Affiliate disclosure: The RX Index earns a commission when you sign up with some of the providers mentioned on this page. It does not affect what you pay, and it never determines our rankings or which providers we cover. Read the full disclosure.
Disclosure: Some links on this page are affiliate links. If you purchase through these links, we may earn a commission at no extra cost to you.
Does Medicare Cover Foundayo? Yes — $50/Month Starting July 1, 2026 (If You Qualify)
Published: · Last updated:

✅ What we actually verified for this page (April 19, 2026)
- The Medicare GLP-1 Bridge is a nationwide CMS demonstration running July 1, 2026 – December 31, 2027 (18 months), authorized under Section 402 of the Social Security Amendments. BALANCE did not launch for Medicare Part D in 2027 — CMS extended the Bridge.
- Eligible beneficiaries pay a flat $50 per month — regardless of dose.
- CMS uses a single central processor (BIN 028918, PCN MEDDGLP1BR) to handle prior authorization, claims, and pharmacy payment.
- Bridge claims sit outside the normal Part D payment flow — the $50 does not count toward TrOOP, and the Low-Income Subsidy does not reduce it.
- Part D sponsors do not have to opt in. Pharmacies do not have to opt in.
- The Foundayo Savings Card is not usable by Medicare beneficiaries — Eli Lilly’s own terms exclude Medicare, Medicare Part D, Medicare Advantage, and Medigap.
- The 2027 BALANCE Model is at real risk — CMS has said it will not launch BALANCE in Medicare Part D in 2027 if fewer than 80% of eligible Part D sponsors sign up.
The short answer — in 100 words
Does Medicare cover Foundayo? Today, no. Standard Medicare Part D excludes weight-loss drugs by law, and Foundayo is currently FDA-approved only for chronic weight management. Starting July 1, 2026, eligible Medicare Part D beneficiaries can get Foundayo for a $50 monthly copay through the Medicare GLP-1 Bridge — a nationwide CMS program that operates outside your Part D plan. To qualify, you need an eligible Part D plan type and BMI ≥35 at therapy start, or BMI ≥30 with a cardiometabolic condition, or BMI ≥27 with prediabetes or a prior cardiovascular event. The $50 does not count toward TrOOP, and Extra Help does not reduce it.
Your fastest path at a glance
| Path | Monthly Cost | Who It’s For | When Available |
|---|---|---|---|
| Medicare GLP-1 Bridge | $50 flat | Eligible Part D beneficiaries meeting Bridge clinical criteria | July 1, 2026 – Dec 31, 2027 |
| BALANCE Model (Part D) | $50 enhanced plans; $125 basic plans; plus deductible phase | Beneficiaries in BALANCE-participating plans | January 1, 2027 onward |
| Foundayo Savings Card | $25 | Commercial insurance only — not Medicare | Available now |
| LillyDirect self-pay | $149 (0.8 mg) · $199 (2.5 mg) · $299 (5.5–17.2 mg) | Anyone paying cash | Available now |
🔵 Start here: Take our free 60-second Medicare Foundayo Path quiz
Answer four quick questions about your plan type, BMI, and diagnoses. We’ll tell you whether you’re likely Bridge-eligible on July 1, flag the documents your doctor will need, and if you don’t qualify we’ll route you to an honest interim option. No email required to see your result.
Check my Medicare Foundayo path →Does Medicare Cover Foundayo Right Now?
The short answer: No. As of April 2026, no Medicare plan covers Foundayo for weight loss. Standard Medicare Part D excludes weight-management drugs by law. That changes July 1, 2026, when CMS launches the Medicare GLP-1 Bridge — a nationwide demonstration that provides Foundayo (orforglipron), Wegovy, and the Zepbound KwikPen to eligible Part D beneficiaries at $50 per month.
Why standard Medicare Part D still says no
When Congress created Medicare Part D in 2003, the law specifically excluded coverage of drugs used for anorexia, weight loss, or weight gain. That exclusion has held for 20+ years. Ozempic and Mounjaro (both GLP-1s) have been covered by Medicare Part D for many beneficiaries only because they carry FDA approval for type 2 diabetes — not weight loss.
Foundayo is different. Right now it’s FDA-approved for one thing: chronic weight management in adults with obesity or overweight with weight-related medical problems. Eli Lilly has said it plans to file for a type 2 diabetes indication later in 2026, but until that approval lands, Medicare has no standard pathway to cover Foundayo for any indication.
The exception that actually matters: the Medicare GLP-1 Bridge
On December 23, 2025, CMS announced two new programs to expand Medicare access to GLP-1s for weight loss:
- The BALANCE Model — a longer-term program launching in Medicaid as early as May 2026. BALANCE did not launch for Medicare Part D in 2027 (the 80% plan participation threshold was not met) — watch for BALANCE 2028 announcements during fall 2027 open enrollment.
- The Medicare GLP-1 Bridge — an 18-month program running July 1, 2026 through December 31, 2027. CMS extended the Bridge (originally planned for 6 months) because BALANCE did not meet its Medicare Part D launch threshold. Foundayo is a covered drug on the Bridge.
CMS released detailed Bridge rules on March 3, 2026, and later updated the drug list to include Foundayo after its FDA approval on April 1, 2026. Starting July 1, Foundayo joins Wegovy and the Zepbound KwikPen as Bridge-covered drugs for eligible beneficiaries — at a fixed $50 copay.
The one-sentence version
Standard Part D: no. Bridge from July 1, 2026 through December 31, 2027: yes, if you meet the criteria ($50/month). BALANCE did not launch for Medicare Part D in 2027 — CMS extended the Bridge instead. After December 2027: watch for BALANCE 2028 announcements.
Who Qualifies for the Medicare GLP-1 Bridge?
The short answer: Two things have to be true. First, you must be enrolled in an eligible Medicare Part D plan type. Second, your prescribing provider must attest you meet one of three clinical pathways based on BMI and qualifying conditions. Get both right, and you pay $50/month starting July 1, 2026.
This is the single most misreported part of the Bridge. Several high-ranking pages are quoting criteria that look close but aren’t. We pulled the criteria directly from the official CMS Medicare GLP-1 Bridge FAQ.
The three clinical pathways (you only need to meet one)
| Pathway | Age | BMI at therapy start | Qualifying diagnosis required? |
|---|---|---|---|
| Pathway 1 — BMI alone | 18+ | ≥35 | None — BMI is enough |
| Pathway 2 — BMI + cardiometabolic | 18+ | ≥30 | One of: HFpEF, uncontrolled hypertension, or CKD stage 3a or higher |
| Pathway 3 — BMI + prior event or prediabetes | 18+ | ≥27 | One of: prediabetes (per ADA guidelines), previous heart attack, previous stroke, or symptomatic peripheral artery disease |
Nuances most pages miss
- “Uncontrolled hypertension” has a specific CMS definition. CMS defines it as systolic blood pressure above 140 mm Hg or diastolic above 90 mm Hg despite concurrent treatment with two antihypertensive medications. Being on one blood-pressure pill with a high reading does not automatically qualify under Pathway 2.
- Type 2 diabetes alone is not a Bridge qualifier. Neither is high cholesterol alone. Both are common. Both get miscited as qualifying conditions on competitor pages. They’re not on the CMS list.
- Prediabetes qualifies — but only under Pathway 3 at BMI ≥27, and only as defined by the American Diabetes Association (A1C 5.7%–6.4%, fasting glucose 100–125 mg/dL, or 2-hour OGTT 140–199 mg/dL).
The “starting BMI” rule that matters a lot
Here’s the thing that trips up almost everyone. CMS ties Bridge qualification to BMI at the time GLP-1 therapy was initiated, not BMI the day your provider submits the prior authorization.
Already taking a GLP-1 today? Your starting BMI — the one in your chart from when you first began — is what counts. CMS uses this exact example in their FAQ: a patient who started at a BMI of 37 in 2024 and is at BMI 34 today still qualifies under Pathway 1, because starting BMI is the anchor.
This matters because your provider’s documentation of your original weight and height is what gets attested to on the Bridge prior authorization form. If you’ve already lost weight on a compounded GLP-1, or on Wegovy or Zepbound, pull that starting chart note and make sure it’s clean before July.
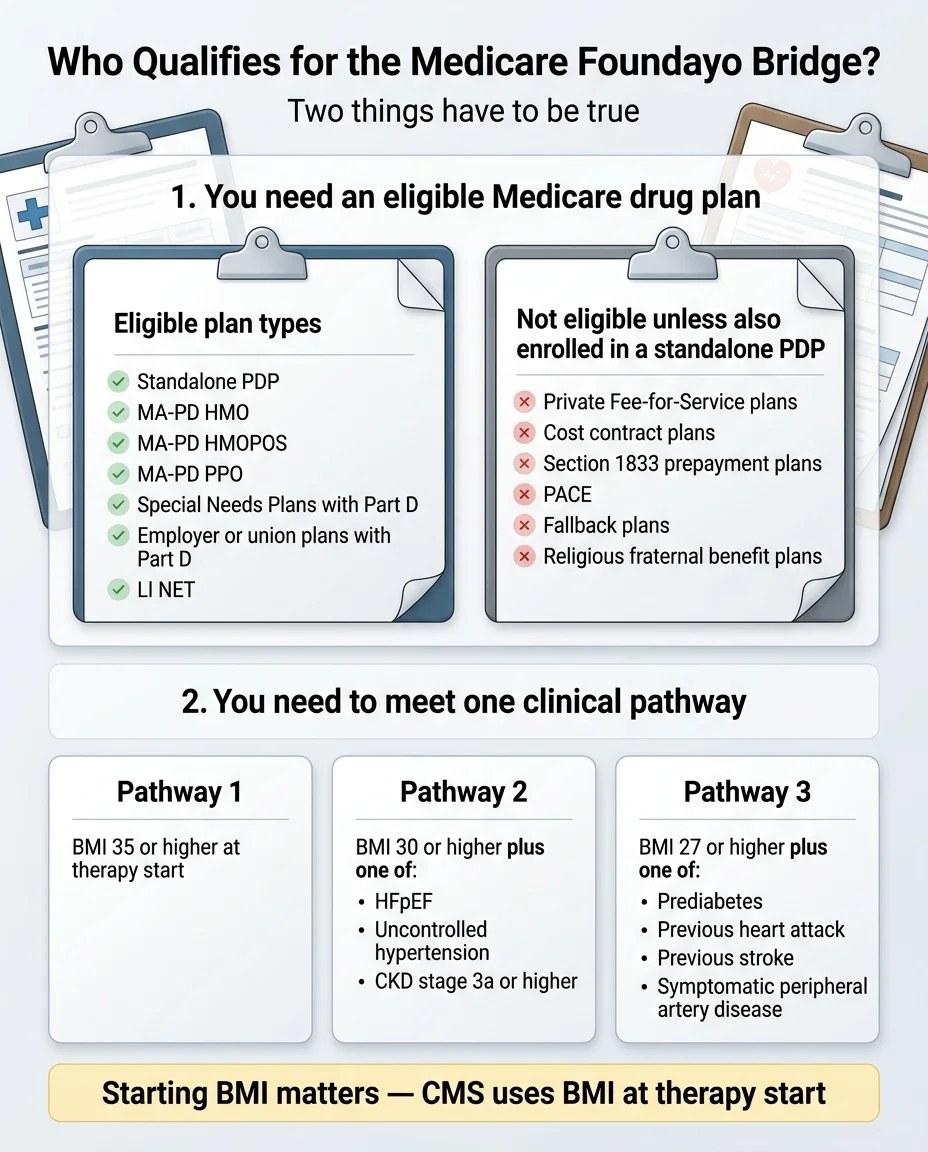
Which Medicare plan types qualify for the Bridge?
✅ Eligible plan types
- Standalone Prescription Drug Plans (PDPs)
- Medicare Advantage HMO with drug coverage (MA-PD)
- MA-PD HMOPOS
- Local and Regional PPO-PD
- Special Needs Plans (SNPs) with Part D
- Employer/Union Group Waiver Plans (EGWPs) with Part D
- Limited Income Newly Eligible Transition (LI NET)
- Dual-eligible beneficiaries enrolled in any of the above
❌ Not eligible (unless also enrolled in a standalone PDP)
- Private Fee-for-Service (PFFS) plans
- Section 1876 cost contract plans
- Section 1833 health care prepayment plans
- PACE organizations
- Fallback plans
- Religious fraternal benefit plans
That second list matters. If you’re in a PFFS Medicare Advantage plan, in PACE, or in a cost contract, the Bridge won’t help you on July 1 unless you also pick up standalone drug coverage. That’s a plan-change conversation to have before Medicare’s 2026 Annual Enrollment Period closes on December 7, 2026.
What real Medicare beneficiaries are asking
- “Does anyone know if and when Foundayo pill will be available on Medicare?”
- “I don’t know how much longer I can wait for the $50 thing.”
- “Not sure what exactly ‘meet the criteria’ and ‘eligible beneficiaries’ means for me.”
Real user questions from public discussion threads. Not medical evidence.
🔵 See whether you qualify — in 60 seconds
Our Medicare Foundayo Path quiz asks about your plan type, BMI, and diagnoses, then tells you which of the three pathways applies to you (or whether you’ll need an interim option).
Check my Bridge eligibility →Does Medicare Advantage or Medigap Cover Foundayo Differently?
The short answer: Medicare Advantage changes the answer only if you have an MA coordinated-care plan with Part D (HMO, HMOPOS, PPO, or SNP). Medigap doesn’t cover prescription drugs at all, so Medigap by itself is not a Foundayo pathway.
Medicare Advantage with Part D (MA-PD HMO, PPO, etc.)
Good news: these are Bridge-eligible plan types. Your MA-PD plan does not have to “opt in” — the Bridge runs outside the Part D benefit anyway, with a single central processor handling claims on behalf of CMS. As long as you meet the clinical criteria and your provider submits the prior authorization to the Bridge processor (not your MA plan), you pay $50/month.
Medicare Advantage without drug coverage (MA-only)
If your MA plan doesn’t include Part D — sometimes true for Medical Savings Account MA plans or certain PFFS plans — you’re not Bridge-eligible unless you also enroll in a standalone PDP where that’s permitted. This is a plan-structure conversation worth having with your agent before July.
Medigap (Medicare Supplement)
Medigap is not prescription drug coverage. It’s a supplement that fills in Parts A and B gaps. If your only drug coverage is through a standalone PDP that sits alongside Original Medicare + Medigap, then your PDP is what determines your Bridge eligibility, not the Medigap plan. If you have Medigap but no PDP, you have no Medicare drug coverage at all, Bridge or otherwise.
Dual-eligibles (Medicare + Medicaid) and the LIS reality
If you’re enrolled in Medicare and full Medicaid, you can still access the Bridge if you’re in an eligible Medicare Part D plan type. But a critical note most pages bury: the Low-Income Subsidy (Extra Help) does not reduce the Bridge copay. You will still pay the full $50 per month, even if you normally pay pennies for Part D drugs. For some readers on tight fixed incomes, that $50 is real money.
VA, TRICARE, and DoD beneficiaries
Government-program beneficiaries — VA, TRICARE, DoD — are excluded from Lilly’s commercial Foundayo Savings Card. The Bridge is a separate question: whether you qualify depends on whether you’re also enrolled in an eligible Medicare Part D plan. If you’re covered solely through the VA, TRICARE, or DoD and do not have Medicare Part D, you don’t have a Bridge pathway. Check with your benefits administrator for any formulary-based coverage.
How Much Does Foundayo Cost with Medicare?
The short answer: Under the Medicare GLP-1 Bridge, eligible beneficiaries pay a flat $50 per month for Foundayo, regardless of dose, regardless of your Part D deductible status, and regardless of Low-Income Subsidy enrollment. The rest of the drug’s cost is paid to the pharmacy by a CMS-contracted central processor.
The structural math of the $50
CMS negotiated directly with Eli Lilly. Participating manufacturers provide eligible GLP-1 drugs at a net price of $245 per monthly supply to CMS. Pharmacies are reimbursed by the central processor at the drug’s wholesale acquisition cost, minus the $50 copay you paid, plus a dispensing fee and applicable sales tax.
Three things most pages skip
- The $50 copay does not count toward your Part D True Out-of-Pocket (TrOOP) threshold. If you’re taking other expensive drugs and hoping the Foundayo spend pushes you into Part D catastrophic coverage faster, it won’t. The Bridge is walled off from the regular Part D benefit.
- The $245 net price CMS pays does not count toward Gross Covered Prescription Drug Costs (GCPDC). Your plan’s reporting and benchmarks don’t see it.
- Extra Help / Low-Income Subsidy does not reduce the $50. If you normally pay $4.90 for generics under LIS, you still pay the full $50 for Foundayo through the Bridge.
How the Bridge $50 compares to other paths
| You are… | What you’ll pay for Foundayo |
|---|---|
| On Medicare, Bridge-eligible, July 2026–Dec 2027 | $50/month flat |
| On Medicare, Bridge-ineligible | Self-pay only: $149–$349/month through LillyDirect |
| On commercial insurance that covers Foundayo | $25/month with the Lilly Savings Card (plan deductible still applies) |
| On commercial insurance that does NOT cover Foundayo | $149–$299/month with Lilly’s Self-Pay Savings Card |
| VA / TRICARE / DoD only | Not eligible for either savings card or the Bridge. Check benefits administrator. |
What if I’m paying cash right now and want to switch to the Bridge on July 1?
You can. Because CMS uses “BMI at therapy initiation” as the eligibility anchor, starting Foundayo on cash-pay via LillyDirect now — then transitioning to the Bridge on July 1 — preserves your starting-BMI qualification. Between now and July 1, that’s $149–$349/month depending on dose. After July 1, it drops to $50/month if you’re eligible.
🔵 Which path is actually cheapest for your situation?
Our quiz maps your coverage type, BMI, and diagnoses to the lowest realistic out-of-pocket cost — whether that’s the Bridge, LillyDirect, or a telehealth path.
Find my cheapest Foundayo path →How Does the Medicare GLP-1 Bridge Actually Work?
This is the mechanical piece every other page glosses over. If your prescriber sends the prior authorization to the wrong place, or your pharmacy bills the wrong payer, you’re going to find out the hard way at the counter.
Step 1 — Your provider submits a Bridge prior authorization to the central processor
CMS runs the entire Bridge through one central processor that handles prior authorization, claims adjudication, and pharmacy payment. Your provider does not submit the PA to your Part D plan. If they submit it to the plan by mistake, CMS has asked plans to return a message directing them to the central processor — but that’s friction you don’t want. Print or forward the CMS Bridge FAQ to your provider before the appointment.
Critical detail: Your provider doesn’t have to be enrolled in Medicare to submit a Bridge PA, but they cannot be on the CMS Preclusion List. This is unusually permissive and matters for telehealth readers — a telehealth obesity medicine provider can submit a Bridge PA even if they aren’t a traditional Medicare-enrolled clinician.
Step 2 — Your pharmacy bills the Bridge-specific BIN/PCN
Pharmacies submit Bridge claims to:
BIN: 028918
PCN: MEDDGLP1BR
These are published by CMS in the Bridge FAQ. Pharmacies do not have to “opt in.” The Bridge is the primary payer — it does not coordinate benefits with other payers, and coupons and discount programs cannot be applied. Paper claims and direct member reimbursements will not be accepted by the central processor.
If a pharmacy staff member tries to bill your regular Part D plan for a Foundayo prescription written under the Bridge, the claim will likely reject. Show them the CMS Bridge FAQ or ask them to bill the Bridge-specific BIN/PCN.
Step 3 — You pay $50 at the counter
The pharmacy collects your $50 copay. The central processor reimburses the pharmacy for the rest of the drug’s wholesale acquisition cost, plus a dispensing fee and any sales tax. You walk out with your prescription.
When a prescription should NOT go through the Bridge
If Foundayo is ever prescribed for a use that’s already coverable under the basic Part D benefit — for example, if it eventually gets an FDA indication for type 2 diabetes — your provider needs to go through your regular Part D plan’s utilization management process, not the Bridge. Wegovy is already in this situation today for its cardiovascular indication; Zepbound is in this situation today for its obstructive sleep apnea indication. For now, Foundayo is only approved for weight management, so Bridge is the only Medicare route.
Appeal rights are not modified by the Bridge. If you’re denied by the central processor, the standard Medicare Part D drug-appeal process still applies. See the appeal section below.
Can You Use the Foundayo Savings Card with Medicare?
The short answer: No. Eli Lilly’s Foundayo Savings Card terms explicitly exclude all government-program beneficiaries — including Medicare, Medicare Part D, Medicare Advantage, and Medigap. CMS has also stated coupons and discount programs cannot be applied to Bridge claims.
Why the $25 card doesn’t work for Medicare
Federal anti-kickback rules effectively prohibit drug manufacturers from offering copay assistance to Medicare and other government-program beneficiaries. This isn’t a Foundayo-specific rule — every major brand-name drug in the U.S. has the same exclusion on its manufacturer savings card. Lilly’s published Foundayo Savings Card terms spell it out: governmental beneficiaries, including Medicaid, Medicare, Medicare Part D, Medicare Advantage, Medigap, DoD, VA, and TRICARE/CHAMPUS, are not eligible for the card.
Why coupons and discount cards don’t stack on Bridge claims either
CMS has been explicit in the Bridge FAQ: Bridge claims are processed by the central processor, not through normal Part D rails, and coupons or discount programs may not be applied. The $50 is the $50. It’s not a starting point you can negotiate down with GoodRx, SingleCare, or a manufacturer coupon.
The trade-off most people miss
$25/month (commercial) vs. $50/month (Medicare Bridge) — which is actually cheaper?
- A commercially insured reader paying $25 usually has to first meet their plan’s prescription deductible — which can be hundreds to thousands of dollars.
- A Medicare Bridge beneficiary paying $50 has no deductible to meet first and the $50 copay stays fixed through the Bridge period.
Net-net: first-year Medicare Bridge cost is often lower than first-year commercial cost, despite the higher per-month copay on paper.
Foundayo vs. Wegovy vs. Zepbound Under Medicare — Which One Wins?
The short answer: Three drugs are on the Medicare GLP-1 Bridge list at the same $50 monthly copay — Foundayo (orforglipron), Wegovy (injection and oral tablets), and the Zepbound KwikPen (tirzepatide, injection). Foundayo and Wegovy tablets are the two oral choices. Wegovy has an FDA cardiovascular indication that can unlock regular Part D coverage for some readers; Zepbound has an FDA obstructive sleep apnea indication that can do the same.
The GLP-1 Bridge drug menu, side by side
| Feature | Foundayo (orforglipron) | Wegovy (semaglutide) | Zepbound (tirzepatide) |
|---|---|---|---|
| Forms on the Bridge list | Oral pill, once daily | Pen injection or oral tablet | KwikPen only — single-dose vial and single-dose pen are not Bridge-covered |
| Timing | Anytime, with or without food | Injection: weekly. Tablet: empty stomach, limited water | Weekly injection |
| Average weight loss, highest approved dose | ~11.1% over 72 weeks (ATTAIN-1) | ~15% range, injection (STEP trials) | ~22% (SURMOUNT-1) |
| Bridge copay | $50/month | $50/month | $50/month (KwikPen only) |
| Self-pay (LillyDirect / NovoCare) | $149–$349 | ~$199+ (form-dependent) | $299–$449 |
| Storage | Room temperature | Some forms need refrigeration | Refrigeration required |
| FDA indications that may unlock regular Part D | None yet | Cardiovascular risk reduction in established CV disease | Obstructive sleep apnea in adults with obesity |
Weight-loss percentages reflect different trial populations, durations, and baseline characteristics. Direct head-to-head trials have not been run. Individual results vary.
Why Foundayo is a quiet winner for many Medicare beneficiaries
A pill is a pill. For readers 55 and older, the practical advantages stack up fast:
- No injection. Arthritis, tremor, and visual impairment all complicate self-injection. Foundayo removes that friction entirely.
- No refrigeration. Travel becomes easier. A snowbird migration to Florida doesn’t require an insulated drug cooler.
- No timing rule. Unlike the Wegovy pill (empty stomach, limited water, morning), Foundayo can be taken with coffee, with breakfast, with dinner — whenever fits your routine.
The honest trade-off: clinical trial weight loss on Foundayo is lower than what Zepbound injections produced. But a pill you take every day often beats an injection you skip — adherence is what determines real-world outcomes.
When Wegovy or Zepbound might be a smarter Bridge choice
- Wegovy if you have established cardiovascular disease. Its FDA CV indication means your provider may be able to route a prescription through your regular Part D plan (outside the Bridge), potentially with different cost-sharing.
- Zepbound KwikPen if you have moderate-to-severe obstructive sleep apnea with obesity. The OSA indication may unlock regular Part D coverage.
What to Do Before July 1, 2026 — Your Readiness Plan
The short answer: Use the window between now and July to lock down three things your provider will need on the prior authorization: your starting BMI documented in your chart, your qualifying diagnosis documented if BMI is 27–34, and a prescribing provider who will submit the Bridge PA correctly. Get those in place and July 1 becomes a 10-minute pharmacy pickup.
The 4-step readiness checklist
1. Confirm your plan type is eligible
Look up your plan. Standalone PDP, MA-PD HMO/PPO/HMOPOS, SNP with Part D, EGWP with Part D, or LI NET — you’re in the right bucket. If you’re in a PFFS plan, PACE, a cost contract, a fallback plan, or a religious fraternal benefit plan without a separate PDP — you’ll need to evaluate switching during Medicare’s Annual Enrollment Period (October 15 – December 7, 2026) to have Foundayo coverage in 2027.
2. Get your BMI documented now
Book a primary care visit or obesity medicine consult. Have your weight and height recorded. If you’ve already been on a GLP-1 at any point, ask your provider to pull and re-document your starting BMI — that’s the number CMS uses. If you’ve lost weight since then, your current BMI doesn’t disqualify you.
3. Address your qualifying condition if your BMI is 27–34
The easiest unlock at BMI 27–29 is prediabetes. If your A1C hasn’t been checked in the last 12 months, ask for it — Medicare Part B covers up to two diabetes screening tests per year for at-risk beneficiaries. An A1C between 5.7% and 6.4% qualifies under ADA criteria.
If your BMI is 30–34, an HFpEF diagnosis, documented chronic kidney disease stage 3a+ (eGFR 45–59), or uncontrolled hypertension (SBP >140 or DBP >90 despite two BP medications) unlocks eligibility under Pathway 2.
4. Identify a Bridge-ready prescriber
Not every primary care physician is comfortable with GLP-1 prior authorizations. If yours is in that camp, you have options: request a referral to an obesity medicine specialist, get a second opinion, or use a telehealth provider experienced with GLP-1 prior authorizations. Bridge PAs can be submitted by any provider not on the CMS Preclusion List — they don’t need to be Medicare-enrolled.
If you qualify but don’t want to wait 10+ weeks
Two honest paths:
Path A — Start on cash-pay LillyDirect now
$149/month at the 0.8 mg starting dose. When July 1 arrives, your starting BMI carries forward and you transition to $50/month through the Bridge with a provider-submitted prior authorization. Start at LillyDirect → (sponsored affiliate link, opens in a new tab)
Path B — Telehealth path for readers who need a prescriber
If you don’t have a Bridge-ready provider of your own, a telehealth platform can handle the prescription and help you prepare. These aren’t replacements for Medicare — they’re bridges to the Bridge for readers who can’t wait.
🔵 Build your July 1 readiness plan
Our quiz asks about your plan type, BMI, diagnoses, and whether you want to start now or wait. Output is a personalized readiness checklist — exactly what to bring to your next doctor visit and what to watch for between now and July 1.
Get my July 1 readiness plan →What Happens After December 31, 2027?
The Bridge runs through December 31, 2027. BALANCE did not launch for Medicare Part D in 2027 — the 80% plan participation threshold was not met. Watch for BALANCE 2028 announcements during fall 2027 open enrollment.
The two-program handoff, in plain English
- July 1, 2026 – December 31, 2027 = Medicare GLP-1 Bridge (18 months, extended). Nationwide. Every eligible Part D beneficiary is in. No plan opt-in needed. CMS extended the Bridge because BALANCE did not meet its 80% Part D plan participation threshold for 2027.
- After December 2027 = BALANCE Model may launch for Medicare Part D in 2028 (if CMS runs a new participation round). Watch for announcements during fall 2027 open enrollment (October 15–December 7, 2027).
The 80% participation threshold — this is a real risk
CMS made BALANCE participation voluntary for Part D plans. The BALANCE Part D Plans Request for Applications states that CMS will only launch the model in Medicare if at least 80% of eligible Part D parent organizations sign up. CMS plans to notify manufacturers and plan sponsors by April 30, 2026 whether that threshold has been reached. If it hasn’t, BALANCE does not launch in Medicare Part D in 2027 at all. KFF’s published analysis calls this out directly: Medicare beneficiaries with coverage through the Bridge in the latter half of 2026 could lose access in 2027 if BALANCE doesn’t launch.
We’ll update this page the day CMS releases the April 30 notification.
2027 BALANCE cost-sharing — the numbers CMS has actually published
| Part D plan type | Deductible phase | Initial coverage phase | Catastrophic phase |
|---|---|---|---|
| Enhanced Alternative (EA) and EGWP | Up to $245 + dispensing fee per 30-day supply | Up to $50/month | $0 (after 2027 OOP cap of $2,400) |
| Actuarially Equivalent Standard (AE) and Basic Alternative (BA) | Up to $245 + dispensing fee per 30-day supply | Up to $125/month | $0 (after 2027 OOP cap of $2,400) |
| Defined Standard (DS) | Not eligible to participate as DS | ||
Plan sponsors can choose lower cost-sharing, but $50 (enhanced/EGWP) and $125 (basic) are the ceilings BALANCE sets. Public Citizen’s analysis flagged that roughly 60% of Medicare Part D standalone beneficiaries are in enhanced plans that would hit the $50 cap; the other ~40% in basic plans would face the $125 cap.
Key BALANCE dates to watch
What this means for your 2027 planning
- By late May 2026 you should know whether BALANCE is launching in Medicare Part D at all.
- By early summer 2026 you should know which plans in your area have chosen to participate.
- During Open Enrollment (October 15 – December 7, 2026), you pick your 2027 plan — and if you want continued $50-or-less Foundayo, you need a BALANCE-participating plan with an enhanced benefit structure.
- Switching plans can affect other drugs you take — formularies, tiers, and pharmacy networks can all change.
What If You Don’t Qualify — Or Can’t Wait?
The short answer: If the Bridge isn’t available to you (wrong plan type, BMI too low without a qualifying condition, timing), you have three realistic options: cash-pay LillyDirect, a telehealth path for FDA-approved Foundayo, or a second look at whether you have a missed qualifying diagnosis like prediabetes.
The honest admission we have to make
If you’re on Medicare, qualify for the Bridge, and we route you to any telehealth affiliate instead of Medicare, we are ripping you off. Nothing in our affiliate partner stack beats $50/month through a federal program. That’s just math.
So we won’t do that. For the reader who qualifies for the Bridge: wait for the Bridge, use the pre-July window to prepare, and pay $50/month from July 1. We make $0 on that outcome — and that’s fine, because the right page for a Medicare beneficiary is the page that tells the truth about which door is cheapest.
The alternatives below are for readers the Bridge doesn’t fit — or for readers who legitimately can’t wait 10+ weeks.
Path A — LillyDirect self-pay (cheapest cash route)
Direct from Lilly. No telehealth visit needed if you already have a prescription from your doctor.
- 0.8 mg starting dose: $149/month
- 2.5 mg: $199/month
- 5.5 mg / 9 mg / 14.5 mg / 17.2 mg: $299/month (14.5 mg and 17.2 mg rise to $349 if not refilled within 45 days)
Path B — Telehealth with an FDA-approved lane
If you need a provider and want a straightforward path to brand-name FDA-approved Foundayo:
Sesame Care (sponsored affiliate link, opens in a new tab)
Clinician-led FDA-approved telehealth. Obesity medicine physicians who prescribe FDA-approved GLP-1s, not compounded. The consult flow is calm, doctor-first, and built for skeptical buyers who want a real physician on the other side of the screen.
See Sesame Care Foundayo options → (sponsored affiliate link, opens in a new tab)SHED (tryshed.com) (sponsored affiliate link, opens in a new tab)
A Foundayo-focused telehealth platform built around the new oral GLP-1 class. If your search intent is specifically “I want Foundayo the pill from a telehealth provider that specializes in it,” SHED is the direct match. It pairs well with LillyDirect self-pay pricing because it’s organized around the brand you’re already asking about.
Get started with SHED → (sponsored affiliate link, opens in a new tab)Path C — The A1C test many people haven’t taken
Here’s the single highest-leverage thing a reader with BMI 27–34 and no obvious qualifying condition can do before July 1: get an A1C test.
Undiagnosed prediabetes is common. Per the CDC, more than 1 in 3 American adults has prediabetes and the large majority don’t know it. An A1C of 5.7%–6.4% qualifies under ADA guidelines — which is a qualifying condition for Bridge eligibility under Pathway 3 (BMI ≥27). Medicare Part B covers up to two diabetes screening tests a year for at-risk beneficiaries.
If the test comes back in the prediabetes range, you’re Bridge-eligible on July 1 for $50/month — no telehealth affiliate needed, no cash-pay workaround. This is the advice we’d give you if we were your brother-in-law, and it’s the advice we’re giving you here.
Route off if you’re just not a Medicare shopper: If Medicare isn’t your coverage path at all — you’re on commercial insurance or uninsured and this page came up in your search — head to our Foundayo cost and coverage guide instead. That page is built for your situation.
How Does Foundayo Fit with Existing Medicare-Covered GLP-1s?
The short answer: Ozempic and Mounjaro are already covered by many Medicare Part D plans — but only because they’re FDA-approved for type 2 diabetes. Foundayo is not in that club yet; it only has a weight-management indication. If you have T2D and want a GLP-1, ask your provider about Ozempic, Mounjaro, or Rybelsus through your regular Part D benefit — those may be cheaper than the $50 Bridge copay depending on your plan.
What Medicare already covers for GLP-1s today
- Ozempic (semaglutide injection) — covered by most Part D plans for type 2 diabetes.
- Rybelsus (oral semaglutide) — covered by most Part D plans for type 2 diabetes.
- Mounjaro (tirzepatide injection) — covered by most Part D plans for type 2 diabetes.
One note worth knowing: Ozempic/Rybelsus/Wegovy (all semaglutide) was selected for Medicare Drug Price Negotiation. A Maximum Fair Price takes effect January 1, 2027 — which is after the Bridge period and separate from the Bridge and BALANCE pricing structures.
The Foundayo distinction
Foundayo is currently the only weight-loss-only GLP-1 on the Bridge list without a separate Medicare-covered indication. For readers without T2D, OSA, or an established CV indication, Foundayo is a clean Bridge option with real pill-versus-injection convenience advantages.
What If My Medicare Prescription Is Denied?
The short answer: Appeal — and know the actual Part D drug-appeal deadlines. You have 65 calendar days from the date of the denial notice to file a redetermination request with the plan. The plan must respond within 7 calendar days for a standard drug appeal (72 hours if expedited, or 14 days for a payment appeal). Medicare’s Part D drug-appeal system has five levels in total.
The five-level Part D drug-appeal ladder
- Redetermination by your plan. File within 65 calendar days of the denial notice. Plan responds within 7 calendar days for a standard appeal, 72 hours for expedited, or 14 days for a payment appeal.
- Reconsideration by an Independent Review Entity (IRE). File within 65 calendar days of the redetermination decision.
- Administrative Law Judge (ALJ) hearing. Minimum dollar amount in controversy applies.
- Medicare Appeals Council review.
- Federal court review.
Three things that increase your appeal success rate
- A Letter of Medical Necessity from your prescriber. Specific, dated, referencing your BMI at therapy initiation and your qualifying diagnosis. Generic letters don’t help.
- Documented prior attempts. Weight-management attempts, structured lifestyle interventions, other medications tried and failed — all strengthen the record.
- Specific diagnosis codes. Z68.3x and Z68.4x for BMI; E66.01/E66.09 for obesity; specific codes for prediabetes, prior MI, prior stroke, or PAD depending on which pathway applies.
KFF’s analysis of CMS data on Medicare Advantage prior-authorization appeals found that more than 80% of MA prior-authorization appeals that were filed were overturned, but only about 11% of denied patients ever filed an appeal. If you’re denied, appeal.
Frequently Asked Questions
Does Medicare Part D cover Foundayo for weight loss?⌄
Not under standard Part D rules. Weight-loss drugs are excluded from the basic Part D benefit by law. Foundayo is FDA-approved for weight management. The exception is the Medicare GLP-1 Bridge — an 18-month program running July 1, 2026 through December 31, 2027, that covers Foundayo for eligible Part D beneficiaries at $50/month outside the normal Part D benefit. BALANCE did not launch for Medicare Part D in 2027.
Does Medicare Advantage cover Foundayo?⌄
Medicare Advantage plans with prescription drug coverage (MA-PD HMO, PPO, HMOPOS, and SNP plans) are eligible plan types for the Medicare GLP-1 Bridge. Medicare Advantage plans without drug coverage, PFFS plans, PACE organizations, and cost contract plans are not eligible for the Bridge unless paired with a standalone PDP.
Does Medigap cover Foundayo?⌄
No. Medigap doesn’t cover outpatient prescription drugs — it supplements Parts A and B. If you have Medigap without a standalone Part D plan, you have no Medicare drug coverage, Bridge or otherwise.
Can Medicare patients use the Foundayo Savings Card?⌄
No. Eli Lilly’s Foundayo Savings Card terms explicitly exclude Medicare, Medicare Part D, Medicare Advantage, and Medigap beneficiaries. Federal rules prohibit manufacturer copay assistance for government-program beneficiaries. The Bridge $50 copay is the path, not the card.
What BMI do I need to qualify for the Medicare GLP-1 Bridge?⌄
BMI ≥35 at therapy initiation qualifies on its own (Pathway 1). BMI ≥30 qualifies with HFpEF, uncontrolled hypertension, or CKD stage 3a or higher (Pathway 2). BMI ≥27 qualifies with prediabetes, previous heart attack, previous stroke, or symptomatic peripheral artery disease (Pathway 3).
Does current BMI or starting BMI matter for the Bridge?⌄
Starting BMI — BMI at the time you initiated GLP-1 therapy — is what CMS uses. If you started at BMI 37 in 2024 and you’re at BMI 34 today, you still qualify under Pathway 1.
Is Foundayo covered by Medicare Part B?⌄
No. Part B covers drugs administered in clinical settings (infusions, injections given by a provider in-office). Foundayo is a self-administered oral tablet, so Part B isn’t the coverage pathway. Part D is.
What happens when the Medicare GLP-1 Bridge ends on December 31, 2027?⌄
The Bridge runs through December 31, 2027 (18 months) — CMS extended it because BALANCE did not meet its 80% Part D sponsor participation threshold for 2027. After December 2027, watch for BALANCE 2028 announcements during fall 2027 open enrollment (October 15–December 7, 2027). CMS will decide whether to run a new BALANCE participation round for 2028.
How much will Foundayo cost under the 2027 BALANCE Model?⌄
Enhanced Alternative and Employer Group Waiver Plans participating in BALANCE must cap cost-sharing at $50/month during the initial coverage phase. Basic Alternative and Actuarially Equivalent Standard plans can cap at up to $125/month. All plan types can charge up to $245 plus dispensing fee during the deductible phase. Defined Standard plans are not eligible to participate.
What if my doctor sends the Bridge prior authorization to the wrong place?⌄
The Bridge uses a single central processor (BIN 028918, PCN MEDDGLP1BR), not your Part D plan. If your provider submits the PA to your Part D plan by mistake, CMS has asked plans to return a message directing providers to the central processor. This introduces delay. Bring the CMS Bridge FAQ to your appointment to get the PA submitted correctly the first time.
Does the Medicare GLP-1 Bridge cover compounded semaglutide or compounded tirzepatide?⌄
No. The Bridge drug list is limited to specific FDA-approved formulations: Foundayo, Wegovy (injection and tablets), and the Zepbound KwikPen. Compounded GLP-1s from telehealth providers are not on the Bridge drug list.
I have VA or TRICARE. Can I use the Medicare Bridge?⌄
VA and TRICARE beneficiaries are excluded from the commercial Foundayo Savings Card. Bridge eligibility depends on whether you’re also enrolled in an eligible Medicare Part D plan type. If VA or TRICARE is your only coverage and you don’t have Medicare Part D, you don’t have a Bridge pathway. Check with your benefits administrator for any formulary-based coverage.
Can I stack a manufacturer coupon or GoodRx card on my Bridge copay?⌄
No. CMS has been explicit: Bridge claims are processed by the central processor and coupons or discount programs cannot be applied. The $50 copay is the $50 copay.
What’s the difference between the Medicare GLP-1 Bridge and the BALANCE Model?⌄
The Bridge is an 18-month (July 2026–December 2027) nationwide program that every eligible Part D beneficiary can access without their plan opting in. BALANCE did not launch for Medicare Part D in 2027 — the 80% sponsor participation threshold was not met. BALANCE is the longer-term model that may launch for Medicare Part D in 2028 if CMS runs a new participation round.
How do I appeal if the Bridge denies my Foundayo prior authorization?⌄
You have 65 calendar days from the date of the denial notice to file a redetermination request. The plan must respond within 7 calendar days for a standard drug appeal (72 hours for expedited, 14 days for a payment appeal). If denied again, request a Reconsideration by an Independent Review Entity within 65 calendar days. The process has five levels total, ending with federal court review.
Why We Built This Page the Way We Did
Most “Does Medicare cover Foundayo” pages stop at the first answer: “no, but maybe starting July 1.” That’s not useful. The useful page answers which plan types qualify and which don’t, explains the three clinical pathways with the nuances most pages get wrong, tells you what the $50 actually costs you in context (TrOOP, LIS, deductibles), maps the risk that BALANCE doesn’t launch in 2027, and gives you the A1C test tip that most pages leave out.
We also route Medicare-eligible readers to Medicare — not to our affiliates — when Medicare is the clearly better path. We earn commissions from Sesame Care and SHED. Those commissions don’t change our routing logic for someone who qualifies for $50/month through a federal program.
Still Not Sure Which GLP-1 Program Is Right for You?
Sources
Primary:
- CMS Medicare GLP-1 Bridge FAQ — cms.gov/medicare/coverage/prescription-drug-coverage/medicare-glp-1-bridge
- CMS BALANCE Model page — cms.gov/priorities/innovation/innovation-models/balance
- CMS BALANCE Part D Plans Request for Applications — cms.gov/priorities/innovation/files/balance-part-d-plans-rfa.pdf
- CMS Part D Redetermination rules — cms.gov/medicare/appeals-grievances/prescription-drug/redetermination-part-d-plan-sponsor
- CMS BALANCE Model press release, December 23, 2025
- FDA approval letter for Foundayo (orforglipron), April 1, 2026
- FDA-approved Foundayo prescribing information
- Eli Lilly Foundayo coverage and savings page — foundayo.lilly.com/coverage-savings
- Eli Lilly Foundayo Savings Card terms and conditions
Secondary analysis:
- KFF brief: “What to Know About the BALANCE Model for GLP-1s in Medicare and Medicaid”
- KFF Quick Take: “What Medicare’s Temporary Program Covering GLP-1s for Obesity Means for Beneficiaries”
- Public Citizen analysis: “Off-BALANCE? Trump’s Obesity Drug Demo May Not Live Up To The Hype”
Affiliate and editorial disclosure: The RX Index earns commissions when readers sign up with some of the telehealth providers we mention, including Sesame Care and SHED. These partnerships do not influence our editorial recommendations. We verified all pricing and program information independently before publishing, and we route Medicare-eligible readers to the Medicare pathway first whenever it’s the best option for them. When Medicare is genuinely the cheapest and cleanest path, we say so — even when it costs us the click.
The RX Index is a pricing intelligence and comparison resource for GLP-1 telehealth providers. This page is for informational purposes only and is not medical advice. Consult your healthcare provider before starting any medication.