Insurance Coverage Guide · Last verified: May 14, 2026 · Updated monthly
Does Express Scripts Cover Mounjaro? (2026 Coverage, PA Rules & Real Cost)
Published: · Last reviewed:
By The RX Index Editorial Team
Verified against: 2026 ESI National Preferred Formulary · Express Scripts Medicare PDP 2026 · TRICARE/DoD Mounjaro PA Form · Cigna/Evernorth GLP-1 PA Policy · Lilly Mounjaro Savings Card Terms
The 60-second answer
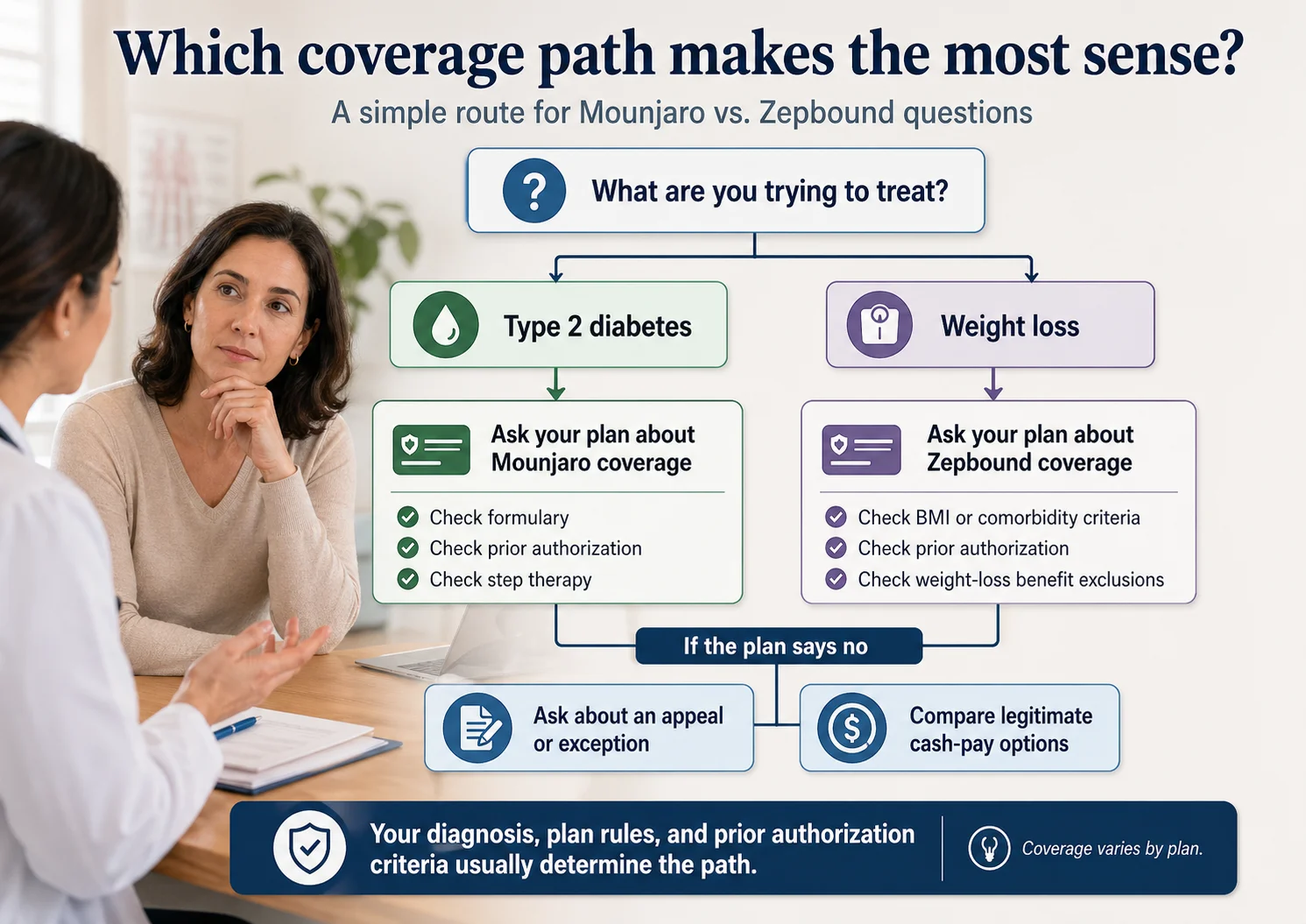
Yes — Express Scripts can cover Mounjaro for type 2 diabetes, and many Express Scripts-administered plans require prior authorization. Mounjaro appears as MOUNJARO [INJ] on the 2026 Express Scripts National Preferred Formulary, and the Express Scripts Medicare PDP lists it as Tier 2 with PA and a quantity limit. Your specific plan still controls coverage, restrictions, and cost.
With commercial Express Scripts coverage plus the Lilly Mounjaro Savings Card, eligible patients can pay as little as $25 a month. Without the savings card, your plan’s brand-tier copay typically runs $25–$100. The list price is around $1,112 per 28-day supply (4 pens).
The single biggest reason people get denied: asking Express Scripts to cover Mounjaro for weight loss. Mounjaro is FDA-approved only for type 2 diabetes. If weight loss is your real goal, the right covered alternative is Zepbound — same molecule, different FDA label, different PA path.
Your situation → what to expect
Find yourself in this table first. The rest of the guide goes deeper on each path.
| Your situation | Does Express Scripts cover Mounjaro? | Likely monthly cost (2026) | Your next step |
|---|---|---|---|
| Commercial Express Scripts + type 2 diabetes | Often yes, with PA | $25–$100 plan copay → as low as $25 with Lilly Savings Card stacked on top | Have your prescriber submit the diabetes PA + activate the savings card before pickup |
| Commercial Express Scripts + weight loss only (no T2D) | No for Mounjaro | N/A — denial expected | Ask your prescriber whether Zepbound fits under your plan's weight-management benefit |
| Express Scripts Medicare PDP + type 2 diabetes | Yes — Tier 2 with PA + quantity limit | Plan copay only (savings card not eligible for Medicare) | Submit PA; consider the Medicare Prescription Payment Plan to spread costs |
| TRICARE through Express Scripts + type 2 diabetes | Yes, with PA + medical-necessity form | $0–$44 at military pharmacy or Home Delivery | See our TRICARE GLP-1 coverage guide |
| Commercial plan that doesn't cover Mounjaro | No unless exception approved | As low as $499/month via Lilly savings card 'commercial-without-coverage' path | File a formulary exception; Lilly's savings card covers this scenario if you have commercial drug insurance |
| Uninsured, no Express Scripts plan | N/A | ~$1,112 list price; ~$1,096.59 GoodRx as of May 14, 2026 | Call Lilly Support Services (1-800-LillyRx) and check current Lilly Cares eligibility |
Sources: Express Scripts 2026 National Preferred Formulary; Express Scripts Medicare PDP 2026 Formulary; Lilly Mounjaro Savings Card Terms (current card expires Dec 31, 2026); Lilly Mounjaro pricing disclosure; GoodRx Mounjaro cash price as of May 14, 2026.
Not sure which row you’re in?
Ro’s free GLP-1 Insurance Coverage Checker runs your specific Express Scripts plan, tells you whether Mounjaro or Zepbound is covered, and shows your estimated monthly cost.
Check your GLP-1 coverage with Ro → (sponsored affiliate link, opens in a new tab)What we actually verified for this guide
We separated general formulary evidence from personal plan coverage so you know exactly what’s proven and what isn’t.
| Claim checked | What we verified | What it does and does not prove |
|---|---|---|
| Express Scripts commercial formulary | 2026 NPF lists MOUNJARO [INJ] in the diabetes-medication section | Proves Mounjaro appears on the abbreviated NPF; does not prove your plan covers it |
| Commercial plan caveat | The NPF document states it is abbreviated, not all-inclusive, and does not guarantee coverage | Why members must run Price a Medication for personal coverage |
| Express Scripts Medicare PDP | The 2026 Medicare PDP formulary lists Mounjaro as Tier 2 with PA and QL | Applies to that PDP formulary; specific Medicare Advantage rules can differ |
| Public Mounjaro PA form | The public, downloadable Mounjaro PA form on the Express Scripts site is the TRICARE/DoD form | Don't apply that hard-stop logic to all commercial plans |
| Lilly Mounjaro Savings Card | $25 path requires commercial insurance that covers Mounjaro; $499 path requires commercial insurance that doesn't cover Mounjaro | Not an uninsured workaround. Not eligible for Medicare, Medicaid, TRICARE, or VA. |
| CMS Medicare GLP-1 Bridge | Covers Foundayo, Wegovy injection/tablets, and Zepbound KwikPen from July 1, 2026 through Dec 31, 2027 | Helps Medicare weight-management intent, but Mounjaro is NOT on the Bridge eligible-drug list |
| Zepbound formulary status | Zepbound pens appear on the 2026 ESI National Preferred Formulary; Zepbound vials appear on the formulary exclusions list | Pens are covered if employer opted into the weight-management benefit; vials require the cash/LillyDirect path |
Why “does Express Scripts cover Mounjaro?” doesn’t have one simple answer
Express Scripts decides which drugs appear on its big formulary lists. Your employer or plan sponsor decides whether your specific plan actually uses those lists, and what extra rules to layer on top. That’s the split most coverage articles skip — and it’s why two people with “Express Scripts” cards can get totally different answers about the same drug.
Express Scripts is a PBM, not your insurance plan
Express Scripts is a pharmacy benefit manager — a company that negotiates drug prices and manages prescription benefits on behalf of insurance plans, employers, and Medicare drug plans. Express Scripts is owned by Evernorth, which is part of The Cigna Group. Your insurance card might say “Cigna” or your employer’s name — but if your prescriptions are processed by Express Scripts, they’re running your coverage decisions.
Express Scripts publishes several different formularies — a National Preferred Formulary for many commercial and employer plans, an Express Scripts Medicare PDP formulary for Part D members, and it administers the TRICARE Pharmacy Program for military beneficiaries. Mounjaro shows up on all three for type 2 diabetes, but the rules and forms are different on each one.
Then your plan sponsor — your employer, your union, or your Medicare plan — gets to make changes. They can:
- •Add extra exclusions on top of the Express Scripts formulary
- •Choose to cover or not cover weight-loss medications
- •Require enrollment in a digital health program (like Omada) for some GLP-1 coverage
- •Switch you to a specialty home-delivery pharmacy like EnGuide for injectable GLP-1s
- •Set their own copay tiers and deductibles
“Covered” can mean five different things
| What you hear | What it often really means |
|---|---|
| "Mounjaro is on the formulary" | It's eligible. PA and quantity limits may still block your fill. |
| "Covered with PA" | Your prescriber has to submit clinical proof before the plan pays. |
| "Not covered" | Could be a plan exclusion, missing PA, or wrong diagnosis code. |
| "Covered but expensive" | Your deductible isn't met yet, or you're paying coinsurance instead of a flat copay. |
| "Use mail order or EnGuide" | Your plan routes injectable GLP-1s through a specific specialty pharmacy. |
What exact source proves Mounjaro is on the Express Scripts formulary?
The 2026 Express Scripts National Preferred Formulary PDF lists MOUNJARO [INJ] in its alphabetical drug list. Express Scripts also publishes the 2026 Medicare PDP formulary that lists Mounjaro specifically as Tier 2 with prior authorization and a quantity limit. Both are public documents you can verify yourself — but neither proves your personal plan covers it.
The 2026 National Preferred Formulary (commercial/employer plans)
The NPF is the abbreviated drug list at the core of many commercial and employer Express Scripts plans (effective Jan 1 – Dec 31, 2026).
Mounjaro listing: Yes — appears as MOUNJARO [INJ]
Caveats Express Scripts prints on the document: The PDL is abbreviated; not all-inclusive; does not guarantee coverage; not all medications listed are covered by all prescription plans; check your benefit materials or member tools for plan-specific coverage and copays.
In plain English: appearing on the NPF means Mounjaro is eligible under many Express Scripts-administered plans, not that your plan will pay.
The 2026 Express Scripts Medicare PDP Formulary
Separate formulary for Express Scripts Medicare Part D members.
Mounjaro listing: Tier 2, with PA (prior authorization required) and QL (quantity limit) restrictions
Caveats: Specific plan rules can change; restrictions can be added or removed mid-year; check your specific PDP plan’s drug list
The 2026 Express Scripts Formulary Exclusions List
Mounjaro: Not on the exclusions list for 2026 ✓
Zepbound vials: On the weight-loss exclusions list, with preferred alternatives shown (liraglutide, Wegovy injection, Wegovy tablets, and Zepbound pens)
Zepbound pens: On the NPF; coverage still depends on whether your employer opted into the weight-management benefit
Is the Express Scripts Mounjaro PA form the same for every plan?
No. The public, easy-to-find Express Scripts Mounjaro prior authorization form is a TRICARE/Department of Defense form. It applies only to TRICARE pharmacy program prescriptions. Commercial, employer-sponsored, Medicare PDP, Cigna/Evernorth, and union plans can use different criteria and different submission forms. Use the TRICARE form as a warning of what your plan will likely ask for — not as universal proof.
The TRICARE/DoD Mounjaro PA decision tree
The TRICARE form uses a fixed sequence. If the answer hits a “stop” anywhere, coverage is denied — no exceptions.
Is the prescription for weight loss?
If yes: STOP. Coverage not approved. If no: continue.
Does the patient have a diagnosis of type 2 diabetes mellitus?
If no: STOP. Coverage not approved. If yes: continue.
Has the patient tried metformin (alone or in combination) and failed to achieve adequate blood sugar control?
If yes: continue to clinical-criteria approval. If no: continue to Step 4.
Has the patient experienced an adverse event with metformin that precludes its use?
If yes: continue to clinical-criteria approval. If no: continue to Step 5.
Does the patient have a contraindication to metformin?
If yes: continue to clinical-criteria approval. If no: STOP. Coverage not approved.
Source: TRICARE/Department of Defense Ozempic, Mounjaro Prior Authorization Request Form, administered through Express Scripts for TRICARE beneficiaries.
What your commercial PA submission will likely require
Based on the TRICARE form, Cigna/Evernorth’s published PA policy, and the Lilly Mounjaro PA submission guide:
An ICD-10 type 2 diabetes diagnosis code: The E11.x family — for example, E11.9 for type 2 diabetes without complications
A current A1C lab result: Confirming the diagnosis
Metformin history: Dates, doses, duration, outcome. Or documented intolerance, contraindication, or kidney function that rules it out.
Current diet and exercise documentation: Mounjaro's FDA label is 'as an adjunct to diet and exercise,' so most PAs ask
Helpful comorbidities: Hypertension, dyslipidemia, cardiovascular disease, or kidney disease that strengthen medical necessity
How long the PA process takes
| Review type | Typical timeline |
|---|---|
| Standard PA review | Often 1–3 business days from when the complete form arrives |
| Expedited review (urgent medical necessity) | Typically 24 hours |
| Internal appeal | Usually up to 30 days for a decision |
| External review | Timelines and rights vary by state |
Exact timelines live on your plan’s PA decision letter and your denial letter.
A short, honest note: If your prescriber isn’t experienced with Mounjaro PAs, isn’t responsive on paperwork, or you’ve already been denied — your fastest path to approval is often a telehealth platform with an in-house insurance concierge. Ro Body membership is $39 for the first month, then $149/month (or as low as $74/month with annual plan paid upfront). If your PCP is willing and competent on PA paperwork, skip Ro and save the $149.
See if Ro Body fits your PA situation → (sponsored affiliate link, opens in a new tab)How to check if your specific Express Scripts plan covers Mounjaro in 5 minutes
The only definitive answer for your plan comes from Express Scripts itself, through the Price a Medication tool inside your member account. The tool shows whether Mounjaro is covered under your plan, what tier it’s on, whether PA or quantity limits apply, and your estimated cost at different pharmacies.
Price a Medication: step-by-step
- 1
Go to express-scripts.com and log into your member account. If you don't have one, you'll need your member ID from your prescription card to register.
- 2
Click "Price a Medication" on the homepage or under the Prescriptions menu.
- 3
Type "Mounjaro" into the search bar. Select your dose (2.5 mg, 5 mg, 7.5 mg, 10 mg, 12.5 mg, or 15 mg) and quantity (typically 4 pens for a 28-day supply).
- 4
Enter your ZIP code so the tool shows pharmacy options near you.
- 5
Read the result carefully. Look for: Coverage status ("Covered," "Not covered," or "Covered with restrictions"); Restriction codes — PA (prior authorization), QL (quantity limit), ST (step therapy), AGE (age limit); Tier (1, 2, 3, or specialty); Estimated cost at retail vs. Home Delivery vs. EnGuide.
- 6
Screenshot the result. You'll want this when you call your prescriber's office to ask about the PA.
What to ask Express Scripts customer service
“I’m checking plan-specific coverage for Mounjaro, not the general formulary. Three questions: (1) Is Mounjaro covered under my plan? (2) Does it require prior authorization or quantity limits, and what’s the exact PA form my prescriber needs? (3) Does my plan cover Mounjaro for type 2 diabetes only, or also for weight management?”
What to ask your prescriber
“Express Scripts requires prior authorization for Mounjaro. Can you submit the diabetes PA with my A1C history, prior metformin documentation, current dose, and the reason Mounjaro is medically appropriate for me?”
Be specific. PA forms get rejected most often for missing documentation, not for missing eligibility.
The Express Scripts Mounjaro Coverage Prep Worksheet
Fill this in before you call Express Scripts and before your prescriber’s appointment.
| Question | Your answer |
|---|---|
| What plan are you on? (commercial, Medicare PDP, TRICARE, Cigna) | Fill in before your call |
| What's your diagnosis? (T2D, weight loss, both, unsure) | Fill in before your call |
| Have you called Express Scripts yet? What did they say? | Fill in before your call |
| Did you run Price a Medication? What was the result? | Fill in before your call |
| Is PA required? Has it been submitted? | Fill in before your call |
| Have you been denied? What was the denial reason? | Fill in before your call |
| Do you have commercial insurance (savings card eligible)? | Fill in before your call |
| Have you tried metformin? Did it work? Side effects? | Fill in before your call |
Not sure which row of the decision matrix you’re in? Take our free 60-second GLP-1 matching quiz →
What Mounjaro actually costs with Express Scripts in 2026
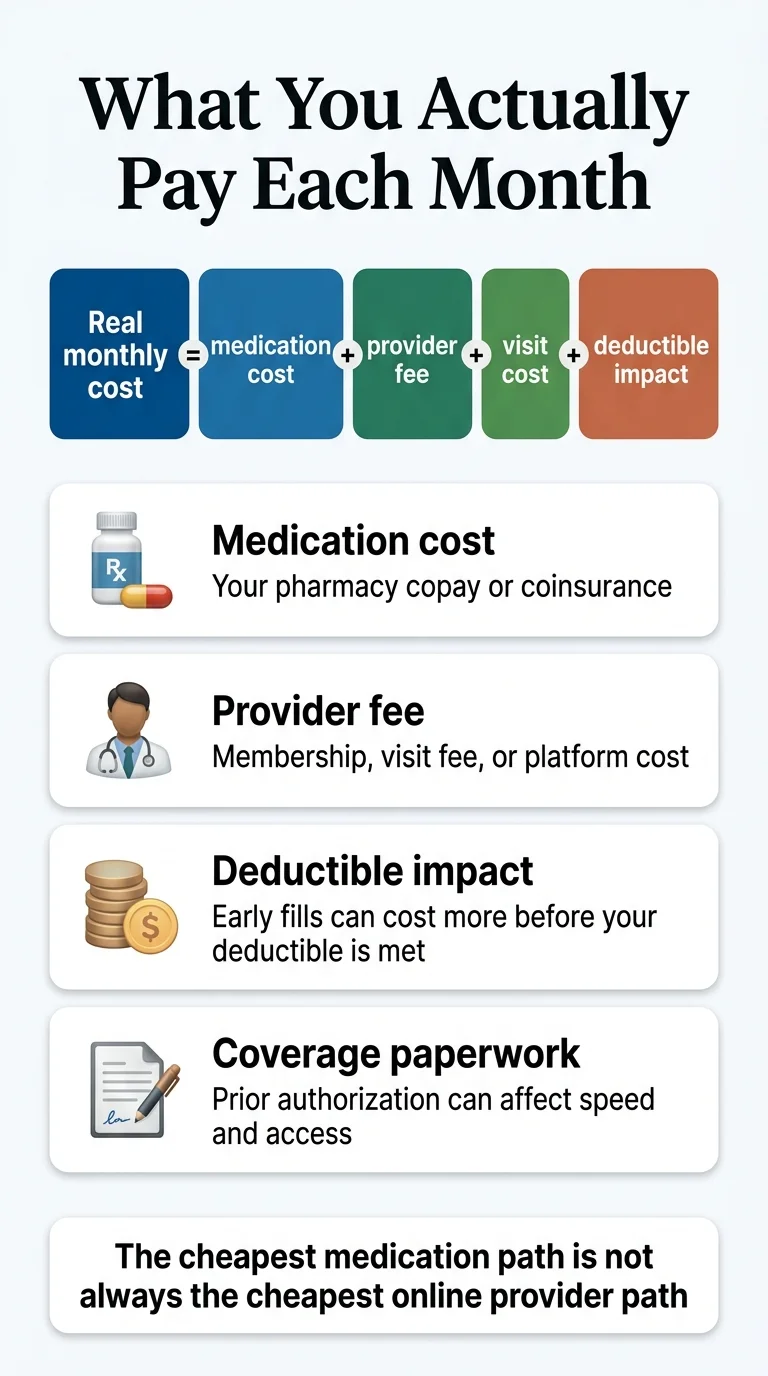
Mounjaro’s list price for a 28-day supply (4 pens) is approximately $1,112.16 according to Lilly’s pricing disclosure. With Express Scripts commercial coverage that covers Mounjaro plus the Lilly Mounjaro Savings Card, eligible patients can pay as little as $25 a month. If your commercial plan doesn’t cover Mounjaro, Lilly’s savings card has a separate path that can bring the price to about $499 a month — but that path also requires commercial insurance, and Medicare/Medicaid/TRICARE members are excluded from both paths.
The 2026 cost ladder
| Scenario | Your monthly cost | How it works |
|---|---|---|
| Commercial ESI covers Mounjaro + Lilly Savings Card | As low as $25 | Card stacks on top of your insurance copay. Max savings: $150 per 1-month fill, $300 per 2-month, $450 per 3-month, up to $1,950 per calendar year, up to 13 fills per year. |
| Commercial ESI covers Mounjaro, no savings card applied | Your plan's brand-tier copay (often $25–$100) | Activate the savings card — it costs nothing and stacks on top of insurance. |
| Commercial ESI doesn't cover Mounjaro + Lilly Savings Card | As low as $499 per month | Card explicitly covers this scenario. Max savings: up to $647 per fill, up to $8,411 per calendar year. Still requires commercial insurance. |
| Express Scripts Medicare PDP + T2D diagnosis | Your plan's Part D copay (varies by tier and benefit phase) | Savings card is NOT eligible for Medicare beneficiaries by federal law. |
| TRICARE via Express Scripts | $0 at a military pharmacy, $44 for a 90-day Home Delivery fill | Savings card not eligible. |
| Uninsured, no insurance at all | ~$1,112 list price, or ~$1,096.59 with GoodRx coupon (May 14, 2026) | Call Lilly Support Services; Lilly's savings card requires commercial drug insurance. |
Sources: Lilly Mounjaro pricing disclosure; Lilly Mounjaro Savings Card Terms (current card expires Dec 31, 2026); GoodRx Mounjaro cash price as of May 14, 2026.
How to get to $25 — the actual workflow
- 1
Confirm your commercial Express Scripts plan covers Mounjaro (Price a Medication tool, above).
- 2
Have your prescriber submit the diabetes PA. Get the approval confirmation.
- 3
Go to mounjaro.lilly.com/savings-resources or text "MJ" to 85099. Activate the Lilly Mounjaro Savings Card. Costs nothing.
- 4
Save the digital card to your phone wallet (Apple Wallet or Google Wallet works at most pharmacies).
- 5
At the pharmacy: the pharmacist runs your Express Scripts insurance first, then applies the savings card on top. Total out-of-pocket can be $25 for a 1-month, 2-month, or 3-month fill.
Who gets locked out of the $25 path
For Medicare beneficiaries, main backups are the Medicare Prescription Payment Plan (M3P — spreads out-of-pocket costs into monthly payments), Extra Help through Social Security if income-eligible, and a call to Lilly Support Services at 1-800-LillyRx about current Lilly Cares Foundation eligibility.
Does Express Scripts cover Mounjaro for weight loss?

Almost always no. The Express Scripts Mounjaro PA process stops cold when “weight loss” is the indication. Mounjaro is FDA-approved only for type 2 diabetes in adults and pediatric patients 10 years and older; Lilly itself says Mounjaro is not a weight-loss drug. If your real goal is weight management, the right covered alternative is Zepbound — the FDA-approved tirzepatide product for chronic weight management.
Mounjaro vs. Zepbound on Express Scripts
| Drug | FDA-approved for | Express Scripts status | PA criteria |
|---|---|---|---|
| Mounjaro | Type 2 diabetes (adults and kids 10+) | On 2026 National Preferred Formulary | T2D diagnosis + typically metformin step therapy |
| Zepbound pens | Chronic weight management + obstructive sleep apnea | On 2026 National Preferred Formulary (employer must opt into weight-management benefit) | BMI ≥30, or BMI ≥27 with at least one weight-related condition |
| Zepbound vials | Same FDA indications as pens | On the 2026 ESI formulary exclusions list (weight-loss section) | Preferred alternatives listed: liraglutide, Wegovy injection, Wegovy tablets, and Zepbound pens |
Same molecule (tirzepatide). Different FDA labels. Different formulary positions. Different coverage outcomes.
When your employer covers Zepbound pens
The fastest way to find out: (1) Run Price a Medication on Zepbound pen — not Mounjaro, not Zepbound vial. (2) If it shows covered with PA, you’re in. (3) If it shows “not covered,” your employer didn’t opt into the weight-management benefit, and no amount of fighting for Mounjaro will fix it.
If Zepbound is covered, typical PA criteria are:
- •BMI ≥30, or BMI ≥27 with at least one weight-related condition (hypertension, dyslipidemia, type 2 diabetes, obstructive sleep apnea, cardiovascular disease)
- •Documented lifestyle/diet attempts
- •Sometimes enrollment in a digital health program — Omada is the most common requirement for ongoing Zepbound coverage on Express Scripts plans
- •Reauthorization typically requires documented weight loss (often ≥5% baseline weight loss at 6–12 months)
The exact ask for your prescriber
“Express Scripts denied Mounjaro because I don’t have type 2 diabetes. Can we explore whether Zepbound fits under my plan’s weight-management benefit using my BMI of [your BMI] and my history of [hypertension / sleep apnea / dyslipidemia / etc.]?”
Want help getting Zepbound covered?
Ro’s free GLP-1 Insurance Coverage Checker runs your specific Express Scripts plan, tells you whether Zepbound or another GLP-1 is covered, and shows your estimated monthly cost. Ro says its insurance concierge helps fight for coverage and handles insurance paperwork.
Check your GLP-1 coverage with Ro’s free insurance checker → (sponsored affiliate link, opens in a new tab)Does Express Scripts Medicare cover Mounjaro?
Yes for type 2 diabetes with prior authorization. The Express Scripts Medicare PDP 2026 formulary lists Mounjaro as Tier 2 with PA and a quantity limit. Medicare does not cover Mounjaro for weight loss alone — and the new CMS Medicare GLP-1 Bridge does not include Mounjaro on its eligible-drug list.
What Express Scripts Medicare PDP does cover
- ✓Mounjaro for type 2 diabetes with prior authorization
- ✓Quantity limit applies (typically aligned with FDA dosing)
- ✓Step therapy through metformin is commonly required
- ✓Reauthorization typically required at 12 months
What it doesn’t cover: Mounjaro for weight loss, period. Medicare statute excludes weight-loss drugs from Part D coverage, and Mounjaro’s FDA label doesn’t include a weight-loss indication anyway.
The CMS Medicare GLP-1 Bridge — read carefully
CMS launched a temporary Medicare GLP-1 Bridge running from July 1, 2026 through December 31, 2027 with a flat $50 monthly copay for eligible beneficiaries.
✓ Bridge covers (for weight reduction)
- • Foundayo (orforglipron) — all formulations
- • Wegovy injection and oral tablets
- • Zepbound KwikPen formulation
$50/month flat copay through Dec 31, 2027
✗ Bridge does NOT cover
- • Mounjaro
- • Ozempic / Rybelsus
- • Zepbound single-dose vials/pens
- • Compounded GLP-1s
If you’re a Medicare beneficiary on Express Scripts looking at Mounjaro for weight loss specifically, the Bridge doesn’t help. Options: (1) Confirm a T2D diagnosis and pursue Mounjaro through standard Part D with PA; (2) Switch to Zepbound KwikPen under the Bridge for weight loss; (3) Apply for Extra Help through Social Security; (4) Call Lilly Support Services at 1-800-LillyRx.
What to do if Express Scripts denied your Mounjaro
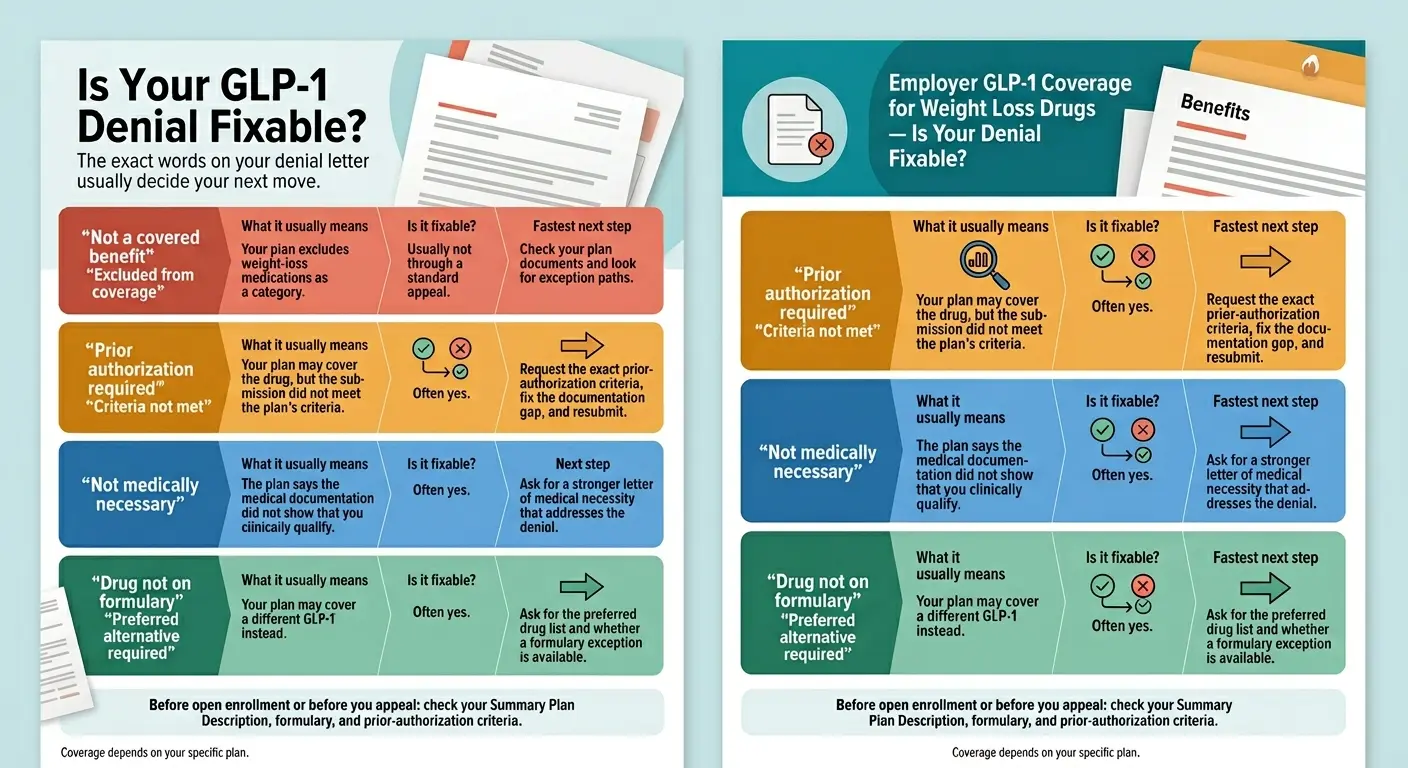
Don’t appeal blind. Pull out the denial letter first — every Express Scripts denial cites the exact reason in plain language, and the right next step depends entirely on which reason was used. Most denials fall into one of five categories, and four of them are fixable in 1–2 submissions.
The Express Scripts Mounjaro denial decoder
| What your denial letter says | What it really means | What to do |
|---|---|---|
| "Not on formulary" / "Plan exclusion" | Your employer or plan removed Mounjaro from your tier list (or never had it) | File a formulary exception with a medical-necessity letter showing why covered alternatives won't work |
| "Off-label use" / "Not for weight loss" | The PA was submitted with weight loss as the indication, or no T2D diagnosis was confirmed | If you have T2D: resubmit with the ICD-10 E11.x code. If you don't: ask about switching to Zepbound. |
| "Step therapy required" | You haven't tried metformin (or it wasn't documented in the PA) | Your prescriber documents metformin history (or contraindication/intolerance) and resubmits |
| "Insufficient clinical documentation" | A1C labs, diagnosis code, or comorbidity documentation was missing | Resubmit with the missing labs and chart notes |
| "Quantity limit exceeded" | You requested more than the plan's monthly cap | Confirm the dose matches FDA label; request a QL exception if dose escalation legitimately requires more |
| "PA expired" | Your old approval lapsed — common at 12 months | Submit continuation-of-care documentation with current and historical A1C |
How to file a formulary exception
- 1
Read the denial letter. It tells you exactly where to send the appeal and the deadline.
- 2
Your prescriber writes a Letter of Medical Necessity — Lilly publishes a sample template at mounjaro.lilly.com. The letter should cite the denial reason, your diagnosis, A1C history, prior medication trials, comorbidities, and why covered alternatives are inappropriate.
- 3
Submit by the deadline printed in your denial letter. First-level internal appeals typically allow 30 days for a decision.
- 4
If denied at internal appeal: Your denial letter should explain whether external review is available and how to request it. External review goes through your state's Department of Insurance.
What goes in a strong Letter of Medical Necessity
The exact denial reason cited
ICD-10 type 2 diabetes diagnosis code
A1C history (current and pre-treatment if you're on Mounjaro already)
Documented metformin trial (dates, doses, duration, outcome) OR contraindication
Comorbidities that strengthen the case — hypertension, dyslipidemia, cardiovascular history, kidney function, sleep apnea
Why specific covered alternatives won't work (intolerance to other GLP-1s, prior failure on Ozempic, etc.)
Prescriber attestation and signature
When to bring in outside help
Filing a Mounjaro appeal alone takes 4–8 hours of phone calls, paperwork, and follow-up. If your prescriber’s office isn’t experienced with PBM appeals, or you’ve already been denied once, Ro’s insurance concierge submits the paperwork and follows up on your behalf. Sesame Care offers provider-choice visits for self-pay prescriptions if you want a cash-pay alternative while you appeal.
Why Express Scripts Mounjaro coverage feels so confusing
Members repeatedly report that “covered” can mean five different things, that prior authorization criteria aren’t always disclosed up front, and that continuation-of-care denials catch long-time users off-guard. Express Scripts’ own NPF document acknowledges this. The Price a Medication tool is the official member-level check.
"Mounjaro is covered under my insurance (Express Scripts) with a PA."
— Reddit user describing the standard T2D coverage path.
"Has anyone ever experienced their insurance NOT be willing to give PA criteria/requirements?"
— Reddit user describing the frustration of not being told what the PA actually requires.
"Express scripts tried denying me after a year on MJ… your doctor just needs to submit a 'continuation of care.'"
— Reddit user describing how a 12-month reauthorization got resolved.
Can a telehealth provider help with Mounjaro on Express Scripts?
A telehealth provider can’t force Express Scripts to cover Mounjaro, but the right one can run your coverage check, submit the PA correctly the first time, support appeals, and switch your prescription to Zepbound if Mounjaro isn’t the right insurance fit.
Ro Body: best for insurance concierge + PA support
Ro is a telehealth platform focused on access to FDA-approved GLP-1 options. For Express Scripts members, Ro’s value isn’t the medication price — it’s the concierge. Ro carries Wegovy, Ozempic, Zepbound (pen and vial), and Foundayo.
Pricing: $39 first month, then $149/month — or as low as $74/month with the annual plan paid upfront. Medication cost is separate.
Honest admission: Ro is not the cheapest path if you have a PCP who will handle your PA and commercial insurance covering Mounjaro. In that scenario, your $25/month with the Lilly Savings Card beats any telehealth membership. If that’s you — skip Ro and use your prescriber plus the Lilly Mounjaro Savings Card.
Who Ro fits: Commercial ESI members whose PA was denied; people switching from Mounjaro to Zepbound; anyone without a PCP who will fight the GLP-1 paperwork.
Check your Express Scripts coverage with Ro — free → (sponsored affiliate link, opens in a new tab)Sesame Care: best when you want provider choice
Sesame Care is a marketplace where you choose your specific provider for an online visit. The Success by Sesame online weight-loss program starts at $59/month with annual subscription. Sesame’s subscription does not bill health insurance — medication cost is separate, and any pharmacy benefit you have is separate too.
Who Sesame fits: You want to choose your specific provider; you want a transparent self-pay path for the visit and will route the prescription through your ESI plan yourself; you want a cash-pay alternative if your plan won’t cover what you need.
Compare Sesame’s FDA-approved GLP-1 options → (sponsored affiliate link, opens in a new tab)A note on EnGuide Pharmacy: If your Express Scripts plan tells you to fill Mounjaro through EnGuide Pharmacy, that’s not a denial — it’s a specialty home-delivery channel Express Scripts uses for injectable GLP-1s. Availability depends on your plan sponsor’s selection. Log into your Express Scripts account and check your pharmacy options — if EnGuide is your assigned channel, you’ll see it there.
Express Scripts Mounjaro: quick answers to the edge cases
Can I use Mounjaro for prediabetes on Express Scripts?
Almost never under the standard PA. The diabetes PA criteria require a type 2 diabetes diagnosis (E11.x), not prediabetes (R73.x). A prediabetes-only diagnosis typically triggers an automatic denial.
Will Express Scripts cover Mounjaro for PCOS or insulin resistance?
Rarely. PCOS and insulin resistance are considered off-label uses. Coverage requires a formulary exception with a strong medical-necessity argument, and outcomes are mixed even with good documentation.
Can I use GoodRx with Express Scripts for Mounjaro?
Not at the same time — you choose one or the other at the pharmacy counter. GoodRx Mounjaro cash prices as of May 14, 2026 list around $1,096.59 — almost never cheaper than your insurance copay plus the Lilly Savings Card.
What tier is Mounjaro on Express Scripts?
Tier 2 (preferred brand) or Tier 3 (non-preferred brand) on most commercial plans. Express Scripts Medicare PDP lists it as Tier 2. Your specific tier shows up in the Price a Medication tool.
Can I get a 90-day supply of Mounjaro through Express Scripts Home Delivery?
Yes, if your plan allows 90-day fills and your prescription is written for that quantity. The Lilly Savings Card supports up to 3-month fills at the $25 rate, so 90-day Home Delivery plus savings card is one of the cheapest combos available.
Does Express Scripts cover compounded tirzepatide?
No. Express Scripts coverage for Mounjaro or Zepbound does not extend to compounded tirzepatide. If you've been using compounded tirzepatide and want to switch to an insurance-covered path, file a fresh PA for FDA-approved Mounjaro (if you have T2D) or Zepbound (for weight management).
How long does an Express Scripts Mounjaro PA last?
Typically 12 months before re-authorization is required. Continuation-of-care documentation (A1C improvement and tolerability) makes renewal smoother.
What if I switch employers and lose Express Scripts mid-treatment?
Coverage is plan-specific and resets when you switch. Run Price a Medication on your new plan before your first refill. If the new plan doesn't cover Mounjaro, your fastest options are filing a formulary exception or the Lilly Savings Card's 'commercial-without-coverage' path (~$499/month).
How we verified this guide
We read primary source documents directly — not other blog posts. Here’s the full source list with the date we accessed each.
- –Express Scripts 2026 National Preferred Formulary (effective Jan 1 – Dec 31, 2026) — verified May 14, 2026
- –Express Scripts 2026 National Preferred Formulary Exclusions (Zepbound vials listed under weight-loss exclusions) — verified May 14, 2026
- –Express Scripts Medicare PDP 2026 Formulary (updated Aug 27, 2025) — verified May 14, 2026
- –Express Scripts TRICARE/DoD Mounjaro Prior Authorization Form (the public, downloadable form for TRICARE pharmacy program prescriptions) — verified May 14, 2026
- –Express Scripts 'Price a Medication' tool documentation — verified May 14, 2026
- –Express Scripts EnGuide Pharmacy FAQ — verified May 14, 2026
- –Cigna/Evernorth GLP-1/GIP Prior Authorization Coverage Policy — verified May 14, 2026
- –Mounjaro Prescribing Information (Eli Lilly, current FDA label) — verified May 14, 2026
- –Mounjaro Savings Card Terms & Conditions (current card expires Dec 31, 2026) — verified May 14, 2026
- –Lilly Mounjaro FAQ and pricing disclosure (list price $1,112.16 for 28-day supply) — verified May 14, 2026
- –Lilly Mounjaro Prior Authorization Tips Guide — verified May 14, 2026
- –FDA statements on GLP-1 compounding policy — verified May 14, 2026
- –CMS Medicare GLP-1 Bridge program (Foundayo, Wegovy injection/tablets, Zepbound KwikPen — Mounjaro not included; effective July 1, 2026 through Dec 31, 2027) — verified May 14, 2026
- –Ro pricing and insurance pages ($39 first month, $149/month, as low as $74/month with annual plan) — verified May 14, 2026
- –Sesame Care online weight-loss program page (subscription starts at $59/month annual; medication separate; subscription does not bill insurance) — verified May 14, 2026
- –GoodRx Mounjaro cash price page — verified May 14, 2026
Last verified: May 14, 2026. We update this page monthly, or sooner when Express Scripts, Lilly, or CMS publishes a material change.
Published: · Last reviewed:
Frequently asked questions
Does Express Scripts cover Mounjaro in 2026?
Express Scripts can cover Mounjaro for type 2 diabetes, and many Express Scripts-administered plans require prior authorization. Mounjaro appears on the 2026 Express Scripts National Preferred Formulary, but the formulary itself states the list is abbreviated and does not guarantee coverage for every plan. Use Price a Medication inside your account to confirm your specific plan.
Does Express Scripts cover Mounjaro for weight loss?
No. Mounjaro is FDA-approved only for type 2 diabetes, and the Express Scripts PA process stops approval when 'weight loss' is the indication. For weight loss, ask your prescriber whether Zepbound fits under your plan's weight-management benefit.
Does Express Scripts cover Mounjaro for type 2 diabetes?
Often yes, with prior authorization. Your prescriber's PA submission typically needs your ICD-10 type 2 diabetes diagnosis, A1C history, and metformin trial documentation (or a documented contraindication to metformin). Specific criteria vary by plan.
Does Express Scripts Medicare cover Mounjaro?
Yes for type 2 diabetes — Mounjaro is listed as Tier 2 with prior authorization and a quantity limit on the 2026 Express Scripts Medicare PDP formulary. Medicare does not cover Mounjaro for weight loss, and the Lilly Mounjaro Savings Card is not eligible for Medicare beneficiaries.
How much does Mounjaro cost with Express Scripts?
With commercial coverage that covers Mounjaro plus the Lilly Mounjaro Savings Card: as low as $25 per month. Without the savings card: your plan's brand-tier copay, typically $25–$100. If you have commercial insurance that does not cover Mounjaro, Lilly's savings card has a separate path as low as $499 per month. List price is approximately $1,112 per 28-day supply.
How do I check if Express Scripts covers my Mounjaro?
Log into your Express Scripts member account, go to 'Price a Medication,' search for Mounjaro, enter your dose and quantity, and read the coverage result. The tool shows tier, restrictions (PA, QL, ST), and estimated cost specific to your plan.
Why did Express Scripts deny my Mounjaro?
The five most common denial reasons: not on your plan's formulary, off-label use for weight loss, step therapy not documented (metformin trial), insufficient clinical documentation, or quantity limit exceeded. Your denial letter cites the exact reason.
Can I appeal an Express Scripts Mounjaro denial?
Yes. File a formulary exception or first-level internal appeal within the timeframe printed in your denial letter. Include a Letter of Medical Necessity from your prescriber. If denied at internal appeal, your denial letter should explain whether external review is available and how to request it.
How long does Express Scripts prior authorization take for Mounjaro?
Standard PA review is often 1–3 business days from when the complete form arrives. Expedited reviews are typically 24 hours. Internal appeals usually allow up to 30 days for a decision. The exact deadlines appear on your plan's PA decision letter and your denial letter.
Can I use the Lilly Mounjaro Savings Card with Express Scripts?
Yes, if you have commercial Express Scripts coverage. The card excludes Medicare, Medicaid, TRICARE, VA, other government health programs, and uninsured patients. Activate at mounjaro.lilly.com/savings-resources or text 'MJ' to 85099.
Does Express Scripts cover Zepbound?
Zepbound pens appear on the 2026 National Preferred Formulary for chronic weight management — coverage requires your employer to have opted into the weight-management benefit. PA criteria typically include BMI ≥30 or BMI ≥27 with one weight-related condition. Zepbound vials are on the 2026 formulary exclusions list with preferred alternatives shown.
Is the Express Scripts Mounjaro PA form the same for every plan?
No. The public, downloadable Mounjaro PA form on the Express Scripts site is the TRICARE/Department of Defense form, applicable only to TRICARE pharmacy program prescriptions. Commercial, Medicare PDP, Cigna/Evernorth, and employer-sponsored plans can use different criteria and submission forms — though the typical documentation requirements (T2D diagnosis, A1C, metformin history, comorbidities) overlap.
Does Express Scripts cover Mounjaro through EnGuide Pharmacy?
Possibly. EnGuide is the Express Scripts specialty home-delivery channel for injectable GLP-1s. Availability depends on your plan sponsor's selection. Log into Express Scripts to see if EnGuide is your assigned pharmacy channel.
The bottom line
If you have type 2 diabetes and commercial Express Scripts: Your path is your prescriber + the diabetes PA + the Lilly Mounjaro Savings Card. Total cost can be as low as $25/month. You don't need a telehealth platform for this.
If you have Express Scripts Medicare and T2D: Your path is your prescriber + the diabetes PA + your plan copay. The savings card is off the table. Consider the Medicare Prescription Payment Plan to smooth costs, and call Lilly Support Services about current assistance options.
If you have TRICARE through Express Scripts and T2D: Your path is the diabetes PA + a medical-necessity form. Military pharmacy and Home Delivery are your cheapest fills.
If you have Express Scripts but want Mounjaro for weight loss without T2D: Don't fight a losing PA. Ask your prescriber whether Zepbound fits under your plan's weight-management benefit. If your employer didn't opt in, Ro can help check whether another path works for you.
If your PA was denied or your prescriber won't fight the paperwork: Ro's insurance concierge submits Mounjaro and Zepbound PAs and helps with formulary exceptions as part of the Ro Body membership.
If you're uninsured or your plan doesn't cover Mounjaro: Call Lilly Support Services at 1-800-LillyRx to check current Lilly Cares Foundation eligibility. If you have other commercial drug insurance, the savings card's 'commercial-without-coverage' path can bring the cost to about $499/month.
Still not sure which path fits you?
Take our free 60-second GLP-1 matching quiz — we’ll match you to the right path based on your insurance type, diagnosis, budget, and goal.
Take the matching quiz →Related guides
- →Does Aetna Cover Mounjaro? 2026 PA Rules & Costs
- →Does CVS Caremark Cover Mounjaro? PA & Costs
- →Does Medicare Cover Mounjaro for Weight Loss?
- →Mounjaro Cost Without Insurance: Real 2026 Prices
- →Does Express Scripts Cover Foundayo?
- →Does TRICARE Cover GLP-1 Medications?
- →The 60-Second GLP-1 Matching Quiz
About The RX Index: The RX Index is a pricing intelligence and comparison resource for GLP-1 telehealth providers. We do not give medical advice. We do not decide insurance coverage. We do not guarantee approval. We translate public coverage rules, manufacturer-stated pricing, and PBM formulary documents into a clearer decision path. Coverage outcomes depend on your specific plan and your prescriber’s submission.
Affiliate disclosure: The RX Index has affiliate relationships with Ro and Sesame Care. We earn a commission if you start service through our links. These relationships do not change the coverage rules, PA logic, or denial paths above — those come from primary source documents. Full disclosure.
This guide is for educational and informational purposes only. It is not medical advice and is not a substitute for consultation with a qualified healthcare provider. Always confirm coverage details directly with Express Scripts and discuss treatment decisions with your prescriber.