How to Appeal a Foundayo Denial
Published: · Last updated:
Your pharmacy called. Your portal lit up. Or a letter landed saying Foundayo isn’t covered. Here’s the honest version: many Foundayo denials are fixable, but only when you match the right counter-argument to the right denial reason. Paperwork problems, step therapy, medical-necessity disputes, and missing lifestyle documentation all have real appeal paths. True plan-level category exclusions usually don’t — those need a different move. On most commercial and ACA plans you have 180 days from the denial date to file an internal appeal. Medicare Advantage runs on a shorter 65-calendar-day clock.
This page does three things fast: tells you whether your denial is fixable, gives you the exact packet to send, and shows you what to do if appealing isn’t the right fight. You’ll find a denial triage matrix, a packet checklist, a deadline table, and a provider-stated vs. verified self-pay comparison.
Why Foundayo denials are everywhere right now
Foundayo launched on April 1, 2026. Commercial formularies, payer prior-authorization criteria, and pharmacy claims systems are still settling. A large share of early Foundayo denials aren’t a final “no” — they’re a launch-phase coverage or documentation problem that looks permanent but often isn’t.
Most of what triggers these early denials is fixable — but only if you know which fight you’re actually in.
Can you actually appeal a Foundayo denial?
Almost always yes — but the real question is which of four moves is right for your specific denial. The right move depends entirely on what your denial letter says.
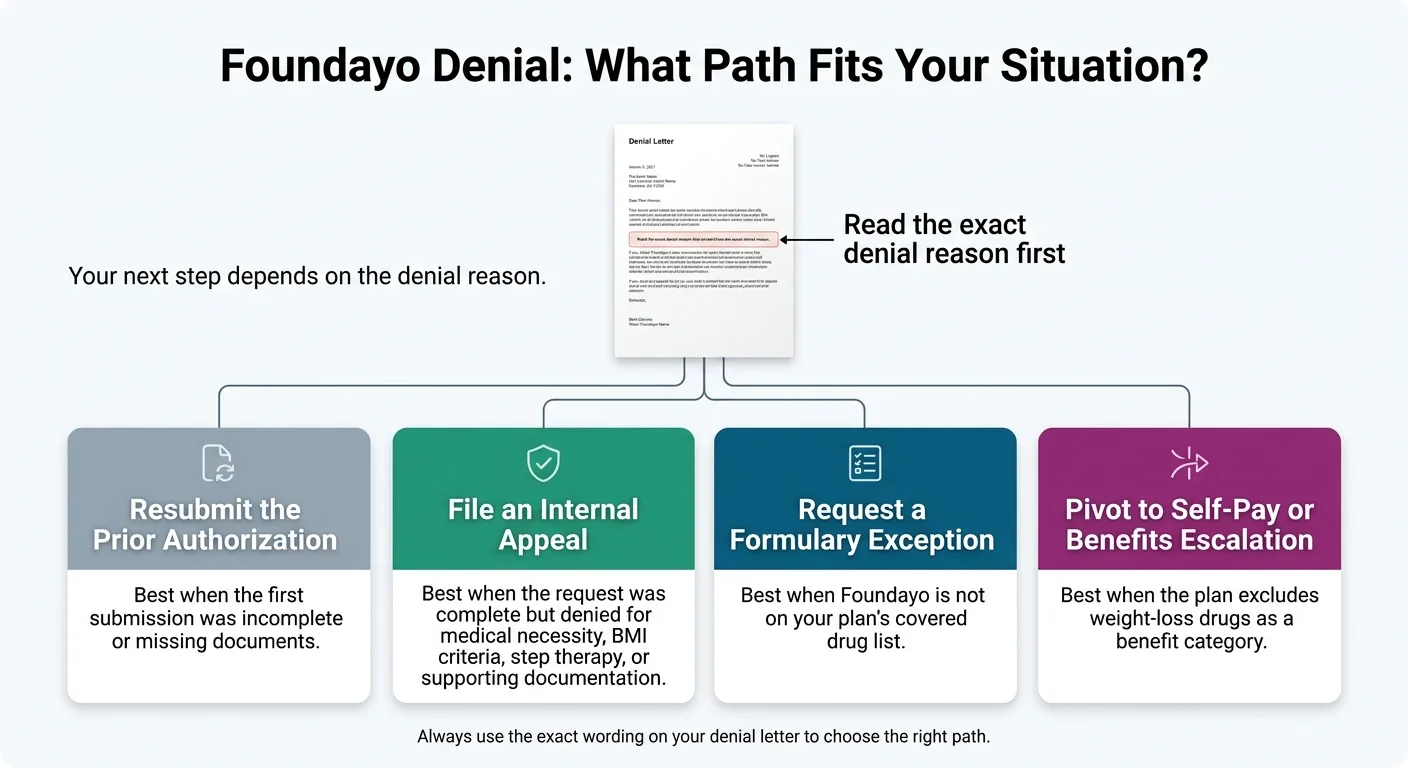
Path 1 — Resubmit the prior authorization
When your doctor’s office sent an incomplete PA the first time — missing BMI, missing diagnosis code, missing lifestyle documentation — a clean resubmission is usually faster than a formal appeal. No new forms, no formal deadline clock, just a corrected packet routed back through the PA process. This is the most underrated move in the denial playbook.
Path 2 — File a formal internal appeal
When the original PA was complete and the plan still denied it, or when the denial is about medical necessity, step therapy, or a BMI judgment. On most commercial and ACA plans you have 180 days from the denial to file, and decisions must come back within 30 days (pre-service) or 60 days (post-service).
Path 3 — Request a formulary exception
When the denial says Foundayo simply isn’t on your plan’s covered drug list. You’re asking the plan to cover a non-formulary drug because no covered alternative works clinically. This has its own form and process — generally lower success odds than a medical-necessity appeal, but it exists and is worth attempting.
Path 4 — Stop and pivot
When your plan has a blanket category exclusion for weight-loss medications — meaning your employer explicitly carved out all anti-obesity drugs from the benefit. A standard appeal rarely moves a contract provision. Self-pay via Ro (with an insurance concierge still working your coverage), LillyDirect, or Sesame Care is almost always the faster answer.
The Foundayo Denial Triage Matrix
Your denial letter names one of roughly eight reasons, and each has a different counter-argument, a different evidence packet, and a different realistic likelihood of success. Use your denial letter’s exact phrasing to find your row.
The “Practical verdict” column is our editorial calibration based on reported appeal-overturn patterns across GLP-1 medications. It is not a guaranteed win rate — your specific plan, denial language, and documentation quality matter more than any benchmark.
| Denial language on your letter | What it usually means | Best next move | What to attach | Practical verdict |
|---|---|---|---|---|
| “Medical necessity not demonstrated” | Chart note, diagnosis codes, comorbidities, or LMN didn’t satisfy the plan’s internal rules | Formal internal appeal | Updated chart note with dated BMI, comorbidity ICD-10 codes, denial-specific LMN, prior-therapy history | Usually appealable with a strong clinical record |
| “Missing or insufficient lifestyle documentation” | Plan requires 3–6 months of documented diet/exercise/behavioral attempts | Formal appeal with documentation | Nutrition visit notes, structured-program enrollment (WW, Noom, CDC DPP), dietitian records, fitness-tracker data, clinician attestation | Usually appealable when the history exists and is dated |
| “BMI criteria not met” | Chart BMI is outdated, missing a date, or you genuinely don’t meet the threshold | Resubmit if chart is fixable; appeal only if you can document the threshold | Dated height/weight measurement, comorbidity diagnosis for BMI 27–29.9, updated vitals | Depends on whether the chart matches the label threshold |
| “Step therapy required” | Plan wants you to try and fail phentermine, Contrave, Qsymia, or metformin first | Formal appeal — step-therapy exception | Prior medication history with dates, doses, outcomes; documented side effects or contraindications; clinician rationale for Foundayo now | Often appealable when prior failure or contraindication is clean |
| “Missing clinical information” / “incomplete submission” | PA packet was too thin — insurer couldn’t even evaluate | Resubmit the PA first (Path 1) | Corrected PA with all chart notes, diagnosis codes, starting weight, current weight | High-fixability — often resolved without a formal appeal |
| “Drug not on formulary” | Foundayo isn’t on your plan’s covered drug list | Formulary exception request, then formal appeal if denied | LMN explaining why covered alternatives aren’t appropriate, documented failures with other GLP-1s if applicable, denial letter | Harder than a standard PA denial; exception process is different |
| “Weight-loss drugs excluded” / “Not a covered benefit category” | Your employer or insurer carved out all anti-obesity medications as a benefit design choice | HR/benefits escalation or self-pay is usually faster | Plan language, benefits-department contact, exception request with LMN (for completeness, but low-yield) | Usually low-yield through a standard appeal |
| “Reauthorization denied” / “Insufficient treatment response” | You were on Foundayo, the refill got blocked, and the plan wants proof of continued benefit | Formal appeal with continuation evidence | Starting weight before Foundayo, current weight, weight-loss percentage, refill history showing adherence, clinician note documenting clinical benefit | Appealable when the clinical response exists and is documented |
Insurers sometimes use hybrid language (“medical necessity not demonstrated per plan criteria, specifically lifestyle documentation”) that straddles two rows. When this happens, treat it as both denial types and build a packet that addresses both.
What to put in your Foundayo appeal packet
A complete Foundayo appeal packet contains seven components in a specific order: your denial notice, your plan’s coverage document, a denial-specific Letter of Medical Necessity, dated BMI and comorbidity documentation, prior-therapy and lifestyle history, your appeal cover letter, and proof of submission.
Every piece has a job. Missing any one of them is usually how otherwise-winnable appeals get rejected on procedural grounds.

| # | Document | Why it matters / what to read it for | Who provides it |
|---|---|---|---|
| 1 | Denial notice (EOB or PA denial letter) | Read for: exact denial reason phrase, appeal deadline, submission address, whether peer-to-peer review is offered | Your insurer — member portal, mail, or email. Call member services if you don’t have it. |
| 2 | Plan coverage document (EOC or Summary of Benefits) | Confirms your specific coverage rules, formulary tier, PA criteria, and whether Foundayo is listed at all | Member portal or your employer’s benefits site |
| 3 | Letter of Medical Necessity (denial-specific) | The most important document. Must address the exact denial reason and connect your clinical picture to the FDA label criteria (BMI ≥30, or ≥27 + weight-related comorbidity). Generic LMNs fail. | Your prescribing physician — must be specific to this denial, not a re-send of the original |
| 4 | BMI and comorbidity documentation | Dated height/weight measurements (not a single reading — typically from recent office visits), ICD-10 codes for qualifying comorbidities (T2D, HTN, OSA, dyslipidemia, CVD, etc.), relevant labs (A1c, BP readings, lipid panel) | Your medical records; your prescriber can pull from the EHR |
| 5 | Prior-therapy and lifestyle history | Prior medication history with dates, doses, and outcomes (especially if step therapy is required); nutrition visit notes; structured-program enrollment (WW, Noom, CDC DPP); dietitian records; Wisconsin’s published PA criteria is one documented example requiring a weight-loss treatment plan within 6 months | Your medical records + program enrollment confirmation |
| 6 | Appeal cover letter | Opens with the exact denial reason phrase from the letter, states why the denial was incorrect, indexes every attached document with tab numbers, and references the relevant FDA label language and your plan’s own coverage criteria. Keep it under 2 pages. | You and/or your prescriber’s office |
| 7 | Proof of submission | Screenshot of portal upload confirmation, certified-mail receipt, or fax confirmation. Your appeal deadline protection depends on proving you filed within the window. | Save immediately upon submission |
$39 first month, then $149/month. Ro handles prior authorization and appeal submissions on your behalf while you start Foundayo through LillyDirect pricing. (Partner link — does not change what you pay.)
Should you resubmit the PA — or file a formal appeal?
Resubmit when the original prior authorization was obviously incomplete. File a formal appeal when the PA was complete and the plan still denied it. The two paths have different speeds and different rules, and picking the wrong one can cost weeks.
| Your situation | Best move | Typical speed |
|---|---|---|
| Original PA was missing documents the plan now says it needs | Resubmit with the missing documents | Days to two weeks |
| Original PA was complete but denied for “medical necessity not demonstrated” | Formal internal appeal with LMN | 30 days (pre-service) / 60 days (post-service) |
| Original PA was denied for step therapy | Formal appeal with step-therapy exception | Standard internal-appeal timing |
| Foundayo isn’t on formulary | Formulary exception request, then appeal if denied | Varies; exception decisions often quick |
| Plan excludes all weight-loss drugs | HR/benefits escalation or self-pay; standard appeal rarely works | Situation-specific |
| Urgent clinical situation | Expedited internal appeal + simultaneous external review request | Expedited external review must be decided within 72 hours |
How long do you have to appeal?
| Stage | Your deadline to file | Insurer’s deadline to decide |
|---|---|---|
| Internal appeal — commercial/ACA (pre-service) | 180 days from denial | 30 days |
| Internal appeal — commercial/ACA (post-service) | 180 days from denial | 60 days |
| Internal appeal — Medicare Advantage reconsideration | 65 calendar days from the notice | Per CMS MA-appeals rules |
| External review request (commercial/ACA) | Up to 4 months from final internal denial | — |
| External review (standard) | — | 45 days |
| External review (expedited) | — | 72 hours |
“Urgent” in insurance-regulatory terms is a high bar — generally a situation where standard timing would seriously jeopardize the patient’s life, health, or ability to regain maximum function. For chronic weight management, that bar usually isn’t met on its own. If your prescriber can document a situation that clears it, you can request expedited internal appeal and simultaneous expedited external review.
“Drug not on formulary” vs. “weight-loss drugs excluded” — why it matters
These two denials look similar but require completely different responses. Conflating them is how otherwise-winnable appeals get filed at the wrong target.
- HR/benefits escalation (for employer-sponsored plans). Employers sometimes add GLP-1 coverage mid-year when enough employees ask. A well-written email to benefits, with your clinical situation and the business case (productivity, chronic-disease cost reduction, retention), occasionally works — but slowly.
- Open enrollment switch. If another plan at your employer covers GLP-1s for obesity, switch when the window opens. Gather your BMI and comorbidity documentation now to pre-qualify.
- Self-pay bridge while your HR conversation plays out. Ro’s insurance concierge keeps working your coverage while you pay cash. See the comparison table below.
Medicare and Foundayo — the GLP-1 Bridge and BALANCE Model
Medicare has historically not covered GLP-1s for weight loss at all. That changes with the CMS Medicare GLP-1 Bridge, which runs July 1, 2026 through December 31, 2027 (18 months). BALANCE did not launch for Medicare Part D in 2027 — CMS extended the Bridge. Foundayo is on the eligible Bridge drug list. If you were denied Foundayo coverage under Medicare before July 1, 2026, the denial is technically correct under current rules — but the door opens this summer.
Medicare GLP-1 Bridge eligibility criteria (per CMS)
You must meet one of the following at the time therapy begins:
| Phase | Timeline | Cost | Who it affects |
|---|---|---|---|
| Medicare GLP-1 Bridge | July 1, 2026 – December 31, 2027 (18 months; BALANCE not launching Medicare Part D 2027) | ~$50/month | Eligible Part D beneficiaries meeting CMS criteria |
| BALANCE Model Part D | January 1, 2027 onward | Negotiated pricing via participating Part D plans | Medicare enrollees in participating plans |
What to do while your appeal is pending
You have three legitimate brand-name self-pay paths while an appeal works: Ro, with an insurance concierge that keeps fighting for coverage in the background while you self-pay at LillyDirect-matched prices; LillyDirect, Lilly’s official direct-to-patient channel; or Sesame Care, which offers Foundayo through provider choice with a lower-entry membership. Which one fits depends on whether you want someone working your coverage in parallel or want the cleanest cash transaction possible.
Provider-stated vs. verified — Foundayo self-pay comparison
Every cell was checked on April 20, 2026. We include what each provider publicly states and what we independently verified.
| Feature | Ro | LillyDirect | Sesame Care |
|---|---|---|---|
| Foundayo publicly available | Yes — ro.co/weight-loss/foundayo | Yes — foundayo.lilly.com | Yes — sesamecare.com/medication/foundayo |
| Program/membership cost | $39 first month, then $149/mo; or as low as $74/mo with annual prepay | No membership | Success by Sesame: $59/mo annual; or $99/mo month-to-month |
| Foundayo medication pricing | Matches LillyDirect tiers (verified) | 0.8 mg: $149 · 2.5 mg: $199 · 5.5–9 mg: $299 · 14.5–17.2 mg: $299 (45-day refill) or $349 (regular) | Higher-dose pricing at $299 (45-day refill condition and $349 regular price line not found on Sesame’s public page) |
| Insurance concierge / appeals handling | Yes — handles PA submission and appeal on your behalf | Not advertised | Not advertised as primary feature |
| Free coverage checker | Yes — Ro GLP-1 Insurance Coverage Checker (free, no signup) | No public checker | No public checker |
| Medicare/Medicaid support | Generally not supported for GLP-1 coverage (FEHB is a noted exception) | Self-pay accessible to anyone | Self-pay accessible to anyone |
| Clinical support included | Unlimited provider messaging, titration support, weight tracking, 1:1 health coaching; Quest labs included if ordered | Telehealth evaluation through third-party platform for prescription | Provider choice; messaging and program features in Success by Sesame |
Why we don’t quote a single “appeal success rate”
You’ll see pages claim “80% of appeals succeed.” KFF’s 80.7% figure is specifically for appealed Medicare Advantage prior-authorization denials in 2024 — one narrow slice of the data. Commercial and ACA marketplace denials look different, with fewer appeals filed and insurers upholding a material share of appealed denials. Collapsing this into one headline number misleads readers. What matters is your specific denial type, your plan, and your documentation quality.
Frequently asked questions
Can you actually appeal a Foundayo denial?
In most cases yes. Foundayo denials for medical necessity, step therapy, missing lifestyle documentation, and BMI documentation gaps are all appealable under federal ACA rules, with internal appeal deadlines of 180 days from the denial on most commercial/ACA plans. Denials based on a true plan-level category exclusion for weight-loss medications are technically appealable but rarely succeed through clinical arguments — those typically require HR/benefits escalation or a switch to self-pay.
How long do I have to appeal a Foundayo denial?
On most commercial and ACA plans, 180 days from the denial date for internal appeals, and up to 4 months after a final internal denial to request external review. Medicare Advantage is shorter: 65 calendar days from the date of the notice. Your denial letter is the authoritative source for your specific deadlines.
Should I resubmit the prior authorization or file a formal appeal?
Resubmit when the original prior authorization was incomplete or missing documents. File a formal appeal when the PA was complete and the plan still denied it. Resubmission is often faster when it applies.
What’s the difference between a Foundayo appeal and a formulary exception?
A standard appeal argues that the plan’s criteria were incorrectly applied or that the documentation supports coverage. A formulary exception argues that a non-formulary drug should be covered because formulary alternatives aren’t clinically appropriate for you. Different forms, different processes, different success rates.
Can I start Foundayo while my appeal is pending?
Yes. Many patients start Foundayo through Ro, LillyDirect, or Sesame Care self-pay while an appeal processes. If the appeal wins, you can switch to insurance coverage. If it loses, you continue self-pay. Ro is the option that keeps an insurance concierge working your coverage in the background.
Does Medicare cover Foundayo?
Not under standard Part D rules as of April 2026. Starting July 1, 2026, the CMS Medicare GLP-1 Bridge covers Foundayo at approximately $50/month for eligible Part D beneficiaries meeting CMS clinical criteria (BMI ≥35, or BMI ≥30 with HFpEF / uncontrolled hypertension / CKD stage 3a+, or BMI ≥27 with prediabetes / prior MI / prior stroke / symptomatic PAD). The broader BALANCE Model Part D pathway begins January 1, 2027.
What if my plan excludes all weight-loss medications?
A category exclusion is a plan-design decision, not a clinical disagreement — standard appeals rarely move it. Your realistic paths are HR/benefits escalation (for employer-sponsored plans), switching plans at open enrollment if another plan covers GLP-1s for obesity, or self-pay via Ro (with continued coverage monitoring), LillyDirect, or Sesame Care.
Do I need a lawyer to appeal?
Almost never. Internal appeals and external reviews are designed to be navigable by patients and their prescribers. Consider legal help only after all appeal levels have failed and you believe your insurer acted in bad faith under ERISA.
Is orforglipron the same as Foundayo?
Yes. Orforglipron is the generic name of the active ingredient; Foundayo is Eli Lilly’s FDA-approved brand name.
Does Ro carry Foundayo?
Yes. Ro publicly offers Foundayo, lists Foundayo-specific pricing at ro.co/weight-loss/foundayo, and Ro’s insurance concierge handles prior authorizations and appeals for Foundayo, including for readers currently in a denial appeal process.
Your next step
You now know whether your denial is likely fixable, what to send, and your deadline. If you want someone handling the paperwork while you focus on starting Foundayo, Ro’s insurance concierge handles the PA and the appeal on your behalf.
Related guides
- Foundayo Prior Authorization Guide — if you haven’t filed the PA yet, start here first to minimize the chance of a denial
- Does Insurance Cover Foundayo? — coverage basics by plan type, formulary status, and what to expect from commercial insurance
- Does Medicaid Cover Foundayo? 7 States Checked — Medicaid-specific coverage status, BALANCE Model timeline, and state tracker
- Does Medicare Cover Foundayo? Bridge & BALANCE Model (2026) — Medicare GLP-1 Bridge eligibility, $50/month pathway, and what changes January 2027
- Foundayo Cost Without Insurance: Full Pricing Guide — self-pay pricing for all six doses at every channel
- Foundayo Savings Card 2026: $25, $149, or $349? — commercial insurance savings card eligibility and limits
How we built and verified this page
Written and verified by The RX Index editorial team against primary sources on April 20, 2026. We do not accept payment for placement in our recommendations.
Sources consulted: Foundayo prescribing information (pi.lilly.com); foundayo.lilly.com/coverage-savings for pricing and savings-card eligibility; HealthCare.gov and CMS.gov for internal-appeal (180 days) and external-review (up to 4 months) deadlines; cms.gov/medicare/coverage/prescription-drug-coverage/medicare-glp-1-bridge for Bridge eligibility and dates; cms.gov/medicare/appeals-grievances/managed-care for Medicare Advantage 65-day appeal timing; ro.co/weight-loss/foundayo and ro.co/weight-loss/pricing; sesamecare.com/medication/foundayo; KFF’s 2024 Medicare Advantage prior-authorization analysis (the 80.7% figure is MA-specific, not universal).
Affiliate disclosure: The RX Index may earn commissions when readers sign up with certain providers through our links, including Ro. This does not change the price you pay. We only recommend providers that publicly carry Foundayo, and we lead with Ro on this page because Ro’s insurance concierge is directly relevant to the post-denial use case this page serves. This page is informational only and does not constitute medical advice. Foundayo is a prescription medication with a boxed warning and several contraindications; talk to a licensed provider before starting, stopping, or changing any medication. Last verified: April 20, 2026 · Next scheduled refresh: May 20, 2026.