Insurance Guide · Last verified: May 22, 2026
Does CVS Caremark Cover Wegovy? 2026 Coverage, PA & The “Covered But $1,300” Problem
Published: · Last updated:
By The RX Index Editorial Team — a pricing intelligence and comparison resource for GLP-1 telehealth providers · Next scheduled review: August 22, 2026
Does CVS Caremark cover Wegovy? Often yes. CVS Caremark prefers Wegovy on its Standard Control, Advanced Control, and Value formularies effective July 1, 2025, and Wegovy continues as the preferred GLP-1 for weight loss through 2026. But three things actually decide your coverage: (1) whether your employer’s plan includes weight-loss-medication coverage at all — roughly 1 in 3 employer-sponsored lives on Caremark don’t; (2) whether you clear prior authorization; and (3) what your plan’s cost-sharing looks like — because “covered” doesn’t automatically mean cheap.
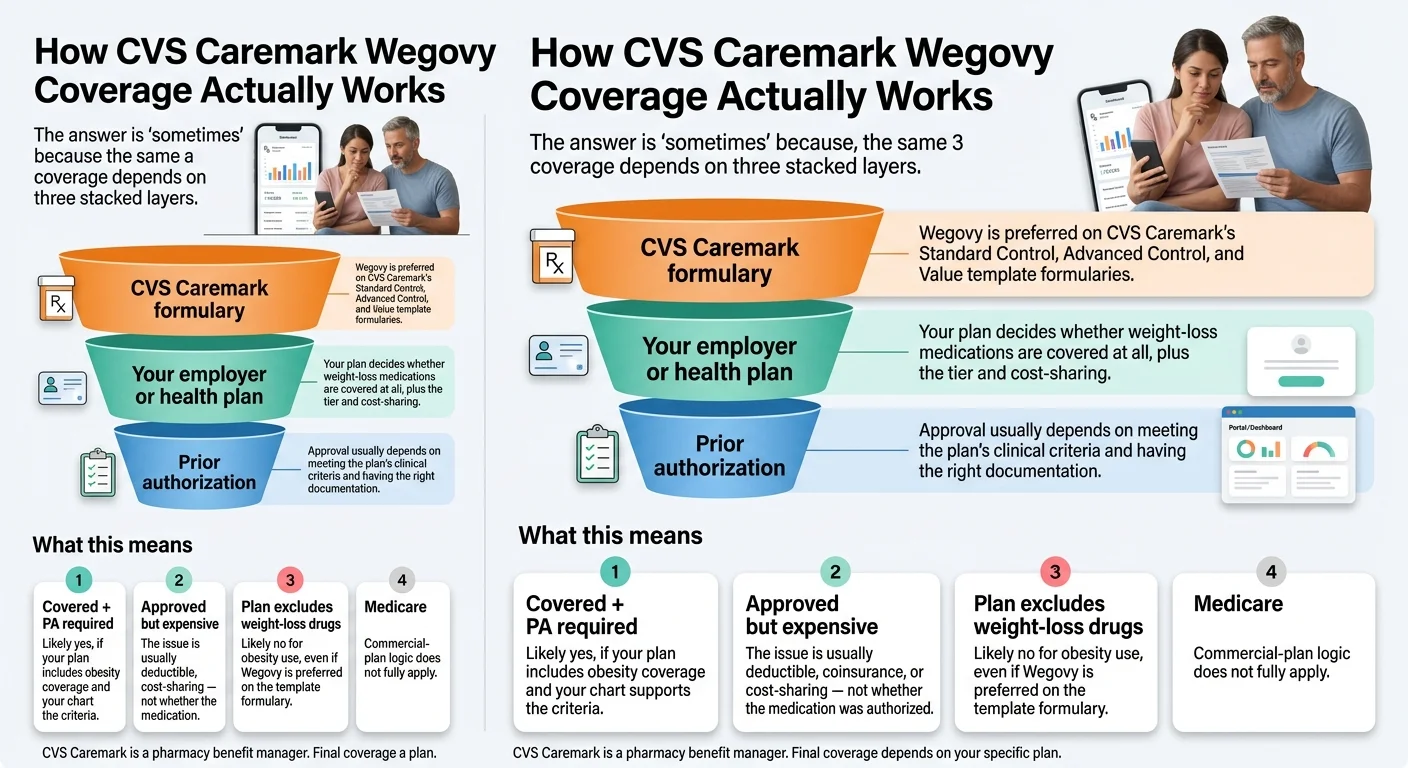
CVS Caremark is a pharmacy benefit manager. Final coverage depends on your specific plan design.
CVS Caremark Wegovy verdict at a glance
Find your situation in the table to jump straight to the right answer.
| Your situation | Likely answer | Your next move |
|---|---|---|
| CVS Caremark card, standard commercial plan | Wegovy is likely preferred; PA usually required | Check the Caremark drug-cost tool for your exact copay |
| HR confirms your plan excludes weight-loss drugs | Your plan won’t pay | Ask about the cardiovascular indication or compare cash-pay routes |
| Caremark tool says "Covered — PA required" | Coverage is possible; documentation decides it | Build the PA checklist below before your doctor submits |
| PA approved, but the pharmacy quoted $1,300+ | Likely an unmet deductible on an HDHP | Ask if the price counts toward your deductible/OOP max |
| You were switched off Zepbound | Wegovy is now your plan’s preferred GLP-1 | Many plans transfer the PA dates; doctor still must send a new Rx |
| Medicare Part D | Standard rules differ — Bridge program may help | See the Medicare GLP-1 Bridge section below |
Want the answer specific to your plan, without making the calls yourself?
Ro’s free GLP-1 Insurance Coverage Checker contacts your insurance plan, confirms coverage details, and emails you a personalized report — including whether prior authorization is required and what your expected cost looks like. No charge, no Ro signup required.
Check My Wegovy Coverage with Ro (Free) → (sponsored affiliate link, opens in a new tab)First, the thing nobody explains: CVS Caremark is not your insurance
CVS Caremark is a Pharmacy Benefit Manager (PBM) — the middle layer between you, the pharmacy, and your insurance plan. Your employer or health insurer hires CVS Caremark to manage which drugs are covered, how much you pay, and what paperwork is required. The card in your wallet might say Aetna, Blue Cross, or any other carrier. If Caremark appears on it, Caremark sets the prescription rules.
This single point of confusion produces about half the frustration people have with CVS Caremark and Wegovy. Three different parties decide your coverage:
- CVS Caremark decides which drugs are on the template formulary, the prior authorization rules, and the pharmacy network.
- Your employer (or health plan) decides whether weight-loss medications are a covered benefit at all, whether to opt into the standard template formulary or customize it, and how to tier copays.
- The pharmacy decides nothing — it just processes the claim using the rules Caremark and your employer set.
Two people holding identical-looking CVS Caremark cards can get totally different answers because their employers made different benefit choices. That isn’t Caremark being inconsistent. That’s how the system is designed.
How to tell if CVS Caremark manages your pharmacy benefits
- Flip your insurance card over. Look for “Caremark,” “CVS Caremark,” or an RxBIN tied to CVS Caremark.
- Log into your HR benefits portal — there’s usually a line that reads “Pharmacy benefits administered by CVS Caremark.”
- If you’ve been filling prescriptions through caremark.com or the CVS Caremark app, you’re a Caremark member.
Does CVS Caremark cover Wegovy in 2026?
Yes. CVS Caremark prefers Wegovy 2.4 mg injection on its Standard Control, Advanced Control, and Value formularies effective July 1, 2025, and that preference continues through 2026. Your specific plan still has to opt into weight-loss-medication coverage, and you still have to clear prior authorization.
What changed in July 2025
For years, CVS Caremark covered multiple GLP-1 weight-loss drugs at the preferred tier — Saxenda, Wegovy, Qsymia, and Zepbound. That ended on July 1, 2025. CVS Caremark struck a preferred-pricing deal with Novo Nordisk that designated Wegovy as the preferred GLP-1 for obesity and removed Zepbound from the three standard template formularies. CVS Caremark’s stated reason: preferring one product drives competition and brings prices down.
If you had a Zepbound prior authorization in June 2025, many plans automatically transferred the PA dates to Wegovy when the change took effect. Your doctor still had to send a new Wegovy prescription, but the PA paperwork carried over on most plans. Confirm with your specific plan if you’re not sure. (See also: Does CVS Caremark cover Zepbound?)
What “preferred” usually means for your wallet
- Lower copay tier. Wegovy often lands at Tier 2 on plans that include weight-loss coverage.
- Smoother prior authorization. Plans usually apply Caremark’s standard PA criteria rather than custom criteria that may be stricter.
- No step therapy at the template level. You don’t have to fail a cheaper drug first to get Wegovy. Some employers do add step therapy on top — more on that in our step therapy guide.
Where Wegovy stands on each Caremark formulary
| CVS Caremark formulary | Wegovy status (July 1, 2025 → 2026) | Zepbound status |
|---|---|---|
| Standard Control | Preferred GLP-1 for obesity | Not included |
| Advanced Control | Preferred GLP-1 for obesity | Not included |
| Value | Preferred GLP-1 for obesity | Not included |
| Custom employer/union formularies | Varies by plan sponsor | May still include Zepbound |
| 2026 employer add-on tier (plans that previously excluded GLP-1s) | Available with patient copays up to $200/month | Available with patient copays up to $200/month |
Source: CVS Caremark official GLP-1 formulary page; CVS spokesperson statement, October 2025. Verified May 22, 2026.
What “covered” actually means (the part that explains the $1,300 problem)
“Covered” is one word doing four different jobs. It can mean the drug is on the formulary, that prior authorization was approved, that the drug is preferred (better tier), or that a non-insurance discount is being shown. None of those guarantees a low price at the pharmacy counter. This single ambiguity causes most “covered but $1,300” surprises.
The four versions of “covered”
| What the system says | What it actually means | What it does NOT guarantee |
|---|---|---|
| "On formulary" | The drug is on Caremark’s list of covered medications | That your specific employer plan includes weight-loss meds |
| "Preferred" | Better formulary position than alternatives | A low out-of-pocket cost |
| "PA approved" | Caremark accepted the clinical reason for the drug | That your deductible is met or your coinsurance is low |
| "Discount price shown" | A discount card or third-party tool is giving you a lower price than retail | That this price counts toward your plan’s actual benefit |
Why your PA can be approved and the pharmacy can still quote $1,300
Five common reasons:
- You’re on a high-deductible health plan (HDHP) and the deductible isn’t met. Some CVS Caremark-administered HDHPs removed weight-loss medications from their preventive drug list, which means members pay toward the deductible first — even when the drug is covered. Ask whether your Wegovy claim is subject to the deductible.
- You’re paying coinsurance, not a flat copay. A 30% coinsurance on Wegovy’s list price is hundreds of dollars per month — even though the drug is “covered.”
- The pharmacy quoted you a discount-card price, not your plan’s price. Sometimes the lowest price shown at checkout is from a third-party discount tool rather than your actual benefit. Those discounts usually don’t apply toward your deductible.
- Wrong product or wrong NDC. Wegovy comes in multiple forms (injection pen, oral tablets, Wegovy HD 7.2 mg). If your formulary covers one form and your prescription is for a different form, the price changes drastically.
- The 2026 $200 employer copay tier. Some employers chose a 2026 Caremark cost-sharing option with patient copays up to $200 when they added weight-loss GLP-1 coverage. It’s plan-sponsor-specific, not automatic.
How to find out which version of “covered” applies to you
Call CVS Caremark member services. Ask these four questions in order:
- “Is my Wegovy claim on benefit, or am I being shown a discount price?”
- “Has my prior authorization been approved? If yes, what’s my exact copay or coinsurance?”
- “Has my deductible been met for this plan year? Does this Wegovy payment apply to it?”
- “Does the payment count toward my out-of-pocket maximum?”
If they can’t answer those clearly, ask for a supervisor or request the answers in writing. You’re allowed to request a written coverage determination.
How to check your exact CVS Caremark Wegovy coverage in 10 minutes
Log into caremark.com or the CVS Caremark app, search “Wegovy” in the drug cost and coverage tool, screenshot the result, then confirm with HR whether your employer includes weight-loss-medication coverage. If you’d rather not make the phone calls yourself, Ro’s free Insurance Coverage Checker reaches out to your plan on your behalf and emails you a personalized report.
Step 1
Use Caremark’s drug cost and coverage tool
Step 2
Confirm with HR
Step 3
Call CVS Caremark with the right questions
Step 4
Or have Ro do it for you
Free. No commitment to see the result.
CVS Caremark’s Wegovy prior authorization: exactly what they want
Prior authorization (PA) is the paperwork your doctor sends to CVS Caremark proving you medically qualify for Wegovy. The core requirements are a BMI of 30 or higher (or 27 with a qualifying weight-related condition), documentation of a structured weight-management program for at least six months, no contraindications, and confirmation that you’re not on another GLP-1. Most denials happen because of missing paperwork — not because the patient doesn’t qualify.
The actual CVS Caremark PA criteria for adults
Pulled directly from CVS Caremark’s published Wegovy PA criteria (policy 4774-C):
- Age: 18 or older
- BMI: ≥30 kg/m² (obesity), OR ≥27 kg/m² (overweight) with at least one weight-related comorbid condition
- Qualifying comorbidities: hypertension, type 2 diabetes mellitus, or dyslipidemia (high cholesterol) per FDA labeling
- Lifestyle program: documented participation in a comprehensive weight-management program (typically six months) including diet, increased physical activity, and behavioral counseling
- No contraindications: no personal or family history of medullary thyroid carcinoma (MTC) or Multiple Endocrine Neoplasia syndrome type 2 (MEN 2)
- No concurrent GLP-1: you can’t be on another semaglutide product or another GLP-1 receptor agonist at the same time
What your doctor needs to send
Hand this checklist to your doctor before they submit. Missing documentation is the most common denial cause.
| Document | Why it matters |
|---|---|
| Current height, weight, BMI, and date of measurement | Caremark needs the BMI in the chart note, not just on the PA form |
| Baseline BMI before any prior weight-loss drug | If you’ve already tried something, they want the starting point |
| ICD-10 diagnosis codes | Specific codes for obesity (E66.x) and any comorbidities |
| Six months of documented diet/exercise effort | Chart notes, dietitian visits, Noom/WW receipts, supervised program records — dated and specific |
| Lab results supporting comorbidities | A1c for diabetes, lipid panel for dyslipidemia, BP readings for hypertension |
| Prior weight-loss medication history | Names, doses, duration, why stopped — satisfies any plan-added step therapy |
| Cardiovascular disease documentation | Only if pursuing the CV indication |
| Confirmation of no MTC/MEN 2 history | Standard PA form question |
| Confirmation that the patient is not on another GLP-1 | Standard PA form question |
How long the PA takes
PA timing varies by plan, submission method, and whether the request is standard or urgent. NovoCare patient guidance says PA requests can take up to 10 business days. When the PA is submitted, ask your prescriber’s office for the case number and expected decision deadline.
Renewal (continuation) criteria
CVS Caremark’s public continuation criteria for adult long-term weight reduction require at least 3 months of therapy at a stable maintenance dose and documentation that the patient lost at least 5% of baseline body weight or maintained the initial 5% weight loss. If you haven’t hit 5%, the PA can be denied for non-response — and a peer-to-peer review with your prescriber is the right next step.
One honest tradeoff before you go further
The CVS Caremark insurance path is not the fastest way to start Wegovy. A typical insurance approval takes 1–2 weeks of PA paperwork, plus another week or two of pharmacy back-and-forth. But if your plan covers Wegovy and you qualify for the PA, the insurance path is dramatically cheaper than cash — a $25/month copay with the Wegovy Savings Card vs. $349/month cash for the standard injection is $324/month saved — about $3,888 a year. If you’d rather have a team handle the paperwork while keeping the insurance-discounted price, that’s what Ro’s insurance concierge does.
Ro Body is $39 your first month, then $149/month ongoing (or as low as $74/month with an annual plan paid upfront). The membership covers provider visits, the insurance concierge, the Wegovy Savings Card activation, and ongoing care. Medication is billed separately at your insurance copay if you’re approved, or at NovoCare-matched cash-pay pricing if you pay out of pocket.
Check if Ro can help with my Wegovy PA → (sponsored affiliate link, opens in a new tab)What you’ll actually pay for Wegovy with CVS Caremark
With CVS Caremark coverage plus the Wegovy Savings Card, eligible commercially insured patients can pay as low as $25/month. Without the savings card, your copay depends on tier — typically $25 to $150/month — or you might be on the 2026 $200 employer copay tier. If you’re on a high-deductible plan and haven’t met your deductible, you may pay close to the full list price (~$1,349/month) until the deductible is hit.
Your real cost paths compared
| Path | Who it’s for | Typical out-of-pocket | Notes |
|---|---|---|---|
| CVS Caremark + Wegovy Savings Card | Commercial Caremark plan that covers Wegovy, PA approved | $0–$25/month | Card caps at $100 off 1-month, $200 off 2-month, $300 off 3-month. Not valid for Medicare/Medicaid/Tricare/VA. |
| CVS Caremark covered, savings card ineligible | Government insurance through Caremark | Plan copay/coinsurance | Often $30–$150; verify your tier |
| CVS Caremark covered, HDHP, deductible not met | High-deductible plan members | Full cost until deductible | Each payment may count toward the deductible — verify with your plan |
| 2026 employer $200 copay tier | Employers/unions that added GLP-1 coverage via this tier | $200/month | Plan-sponsor-specific; verify whether the cost counts toward your OOP max |
| Plan excludes → NovoCare Pharmacy (injection) | Anyone, no insurance needed | $349/month after intro offer; $199/month intro for first two fills through June 30, 2026 | Manufacturer-direct, mail order |
| NovoCare Pharmacy (Wegovy HD 7.2 mg) | Higher-dose patients paying cash | $399/month | Same direct channel |
| NovoCare Pharmacy (Wegovy tablets) | Needle-averse patients paying cash | $149/month for 1.5 mg and 4 mg (4 mg offer through Aug 31, 2026) | Verify current dose pricing |
| Plan excludes → Ro Body | People who want one team handling everything | $39 first month, $149/month ongoing ($74/month with annual prepay) + medication | Insurance concierge tries for coverage first; falls back to cash-pay if denied |
| Novo Nordisk Patient Assistance Program | Uninsured, income limits | Free | Application-based at NovoCare.com |
All prices verified May 22, 2026. Recheck before filling.
The Wegovy Savings Card explained
Novo Nordisk runs a manufacturer copay program through NovoCare. If you have commercial (non-government) insurance that covers Wegovy, the savings card brings your monthly copay as low as $25.
- $100 off a 1-month supply
- $200 off a 2-month supply
- $300 off a 3-month supply
Enroll at novocare.com/wegovy/savings-card.html. Important: not valid for Medicare, Medicaid, Tricare, VA, or any government insurance. Savings card payments usually don’t count toward your insurance deductible on an HDHP. See our full Wegovy Savings Card guide for enrollment steps.
Why some plans now show a $200 copay
In late 2025, CVS Caremark introduced a new cost-sharing option for employer plans that had been excluding weight-loss medications. The deal: employers and unions can opt to cover Wegovy and Zepbound for their members at a patient copay of up to $200 per 30-day supply. It’s plan-sponsor-specific, not automatic. It’s not as good as a $25 copay with the savings card. It’s a lot better than $1,300 cash.
If your CVS Caremark plan excludes weight-loss medications
About one in three CVS Caremark-managed employer plans excludes weight-loss medications entirely. If that’s you, no amount of better paperwork forces coverage. Your options:
Confirm the exclusion in writing first
Don’t take a verbal answer. Email HR or send a Caremark portal message asking for written confirmation that anti-obesity medications are excluded from your prescription benefit. You want this in writing for two reasons: appeals require documentation, and the Novo Nordisk Patient Assistance Program asks for proof that your plan doesn’t cover Wegovy.
Option 1 — The cardiovascular indication pathway
Wegovy is FDA-approved to reduce the risk of major adverse cardiovascular events in adults with established cardiovascular disease who are overweight or obese. If you qualify medically, your doctor can submit the PA under this indication instead of weight management. Caremark’s published CV pathway criteria require: documented established cardiovascular disease (previous heart attack, previous stroke, symptomatic peripheral artery disease, or prior revascularization), baseline BMI ≥27, no type 2 diabetes (Caremark routes T2D + CVD patients to Ozempic, not Wegovy, for CV risk), and current guideline-directed management and therapy (GDMT). Some employer plans that exclude “weight-loss medications” still cover medications prescribed for cardiovascular conditions.
Option 2 — Advocate during open enrollment
Employers add GLP-1 coverage every year. Send a short, specific email to your benefits team: “I’d like to request that our prescription benefit add coverage for FDA-approved anti-obesity medications during the next open enrollment. CVS Caremark introduced a cost-sharing option in 2025 that allows employers to add this coverage at a $200/month patient copay, which is meaningfully cheaper than the prior $1,000+ list price. I’d appreciate the benefits committee considering it.” You’re handing them a specific, low-cost option to add.
Option 3 — Cash-pay through NovoCare Pharmacy
Novo Nordisk’s direct-to-consumer pharmacy sells FDA-approved Wegovy at:
- $349/month for the standard injection (0.25 mg through 2.4 mg) after the intro offer
- $199/month introductory for the first two fills of 0.25 mg or 0.5 mg through June 30, 2026
- $399/month for Wegovy HD 7.2 mg
- $149/month for Wegovy tablets at 1.5 mg and 4 mg (4 mg intro runs through August 31, 2026)
Compare all self-pay routes in our cheapest Wegovy without insurance guide.
Option 4 — Cash-pay through Ro with insurance-fight backup
Ro’s pricing for FDA-approved Wegovy matches NovoCare. The membership ($39 first month, then $149/month, or as low as $74/month with annual prepay) buys you provider visits, ongoing care, and an insurance concierge that will fight for coverage first — and fall back to cash-pay if your plan refuses. One platform, three possible outcomes: covered path, PA fight, or seamless cash-pay.
Option 5 — Sesame Care for branded GLP-1 self-pay
If you want a broader branded GLP-1 menu without the membership model, Sesame Care lists Wegovy, Zepbound, Ozempic, Mounjaro, Foundayo, and Saxenda. Costco members can access lower self-pay pricing on Wegovy injections through the Sesame–Costco partnership.
Option 6 — Novo Nordisk Patient Assistance Program
For uninsured patients who meet income limits, Novo Nordisk offers free Wegovy through their Patient Assistance Program. The application is at NovoCare.com. This is the right option for low-income patients without any insurance — it requires lack of any insurance coverage, not just lack of Wegovy coverage.
If your Wegovy prior authorization is denied
Read the denial reason first — it tells you which fix applies. Missing-documentation denials are often resubmitted quickly once the right paperwork is attached. True plan-exclusion denials require a different strategy. Many fixable denials are documentation problems matched to the wrong response. See our full Wegovy denial appeal guide for letter templates and peer-to-peer request scripts.
Denial triage table
| Denial reason | What it means | Your best next move |
|---|---|---|
| BMI not documented or below threshold | The PA didn’t show a qualifying BMI | Resubmit with a recent in-clinic BMI measurement, dated and signed |
| Missing comorbidity (for BMI 27–29.9 pathway) | No qualifying condition was listed | Add updated ICD-10 codes for hypertension, T2D, or dyslipidemia with supporting labs |
| No lifestyle program documentation | The six-month effort wasn’t documented | Submit dated chart notes, dietitian visits, or program records (Noom, WW, supervised program) |
| Step therapy not completed | Your employer added step therapy | Document prior trials of phentermine, Qsymia, Contrave, or orlistat — dates, doses, outcomes, why stopped |
| Plan exclusion | Your employer doesn’t cover weight-loss meds at all | Not a PA appeal issue. Pursue the CV pathway or cash-pay options |
| Continuation denied (renewal) | Didn’t show 5% weight loss after ≥3 months at maintenance dose | Submit weight logs and chart notes; request peer-to-peer review |
| Wrong product/form/dose | The Rx is for a Wegovy form not on your formulary | Confirm the exact NDC and resubmit |
| No contraindication screen | The PA form was missing the MTC/MEN 2 and other-GLP-1 questions | Resubmit with answers; your doctor’s office can fix this quickly |
Three appeal levels
- Formulary exception / letter of medical necessity. Your doctor submits a written request explaining why Wegovy is medically necessary for you specifically, citing FDA labeling, prior treatment failures, and the specific clinical reason that addresses the denial.
- Peer-to-peer review. Your prescribing doctor calls a CVS Caremark clinical reviewer directly to discuss the case. Peer-to-peer often resolves denials faster than written appeals because the conversation can clarify documentation gaps in real time. Your provider’s office requests this by calling the number on the denial letter.
- External appeal. If internal appeals fail, you have the right to a formal external appeal through an Independent Review Organization (IRO). State insurance regulators publish overturn rates, and Wegovy appeals have been overturned in real cases when documentation supports medical necessity.
What to put in a Wegovy letter of medical necessity
Your doctor’s letter should include, in order:
- Patient identification — name, DOB, member ID.
- Current BMI and weight-related comorbidities with ICD-10 codes.
- Documented prior weight-loss attempts — medications tried with dates and outcomes, supervised programs, surgeries.
- Clinical justification for Wegovy specifically — FDA labeling, why semaglutide vs. alternatives, cardiovascular benefit if applicable, contraindications to alternative drugs.
- Direct response to the denial reason — address the specific criterion that wasn’t met.
- Statement of medical necessity signed by the prescribing physician.
Does CVS Caremark cover Wegovy for MASH?
Possibly — under a different pathway than weight loss. CVS Caremark’s public criteria include a Wegovy-injection-only pathway for noncirrhotic metabolic dysfunction–associated steatohepatitis (MASH) with moderate-to-advanced liver fibrosis (F2–F3) in adults, when prescribed by or in consultation with a gastroenterologist or hepatologist. This is separate from the weight-loss PA pathway and is only available for Wegovy injection, not Wegovy tablets.
If your plan excludes weight-loss medications but you have documented F2–F3 fibrosis from MASH, the MASH indication may be a separate path to coverage. Your gastroenterologist or hepatologist drives this submission, not your primary care doctor.
Does CVS Caremark cover Wegovy if I have type 2 diabetes?
You can still take Wegovy for weight loss if you have type 2 diabetes — it’s actually one of the qualifying comorbidities. But CVS Caremark’s published cardiovascular-risk pathway for Wegovy specifies the patient does NOT have type 2 diabetes; for T2D patients with established CVD, Caremark’s criteria route to Ozempic for CV risk reduction. Talk to your prescriber about which GLP-1 product fits both your diagnosis and your plan’s coverage rules.
Wegovy injection vs. tablets vs. HD — does CVS Caremark cover them the same?
Not necessarily. Each form has different FDA indications, and coverage rules can differ from plan to plan.
Wegovy injection (0.25 mg → 2.4 mg pens)
The most established coverage path. Preferred on the three CVS Caremark template formularies, eligible for the savings card, and the form most prior authorization templates default to. The injection has the broadest FDA indications: adult weight management, adult cardiovascular risk reduction, pediatric weight management (ages 12+), and noncirrhotic MASH with F2–F3 fibrosis.
Wegovy tablets (semaglutide oral)
FDA-approved December 22, 2025 and launched in early January 2026. Available through Ro and several other telehealth platforms. Wegovy tablets are FDA-approved for adult weight reduction/maintenance and adult cardiovascular risk reduction — not pediatric weight management or the MASH indication. CVS Caremark coverage of Wegovy tablets is rolling out plan-by-plan. Check the exact tablet dose in the Caremark drug cost tool.
Wegovy HD (semaglutide 7.2 mg injection)
FDA-approved March 19, 2026; launched in April. FDA says the 7.2 mg dose produces additional average weight reduction compared with previously approved doses. The Wegovy Savings Card covers Wegovy HD under the same program. NovoCare cash-pay pricing is $399/month.
Does the Medicare GLP-1 Bridge cover Wegovy through CVS Caremark?
Yes, beginning July 1, 2026. CMS says eligible Medicare Part D beneficiaries may access Wegovy injection and Wegovy tablets for weight reduction and maintenance through the Medicare GLP-1 Bridge at $50 for a monthly supply. This is separate from standard Medicare Part D weight-loss rules and separate from Wegovy’s cardiovascular-risk indication coverage on Part D.
Standard Medicare Part D rules
Federal law prohibits Medicare Part D from covering drugs prescribed for weight loss alone. That has been true since Part D launched. However, Medicare Part D plans (including plans administered through CVS Caremark) can cover Wegovy for cardiovascular risk reduction in adults with established cardiovascular disease and BMI ≥27, with prior authorization typically required.
If you’re on Medicare Part D through CVS Caremark and you’ve been told Wegovy isn’t covered for weight loss, ask your plan specifically about Bridge eligibility starting July 1, 2026. See our full guide: Does Medicare cover Wegovy?
Medicaid, TRICARE, and FEHB through CVS Caremark
Medicaid through CVS Caremark
Medicaid is state-administered. Some state Medicaid programs cover Wegovy for weight management; many do not. California Medi-Cal removed Wegovy from its weight-loss coverage effective January 1, 2026 — Wegovy is now only covered in California for noncirrhotic MASH or cardiovascular disease indications. See our Medicaid Wegovy coverage guide for state-by-state details.
TRICARE
TRICARE covers Wegovy, Saxenda, and Zepbound for weight management for specified beneficiary groups — including TRICARE Prime, Select, US Family Health Plan, Young Adult, Reserve Select, Retired Reserve, and Continued Health Care Benefit Program members — when clinical criteria, network-prescriber requirements, and prior authorization are met. TRICARE does not cover weight-loss medications for TRICARE For Life beneficiaries and certain other groups. Confirm your specific plan with your TRICARE pharmacy contractor. See also: Does TRICARE cover Wegovy?
Note: The Wegovy Savings Card is not valid for any government insurance.
Federal Employees Health Benefits Program (FEHB)
FEHB is a marketplace of plans from different carriers, some of which use CVS Caremark and some of which don’t. Coverage of Wegovy varies dramatically by carrier and plan year. The 2026 FEHB plan brochures list which carriers cover anti-obesity medications. If you’re a federal employee on an FEHB plan using CVS Caremark, Ro’s insurance concierge can handle the coverage paperwork.
Common CVS Caremark Wegovy scenarios
These aren’t testimonials — they’re patterns mapped from public coverage questions and the CVS Caremark policies above.
Scenario 1
PA approved, but the pharmacy quoted the full list price.
Almost always an unmet deductible on a high-deductible plan, especially when the plan removed weight-loss drugs from its preventive list. Action: call Caremark, ask whether the claim is on benefit and whether the payment counts toward the deductible and OOP max.
Scenario 2
Denied — six-month program missing.
The PA didn’t document a structured weight-management program. Action: resubmit with chart notes from your doctor’s office, dietitian visits, or program receipts (Noom, WW, supervised program). The denial is fixable.
Scenario 3
Denied — plan exclusion.
No amount of better paperwork forces coverage. Action: check the cardiovascular pathway if you have CVD without T2D, advocate during open enrollment, or move to a cash-pay route.
Scenario 4
Switched off Zepbound.
Your PA may have transferred to Wegovy automatically. Your doctor still needs to send a new Wegovy prescription. If Wegovy isn’t working as well after the switch, your provider can request a formulary exception for Zepbound based on medical necessity.
Scenario 5
Approved, $25 with savings card.
This is the goal. Activate the Wegovy Savings Card at novocare.com/wegovy/savings-card.html once your PA is approved; the pharmacy processes it alongside your insurance card.
Wegovy safety basics
Not medical advice — talk to your clinician.
Wegovy is a prescription medication. A clinician must decide whether Wegovy is appropriate for you. Per FDA labeling:
- Wegovy should not be used with other semaglutide-containing products or other GLP-1 receptor agonists.
- Wegovy is contraindicated in patients with a personal or family history of medullary thyroid carcinoma (MTC) or Multiple Endocrine Neoplasia syndrome type 2 (MEN 2).
- Labeling includes warnings for pancreatitis, gallbladder disease, hypoglycemia (especially in patients with type 2 diabetes), acute kidney injury, severe gastrointestinal adverse reactions, hypersensitivity reactions, diabetic retinopathy complications, heart rate increase, suicidal ideation, and pulmonary aspiration during anesthesia or deep sedation.
This page covers coverage and access — not medical guidance on whether Wegovy is right for you.
What we actually verified for this page
| Claim | Source | Verified |
|---|---|---|
| Wegovy is CVS Caremark’s preferred GLP-1; Zepbound removed from Standard Control, Advanced Control, Value formularies July 1, 2025 | business.caremark.com (official) | May 22, 2026 |
| CVS Caremark states ~1 in 3 employer-sponsored lives lack weight-loss medication coverage | CVS Caremark official communication | May 22, 2026 |
| 2026 cost-sharing option with patient copays up to $200 for employers adding GLP-1 coverage | CVS spokesperson statement reported in industry press | May 22, 2026 |
| Wegovy adult PA criteria (BMI, comorbidity, lifestyle program, contraindications) — policy 4774-C | CVS Caremark Wegovy PA criteria policy 4774-C | May 22, 2026 |
| CV indication pathway: no T2D, BMI ≥27, established CVD, GDMT documentation | CVS Caremark Wegovy PA criteria policy 4774-C | May 22, 2026 |
| MASH pathway: Wegovy injection only, F2–F3 fibrosis, GI/hepatology prescriber | CVS Caremark Wegovy PA criteria policy 4774-C | May 22, 2026 |
| Continuation criteria: ≥3 months at stable maintenance dose, ≥5% baseline weight loss | CVS Caremark Wegovy PA criteria policy 4774-C | May 22, 2026 |
| Wegovy Savings Card: as low as $25/month, $100 max savings per 1-month fill | NovoCare Wegovy Savings Offer page | May 22, 2026 |
| NovoCare Pharmacy: $349/mo standard injection (after $199 intro for 0.25/0.5 mg through June 30, 2026); $399/mo HD; $149/mo tablets at 1.5/4 mg | NovoCare.com pharmacy page | May 22, 2026 |
| Wegovy HD FDA approval March 19, 2026 | FDA approval announcement | May 22, 2026 |
| Wegovy tablets FDA approval December 22, 2025 | Novo Nordisk announcement | May 22, 2026 |
| Wegovy tablets indications: adult weight reduction/maintenance + CV risk reduction (no pediatric, no MASH) | FDA label | May 22, 2026 |
| Ro Body pricing: $39 first month, $149/month ongoing, $74/month with annual prepay | ro.co/weight-loss/pricing/ | May 22, 2026 |
| Medi-Cal removed Wegovy weight-loss coverage effective January 1, 2026 | California Medi-Cal Rx December 12, 2025 GLP-1 Coverage Considerations | May 22, 2026 |
| TRICARE covers Wegovy/Saxenda/Zepbound for weight management for specified beneficiary groups | TRICARE Newsroom | May 22, 2026 |
| Medicare GLP-1 Bridge: beginning July 1, 2026, eligible Part D beneficiaries may access Wegovy injection and tablets for weight reduction/maintenance at $50 monthly | CMS Medicare GLP-1 Bridge page | May 22, 2026 |
What we can’t verify for you specifically
These depend on your exact situation and you’ll need to confirm them: your exact CVS Caremark plan’s coverage of Wegovy, whether your employer customized the formulary or excluded weight-loss meds, your specific copay or coinsurance amount, your current deductible status, your pharmacy’s live inventory, your final prior authorization outcome, your state’s specific Medicaid GLP-1 rules, and any unannounced plan amendments. For all of these, use the CVS Caremark drug cost tool, your HR benefits team, or Ro’s free Coverage Checker.
Frequently asked questions
Does CVS Caremark cover Wegovy in 2026?
Often yes. CVS Caremark prefers Wegovy on its Standard Control, Advanced Control, and Value template formularies effective July 1, 2025, and that preference continues through 2026. Your specific plan still needs to opt into weight-loss-medication coverage, and you still need prior authorization approval.
How much does Wegovy cost with CVS Caremark?
With CVS Caremark coverage plus the Wegovy Savings Card, eligible commercially insured patients can pay as low as $25 per month. Without the savings card, copays typically range from $25 to $150/month depending on your plan’s tier. Some 2026 employer plans use a $200/month copay tier; high-deductible plan members may pay the full list price until their deductible is met.
Why is Wegovy “covered” but the pharmacy still says $1,300?
The most common reason is an unmet deductible on a high-deductible health plan. Some CVS Caremark-administered HDHPs removed weight-loss medications from their preventive drug list, which means HDHP members pay toward the deductible first. Other causes include coinsurance vs. a flat copay, the pharmacy showing a discount-card price rather than your plan’s actual price, or a wrong product/NDC.
Does CVS Caremark require step therapy for Wegovy?
CVS Caremark’s standard PA policy does not require step therapy on Wegovy as the preferred GLP-1. Individual employer plans can add step therapy on top, requiring you to try cheaper weight-loss medications first. Check your plan-specific PA form to confirm.
Why did CVS Caremark drop Zepbound?
CVS Caremark removed Zepbound from its Standard Control, Advanced Control, and Value formularies on July 1, 2025, after negotiating a preferred-pricing agreement with Novo Nordisk for Wegovy. CVS Caremark cited Wegovy’s longer track record and its FDA approval for cardiovascular risk reduction. Some CVS Caremark-managed plans use custom designs that may still include Zepbound.
Is Wegovy the same as Zepbound?
No. Wegovy is semaglutide; Zepbound is tirzepatide. They are different drugs. Your clinician should decide whether a switch between them is medically appropriate.
Can I appeal a CVS Caremark Wegovy denial?
Yes. You have three levels of recourse: a formulary exception with a letter of medical necessity from your physician, a peer-to-peer review where your physician speaks directly with a CVS Caremark clinical reviewer, and a formal external appeal through an Independent Review Organization if internal appeals fail. Match your response to the specific denial reason on the letter.
What if my employer excludes weight-loss medications?
About one in three CVS Caremark-managed employer plans exclude weight-loss medications entirely. Your options are: pursue Wegovy under the cardiovascular risk reduction indication if you have established heart disease (and no type 2 diabetes), advocate for coverage with HR during open enrollment, use cash-pay through NovoCare ($349/month for the standard injection) or a telehealth platform with insurance backup like Ro, or apply to the Novo Nordisk Patient Assistance Program if you’re uninsured and meet income limits.
Does the Medicare GLP-1 Bridge cover Wegovy?
Yes. CMS says beginning July 1, 2026, eligible Medicare Part D beneficiaries may access Wegovy injection and Wegovy tablets for weight reduction and maintenance through the Medicare GLP-1 Bridge at $50 for a monthly supply. This is separate from standard Medicare Part D rules.
Does CVS Caremark cover Wegovy for MASH?
Possibly — under a separate pathway. CVS Caremark’s published criteria include a Wegovy-injection-only pathway for noncirrhotic MASH with moderate-to-advanced liver fibrosis (F2–F3) in adults, prescribed by or in consultation with a gastroenterologist or hepatologist. This is distinct from the weight-loss PA pathway.
Does CVS Caremark cover Wegovy if I have type 2 diabetes?
Wegovy can be prescribed for weight loss in patients with type 2 diabetes — T2D is one of the qualifying comorbidities. But Caremark’s published cardiovascular-risk pathway for Wegovy specifies the patient does NOT have type 2 diabetes; for T2D patients with established CVD, Caremark’s criteria route to Ozempic for cardiovascular risk reduction. Talk to your prescriber about which GLP-1 fits both your diagnosis and your plan’s rules.
Does Wegovy tablet coverage transfer from Wegovy pen coverage?
Not automatically. Wegovy tablets and Wegovy injection are different products with different indications and different plan-level coverage. Always search the exact product, form, and dose in the Caremark drug cost tool before assuming coverage transfers.
Does CVS Caremark cover Wegovy HD?
When it’s on your plan’s formulary, yes. Wegovy HD 7.2 mg was FDA-approved on March 19, 2026 and is eligible for the Novo Nordisk savings card under the same program as the original injection. NovoCare cash-pay pricing is $399/month.
How long does the prior authorization take?
PA timing varies by plan and submission method. NovoCare patient guidance says PA requests can take up to 10 business days. Ask your prescriber’s office for the case number and expected decision deadline when the PA is submitted.
Do I have to fill Wegovy at a CVS pharmacy?
No. CVS Caremark members can fill prescriptions at any in-network pharmacy, including non-CVS retail pharmacies, mail-order pharmacies, and specialty pharmacies. Your plan’s network is listed in the CVS Caremark portal.
Can Ro submit a prior authorization to CVS Caremark for me?
Yes — Ro says its insurance concierge handles prior authorization paperwork for Ro Body members. This is included in the $39 first-month / $149-ongoing membership (or as low as $74/month with annual prepay); medication is billed separately based on your insurance copay or cash-pay price.
Your action plan
If you took nothing else from this page, do these five things in this order:
- Sign into caremark.com or the CVS Caremark app. Search “Wegovy” in the drug cost and coverage tool. Screenshot the result.
- Email HR. Ask whether anti-obesity medications are a covered benefit and whether your plan uses a standard or custom CVS Caremark formulary.
- Send your doctor the PA checklist in the prior authorization section above. The right paperwork the first time is the difference between a 5-day approval and a 5-week denial spiral.
- Activate the Wegovy Savings Card at novocare.com/wegovy/savings-card.html if you have commercial insurance. This is the single biggest lever for getting your copay down to $25.
- If your plan excludes weight-loss meds, or you want help with the paperwork, use Ro’s free GLP-1 Insurance Coverage Checker to confirm in writing, then decide whether Ro’s insurance concierge or a cash-pay path makes more sense for you.
Still not sure which GLP-1 program is right for you?
If none of this fits your situation cleanly — you’re not sure which provider to use, your plan is unusual, or you’re considering both Wegovy and Zepbound — our free 60-second matching quiz routes you by insurance type, state, budget, and whether you want brand-name or alternative options.
No sign-up to see the match. Routes by insurance type, state, and budget.
About this page
This page is maintained by The RX Index Editorial Team. The RX Index is a pricing intelligence and comparison resource for GLP-1 telehealth providers. We verify formulary status, prior authorization criteria, and pricing from primary sources — CVS Caremark, Novo Nordisk/NovoCare, the FDA, CMS, TRICARE, and the published policies of each provider mentioned — and we update this page on the quarterly schedule listed in the verification table above.
We are not licensed clinicians, insurance agents, or financial advisors. Nothing on this page is medical advice or a guarantee of coverage. Confirm your specific plan’s coverage with CVS Caremark and your benefits administrator before making any treatment decisions.
Affiliate disclosure: Links to Ro and Sesame Care in this article are affiliate links. The RX Index may earn a commission if you sign up through them, at no additional cost to you. We feature Ro on this page because Ro offers FDA-approved Wegovy with an insurance concierge that handles CVS Caremark prior authorizations. Sesame Care appears as a secondary option for branded GLP-1 self-pay access. We do not feature compounded GLP-1 providers on this page because the reader’s intent is FDA-approved branded Wegovy. Compensation does not influence whether or how we describe providers; we verify the facts independently.
Last verified: May 22, 2026. Next scheduled review: August 22, 2026 (or sooner if CVS Caremark, Novo Nordisk, CMS, or a featured provider announces a material change).
Wegovy® is a registered trademark of Novo Nordisk. CVS Caremark® is a registered trademark of CVS Health. This page is for educational information only and is not medical, legal, or financial advice.
Related guides
- Does CVS Caremark cover Zepbound?
- Does Express Scripts cover Wegovy?
- Does Cigna cover Wegovy?
- Aetna Wegovy prior authorization guide
- Does Medicare cover Wegovy?
- Wegovy Savings Card: who qualifies and what it costs
- How to appeal a Wegovy denial
- Cheapest ways to get Wegovy without insurance
- Zepbound vs. Wegovy: which is better for weight loss?