Affiliate disclosure: The RX Index earns a commission when you sign up with some of the providers mentioned on this page. It does not affect what you pay, and it never determines our rankings or which providers we cover. Read the full disclosure.
How to Check if GLP-1 Is Covered by Insurance in 2026
Published: · Last updated:
By The RX Index Research Team • Last verified: April 18, 2026 • Published April 18, 2026
The RX Index is a pricing intelligence and comparison resource for GLP-1 telehealth providers.
Not medical, legal, or financial advice. Coverage policies and pricing change — always verify with your specific plan and provider before making a treatment decision.
Disclosure: Some links on this page are affiliate links. If you purchase through these links, we may earn a commission at no extra cost to you.

The fastest way to check if GLP-1 is covered by insurance: pull out your insurance card, open the pharmacy-benefit tool printed on the back (CVS Caremark, Express Scripts, Optum Rx, etc.), and search the formulary for the exact drug name — Wegovy, Zepbound, Ozempic, Mounjaro, Saxenda, Rybelsus, or Foundayo. Then call the 800 number on that same card and confirm three things: is the drug covered for your specific diagnosis, is prior authorization required, and is it an excluded benefit or just non-formulary.
Here’s what most people get wrong: insurance doesn’t cover “GLP-1s.” It covers a specific drug for a specific diagnosis under a specific plan’s rules for the current year. That’s why your coworker pays $25 and you’re staring at a $1,080 price tag.
What’s actually at stake
The cost difference between “covered” and “not covered” isn’t small. Without coverage, branded GLP-1s run over $1,000/month at retail. With commercial-insurance coverage and a manufacturer savings card, eligible patients can pay as little as $25/month on Zepbound and Wegovy. That’s not a rounding error — it’s the difference between doing this and not.
And the landscape just shifted. Through 2025 and into 2026, several major insurers tightened GLP-1 rules significantly. CVS Caremark removed Zepbound from its standard commercial formularies on July 1, 2025. Mass General Brigham Health Plan, Health New England, and Fallon Health Community Care dropped GLP-1 weight-management coverage for 2026. Your 2025 answer may not be your 2026 answer.
Start here: build your 5-minute GLP-1 coverage plan
Answer four quick questions — your insurer, drug, diagnosis, and plan type — and we’ll give you the right tool to use first, the exact script to read, and your best next step if the answer is no.
Build my 5-minute GLP-1 coverage plan →How to Check if GLP-1 Is Covered by Insurance: The 5-Step Verification Protocol
Run these five steps in order — pharmacy-benefit tool, phone call, pharmacist test claim, prescriber confirmation, and HR. Most people get a real answer by step 2. Total time: 15–30 minutes. Each step catches what the step before it missed.
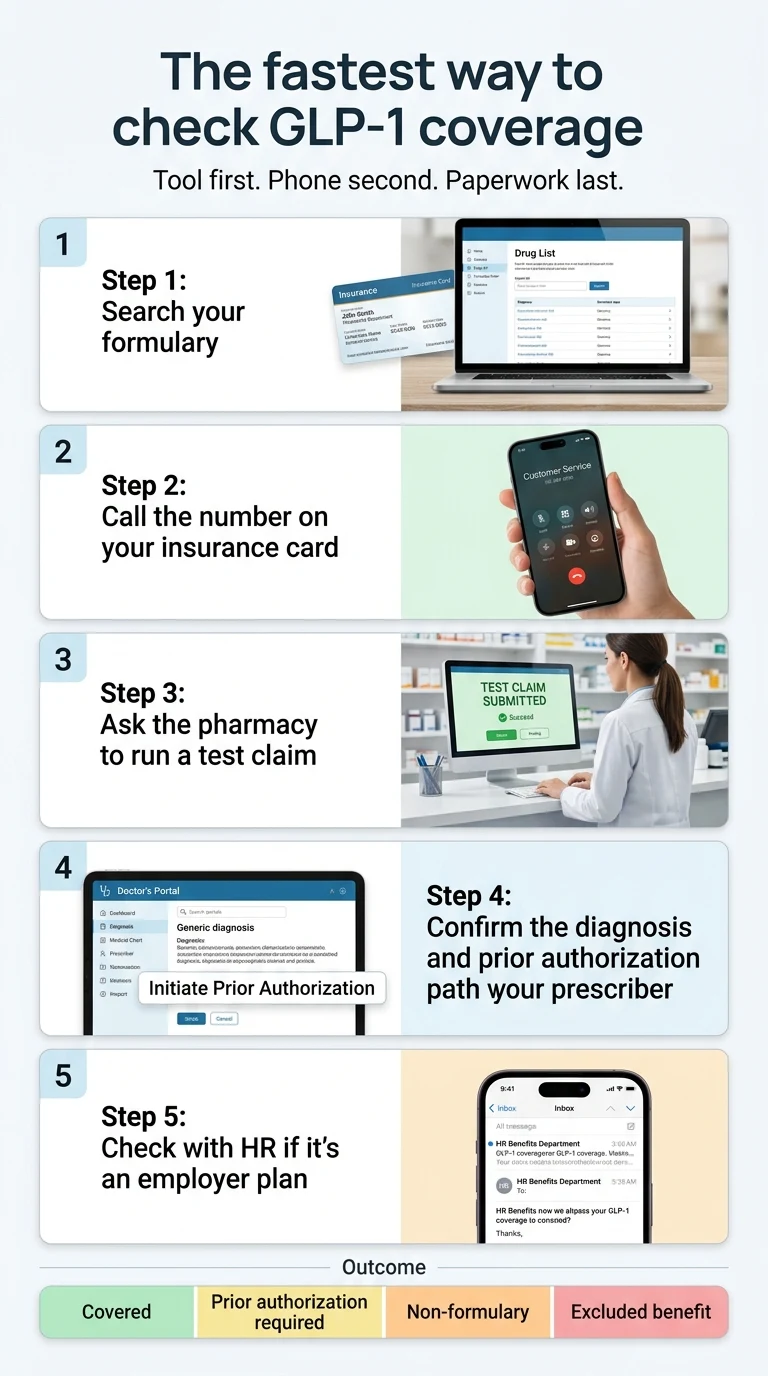
Find your formulary and search the exact drug (2 minutes)
Your formulary (sometimes called a “prescription drug list” or PDL) is your insurance plan’s list of covered medications. Flip over your insurance card — the PBM is printed somewhere. The three big ones:
CVS Caremark
Runs Aetna and many employer plans
Express Scripts
Runs Cigna and many employer plans
Optum Rx
Runs UnitedHealthcare
Go to that PBM’s member site, log in, and search for the exact brand name your doctor prescribed. Don’t search “semaglutide” if your prescription says “Wegovy.” Don’t search “tirzepatide” if it says “Zepbound.”
What you’re looking for in the result:
- A tier number (1–6; lower tier = lower copay)
- Restriction codes: PA (prior authorization), ST (step therapy), QL (quantity limit), AL (age limit), or NF (non-formulary)
- Your estimated copay or coinsurance
Call the 800 number on your card (5–10 minutes)
This is the step most people skip. Don’t. The portal can say one thing and the actual claim can adjudicate differently. A five-minute phone call gets you a real answer and, critically, a reference number you can point to later if you need to appeal. The exact 7-question script is below — copy it before you dial.
Ask your pharmacist for a test claim (5 minutes)
Your pharmacist can run your prescription through your insurance without actually filling it. The claim comes back with a real rejection code (or an approval) that tells you exactly what the plan does.
Call the pharmacy and ask: “Can you run a test claim on [drug name] against my insurance and tell me what the rejection reason is, if any?”
Loop in your prescriber’s office (3 minutes)
Most telehealth clinics and weight-management practices have an internal benefits-check workflow. Email or portal-message them: “Can you verify whether my insurance covers [drug] for [diagnosis] and start a prior authorization if needed?”
Verify with HR if it’s an employer plan (5 minutes)
This is the gotcha of 2026. Self-funded employers — the ones who use an insurer like Aetna or UHC just to administer the plan, not to actually insure it — can add or remove GLP-1 coverage independently of whatever the PBM’s default formulary says. Caremark.com might show “Wegovy covered.” Your employer plan might have carved out weight-loss drugs.
Email HR or your benefits administrator:
- “Does our plan cover GLP-1 medications for weight management?”
- “If yes, what’s the prior authorization process?”
- “If no, is there a pathway for a medical exception?”
Which Coverage-Check Tool Should You Use First?
Use the tool closest to your actual pharmacy benefit. PBM member tools (Caremark, Express Scripts, Optum Rx) are usually the best first stop; manufacturer tools (NovoCare for Wegovy, Lilly for Zepbound) are best for single-drug cost estimates; and done-for-you checkers (Ro, Found) are best when you want someone else to handle the insurer call. No single tool gives you everything — use them in combination.
How to pick in 30 seconds:
- You have time and a member login: Start with your PBM tool (step 1), then call to confirm.
- You only want to check one drug: The manufacturer tool (NovoCare, Lilly’s Zepbound tool, LillyDirect for Foundayo) gives you a fast read.
- You don’t want to deal with insurance yourself: Ro’s free checker calls your insurer on your behalf (commercial insurance only).
- You’re already denied: Skip to What to Do If You’re Denied.
The RX Index GLP-1 Coverage Check Route Matrix — April 2026
| Route | Best for | What it gives you | Biggest caveat |
|---|---|---|---|
| Call your insurer/PBM directly | The final, authoritative answer for your exact plan | Plan-specific coverage, PA rules, exclusion status, reference number | Requires good questions; rep answers can be incomplete unless you push |
| CVS Caremark — Check Drug Cost and Coverage | Members whose card routes through Caremark (Aetna, many employer plans) | Coverage status, covered alternatives, and estimated cost | Login required; plan-specific |
| Express Scripts — Price a Medication | Express Scripts / Cigna members | Coverage status and pricing info | Requires member access |
| Aetna personalized medication search | Aetna members | Coverage check, retail vs. mail-order pricing, generic alternatives | Login required; some plans route through Caremark instead |
| Optum Rx Drug Pricing tool | Optum Rx / UnitedHealthcare members | Coverage, pricing when covered, or “Drug not covered” notice | Details vary by benefit setup |
| Cigna / myCigna drug list + member portal | Cigna members | Coverage under your specific plan; PDL lookup | Login required for plan-specific detail |
| UnitedHealthcare PDL + member tools | UHC members | Plan-specific formulary view and pharmacy-benefit details | Most detail sits behind login |
| NovoCare Wegovy cost & coverage tool | Checking Wegovy specifically | Coverage lookup + estimated out-of-pocket cost | Single drug only |
| Zepbound coverage & access tool (Lilly) | Checking Zepbound specifically | Coverage check + savings options | Not a guarantee; Lilly directs users to confirm with insurer |
| LillyDirect — Foundayo & Zepbound self-pay | Readers who want direct-to-consumer pricing | Self-pay pricing without a coverage check | Self-pay only, not an insurance check |
| Ro GLP-1 Insurance Coverage Checker | Commercially insured readers who want a done-for-you call | Free personalized coverage report including PA status and copay estimates | Commercial insurance only; does not coordinate government plan coverage |
| Found GLP-1 Coverage Checker | Readers who want a report plus ongoing obesity-care support | Coverage breakdown per drug, PA status, estimated copays when available | Commercial workflow, not a neutral resource |
| WeightWatchers Cost Estimator | Readers who want a quick cost ballpark | Fast estimate based on member experiences | Estimator, not plan verification |
Source: The RX Index, verified April 18, 2026. Your specific plan’s rules may differ from any tool’s estimate.
The Exact Phone Script
A good phone call distinguishes between four very different outcomes: covered, covered with PA, non-formulary but switchable, and excluded benefit. Ask the seven questions below in order. Save the call reference number. Get the plan’s written policy link if you can.
Before you dial — have ready:
- Your member ID
- Your date of birth
- The exact name and dose of the drug your doctor prescribed (e.g., “Wegovy 0.25 mg injection”)
- The diagnosis your doctor is using (e.g., “weight management with BMI 32 and hypertension” or “type 2 diabetes”)
Opening line when they pick up:
“Hi, I need to check pharmacy coverage for a specific medication. My member ID is [XXXX]. The drug is [Wegovy / Zepbound / Ozempic / etc.] prescribed for [diagnosis]. I have seven questions.”
The seven questions, in order:
- 1
"Is [drug] on my plan's formulary?" (If no, skip to question 5.)
- 2
"What tier is it on, and what's my copay or coinsurance at that tier?"
- 3
"Does it require prior authorization?"
→ If yes: "Can you email or mail me the PA criteria and the form my doctor needs to complete?"
- 4
"Does my plan require step therapy for this drug?"
→ If yes: "Which drugs count as the required step, and how long does the trial need to be?"
- 5
"Is this drug covered for [my diagnosis], or only for other uses like type 2 diabetes or cardiovascular risk reduction?"
- 6
"Is this drug listed as non-formulary, or is it an excluded benefit?"
→ Most important question. Non-formulary often has a path. Excluded benefit usually doesn't.
- 7
"What pharmacy do I have to use — retail, mail-order, or specialty?"
Before you hang up:
- “What’s the reference number for this call?” Write it down.
- “Can you email me a summary of what we discussed, or point me to the written coverage policy?”
- Get the rep’s first name.
That call, done right, takes under 10 minutes and gives you everything you need for step 3 onward.
What “Covered” Actually Means (And Doesn’t)
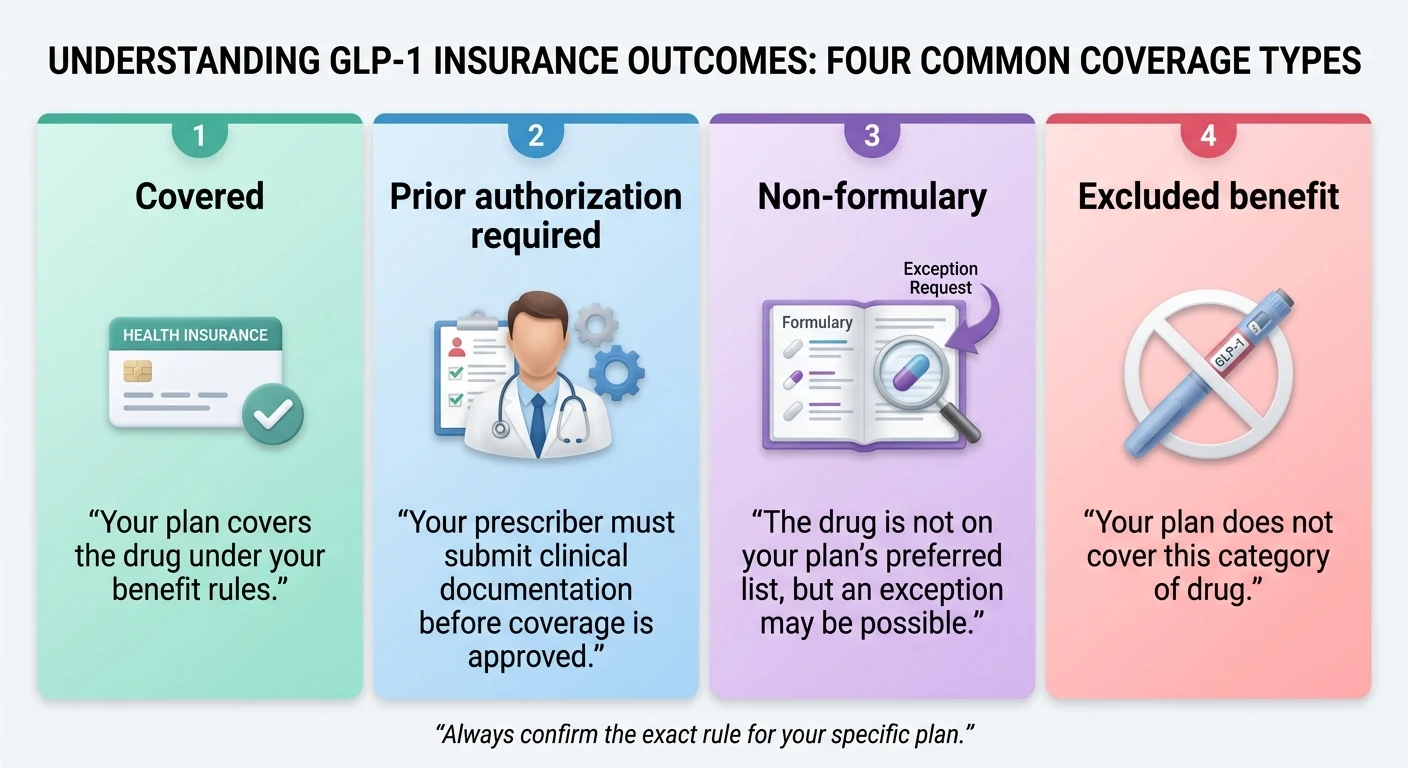
“Covered” is not the same as “free,” and “PA required” is not the same as “excluded.” Four terms do most of the damage.
| Term | What it means | Your next step |
|---|---|---|
| Prior authorization (PA) | The plan can cover it, but only after your prescriber submits clinical documentation proving medical necessity | Get the PA form, have your prescriber submit with BMI, labs, and diagnosis |
| Step therapy (ST) | The plan requires you to try — and fail or be intolerant to — a lower-cost alternative first | Ask which drugs qualify as the step; document any prior trials |
| Non-formulary (NF) | The drug isn’t on your plan’s preferred list, but an exception may be possible | Request a formulary exception with clinical justification |
| Excluded benefit | The plan has chosen not to cover this category of drug at all — often “weight-loss medications” as a class | Appeal rarely wins; look at alternate FDA indication, manufacturer cash program, or self-pay |
Covered ≠ affordable
Even when your plan covers a GLP-1, you might still pay hundreds of dollars until you hit your deductible. Before you celebrate a “covered” answer, ask your PBM rep:
- What’s my cost before I hit my deductible?
- What’s my cost after I hit my deductible?
- Is there a copay accumulator that blocks manufacturer savings cards from counting toward my deductible?
Don’t skip that third question. Copay accumulators are an underreported gotcha that can blow your math for the year.
Does Your Diagnosis Change the Answer?
Yes — this is the biggest hidden lever in GLP-1 coverage. Insurance approves a specific drug for a specific FDA-approved indication, so the same molecule can be easy to cover for type 2 diabetes and almost impossible to cover for weight loss alone. If weight management is blocked on your plan, an alternate FDA indication you already qualify for (cardiovascular risk, obstructive sleep apnea, MASH) may unlock coverage you thought was gone.
| Your situation | Best-fit drug(s) | Coverage odds on commercial insurance |
|---|---|---|
| Type 2 diabetes | Ozempic, Mounjaro, Trulicity, Rybelsus, Victoza | Strongest. Usually covered with PA on most commercial plans; diabetes is the most accepted indication by insurers |
| Weight management only, BMI ≥30 (or ≥27 + comorbidity) | Wegovy, Zepbound, Saxenda, Foundayo | Mixed. Roughly 43% of companies with 5,000+ employees cover GLP-1s for weight loss, dropping to 30% at 1,000–4,999 and 16% at 200–999 employees per KFF data reported for 2025 |
| Obesity + established cardiovascular disease | Wegovy (cardiovascular risk reduction indication) | Better than weight-only. CV indication can unlock coverage that pure obesity can’t |
| Obesity + moderate-to-severe obstructive sleep apnea | Zepbound (OSA indication) | Newer pathway. Unlocks coverage on many plans that exclude weight-loss-only use |
| Type 2 diabetes + chronic kidney disease | Ozempic | Strong. Approved CKD indication reinforces the T2D coverage case |
| Obesity + noncirrhotic MASH with moderate-to-advanced (F2–F3) liver fibrosis | Wegovy (MASH accelerated approval, August 2025) | New lane. FDA accelerated approval can unlock coverage when weight-loss alone would not |
The BMI and comorbidity bar most plans set for weight management coverage:
- BMI ≥30, OR
- BMI ≥27 with at least one weight-related comorbidity — hypertension, dyslipidemia, obstructive sleep apnea, cardiovascular disease, prediabetes, or fatty liver disease
Some plans set the bar higher — BMI ≥35, multiple comorbidities, or documented participation in a structured weight-loss program. That’s the plan’s call, not a clinical standard.
Foundayo is a weight-management drug — not a diabetes drug (yet)
Foundayo (orforglipron, FDA-approved April 1, 2026) is currently approved only for chronic weight management in adults with obesity or overweight with at least one weight-related comorbidity. It is not FDA-approved for type 2 diabetes as of April 18, 2026. If you’re being prescribed Foundayo, coverage will typically follow weight-management rules, not diabetes rules.
How Much Does GLP-1 Cost With Insurance?
Even with insurance, “covered” doesn’t mean $25. Real out-of-pocket cost depends on your deductible status, your plan’s coinsurance percentage, whether a manufacturer savings card applies, and whether your plan uses a copay accumulator. Typical ranges:
With coverage + manufacturer savings card
For eligible commercially insured patients on the Zepbound Savings Card, Lilly’s published terms advertise pricing as low as $25/month (max $100 monthly savings, max $1,300 annual savings). The Wegovy Savings Offer advertises $199 for each of the first 2 monthly fills of 0.25 mg or 0.5 mg through June 30, 2026 for eligible new users, then $349/month standard and $399/month for Wegovy HD 7.2 mg.
Note: Gotcha: savings cards generally exclude government insurance (Medicare, Medicaid, TRICARE) and have per-fill and annual caps.
With coverage, no savings card, deductible unmet
If you haven’t hit your plan deductible yet (often $1,500–$4,000 on high-deductible plans), you may pay the full negotiated drug price — often $700–$1,000 — until the deductible is satisfied. Coinsurance after deductible typically runs 20–40%.
With coverage, deductible met, “just” coinsurance
Even in the best plan scenario, 20% coinsurance on a $1,000 drug is $200/month. Many plans cap out-of-pocket maximums, which can reduce this ceiling but doesn’t eliminate it.
Cash price (no coverage)
Wegovy via NovoCare Pharmacy: $149–$399/month depending on formulation and dose. Zepbound self-pay via LillyDirect (KwikPen): $299/month for 2.5 mg, $399 for 5 mg, $449 for 7.5/10/12.5/15 mg. Foundayo via LillyDirect: self-pay starting at $149/month for the lowest dose. Compounded semaglutide or tirzepatide via telehealth: $200–$500/month depending on provider.
Note: Always verify current pricing at checkout — manufacturer programs change periodically.
Verified 2025–2026 GLP-1 Coverage Changes
Through 2025 and into 2026, several specific commercial plans and PBMs tightened or removed weight-loss GLP-1 coverage. The table below reflects verified changes with effective dates we could source directly to the insurer, PBM, or government agency. It is not a universal carrier matrix — your specific employer group or affiliate plan may differ. Always confirm with your own formulary.
| Date | Entity | Change |
|---|---|---|
| January 1, 2025 | BCBS of Michigan | Coverage change for GLP-1 drugs for certain fully insured large-group commercial members |
| January 1, 2025 | Kaiser Permanente (selected plans) | Coverage reductions for select GLP-1s on specific plans |
| July 1, 2025 | CVS Caremark (standard commercial formularies) | Zepbound removed from Standard Control, Advanced Control, and Value formularies; Wegovy remained preferred |
| August 31, 2025 | TRICARE For Life | Weight-loss GLP-1 coverage (Wegovy, Zepbound) ended for TRICARE For Life beneficiaries; diabetes indications continue with PA |
| January 1, 2026 | Mass General Brigham Health Plan | Dropped GLP-1s for weight management on fully insured commercial plans; diabetes coverage unchanged |
| January 1, 2026 | Health New England | Dropped Wegovy / Zepbound / Saxenda for individual and small group commercial |
| January 1, 2026 | Fallon Health Community Care | Weight-loss GLP-1 coverage removed |
| 2025–2026 | Point32Health / Harvard Pilgrim | Weight-loss medication coverage exclusions announced for many 2026 products |
| 2025–2026 | Various BCBS affiliates, UHC and Cigna employer plans | Plan-level tightening; many employer plans moved to type 2 diabetes–only. Inclusion in a carrier formulary does not guarantee coverage on your specific plan. |
Quick carrier orientation (your specific plan rules are still on your formulary)
- BCBS: Varies significantly by state affiliate and plan type. Several affiliates (including Michigan) have reduced or restricted weight-loss GLP-1 coverage. Always check your specific BCBS affiliate’s formulary.
- UnitedHealthcare / Optum Rx: Some Optum Rx formularies continued to list Zepbound after CVS Caremark dropped it. UHC’s provider materials note that inclusion in its prior-authorization list does not indicate a drug is covered by any particular plan.
- Aetna / CVS Caremark: On standard commercial formularies, Wegovy is preferred over Zepbound per CVS Caremark’s July 1, 2025 formulary change.
- Cigna / Express Scripts: Coverage varies by plan; many employer plans require PA and may require step therapy.
- Kaiser Permanente: Regional plans with varying coverage; check your specific region.
Why so many plans pulled back
Branded GLP-1s run over $1,000/month at list price, and covering them broadly drives up premiums for everyone on the plan. Some plans made the actuarial call that weight-loss coverage wasn’t sustainable at current prices and dropped it. Others tightened PA criteria instead. Expect the trend to continue until negotiated prices and manufacturer direct-to-patient programs bring net costs down.
Medicare, Medicaid, TRICARE — The Government Lanes
Medicare Part D covers GLP-1s for type 2 diabetes and for newer FDA indications like Wegovy for cardiovascular risk and Zepbound for obstructive sleep apnea. Federal statute still blocks Part D coverage solely for weight loss today, but that’s changing. Medicaid coverage varies by state, with 13 states covering GLP-1s for weight loss as of January 2026.
Medicare right now
Covered with PA:
- GLP-1s for type 2 diabetes (Ozempic, Mounjaro, Trulicity, Rybelsus, Victoza)
- Wegovy for adults with established heart disease (cardiovascular risk indication)
- Zepbound for adults with moderate-to-severe OSA and obesity
Not covered on standard Part D:
Any GLP-1 prescribed solely for weight loss — blocked by federal statute. If you have Medicare and your doctor wants you on Wegovy or Zepbound for weight, the most important conversation is whether you qualify for the CV or OSA indication.
The Medicare GLP-1 Bridge (July 1, 2026 – December 31, 2027)
CMS is running an 18-month demonstration from July 1, 2026 through December 31, 2027. BALANCE did not launch for Medicare Part D in 2027 — CMS extended the Bridge. Per CMS FAQs (updated April 6, 2026 to include Foundayo):
- Eligible drugs: all formulations of Foundayo, all formulations of Wegovy, and the Zepbound KwikPen only (single-dose vials and pens excluded)
- $50/month copay for eligible beneficiaries
- Eligibility: BMI ≥35 alone, or BMI ≥27 with specific cardiovascular, metabolic, or kidney conditions documented by a prescriber
- Runs outside the Part D benefit — your Part D plan doesn’t need to opt in
- LIS/Extra Help cost-sharing subsidies will not apply to the Bridge
The BALANCE Model (2028+ if launched for Medicare Part D)
BALANCE did not launch for Medicare Part D in 2027 — the 80% plan participation threshold was not met, so CMS extended the Bridge through December 2027. Manufacturers have agreed to a $245 net price per 30-day supply for model drugs under Medicare. Expected medications if BALANCE eventually launches: all formulations of Mounjaro, Ozempic, Rybelsus, Wegovy; the Zepbound KwikPen; and Foundayo. Watch for BALANCE 2028 announcements during fall 2027 open enrollment.
Medicaid (state by state)
As of January 2026, 13 states cover GLP-1 medications for weight loss through Medicaid per KFF — down from 16 states in 2025. Requirements are typically stricter: BMI ≥35 is common, some states require ≥40. For type 2 diabetes, coverage is broader and more consistent across all states.
What to check for your state:
- Your state Medicaid preferred drug list (PDL)
- Any prior authorization criteria specific to GLP-1s
- Whether your state has opted into the BALANCE Model for Medicaid
TRICARE
TRICARE weight-loss GLP-1 rules changed as of August 31, 2025:
Verify through your TRICARE regional contractor (East or West) — PA processes differ.
What to Do If You’re Denied or Your Plan Excludes It
A denial isn’t the end. Figure out whether you’re dealing with a prior authorization denial (often fixable with better documentation) or a plan exclusion (usually not fixable on appeal, but you have real alternatives).
First: is it a denial or an exclusion?
PA denial
The plan covers this drug in principle but denied your specific request. Appeal.
Denial letter says: “Does not meet medical necessity criteria”
Plan exclusion
The plan doesn’t cover weight-loss drugs as a category. Appeal rarely wins — pivot to alternate indication or cash-pay.
Denial letter says: “Not a covered benefit” or “excluded”
How to appeal a PA denial
Appeals work more often than people think. Patient-advocacy research cited by Honest Care reports internal-appeal success rates running 39–59%, with most denied patients never filing one. If you were denied, appealing is worth doing.
- Get the denial letter in writing. It must state the specific denial reason and cite the plan’s coverage policy.
- File the internal appeal within the plan’s deadline (usually 60–180 days from denial).
- Attach a letter of medical necessity from your prescriber that specifically addresses the denial reason. Missing BMI documentation? Include it. Missing comorbidity? Include it.
- Include primary-source evidence — the FDA label for the drug, peer-reviewed evidence supporting the indication, your chart notes and labs.
- If the internal appeal is denied, request an external review — a third-party reviewer outside the insurer evaluates the case. You have this right under federal law.
If your plan truly excludes weight-loss GLP-1s
Option 1: Check for an alternate FDA indication
Your diagnosis may support coverage under CV risk reduction (Wegovy), OSA (Zepbound), MASH (Wegovy), or type 2 diabetes. If your prescriber can truthfully justify a covered indication that you actually qualify for, re-submission under that indication can unlock coverage “weight loss” wouldn’t.
Option 2: Use a manufacturer savings program
- Wegovy: $199 intro for first 2 fills (0.25 mg or 0.5 mg) through June 30, 2026, then $349/month standard, $399/month HD
- Zepbound: $25 copay savings card for eligible commercial-insurance patients (max $100/month, max $1,300/year)
- Foundayo: eligible commercially insured patients may pay as little as $25/month under Lilly’s savings terms
Option 3: Move to telehealth self-pay
Covered in the next section.
If You’re Paying Out of Pocket: Your Real Options
If your plan excludes weight-loss GLP-1s — or the PA and appeal process isn’t worth the time — telehealth self-pay is a legitimate alternative. The cleanest FDA-approved branded paths are Sesame Care and Eden, each best for different priorities. If you want someone to check insurance first and offer a fallback in the same funnel, Ro is the natural fit.
Eden
Branded Self-PayThe broad self-pay path for branded Wegovy and Zepbound. HSA/FSA eligible, no membership fees, same price at every dose. Best for readers who want branded coverage without wrestling with insurance at all.
See current branded Wegovy or Zepbound pricing on Eden → (sponsored affiliate link, opens in a new tab)No membership fee · HSA/FSA eligible · Same price at every dose · Verified April 2026
Sesame Care
FDA-Approved LaneThe cleanest scalable FDA-approved lane — best if you want a straightforward telehealth visit and a branded medication without insurance friction. Strong fit for Wegovy, Zepbound, and the newer oral Foundayo (orforglipron).
See Sesame Care GLP-1 pricing → (sponsored affiliate link, opens in a new tab)Ro
Insurance + Cash-Pay FallbackThe natural fit for the reader who started this page by searching how to check if GLP-1 is covered by insurance. Ro offers a free insurance coverage checker that calls your insurer on your behalf, generates a personalized coverage report, and if you’re not covered, you’re already in a funnel that can prescribe FDA-approved GLP-1s on cash-pay. Ro carries FDA-approved Zepbound® (tirzepatide) and Foundayo™ (orforglipron).
Honest admission: Ro’s checker is designed for commercial-insurance users — if you have Medicare or Medicaid, a different route is better. But for commercial-insurance readers who mostly just want someone else to make the call and have a cash-pay fallback ready, Ro is unusually well-fitted to this exact moment.
Current Ro pricing: $39 to start, then as low as $74/month with annual plan paid upfront, or $149/month month-to-month. Medication billed separately.
Check my GLP-1 coverage for free with Ro → (sponsored affiliate link, opens in a new tab)$39 to start · Verify current pricing on ro.co before signing up · Verified April 18, 2026
When to skip Ro and the rest:
- You have Medicare or Medicaid. Use the government lane section above and call your plan directly.
- You’re already mid-appeal. Finish the appeal. Don’t start a new funnel.
- You want a non-branded, async, low-friction path — the self-pay telehealth landscape has other legitimate players for that.
Three Real Situations, Three Different Answers
Find yours.
“I have an employer plan and I don’t know if it covers GLP-1s”
Start with your PBM tool (Caremark, Express Scripts, or Optum Rx depending on your card) and finish with HR. Self-funded employer plans can diverge from the insurer’s default formulary — HR has the real answer your PBM tool won’t show.
“My plan dropped GLP-1 coverage for 2026”
You still have options. First check whether you qualify for an alternate FDA indication — CV risk, OSA, MASH, T2D. If yes, re-submit under that indication. If no, manufacturer savings programs (Wegovy $199 intro, Zepbound $25 copay card, Foundayo as low as $25 for eligible commercially insured patients) or self-pay branded through Eden or Sesame Care are the cleanest paths.
“I have Medicare and my doctor wants me on Wegovy or Zepbound”
Federal statute blocks Part D coverage for weight loss alone, but Wegovy can be covered under its CV indication (adults with established heart disease) and Zepbound under its OSA indication (adults with moderate-to-severe sleep apnea and obesity). The Medicare GLP-1 Bridge runs July 1, 2026–December 2027 (18 months) at $50/month for eligible beneficiaries — covering Wegovy, Zepbound KwikPen, and Foundayo. BALANCE did not launch for Medicare Part D in 2027 — watch for 2028 announcements.
“I have Medicaid”
Check your state’s preferred drug list. Only 13 states cover GLP-1s for weight loss through Medicaid as of January 2026, and BMI thresholds are typically stricter (≥35 is common). If your state isn’t one of them, look at T2D pathways if applicable or move to self-pay.
“I have TRICARE”
TRICARE For Life lost coverage for weight-loss GLP-1s as of August 31, 2025. TRICARE Prime and TRICARE Select members may still qualify with strict clinical criteria and prior authorization. Diabetes GLP-1s remain covered for qualifying patients with PA.
“My pharmacy just told me my prescription is $1,080”
The claim rejected. Call the pharmacy and ask for the specific rejection code — PA required, not covered, step therapy, quantity limit, or plan exclusion. That code tells you exactly which step of this guide to use next.
Related guides on The RX Index
Frequently Asked Questions
How do I know if my insurance covers Wegovy?
Log into your PBM member site (CVS Caremark, Express Scripts, or Optum Rx depending on your card) and search “Wegovy.” Check for restriction codes (PA, ST, QL). Call the 800 number on your card to confirm coverage for your specific diagnosis — weight management, cardiovascular risk reduction, or noncirrhotic MASH with F2–F3 fibrosis can each change the answer substantially.
How do I know if my insurance covers Zepbound?
Same process as Wegovy — PBM tool first, phone call second. Note that CVS Caremark removed Zepbound from its standard commercial formularies on July 1, 2025, while some Optum Rx formularies kept it. Zepbound is also FDA-approved for obstructive sleep apnea in adults with obesity, which can unlock coverage on plans that exclude weight-loss-only use.
Does insurance cover Ozempic for weight loss?
Usually not. Ozempic is FDA-approved for type 2 diabetes and cardiovascular risk reduction in patients with type 2 diabetes and heart disease, and most plans cover it only for those indications. Prescribing Ozempic off-label for weight loss is legal but typically isn’t covered — for weight loss, Wegovy (semaglutide, FDA-approved for chronic weight management) is the on-label choice.
Does prior authorization mean my plan covers the drug?
Not automatically. PA means the plan will consider covering it if your prescriber submits the required clinical documentation. Approval depends on whether your case meets the plan’s medical-necessity criteria. Many initial denials are caused by incomplete paperwork rather than true ineligibility.
What’s the difference between non-formulary and excluded benefit?
Non-formulary means the drug isn’t on your plan’s preferred list but you may be able to get it through a formulary exception. Excluded benefit means the plan has chosen not to cover this category of drug at all — for example, “all weight-loss medications excluded.” Appeals rarely overcome a true category exclusion.
Does my employer decide whether GLP-1 is covered?
For self-funded employer plans, often yes — your employer can add or remove GLP-1 coverage independently of what the insurer’s default formulary shows. That’s why your Caremark.com account can say “covered” while your HR department says “not covered under our plan.” Always confirm with HR for employer plans.
Does Medicare cover GLP-1 for weight loss?
Not on standard Part D — federal statute currently blocks it. But Medicare Part D does cover GLP-1s for type 2 diabetes, for Wegovy's cardiovascular risk indication, and for Zepbound's obstructive sleep apnea indication. The Medicare GLP-1 Bridge runs July 1, 2026 through December 31, 2027 (18 months) and covers Wegovy, Zepbound KwikPen, and Foundayo at $50/month for beneficiaries meeting BMI and clinical criteria. BALANCE did not launch for Medicare Part D in 2027 — CMS extended the Bridge instead.
Does Medicaid cover GLP-1 for weight loss?
In 13 states as of January 2026 per KFF. Requirements are stricter than commercial plans — BMI ≥35 is common, and some states require ≥40. For type 2 diabetes, coverage is much broader and more consistent across states. The BALANCE Model may expand state Medicaid access for participating states starting May 2026.
Can a telehealth company check coverage for me?
Yes. Ro and Found both offer free insurance coverage checkers that contact your insurer on your behalf and return a personalized report including prior authorization status and estimated copays. Ro focuses on commercial insurance. These services are useful when you don’t want to make the call yourself, but they’re still commercial funnels — the neutral 5-step check above is usually the better first move.
What should I do if I already got denied?
Request the denial letter in writing. Identify whether it’s a PA denial or a plan exclusion. For PA denials, file an internal appeal with a letter of medical necessity addressing the specific denial reason. For true plan exclusions, check for an alternate FDA indication (CV risk, OSA, MASH, T2D), use a manufacturer savings program, or move to telehealth self-pay.
How long does GLP-1 prior authorization take?
It varies by payer and benefit. Electronic submissions with complete documentation generally return faster than paper or incomplete submissions. Denied cases that go to peer-to-peer review or appeal can take several additional weeks. Ask your plan for its specific PA turnaround time when you call.
Is compounded semaglutide covered by insurance?
Generally no. Compounded medications are not FDA-approved versions of branded drugs and are typically not covered by commercial insurance, Medicare, or Medicaid.
Still not sure which GLP-1 program is right for you?
You now know how to check if GLP-1 is covered by insurance in 15 minutes. But the right next step — appeal vs. alternate indication vs. Medicare Bridge vs. cash-pay — depends on the specifics of your situation. We’ll help you sort it out in 60 seconds.
Take our free 60-second GLP-1 matching quiz →What we actually verified
To build the Coverage Check Route Matrix, the Indication → Coverage Shortcut Table, and the Verified 2025–2026 Change Tracker, we directly reviewed: PBM and insurer tools (CVS Caremark, Express Scripts, Optum Rx, Aetna, Cigna, UnitedHealthcare pharmacy benefit pages); manufacturer pages (NovoCare/Wegovy.com, Zepbound.Lilly.com, LillyDirect); done-for-you checker pages (Ro, Found); government sources (CMS Medicare GLP-1 Bridge FAQs updated April 6, 2026, BALANCE Model pages; FDA press announcements and approval letters); formulary change announcements (Mass General Brigham Health Plan, Health New England, Fallon Health Community Care, Point32Health/Harvard Pilgrim, CVS Caremark July 1, 2025 change, TRICARE Newsroom August 2025, BCBS of Michigan 2025 alert); and policy/cost research (KFF 2025 Employer Health Benefits Survey, KFF BALANCE Model brief March 2026, KFF Medicare GLP-1 Bridge quick take).
Last verified: April 18, 2026 • Coverage policies change mid-year — always confirm with your specific plan and formulary before relying on anything here for a coverage decision.
The RX Index is a pricing intelligence and comparison resource for GLP-1 telehealth providers. We don’t sell insurance, write prescriptions, or dispense medication. When you click links to Eden, Sesame Care, Ro, or other providers from this page, The RX Index may receive a commission at no additional cost to you. This page is educational and is not medical, legal, or financial advice.