA documentation from your sleep clinic first, then any in-network prescriber can submit the PA. |
| Coverage status | Your MA-PD plan will not cover GLP-1s for weight loss alone right now |
| Your real options | Wait for the Bridge (most cost-effective). Cash-pay through NovoCare, LillyDirect, or TrumpRx at manufacturer pricing. Cash-pay through Ro or Sesame for clinical support. |
| Avoid | Compounded GLP-1 platforms. They're cheaper, but they're not FDA-approved and they don't position you for Bridge coverage when it opens. |
| First step | Check your Bridge eligibility against the three pathways above |
| PA submission | Have any prescriber who agrees to handle Bridge paperwork submit the Bridge PA to Humana. The prescriber must not be on the CMS Preclusion List. |
| Your medication | Wegovy, Zepbound KwikPen, or Foundayo at $50/month |
Can online GLP-1 doctors prescribe medication if you have Medicare Advantage?
Answer capsule
Yes — an online clinician can prescribe an FDA-approved GLP-1 if it's clinically appropriate. But that does not mean your Medicare Advantage plan will pay for the visit or the medication. For Medicare Advantage members, the real test is whether the provider can bill your plan, support prior authorization, and route the prescription through Part D or the Bridge.
When online care makes sense
- ✓Your specific plan accepts the online provider (Form Health and knownwell are the most likely to verify in)
- ✓You need an obesity-medicine specialist and there's no good local option
- ✓Your PCP is fine, but the wait is months long
- ✓The provider can handle your documentation and PA
When online care is the wrong first move
- ✗Your HMO requires a PCP referral and you're trying to skip it
- ✗You want a Bridge PA submitted and the provider hasn't publicly confirmed they'll do that workflow
- ✗The program is cash-pay only and your real goal is plan-covered care
- ✗The membership fee is non-refundable and you haven't verified your plan first
The four telehealth providers worth verifying first
Answer capsule
If you want a virtual or hybrid GLP-1 program that may work with Medicare Advantage, four are worth your time to verify: Form Health, knownwell, Shapely (CA/FL/NY/TX only), and One Medical Seniors. Each fits a different reader. None is the right answer for every Medicare Advantage member.
Form Health
Best virtual obesity-medicine clinicWho it's for: You have MA-PD, BMI 30+ (or 27+ with comorbidities), and you want a clinical team that specializes in obesity. You're willing to coordinate with your PCP and you're OK with a structured program over a fast prescription.
What they say about insurance: Form Health publicly states it's covered by national health insurance plans including Medicare, with Care Team visits, labs, and medications billed through insurance. You pay your copay or deductible like any in-network visit. Medication costs depend on your plan; Form's team reviews coverage and supports prior authorizations. (Source)
Pricing: Insurance copays apply, or $299/month self-pay covering visits, dietitian, and messaging (does not include labs or medication).
The honest tradeoff: Form Health requires a recent PCP visit (within 12 months) as part of enrollment. If you haven't seen your PCP in over a year, add a few weeks. If speed matters most, knownwell or your own PCP will move faster. If clinical depth matters most, Form is the strongest choice.
knownwell
Best no-membership-fee optionWho it's for: You want pay-per-visit billing instead of a subscription. You don't want a recurring membership. You're fine routing your medication through a manufacturer pharmacy when that gets you the discount.
What they say about insurance: knownwell's pricing page states obesity care is covered by Aetna, Cigna, BCBS, United, and Medicare with no membership fee. Medicare or government-insurance patients may need to fill through certain pharmacies, such as NovoCare or LillyDirect, to receive manufacturer discounts. (Source)
Pricing: Insurance copays apply, or $299 first visit / $149 per follow-up self-pay. No recurring membership fee.
The honest tradeoff: knownwell does not dispense medications and is not a pharmacy. They write the prescription — you get the medication through your MA-PD plan's pharmacy network or a manufacturer pharmacy. That's one more step than Form Health's more integrated model, but it saves you a monthly membership fee.
Shapely
Best for MA PPO members in CA, FL, NY, TXWho it's for: You live in California, Florida, New York, or Texas. You have Original Medicare or a Medicare Advantage PPO. You want a focused weight-management practice that publicly advertises Medicare and MA acceptance.
What they say about insurance: Shapely says it's in-network with Medicare and most Medicare Advantage PPO plans. (Source)
Pricing: $49/month membership + your normal Medicare copays and deductibles. Medication is not included.
The honest tradeoff: Shapely is state-limited. If you're outside CA/FL/NY/TX, this isn't your provider. For Medicare members, only the FDA-approved path connects to your insurance or to the Bridge.
One Medical Seniors / Amazon One Medical
Best primary-care continuityWho it's for: You want your GLP-1 care integrated with your primary care, not a standalone weight-loss program. You want one doctor's office handling your blood pressure, your cholesterol, and your GLP-1 together.
What they say about insurance: One Medical says it's a Medicare-participating provider and accepts Original Medicare plus select Medicare Advantage plans. Plan acceptance varies by location — you have to check your specific plan in your specific city. (Source)
Pricing: Standard Medicare copays apply when billed through insurance.
The honest tradeoff: Plan acceptance is local. One Medical works for your neighbor and not for you depending on which MA plan you have and where you live. Always verify your exact plan at your exact address before booking.
What to ask before you pay any GLP-1 program a single dollar
Answer capsule
Before paying any membership fee or subscription, ask the provider these ten questions in writing or by chat. If they can't answer #1, #2, and #6 with a clear yes for your specific Medicare Advantage plan, choose a different provider.
10 questions to ask any GLP-1 program before paying:
- 1
Do you accept my exact Medicare Advantage plan name and policy, not just the carrier brand?
("Yes, we take Humana" is not the same as "Yes, we take Humana Gold Plus HMO H1036-188.")
- 2
Are you in-network for my plan type — HMO, HMOPOS, Local PPO, Regional PPO, or SNP?
- 3
Will my medical visit be billed to my MA plan, or am I paying a cash-pay membership for the visit?
- 4
Is the medication included in your monthly fee, or is it a separate cost? Where does it get filled?
- 5
Do you prescribe only FDA-approved GLP-1s, or do you also prescribe compounded? (For Medicare coverage purposes, only FDA-approved matters.)
- 6
Will your team submit a prior authorization on my behalf to my MA-PD plan?
- 7
Will your team submit a Medicare GLP-1 Bridge prior authorization to Humana once the program is live (July 1, 2026)?
- 8
Will you document my BMI and qualifying conditions in the format CMS or my plan wants?
- 9
What happens if my plan denies the medication? Do you help with the appeal?
- 10
What's your cancellation policy if my plan won't cover the medication and I want to stop?
If you get hedging answers on #1, #2, or #6, this isn't your provider.
What to do if your MA-PD plan denies your GLP-1
Answer capsule
A denial from your Medicare Advantage plan is not the end of the road. Most denials use the same handful of phrases — match yours to the table below.
The denial decoder
| What the denial letter says | What it actually means | Your next move |
|---|---|---|
| “Drug not covered when used for weight loss” | Standard Part D weight-loss exclusion | Check Bridge eligibility (July 1, 2026) OR ask if you qualify under a non-weight-loss FDA indication (CV risk, OSA, MASH) |
| “Prior authorization required” | Your prescriber didn't submit PA, or PA was incomplete | Ask your prescriber to submit a complete PA with BMI, comorbidities, and prior weight-loss attempts |
| “Drug not on formulary” | Your plan doesn't list this specific drug | Ask for a formulary exception with medical necessity, or switch to a covered alternative on your plan's list |
| “Step therapy required” | Plan wants you to try a cheaper option first | Ask prescriber to submit a step-therapy exception if the cheaper option is medically inappropriate |
| “Wrong formulation” | The Bridge covers only Zepbound KwikPen, not single-dose vials/pens | Ask your prescriber to write the prescription for the KwikPen specifically |
| “Bridge PA sent to wrong processor” | PA went to your Part D plan instead of Humana | Ask your prescriber to resubmit through the CMS central processor (Humana) under BIN 028918 / PCN MEDDGLP1BR |
| “Coverage gap / non-covered service” | Could be a billing-code issue | Ask the plan to clarify the specific denial code and whether a different code applies |
| “Out-of-network provider” | Visit problem, not drug problem | Use an in-network prescriber or request a network exception |
Your appeal levels for Part D / MA-PD drug denials
Redetermination
Ask your plan for a redetermination within 65 days from the date of the coverage determination notice. Include a Letter of Medical Necessity from your prescriber.
Source: Medicare.gov 'Medicare Appeals' publication
Reconsideration by the Independent Review Entity (IRE)
Automatic next step if redetermination fails.
Administrative Law Judge (OMHA) hearing
For 2026, the amount remaining in controversy must be $200 or more.
Source: CMS OMHA third-level appeal
Match my denial to the right next step
Pick the phrase that matches your denial letter. We'll give you the exact next call, the form to file, and the question to ask your prescriber.
→ Find My Denial FixWhen cash-pay actually makes sense — and where Ro or Sesame fit
Answer capsule
Cash-pay GLP-1 makes sense for Medicare Advantage members in three situations: you don't qualify for the Bridge, you don't want to wait until July 1, 2026, or your plan keeps denying and you're done fighting. The main cash-pay options are manufacturer-direct (NovoCare Pharmacy, LillyDirect, TrumpRx) and clinical-support telehealth (Ro, Sesame). Neither Ro nor Sesame bills your Medicare Advantage plan for visits. Both are honest about that.
Cash-pay comparison
| Path | Visit/support included? | Medication options | Starting cash price | Medicare-eligible? |
|---|---|---|---|---|
| NovoCare Pharmacy | No — direct from manufacturer | Wegovy (injection and pill), Ozempic | Manufacturer-set; verify at checkout | Direct-pay channel; verify current Medicare eligibility rules at NovoCare |
| LillyDirect | No — direct from manufacturer | Zepbound (multiple formulations) | Manufacturer-set; verify at checkout | Direct-pay channel; verify current Medicare eligibility rules at LillyDirect |
| TrumpRx | No — federal direct-to-consumer portal | Brand-name GLP-1s at MFN-negotiated prices | Varies by drug; verify at checkout | Direct-pay channel; verify current rules |
| Ro Body | Yes — telehealth clinical team and dose management | Wegovy pill, Foundayo pill, Zepbound KwikPen, Wegovy pen, Ozempic | $39 first month, then as low as $74/month with annual plan paid upfront, or $149/month month-to-month; medication billed separately | Medicare users may join and pay out of pocket; Ro does not coordinate government insurance for GLP-1 coverage |
| Sesame | Yes — subscription with provider choice | Wegovy pill, Zepbound KwikPen, Wegovy pen, Foundayo, Zepbound vial, Zepbound pen, Ozempic | Subscriptions starting at $59/month on an annual plan; medication separate; Sesame says providers set their own prices | Sesame does not bill health insurance for the program; medication may still fill through your plan or a manufacturer pharmacy for covered indications |
Ro Body — for the cash-pay path with clinical support
Cash-pay only, no Medicare billingWho it's for: You want FDA-approved brand-name medication with a real clinical team and dose-management support, you're OK paying out of pocket, and you want a coverage report you can use later.
Pricing
$39 for the first month, then as low as $74/month with the annual plan paid upfront, or $149/month month-to-month. Medication is billed separately.
Medications: FDA-approved Wegovy pill, Foundayo pill, Zepbound KwikPen, Wegovy pen, and Ozempic. Ro states its FDA-approved cash-pay GLP-1 prices are the same as LillyDirect, NovoCare, and TrumpRx.
Ro cannot coordinate GLP-1 coverage for government insurance plans including Medicare.
Medication requires clinician approval and a valid prescription. Ro does not coordinate government insurance coverage.
Sesame — for Medicare members with a covered indication who want lower visit costs
Cash-pay visits; medication may fill through your plan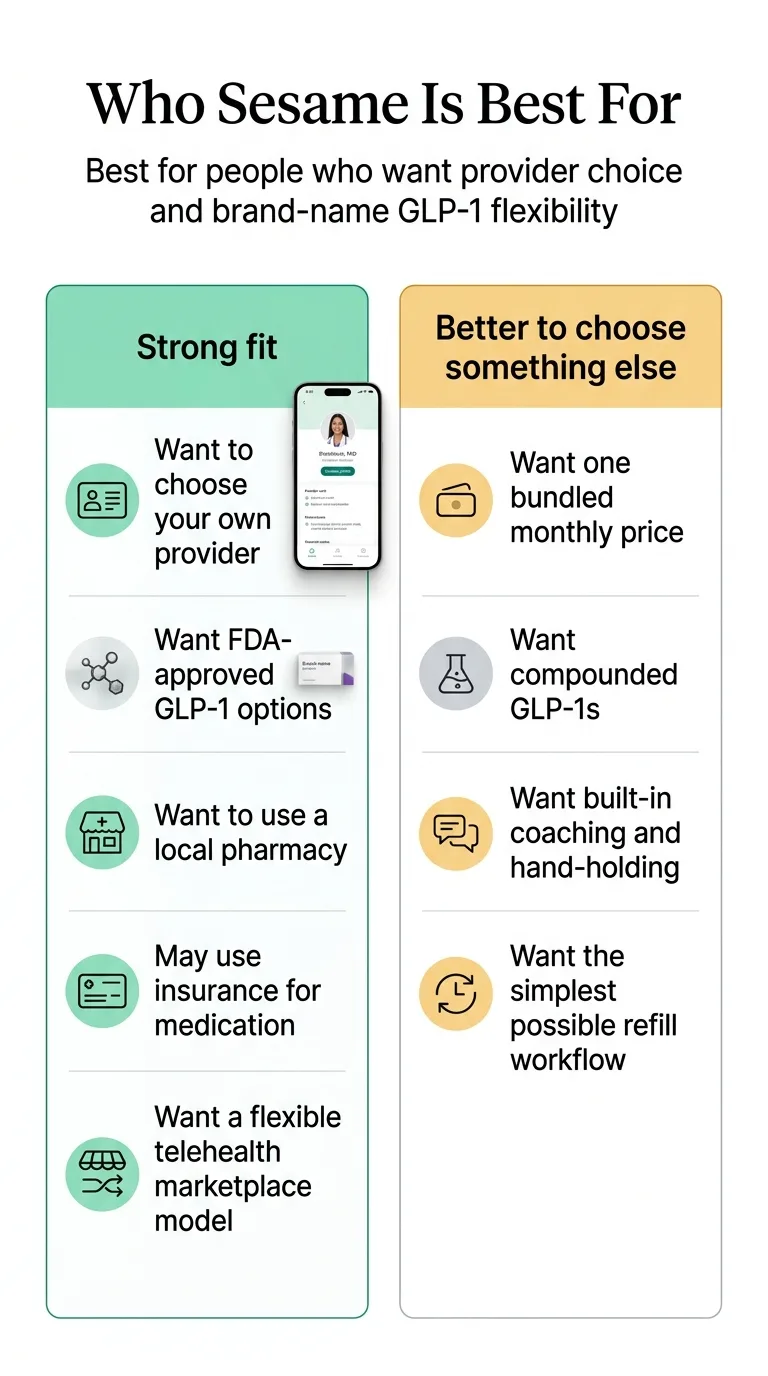
The honest framing: Sesame says directly that it does not bill health insurance for the program. Your visits are cash-pay. But the medication itself can be filled through your MA-PD plan's pharmacy network for covered indications (diabetes, CV risk, OSA), or routed to NovoCare or LillyDirect for cash-pay manufacturer pricing. Sesame providers can also assist with insurance preauthorization paperwork.
Pricing
Subscriptions from $59/month on an annual plan. Medication is not included; providers set their own medication prices.
Sesame does not bill health insurance for the program.
Sesame does not bill health insurance for the program. Medication may fill through your plan for covered indications.
One thing to know about manufacturer savings cards
Manufacturer commercial savings cards generally exclude Medicare, Medicaid, and other government-program beneficiaries. NovoCare's Wegovy Savings Offer states that patients enrolled in Medicare, Medicaid, or other government programs are not eligible. Medicare members may still have direct-pay options through NovoCare Pharmacy, LillyDirect, TrumpRx, Ro, or Sesame — verify the live price and Medicare eligibility at checkout.
What Medicare Advantage members should not do
Answer capsule
Five mistakes account for almost every “I paid $300 and got nothing” story from Medicare Advantage members shopping for GLP-1 telehealth.
Don't pay a membership fee before verifying the provider accepts your exact MA plan — not just 'Aetna' but your specific Aetna policy.
Don't confuse the parts of Medicare. Part B is medical visits. Part D is prescription drugs. Part C is Medicare Advantage (combines A, B, and usually D). MA-PD is Part C with drug coverage included. The Bridge is a separate program from all of these.
Don't try to route compounded GLP-1s through Medicare. Compounded semaglutide and compounded tirzepatide are not FDA-approved, are not Medicare-covered, and are not Bridge-eligible. For Medicare members specifically, choosing FDA-approved brand-name GLP-1s is what positions you for $50/month Bridge coverage once it opens.
Don't use commercial manufacturer savings cards. The Wegovy and Zepbound commercial savings offers generally exclude Medicare beneficiaries. If a telehealth platform tells you to apply a savings card and you're on Medicare, ask twice.
Don't sign up without reading the cancellation terms. If the program can't get your medication covered, can you cancel? When? How? Get the answer in writing.
How we built this guide and what we actually verified
Answer capsule
Every factual claim in this guide is tied to either a federal source (CMS, FDA, KFF, Medicare.gov) or to a provider's own public insurance and pricing page. We ranked providers by Medicare Advantage usefulness — not by affiliate payout. This page was last verified May 13, 2026 and is on a monthly verification cycle through Bridge launch.
What we verified
- ✓CMS Medicare GLP-1 Bridge page (last modified May 12, 2026): eligibility criteria, drug list, Humana as central processor, BIN/PCN, $50 copay treatment
- ✓KFF BALANCE Model brief (updated May 11, 2026): Bridge extension through Dec 2027
- ✓Form Health public pages: Medicare and major-insurance acceptance language, self-pay rate
- ✓knownwell FAQ and pricing pages: Medicare acceptance, no membership fee, NovoCare/LillyDirect routing
- ✓Shapely Medicare and Humana pages: in-network claims, state availability (CA, FL, NY, TX), membership pricing
- ✓One Medical's insurance page: Medicare-participating status, select MA plans
- ✓Ro pricing and insurance pages: $39 first month; cannot coordinate government insurance
- ✓Sesame online weight-loss program: $59/month annual subscription; does not bill health insurance
- ✓PlushCare Medicare coverage page: Part B dropped January 1, 2026
- ✓FDA pages: Wegovy CV indication; Zepbound OSA indication; Foundayo approval; compounded GLP-1 position
- ✓NovoCare Wegovy Savings Offer: Medicare exclusion language
- ✓Medicare.gov: 65-day redetermination window
- ✓CMS OMHA: 2026 amount-in-controversy threshold of $200
What we did not verify
- !Exact plan-name acceptance for every Medicare Advantage policy in every ZIP code (this changes constantly — you have to verify yourself with your plan and the provider)
- !Whether every provider's PA workflow will be ready for the Humana Bridge processor on day one (July 1, 2026) — Bridge PA readiness is not publicly verifiable for any specific telehealth provider as of May 2026
- !Your individual clinical eligibility (only your doctor can confirm this)
Our ranking methodology
Frequently asked questions
Do GLP-1 providers actually accept Medicare Advantage?
A small number do. Form Health, knownwell, Shapely (in CA, FL, NY, TX), and One Medical Seniors are the four telehealth or hybrid clinics with the strongest Medicare and Medicare Advantage signals as of May 2026. Most other GLP-1 telehealth platforms -- Ro, Sesame, Hims, Hers, WeightWatchers Clinic, LifeMD, and compounded providers like MEDVi and Eden -- are cash-pay only and do not bill Medicare Advantage for visits.
Does Medicare Advantage cover Wegovy?
Medicare Advantage with prescription drug coverage (MA-PD) may cover Wegovy when prescribed for cardiovascular risk reduction in adults with established cardiovascular disease and obesity or overweight, or for MASH liver disease where plan criteria are met. It does not cover Wegovy for weight loss alone through standard Part D. Starting July 1, 2026, eligible Medicare Part D and MA-PD enrollees can access Wegovy through the Medicare GLP-1 Bridge for $50/month for weight management.
Does Medicare Advantage cover Zepbound?
Medicare Advantage may cover Zepbound when prescribed for moderate-to-severe obstructive sleep apnea in adults with obesity. It does not cover Zepbound for weight loss alone through standard Part D. Starting July 1, 2026, the Medicare GLP-1 Bridge covers the Zepbound KwikPen formulation only (not single-dose vials or single-dose pens) for $50/month for eligible enrollees.
Does Medicare Advantage cover Ozempic?
Yes -- Medicare Advantage with Part D generally covers Ozempic for type 2 diabetes, subject to plan formulary, prior authorization, and step-therapy rules. Ozempic is not Medicare-covered for off-label weight loss, and Ozempic is not included in the July 2026 Medicare GLP-1 Bridge.
Does Medicare Advantage cover Mounjaro?
Mounjaro may be covered by Medicare Advantage with Part D for type 2 diabetes if it's on your plan's Drug List and you meet plan criteria. It is not covered for weight loss alone and is not part of the Bridge program.
Does Medicare Advantage cover Foundayo?
Foundayo (orforglipron) is an FDA-approved once-daily oral GLP-1 tablet for weight management. It is not covered through standard MA-PD Part D for weight loss alone. It is included in the Medicare GLP-1 Bridge starting July 1, 2026, for eligible enrollees at $50/month.
What is the Medicare GLP-1 Bridge?
The Medicare GLP-1 Bridge is a CMS demonstration program running July 1, 2026 through December 31, 2027. It provides eligible Medicare Part D and MA-PD beneficiaries with access to Wegovy, Zepbound KwikPen, or Foundayo for $50/month for weight management. The program runs outside your Part D plan, uses Humana as the central processor for prior authorizations (BIN 028918 / PCN MEDDGLP1BR), and requires you to meet one of three clinical pathways based on BMI and qualifying conditions.
Who submits the Medicare GLP-1 Bridge prior authorization?
Your prescriber submits the prior authorization directly to Humana, the CMS central processor -- not to your individual Part D or MA-PD plan. CMS says any prescriber can submit a Bridge PA, as long as they are not on the CMS Preclusion List. As of May 2026, no specific telehealth platform has publicly confirmed its Humana Bridge PA workflow.
Can Ro help if I have Medicare Advantage?
Ro can prescribe FDA-approved GLP-1 medication on a cash-pay basis and offers a free Insurance Coverage Checker. However, Ro states directly that it cannot coordinate GLP-1 coverage for government insurance plans, including Medicare and Medicare Advantage. Ro is a cash-pay option for Medicare members, not a Medicare Advantage-billed provider.
Does Sesame bill Medicare Advantage?
No -- Sesame does not bill health insurance for its weight-loss program. Your visits are paid out of pocket through a subscription that starts at $59/month on an annual plan. However, the medication itself can be filled through your MA-PD plan's pharmacy network for covered indications, and Sesame providers can assist with prior authorization paperwork.
Does WeightWatchers Clinic accept Medicare Advantage?
WeightWatchers Clinic's care team works with insurance and its cost estimator includes a Medicare-related bucket. Exact Medicare Advantage acceptance for clinical visits is plan-specific and should be verified at booking. Membership runs $25 first month then $74/month on an annual plan, with medication separate.
Does PlushCare accept Medicare Advantage?
PlushCare dropped Medicare Part B as of January 1, 2026. Some Medicare Advantage (Part C) plans may still be accepted at booking. PlushCare is not a top recommendation for Medicare members because its Medicare acceptance has narrowed -- verify your exact plan before paying.
Are compounded GLP-1s covered by Medicare Advantage?
No. Compounded semaglutide and compounded tirzepatide are not FDA-approved, are not covered by Medicare Advantage or Medicare Part D, and are not eligible for the Medicare GLP-1 Bridge program. For Medicare members, the FDA-approved brand-name path (Wegovy, Zepbound, Ozempic, Mounjaro, Foundayo) is the only route that connects to insurance or Bridge coverage.
Can I use manufacturer coupons with Medicare Advantage?
Generally, no. Commercial manufacturer savings cards -- including the Wegovy Savings Offer and Zepbound Savings Card -- exclude Medicare, Medicaid, and other government-program beneficiaries. Medicare members can still access manufacturer pricing through NovoCare Pharmacy, LillyDirect, and TrumpRx -- those are direct-pay channels, not coupon programs. Verify current rules at each program before checkout.
Should I use my PCP or an online GLP-1 provider?
For most Medicare Advantage members, starting with your in-network PCP is the simplest and most affordable path because they can submit prior authorizations through your existing plan with no membership fee. Online providers like Form Health and knownwell are good options if your PCP isn't comfortable with GLP-1 prescribing, doesn't have obesity-medicine expertise, or has long appointment delays.
How often should I re-check my plan's formulary?
At least once a year during the Annual Enrollment Period (October 15 through December 7), and whenever your plan sends you a Notice of Change. Plans update their formularies annually, and GLP-1 coverage rules are evolving fast -- what your plan covers in 2026 may change for 2027.
What if I qualify for both Medicare and Medicaid?
If you're dual-eligible and enrolled in an eligible plan type (like a Special Needs Plan), you can participate in the Medicare GLP-1 Bridge. However, Low-Income Subsidy (Extra Help) does not apply to the Bridge -- you pay $50/month either way. If your state Medicaid program covers GLP-1s for obesity, Medicaid may give you a lower copay than the Bridge.
Still not sure which GLP-1 program is right for you?
This page covered every Medicare Advantage GLP-1 question we could think of. If you're still unsure which path fits your situation — your plan type, your state, your indication, your timing — let our quiz do the matching for you.
Get my personalized Medicare GLP-1 path
Six questions. Sixty seconds. Get your route (Bridge, Part D, in-network provider, or cash-pay), your verified provider shortlist, the questions to ask before paying, and a printable doctor visit script.
→ Find My Medicare GLP-1 PathRelated guides on The RX Index
- Medicare GLP-1 Bridge Program: Complete Guide (2026)
- Does Medicare Cover Wegovy for Weight Loss? (2026)
- Does Medicare Cover Zepbound? (2026)
- Does Medicare Cover Foundayo? Bridge Program & Part D Guide
- Does Medicare Cover Mounjaro for Weight Loss? (2026)
- Best GLP-1 Providers That Accept Insurance (2026)
- GLP-1 Providers That Accept CHAMPVA: 4 Coverage Paths (2026)
- GLP-1 Providers That Accept TRICARE (2026): Coverage Paths and PA Guide
Sources
- Centers for Medicare & Medicaid Services — Medicare GLP-1 Bridge
- Centers for Medicare & Medicaid Services — BALANCE Model
- Centers for Medicare & Medicaid Services — Third Level of Appeal: OMHA
- Kaiser Family Foundation — What to Know About the BALANCE Model for GLP-1s
- Medicare.gov — Medicare Appeals publication
- FDA — FDA Approves First Treatment to Reduce Risk of Serious Heart Problems Specifically in Adults with Obesity or Overweight
- FDA — FDA Approves First Medication for Obstructive Sleep Apnea
- FDA — FDA Warns 30 Telehealth Companies Against Illegal Marketing of Compounded GLP-1s
- Form Health — Homepage
- knownwell — Weight Loss Medication Pricing
- Shapely — Humana coverage page
- One Medical — Insurance page
- Ro — Pricing
- Ro — Insurance
- Sesame Care — Online weight-loss program
- NovoCare — Wegovy Savings Offer
Last verified: May 13, 2026. The RX Index Editorial Team. This page is on a monthly verification cycle through Medicare GLP-1 Bridge launch and is updated within 30 days of any announced CMS, FDA, or major provider policy change.
This page is for informational purposes only and is not medical advice. Talk to a licensed clinician before starting, stopping, or changing any GLP-1 medication. Insurance coverage, plan formularies, and federal programs change frequently — always verify with your Medicare Advantage plan and your prescriber before making decisions. Methodology · Editorial Standards
