Affiliate disclosure: The RX Index earns a commission when you sign up with some of the providers mentioned on this page. It does not affect what you pay, and it never determines our rankings or which providers we cover. Read the full disclosure.
Insurance Guide ·
By The RX Index Editorial Team · · Sources: FEP Blue, BCBS Michigan/BCN, Highmark, BCBS Massachusetts, Independence Blue Cross, BCBS North Dakota, Blue Shield of California, FDA, NovoCare, NovoMedLink, Ro
Blue Cross Wegovy Prior Authorization: What Blue Plans Actually Require, Step by Step
Published:
Blue Cross Wegovy prior authorization is not one universal checklist — and that single fact is what trips up most people reading this page.
Your doctor prescribed Wegovy. Your pharmacy or insurer said prior authorization is required. And the Blue Cross logo on your card didn’t produce a clear answer. We’ve spent months pulling apart the official policy documents from FEP Blue, BCBS Michigan, Highmark, BCBS Massachusetts, Independence Blue Cross, BCBS North Dakota, and Blue Shield of California — and they don’t all say the same thing.
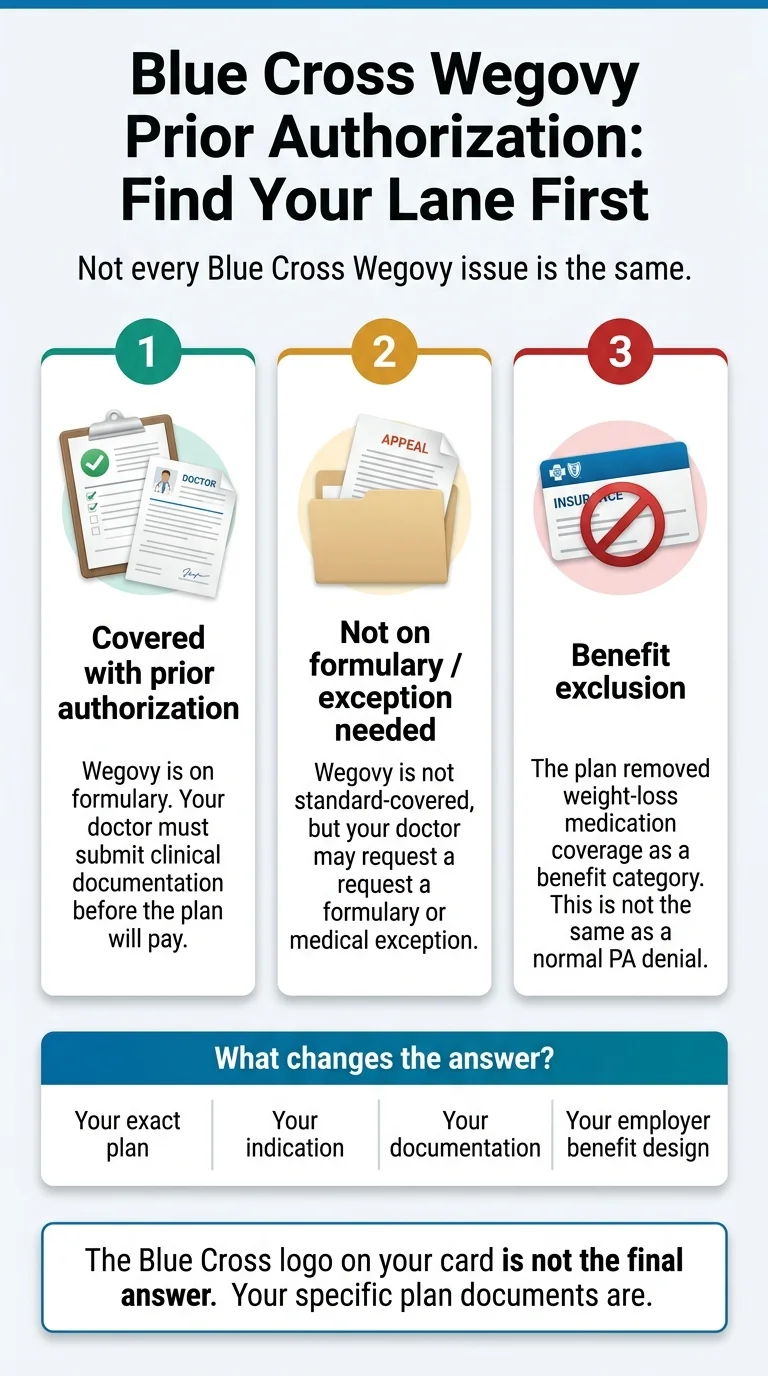
Some Blue plans cover Wegovy with standard prior authorization. Some will only consider it through a formulary-exception request. And some — including several that covered it as recently as 2024 — have removed weight-loss GLP-1 coverage entirely for certain member populations. The Blue Cross Blue Shield Association describes the system as 34 independent, locally operated companies. That means “Blue Cross covers Wegovy” is never the final answer. Your specific plan documents are.
| What your plan is really saying | What it means | What to do next |
|---|---|---|
| ✅ Covered with prior authorization | Wegovy is on your plan's formulary. Your doctor must prove you meet the criteria before the plan will pay. | Build the PA packet — see the checklist below |
| ⚠️ Not on formulary / exception needed | Wegovy isn't standard-covered, but your doctor can request a formulary exception arguing medical necessity. | Use medical-necessity documentation — see the lane guide below |
| ❌ Benefit exclusion | Your plan removed weight-loss GLP-1 coverage as a category. | Stop treating this like a PA problem — see the exclusion section below |
What We Actually Verified
We reviewed the following public documents to build this page. Every claim in the Blue-plan comparison below is sourced to one of these. Where we could not confirm details from public documents, we say so explicitly rather than guessing.
- FEP Blue Wegovy policy, effective Feb. 13, 2026 (fepblue.org)
- BCBS Michigan / BCN prior-authorization criteria PDF, revised Apr. 1, 2026 (bcbsm.com)
- BCBS Michigan 2024 provider alert on GLP-1 coverage changes (providerinfo.bcbsm.com)
- Highmark Wegovy prior authorization form (providers.highmark.com)
- BCBS Massachusetts medication detail page, Jan. 2026 policy, formulary notes, and medical policy 572 (bluecrossma.org)
- Independence Blue Cross coverage change notice, Jan. 1, 2025 (provcomm.ibx.com)
- BCBS North Dakota oral Wegovy update, Jan./Feb. 2026 (bcbsnd.com)
- Blue Shield of California prior-authorization page, updated Jan. 14, 2026 (blueshieldca.com)
- FDA Wegovy prescribing information · NovoCare pricing and coverage resources · NovoMedLink PA guide and denial/appeal guide · Ro coverage checker and pricing pages
Is Wegovy Covered by Blue Cross with Prior Authorization?
Sometimes. Public Blue-plan documents show three distinct realities: standard coverage with prior authorization, non-formulary or exception handling, and outright benefit exclusion for weight-loss use. Because the Blue Cross Blue Shield system is made up of 34 independent, locally operated companies, the answer depends entirely on your specific plan and employer.
What “prior authorization” actually means
Prior authorization (PA) means Wegovy is on your plan’s formulary — the list of drugs the plan agrees to cover — but the plan requires your doctor to submit clinical documentation proving you meet their criteria before they’ll pay. PA is a review step, not a denial. If your paperwork is complete and you meet the criteria, the plan is expected to approve coverage.
What “formulary exception” means
A formulary exception means Wegovy is not on your plan’s standard drug list. Your doctor can still request coverage by arguing medical necessity — essentially making the case that no formulary-covered alternative works for you. Novo Nordisk’s own Wegovy access materials note that a medical-exception request with a Letter of Medical Necessity (LOMN) may be required when Wegovy is non-formulary. This is a different administrative process than a standard PA, and it requires stronger clinical justification.
What “benefit exclusion” means
A benefit exclusion means the plan has removed the entire category — typically “weight-loss medications” or “anti-obesity medications” — from covered benefits. This is not a documentation problem. It’s a plan-design decision, often made by the employer (for self-funded plans) or the Blue affiliate (for fully insured plans). Novo Nordisk’s denial and appeal guide notes that benefit exclusions typically do not have standard appeal rights.
Why the logo on your card is not enough
Two people with Blue Cross cards sitting in the same pharmacy can have completely different answers. One might have a self-funded employer plan that covers Wegovy with PA. The other might have a fully insured large-group plan that excluded GLP-1 weight-loss drugs entirely as of January 2025. The Blue Cross logo tells you the network — it doesn’t tell you the benefit design.
Which Blue Cross Lane Are You Actually In?
This is the section that saves you the most time. Before you think about appeals, documents, or provider options, figure out your lane — because the right lane determines everything that follows.
Lane 1: Wegovy is on formulary and needs PA
Your plan covers Wegovy, but the insurer wants to confirm you meet the criteria before paying. This is the most straightforward path. Your doctor submits documentation, the plan reviews it, and you get a decision. Blue Shield of California publicly says typical processing takes 24 to 72 hours, though real-world timelines often stretch when documentation is incomplete.
Lane 2: Wegovy is non-formulary and may need an exception request
Wegovy isn't on your plan's standard drug list, but your doctor can request a formulary exception — a separate process from standard PA that requires a Letter of Medical Necessity and stronger clinical documentation.
Lane 3: Weight-loss use is excluded from your plan
The plan has removed the entire weight-loss medication category from covered benefits. No amount of PA paperwork will fix this, because the barrier is plan design, not clinical documentation. Multiple BCBS affiliates — including Michigan (fully insured large group), Massachusetts (certain fully insured group/individual commercial members), Independence Blue Cross, and Blue Shield of California (certain commercial plans) — have made these changes since 2025.
Lane 4: A different FDA-approved indication may still have a path
Even when a plan excludes weight-loss drugs, a separate FDA-approved indication might still be reviewable. Wegovy is FDA-approved for reducing the risk of major adverse cardiovascular events in adults with established cardiovascular disease who have obesity or overweight. Independence Blue Cross says GLP-1s for FDA-approved medical conditions like cardiovascular disease can still be covered with PA even when the weight-loss benefit is excluded.
What Blue Plans Actually Require for Wegovy Prior Authorization
There is no single Blue Cross Wegovy checklist. But the public plan documents we reviewed repeat a recognizable pattern: BMI and diagnosis thresholds, documentation of lifestyle modification, baseline and current weight, no conflicting GLP-1 use, and tougher renewal rules once treatment starts. The differences between affiliates are material enough that a generic “BMI 30 or 27 with comorbidity” answer won’t reliably get you approved.
The RX Index Blue Cross Wegovy PA Snapshot
Last verified: . Based on publicly available plan documents. Your specific plan may differ — always confirm with your insurer.
| Blue Plan | Coverage Lane | Initial Criteria | Renewal Criteria | Hidden Gotcha | Who It Affects | Source |
|---|---|---|---|---|---|---|
| FEP Blue | ✅ Covered with PA | BMI ≥30, or ≥27 + established CV disease or weight-related comorbidity; comprehensive weight-management program required; adults 18+ | ≥5% baseline weight loss or maintenance; continued program participation; no dual GLP-1 therapy; 12-month renewal duration | Quantity limit: 12 pens per 84 days (injection), 90 tablets per 90 days (pill); initial approval is 6 months for chronic weight management, 12 months for MASH | Federal employees on FEP Standard/Basic | FEP Blue policy 5.99.030, Feb. 2026 |
| BCBS Michigan/BCN — Standard | ✅ Group benefit controls | BMI ≥30, or ≥27 + comorbidity; CV and MASH pathways also available; age 18+; baseline weight; ongoing lifestyle modification | 1-year initial approval; maintain ≥5% weight loss; current weight submission; continued lifestyle activity | Not one universal Michigan rule — the group benefit design determines which criteria branch applies | Members whose employer/group benefit includes GLP-1 coverage | BCBSM/BCN criteria PDF, revised Apr. 1, 2026 |
| BCBS Michigan/BCN — Fully Insured Large Group | ❌ Benefit excluded (eff. Jan. 1, 2025) | Historical: BMI ≥35, 6 months documented lifestyle work, Teladoc Health participation with summary report, in-person prescriber relationship | Historical: maintain ≥5% weight loss + program documentation | This population lost GLP-1 weight-loss coverage entirely — this is Lane 3, not Lane 1 | ~10,000 affected Michigan members in fully insured large-group commercial plans | BCBSM provider alert, June 2024; Bridge Michigan, May 2025 |
| Highmark (PA, WV, NY, DE) | ✅ Covered with PA (documentation-heavy) | Months in lifestyle program; diet proof (nutrition counseling receipts, medical nutrition therapy); physical-activity proof (wearable data, trainer receipts); weight-related comorbidities with chart notes; prior weight-loss meds; baseline weight/BMI | Continuation criteria not fully detailed in the public PA form | Form also asks about Zepbound intolerance and detailed CV, PAD, diabetes, prediabetes, and MASH questions — which could open separate approval pathways | Members in Highmark-administered plans across PA, WV, NY, DE | Highmark Wegovy PA form, providers.highmark.com |
| BCBS Massachusetts — Standard Control Formulary | ✅ Covered with PA | 6-month comprehensive weight-management program before therapy; separate lanes for CV risk reduction and MASH with distinct criteria | ≥5% baseline body-weight loss after first 16 weeks; continued loss or maintained plateau; ongoing comprehensive plan adherence | 1-month supply per fill; 75% of days must be exhausted before refill; mail-order pharmacy benefit excluded for these prescriptions | Members on the Standard Control formulary | BCBSMA medication detail page; medical policy 572 |
| BCBS Massachusetts — Focused Formulary | ❌ Benefit excluded for weight loss | N/A — GLP-1/GLP-1-GIP drugs approved for weight loss and other medical indications are excluded under this formulary | N/A | Separately: fully insured group and individual commercial members face exclusion upon renewal eff. Jan. 1, 2026, unless employer (100+ employees) buys optional coverage. Check which applies to you. | Members on the Focused formulary; affected fully insured group/individual commercial members | BCBSMA Standard Control Formulary page; BCBSMA FAQ |
| Independence Blue Cross (PA) | ❌ Excluded for weight loss (eff. Jan. 1, 2025) | Not a PA problem — IBX says GLP-1s for FDA-approved medical conditions (e.g., CV disease) can still be covered with PA | Per-indication details not fully public | People waste weeks pushing PA paperwork when the actual barrier is plan design | Fully insured group and individual commercial members | IBX coverage change notice, Jan. 2025 |
| BCBS North Dakota | ✅ Covered with PA (MASH and oral Wegovy) | MASH can be a live coverage lane even when weight-loss benefits are limited; oral Wegovy added to Commercial Formulary Feb. 1, 2026 (preferred brand tier for Marketplace/NetResults) | Per-formulation renewal details not fully public | Switching from injectable to oral Wegovy requires a brand-new PA — existing injectable approvals do not transfer | BCBSND commercial members | BCBSND pharmacy updates, Jan./Feb. 2026 |
| Blue Shield of California | ⚠️ Varies by plan | For affected plans: current or previous Class III obesity diagnosis + comprehensive weight-loss program participation; PA typically processed in 24–72 hours | Per-plan renewal specifics not fully public | Benefit changes affect certain commercial PPO/HMO plans, not everyone under the Blue Shield name | Certain Blue Shield CA commercial members | Blue Shield CA prior-auth page, updated Jan. 14, 2026 |
That’s seven Blue-plan sources showing seven different versions of “Wegovy prior authorization.” This is why generic advice fails — and why you need to know your plan before you start paperwork.
What to Hand Your Doctor Before They Submit the PA
Incomplete or missing documentation is one of the most common reasons Wegovy PAs get denied. Novo Nordisk’s own denial and appeal guide lists criteria not met, non-formulary/not-covered status, formulary alternative not tried, and missing or incorrect documentation as common denial categories. The public Blue-plan forms confirm the pattern: when the form asks for something specific and it isn’t attached, the request gets rejected.
Your doctor’s office handles the PA submission, but you can dramatically improve your odds by walking into the appointment with the right material already organized.
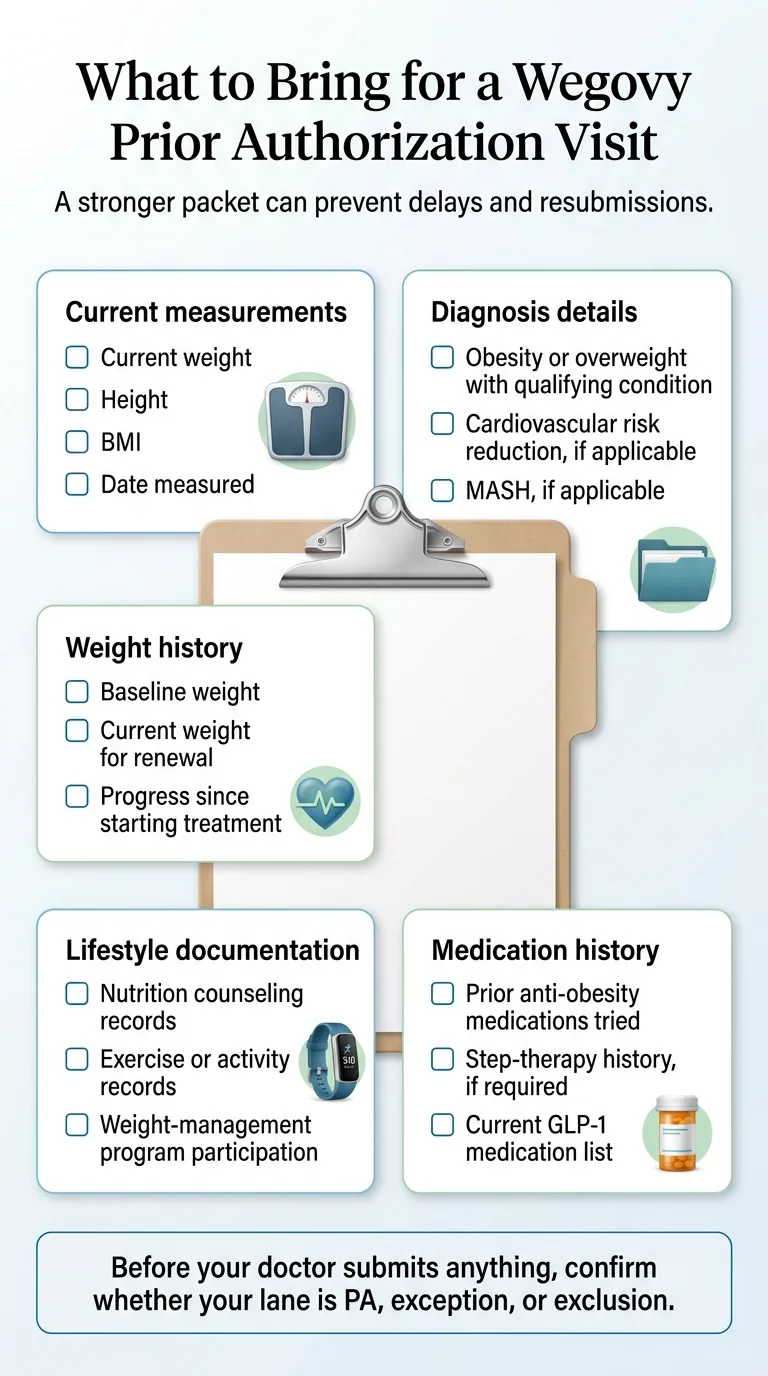
Blue Cross Wegovy PA Packet Checklist
Print this. Bring it to your appointment. Check each item off with your doctor.
Clinical documentation
- ☐Current height, weight, and BMI — measured and dated recently (some Blue plans specify within 30 days; others require current values without a specific window — ask your plan)
- ☐Baseline weight before treatment (if this is a renewal or continuation)
- ☐Current weight (if this is a renewal)
- ☐Exact indication documented: obesity, overweight + comorbidity, cardiovascular risk reduction, or MASH
- ☐Diagnoses actually coded in your medical chart with correct ICD-10 codes (E66.01 for morbid obesity, E66.09 for other obesity, etc.)
- ☐List of weight-related comorbidities with supporting chart notes: hypertension, type 2 diabetes, high cholesterol, cardiovascular disease, obstructive sleep apnea
Lifestyle documentation — this is where PAs commonly fail
Most Blue plans require documented evidence of structured weight-management efforts, not just “I tried dieting.” Acceptable examples from the Highmark PA form include:
- ☐Recurring appointments for nutritional counseling or medical nutrition therapy (receipts or records)
- ☐Summary report from a wearable device showing physical activity frequency (elevated heart rate for 20+ minutes, at least 3 times per week, for at least a month)
- ☐Personal trainer receipts with notes specifying type, duration, and frequency of physical activity
- ☐Participation in a comprehensive weight management program (documentation of enrollment and attendance)
- ☐Duration of lifestyle modification — how many months actively participating (FEP requires a comprehensive program; BCBSMA’s obesity pathway requires 6 months before therapy)
Medication history
- ☐Prior anti-obesity medications tried and outcomes (phentermine, Contrave, Saxenda, etc.) — some plans require step therapy
- ☐Confirmation that you are NOT currently using another semaglutide product (Ozempic, Rybelsus) or another GLP-1 medication
Plan-specific confirmation
- ☐Your formulary lane confirmed — PA, exception, or exclusion
- ☐Whether step therapy is required for your specific plan
- ☐Whether the cardiovascular indication pathway applies to your clinical situation
The lifestyle documentation is the item that separates approved PAs from denied ones
Highmark wants wearable device data and nutrition counseling receipts. FEP wants proof of comprehensive weight-management program participation. BCBSMA wants six months of documented effort before therapy begins on the obesity pathway. A verbal attestation from your doctor that you “tried diet and exercise” is not sufficient for most Blue plans. Start collecting it now — even if it means delaying the PA submission by a few weeks to build a stronger packet. A clean first submission beats a denied-and-resubmitted one every time.
How the Blue Cross Wegovy Prior Authorization Process Works
The prescriber — not the patient — submits the prior authorization request to the Blue plan. FEP says doctors can submit electronically, by fax, or by mail. Blue Shield of California’s member page says typical PA processing takes 24 to 72 hours. But real-world timelines vary significantly — Ro, which handles PA submissions for its members, says its insurance process typically takes 2–3 weeks. The gap between “24 to 72 hours” and “2 to 3 weeks” is almost always explained by incomplete documentation and insurer back-and-forth.
Step 1: Confirm the plan actually covers Wegovy
Call the number on your BCBS card before anything else. Ask these exact questions and write down the representative's name, date, time, and any reference number:
- Is Wegovy (semaglutide) on my plan's formulary for weight management?
- Is it covered with prior authorization, available through formulary exception, or excluded?
- What are the exact PA criteria for my specific indication?
- Is step therapy required — do I need to try other medications first?
- What specific documents does the PA reviewer need?
- What is the tier, copay, or coinsurance after approval?
- If denied, what is the exact appeal deadline and process for my plan?
Step 2: Confirm whether PA, exception, or exclusion applies
If the answer from Step 1 is "covered with PA," proceed to building your packet. If the answer is "not on formulary" or "excluded benefit," you need a different strategy — see the lane guide above.
Step 3: Prescriber submits the request
Your doctor completes the PA form with all clinical documentation. The form could be a single page or a multi-page document depending on the Blue affiliate — Highmark's form, for example, is several pages long with detailed clinical questions. FEP and CoverMyMeds support electronic submission, which tends to be faster. Make sure your doctor's office submits everything in one batch — incomplete submissions are one of the most common causes of delays and denials.
Step 4: Follow status and respond fast to missing-info requests
Check the status within 3 business days. You can typically call your BCBS plan or log into the member portal. If the plan requests additional information, respond within 48 hours. Every day of delay extends your timeline.
Step 5: Decision, resubmission, or appeal
If approved — let your pharmacy know so they can resubmit the claim. If denied — read the denial letter carefully. The exact wording tells you whether to resubmit with corrections, appeal with stronger evidence, or pivot to a different path entirely.
Don’t want to manage this yourself?
Ro’s free GLP-1 Insurance Coverage Checker produces a coverage report for your specific plan, and if a Ro-affiliated provider prescribes Wegovy, their insurance concierge handles benefit verification, prior-authorization submission, follow-up, and appeals. Ro carries FDA-approved GLP-1 options including Zepbound® (tirzepatide) and Foundayo™ (orforglipron), and connects to NovoCare Pharmacy for Wegovy fulfillment.
Ro does not handle benefit exclusions — if your plan has removed weight-loss GLP-1 coverage entirely, their concierge can confirm that for you, but the solution at that point is a different path, not more insurance paperwork.
Check your Blue Cross Wegovy coverage with Ro’s free tool → (sponsored affiliate link, opens in a new tab)Get started for $39 for the first month, then as low as $74/month with the annual plan paid upfront, or $149/month on the monthly plan.
Why Blue Cross Denies Wegovy Prior Authorization
The common denial reasons are consistent across official Blue-plan documents and Novo Nordisk’s denial and appeal guide. Understanding which category your denial falls into determines your next move.
Missing or incomplete documentation
A fixable problem. The PA form had blank fields, missing chart notes, or absent lifestyle-modification proof. Solution: resubmit with the complete packet. This is why the checklist above exists — front-loading the documentation prevents this.
BMI or comorbidity threshold not met
Your documented BMI doesn't meet the plan's threshold, or the required comorbidity isn't coded in the chart. Solution: verify the measurements are current, check that the ICD-10 codes match the plan's criteria, and make sure the comorbidity is explicitly documented in the chart notes — not just mentioned verbally.
No documented lifestyle program
The plan requires evidence of structured weight-management efforts, and the submission didn't include it. Solution: gather the specific documentation types the plan accepts (see the Highmark examples in the checklist above) and resubmit.
Wrong diagnosis coding
The PA was submitted with an obesity code, but the plan only covers Wegovy under a cardiovascular risk-reduction or MASH indication. Or the codes don't match the plan's required criteria. Solution: review the denial letter, confirm which indication codes the plan accepts, and work with your prescriber to ensure the right diagnosis is documented and coded.
Formulary exclusion vs. benefit exclusion
Two different problems that look the same on a pharmacy rejection screen. A formulary exclusion means Wegovy isn't on the preferred drug list but might be obtainable through a medical-necessity exception. A benefit exclusion means the entire medication category is not covered. The denial letter should specify which one applies. If it doesn't, call and ask directly: "Is this a formulary issue or a benefit-design exclusion?"
Step therapy requirement
The plan requires you to try and fail cheaper alternatives — often phentermine, Contrave, or Saxenda — before approving Wegovy. If you've already tried these medications, make sure that history is documented in the PA. If you haven't, your doctor can request a step-therapy exception if there are clinical reasons those alternatives aren't appropriate.
Renewal failure
The plan wants proof Wegovy is working. Most Blue plans that publish renewal criteria require at least 5% body-weight loss from baseline at the first renewal checkpoint. If you haven't met this threshold, or if the documentation wasn't submitted, the renewal PA will be denied.
PA approval does NOT guarantee a low copay
Prior-authorization approval and out-of-pocket cost are two separate problems. Even after PA approval, your Wegovy cost depends on your plan's tier placement, copay or coinsurance structure, and deductible status. Always ask: "What tier is Wegovy on, and what will my copay or coinsurance be after approval?" With commercial insurance that covers Wegovy and the Novo Nordisk Savings Card applied, your copay can drop to as little as $25/month (maximum savings of $100 per one-month supply). But you need to know the base copay first, because the savings card caps at $100 off.
What to Do If Blue Cross Denies Wegovy
The right response depends entirely on why you were denied. A corrected resubmission, a formal appeal, and a full pivot are three completely different actions — and choosing the wrong one wastes time you don’t have.
| Denial wording | What it usually means | Best next move |
|---|---|---|
| "Incomplete information" or "additional documentation needed" | The PA form was missing required fields or attachments. | Resubmit with corrected and complete documentation. Not an appeal — a clean resubmission. |
| "Does not meet medical necessity criteria" | Your documented BMI, comorbidities, or lifestyle modification didn't satisfy the plan's threshold. | Gather stronger clinical evidence. Ask your doctor about a peer-to-peer review with the plan's medical director. |
| "Step therapy required" | The plan wants you to try cheaper alternatives first. | Document prior medication attempts, or have your doctor submit a step-therapy exception request. |
| "Not on formulary" / "Non-covered drug" | Wegovy isn't on your plan's drug list, but an exception may be possible. | Submit a formulary exception with a Letter of Medical Necessity — different from standard PA paperwork. |
| "Excluded benefit" / "Weight-loss medications are not covered" | The plan removed this medication category from benefits. | This usually cannot be resolved through standard PA appeal channels. Check whether a different FDA indication applies, talk to HR, or consider fallback options. |
When to ask for peer-to-peer review
If the denial says “criteria not met” and you believe the clinical documentation supports approval, ask your prescriber to request a peer-to-peer review — a direct conversation between your doctor and the plan’s reviewing physician. This is often more productive than a written resubmission alone.
When to file a formal appeal
Your denial notice will include the specific appeal deadline and process for your plan — follow those instructions exactly. KFF analysis of CMS data found that among Medicare Advantage plans, 83.2% of appealed prior-authorization denials were overturned. Commercial plan appeal success rates are less well-documented, but many initial denials are reversed when stronger documentation is submitted. If your first attempt was denied, it’s worth appealing — particularly if the denial was based on missing documentation or criteria you can now satisfy.
When to stop and pivot
If the denial is a benefit exclusion — not a PA denial — standard appeals usually won’t resolve it. At that point, your options shift. See the exclusion section below.
What If Your Blue Plan Excludes Weight-Loss GLP-1s Entirely?
This is the most important “stop wasting time” section on this page. BCBS Massachusetts, BCBS Michigan (fully insured large group), Independence Blue Cross, Blue Shield of California, and others have all publicly confirmed benefit exclusions for weight-loss GLP-1s in some or all member populations since 2025. If you’re in this lane, calling about PA paperwork won’t help. The barrier is the benefit design itself.
We won’t pretend this isn’t frustrating.
Losing coverage for a medication that was working — or never being able to access it through insurance — is one of the more demoralizing experiences in healthcare. Multiple BCBS affiliates cut GLP-1 weight-loss coverage because the costs were genuinely unsustainable: BCBS Massachusetts alone spent $300 million on GLP-1s in a single year, and BCBS Michigan’s GLP-1 costs went from $8 million to $300 million in three years. That context doesn’t make it easier when you’re the one affected — but it does explain why this is happening and why it’s unlikely to reverse quickly.
First: ask whether a non-weight-loss indication applies
If you have documented cardiovascular disease (prior heart attack, stroke, or peripheral artery disease), your doctor may be able to prescribe Wegovy for cardiovascular risk reduction — a separate FDA-approved indication that some plans still cover even when weight-loss use is excluded. Independence Blue Cross explicitly makes this distinction. This is not a loophole. It only applies if you genuinely have the qualifying condition.
Second: ask whether your plan has a formulary or medical exception pathway
Some plans that exclude the category broadly will still consider individual exception requests with strong medical-necessity documentation. Ask explicitly: “Does my plan have any exception pathway for a weight-loss medication if my doctor can demonstrate medical necessity?”
Third: if no insurance path exists, your options shift
Cash-pay for FDA-approved Wegovy through NovoCare Pharmacy: Novo Nordisk sells Wegovy directly through NovoCare Pharmacy at reduced self-pay prices — no prior authorization required because no insurance is involved, delivered to your home. Current NovoCare self-pay pricing (verified ):
| Formulation | Dose | Monthly price | Notes |
|---|---|---|---|
| Wegovy pill | 1.5 mg | $149/mo | — |
| Wegovy pill | 4 mg | $149/mo | Temporary offer through Aug. 31, 2026; then $199/mo |
| Wegovy pill | 9 mg, 25 mg | $299/mo | — |
| Wegovy injection | 0.25 mg, 0.5 mg | $199/mo | Intro offer for new patients, first 2 fills only through June 30, 2026 |
| Wegovy injection | Maintenance doses | $349/mo | Standard self-pay rate |
Source: NovoCare savings offer terms and Wegovy price guide, novocare.com. Government beneficiaries excluded. Prices subject to change. Note: compounded semaglutide is not FDA-approved and is not the same as FDA-approved Wegovy. NovoCare Pharmacy only dispenses FDA-approved Wegovy.
Telehealth with insurance support + cash-pay fallback
Ro’s platform starts at $39 for the first month, includes benefit verification and PA/appeal handling, and connects to NovoCare pricing for Wegovy fulfillment. If insurance fails, you can continue through Ro at NovoCare self-pay pricing without starting over with a new provider.
Check coverage or start cash-pay Wegovy through Ro → (sponsored affiliate link, opens in a new tab)For readers who need to compare all available GLP-1 paths — including which providers handle insurance, which are cash-pay only, and how pricing compares across different programs — our Blue Cross GLP-1 provider guide covers the complete comparison.
How Blue Cross Wegovy Renewals Work
Getting approved is only half the fight. Public Blue-plan policies show that reauthorization happens on a plan-specific schedule and commonly requires continued lifestyle participation, ongoing use of an approved maintenance dose, and clinical evidence that treatment is working.
The 5% threshold
Most Blue plans that publish renewal criteria require at least 5% body-weight loss from baseline at the first renewal checkpoint. FEP Blue specifies this threshold with a renewal duration of 12 months. BCBS Michigan’s standard route ties continuation to 5% weight loss plus current weight submission. BCBSMA has a more specific timeline: at least 5% baseline body-weight loss after the first 16 weeks, with continued loss or maintenance of achieved plateau at subsequent renewals. FEP’s initial approval for chronic weight management is 6 months — meaning you could face your first renewal checkpoint sooner than you expect.
What to track from day one
- Baseline weight: The weight on record when treatment started. This is your reference point for the 5% calculation. Make sure it’s documented in your chart.
- Weight at each visit: Even routine visits should include a weigh-in if you’re on Wegovy. The renewal PA will need current weight.
- Ongoing lifestyle participation: Keep those nutrition counseling receipts, gym check-ins, or wearable data exports. The renewal often requires the same lifestyle documentation as the initial PA.
- Fill history: Consistent prescription fills demonstrate adherence. Gaps in fill history can trigger renewal questions.
How early to start the renewal
Start the renewal process at least 30 days before your current PA expires. This gives your doctor time to gather updated documentation, submit the request, and handle any back-and-forth with the plan. If you wait until the PA expires, you risk a gap in coverage — and potentially paying full price for one or more refills while the renewal processes.
BCBSMA members: watch the refill rules
BCBSMA’s current policy limits GLP-1 prescriptions to a 1-month supply per fill and requires that 75% of days in the supply must be exhausted before refill. These prescriptions are also excluded from the mail-order pharmacy benefit. That means you’ll be picking up Wegovy at a retail pharmacy monthly — plan your schedule accordingly.
Questions to Ask Blue Cross and Your Doctor’s Office
The goal is to get the exact lane, the exact criteria, the exact form, and the exact cost in writing. Because “covered with PA” still doesn’t tell you what happens next.
Questions for your Blue Cross plan
- Is Wegovy (semaglutide) on my plan’s formulary for my specific plan and indication?
- Is it covered with prior authorization, available through formulary exception, or excluded?
- What are the exact PA criteria for my indication (weight management, cardiovascular risk reduction, or MASH)?
- Is step therapy required? If so, which medications must I try first?
- What specific documentation does the PA reviewer need?
- What is the drug tier, copay, coinsurance, and deductible requirement after PA approval?
- If denied, what is the exact appeal deadline, method, and mailing address for my plan?
Questions for your prescriber’s office
- Have you submitted Wegovy PAs for Blue Cross patients before? (Experience with the specific form matters.)
- Can we review the PA form together to make sure we’re documenting everything the plan asks for?
- Are all my diagnoses properly coded in the chart?
- Do you have my current weight, baseline weight, and BMI documented?
- Can you submit a peer-to-peer review if the PA is denied?
Questions for the pharmacy
- Was the claim rejected because of PA requirements, or because the drug isn’t covered at all?
- Can you tell me the exact rejection code? (The code often reveals whether it’s a PA issue or a benefit-design issue.)
- If I get PA approval, what will my copay be at this pharmacy?
How We Verified This Page
The RX Index is a pricing intelligence and comparison resource for GLP-1 telehealth providers. We are not a medical practice, insurance company, or pharmacy. We don’t prescribe medications or process insurance claims. For this page, we reviewed current public documents from seven Blue-plan sources, manufacturer PA and appeal resources from Novo Nordisk (NovoMedLink and NovoCare), the FDA Wegovy prescribing information, and Ro’s pricing and coverage-checker pages.
| What we could verify from public documents | What no website can verify for you |
|---|---|
|
|
Frequently Asked Questions
Does Blue Cross require prior authorization for Wegovy?
Sometimes. Many Blue plans require prior authorization for Wegovy, but some plans use a formulary-exception process instead, and some plans — including certain BCBS Michigan, BCBS Massachusetts, and Independence Blue Cross populations — exclude weight-loss use entirely. There is no single Blue Cross answer without checking your specific plan.
What BMI does Blue Cross need for Wegovy?
There is no single Blue Cross BMI rule. Public Blue-plan criteria commonly require BMI ≥30, or BMI ≥27 with a qualifying comorbidity such as hypertension, type 2 diabetes, or cardiovascular disease. However, some Blue affiliates use stricter thresholds — BCBS Michigan's historical fully insured large-group lane required BMI ≥35.
What counts as a weight-management program for Wegovy prior authorization?
Most Blue plans require documented evidence of structured lifestyle modification — not just a verbal statement. Acceptable documentation examples from the Highmark PA form include nutritional counseling receipts, wearable device activity summaries showing exercise frequency, and personal trainer records. FEP and BCBSMA reference 'comprehensive weight-management programs' that include behavioral modification, reduced-calorie diet, and increased physical activity.
How long does Blue Cross prior authorization for Wegovy take?
It varies by plan and completeness of paperwork. Blue Shield of California says typical PA processing takes 24 to 72 hours. Ro says its insurance process typically takes 2 to 3 weeks. The gap is almost always explained by incomplete documentation and insurer back-and-forth — a clean first submission with everything attached is the fastest path.
Can Blue Cross deny Wegovy even if it says prior authorization is required?
Yes. Prior authorization means review, not automatic approval. A PA request can be denied for missing documentation, unmet clinical criteria, step-therapy requirements, wrong diagnosis coding, or because the plan excludes the benefit. 'Requires PA' only means the plan is willing to consider coverage if you meet their criteria.
Can you appeal a Blue Cross benefit exclusion for Wegovy?
Usually not through standard PA appeal channels. Novo Nordisk's denial guide notes that benefit exclusions typically do not have standard appeal rights. However, a separate FDA-approved indication (such as cardiovascular risk reduction) may create a different coverage pathway for patients who qualify clinically. You can also request a formulary or medical exception, talk to HR about adding GLP-1 coverage, or switch plans during open enrollment.
Does switching to oral Wegovy require a new prior authorization?
Yes, in at least some Blue plans. BCBS North Dakota explicitly states that members transitioning from Wegovy injectable to Wegovy tablets must obtain a new PA even if they have an existing approval for the injectable. Other Blue affiliates may have similar requirements. Always confirm with your plan before switching formulations.
Does an approved PA guarantee a low copay?
No. PA approval means the plan agrees to cover Wegovy — it does not determine your out-of-pocket cost. Your copay depends on the drug's tier placement, your plan's coinsurance structure, and how much of your deductible you've met. Always ask about cost-sharing when confirming PA status.
Still not sure which GLP-1 program is right for you?
Take our free 60-second matching quiz and get a personalized recommendation based on your insurance, budget, and goals.
Related guides
- GLP-1 providers that accept Blue Cross — full comparison for 2026
- Best Wegovy providers that accept insurance in 2026
- Foundayo (orforglipron) prior authorization — how to get it covered
- Ro Body reviews — FDA-approved GLP-1 with insurance support
- Cheapest GLP-1 options without insurance — full pricing breakdown
- Best compounded GLP-1 providers in 2026 — cash-pay options
- Best GLP-1 telehealth providers compared for 2026
- Orforglipron vs Retatrutide — 2026 data and verdict
The RX Index is a pricing intelligence and comparison resource for GLP-1 telehealth providers. This page is for informational purposes only and does not constitute medical, legal, or insurance advice. Always consult your healthcare provider and insurance plan for guidance specific to your situation.