Does Humana Cover Zepbound? 2026 Plan-by-Plan Rules
By The RX Index Editorial Team ·
Published: · Last reviewed:
Does Humana cover Zepbound? Sometimes — and the honest version of "yes or no" depends on four things: which Humana plan you have, why your doctor is prescribing it, the exact formulation, and whether the new Medicare GLP-1 Bridge applies to you starting July 1, 2026. Coverage on Humana commercial and employer plans is plan-specific (some include anti-obesity medications, many don't). Humana Medicare Part D plans don't cover Zepbound for weight loss alone because federal law blocks Medicare from covering weight-loss drugs, but Zepbound for moderate-to-severe obstructive sleep apnea in adults with obesity may be handled through normal Part D formulary rules. And starting July 1, 2026, eligible Medicare Part D members can get Zepbound KwikPen at a flat $50 per month through the Medicare GLP-1 Bridge — a federal demonstration program that Humana itself runs as the central processor.
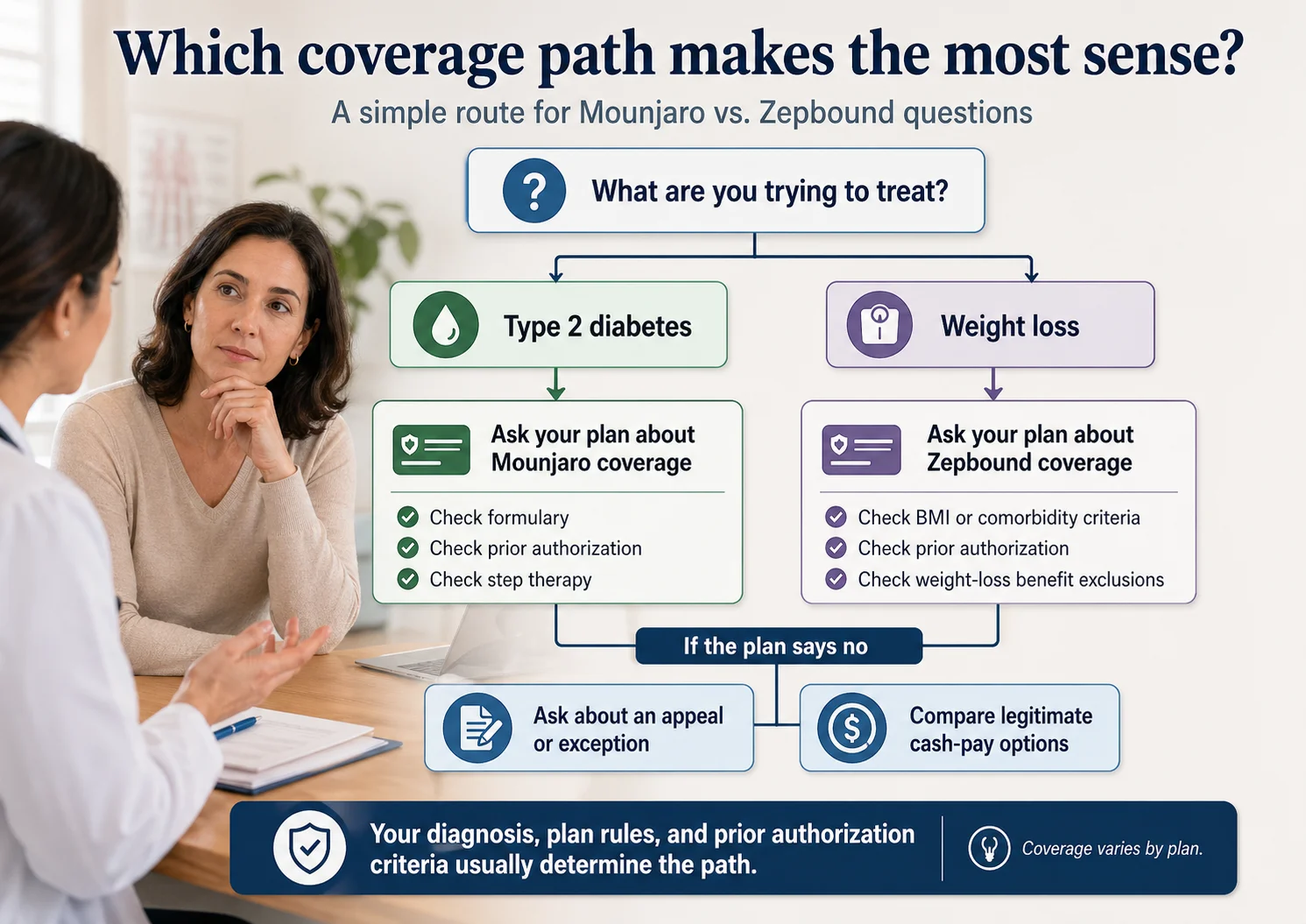
Coverage paths for Humana Zepbound — weight loss, sleep apnea, Medicare Bridge, and cash-pay options.
The Humana Zepbound Decision Matrix
Find your row. The "next step" column is the one that matters.
| Your Humana situation | Likely answer | What changes the answer | Your next step | Verified source basis |
|---|---|---|---|---|
| Humana commercial / employer — weight loss only | Plan-specific (often excluded) | Whether your plan includes anti-obesity medications as a covered benefit | Check MyHumana drug list and ask HR if anti-obesity meds are covered | Humana directs members to MyHumana for plan-specific coverage |
| Humana commercial / employer — moderate-to-severe OSA + obesity | Possibly covered with PA | Plan formulary, documentation quality, exact formulation | Submit a PA documenting OSA, sleep-study evidence, and BMI | FDA label confirms OSA indication; Humana PA guidance |
| Humana Medicare Advantage / PDP — weight loss only (before July 1, 2026) | Not covered under normal Part D | Bridge eligibility once it launches July 1, 2026 | Plan for the Medicare GLP-1 Bridge — confirm your eligibility | Medicare Modernization Act 2003 blocks weight-loss drug coverage |
| Humana Medicare Advantage / PDP — OSA + obesity | May be covered through normal Part D rules | Plan-specific formulary, PA, or exception requirements | Ask Humana specifically about Zepbound for moderate-to-severe OSA in adults with obesity | CMS Bridge FAQ: OSA use may be coverable under basic Part D, not Bridge |
| Humana Medicare Employer Plan (retiree/union) | Plan-specific — some list Zepbound | Your employer/union plan's specific formulary | Read your plan's Prescription Drug Guide, not generic Humana info | NDPERS-hosted 2026 Humana Medicare Employer formulary lists Zepbound Tier 4 with PA |
| Medicare GLP-1 Bridge (weight reduction, starts July 1, 2026) | Yes if you qualify | Three BMI/clinical paths (see below) | Provider submits PA to the central processor (Humana) for Zepbound KwikPen at $50/month | CMS Medicare GLP-1 Bridge FAQ (May 2026) |
| Humana Healthy Horizons Medicaid (FL, IN, KY, LA, OH, OK, SC, VA) | State-specific | Your state's Preferred Drug List and PA rules | Call your state's Humana Medicaid line; verify the PDL | Humana provider drug-list page lists 8 states |
| No Humana coverage path applies | Cash-pay only | Self-pay program eligibility | LillyDirect Self Pay Journey: $299–$449/month for vials | Eli Lilly Self Pay Journey Program terms |
Sources: Humana Medicare Drug List page; 2026 Humana Medicare Employer Plan formulary (NDPERS hosted PDF, formulary updated 09/29/2025); CMS Medicare GLP-1 Bridge FAQ (May 2026); Zepbound FDA Prescribing Information; Eli Lilly Zepbound Self Pay Journey Program terms. See "What we actually verified" below for direct citations.
Don't want to guess — have Ro check what your Humana plan says
The fastest move if you have a Humana commercial or employer card in your wallet right now: run Ro's free GLP-1 Insurance Coverage Checker. Ro says its checker contacts your insurance plan by phone, collects coverage eligibility information, and sends you a personalized report showing GLP-1 coverage and whether prior authorization may be required. It doesn't write prescriptions or submit treatment requests — it tells you what's covered before you commit to anything. Free. About two minutes to start.
Note: Ro currently states it can't coordinate GLP-1 coverage for most government-funded plans (Medicare, Medicaid, TRICARE, VA), with limited exceptions. If you have Humana Medicare, Humana Medicaid, or other government coverage, use the MyHumana call script further down this page first.
Check My Humana Commercial Coverage — Free →Does Humana cover Zepbound? Why the answer depends on your plan
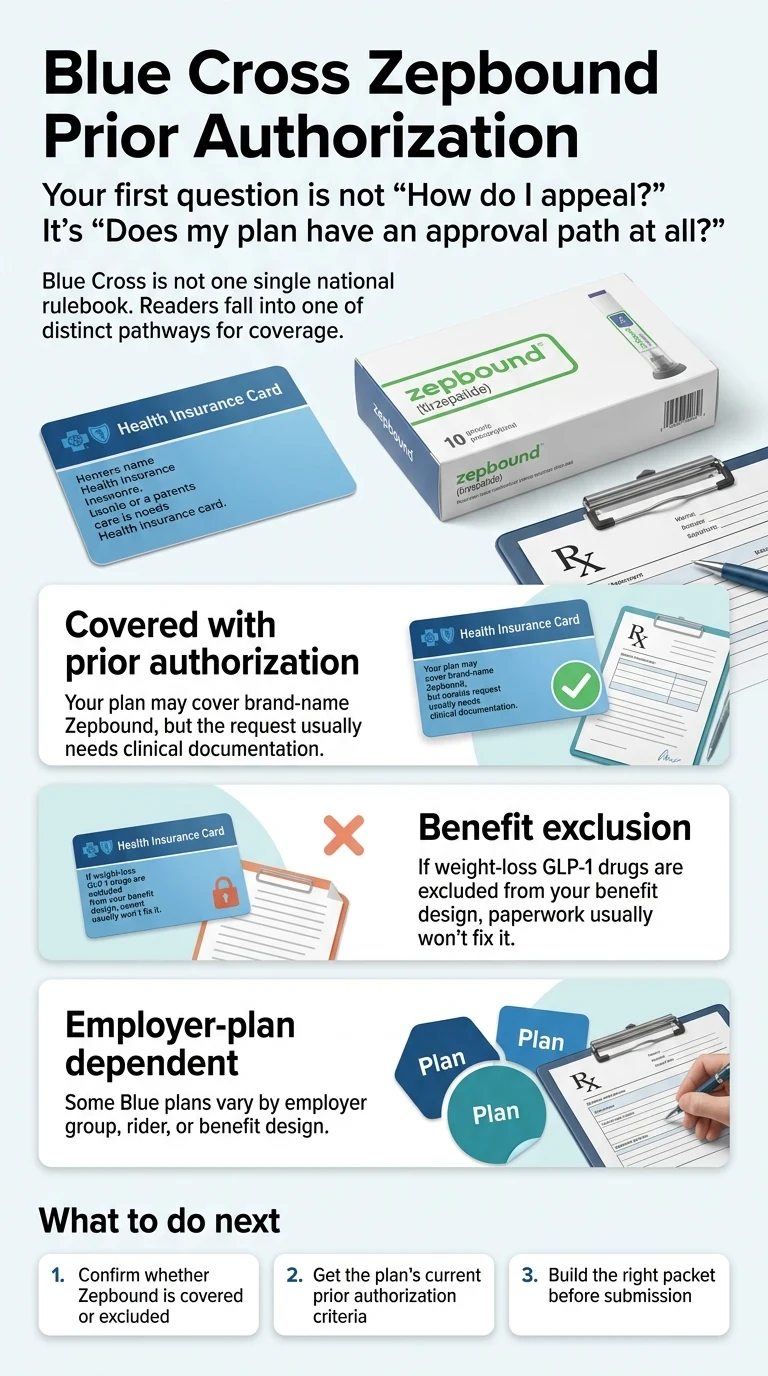
Answer capsule: Humana isn't one insurance plan — it's dozens. Coverage for Zepbound varies across commercial employer plans, Medicare Advantage, standalone Part D plans, Medicare Employer Plans, and state Medicaid (Humana Healthy Horizons). The same medication can be covered on one plan and denied on another, depending on benefit design, formulary tier, prior authorization rules, and the diagnosis your doctor submits.
Here's what most pages miss: a Humana "denial" can mean three completely different things.
- The claim rejected at the pharmacy before a full PA review — this can happen when the medication requires prior authorization, when the submitted diagnosis doesn't match the plan's covered use, when the formulation doesn't match the plan record, or when the drug is excluded from your benefit entirely. The rejection at the counter feels final, but it isn't necessarily.
- The prior authorization was denied — a human reviewed it and said no, usually because the documentation was thin or the diagnosis didn't match the plan's criteria.
- The benefit doesn't exist — your specific plan has a hard exclusion for anti-obesity medications. No PA can fix this. Only a formulary exception or a different plan can.
You can't fix #3 with a better appeal letter. You can often fix #1 and #2.
The single most useful thing you can do right now: get the actual denial language in writing. If you don't know which kind of "no" you got, you can't pick the right next step.
Does Humana cover Zepbound for weight loss?
Answer capsule: For Humana commercial or employer plans, weight-management coverage is plan-specific — some employer plans include anti-obesity medications, many exclude them entirely. For Humana Medicare Part D and Medicare Advantage plans, Zepbound for weight reduction is not covered under normal Part D rules because federal law blocks Medicare from covering drugs used solely for weight loss. Starting July 1, 2026, eligible Medicare Part D members can access Zepbound KwikPen at $50 per month through the Medicare GLP-1 Bridge — a federal demonstration that operates outside normal Part D.
The honest version (our one damaging admission)
We could write a Humana commercial PA letter packed with BMI documentation, comorbidities, and lifestyle attempts — and it would still likely fail if your specific plan has a hard weight-loss exclusion. That's not a paperwork problem. It's a benefit-design problem. Appealing a benefit exclusion almost never wins because there's no medical-necessity question being asked. The plan simply doesn't cover that category of drug.
Ro doesn't fight benefit exclusions either — nobody does, because they aren't fightable. But because Ro skips the appeals theater on hopeless cases, the team can move fast on the cases that actually work: confirming coverage on commercial plans that do include GLP-1s, and routing eligible cash-pay patients to FDA-approved Zepbound at published LillyDirect-style pricing. If your priority is "I have a Humana commercial plan with no weight-loss benefit and I want to start Zepbound this month," that's the path.
If your plan does cover anti-obesity meds, prior authorization is almost always required and worth pursuing. Here's how to tell which group you're in.
How to tell PA denial from benefit exclusion
| Denial language on your letter or pharmacy receipt | What it usually means | Best next step |
|---|---|---|
| "Prior authorization required" | Coverage may exist — paperwork is missing | Submit a PA with full documentation |
| "Prior authorization denied" | Coverage may exist — your PA didn't meet criteria | Read the denial reason; resubmit or appeal |
| "Not on formulary" | The drug isn't on your plan's covered list | Request a formulary exception |
| "Not a covered benefit" | Hard plan exclusion | Don't appeal — look at Bridge, OSA, or cash-pay |
| "Diagnosis not covered" | Wrong or unsupported diagnosis on the claim | Verify diagnosis matches FDA indication; have your doctor resubmit |
| "Bridge-eligible drug" | Medicare claim should route through the central processor | Use the Bridge process (starting July 1, 2026) |
Does Humana cover Zepbound for sleep apnea?
Answer capsule: Zepbound is FDA-approved for moderate-to-severe obstructive sleep apnea (OSA) in adults with obesity, and CMS has confirmed that this use may be coverable under basic Medicare Part D rules — separate from the new Medicare GLP-1 Bridge, which covers weight reduction only. Humana members still need to verify their exact plan's formulary status, prior authorization requirements, and any exception process. Coverage is not automatic anywhere, but the OSA indication opens a coverage door that "weight loss" doesn't.
Why OSA changes the coverage conversation
In December 2024, the FDA approved Zepbound for moderate-to-severe obstructive sleep apnea in adults with obesity. That was a real coverage opening. OSA is a covered medical condition under Medicare. Pure weight loss isn't. So when Zepbound is prescribed for OSA, Medicare's "no weight-loss drugs" rule doesn't block it.
CMS confirmed this in its May 2026 Medicare GLP-1 Bridge FAQ: Zepbound for moderate-to-severe OSA in adults with obesity may be coverable under basic Part D rules. It does not go through the Bridge — the Bridge is specifically for the weight-reduction indication. So if you have OSA, the path is normal Part D coverage with prior authorization or a formulary exception, not the new program.
What your prescriber should include in a Humana OSA prior authorization
Plan-specific PA criteria vary, so always verify with your exact Humana plan. As a practical preparation checklist, ask the prescriber to include:
- Sleep study results (polysomnogram or home sleep apnea test) showing AHI documentation consistent with moderate-to-severe OSA.
- BMI documentation confirming adult obesity.
- OSA as the diagnosis driving the request — ask Humana and your prescriber whether the PA should identify obstructive sleep apnea (ICD-10 G47.33) as the primary diagnosis.
- Obesity diagnosis as a secondary code where appropriate (Z68.3x or Z68.4x for BMI category).
- Concurrent lifestyle modification plan noted in the chart (reduced-calorie diet and physical activity, per the FDA label).
- Current medication list to confirm no contraindications.
- Exact Zepbound formulation and dose matching what the plan record covers.
- Formulary exception request if Zepbound isn't on your plan's formulary.
When OSA prior authorizations fail
"The appeal she submitted was basically a few sentences… she didn't submit any proof of it."— Public Reddit post, r/Zepbound, 2025
Translation: a doctor's office sent a thin appeal with no documentation. The plan denied it because there was nothing to review. The fix isn't a longer letter — it's attaching the sleep study, BMI documentation, and a clinical narrative that meets the plan's specific criteria.
A useful framework for figuring out where a PA went wrong:
- Did the PA clearly identify the OSA indication, not just "weight loss"?
- Was the sleep study attached with AHI documentation?
- Was BMI/obesity documentation included?
- Was the exact formulation matched to the plan record?
- Did the request use your plan's actual PA form?
If you already have a Humana commercial plan and OSA, Ro can confirm whether your specific plan covers Zepbound for OSA and what PA documentation is needed. If you're on Humana Medicare, Ro can't currently coordinate the OSA coverage check for you — use the MyHumana call script further down this page and call Humana directly, asking specifically about Zepbound for moderate-to-severe OSA in adults with obesity.
Check My Humana Commercial OSA Coverage with Ro →Does Humana Medicare cover Zepbound? (And the new $50/month Medicare GLP-1 Bridge)
Answer capsule: Humana Medicare Advantage and standalone Part D plans don't cover Zepbound for weight loss alone — that's federal law from the 2003 Medicare Modernization Act, not a Humana choice. But Zepbound for moderate-to-severe OSA in adults with obesity may be handled through normal Part D formulary or exception rules. And starting July 1, 2026, eligible Medicare Part D beneficiaries can get Zepbound KwikPen at a flat $50/month copay through the Medicare GLP-1 Bridge — a federal demonstration program that Humana runs as the CMS central processor nationally.
How standard Humana Medicare treats Zepbound right now
Two different rules apply at the same time — neither has anything to do with Humana specifically. They're federal:
- Medicare cannot cover drugs used only for weight loss. Medicare Modernization Act of 2003. This applies to every Part D plan, including all of Humana's.
- Medicare can cover drugs used for FDA-approved medical conditions on the plan's formulary. That's why Zepbound for OSA in adults with obesity may be covered, while Zepbound for "obesity alone" is not.
So your coverage today depends entirely on the diagnosis your doctor writes on the prescription and your specific plan's formulary.
The Medicare GLP-1 Bridge — what's actually happening July 1, 2026
CMS announced this in December 2025 and published the operational FAQ in May 2026. The short version:
- What it is: A federal demonstration program that lets eligible Medicare Part D beneficiaries get certain GLP-1 weight-loss drugs at $50/month.
- When: July 1, 2026 through December 31, 2027.
- Eligible drugs: Wegovy (pill and injectable), Foundayo (pill), and Zepbound KwikPen only. Zepbound single-dose vials and the original single-dose pens are not Bridge-eligible.
- Who processes the claims: CMS contracted with Humana as the central processor. This is a national role — it doesn't give Humana members a special pathway. Bridge eligibility is based on CMS criteria, not on having a Humana-branded Medicare plan.
Who qualifies for the Bridge — the three clinical paths
CMS lists three separate paths to Bridge eligibility. You qualify if you meet any one of these at the time GLP-1 therapy is initiated:
| Path | BMI requirement | Required additional condition |
|---|---|---|
| Path 1 | BMI ≥ 35 | None — automatic qualifier |
| Path 2 | BMI ≥ 30 | Plus heart failure with preserved ejection fraction (HFpEF), uncontrolled hypertension, or chronic kidney disease stage 3a or above |
| Path 3 | BMI ≥ 27 | Plus prediabetes, prior heart attack (MI), prior stroke, or symptomatic peripheral artery disease |
The four things every Medicare member needs to know about the Bridge
- The Bridge ends December 31, 2027. It's a demonstration program, not a permanent expansion. CMS has signaled a longer-term program called the BALANCE Model may follow, but it's not law yet.
- The $50 copay does not count toward the $2,100 Part D out-of-pocket cap because the Bridge operates outside Part D. If you're juggling other expensive medications, plan accordingly.
- Only Zepbound KwikPen is Bridge-eligible. Single-dose vials and the original single-dose pens are excluded. If your doctor writes you a prescription for the wrong formulation, you'll pay the standard self-pay price.
- Doctors don't need to be enrolled as Medicare providers to write the Bridge prescription or submit the PA. Your prescribing physician submits it directly to the central processor (Humana) using specific BIN and PCN identifiers that CMS will publish in operational form in Spring 2026.
Already on a GLP-1 for weight loss before Bridge launches?
CMS has built in continuity. If you started a GLP-1 in, for example, September 2024 with a BMI of 37 and you've since lost weight to a BMI of 34, your prescriber attests in the PA that you met the BMI ≥35 criterion at the time therapy began. You don't lose eligibility because the medication worked.
Bridge path: your next move. If you're a Medicare member and you think you may qualify, mark your calendar for July 1, 2026 and talk to your doctor in advance. Have BMI history documented along with any qualifying conditions. CMS will publish the operational PA workflow in Spring 2026 — when it does, we update this page within seven days.
See If You Qualify for the Medicare GLP-1 Bridge →Which Zepbound formulation matters for Humana coverage — pen, vial, or KwikPen?
Answer capsule: Formulation matters because normal plan coverage, manufacturer savings, cash-pay programs, and the Medicare GLP-1 Bridge don't all treat Zepbound the same way. CMS limits the Bridge to Zepbound KwikPen only. Manufacturer savings card terms apply specifically to single-dose pen fills. LillyDirect's self-pay program offers both vials and KwikPen at the same dose-by-dose pricing. Always confirm with Humana and your prescriber which formulation is being submitted before you assume a quoted price or coverage path applies.
| Formulation | Standard Humana coverage | Medicare GLP-1 Bridge | Lilly commercial savings card | LillyDirect Self Pay |
|---|---|---|---|---|
| Zepbound single-dose pen | Plan-specific; may be covered with PA | Not Bridge-eligible | Yes — as little as $25 for commercially insured eligible patients | Not the primary self-pay formulation |
| Zepbound KwikPen (multi-dose pen) | Plan-specific; may be covered with PA | Bridge-eligible at $50/month | Pen-specific terms apply | $299–$449/month with 45-day refill discipline |
| Zepbound single-dose vial | Plan-specific (less common as covered benefit) | Not Bridge-eligible | Vial typically falls outside the commercial card | $299–$449/month — Lilly's cheapest path |
Does Humana commercial or employer insurance cover Zepbound?
Answer capsule: It depends almost entirely on what your employer paid for. Humana administers the plan, but the employer decides whether anti-obesity medications are a covered benefit. Some Humana commercial plans cover Zepbound with prior authorization; many exclude weight-loss medications entirely. To know for sure, check your specific plan's formulary in MyHumana and read the benefit exclusion list in your plan documents.
When your employer buys a Humana plan, they pick a benefit design. Some employers include anti-obesity medications. Many don't. Humana administers what the employer bought. Two coworkers can both have "Humana" on their cards and get completely different Zepbound answers — the difference is the employer's plan design, not the insurance company.
What to ask — and where
Inside MyHumana
- Sign in and search the drug list for "Zepbound" and "tirzepatide."
- Look at the tier and utilization management flags (PA, QL, ST).
- Note whether your plan shows Zepbound at all.
On the phone with Humana
- "Is Zepbound on my plan's formulary?"
- "Is the indication for weight management covered?"
- "What's the prior authorization process?"
- "Is a formulary exception possible?"
With your HR team
- "Does our plan include anti-obesity medications?"
- "If not, can we add them at open enrollment?"
Humana Medicare Employer Plan is a different animal
If your Medicare coverage comes through a former employer or union retiree plan (a Humana Medicare Employer Plan), don't assume the rules are the same as standard Medicare Advantage. A 2026 Humana Medicare Employer Plan Comprehensive Drug Guide — hosted by NDPERS, formulary updated 09/29/2025 — lists Zepbound Pen Injector on Tier 4 with prior authorization. That's not a guarantee your plan covers it, but it means you shouldn't accept a generic "Medicare doesn't cover weight-loss drugs" answer at face value if you're on a retiree plan. Read your Evidence of Coverage and ask Humana to confirm specifically for your contract.
Does Humana Healthy Horizons (Medicaid) cover Zepbound?
Answer capsule: Coverage varies by state. Humana currently lists Medicaid drug-list resources for Florida, Indiana, Kentucky, Louisiana, Ohio, Oklahoma, South Carolina, and Virginia. Each state's Medicaid program runs its own Preferred Drug List and prior authorization rules. KFF reported that 13 state Medicaid fee-for-service programs covered GLP-1s for obesity as of January 2026, but that's a national snapshot, not a Humana Healthy Horizons-specific number. The only reliable way to know what your plan covers is to call your state's Humana Medicaid line directly.
- Find your state's Humana Medicaid number on the back of your card.
- Ask specifically: "Is Zepbound covered on this state's PDL for [weight management / obstructive sleep apnea]?"
- If it's covered, ask for the prior authorization form and required documentation.
- If it's not on your state's PDL, ask about the medical exception process and appeal rights.
Medicaid PDL decisions change frequently. What's covered in 2026 may shift in 2027. Verify before you make any plan decision.
How to check your exact Humana Zepbound coverage in 10 minutes
Answer capsule: The fastest reliable check has three steps: sign in to MyHumana and search the formulary for "Zepbound," call the member-services number on the back of your card using a specific script, and write down the answer. The mistake most people make is asking "Do you cover Zepbound?" — that question doesn't tell you whether the issue is the formulary, the diagnosis, the formulation, or the prior authorization.
Step 1: MyHumana drug-list lookup
Sign in at humana.com or in the MyHumana app. Search the drug list for "Zepbound" and also for "tirzepatide" (the active ingredient name). Note three things: whether the drug appears, what tier it's on, and any letters next to it (PA, QL, ST — prior authorization, quantity limit, step therapy).
Step 2: The Humana coverage call script
COPY AND PASTE — have your member ID ready
"Hi, I'm calling to confirm coverage for Zepbound under my exact plan. My member ID is [NUMBER]. I need to know four things. One, is Zepbound on my plan's formulary, and if so, at what tier? Two, is it covered for [the diagnosis your doctor is using: weight management / moderate-to-severe obstructive sleep apnea in adults with obesity / etc.]? Three, which formulation is covered — single-dose pen, KwikPen, or single-dose vial? And four, is prior authorization, step therapy, or quantity limit required? If Zepbound isn't on my plan, can my prescriber request a formulary exception? Please give me a call reference number so I can document this conversation."
Step 3: The denial-language worksheet
If you've already been denied, write down everything from the denial letter:
- Date of denial
- Exact denial language (copy it word for word)
- Whether it says "PA required," "PA denied," "not on formulary," "not a covered benefit," or something else
- Appeal deadline
- Required documentation for appeal
- Reference number
That language tells you which row of the denial triage table below applies.
The Humana Zepbound prior authorization playbook
Answer capsule: A Humana prior authorization is won on documentation and lost on small mistakes. The most important factors are matching the diagnosis on the PA to a covered indication, submitting the correct ICD-10 codes, attaching complete documentation (including sleep studies for OSA cases), and using the exact Zepbound formulation your plan covers.
What to put in the PA — checklist
| Document | Why it matters |
|---|---|
| Current weight and BMI | Required to confirm obesity indication |
| Sleep study (polysomnogram or HSAT) results | Required for OSA pathway; AHI documentation must be on file |
| Primary diagnosis ICD-10 code | OSA = G47.33; weight management may use E66.x — confirm with the plan |
| Secondary diagnoses (Z68.xx for BMI category) | Supports the primary diagnosis |
| Comorbidities (HTN, T2D, CV disease) | Strengthens medical necessity |
| Medication history | Required if plan has step therapy |
| Prior weight-loss attempts | Required by some commercial plans |
| Prescriber statement | Confirms medical necessity in clinical language |
| Specific Zepbound formulation and dose | Must match what the plan covers |
| Formulary exception request | Use this if Zepbound isn't on your plan's formulary |
What not to do
- Don't use "weight loss" language alone on a Humana Medicare PA. Federal law blocks Medicare from covering drugs solely for weight loss. If you actually qualify for the OSA pathway, that's what the PA should describe.
- Don't assume Mounjaro = Zepbound for coverage purposes. They contain the same active ingredient (tirzepatide), but they're separate FDA-approved brand pathways with different indications.
- Don't fill at the pharmacy before the PA is approved. Humana states that some high-cost medications require PA, and filling without approval may leave the member responsible for the full cost.
- Don't appeal without the denial letter in hand. You need to know exactly what the plan said no to.
What to do if Humana denies Zepbound — the denial triage table
Answer capsule: Different denials need different responses. A "PA required" letter means coverage may exist but paperwork is missing — fix the paperwork. A "not a covered benefit" letter means the plan has a hard exclusion — appealing rarely works, and your time is better spent on the Bridge, OSA, or cash-pay paths. Get the actual denial letter, find your row, take the matching next step.
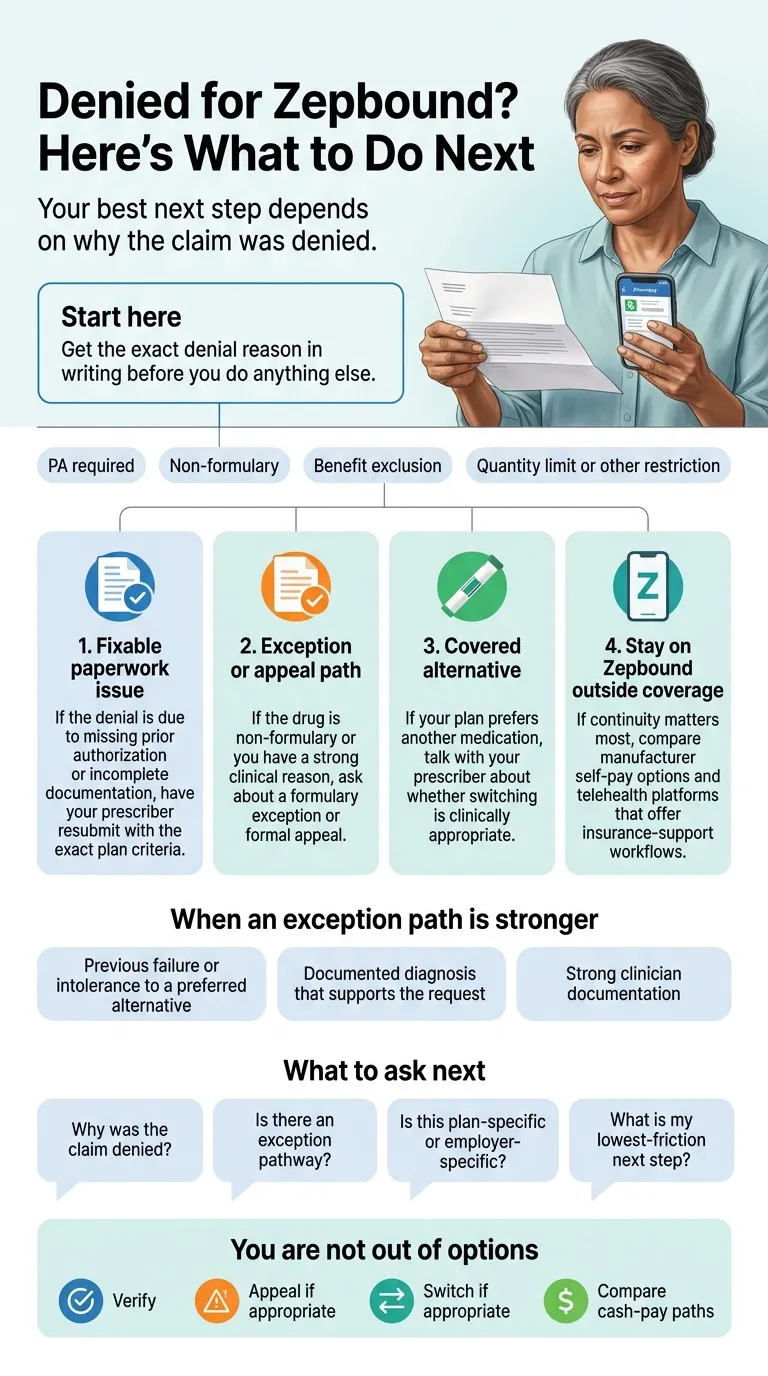
| Denial reason | What it actually means | Best next step |
|---|---|---|
| PA not submitted | Pharmacy billed without authorization; coverage may exist | Have prescriber submit PA |
| PA denied — missing documentation | Insurer reviewed but documents were incomplete | Get the letter; resubmit with sleep study, BMI, history |
| PA denied — diagnosis not covered | Diagnosis on claim doesn't match a covered indication | Verify the prescription's primary diagnosis matches a covered use |
| Denied — weight-loss exclusion | Plan doesn't cover anti-obesity meds at all | Skip the appeal; pursue Bridge (Medicare), formulary exception (rarely works), or cash-pay |
| Denied — despite OSA documentation | OSA proof was insufficient or didn't meet plan criteria | Review sleep study; resubmit with stronger evidence |
| Not on formulary | Drug isn't on this plan's covered list | Request a formulary exception |
| Wrong formulation | KwikPen/single-dose pen/vial mismatch with what's covered | Have prescriber and pharmacy verify formulation |
| Medicare Bridge–eligible (after July 1, 2026) | Claim should route through central processor | Use Bridge process via the prescriber |
| Medicaid denial | State PDL / PA rules apply | Check state Medicaid appeal rights |
Before you spend another two months on appeals, run Ro's free coverage checker (commercial plans only). Ro can help clarify what your plan reports about GLP-1 coverage and whether prior authorization may be required. If the answer is "no path here," Ro can route eligible cash-pay patients to FDA-approved Zepbound KwikPen at LillyDirect-style pricing.
Run My Commercial Coverage Check Before the Next PA →What to do if Humana won't cover Zepbound: the cash-pay paths that work
Answer capsule: If Humana denies Zepbound and the denial isn't fixable, three legal cash-pay paths remain. One: get FDA-approved Zepbound vials direct from Eli Lilly's LillyDirect Self Pay Journey at $299/month (2.5 mg starter), $399/month (5 mg), or $449/month (7.5–15 mg vials with the 45-day refill discipline). Two: get Zepbound KwikPen cash-pay through Ro at the same Lilly self-pay pricing. Three: push your employer to add GLP-1 coverage at the next open enrollment cycle.
Path 1: LillyDirect Self Pay Journey vials — the cheapest legal route
Eli Lilly sells Zepbound directly through LillyDirect at these prices (verified May 2026):
| Dose | Self-pay price with 45-day refill discipline | Regular self-pay price (if you miss the 45-day window) |
|---|---|---|
| 2.5 mg vial (starter dose) | $299/month | $299/month |
| 5 mg vial | $399/month | $399/month |
| 7.5 mg vial | $449/month | $499/month |
| 10 mg vial | $449/month | $699/month |
| 12.5 mg vial | $449/month | $699/month |
| 15 mg vial | $449/month | $699/month |
| 7.5–15 mg KwikPen | $449/month | $499–$699/month (by dose) |
Path 2: Ro's Zepbound KwikPen cash-pay
Ro sells the FDA-approved Zepbound KwikPen at the same LillyDirect Self Pay Journey pricing — $299 (2.5 mg), $399 (5 mg), and $449/month for 7.5 through 15 mg with the same 45-day refill rule. Medication is billed separately from Ro Body membership — listed at $39 for the first month, then $149/month if paid monthly, or as low as $74/month with annual prepay. The membership covers provider visits, lab work where appropriate, and (for eligible non-government insurance) an insurance concierge. If you have a Humana commercial plan, Ro's free coverage check might find a covered path you missed before you commit to cash-pay.
Path 3: Push your employer at open enrollment
If your Humana coverage is employer-sponsored and the plan doesn't include GLP-1s, the lever is your employer — not Humana. Three useful talking points: (1) The 2026 Part D cap of $2,100 has changed the cost math for self-funded employer plans. (2) GLP-1 coverage with PA criteria can be cost-managed, not unlimited. (3) Direct-to-consumer pricing means even partial reimbursement at $299–$449/month is meaningfully cheaper than the old $1,000+ retail.
Cash-pay decision: what to pick
- Start with Ro if you have a Humana commercial card and aren't 100% sure about coverage. The free check costs nothing and might find a path you missed.
- Go direct to LillyDirect if you've already confirmed Humana won't cover, prefer vials, and want the absolute lowest sticker price (no membership cost).
- Pick Ro KwikPen if you'd rather have provider support, automatic refill reminders, and the pen rather than syringes.
Can you use the Zepbound savings card with Humana?
Answer capsule: Maybe — and only if you have Humana commercial insurance, not Medicare or Medicaid. Eli Lilly's Zepbound Savings Card terms exclude anyone enrolled in any state, federal, or government-funded healthcare program. Commercially insured Humana members whose plan covers Zepbound may pay as little as $25 for a single-dose pen fill, subject to Eli Lilly's program limits.
| Your Humana coverage | Can you use the Zepbound Savings Card? |
|---|---|
| Humana commercial / employer plan (covers Zepbound) | Yes, may pay as little as $25/month under Lilly's terms |
| Humana Medicare Advantage / Part D | No — government-funded plan, excluded |
| Humana Medicare Employer Plan | No — still government-funded |
| Humana Healthy Horizons Medicaid | No — Medicaid is excluded |
| No coverage, paying cash | No, but you can use the Self Pay Journey pricing instead |
The Lilly commercial savings card applies to the Zepbound single-dose pen formulation. CMS has been explicit on the Bridge: coupons and manufacturer discount programs cannot be applied to Medicare GLP-1 Bridge claims. The Bridge $50 copay is the price. Verify current terms at zepbound.lilly.com/savings before assuming anything.
What about Mounjaro? Compliance note
Don't try to switch to Mounjaro as an insurance workaround for Zepbound. Mounjaro and Zepbound contain the same active ingredient (tirzepatide), but they're separate FDA-approved brand pathways with different indications. Mounjaro is FDA-approved for type 2 diabetes management; Zepbound is FDA-approved for weight reduction and moderate-to-severe OSA in adults with obesity. Insurance coverage follows the brand and the FDA indication on the prescription, not the active ingredient.
Some patient forums suggest asking a doctor to prescribe Mounjaro "off-label" for weight management to bypass a Zepbound denial. That's a clinical decision — not a coverage hack — and most insurers screen for it. Ask your doctor which FDA-approved medication is appropriate for your actual diagnosis.
Is Zepbound safe for everyone Humana might cover?
No. Coverage approval doesn't mean Zepbound is medically right for every person, and a prescriber must evaluate medical history, contraindications, drug interactions, pregnancy considerations, and side-effect risk before prescribing.
Zepbound has a boxed warning for risk of thyroid C-cell tumors and is contraindicated in people with a personal or family history of medullary thyroid carcinoma or Multiple Endocrine Neoplasia syndrome type 2 (MEN 2). The FDA prescribing information also describes risks including severe gastrointestinal adverse reactions, pancreatitis, gallbladder disease, hypoglycemia when used with insulin or insulin secretagogues, and monitoring requirements for suicidal behavior or ideation. This page explains coverage pathways, not medical suitability. Your clinician decides whether Zepbound is appropriate for your health history.
Real Humana members on the Zepbound question
Public forum discussions show three consistent friction points for Humana members trying to access Zepbound: getting clear answers from member services, navigating the prior authorization process, and figuring out whether a denial is fixable or final. These are anecdotal patient experiences from public forums — not coverage policy, and not evidence of typical results.
"I called Humana… The agent told me they don't cover Zepbound… The agent told me I had to get 'prior authorization' from my doctor."
— Public Reddit post, r/medicare, 2025
"This is my second time submitting a PA and was denied… Am I missing something? What can I do to submit or appeal?"
— Public Reddit post, r/Zepbound, 2025
The pattern in these posts is consistent: confusion when the agent says "we don't cover it" without explaining whether that means the plan, the diagnosis, or the formulation. Denials usually happen when the diagnosis on the claim doesn't match a covered indication, or when documentation is thin. Translation: the first phone call rarely tells you the full picture. Get the specific reason in writing, document it, and pick your next step from the triage table above.
What we actually verified for this guide
Trust requires showing our work. Here's what we directly confirmed before publishing, with dates and sources.
- Humana Medicare Drug List page — confirmed Humana directs members to sign in to MyHumana to search their specific plan's covered drug list and pricing. (humana.com/pharmacy/medicare-drug-list, accessed May 14, 2026)
- 2026 Humana Medicare Employer Plan Comprehensive Drug Guide — confirmed Zepbound Pen Injector listed on Tier 4 with prior authorization. (NDPERS-hosted PDF, formulary updated 09/29/2025)
- Humana Prior Authorization Guidelines — confirmed Humana states high-cost/high-risk medications may require PA and that filling without approval may leave the member responsible for all costs. (humana.com/pharmacy/prior-authorization-medication-approvals, accessed May 14, 2026)
- CMS Medicare GLP-1 Bridge FAQ — confirmed July 1, 2026 launch, December 31, 2027 end date, Humana as central processor, $50 copay, Zepbound KwikPen-only Bridge eligibility, and the three clinical eligibility paths. (cms.gov, May 2026)
- Zepbound FDA Prescribing Information — confirmed FDA indications include adult weight reduction and moderate-to-severe OSA in adults with obesity, and the boxed warning for thyroid C-cell tumors. (accessdata.fda.gov, 2026 label revision)
- Eli Lilly Zepbound Self Pay Journey Program terms — confirmed all dose-specific cash-pay pricing and the 45-day refill discipline rule. (lilly.com/lillydirect, accessed May 14, 2026)
- Eli Lilly Zepbound Savings Card terms — confirmed government-insurance exclusions and the "as little as $25" benefit for eligible commercial single-dose pen fills. (zepbound.lilly.com/savings, accessed May 14, 2026)
- Ro GLP-1 Insurance Coverage Checker — confirmed Ro publicly describes a free coverage check that contacts the insurance plan by phone, collects eligibility information, and generates a personalized report. (ro.co/weight-loss/glp1-insurance-checker, accessed May 14, 2026)
- Ro Body Membership pricing — confirmed $39 first month, $149/month ongoing, or as low as $74/month with annual plan. Medication billed separately. (ro.co/weight-loss/pricing, accessed May 14, 2026)
- Business Group on Health 2026 GLP-1 Survey — confirmed 67% of surveyed employers currently cover GLP-1s for weight management; 72% of those covering them said they were likely to continue in 2027. (businessgrouphealth.org, 2026)
- Humana provider drug-list page — confirmed Humana lists Medicaid drug-list resources for Florida, Indiana, Kentucky, Louisiana, Ohio, Oklahoma, South Carolina, and Virginia. (provider.humana.com, accessed May 14, 2026)
- KFF Medicaid GLP-1 coverage analysis — confirmed 13 state Medicaid fee-for-service programs covered GLP-1s for obesity as of January 2026. (kff.org)
Next scheduled review: July 2026, or sooner if Humana, CMS, Eli Lilly, or Ro publishes a meaningful change.
Take the next step — based on your situation
If you have Humana commercial / employer insurance
Have Ro check your specific plan for free. The check is just a coverage report — no commitment, no prescription written.
Check My Humana Commercial Coverage with Ro →If you have Humana Medicare and you'll qualify for the Bridge
Mark July 1, 2026 on your calendar. Make sure your doctor has BMI history and any qualifying conditions on file. Your prescription must specify Zepbound KwikPen formulation to be Bridge-eligible.
See If You Qualify for the Medicare GLP-1 Bridge →If you have Humana Medicare and want Zepbound for sleep apnea
Use the MyHumana call script above. Ask specifically about Zepbound for moderate-to-severe OSA in adults with obesity, and ask whether your plan handles it through normal formulary rules or requires a coverage determination.
If you have Humana Medicaid
Call your state's Humana Healthy Horizons line. Coverage is state-specific and changes — there's no shortcut here.
If no Humana coverage path applies
You don't have to wait or appeal forever. LillyDirect Self Pay Journey vials are $299–$449/month — same FDA-approved medication, no insurance fight.
Compare LillyDirect vs. Ro KwikPen →Still not sure which path is yours?
Take our free 60-second matching quiz. We'll route you to the right Zepbound path based on your Humana plan, diagnosis, and BMI. No insurance card needed to start.
Take the 60-Second Match Quiz →Frequently asked questions
Does Humana cover Zepbound in 2026?
Sometimes. Coverage depends on your specific Humana plan, the diagnosis on the prescription, the formulation, and prior authorization rules. Some Humana Medicare Employer Plans list Zepbound on Tier 4 with PA. Standard Humana Medicare Part D plans don't cover Zepbound for weight loss alone, but may cover it for moderate-to-severe OSA in adults with obesity through normal formulary rules. Humana commercial plans vary widely by employer. Humana also administers the Medicare GLP-1 Bridge starting July 1, 2026 as the CMS central processor.
Does Humana cover Zepbound for weight loss?
For Humana commercial and employer plans, weight-management coverage is plan-specific — some include anti-obesity medications, many exclude them. Standard Humana Medicare Part D plans don't cover Zepbound for weight loss alone because federal law blocks Medicare from covering weight-loss drugs. Starting July 1, 2026, eligible Medicare Part D members can get Zepbound KwikPen at $50/month through the Medicare GLP-1 Bridge.
Does Humana Medicare cover Zepbound for sleep apnea?
It may be coverable through normal Part D formulary or coverage-determination rules, subject to your plan's PA and exception requirements. CMS confirmed in 2026 that Zepbound for moderate-to-severe OSA in adults with obesity may be handled through basic Part D rules and is not routed through the Medicare GLP-1 Bridge. Verify in MyHumana or by calling Humana directly.
Why did Humana deny my Zepbound prescription at the pharmacy?
A pharmacy rejection can happen before a full PA review if the medication requires prior authorization, the submitted diagnosis doesn't match the plan's covered use, the formulation doesn't match the plan record, or the drug is excluded from the benefit entirely. Get the exact denial language in writing before deciding whether to appeal, resubmit, or move to another path.
Does the Medicare GLP-1 Bridge through Humana cover Zepbound?
Yes. Zepbound KwikPen is one of three drugs covered by the Bridge starting July 1, 2026. Eligible Medicare Part D members pay $50/month. Qualifying criteria: BMI of 35 or higher; OR BMI of 30 or higher plus HFpEF, uncontrolled hypertension, or CKD stage 3a or above; OR BMI of 27 or higher plus prediabetes, prior heart attack, prior stroke, or symptomatic peripheral artery disease. Humana is the CMS central processor for the Bridge nationally, not just for Humana members.
Which Zepbound formulation matters for Humana coverage?
Formulation affects every path. The Medicare GLP-1 Bridge covers Zepbound KwikPen only — not vials or the original single-dose pen. The Eli Lilly commercial savings card terms apply specifically to single-dose pen fills. LillyDirect's self-pay program covers both vials and KwikPen at the same dose-by-dose pricing. Confirm the exact formulation on your prescription before you fill anything.
Does Humana require prior authorization for Zepbound?
Often, yes. Humana states that high-cost or high-risk medications may require prior authorization, and filling a PA-required drug without approval can leave the member responsible for the full cost. At least one 2026 Humana Medicare Employer Plan formulary lists Zepbound with PA. Verify the PA flag in your exact plan drug list.
Can I use the Zepbound Savings Card with Humana?
Only if your Humana plan is commercial (employer or individual). Medicare, Medicare Advantage, Medicaid, and other government-funded plans are excluded from Eli Lilly's commercial savings card terms. Commercially insured Humana members whose plan covers Zepbound may pay as little as $25/month under the program for the single-dose pen.
How much does Zepbound cost without Humana coverage?
The cheapest legal cash-pay path is Eli Lilly's LillyDirect Self Pay Journey: $299/month for 2.5 mg vials (starter dose), $399 for 5 mg, and $449 for 7.5–15 mg vials with refills within 45 days. Miss the 45-day window for higher doses and the regular self-pay price applies — currently $499 for 7.5 mg and $699 for 10 mg, 12.5 mg, or 15 mg.
How long does a Humana Zepbound prior authorization take to approve?
For Medicare Part D coverage determinations, CMS requires plans to respond within 72 hours for standard requests or 24 hours for expedited requests. Humana's specific Zepbound approval duration and reauthorization criteria vary by plan and indication — don't assume a universal approval length or reauthorization rule until your plan's PA criteria or determination letter confirms it.
Should I switch from Zepbound to Mounjaro because Humana covers it?
No — and don't ask your doctor to swap brands for insurance reasons. Mounjaro and Zepbound contain the same active ingredient but are FDA-approved for different conditions. Mounjaro is for type 2 diabetes; Zepbound is for weight reduction and OSA in adults with obesity. The right medication is a clinical decision based on your diagnosis, not a coverage workaround.
Related insurance and coverage guides
Sources
- Humana — Medicare Prescription Drugs List and Rx Availability. humana.com/pharmacy/medicare-drug-list
- Humana — Prior Authorization Guidelines and Forms. humana.com/pharmacy/prior-authorization-medication-approvals
- Humana — Drug lists for providers (Medicaid state resources). provider.humana.com/pharmacy-resources/tools/humana-drug-lists
- NDPERS — 2026 Humana Medicare Employer Plan Comprehensive Drug Guide (formulary updated 09/29/2025). ndpers.nd.gov
- CMS — Medicare GLP-1 Bridge FAQ. cms.gov/medicare/coverage/prescription-drug-coverage/medicare-glp-1-bridge
- CMS — Coverage Determinations. cms.gov/medicare/appeals-grievances/prescription-drug/coverage-determinations
- KFF — Medicaid Coverage of and Spending on GLP-1s. kff.org/medicaid
- FDA — Zepbound (tirzepatide) Prescribing Information, 2026 revision. accessdata.fda.gov
- Eli Lilly — Zepbound Savings Options. zepbound.lilly.com/savings
- Eli Lilly — Zepbound Self Pay Journey Program Terms. lilly.com/lillydirect/medicines/zepbound
- Ro — GLP-1 Insurance Coverage Checker. ro.co/weight-loss/glp1-insurance-checker
- Ro — Weight Loss Program Pricing. ro.co/weight-loss/pricing
- Medicare.gov — Part D Costs. medicare.gov/health-drug-plans/part-d/basics/costs
- Business Group on Health — 2026 GLP-1 Survey. businessgrouphealth.org/newsroom